Thumb Carpometacarpal Arthrodesis: An Intraoperative Masterclass for Basal Joint Arthritis
Key Takeaway
This masterclass provides an exhaustive, real-time guide to thumb carpometacarpal (CMC) joint arthrodesis. Fellows will learn intricate surgical anatomy, precise intraoperative techniques, and critical pearls for managing advanced basal joint arthritis, ensuring optimal patient outcomes. We cover patient selection, detailed dissection, joint preparation, K-wire fixation, and postoperative rehabilitation, all from the operating surgeon's perspective.
Fellows, welcome to the operating theater. Today, we are undertaking a technically demanding yet profoundly rewarding procedure: Thumb Carpometacarpal (CMC) Joint Arthrodesis. While suspensionplasty and arthroplasty procedures have dominated the contemporary discourse regarding basal joint arthritis, arthrodesis remains an indispensable, highly effective, and biomechanically sound treatment option. It is specifically tailored for a distinct demographic: high-demand patients, manual laborers, and young individuals presenting with stage II or III disease who require absolute joint stability and maximum power grip. Our paramount objective today is to achieve a rigid, pain-free osseous union at the thumb base, thereby permanently restoring robust pinch and grip strength without the risk of subsequent implant subsidence or soft-tissue attenuation.
Comprehensive Introduction and Patho-Epidemiology
Before we execute our surgical approach, a profound understanding of the underlying pathology and patient presentation is mandatory. Surgical excellence is predicated on a deep respect for the disease process we are attempting to arrest.
Definition and Natural History
Osteoarthritis—or more accurately, osteoarthrosis—of the trapeziometacarpal joint is a pervasive and functionally devastating condition of the human hand. It is second only to the distal interphalangeal joint in absolute frequency but is exponentially more debilitating due to its catastrophic impact on opposition, power grip, and key pinch. This degenerative cascade typically initiates along the palmar aspect of the articulation. It is primarily driven by progressive attenuation and laxity of the anterior oblique ligament (AOL), which subsequently subjects the articular cartilage to unphysiological shear forces and eccentric loading.
This relentless mechanical wear eventually progresses to full-thickness cartilage loss, eburnation of the subchondral bone, marginal osteophyte formation, and ultimately, global involvement of the entire joint surface. In advanced stages, the degenerative process extends to the entire trapezium and frequently involves the scaphotrapezio-trapezoidal (STT) joint. It is imperative to remember that any articular fracture, particularly a Bennett or Rolando fracture at the base of the thumb metacarpal, drastically accelerates this post-traumatic arthritic process. Paradoxically, a perfectly reduced Bennett fracture might theoretically protect the joint by offloading the vulnerable volar-ulnar aspect, though any incongruity guarantees rapid degeneration.
Pathogenesis and Biomechanical Influences
The genesis of CMC joint arthrosis is multifactorial, encompassing a complex interplay of biochemical degradation and biomechanical instability. Synovial fluid laden with inflammatory cytokines (such as IL-1 and TNF-alpha) directly contributes to matrix metalloproteinase up-regulation and subsequent cartilage degradation. Epidemiologically, there is a vastly increased incidence in postmenopausal women, suggesting a complex, potentially protective role for estrogen that is lost with age, coupled with inherent differences in joint congruity and ligamentous laxity between sexes.
The critical biomechanical player in this pathology is the anterior (palmar) oblique ligament, colloquially referred to as the "beak ligament." Its degeneration, traumatic rupture, or functional incompetence leads to dorsal and radial subluxation of the metacarpal base during pinch activities. This abnormal translation on the biconcave saddle of the trapezium escalates the destructive shear forces, creating a vicious cycle of instability, cartilage wear, and further ligamentous attenuation.
Detailed Surgical Anatomy and Biomechanics
A masterclass in arthrodesis requires an intimate, three-dimensional understanding of the regional anatomy. We must navigate a dense network of neurovascular and tendinous structures to achieve adequate exposure without inducing iatrogenic morbidity.
Osteology and Articular Geometry
The thumb CMC joint is a classic biconcave saddle joint (articulatio sellaris). The trapezium is concave in the radioulnar plane and convex in the dorso-palmar plane, while the base of the first metacarpal has the reciprocal geometry. This unique configuration allows for a wide arc of motion—flexion, extension, abduction, adduction, and the composite motion of opposition—but renders the joint inherently unstable. It relies almost entirely on its capsuloligamentous envelope for stability, making these structures paramount.
Ligamentous Stabilizers
While anatomical studies have described up to 16 distinct ligaments surrounding the trapeziometacarpal joint, seven are considered the primary stabilizers of the thumb metacarpal. You must conceptualize these as a dynamic stabilizing network:
* Superficial and deep anterior oblique ligaments (sAOL and dAOL)
* Dorsal radial ligament (DRL) - increasingly recognized as a primary restraint to dorsal subluxation
* Posterior oblique ligament (POL)
* Ulnar collateral ligament (UCL)
* Intermetacarpal ligament (IML)
* Dorsal intermetacarpal ligament (DIML)
The remaining ligaments stabilize the trapezium itself to the scaphoid, trapezoid, and second metacarpal, providing a rigid foundation for thumb kinematics.
Neurovascular Structures
This is where meticulous surgical technique separates the master from the novice. The dorsal approach places several critical structures at immediate risk.
* Radial Sensory Nerve (RSN): This nerve courses superficially in the subcutaneous tissue over the dorsoradial aspect of the wrist. Its branching pattern is notoriously variable. It is extremely vulnerable during the initial skin incision and superficial dissection. Iatrogenic injury, traction neuropraxia, or entrapment in scar tissue can lead to debilitating neuromas or complex regional pain syndrome (CRPS), which will completely overshadow a successful bony fusion.
* Lateral Antebrachial Cutaneous Nerve (LABCN): The terminal branches of the LABCN frequently arborize into the radial aspect of the wrist and thumb base. They must be anticipated and protected alongside the RSN.
* Dorsal Branch of the Radial Artery: This critical vessel dives deep to the abductor pollicis longus (APL) and extensor pollicis brevis (EPB) tendons, traversing the anatomic snuffbox typically in a dorsal and ulnar direction before piercing the first dorsal interosseous muscle. It requires careful identification, mobilization, and protection. Laceration or aggressive retraction can compromise radial-sided hand perfusion, making a preoperative Allen test an absolute necessity.
Muscular Intervals and Tendons
- First Dorsal Compartment: Housing the APL and EPB tendons, this compartment forms the radial border of our approach. We will systematically release the retinaculum along its ulnar aspect. These tendons will be retracted to facilitate deep exposure.
- Thenar Musculature: While not directly divided in a dorsal approach, the thenar cone (abductor pollicis brevis, flexor pollicis brevis, opponens pollicis) is crucial for post-operative function. The adductor pollicis, inserting on the ulnar base of the proximal phalanx and metacarpal, is the primary deforming force driving the classic adduction contracture seen in advanced disease.
Exhaustive Patient Evaluation and Diagnostic Workup
Patient selection is the cornerstone of a successful arthrodesis. We must correlate subjective complaints with objective physical and radiographic findings.
Clinical History and Physical Examination
Patients typically present with an insidious onset of aching pain at the base of the thumb. This is invariably exacerbated by activities requiring forceful pinch or torque—turning a key, opening a jar, or wringing out a washcloth. Pain at rest suggests advanced, inflammatory disease. Crucially, subjective symptoms do not always correlate linearly with radiographic severity; treat the patient, not the radiograph.
On physical examination, advanced disease presents a characteristic deformity: dorsal subluxation of the metacarpal base and a severe adduction contracture of the first web space. This forces the metacarpophalangeal (MCP) joint into compensatory hyperextension, creating the classic "zig-zag" deformity of the thumb ray.
Our diagnostic maneuvers must be precise:
* CMC Grind Test: Axial compression coupled with circumduction of the metacarpal on the trapezium. Crepitus and reproduction of sharp pain confirm articular degradation.
* CMC Distraction Test: Axial traction of the metacarpal. Relief of pain suggests joint space narrowing is the primary nociceptive source.
* Finkelstein Maneuver: Essential to rule out concomitant De Quervain tenosynovitis, which frequently coexists.
* Allen Test: A mandatory preoperative assessment of radial and ulnar artery patency and palmar arch dominance, given our proximity to the radial artery.
Radiographic Assessment and Staging
High-quality plain radiographs are our primary imaging modality. Standard views include a pronated AP (Robert view), a true lateral of the thumb ray, and a 30-degree posteroanterior stress view to evaluate for dynamic subluxation.
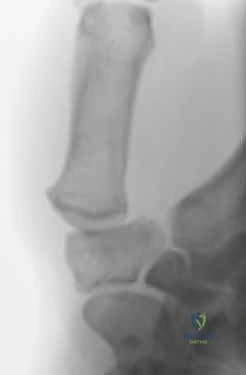
FIG 1 • AP radiograph of the thumb carpometacarpal joint demonstrating joint space narrowing, subchondral sclerosis, and marginal osteophytosis indicative of advanced basal joint arthritis.
We utilize the Eaton and Littler radiographic staging system to guide our interventions:
* Stage I: Normal-appearing joint space, or slight widening due to acute synovitis.
* Stage II: Joint space narrowing, subchondral sclerosis, and osteophytes smaller than 2 mm.
* Stage III: Significant joint space destruction, cystic changes, and osteophytes larger than 2 mm.
* Stage IV: Stage III changes at the CMC joint with concomitant arthrosis of the scaphotrapezial (STT) joint.
Tomaino et al. astutely emphasized the routine assessment of the STT joint to rule out pan-trapezial disease. This is a critical juncture, fellows: pan-trapezial involvement (Stage IV) is a strict contraindication for isolated CMC arthrodesis, as fusing the CMC joint will exponentially increase stress on an already arthritic STT joint, guaranteeing persistent pain.
Exhaustive Indications and Contraindications
The decision to fuse rather than resect or replace requires rigorous patient selection. Arthrodesis sacrifices mobility for absolute stability and power.
Patient Selection Criteria
The ideal candidate for CMC arthrodesis is a young (typically under 55 years of age), highly active individual, or a heavy manual laborer who requires maximum power grip and key pinch. These patients cannot afford the potential weakness, subsidence, or implant failure associated with trapeziectomy and ligament reconstruction tendon interposition (LRTI) or prosthetic arthroplasty.
Table: Indications and Contraindications
| Category | Specific Criteria | Rationale / Clinical Consequence |
|---|---|---|
| Absolute Indications | Stage II or III CMC Osteoarthritis in a young/heavy laborer | Provides definitive pain relief while maximizing grip/pinch strength. |
| Absolute Indications | Post-traumatic CMC arthritis (e.g., malunited Bennett fracture) | Restores anatomic alignment and stability to a destroyed joint. |
| Absolute Indications | Paralytic thumb requiring stabilization for pinch | Provides a rigid post against which other digits can articulate. |
| Absolute Contraindications | Stage IV Disease (STT or pan-trapezial arthritis) | Fusing the CMC joint will overload the arthritic STT joint, causing intractable pain. |
| Absolute Contraindications | Severe, uncorrectable MCP joint hyperextension (>20 degrees) | Fusing the CMC joint will force all motion to the MCP joint; if unstable, function is destroyed. |
| Relative Contraindications | Elderly, low-demand patients | LRTI or simple trapeziectomy provides adequate pain relief with faster recovery and preserved mobility. |
| Relative Contraindications | Advanced osteoporosis | High risk of hardware failure, screw cut-out, and nonunion. |
Pre-Operative Planning, Templating, and Patient Positioning
Meticulous preparation mitigates intraoperative complications. Preoperative templating ensures appropriate hardware selection, whether utilizing low-profile locking plates, headless compression screws, or Kirschner wires.
Anesthesia and Equipment Setup
This procedure is optimally performed under a regional brachial plexus block (supraclavicular or axillary) combined with monitored anesthesia care (MAC). This provides excellent intraoperative hemodynamics and superior postoperative analgesia. A pneumatic tourniquet is applied to the proximal brachium and inflated to 250 mmHg following exsanguination with an Esmarch bandage. A completely bloodless field is non-negotiable for the safe identification of the radial sensory nerve and radial artery.
Positioning and Tourniquet Application
The patient is placed in the supine position. The operative extremity is extended onto a radiolucent hand table. The arm must be meticulously padded to prevent ulnar neuropathy at the cubital tunnel. The C-arm fluoroscopy unit is positioned parallel to the table, entering from the distal or contralateral side to allow unimpeded AP and lateral imaging of the thumb ray throughout the procedure.
Step-by-Step Surgical Approach and Fixation Technique
Now, we commence the operative intervention. Maintain a systematic, tissue-respecting approach.
Incision and Superficial Dissection
We utilize a dorsal longitudinal approach. The incision, approximately 4-5 cm in length, is centered directly over the trapeziometacarpal joint, running parallel to the radial border of the extensor pollicis brevis (EPB).
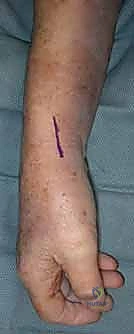
TECH FIG 1 • Surgical outline for the longitudinal incision along the first dorsal compartment, centered over the CMC joint.
Immediately upon incising the dermis, we transition to blunt dissection utilizing fine tenotomy scissors. Our immediate objective is the identification and preservation of the radial sensory nerve (RSN) branches.

TECH FIG 2 • Superficial dissection demonstrating the identification and careful mobilization of the radial sensory nerve branches using vessel loops.
Once identified, these delicate neural structures are gently mobilized and retracted radially or ulnarly using vessel loops. Excessive traction must be strictly avoided to prevent neuropraxia.
Joint Exposure and Capsulotomy
We proceed deep to the subcutaneous tissue to identify the first dorsal compartment. We incise the extensor retinaculum along its ulnar border, releasing the APL and EPB tendons. These tendons are retracted radially.
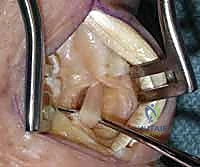
TECH FIG 3 • Deep dissection revealing the interval between the first dorsal compartment tendons and the extensor pollicis longus, with careful protection of the underlying dorsal radial artery.
Deep to the tendons, we must identify the dorsal branch of the radial artery as it crosses the operative field. It is meticulously dissected, mobilized, and protected with a vessel loop. We then perform a longitudinal or T-shaped capsulotomy over the CMC joint. Subperiosteal dissection exposes the base of the first metacarpal and the distal articular surface of the trapezium.
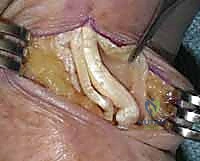
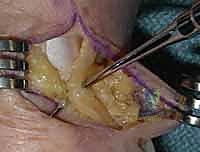
TECH FIG 4 • Completion of the capsulotomy and exposure of the degenerative trapeziometacarpal joint surfaces, revealing extensive cartilage eburnation.
Articular Preparation and Cartilage Resection
The success of an arthrodesis is entirely dependent on meticulous preparation of the osseous beds. All remaining articular cartilage and subchondral sclerotic bone must be radically excised down to healthy, bleeding cancellous bone.
We have two primary techniques for joint preparation: flat planar cuts using an oscillating saw, or cup-and-cone reaming. Today, we will employ the cup-and-cone technique, which maximizes the cancellous surface area for fusion and allows for multi-planar micro-adjustments of the thumb position prior to definitive fixation.
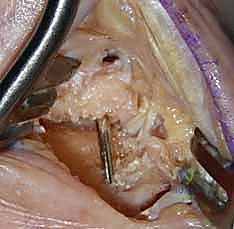
TECH FIG 5 • Utilizing a specialized concave reamer to prepare the base of the first metacarpal, creating a uniform, bleeding cancellous surface.
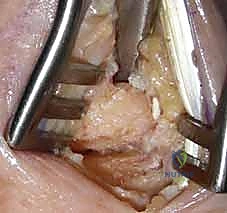
TECH FIG 6 • Curettage and further decortication of the trapezial articular surface. All sclerotic bone must be removed to ensure osteogenic potential.
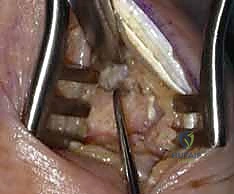
TECH FIG 7 • Final inspection of the prepared articular surfaces. Note the exposed, highly vascular cancellous bone architecture essential for a robust arthrodesis.
Coaptation, Alignment, and Provisional Fixation
This is the most critical juncture of the procedure. Fusing the thumb in an improper position will result in a catastrophic functional deficit. The thumb must be positioned in the "fist" or "pinch" position.
The exact biomechanical parameters for fusion are:
1. Palmar Abduction: 35 to 40 degrees.
2. Radial Extension: 10 to 15 degrees.
3. Pronation: 15 to 20 degrees, ensuring the pulp of the thumb perfectly opposes the pulps of the index and middle fingers.
Once optimal alignment is achieved, we provisionally stabilize the joint using two 0.045-inch or 0.062-inch Kirschner wires driven from the metacarpal into the trapezium.
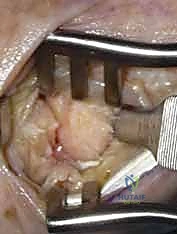
TECH FIG 8 • Provisional fixation with Kirschner wires. The thumb is held in the optimal position of function (palmar abduction and pronation) while the wires are advanced.
Definitive Internal Fixation Techniques
While K-wires alone can be used, they are associated with unacceptably high nonunion rates (up to 15%). Rigid internal fixation is mandatory. We can utilize dual crossed headless compression screws, a tension band construct, or a low-profile locking plate. Today, we are utilizing a specialized CMC fusion plate to provide absolute biomechanical stability.
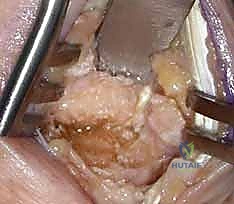
TECH FIG 9 • Application of a low-profile dorsal locking plate. The plate is contoured to match the anatomy of the metacarpal base and trapezium.
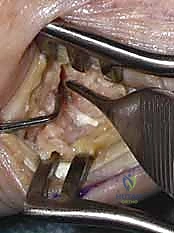
TECH FIG 10 • Final seating of the plate. Care is taken to ensure the hardware does not impinge on the STT joint proximally or irritate the extensor tendons dorsally.
If headless compression screws are chosen, they must be placed orthogonally to the joint surface to maximize compression. We confirm hardware placement and joint reduction with orthogonal fluoroscopic views.
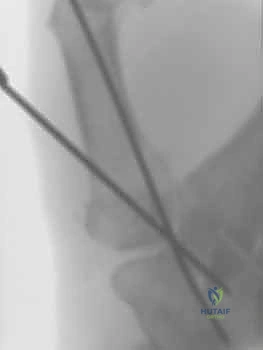
TECH FIG 11 • Intraoperative fluoroscopy demonstrating the placement of a compression screw across the arthrodesis site to augment plate fixation or act as primary fixation.
TECH FIG 12 • Final fluoroscopic AP view confirming anatomic alignment, excellent bony apposition, and appropriate hardware length without joint penetration.
Closure and Immediate Postoperative Care
Following copious irrigation and deflation of the tourniquet to ensure meticulous hemostasis, the capsule is closed with 4-0 absorbable sutures. The extensor retinaculum is loosely reapproximated to prevent tendon bowstringing, ensuring the RSN is completely free of the closure. The skin is closed with non-absorbable monofilament sutures. A sterile dressing and a rigid thumb spica splint are applied in the operating room.
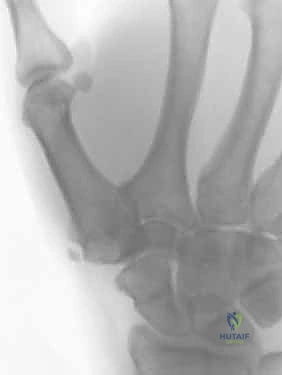
FIG 2 • Postoperative radiograph demonstrating a solid osseous union of the trapeziometacarpal joint at 12 weeks, with hardware intimately conforming to the dorsal cortex.
Complications, Incidence Rates, and Salvage Management
Despite meticulous technique, complications can occur. As surgeons, we must be prepared to identify and manage them aggressively.
Intraoperative and Early Postoperative Complications
- Radial Sensory Nerve Neuritis: The most common early complication (up to 10-15%). Caused by traction or entrapment. Management includes early desensitization therapy, gabapentinoids, and rarely, surgical neurolysis.
- Infection: Superficial infections are managed with oral antibiotics; deep infections require immediate irrigation, debridement, and potential hardware removal.
- Malposition: Fusing the thumb in excessive adduction prevents grasping large objects; excessive extension prevents fine pinch. This requires revision osteotomy if functionally limiting.
Late Complications and Nonunion
- Nonunion: The historical Achilles heel of this procedure, with older studies reporting rates up to 15% with K-wire fixation. Modern locking plates and compression screws have reduced this to <5%. Asymptomatic nonunions require no treatment. Symptomatic nonunions require revision arthrodesis with autologous iliac crest bone grafting (ICBG).
- Hardware Prominence: Due to the paucity of dorsal soft tissue, plates may become symptomatic, necessitating removal after definitive fusion is confirmed (typically after 6-9 months).
- Adjacent Segment Disease: Arthrodesis alters kinematics, increasing stress on the STT and MCP joints. Late STT arthritis may require subsequent STT fusion or excision of the distal scaphoid pole.
Table: Complications and Management Strategies
| Complication | Incidence | Etiology / Risk Factor | Management / Salvage Strategy |
|---|---|---|---|
| Nonunion | 2% - 12% (Fixation dependent) | Inadequate joint prep, smoking, K-wire use | Revision arthrodesis with structural autograft (ICBG) and rigid plate fixation. |
| RSN Neuroma / Neuritis | 5% - 15% | Iatrogenic traction, tight closure, scar entrapment | Aggressive hand therapy, gabapentin; surgical neurolysis or neurectomy for refractory cases. |
| Symptomatic Hardware | 10% - 20% | Prominent dorsal plate, thin subcutaneous tissue | Hardware removal strictly after CT confirmation of solid osseous union. |
| Adjacent Joint Arthritis (STT) | 10% - 25% (Long-term) | Altered biomechanics, unrecognized pre-op stage IV disease | STT arthrodesis, partial trapezoidectomy, or conversion to complete trapeziectomy. |
| Malunion / Poor Positioning | < 5% | Failure to achieve the "fist" position intraoperatively | Corrective closing-wedge osteotomy through the fusion mass. |
Phased Post-Operative Rehabilitation Protocols
A successful surgery can be ruined by poor postoperative rehabilitation. A strict, phased protocol is essential to protect the osteosynthesis while preventing stiffness in adjacent digits.
Immediate Immobilization Phase (Weeks 0-4)
The patient remains in the rigid, custom-molded thumb spica cast applied intraoperatively. The interphalangeal (IP) joint of the thumb and all fingers are left free. Absolute compliance with elevation and active range of motion of the fingers, elbow, and shoulder is mandated to prevent complex regional pain syndrome (CRPS) and dependent edema
