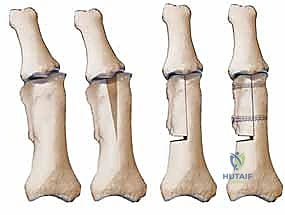
Corrective Osteotomy for Metacarpal and Phalangeal Malunion: An Intraoperative Masterclass
Key Takeaway
Master the art of corrective osteotomy for metacarpal and phalangeal malunions. This immersive guide covers comprehensive surgical anatomy, meticulous preoperative planning, and granular, real-time intraoperative execution. Learn to prevent pitfalls, manage complications, and ensure optimal patient outcomes from a master surgeon's perspective in the operating theater.
Alright team, let's get scrubbed in. Today, we're tackling a challenging but incredibly rewarding procedure: corrective osteotomy for metacarpal and phalangeal malunion. These deformities, often multiplanar, can profoundly impact hand function, and our goal is to restore anatomical alignment and, crucially, functional capacity. Remember, while there might be one dominant component to the deformity, we must always consider the three-dimensional nature of the problem.
Understanding the Deformity: Anatomy and Biomechanics
A malunion, by definition, is a fracture that has healed in an incorrect anatomical alignment. The impact of this misalignment is often magnified distally. Consider this: just one degree of rotation at the fracture site can translate to five degrees of deviation at the fingertip. This seemingly minor rotational error can cause a significant 1.5 cm of digital overlap when the fingers are flexed, leading to scissoring, functional impairment, and patient frustration.
Comprehensive Surgical Anatomy
Let's review the critical anatomy we'll be navigating.
- Metacarpals: These are tubular structures, but critically, they are triangular in cross-section. The medial and lateral surfaces converge volarly to form a distinct volar ridge. This ridge provides crucial attachment points for the interossei muscles. Proximally and distally, the intermetacarpal ligaments help stabilize these bones. This inherent stability explains why functionally significant malunions of the ring and small metacarpals are less common than in the border digits.
- Neurovascular Risks (Metacarpals): When approaching the metacarpals dorsally, we must be vigilant about the dorsal sensory nerves, which run superficially. Deep to the bone, the digital neurovascular bundles run along the lateral aspects of the flexor tendons. While less immediately vulnerable than in the phalanges, careless drilling or excessive retraction can still cause injury.
- Muscular Intervals (Metacarpals): For the second through fourth metacarpals, our dorsal approach typically utilizes the intermetacarpal spaces, carefully retracting the extensor tendons and their sagittal bands.
- Phalanges: In contrast to the metacarpals, phalanges are more bean-shaped in cross-section. The volar aspects of the proximal and middle phalanges are in intimate relation with the flexor digitorum profundus (FDP) and superficialis (FDS) tendons. This relationship is particularly tight in the region of the annular pulleys (A1-A5).
- Neurovascular Risks (Phalanges): The digital neurovascular bundles run along the mid-axial lines of the digits. During a mid-axial approach to the phalanges, these bundles are extremely vulnerable. We must meticulously identify and protect them, often retracting them volarly or dorsally depending on the exact approach and depth. The dorsal sensory nerve branches are also at risk with lateral incisions.
- Muscular/Tendon Intervals (Phalanges): A mid-axial approach for phalanges requires careful dissection to avoid the extensor mechanism dorsally and the flexor tendons/pulleys volarly. The lateral bands of the extensor mechanism may need to be incised and elevated for adequate exposure, but this must be done judiciously to preserve their function.
- A Critical Pitfall: Tendon Vulnerability: The close proximity of the flexor tendons to the volar cortex of the phalanges, especially within the confines of the annular pulleys, makes them highly vulnerable to damage from drills and screws inserted in a dorsovolar direction. This is a crucial point we will emphasize during the procedure.
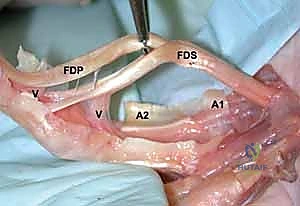
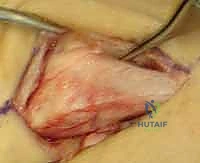
FIG 1 • Structures on the volar aspect of the metacarpals and phalanges. The flexor digitorum profundus (FDP) and flexor digitorum superficialis (FDS) tendons are intimately associated with the volar aspect of the phalanges and, to a lesser extent, the metacarpals. This dissected specimen also depicts the vinculae (V) and the A-1 and A-2 annular pulleys.
Consequences of Malunion:
Beyond the obvious cosmetic issues, significant extra-articular malunions (EAMs) can lead to:
* Digital scissoring or crossing: Impairs grasp and fine motor skills.
* Pain: Due to abnormal joint loading and soft tissue impingement.
* Disturbance of muscle/tendon balance: Leads to weakness, stiffness, and altered biomechanics.
* Reduction of grip strength: A direct consequence of impaired mechanics.
* Extension lag: EAMs associated with shortening, particularly in proximal phalanges, can cause a significant extension lag, leading to a "pseudoclaw" deformity.
* Intra-articular Malunions (IAMs): Even a small step (0.5 mm) or gap (1 mm) in the articular surface can cause joint incongruity, synovitis, capsular loosening or stiffness, and ultimately, painful post-traumatic arthrosis.
Coexisting Soft Tissue Pathology: It's vital to remember that malunions rarely exist in isolation. Neurovascular deficits, trophic changes, joint contractures, and tendon adhesions can all coexist, complicating our surgical strategy and potentially impacting outcomes. Results of corrective osteotomy are significantly poorer in the presence of such complicating factors, highlighting the need for a thorough preoperative assessment.
Preoperative Planning: The Blueprint for Success
Our success in these cases hinges almost entirely on meticulous preoperative planning.
1. Patient History and Physical Examination:
* The Story: We need a detailed history of the original injury, the mechanism, previous treatments (operative or non-operative), and the duration of the malunion. Ask about any complicating factors like infection or chronic pain syndromes.
* The Impact: Crucially, quantify the patient's functional impairment. What are their specific complaints? Pain? Stiffness? Weakness of grip? Digital scissoring? How does this impact their occupation, hobbies, and daily activities? What are their expectations and goals for surgery?
* The Patient: Assess skeletal maturity, hand dominance, and most importantly, their ability to cooperate with the rigorous postoperative therapy regimen. This is not a procedure for non-compliant patients.
* The Exam: Perform a thorough physical examination, assessing:
* Range of Motion (ROM): Both active and passive, of all joints in the affected digit and adjacent digits.
* Digital Cascade: Observe the natural flexion cascade of the fingers. Malrotation will disrupt this.
* Scissoring: Ask the patient to make a fist and observe for any crossing of the digits.
* Grip and Pinch Strength: Quantify any weakness.
* Neurovascular Status: Sensation, capillary refill.
* Soft Tissue Envelope: Quality of skin, presence of scars, adhesions.
* Joint Stability: Ligamentous integrity.
2. Imaging and Other Diagnostic Studies:
* Radiographs: Good-quality radiographs in three precise planes (anteroposterior, true lateral, and oblique) are the cornerstone for simple EAMs.
* Contralateral Comparison: Crucially, obtain radiographs of the opposite, uninjured hand. These serve as our template for restoration of normal anatomy.
* CT Scans with 3D Reconstruction: For complex, multiplanar EAMs, IAMs, or combined deformities, a CT scan with 3D reconstruction is invaluable. It allows us to precisely quantify the angular and rotational components of the deformity and plan our osteotomy cuts in multiple planes.
3. Severity of Deformity and Nonoperative Management:
* Remember, not every malunion requires surgery. Patients have a remarkable capacity to adapt to minor deformities. Slight digital overlap might be unsettling but consistent with good function.
* Hand Therapy First: For less dramatic deformities, physical therapy is the first-line treatment. Many patients will achieve sufficient functional improvement to "live with" the deformity. This also gives us an opportunity to assess patient compliance and realistic expectations.
4. Timing of Correction:
* Nascent Malunions: Treatment of nascent malunions generally leads to improved outcomes.
* Intra-articular Malunions (IAMs): If there's a significant articular step (e.g., >0.5mm) and no overwhelming technical difficulties, IAMs should be corrected as soon as possible to prevent progressive arthrosis.
* Extra-articular Malunions (EAMs): For EAMs, after 6 to 8 weeks from the injury, a "wait and watch" policy is often advisable. This allows the acute inflammatory phase to subside, soft tissues to mature, and for us to fully assess the functional and cosmetic impact of the malunion.
5. Surgical Planning: The Blueprint in Detail
* Location of Correction:
* Angular and Complex EAMs: The osteotomy should ideally be at or near the apex of the deformity.
* Rotational EAMs: Historically, proximal metacarpal osteotomies were performed for P1 rotational malunions, but with improved techniques and implants, correction is now often performed closer to the deformity.
* Type of Osteotomy:
* Angular EAMs:
* Closing Wedge Osteotomy: Preferred for intrinsic tightness and common for dorsal apex metacarpal malunions.
* Opening Wedge Osteotomy: Best for extension lag and pseudoclaw deformities, more common in apex volar phalangeal malunions.
* Incomplete Osteotomy: Can be used for either, preserving a volar or dorsal hinge.
* Rotational and Combined Rotational/Angular EAMs: A complete osteotomy is required to allow full rotational correction.
* Metacarpal Neck EAM (Boxer's Fracture): A pivot osteotomy can be used if there's no significant shortening.
* Preoperative Templating (The Real Work):
* Using the good-quality radiographs or CT scans, we outline the proximal and distal fragments of the malunited bone.
* We then superimpose these outlines over the outline of the contralateral, uninjured bone. This allows us to precisely determine:
* The exact type and location of the osteotomy.
* The size and shape of the bone wedge to be removed (for closing wedge) or the size of the bone graft needed (for opening wedge).
* The optimal method of fixation, including plate size, type (compression, locking, T-plate, Y-plate, condylar plate), and screw length/number. We aim for at least six cortices of fixation (three screws) proximal and distal to the osteotomy if possible.
* Bone Grafting: In the rare cases requiring large corticocancellous interposition grafts, we plan for an ipsilateral iliac crest bone graft harvest. For smaller grafts, we can harvest from the dorsal distal radius.
* Adjunct Procedures: Always anticipate and plan for adjunct procedures such as tenolysis, capsulotomy, or even soft tissue coverage if there are significant adhesions or skin deficiencies.
* Plate Placement:
* Dorsal plates should be avoided in phalanges due to the high risk of extensor tendon adhesions and subsequent loss of motion.
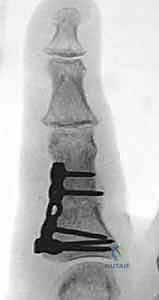
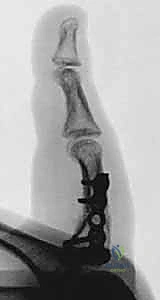
* For phalangeal coronal plane correction, a lateral buttress plate placed over the bone graft is preferred (see Fig 2C,D).
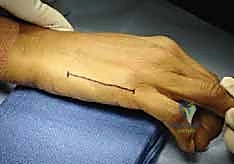
FIG 2 • C,D. Coronal plane correction of a proximal phalangeal malunion. The plate has been placed laterally to avoid interfering with the extensor mechanism, as well to avoid damage to the flexor tendons while drilling and inserting screws.
Patient Positioning and Setup
Alright, let's get our patient positioned.
- Patient Position: The patient is supine on the operating table. The affected shoulder is abducted to 90 degrees, the elbow extended, and the entire extremity placed on a dedicated arm table. This provides us with excellent access and allows for full range of motion assessment intraoperatively.
- Tourniquet: We'll apply a non-sterile pneumatic tourniquet proximally on the arm. This will be inflated after prepping and draping to create a bloodless field, which is absolutely essential for the precision required in hand surgery.
- Iliac Crest Prep (If Needed): If our preoperative planning indicates the need for a large corticocancellous graft, we'll prep the ipsilateral iliac crest simultaneously, allowing a second team to harvest while we're working on the hand.
- Examination Under Anesthesia (EUA): Before we make any incisions, I'll perform an EUA to confirm the joint ROM and stability. This gives us a baseline and can sometimes reveal additional soft tissue contractures not fully appreciated preoperatively.
- Fluoroscopy Setup: The C-arm will be draped sterilely and positioned to allow for immediate, unhindered true AP, lateral, and oblique radiographic views of the hand without requiring repositioning of the extremity. This real-time imaging is critical for confirming our osteotomy cuts and the accuracy of our correction.
Step-by-Step Intraoperative Execution: The Operating Surgeon's Viewpoint
Let's begin. Tourniquet up.
A. Incomplete Osteotomy for Angular Correction: Metacarpal Closing Wedge Osteotomy
This approach is typically used for dorsal apex metacarpal malunions where we need to close a wedge to correct angulation, often in the setting of intrinsic tightness. We're aiming to restore the true anatomical axis.
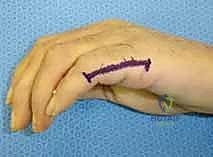
- Incision: "Scalpel, please." We'll make a dorsal longitudinal skin incision in the interval between either the index–long or ring–small metacarpals, depending on the bone we're treating. The longitudinal limb will run precisely in the intermetacarpal space, and we'll gently curve the ends proximally and distally to ensure adequate exposure without creating tension points.
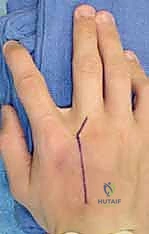
FIG 2 • A. Skin incision used for a dorsal approach to a third metacarpal malunion. The longitudinal limb of the skin incision runs between the metacarpals, and depending on whether the malunion is proximal or distal, the appropriate end is curved.
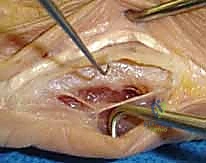
2. Deep Dissection: "Metzenbaum scissors." We carefully dissect through the subcutaneous tissue. Identify the extensor tendons. "Fellow, gently retract the extensor tendon with a small blunt hook." We want to avoid any direct handling or excessive tension on the extensor mechanism. We'll use a "no-touch" technique as much as possible to minimize adhesions.
TECH FIG 1 • A. Extensor tendons have been retracted to expose the dorsal surface of the metacarpal sagittal plane malunion.
3. Periosteal Exposure: "No. 15 blade." We make a dorsolateral incision through the metacarpal's periosteum. "Now, with a small periosteal elevator, carefully free this layer from the dorsum of the metacarpal." We need to subperiosteally expose the circumference of the bone at the planned osteotomy site. This meticulous periosteal elevation is critical, as this layer will be repaired at the end to protect the extensor tendons from the underlying hardware.
TECH FIG 1 • B. The deep subtendinous layer of the metacarpal is demonstrated. Note that the periosteum is still intact. This layer is repaired covering the implant to prevent tendon adhesions.
4. Neurovascular Protection: "Small Hohmann retractors, please." We'll pass two small Hohmann retractors, one radially and one ulnarly, to gently protect the surrounding tendons and neurovascular structures. Be extremely careful not to put undue tension on these delicate structures.
5. Determining the Apex and Axis: "Fluoroscopy on, please." This is a crucial step.
* "Let's place a 0.35-mm K-wire parallel to the true anatomic axis of the proximal fragment under radiographic guidance." Confirm its position in both AP and lateral views.
* "Now, mark the anatomic axis of the proximal fragment on the bone using diathermy or a marking pen, aligning it with our K-wire."
* "Repeat this process for the distal fragment."
* "The intersection of these two marked axes precisely identifies the apex of the deformity." This is where we will design our osteotomy.
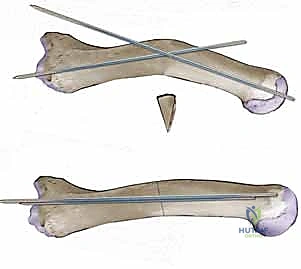
TECH FIG 1 • C,D. Method of using Kwires to determine the apex of the deformity. After removing a wedge, the size of which is determined by preoperative templating ( C ), deformity correction is confirmed when the K-wire markings are observed to be parallel ( D ).
6. Planning the Wedge Resection: "Based on our preoperative templating, we know the size of the bone wedge we need to remove." We plan our cuts perpendicular to the long axis of each fragment to ensure a clean closure.
7. Provisional Plate Application: "Let's grab a six- or seven-hole 2.0- to 2.7-mm compression plate." We'll center and apply this plate provisionally to the dorsum of one fragment, typically the more stable proximal fragment, using two screws. "Moderately tighten these screws." This plate will serve as a guide for our reduction.
8. Osteotomy Cuts: "Now, remove one screw and rotate the plate away from the osteotomy site."
* "I'll use a water-cooled sagittal saw for precision. Make sure the irrigation is running continuously to prevent thermal necrosis."
* "First, we'll make the distal bone cut, precisely following our templated line, perpendicular to the long axis of the distal fragment."
* "Next, the proximal bone cut, again perpendicular to the proximal fragment's axis, meeting the distal cut to form our wedge."
* CRITICAL PEARL: For an incomplete osteotomy, we leave an elastic pillar of bone intact volarly on the concave side. This acts as a hinge, providing stability during correction. In some severe cases, complete correction might require cutting the volar cortex, leaving only the volar periosteum as the hinge. This decision is made intraoperatively based on the degree of correction needed and the tension on the hinge.
9. Wedge Removal and Correction: "Carefully remove the bone wedge." "Now, let's bring the fragments together." As we close the wedge, the dorsal plate should sit flat across both fragments, guiding our reduction.
* "Fluoroscopy on." "We're looking for our K-wire markings to be perfectly parallel, indicating adequate correction of the deformity."
TECH FIG 1 • D. With the deformity adequately corrected, the wire markings are parallel or overlapping.
10. Definitive Fixation: "Re-apply the plate, tightening the two screws already in place." "Now, reduce the osteotomy, bringing the fragments into firm compression." "Insert the remaining screws, ensuring good purchase in both cortices."
* Pearls for Fixation: For juxta-articular osteotomies, consider condylar plates, T-plates, Y-plates, or locking plates for enhanced stability.
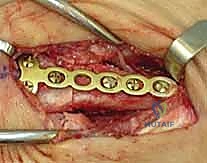
TECH FIG 1 • E. Dorsally applied T-plate with three screws distal and three screws proximal to the osteotomy.
11. Final Assessment: "Fluoroscopy on, AP, lateral, oblique." Confirm reduction clinically and radiographically. Check digital cascade and ROM.
12. Closure: "Now, the crucial soft tissue closure." "Using absorbable suture, we will meticulously close the periosteal and muscle layer over the plate, creating a barrier between the hardware and the extensor tendons." This is paramount to prevent adhesions and preserve tendon gliding. "Subcutaneous layer, then skin closure in the usual manner."
B. Phalangeal Opening Wedge Osteotomy
This approach is typically used for apex volar phalangeal malunions, often associated with an extension lag or pseudoclaw deformity, where we need to lengthen the bone.
- Incision: "Scalpel." We'll make a mid-axial skin incision along the junction of the wrinkled dorsal and smooth volar skin. This provides excellent access to the phalanx while minimizing disruption to the extensor mechanism and flexor sheath.
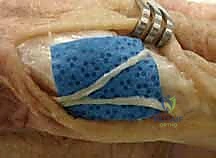
TECH FIG 2 • A. Lateral incision for proximal phalangeal osteotomy.
2. Deep Dissection and Neurovascular Protection: "Metzenbaum scissors, fine forceps." Carefully dissect through the subcutaneous tissue.
* CRITICAL WARNING:
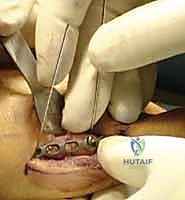
> Surgical Warning: Be acutely aware of the dorsal sensory nerve branches and the digital neurovascular bundles running along the mid-axial line. Meticulously identify and protect these structures throughout the dissection. Injury can lead to permanent sensory deficits or vascular compromise.
TECH FIG 2 • B. Dorsal cutaneous nerve.
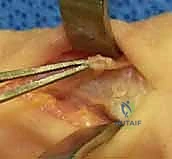
* We may need to incise the lateral band of the extensor mechanism as required to expose the phalanx. This must be done carefully to preserve its function.
<a href="/media/hutaif_opertive/hutaif-ch40
Additional Intraoperative Imaging & Surgical Steps



REFERENCES
-
When not performing ROM exercises, rest the hand in a volar splint in a functional position (MP joints flexed to 60–70 degrees and IP joints fully extended), apply a compression bandage, and elevate.
-
Büchler U, Gupta A, Ruf S. Corrective osteotomy for posttraumatic malunion of the phalanges in the hand. J Hand Surg Br 1996;21:33–42.
-
Freeland AE, Jabaley ME, Hughes JL. Fracture repair: metacarpals and carpals. In Freeland A, Jabaley M, Hughes J, eds. Stable Fixation of the Hand and Wrist. New York: Springer-Verlage, 1986:35–71.
-
Light TR. Salvage of intra-articular malunions of the hand and wrist. The role of realignment osteotomy. Clin Orthop Relat Res 1987;214: 130–135.
-
Opgrande JD, Westphal SA. Fractures of the hand. Orthop Clin North Am 1983;14:779–792.
-
Ring D. Malunion and nonunion of the metacarpals and phalanges. J Bone Joint Surg Am 2005;87A:1380–1388.
-
Rosenwasser MP, Quitkin HM. Malunion and other posttraumatic complications in the hand. In: Berger R, Weiss A, eds. Hand Surgery. Philadelphia: Lippincott Williams & Wilkins, 2003:207–230.
-
Strauch RJ, Rosenwasser MP, Lunt JG. Metacarpal shaft fractures: The effect of shortening on the extensor tendon mechanism. J Hand Surg Am 1998;23:519–523.
-
Teoh LC, Yong FC, Chong KC. Condylar advancement osteotomy for correcting condylar malunion of the finger. J Hand Surg Br 2002; 27:31–35.
-
Thurston AJ. Pivot osteotomy for the correction of malunion of metacarpal neck fractures. J Hand Surg Br 1992;17:580–582.
-
Vahey JW, Wegner DA, Hastings H. Effect of proximal phalangeal fracture deformity on extensor tendon function. J Hand Surg Am 1998;23:673–681.
-
Progress to passive ROM exercises, and use reverse blocking exercises to strengthen and rebalance the extensors.
-
If needed, and if healing is progressing appropriately, use static or dynamic splints to address pending joint contractures.
-
Encourage functional use of the hand long before the radiographs show complete bony consolidation.
OUTCOMES
- Encouraging results have been reported. In the largest reported series of 59 osteotomies Buchler et al 4 reported the following:
-
A 100% union rate
-
Satisfactory correction of the deformity in 76% of cases
-
A net gain in active ROM in 89% of the patients
-
Excellent and good functional results in 96% of patients requiring bony corrections only and 64% for those requiring bony and soft tissue correction

You Might Also Like