Plantarflexion Opening Wedge Medial Cuneiform Osteotomy (Cotton Osteotomy): An Intraoperative Masterclass
Key Takeaway
Join us in the OR for a detailed masterclass on the Plantarflexion Opening Wedge Medial Cuneiform (Cotton) Osteotomy. We'll meticulously cover patient selection, comprehensive surgical anatomy, precise intraoperative technique, critical pearls and pitfalls, and essential postoperative management for correcting fixed forefoot varus in adult flatfoot deformity.
Comprehensive Introduction and Patho-Epidemiology
Welcome, colleagues and fellows, to the operating theater and to this advanced surgical masterclass. Today, we are addressing a structurally critical and frequently underappreciated component of multiplanar pes planovalgus deformity: the fixed forefoot varus. Our procedural focus is the Plantarflexion Opening Wedge Medial Cuneiform Osteotomy, universally referred to in the orthopedic lexicon as the Cotton osteotomy. F.J. Cotton originally described this elegant procedure in 1936 as a method to restore the "triangle of support" of the static foot. In the modern era of foot and ankle reconstruction, this osteotomy serves as a powerful, indispensable tool to restore the medial column's sagittal alignment and declination. It is rarely performed in isolation; rather, it is a vital complementary procedure to hindfoot and midfoot reconstructions in the setting of Progressive Collapsing Foot Deformity (PCFD), formerly known as adult acquired flatfoot deformity.
To truly master the Cotton osteotomy, one must first deeply understand the natural history and pathogenesis of the deformity it aims to correct. Forefoot varus, characterized by the first metatarsal resting dorsally to the transverse plane of the lesser metatarsals, is a ubiquitous sequela of PCFD, primarily driven by posterior tibial tendon insufficiency. While the exact temporal natural history of this specific skeletal adaptation has not been exhaustively mapped in longitudinal studies, clinical consensus dictates that it progresses in tandem with the underlying hindfoot valgus and midfoot collapse. Over time, chronic instability and subluxation, particularly at the talonavicular, naviculocuneiform, and first tarsometatarsal (TMT) joints, lead to adaptive capsular contractures and, eventually, localized osteoarthritis.
This complex deformity arises when the posterior tibialis tendon—the paramount dynamic stabilizer of the medial longitudinal arch—undergoes tendinosis, elongation, or rupture. Consequently, the massive weight-bearing forces of the gait cycle are transferred entirely to the static stabilizers. The spring ligament complex (plantar calcaneonavicular ligament), the plantar fascia, and the plantar intertarsal ligaments (including the long and short plantar ligaments) become progressively attenuated under these repetitive, dorsally directed loads. As the hindfoot drifts into valgus, the forefoot must supinate to maintain a plantigrade foot during stance phase. Initially, this forefoot supination is flexible and dynamically driven.
However, as the chronicity of the condition extends, this compensatory forefoot supination becomes a rigid, fixed forefoot varus. This rigidity occurs even in the absence of overt osteoarthritic changes, primarily due to profound capsular stiffness and adaptive shortening of the dorsal soft tissue structures of the midfoot. This fixed elevation of the first ray completely obliterates the medial point of Cotton’s "triangle of support" (the calcaneal tuberosity, the first metatarsal head, and the fifth metatarsal head). While most commonly seen in adult acquired flatfoot, this fixed forefoot varus is also frequently encountered in severe congenital pes planus, neuromuscular disorders, and post-traumatic midfoot collapse.
Detailed Surgical Anatomy and Biomechanics
Before a scalpel ever touches the skin, a profound three-dimensional understanding of the medial column's surgical anatomy is mandatory. The osteology of the medial cuneiform dictates the parameters of our osteotomy. The medial cuneiform is the largest of the three cuneiform bones, uniquely shaped like a wedge with its broad base directed plantarly and its narrow apex directed dorsally—the exact opposite of the middle and lateral cuneiforms. It articulates proximally with the navicular, distally with the base of the first metatarsal, and laterally with the middle cuneiform and the base of the second metatarsal. The osteotomy must be executed precisely through the midsubstance of this bone. The paramount anatomical feature we rely upon during this procedure is the thick, robust plantar cortex and its confluent plantar periosteum and ligamentous attachments. This plantar tissue complex must be preserved to act as a tension band and a mechanical hinge, preventing dorsal displacement of the distal fragment when the wedge is opened.
The muscular intervals and tendinous structures dictate our surgical approach. We utilize a purely dorsal approach to the medial cuneiform. The primary surgical interval is developed between the extensor hallucis longus (EHL) tendon, which is retracted medially, and the extensor hallucis brevis (EHB) tendon, which is retracted laterally. The massive tibialis anterior tendon inserts broadly into the plantar-medial aspect of the medial cuneiform and the base of the first metatarsal. Attempting a medial approach to the cuneiform is fraught with difficulty and morbidity, as it requires extensive, traumatic subperiosteal stripping and retraction of this robust tendon. The dorsal approach beautifully bypasses the tibialis anterior, minimizing soft tissue trauma and preserving the vascular supply to the medial column.
Navigating the neurovascular landscape is critical to avoiding devastating postoperative complications. Superficially, several dorsal cutaneous branches of the superficial peroneal nerve (specifically the medial dorsal cutaneous nerve) arborize across our surgical field. These must be meticulously identified, mobilized, and gently retracted using vessel loops or blunt retractors. Injury to these branches guarantees a painful postoperative neuroma or a highly irritating sensory deficit over the dorsum of the foot. Deep to the superficial fascia, the deep peroneal nerve and the dorsalis pedis artery run in close proximity. Typically, these structures lie deep and slightly lateral to the EHL tendon, often nestled between the EHL and the EHB/extensor digitorum brevis tendons. While a carefully executed dorsal approach keeps these structures relatively safe, aberrant vascular anatomy is common, and the surgeon must maintain strict awareness of the dorsalis pedis pulse throughout the deep dissection.
Biomechanically, the Cotton osteotomy is a marvel of leverage. By inserting a wedge into the dorsal aspect of the medial cuneiform, we hinge the bone on its intact plantar cortex. This effectively plantarflexes the entire first ray (the distal fragment of the cuneiform and the first metatarsal). This maneuver achieves three critical biomechanical goals: it recreates the medial longitudinal arch, it restores the declination angle of the first metatarsal, and it re-establishes the medial weight-bearing pillar of the foot. By bringing the first metatarsal head back down to the transverse plane of the lesser metatarsals, we eliminate the lateral column overload that plagues these patients and restore a functional, propulsive tripod for the terminal stance phase of gait.
Exhaustive Indications and Contraindications
Patient selection is the crucible in which the success of a Cotton osteotomy is forged. When evaluating patients with PCFD, they will consistently describe localized, aching pain along the dorsal medial column of the midfoot, specifically targeting the tarsometatarsal or naviculocuneiform joints. Pressure-related discomfort beneath the base of the first metatarsal or cuneiform is also a hallmark complaint, representing a direct mechanical result of excessive weight-bearing at the apex of the plantar medial column sag.
The physical examination is the definitive tool for quantifying this deformity. We must isolate the forefoot from the hindfoot. To do this, the patient is seated, and the examiner grasps the calcaneus, placing the hindfoot into strict "subtalar neutral" position. This is the anatomical equivalent of the Silfverskiöld test for the midfoot.
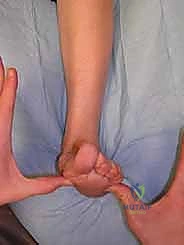
With the hindfoot locked in neutral and the talonavicular joint congruently reduced, the examiner applies a dorsally directed force to the fourth and fifth metatarsal heads until the ankle is dorsiflexed to a neutral, 90-degree position.
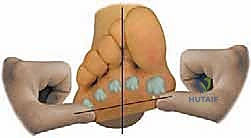
At this exact moment, the examiner sights down the longitudinal axis of the foot. If the first metatarsal head rests visibly above the transverse plane of the fifth metatarsal, forefoot varus is definitively present. We clinically quantify this elevation as mild, moderate, or severe.
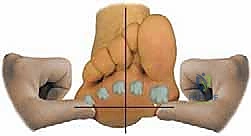
Crucially, the examiner must then apply plantarward pressure to the first metatarsal head to assess flexibility. If the first ray cannot be passively brought down to the level of the lateral column, the deformity is fixed. A fixed forefoot varus in the setting of a symptomatic flatfoot is the absolute, primary indication for a Cotton osteotomy. If the deformity is entirely flexible, soft tissue procedures (like a spring ligament repair or tendon transfer) combined with hindfoot bony correction may suffice. If there is frank, bone-on-bone osteoarthritis at the first TMT joint, a Cotton osteotomy is contraindicated, and a Lapidus procedure (first TMT arthrodesis) must be performed instead to achieve both correction and pain relief.
| Category | Specific Conditions | Clinical Rationale |
|---|---|---|
| Primary Indications | Fixed forefoot varus in PCFD/AAFD | Restores medial column weight-bearing and arch height. |
| Residual forefoot supination after hindfoot correction | Prevents lateral column overload post-calcaneal osteotomy. | |
| Congenital pes planovalgus with rigid medial column | Re-establishes the anatomical tripod of the foot. | |
| Relative Contraindications | Mild, passively correctable forefoot varus | May be managed with orthotics or soft tissue balancing alone. |
| Osteopenia or osteoporosis | High risk of plantar hinge fracture and hardware failure. | |
| Absolute Contraindications | Frank osteoarthritis of the 1st TMT or NC joints | Requires arthrodesis (e.g., Lapidus) for definitive pain relief. |
| Active midfoot infection or osteomyelitis | Hardware and allograft placement will harbor infection. | |
| Severe peripheral arterial disease (PAD) | High risk of wound necrosis and nonunion over the dorsal midfoot. |
Pre-Operative Planning, Templating, and Patient Positioning
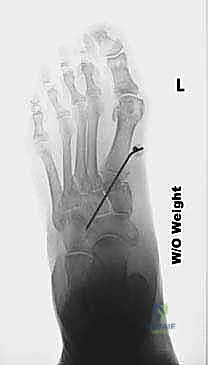
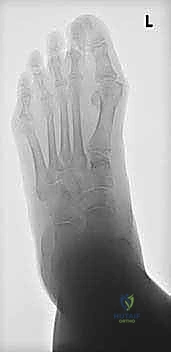
Thorough preoperative radiographic assessment is non-negotiable for precise surgical execution. We require standard weight-bearing anteroposterior (AP), lateral, and medial oblique views of the involved foot. These images are scrutinized to rule out disqualifying osteoarthritis at the first tarsometatarsal or naviculocuneiform joints. The weight-bearing lateral radiograph is the most critical image for our templating. On this view, we measure the lateral talo-first metatarsal angle (Meary's angle) to quantify the exact degree of dorsal elevation of the first ray. We must also definitively identify the apex of the sagittal deformity. While the Cotton osteotomy corrects deformity at the cuneiform level, if the primary apex of collapse is severely localized to the talonavicular joint, isolated cuneiform correction may be biomechanically insufficient.
Templating the size of the opening wedge is a vital preoperative step. Based on the lateral talo-first metatarsal angle and the clinical examination of the first ray's elevation, we calculate the required base width of the dorsal wedge. Typically, a 4 to 7 mm wedge is required to achieve adequate plantarflexion. A general biomechanical rule of thumb is that every 1 mm of dorsal wedge opening results in approximately 2 to 3 degrees of first ray plantarflexion, though this varies based on the AP length of the patient's medial cuneiform. We must also plan for our graft material. In our institution, a frozen tricortical iliac crest allograft is the gold standard. It provides immediate structural integrity, eliminates donor site morbidity, and demonstrates excellent incorporation rates in the highly vascularized cancellous bed of the cuneiform.
Patient positioning is designed to optimize dorsal midfoot exposure and facilitate intraoperative fluoroscopy. The patient is placed strictly supine on the operating table. Because the lower extremity naturally rests in external rotation, we place a gel pad or a rolled blanket under the ipsilateral gluteal region. This internally rotates the limb, bringing the foot into a perfectly neutral, "toes-up" position, which is critical for assessing the rotational and sagittal alignment of the foot intraoperatively.
A pneumatic tourniquet is applied high on the ipsilateral thigh. A completely bloodless field is not just a convenience; it is an absolute requirement for the meticulous identification of the superficial peroneal nerve branches and the precise execution of the osteotomy. The C-arm fluoroscopy unit is positioned on the contralateral side of the table (or distally, depending on room setup), draped sterilely, and verified to easily swing between true AP and lateral projections of the midfoot before the patient is prepped and draped.
Step-by-Step Surgical Approach and Fixation Technique
With the patient prepped, the tourniquet inflated, and the surgical time-out completed, we commence the procedure.
Incision and Superficial Dissection
We begin with a dorsal longitudinal skin incision, approximately 5 to 6 cm in length. This incision is centered precisely over the palpable prominence of the medial cuneiform, extending slightly distally towards the diaphyseal base of the first metatarsal. We utilize a sharp scalpel through the epidermis, immediately switching to blunt, spreading dissection with Metzenbaum scissors through the subcutaneous tissues. This is the danger zone for the medial dorsal cutaneous nerve. We meticulously sweep the subcutaneous fat, identifying any crossing neural branches. These are gently mobilized with fine silastic vessel loops and retracted out of the working window.
Deep Dissection and Interval Development
Once the superficial fascia is breached, we identify our muscular interval. The extensor hallucis longus (EHL) tendon is easily visualized; it is mobilized and retracted medially using an Army-Navy or a Senn retractor. The extensor hallucis brevis (EHB) muscle belly and tendon are identified and retracted laterally. Deep to this interval lies the dorsal periosteum of the medial cuneiform. We utilize a Cobb elevator or a scalpel to incise the periosteum longitudinally, elevating small medial and lateral flaps to expose the bare dorsal bone. We must clearly identify the first tarsometatarsal joint distally and the naviculocuneiform joint proximally to ensure our osteotomy remains extra-articular. Crucially, we do not violate the joint capsules.
Executing the Osteotomy
We bring in the C-arm to fluoroscopically verify the exact midpoint of the medial cuneiform in the sagittal plane. I utilize a sterile marker or the edge of an osteotome to score a transverse line across the dorsal cortex.
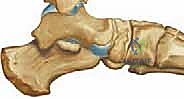
Using a microsagittal saw with a fine, sharp blade, we begin the osteotomy. The cut is made in a strict dorsal-to-plantar direction. Copious cold saline irrigation is applied directly to the saw blade to prevent thermal necrosis of the bone, which is a primary cause of nonunion. The critical technical pearl here is depth control: we saw through the dorsal, medial, and lateral cortices, and through the cancellous bone, but we stop precisely short of the plantar cortex.
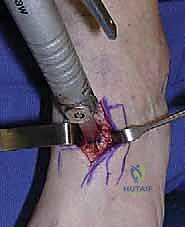
Once the dorsal 80% of the bone is cut, we abandon the saw. We insert a thin, broad osteotome into the cut and gently tap it with a mallet to complete the osteotomy through the remaining cancellous bone, relying on tactile feedback to ensure the plantar cortex and periosteum remain completely intact. This intact plantar hinge is the linchpin of the entire procedure.
Opening the Wedge and Graft Impaction
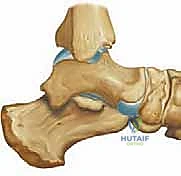
With the osteotome fully seated in the osteotomy, the surgeon gently levers the handle distally. This utilizes the intact plantar cortex as a hinge, opening a dorsal wedge and driving the first metatarsal head into profound plantarflexion.
Alternatively, a specialized lamina spreader or a Hintermann retractor can be inserted into the osteotomy to dial in the exact amount of opening required. We assess the correction clinically by loading the lateral column and verifying that the first metatarsal head now rests congruently on the same plane as the lesser metatarsals.
We measure the dorsal gap with a caliper. The tricortical allograft is then fashioned on the back table using a saw or rongeurs to perfectly match this measured gap, creating a trapezoidal wedge.

The graft is tapped into place, ensuring the cortical edge of the graft sits flush with the dorsal cortex of the cuneiform.
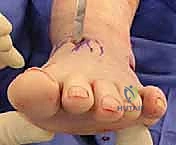
Fixation and Closure
While an intact plantar hinge makes this a highly stable construct, rigid internal fixation is strongly recommended to prevent graft extrusion and micromotion. Fixation options include a dorsal spanning titanium plate with locking screws, memory-compression staples, or independent lag screws.
My preference is a low-profile dorsal spanning plate, which provides excellent biomechanical stability against dorsal bending moments.
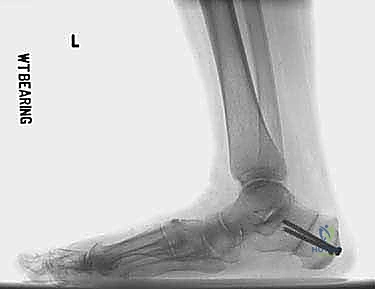
Once fixation is applied, final fluoroscopic images are obtained to confirm hardware placement, graft position, and the restoration of Meary's angle.
The wound is irrigated, the periosteum is closed if possible, and the extensor retinaculum is reapproximated to prevent tendon bowstringing. The skin is closed with non-absorbable sutures, and a well-padded, sterile compression splint is applied with the foot held in neutral.
Complications, Incidence Rates, and Salvage Management
Despite meticulous surgical technique, complications can occur, and the master surgeon must be prepared to manage them. The most dreaded intraoperative complication is the inadvertent fracture or transection of the plantar hinge. This immediately converts a highly stable opening wedge osteotomy into a grossly unstable, multi-fragmentary defect. If the hinge is lost, the distal fragment will inevitably translate dorsally, completely negating the intended plantarflexion. The salvage for this requires immediate transition to rigid, heavy-duty dorsal plate fixation, often requiring compression across the graft and potentially the addition of a plantar-to-dorsal independent lag screw to capture the plantar fragments.
Nonunion and delayed union are significant concerns, particularly given the use of structural allograft. While the medial cuneiform is highly vascular, patient factors such as smoking, uncontrolled diabetes mellitus, and prolonged corticosteroid use drastically increase nonunion rates. Thermal necrosis from aggressive saw use without irrigation is an iatrogenic cause. If a symptomatic nonunion occurs (typically diagnosed via CT scan at 4-6 months post-op), salvage involves revision surgery. This requires removal of hardware, aggressive debridement of the nonunion site down to bleeding bone, grafting with autologous iliac crest bone graft (ICBG) or bone marrow aspirate concentrate (BMAC), and revision rigid plating.
Malcorrection—either overcorrection or undercorrection—can lead to severe functional impairment. Overcorrection (inserting too large a wedge) creates a rigidly plantarflexed first ray. This results in massive overload of the first metatarsal head, leading to intractable sesamoiditis, painful callosities, and potentially plantar ulceration in neuropathic patients. Undercorrection fails to resolve the forefoot varus, leaving the patient with persistent lateral column overload and pain at the base of the fifth metatarsal. Salvage for severe malcorrection often requires a corrective first TMT arthrodesis (Lapidus) to definitively realign the ray.
| Complication | Estimated Incidence | Prevention and Salvage Management |
|---|---|---|
| Plantar Hinge Fracture | 2% - 5% | Prevention: Stop saw early; use osteotome for final cut. Salvage: Rigid dorsal locking plate; consider plantar-directed lag screw. |
| Symptomatic Nonunion | 3% - 8% | Prevention: Copious saw irrigation; strict NWB protocol; smoking cessation. Salvage: Revision with autograft (ICBG) and rigid internal fixation. |
| Overcorrection (Sesamoiditis) | 1% - 4% | Prevention: Precise preoperative templating; intraoperative clinical assessment of the tripod. Salvage: Accommodative orthotics; rarely, revision osteotomy or Lapidus. |
| Superficial Peroneal Neuroma | 3% - 7% | Prevention: Meticulous blunt dissection; gentle retraction with vessel loops. Salvage: Gabapentinoids; targeted steroid injections; surgical neurectomy and burying into muscle. |
| Hardware Prominence/Pain | 5% - 10% | Prevention: Use low-profile plates or staples; ensure flush seating on bone. Salvage: Routine hardware removal after complete radiographic union (usually >6 months). |
Phased Post-Operative Rehabilitation Protocols
The postoperative rehabilitation following a Cotton osteotomy is rigorous and demands strict patient compliance, particularly because this procedure is almost universally performed alongside major hindfoot reconstructions (e.g., medializing calcaneal osteotomy, lateral column lengthening).
Phase I: Maximum Protection (Weeks 0-2)
Immediately postoperatively, the patient is placed in a bulky, well-padded posterior splint with a U-shaped stirrup, locking the ankle in neutral to prevent Achilles contracture. The patient is strictly non-weight-bearing (NWB) on the operative extremity. The primary goals during this phase are wound healing, strict edema control via continuous elevation (toes above the nose), and pain management. At the two-week mark, the patient returns to the clinic for splint removal, wound inspection, and suture removal.
Phase II: Controlled Immobilization (Weeks 2-6)
Following suture removal, the patient is transitioned into a tall, rigid controlled ankle motion (CAM) boot. Strict non-weight-bearing is typically maintained for a total of 6 weeks to allow for initial incorporation of the structural allograft and to protect concomitant hindfoot osteotomies. During this phase, patients are encouraged to perform active range of motion (ROM) exercises of the toes to prevent extensor tendon adhesions, which are common given the dorsal surgical approach. Proximal joint conditioning (knee and hip) is encouraged.
Phase III: Progressive Loading (Weeks 6-12)
At the 6-week postoperative visit, weight-bearing radiographs (AP, lateral, oblique) are obtained out of the boot. We look for the obliteration of the osteotomy lines and the incorporation of the allograft. If radiographic healing is progressing satisfactorily, the patient begins a progressive weight-bearing protocol in the CAM boot, advancing from touch-down weight-bearing to full weight-bearing over a 2-to-4 week period. Formal physical therapy is initiated, focusing on gentle active and active-assisted ROM of the ankle and midfoot, intrinsic foot muscle strengthening, and progressive posterior tibial tendon therapy.
Phase IV: Return to Function (Months 3-6+)
Once the patient is ambulating pain-free in the CAM boot (typically around 8-10 weeks), they are transitioned into a supportive, stiff-soled athletic shoe. We frequently prescribe custom-molded orthotics with medial arch support to protect the reconstruction long-term. Physical therapy intensifies, focusing on proprioception, balance training, and gait normalization. Return to high-impact activities or heavy labor is generally restricted until 6 months postoperatively, contingent upon complete radiographic union and the recovery of dynamic medial column strength.
Summary of Landmark Literature and Clinical Guidelines
The evolution of the Cotton osteotomy is a fascinating journey through orthopedic history. F.J. Cotton's seminal 1936 paper, "Foot statics and surgery," introduced the concept of driving the medial column down to restore the static tripod of the foot. However, the procedure largely fell into obscurity for decades, as the orthopedic community favored arthrodesis for midfoot deformities. It wasn't until the late 1990s and early 2000s, with the paradigm shift towards joint-sparing reconstructions for adult acquired flatfoot, that the Cotton osteotomy experienced a massive resurgence.
Biomechanical studies have definitively validated Cotton's original theories. Landmark cadaveric research has demonstrated that isolated hindfoot corrections (like a medializing calcaneal osteotomy) often fail to fully restore the medial longitudinal arch if a fixed forefoot varus is left un
