Orthopaedic Management of Systemic Arthropathies: Reiter Syndrome, Gout, and Systemic Lupus Erythematosus
Key Takeaway
Systemic arthropathies such as Reiter syndrome, gout, and systemic lupus erythematosus frequently present with profound musculoskeletal manifestations. While primary management is medical, orthopaedic intervention is critical for complications like tophaceous nerve compression, tendon rupture, and severe soft-tissue hand deformities. This guide details the pathophysiology, biomechanics, and step-by-step surgical strategies required to restore function and alleviate pain in patients suffering from these complex connective tissue and crystal deposition diseases.
INTRODUCTION TO SYSTEMIC ARTHROPATHIES IN ORTHOPAEDICS
Systemic arthropathies encompass a diverse group of inflammatory, autoimmune, and crystal deposition diseases that profoundly affect the musculoskeletal system. While the cornerstone of management for conditions such as Reiter syndrome (reactive arthritis), gout, and systemic lupus erythematosus (SLE) remains pharmacological, the orthopaedic surgeon plays a critical role in managing the mechanical and structural sequelae of these diseases. From the acute diagnostic dilemma of a swollen, erythematous joint to the complex reconstruction of a severely deformed hand, a rigorous understanding of the underlying pathophysiology, biomechanics, and surgical indications is paramount for the practicing orthopaedic consultant.
REITER SYNDROME (REACTIVE ARTHRITIS)
Reiter syndrome, now more commonly referred to within the spectrum of reactive arthritis, is classically described by the clinical triad of conjunctivitis, non-gonococcal urethritis, and synovitis. It is an autoimmune condition that develops in response to an infection in another part of the body (cross-reactivity), most notably the genitourinary or gastrointestinal tracts.
Pathophysiology and Clinical Presentation
The condition is strongly associated with the HLA-B27 human leukocyte antigen, placing it within the family of seronegative spondyloarthropathies. The synovitis typically presents as an asymmetrical oligoarthritis, involving four or fewer joints. It exhibits a strong predilection for the lower extremities over the upper extremities, frequently affecting the knees, ankles, and feet.
Beyond the classic triad, patients frequently present with profound enthesopathy—inflammation at the insertion sites of tendons and ligaments into bone. This manifests clinically as severe heel pain (insertional Achilles tendinopathy or plantar fasciitis), back pain (sacroiliitis), and dactylitis ("sausage digits"). Nail deformities, such as pitting and onycholysis, may also occur, making the clinical distinction between Reiter syndrome and psoriatic arthritis challenging.
Clinical Pearl: The presence of keratoderma blennorrhagicum (hyperkeratotic skin lesions on the palms and soles) and circinate balanitis are highly specific mucocutaneous findings that can help differentiate Reiter syndrome from other seronegative arthropathies.
Orthopaedic Management and Surgical Indications
The natural history of Reiter syndrome is generally favorable. Approximately 90% of patients experience a complete remission of symptoms after several weeks to months of targeted medical therapy (NSAIDs, corticosteroids, and disease-modifying antirheumatic drugs [DMARDs]). However, in about 10% of cases, the disease follows a chronic, relapsing course.
Because the primary pathology is a systemic inflammatory response rather than primary mechanical joint destruction, surgery is rarely indicated. Orthopaedic involvement is typically limited to:
* Diagnostic Aspiration: To rule out septic arthritis in the acutely swollen, hot joint.
* Management of Recalcitrant Enthesopathy: In chronic cases where conservative measures (orthotics, physical therapy, judicious corticosteroid injections) fail, surgical debridement of the Achilles insertion or plantar fascia release may be considered, though outcomes are less predictable than in non-inflammatory cohorts.
* Joint Arthrodesis or Arthroplasty: Reserved strictly for the rare subset of patients who develop end-stage secondary osteoarthritis due to chronic, destructive synovitis.
GOUTY ARTHROPATHY AND CRYSTAL DEPOSITION DISEASE
Gout is a disorder of purine metabolism characterized by hyperuricemia and the subsequent deposition of monosodium urate (MSU) crystals in joints, tendons, and periarticular soft tissues. It predominantly affects men and postmenopausal women.
Acute Gout vs. Orthopaedic Emergencies
The acute gouty attack is often sudden, presenting with severe, unremitting pain, typically monoarticular. The first metatarsophalangeal (MTP) joint is the most common site (podagra), though the knee, ankle, and midfoot are frequently involved. The joint becomes massively swollen, erythematous, hot, and exquisitely tender.
Surgical Warning: An acute gout flare can perfectly mimic a severe cellulitis, abscess, or septic arthritis. Direct trauma to an inflamed gouty joint is exceptionally painful. Aspiration and synovial fluid analysis (demonstrating negatively birefringent, needle-shaped MSU crystals under polarized light) are mandatory to rule out concurrent or isolated joint sepsis before initiating high-dose corticosteroid or colchicine therapy.
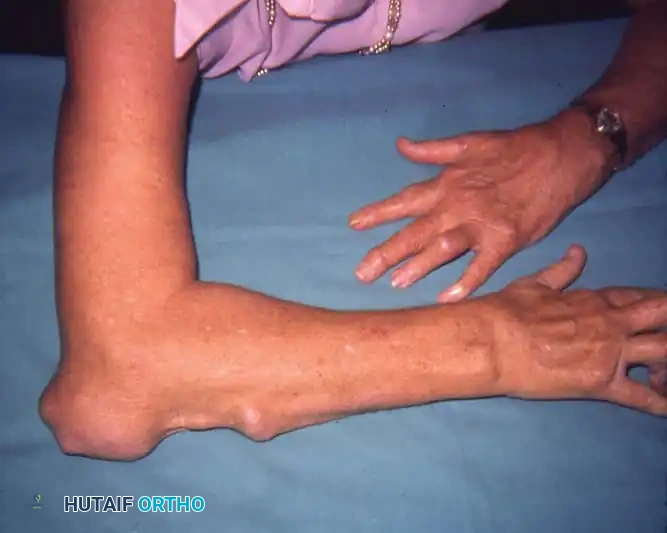
Chronic Tophaceous Gout and Biomechanical Complications
In chronic, poorly controlled gout, massive deposits of MSU crystals—known as tophi—accumulate around joints, within tendon sheaths, and in bursae. These tophi are not merely inert masses; they incite a chronic granulomatous foreign-body reaction that leads to profound orthopaedic complications:
- Nerve Compression: Tophi within the carpal tunnel or cubital tunnel can cause severe compressive neuropathies.
- Tendon Attrition and Rupture: Intratendinous MSU deposition mechanically weakens the tendon architecture. The crystals infiltrate the collagen bundles, leading to localized necrosis and eventual spontaneous rupture. The extensor pollicis longus (EPL), Achilles tendon, and patellar tendon are particularly vulnerable.
- Skin Ulceration and Secondary Infection: Subcutaneous tophi can cause pressure necrosis of the overlying skin from within (e.g., at the olecranon or first MTP joint). The resulting ulceration frequently leads to secondary bacterial colonization, chronic drainage, and osteomyelitis.
Surgical Indications and Operative Techniques
While medical management (allopurinol, febuxostat, pegloticase) is the definitive treatment for hyperuricemia, surgical intervention is indicated for mechanical complications.
1. Tophus Excision and Debridement
Indications include intractable pain, impending skin necrosis, severe joint restriction, or secondary infection.
* Approach: Incisions must be planned carefully, as the skin overlying a tophus is often thin, ischemic, and friable.
* Technique: The tophus is often intimately involved with the neurovascular bundles and tendons. Meticulous sharp dissection is required. The goal is debulking rather than en bloc oncologic resection, as aggressive excision can compromise vital structures.
* Pitfall: Avoid aggressive curettage of the tendon substance, which may precipitate iatrogenic rupture.
2. Nerve Decompression
For gouty carpal tunnel syndrome, a standard open carpal tunnel release is performed.
* Technique: Upon dividing the transverse carpal ligament, a thorough flexor tenosynovectomy is often required to remove the chalky, white MSU deposits infiltrating the tenosynovium. Specimens must be sent in alcohol (not formalin, which dissolves urate crystals) for histopathologic confirmation.
3. Tendon Reconstruction
When intratendinous deposition leads to rupture (e.g., EPL rupture at Lister's tubercle), direct primary repair is usually impossible due to poor tissue quality and gap formation.
* Technique: Tendon transfer is the procedure of choice. For an EPL rupture, an extensor indicis proprius (EIP) to EPL transfer is performed. The EIP is harvested at the level of the index MCP joint, rerouted subcutaneously, and woven into the distal EPL stump using a Pulvertaft weave under appropriate tension.
4. Amputation
In the most extreme phases of bony disruption, where massive tophaceous infiltration has destroyed the joint architecture, compromised the soft tissue envelope, and led to intractable osteomyelitis, amputation (e.g., ray amputation of the digit) may be a necessary salvage procedure to eradicate infection and relieve severe pain.
SYSTEMIC LUPUS ERYTHEMATOSUS (SLE) AND JACCOUD ARTHROPATHY
Systemic lupus erythematosus is a complex, diffuse connective tissue disease capable of affecting virtually every organ system, including the renal, cardiovascular (pericarditis), and pulmonary (pleuritis) systems. Cutaneous involvement (the classic malar rash) is present in up to 85% of patients.
Musculoskeletal Manifestations and Pathomechanics
Musculoskeletal involvement is one of the earliest and most common manifestations of SLE. Patients experience profound stiffness, swelling, tenderness, and pain. Unlike rheumatoid arthritis (RA), which is characterized by a proliferative, erosive pannus that destroys articular cartilage and bone, SLE primarily attacks the soft tissues—tendons, joint capsules, and ligaments.
This soft-tissue predilection leads to a unique biomechanical phenomenon known as Jaccoud's Arthropathy.
* Pathogenesis: Chronic inflammation leads to ligamentous laxity and capsular attenuation.
* Clinical Presentation: This laxity manifests earliest in the hand, specifically at the metacarpophalangeal (MCP) and proximal interphalangeal (PIP) joints.
* Deformities: Patients develop severe, visually striking deformities that mimic rheumatoid hands—ulnar drift of the digits, swan neck deformities, and boutonniere deformities.
* Key Distinction: Because the articular cartilage is well preserved and there is no primary bony erosion, these deformities are initially reducible. Over time, however, secondary soft-tissue contractures can render them fixed.
Raynaud Phenomenon
SLE patients frequently suffer from severe Raynaud phenomenon—an exaggerated vasospastic response to cold or emotional stress. This leads to digital ischemia, characterized by a triphasic color change (pallor, cyanosis, rubor). In severe SLE, this ischemia progresses to tissue necrosis, painful digital ulceration, and profound cold intolerance, threatening the viability of the digits.
Surgical Management of the SLE Hand
Surgical intervention in SLE requires a highly customized approach, balancing the patient's systemic medical status (often complicated by long-term corticosteroid use and immunosuppression) with their functional deficits.
1. Soft Tissue Procedures
Because the articular cartilage is preserved, early, reducible deformities can be managed with soft-tissue realignment.
* Capsulodesis and Tenodesis: For reducible swan neck deformities (PIP hyperextension with DIP flexion), a flexor digitorum superficialis (FDS) tenodesis or volar plate capsulodesis can be performed to restrict PIP hyperextension.
* Tendon Realignment: For reducible ulnar drift at the MCP joints, the extensor tendons (which have subluxated into the ulnar valleys) are centralized. This involves releasing the ulnar sagittal band, reefing the radial sagittal band, and potentially releasing the abductor digiti minimi to correct the deforming forces.
Surgical Pitfall: Soft tissue procedures in SLE have a high recurrence rate because the underlying systemic disease continues to attack the collagenous structures. Patients must be counseled that soft-tissue realignment may stretch out over time.
2. Bone Procedures (Arthrodesis and Arthroplasty)
When deformities become fixed, or when soft-tissue procedures have failed, bony procedures are required.
* Arthrodesis: Fusion of the PIP or DIP joints provides a stable, pain-free digit, albeit at the cost of motion. It is highly reliable for fixed swan neck or boutonniere deformities.
* Arthroplasty: Silicone MCP joint arthroplasty (Swanson implants) is indicated for severe, fixed ulnar drift with secondary joint destruction. The procedure involves resection of the metacarpal heads, extensive soft-tissue release, and insertion of the silicone spacer to act as a dynamic hinge.
3. Digital Sympathectomy
For patients with severe, medically refractory Raynaud phenomenon complicated by digital ulceration and impending necrosis, a digital sympathectomy is a limb-saving procedure.
* Indications: Ischemic rest pain, non-healing digital ulcers, and failure of maximal medical therapy (calcium channel blockers, phosphodiesterase inhibitors, prostacyclin analogues).
* Technique: Using microsurgical magnification, the common and proper digital arteries are exposed in the palm and digits. The adventitia of the arteries—which houses the sympathetic nerve fibers responsible for vasospasm—is meticulously stripped away over a distance of 1 to 2 centimeters. Any constricting fascial bands are released.
* Outcomes: This procedure reliably improves digital perfusion, promotes ulcer healing, and provides significant pain relief, though the underlying systemic vasospastic tendency remains.
POSTOPERATIVE PROTOCOLS AND REHABILITATION
The postoperative management of systemic arthropathies requires a multidisciplinary approach involving the orthopaedic surgeon, rheumatologist, and specialized hand or physical therapists.
- Wound Healing: Patients with SLE and chronic gout frequently have compromised soft-tissue envelopes and are on immunosuppressive medications. Sutures should be left in place longer than usual (14-21 days), and meticulous wound care is essential to prevent infection.
- Rehabilitation: Following soft-tissue realignment for SLE, dynamic splinting is critical to protect the repair while allowing early, controlled motion to prevent adhesions. Following tendon transfers for gout, a strict protocol of immobilization followed by progressive active-assisted range of motion is required to ensure tendon integration without stretching the repair.
- Medical Optimization: Surgical intervention is only one facet of care. Perioperative management of DMARDs and biologic agents must be coordinated with the rheumatologist to balance the risk of postoperative infection against the risk of a systemic disease flare.
By combining a deep understanding of the systemic pathophysiology with precise, mechanically sound surgical techniques, the orthopaedic surgeon can significantly improve the quality of life, restore function, and prevent catastrophic limb loss in patients suffering from Reiter syndrome, gout, and systemic lupus erythematosus.
You Might Also Like