Comprehensive Surgical Management of Lateral Epicondylitis
Key Takeaway
Lateral epicondylitis, commonly known as tennis elbow, is a degenerative tendinopathy primarily affecting the extensor carpi radialis brevis (ECRB) origin. Characterized by angiofibroblastic hyperplasia rather than acute inflammation, it presents with lateral elbow pain exacerbated by resisted wrist extension. While 95% of cases resolve with nonoperative modalities like physical therapy and biologics, recalcitrant cases require surgical debridement of the ECRB, performed via open, percutaneous, or arthroscopic approaches.
ELBOW TENOPATHIES: LATERAL EPICONDYLITIS
Lateral epicondylitis, universally recognized by the colloquialism "tennis elbow," is a ubiquitous term utilized to describe a myriad of symptoms localized around the lateral aspect of the elbow. Despite its moniker, the condition occurs with significantly greater frequency in non-athletes than in athletes. Epidemiological data demonstrate a peak incidence in the early fifth decade of life, with a nearly equal distribution between genders.
Biomechanically, lateral epicondylitis is precipitated by activities that demand repetitive supination and pronation of the forearm while the elbow is held in near-full extension. First described as a distinct clinical entity by Runge in 1873, the etiology of lateral epicondylitis has been the subject of extensive debate, with nearly 30 different conditions historically proposed as the underlying cause.
Pathoanatomy and Histopathology
Although originally conceptualized and treated as an acute inflammatory process (hence the suffix -itis), contemporary orthopedic consensus unequivocally defines lateral epicondylitis as a degenerative tendinosis initiated by microtearing.
The primary anatomical epicenter of this pathology is the origin of the extensor carpi radialis brevis (ECRB). The ECRB is uniquely vulnerable to microtrauma due to its anatomical position; it courses directly over the lateral epicondyle and the capitellum, subjecting its undersurface to significant sheer forces during repetitive elbow flexion and extension, particularly when coupled with forearm rotation. While the ECRB is the primary culprit, the pathological process can extend to involve the adjacent tendons of the extensor carpi radialis longus (ECRL) and the extensor digitorum communis (EDC).
Clinical Pearl: The histopathological hallmark of lateral epicondylitis is angiofibroblastic hyperplasia. Microscopic evaluation of the diseased tendon reveals a disorganized proliferation of immature reparative tissue, characterized by disorganized collagen, hypercellularity, and neovascularization, with a conspicuous absence of acute inflammatory cells (macrophages, neutrophils).
Clinical Evaluation and Diagnosis
The diagnosis of lateral epicondylitis is primarily clinical, predicated on a meticulous history and physical examination.
Physical Examination Findings:
* Point Tenderness: The pathognomonic sign is exquisite tenderness localized precisely to the origin of the ECRB. This point is anatomically located approximately 5 mm distal and anterior to the midpoint of the lateral epicondyle.
* Provocative Testing: Pain is reliably exacerbated by resisted wrist dorsiflexion (extension) and forearm supination with the elbow in full extension (Cozen's test).
* Functional Deficits: Patients frequently report sharp, shooting pain and subjective weakness when grasping objects, pouring liquids, or shaking hands.
Imaging Modalities:
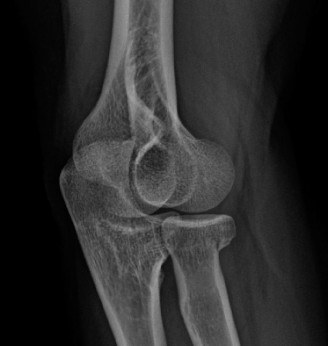
* Radiographs: Plain radiographs of the elbow are typically unremarkable. Occasionally, dystrophic calcification (calcific tendinitis) may be visualized within the extensor origin, or subtle reactive exostosis may be seen at the lateral epicondyle.
* Magnetic Resonance Imaging (MRI): MRI is highly sensitive for evaluating the extent of tendon degeneration. Pathological findings include tendon thickening and increased signal intensity on both T1- and T2-weighted sequences.
* Prognostic Value of MRI: Evidence suggests that the degree of signal alteration correlates with surgical outcomes. Specifically, a high-signal intensity focus on T2-weighted images localized to the ECRB at the lateral epicondyle is highly predictive of excellent outcomes following surgical debridement.
Differential Diagnosis
A critical responsibility of the evaluating surgeon is to differentiate true lateral epicondylitis from other pathologies that generate lateral elbow pain. Misdiagnosis is the leading cause of surgical failure.
- Radial Tunnel Syndrome: This is the most common confounding diagnosis and may coexist with lateral epicondylitis in up to 5% of patients. It is a compressive neuropathy of the posterior interosseous nerve (PIN). Compression can occur at four distinct anatomical sites within the radial tunnel:
- A fibrous band near the anterior aspect of the radiocapitellar joint.
- The vascular leash of Henry (recurrent radial artery).
- The fibrous medial margin of the distal ECRB tendon.
- The arcade of Frohse (the proximal fibrous edge of the superficial head of the supinator).
- Differentiation: Pain in radial tunnel syndrome is typically located 3 to 4 cm distal to the lateral epicondyle over the mobile wad. It may be reproduced by resisted extension of the long finger (Maudsley's test), though this finding, along with electromyography (EMG) abnormalities, can be inconsistent.
- Osteochondritis Dissecans (OCD) of the Capitellum: Typically seen in adolescent throwing athletes or gymnasts. Presents with mechanical symptoms (catching, locking) and radiocapitellar pain.
- Lateral Compartment Arthrosis: Degenerative joint disease of the radiocapitellar articulation. Pain is exacerbated by axial loading and rotation.
- Posterolateral Rotatory Instability (PLRI): Caused by insufficiency of the lateral ulnar collateral ligament (LUCL). Patients report a sensation of the elbow "giving way" when pushing up from a chair.
- Periarticular Ganglion Cysts: Though less common, ganglion cysts arising from the joint capsule can cause localized mass effect or secondary nerve compression.

FIGURE 46-18 Surgical approach for removal of ganglion. SEE TECHNIQUE 46-8.
NONOPERATIVE MANAGEMENT
Regardless of the specific biomechanical trigger, nonoperative management remains the gold standard and is successful in approximately 95% of patients. A structured, phased approach is required.
Phase 1: Acute Symptom Modification
Initial treatment focuses on mitigating pain and halting the cycle of microtrauma. This includes relative rest, cryotherapy, and nonsteroidal anti-inflammatory drugs (NSAIDs)—though the latter primarily provide analgesia rather than altering the non-inflammatory histopathology. Counterforce bracing applied over the proximal forearm muscle belly can effectively dissipate tension forces away from the diseased ECRB origin.
Phase 2: Rehabilitation and Modalities
Physical therapy is the cornerstone of conservative care. Modalities such as ultrasound, iontophoresis, and electrical stimulation may provide symptomatic relief. Manual therapies, including soft tissue mobilization and cross-friction massage, aim to stimulate a healing response. The critical component of therapy is a progressive stretching and eccentric strengthening program for the wrist extensors.
Phase 3: Injections and Biologics
When mechanical therapies plateau, injectable adjuncts are considered.
- Corticosteroid Injections: One or two local injections of a corticosteroid preparation directed at the area of maximal tenderness can provide profound short-term relief. However, long-term data suggest high recurrence rates and potential for tendon atrophy.
- "Completing the Lesion": An older, aggressive adjunct to local anesthetic injection involves forcibly flexing the wrist to intentionally rupture the remaining diseased fibers, theoretically initiating a fresh inflammatory cascade to induce healing.
- Extracorporeal Shock Wave Therapy (ESWT): Early studies were highly promising, but recent randomized controlled trials have yielded conflicting results. Some data indicate no meaningful difference between ESWT combined with stretching versus stretching alone.
- Autologous Blood and Platelet-Rich Plasma (PRP): Biologic augmentation has revolutionized the treatment of recalcitrant tendinopathy. Autologous blood injections have demonstrated up to a 79% success rate in patients failing all other nonoperative measures. More recently, PRP injections—which deliver a concentrated dose of alpha-granules containing growth factors (PDGF, TGF-β, VEGF)—have been reported to be significantly more effective than corticosteroid injections in achieving sustained pain relief and functional improvement.
OPERATIVE MANAGEMENT
Surgical intervention is indicated only after a prolonged period (typically 6 to 12 months) of exhaustive, well-documented nonoperative treatment has failed. In properly selected patients, operative treatment yields a 90% success rate.
Manipulation Under Anesthesia
In patients with concomitant flexion contractures, manipulation under anesthesia has been advocated by some authors. This technique involves sudden, forcible, full extension of the elbow with the wrist and fingers flexed and the forearm pronated. This places the ECRB and common extensors under maximal tension. An audible, palpable snap is frequently elicited as the fibrotic tissue ruptures. While results can be excellent, this represents a highly aggressive, uncontrolled form of "completing the lesion" and is generally superseded by direct surgical debridement.
Open Surgical Techniques
Historically, surgeons utilized extensive procedures, such as the technique popularized by Boyd and McLeod. This radical approach attempted to eliminate all conceivable causes of lateral pain by excising the proximal annular ligament, releasing the entire extensor origin, excising adventitious bursae, and resecting hypertrophic radiocapitellar synovium.
Surgical Warning: Extensive releases that violate the lateral ulnar collateral ligament (LUCL) are the primary cause of iatrogenic posterolateral rotatory instability (PLRI). The modern surgical philosophy strictly dictates a limited, targeted approach.
The Modern Limited Open Approach (Nirschl Procedure):
Currently, the favored technique is a limited, precise excision of the diseased ECRB.
1. Positioning: The patient is positioned supine with the arm draped over a hand table. A tourniquet is applied.
2. Incision: A 3 to 4 cm longitudinal incision is made centered over the lateral epicondyle, extending distally.
3. Exposure: The deep fascia is incised. The interval between the extensor digitorum communis (EDC) and the extensor carpi radialis longus (ECRL) is identified and longitudinally split.
4. Debridement: Retracting the ECRL anteriorly exposes the underlying ECRB origin. The pathological tissue of the ECRB is easily identifiable; it appears grayish, edematous, and friable, contrasting sharply with the glistening white appearance of healthy tendon. This angiofibroblastic tissue is meticulously excised.
5. Decortication: The lateral epicondyle is decorticated or drilled with a Kirschner wire to stimulate bleeding and marrow-derived stem cell migration, fostering a robust healing environment.
6. Repair: The healthy margins of the ECRB and the overlying EDC/ECRL interval are securely repaired side-to-side using non-absorbable sutures.
Percutaneous and Arthroscopic Techniques
Percutaneous Lateral Release:
Percutaneous release has been reported to be as effective as open release in select cohorts. While it does not allow for direct visualization and removal of the diseased tendon, the percutaneous tenotomy triggers an acute inflammatory cascade that leads to the resolution of symptoms.
Arthroscopic Release:
Arthroscopic management of lateral epicondylitis has gained significant traction, offering results equivalent to open procedures with several distinct advantages.
* Intra-articular Evaluation: It allows for concurrent evaluation of the radiocapitellar joint to rule out OCD, loose bodies, or subtle instability.
* Anatomical Preservation: The lesion is treated from the "inside out." The capsule is resected, and the undersurface of the ECRB is debrided without sacrificing or splitting the overlying common extensor origin (EDC/ECRL).
* Technique: Standard proximal anteromedial and anterolateral portals are utilized. The capsule anterior to the radiocapitellar joint is excised to expose the ECRB origin, which is then debrided back to bleeding bone using an arthroscopic shaver and radiofrequency ablation.
MANAGEMENT OF SURGICAL FAILURES
Only a small fraction of patients (1% to 2%) fail to achieve symptomatic relief following surgical intervention. Morrey elegantly divided these surgical failures into two distinct groups based on their postoperative clinical presentation.
Group 1: Unchanged Symptoms
Patients in this cohort report symptoms identical to those experienced prior to surgery.
* Etiology: Failure is almost universally due to either an inadequate surgical release of the ECRB or an incorrect initial diagnosis. The most common missed diagnosis in this group is unrecognized Radial Tunnel Syndrome.
* Management: A rigorous re-evaluation is required. Diagnostic injections into the radial tunnel or EMG studies may be necessary. If radial tunnel syndrome is confirmed, surgical decompression of the posterior interosseous nerve is indicated.
Group 2: Altered Symptom Complex
Patients in this cohort report a different type of pain or mechanical symptoms that were not present preoperatively.
* Etiology: Failure is typically secondary to iatrogenic capsular or ligamentous insufficiency. Overzealous surgical release that inadvertently violates the anterior band of the lateral collateral ligament complex (specifically the LUCL) results in Posterolateral Rotatory Instability (PLRI). Alternatively, failure to close the capsule adequately can result in a synovial fistula.
* Management: A thorough history must determine the exact nature of the new symptoms. Physical examination must focus on instability testing (e.g., the lateral pivot-shift test of the elbow). Advanced imaging, such as MR arthrography, is invaluable for detecting synovial fistulas or LUCL tears. Arthroscopy under anesthesia is the gold standard for definitively diagnosing and subsequently reconstructing iatrogenic instability.
> Clinical Pearl: Recovery following lateral epicondylitis surgery is not instantaneous. The biological remodeling of the tendon origin requires time. Most patients who will ultimately achieve a good result demonstrate significant improvement within 3 to 4 months. It is our institutional protocol to wait a full 12 months before considering repeat surgical intervention for perceived failures, provided iatrogenic instability has been ruled out.
📚 Medical References
You Might Also Like