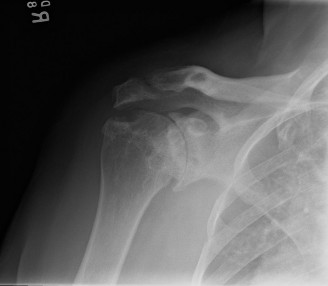
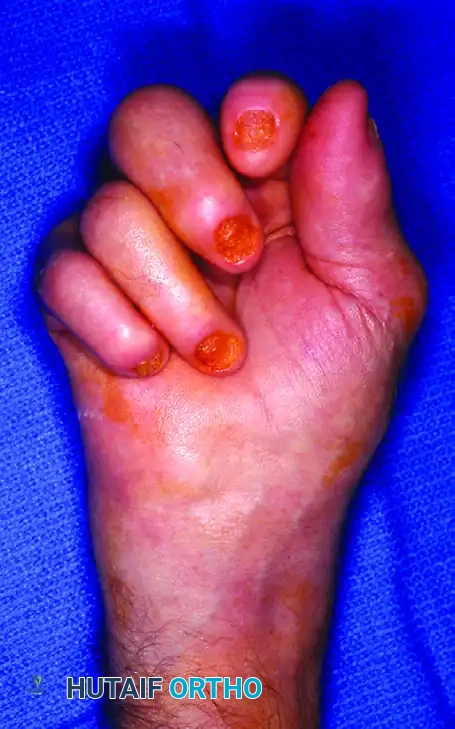
Operative Management of Hand Arthritis: Osteoarthritis, Rheumatoid Arthritis, and SLE
Key Takeaway
Hand osteoarthritis and systemic arthropathies like rheumatoid arthritis and systemic lupus erythematosus present complex reconstructive challenges. This guide details the biomechanics, clinical presentation, and step-by-step surgical management of these conditions. From trapeziometacarpal arthroplasty to soft-tissue realignments for lupus-induced ligamentous laxity, mastering these techniques is essential for restoring hand function, correcting severe deformities, and alleviating debilitating pain in the arthritic hand.
INTRODUCTION TO ARTHROPATHIES OF THE HAND
The human hand is highly susceptible to a variety of degenerative and systemic arthropathies, each presenting with distinct pathoanatomy, biomechanical alterations, and reconstructive challenges. While osteoarthritis (OA) is driven by mechanical wear and cartilage degradation, systemic conditions such as rheumatoid arthritis (RA) and systemic lupus erythematosus (SLE) are characterized by inflammatory cascades that target the synovium and capsuloligamentous structures.
For the reconstructive hand surgeon, distinguishing between the fixed, erosive joint destruction of RA and the reducible, ligamentous laxity of SLE is paramount. This comprehensive guide details the clinical evaluation, biomechanical principles, and step-by-step surgical management of these debilitating conditions.
OSTEOARTHRITIS OF THE HAND
Osteoarthritis is the most common of the rheumatic diseases affecting the upper extremity. While it may present unilaterally, it occurs just as frequently in the minor, non-dominant hand as in the dominant one. Unlike rheumatoid arthritis, OA is less frequently associated with spontaneous tendon ruptures or severe triggering of the fingers, though these pathologies can coexist.
Pathoanatomy and Clinical Presentation
The hallmark of hand osteoarthritis is progressive cartilage fragmentation, subchondral sclerosis, and marginal spur formation (osteophytes), leading to limited motion without frank dislocation. During the active inflammatory phase, pain can be severe, and the overlying skin may become erythematous; direct trauma to these inflamed joints is exquisitely painful.
Specific anatomical manifestations include:
* Trapeziometacarpal (TMC) Joint: The most frequently surgically treated osteoarthritic joint in the hand, predominantly affecting postmenopausal women. It may present as isolated single-joint involvement or as part of a pan-trapezial degenerative process.
* Distal Interphalangeal (DIP) Joint: Osteophyte formations here are known as Heberden nodes. These are frequently accompanied by mucoid cysts—ganglion-like outpouchings of the joint capsule that thin the overlying skin and can cause nail plate deformities due to pressure on the germinal matrix.
* Proximal Interphalangeal (PIP) Joint: Osteophyte formations at this level are termed Bouchard nodes.
Clinical Pearl: When excising a mucoid cyst at the DIP joint, the surgeon must meticulously debride the underlying marginal osteophyte. Failure to remove the bony spur results in an unacceptably high recurrence rate of the cyst.
Surgical Management: Trapeziometacarpal (TMC) Arthroplasty
When conservative measures (splinting, NSAIDs, corticosteroid injections) fail, surgical intervention is indicated. For advanced TMC osteoarthritis (Eaton-Littler Stages III and IV), Trapeziectomy with Ligament Reconstruction and Tendon Interposition (LRTI) remains a gold-standard procedure.
Indications
- Severe, debilitating pain at the base of the thumb refractory to conservative management.
- Radiographic evidence of joint space narrowing, osteophyte formation, and subchondral sclerosis at the TMC joint.
- Preserved metacarpophalangeal (MCP) joint function (or planned concurrent MCP stabilization if hyperextension exceeds 30 degrees).
Surgical Technique: LRTI Step-by-Step
- Positioning and Incision: The patient is positioned supine with the arm on a hand table. A regional block or general anesthesia is utilized with a well-padded upper arm tourniquet. A Wagner or modified dorsal longitudinal incision is made over the TMC joint, taking care to identify and protect the superficial sensory branches of the radial nerve.
- Capsular Exposure: The abductor pollicis longus (APL) and extensor pollicis brevis (EPB) tendons are identified and retracted. A longitudinal or T-shaped capsulotomy is performed to expose the TMC joint.
- Trapeziectomy: The trapezium is fragmented using an osteotome or rongeur and excised piecemeal. Meticulous care is taken to avoid injury to the underlying flexor carpi radialis (FCR) tendon, which lies in the depths of the trapezial fossa.
- Tendon Harvest: The FCR tendon is exposed through a series of small transverse volar incisions. The radial half of the FCR is harvested from its musculotendinous junction distally to the base of the second metacarpal.
- Ligament Reconstruction: A drill hole is created in the base of the first metacarpal (from the dorsal-radial cortex into the medullary canal and exiting the articular base). The harvested FCR slip is passed through this tunnel to reconstruct the volar oblique ligament, suspending the thumb metacarpal to prevent proximal subsidence.
- Tendon Interposition: The remaining FCR tendon slip is folded into an "anchovy" or biologic spacer and sutured into the trapezial void.
- Closure: The capsule is meticulously repaired. The skin is closed, and the thumb is immobilized in a thumb spica splint in palmar abduction.
Postoperative Protocol
- Weeks 0-4: Strict immobilization in a cast or rigid orthosis.
- Weeks 4-8: Transition to a removable splint; initiate active range of motion (AROM) focusing on palmar abduction and opposition.
- Weeks 8-12: Gradual strengthening. Unrestricted activity is typically permitted after 12 weeks.
RHEUMATOID ARTHRITIS: HAND MANIFESTATIONS
While osteoarthritis is driven by mechanical degradation, Rheumatoid Arthritis (RA) is characterized by a proliferative, erosive synovitis (pannus) that destroys articular cartilage and attenuates capsuloligamentous structures. This leads to complex, multi-planar deformities.
Swan-Neck and Boutonnière Deformities
Involvement of the MCP joint frequently results in laxity of the capsuloligamentous structures, particularly the volar plate. This primary pathology leads to a cascade of imbalances: hyperextension of the MCP joint and hyperflexion of the interphalangeal joints, often with a stable carpometacarpal joint.

The Swan-Neck Deformity (seen above) is characterized by PIP joint hyperextension and DIP joint flexion. In RA, this is often initiated by terminal tendon rupture or volar plate laxity at the PIP joint, exacerbated by intrinsic muscle tightness.
Conversely, the Boutonnière Deformity involves PIP joint flexion and DIP joint hyperextension. This occurs when the central slip of the extensor tendon ruptures or attenuates, allowing the lateral bands to subluxate volar to the axis of rotation of the PIP joint.
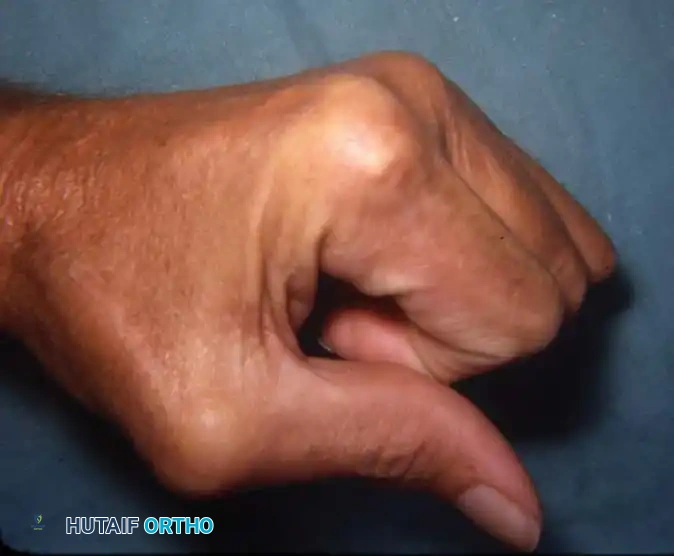
Surgical Warning: When addressing a fixed rheumatoid boutonnière deformity of the thumb (Type I, as seen above), soft-tissue reconstruction alone is universally doomed to fail. Arthrodesis of the MCP joint combined with IP joint release or pinning is the most reliable method to restore a stable pinch mechanism.
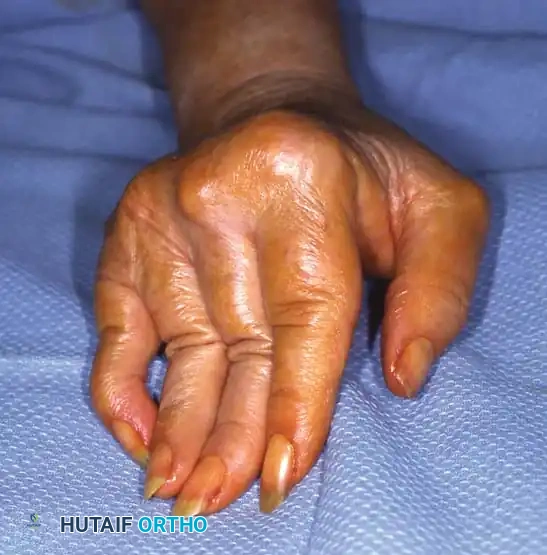
Advanced Erosive Disease: "Main en Lorgnette"
In severe, progressive, and neglected rheumatoid disease, profound osteolysis and articular destruction occur. The phalanges and metacarpals telescope into one another, creating redundant, folded skin. This end-stage presentation is known as the "main en lorgnette" or opera glass hand.
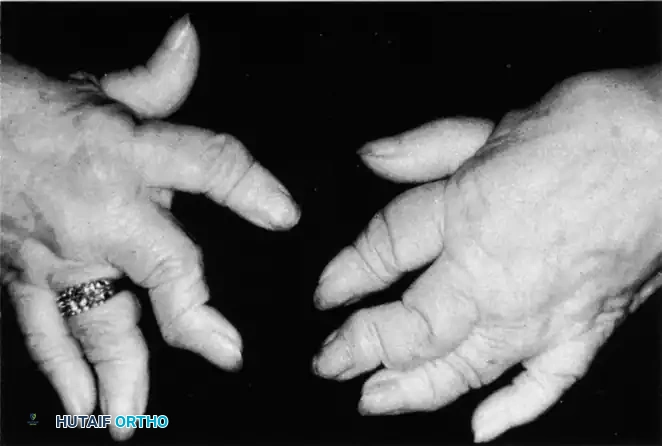
Significant tenosynovitis of the flexor and extensor tendons in the digits, palm, and wrist often accompanies this severe bone loss. Surgical management at this stage is highly complex, often requiring multiple joint arthrodeses (to restore longitudinal stability) and extensive tenosynovectomies to prevent spontaneous tendon ruptures. Silicone arthroplasty (e.g., Swanson implants) may be utilized at the MCP joints to maintain a functional arc of motion, provided there is sufficient bone stock remaining.
SYSTEMIC LUPUS ERYTHEMATOSUS (SLE)
Systemic lupus erythematosus is a diffuse connective tissue disease capable of affecting multiple organ systems, including pericarditis, pleuritis, and renal disease. Cutaneous involvement (such as the classic malar rash) is present in up to 85% of patients.
Pathoanatomy of the Lupus Hand
Musculoskeletal involvement in SLE is characterized by profound stiffness, swelling, tenderness, and pain. Unlike RA, which targets the synovium, SLE primarily attacks the tendons, joint capsules, and ligaments. Hand involvement is frequently among the earliest manifestations of the disease.
The classic presentation begins with ligamentous laxity at the MCP and PIP joints. Because the primary pathology is capsuloligamentous attenuation rather than proliferative erosive synovitis, the articular cartilage is remarkably well preserved until very late in the disease process. This results in severe, yet passively reducible, deformities (often termed Jaccoud's arthropathy).
Clinical Pearl: The hallmark differentiator between RA and SLE hand deformities on physical examination is reducibility. SLE deformities can often be passively corrected to a neutral alignment, whereas RA deformities rapidly become fixed due to joint destruction and contracture.
Raynaud Phenomenon and Digital Ischemia
Patients with SLE frequently suffer from severe Raynaud phenomenon—an exaggerated vasospastic response to cold or emotional stress. In the lupus patient, this is not merely a benign color change; it can progress to severe tissue necrosis, digital ulceration, and profound cold intolerance.
Surgical Management in SLE
Because the articular cartilage is preserved, joint-sacrificing procedures (like arthrodesis or arthroplasty) should be delayed as long as possible. Surgical intervention focuses on soft-tissue rebalancing and vascular salvage.
1. Soft-Tissue Realignment and Capsulodesis
For reducible MCP ulnar drift and volar subluxation:
* Incision: A transverse dorsal incision is made over the metacarpal heads.
* Extensor Realignment: The ulnar sagittal bands are released, and the extensor tendons are centralized over the MCP joints.
* Intrinsic Release: An ulnar intrinsic release is performed to remove the deforming force pulling the digits into ulnar deviation.
* Capsulodesis: The attenuated radial collateral ligaments and dorsal capsule are imbricated or reconstructed to restore stability.
2. Digital Sympathectomy for Raynaud Phenomenon
When medical management (calcium channel blockers, phosphodiesterase inhibitors, prostacyclin analogs) fails to prevent digital ulceration, a periarterial digital sympathectomy is indicated to relieve ischemia.
- Technique: Using loupe magnification or an operating microscope, the common digital arteries are exposed in the palm via a zigzag (Bruner) or longitudinal incision.
- Adventitial Stripping: The adventitia of the artery, which houses the sympathetic nerve fibers, is meticulously stripped over a distance of 1 to 2 centimeters.
- Release of Fascial Bands: Any constricting fascial bands or transverse retinacular ligaments compressing the neurovascular bundles are released.
- Outcome: This procedure disrupts the vasospastic reflex arc, improving baseline perfusion, promoting ulcer healing, and significantly reducing rest pain.
Postoperative Considerations in SLE
Patients with SLE are often on chronic immunosuppressive therapies (corticosteroids, methotrexate, biologic agents). This places them at a significantly elevated risk for postoperative infections and delayed wound healing. Coordination with the patient's rheumatologist is mandatory to optimize perioperative medication management, ensuring a balance between preventing disease flare-ups and allowing for adequate soft-tissue healing.
CONCLUSION
The operative management of hand arthritis requires a profound understanding of the underlying systemic or mechanical pathology. Whether performing a complex ligament reconstruction for basal joint osteoarthritis, addressing the fixed erosive deformities of rheumatoid arthritis, or executing delicate soft-tissue realignments for the reducible deformities of systemic lupus erythematosus, the surgeon must tailor the approach to the specific biomechanical deficits of the patient. Through meticulous surgical technique and rigorous postoperative rehabilitation, significant pain relief and functional restoration can be achieved in the arthritic hand.
You Might Also Like