Complex Pediatric Distal Tibial Physeal Fracture: Risks of Single-Sport Specialization

Key Takeaway
Complex pediatric distal tibial physeal fractures are diagnosed via clinical exam, plain X-rays, and essential CT scans. CT reveals precise fracture morphology, displacement, and articular involvement. This detailed imaging is critical for optimal treatment, especially for injuries linked to single-sport specialization in young athletes.
Introduction and Epidemiology
Clinical Presentation and Patient History
A 14-year-old male, Tanner Stage IV, presented to the emergency department following an acute injury to his right ankle during a competitive soccer match. The patient, a central midfielder, reported planting his right foot firmly while attempting a rapid directional change, followed by an immediate twisting sensation and a loud pop emanating from his ankle. He experienced instant, severe pain, rendering him unable to bear weight, and noted rapid swelling. There was no direct contact with another player or object at the time of injury.
Relevant history revealed the patient is a highly specialized athlete, having participated in competitive soccer year-round for the past seven years. His training regimen involved five to six days per week, often accumulating over 18 hours of high-intensity activity, split between his club team and school team commitments. He reported no structured off-season or regular cross-training in other sports. For the past six months, he had intermittently experienced a vague, deep-seated pain in his right distal tibia, particularly after prolonged training sessions, which he and his coaches attributed to shin splints and managed with rest and ice. There was no history of prior ankle sprains or significant lower extremity injuries. The patient denied any systemic comorbidities or relevant family medical history. He was otherwise fit and healthy, with no known allergies or regular medications.
The mechanism described, an external rotation force on a planted foot, is characteristic of the injury sustained and is frequently observed in sports requiring rapid directional changes on varying surfaces. The insidious onset of prodromal symptoms, initially dismissed as overuse syndrome, is a critical component of the patient's history, highlighting the long-term impact of single-sport specialization and inadequate recovery.
Clinical Examination Findings
Upon arrival, the patient was in acute distress due to pain. Inspection demonstrated significant diffuse edema over the right ankle, particularly prominent over the distal aspect of the tibia and fibula, extending into the midfoot. Moderate ecchymosis was evident along the medial and lateral aspects of the ankle joint. There was a visible, subtle deformity with the foot appearing to be in slight external rotation relative to the tibia. Skin integrity was intact, with no open wounds or signs of impending compartment syndrome.
Palpation elicited marked tenderness circumferentially around the distal tibia and fibula, maximal over the distal tibial metaphysis, physis, and epiphysis. Specific point tenderness was noted over the anterolateral distal tibia and the medial malleolus. The syndesmosis was tender to palpation, and the distal fibula also had associated tenderness. Distal pulses were palpable and strong bilaterally, with brisk capillary refill. Active and passive ankle range of motion was severely restricted in all planes due to pain and guarding. Neurological assessment confirmed intact sensation to light touch in all major nerve distributions of the foot, and motor function, while limited by pain, showed no gross neurological deficits. Gross instability was appreciated with gentle manipulation, though formal stress testing was deferred due to acute pain.
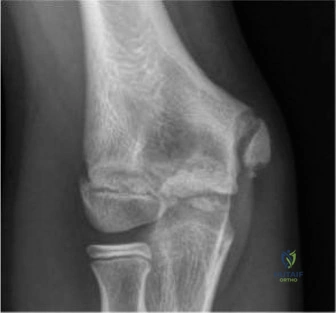
Impact of Single Sport Specialization
The presentation described above serves as a paradigmatic example of a complex pediatric distal tibial physeal fracture, specifically a triplane fracture, exacerbated by the underlying pathophysiology of single-sport specialization. Pediatric sports specialization, defined as intensive, year-round training in a single sport at the exclusion of others, has reached epidemic proportions. The immature pediatric skeleton is uniquely vulnerable to repetitive microtrauma. The prodromal symptoms reported by the patient strongly suggest a pre-existing stress reaction or stress fracture of the distal tibial metaphysis. Continuous high-impact loading without adequate recovery periods disrupts normal osteoblastic and osteoclastic coupling, leading to microscopic trabecular failure. When a structurally compromised metaphysis is subjected to a sudden, high-energy torsional force, the bone fails catastrophically along the path of least resistance, which in the Tanner Stage IV adolescent, involves the partially closed physis. Understanding this epidemiological shift is vital for orthopedic surgeons, as these injuries require meticulous surgical management to prevent long-term articular and physeal complications.
Surgical Anatomy and Biomechanics
Distal Tibial Physeal Closure Sequence
The management of pediatric distal tibial fractures mandates a profound understanding of the chronological and spatial sequence of physeal closure. The distal tibial physis contributes approximately forty-five percent of the total longitudinal growth of the tibia. Closure of this physis typically begins around age twelve to thirteen in females and age fourteen to fifteen in males, corresponding precisely with Tanner Stage IV development.
The closure pattern is highly predictable and asymmetric. It initiates in the central portion of the physis, often referred to as Kump bump, and proceeds medially. The lateral and anterolateral portions of the physis are the final segments to fuse. This asymmetrical closure creates a unique biomechanical vulnerability. During the transitional period of closure, typically spanning eighteen months, the medial aspect of the distal tibia is fused and structurally rigid, while the anterolateral aspect remains cartilaginous and mechanically weaker. This anatomical reality dictates the fracture patterns observed in this age demographic, specifically the juvenile Tillaux fracture and the triplane fracture.
Biomechanics of External Rotation Injuries
The primary mechanism of injury for complex transitional fractures of the distal tibia is an external rotation force applied to a supinated or pronated foot. The anterior inferior tibiofibular ligament connects the distal fibula to the anterolateral epiphysis of the tibia, known as the Chaput tubercle. When the foot is planted and the leg internally rotates, or conversely, when the foot is forcefully externally rotated, the anterior inferior tibiofibular ligament is placed under extreme tension.
Because the ligament is biomechanically stronger than the open anterolateral physis, the avulsion force propagates through the path of least resistance. In a juvenile Tillaux fracture, this results in a Salter-Harris III injury where the anterolateral epiphysis is avulsed. In a triplane fracture, the biomechanical forces are more complex, often involving a combination of external rotation and axial loading. The fracture line propagates through the epiphysis in the sagittal plane, travels along the open physis in the axial plane, and exits through the posterior metaphysis in the coronal plane. If the patient has a pre-existing metaphyseal stress reaction due to over-specialization, the metaphyseal cortical bone is already structurally compromised, facilitating the coronal split and resulting in significant displacement.
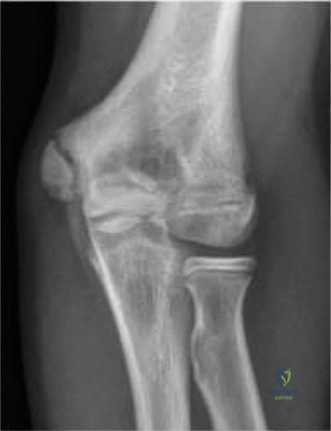
Indications and Contraindications
Operative Decision Making
The primary goal in the management of distal tibial physeal fractures is the anatomic restoration of the articular surface to prevent post-traumatic osteoarthritis, alongside the stabilization of the physis to minimize the risk of asymmetrical growth arrest. However, in patients nearing skeletal maturity, the risk of clinically significant leg length discrepancy or angular deformity is substantially reduced, elevating articular congruity to the paramount clinical objective.
Operative intervention is strictly indicated when there is unacceptable displacement of the articular surface. The universally accepted threshold for surgical intervention in intra-articular fractures of the weight-bearing distal tibia is greater than two millimeters of displacement or step-off. Closed reduction may be attempted; however, the interposition of periosteum or the anterior inferior tibiofibular ligament frequently blocks anatomic reduction, necessitating open intervention.
| Clinical Scenario | Management Strategy | Rationale and Considerations |
|---|---|---|
| Undisplaced Fracture | Non Operative | Cast immobilization for four to six weeks. Requires close radiographic follow up to ensure no secondary displacement occurs as swelling subsides. |
| Displacement Less Than Two Millimeters | Non Operative | Long leg cast initially, transitioning to short leg cast. Weekly radiographs for the first three weeks are mandatory. |
| Displacement Greater Than Two Millimeters | Operative ORIF | Anatomic reduction of the articular surface is mandatory to prevent early onset post-traumatic arthritis. |
| Failed Closed Reduction | Operative ORIF | Soft tissue interposition frequently prevents closed reduction. Open extraction of periosteum is required. |
| Open Fracture | Operative I and D with ORIF | Immediate surgical debridement and stabilization to mitigate infection risk. |
| Impending Compartment Syndrome | Operative Fasciotomy and Fixation | Rare in isolated distal tibia fractures but necessitates emergent decompression and skeletal stabilization. |
Pre Operative Planning and Patient Positioning
Advanced Imaging and Three Dimensional Analysis
Standard orthogonal radiographs of the ankle, including anteroposterior, lateral, and mortise views, are the initial diagnostic modality. However, the complex, multi-planar nature of transitional fractures makes plain radiography insufficient for definitive preoperative planning. Plain films frequently underestimate the degree of articular displacement and the number of fracture fragments.
A high-resolution Computed Tomography scan with sagittal, coronal, and three-dimensional reconstructions is mandatory for all suspected triplane and Tillaux fractures. The CT scan allows the orthopedic surgeon to precisely map the fracture lines, quantify the articular step-off, identify the presence of intercalary articular fragments, and plan the exact trajectory for internal fixation. In a triplane fracture, the CT scan will clearly delineate the coronal metaphyseal fragment, the sagittal epiphyseal fragment, and the axial physeal separation. Identifying the exact location of the Chaput fragment and the integrity of the syndesmosis is critical for determining the surgical approach and the necessity of syndesmotic stabilization.
Operating Room Setup and Positioning
The patient is positioned supine on a radiolucent operating table. A bump is placed under the ipsilateral hip to internally rotate the leg, bringing the foot and ankle into a neutral position, which is particularly helpful for visualizing the anterolateral aspect of the joint. A pneumatic tourniquet is applied to the proximal thigh to ensure a bloodless surgical field, though it should be used judiciously to minimize ischemic time.
Intraoperative fluoroscopy is essential. The C-arm should be positioned on the contralateral side of the table, allowing for unobstructed anteroposterior, lateral, and mortise imaging throughout the procedure. The surgeon must verify that perfect mortise views can be obtained prior to prepping and draping. Prophylactic intravenous antibiotics, typically a first-generation cephalosporin, are administered within one hour prior to incision.
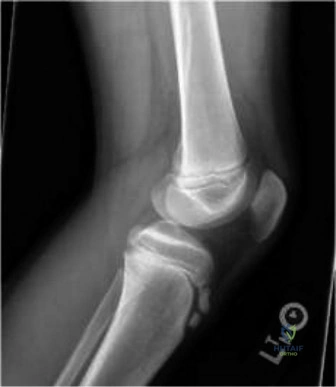
Detailed Surgical Approach and Technique
Anterolateral Approach to the Distal Tibia
For the majority of transitional fractures involving the anterolateral epiphysis, an anterolateral approach to the ankle provides optimal exposure. A longitudinal incision is made centered over the anterolateral distal tibia, typically lateral to the peroneus tertius tendon and extending distally toward the base of the fourth metatarsal.
Subcutaneous dissection must be performed meticulously to identify and protect the branches of the superficial peroneal nerve, which frequently cross the surgical field in this region. The extensor retinaculum is incised, and the extensor digitorum longus tendons are retracted medially. The anterior compartment musculature is elevated from the anterolateral tibia, exposing the joint capsule. The capsule is incised longitudinally, allowing direct visualization of the tibiotalar joint and the displaced anterolateral epiphyseal fragment.
Fracture Reduction Strategies
Upon entering the joint, the surgeon will typically encounter a significant fracture hematoma, which must be thoroughly irrigated and debrided. The fracture edges are often covered with interposed periosteum, which is the most common impediment to closed reduction. This periosteum must be carefully elevated and retracted to expose the raw cancellous bone of the fracture site.
Direct visualization of the articular surface is paramount. The anterolateral epiphyseal fragment is manipulated using a dental pick or a small periosteal elevator. The reduction maneuver typically involves internal rotation and direct pressure over the fragment. A large, pointed reduction clamp can be utilized, placing one tine on the medial malleolus and the other on the anterolateral fragment, to compress the fracture. The reduction must be confirmed visually by inspecting the articular cartilage congruity and fluoroscopically via multiple views. Even a one-millimeter step-off is considered suboptimal and warrants readjustment.
Internal Fixation Construct Execution
Once anatomic reduction is achieved, provisional fixation is obtained using smooth Kirschner wires. For a Tillaux fracture, the K-wire is directed from anterolateral to posteromedial, parallel to the joint line and entirely within the epiphysis. For a triplane fracture, the fixation strategy is inherently more complex due to the multi-planar fragments.
The epiphyseal component of the triplane fracture is typically stabilized first, utilizing the same anterolateral to posteromedial trajectory as the Tillaux fracture. Following epiphyseal stabilization, the metaphyseal component must be addressed. This often requires a separate incision or a proximal extension of the anterolateral incision. The metaphyseal fragment is reduced and provisionally pinned from anterior to posterior or lateral to medial, depending on the specific fracture morphology identified on the preoperative CT scan.
Definitive fixation is achieved using partially threaded cannulated screws, typically 4.0 millimeter or 4.5 millimeter in diameter. The screws are placed over the provisional K-wires. It is imperative to use washers to prevent the screw heads from sinking into the relatively soft pediatric metaphyseal or epiphyseal bone.
When placing the screws, the surgeon must make a critical decision regarding the physis. If the patient is Tanner Stage IV and nearing skeletal maturity, the risk of clinically significant growth arrest from crossing the physis with a smooth screw shaft is negligible compared to the catastrophic risk of articular incongruity. However, whenever anatomically feasible, epiphyseal screws should remain strictly within the epiphysis, parallel to the joint line, and metaphyseal screws should remain strictly within the metaphysis. Following definitive fixation, the syndesmosis must be evaluated using the hook test under fluoroscopy. If syndesmotic instability is present, which is rare but possible if the anterior inferior tibiofibular ligament remains intact while the fibula is fractured, syndesmotic fixation may be required.

Complications and Management
Anticipated Postoperative Challenges
Despite meticulous surgical technique, pediatric distal tibial physeal fractures carry a significant risk of complications. The most dreaded complication is premature physeal closure leading to angular deformity or leg length discrepancy. While the risk is mitigated in older adolescents, precise anatomical reduction of the physis minimizes the formation of a transphyseal bony bar.
Post-traumatic osteoarthritis is a direct consequence of inadequate articular reduction. The ankle joint is highly congruent, and even minor alterations in contact mechanics can lead to accelerated cartilage wear. Hardware prominence is also a frequent complaint, given the paucity of soft tissue coverage over the anterolateral ankle, often necessitating a secondary procedure for implant removal once radiographic union is confirmed.
| Complication | Estimated Incidence | Salvage Strategies and Management |
|---|---|---|
| Premature Physeal Arrest | Ten to Twenty Percent | Close radiographic monitoring. If a bony bar forms and growth remains, bar resection with interposition grafting may be indicated. If near skeletal maturity, completion epiphysiodesis of the injured and contralateral limb prevents discrepancy. |
| Angular Deformity | Five to Fifteen Percent | Typically varus or valgus depending on the arrest location. Managed with corrective osteotomy (e.g., supramalleolar osteotomy) once skeletal maturity is reached or if deformity is severe. |
| Post Traumatic Arthritis | Variable based on reduction | Activity modification, intra-articular injections. In severe, end-stage cases, ankle arthrodesis or total ankle arthroplasty in adulthood. |
| Hardware Prominence | Thirty to Forty Percent | Elective hardware removal after complete radiographic consolidation, typically at six to twelve months postoperatively. |
| Infection | Less than Two Percent | Superficial infections managed with oral antibiotics. Deep infections require prompt surgical irrigation, debridement, and potentially hardware removal if union has occurred. |
Post Operative Rehabilitation Protocols
Phased Weight Bearing and Functional Recovery
The postoperative rehabilitation protocol must be carefully structured to protect the articular reduction while preventing profound joint stiffness and muscle atrophy. Immediately following surgery, the patient is placed in a well-padded short leg splint in a neutral position. The patient is instructed to remain strictly non-weight-bearing on the operative extremity. Elevation and cryotherapy are emphasized to control postoperative edema.
At the two-week postoperative visit, the splint and sutures are removed. Radiographs are obtained to confirm the maintenance of reduction. The patient is then transitioned to a short leg cast or a rigid controlled ankle motion boot. The patient remains non-weight-bearing for a total of four to six weeks from the date of surgery. During this phase, if a removable boot is utilized, the patient may begin gentle, supervised active range of motion exercises out of the boot, focusing strictly on sagittal plane motion (dorsiflexion and plantarflexion) while avoiding any torsional stresses.
At the six-week mark, repeat radiographs are obtained to assess for early callus formation and fracture consolidation. If clinical and radiographic progression is satisfactory, the patient initiates a progressive partial weight-bearing protocol, advancing to full weight-bearing over the subsequent two to four weeks. Physical therapy is intensified at this stage, incorporating proprioceptive training, closed kinetic chain exercises, and strengthening of the peroneal and posterior tibial musculature.
A critical component of the rehabilitation phase for this specific patient population is addressing the underlying etiology of the injury: single-sport specialization. The orthopedic surgeon must engage in a frank discussion with the patient, parents, and coaches regarding the necessity of periodization. Return to competitive soccer is typically permitted between three and five months postoperatively, contingent upon the restoration of full, painless range of motion, symmetrical lower extremity strength, and successful completion of sport-specific functional testing. However, the patient must be counseled to incorporate at least three months of off-season rest or participation in a different sport annually to allow for adequate skeletal remodeling and to mitigate the risk of future stress-related catastrophic failures.
Summary of Key Literature and Guidelines
Evidence Based Practice in Pediatric Traumatology
The management of pediatric distal tibial transitional fractures is heavily informed by a robust body of orthopedic literature. The foundational understanding of the asymmetric closure of the distal tibial physis was elegantly described by Kump, and later expanded upon by Dias and Tachdjian, who provided the definitive classification system for these complex injuries based on the mechanism of injury and radiographic appearance.
Current guidelines from pediatric orthopedic societies emphasize the absolute necessity of computed tomography in the preoperative evaluation of these fractures. Studies by Horn et al. and Crawford have consistently demonstrated that plain radiographs fail to identify the true extent of articular displacement in up to forty percent of triplane fractures, leading to suboptimal non-operative management when surgery is actually indicated.
Furthermore, the American Academy of Pediatrics has published stringent guidelines regarding youth sports specialization. The literature clearly correlates early single-sport specialization and high training volumes (exceeding the child's age in hours per week) with a significantly increased risk of overuse injuries, including metaphyseal stress reactions. The case presented underscores the clinical reality of these guidelines, demonstrating how chronic, unmanaged stress reactions can culminate in acute, complex intra-articular physeal fractures requiring extensive surgical intervention. Orthopedic surgeons must therefore act not only as surgical technicians but also as educators, advocating for diversified athletic participation to protect the developing musculoskeletal system.
