Pediatric Distal Femoral Osteosarcoma: A Detailed Orthopedic Case Study
Key Takeaway
Pediatric distal femoral osteosarcoma diagnosis uses clinical presentation like knee pain and mass. Imaging includes X-rays (lytic/blastic lesions, sunburst reaction, Codman's triangle), MRI for local staging, and CT for pulmonary metastases. This guides critical orthopedic oncology treatment.
Patient Presentation and History
A 14-year-old male, previously healthy and highly active in competitive scholastic athletics, presented to the orthopedic oncology clinic with a five-month history of progressive, insidious onset pain localized to the left knee and distal thigh. The clinical timeline is highly representative of primary malignant bone tumors in the pediatric and adolescent population, where initial symptoms are frequently misattributed to minor athletic trauma, overuse syndromes, or physiological growth spurts.
Initially, the patient described the pain as intermittent, dull, and mechanically related to high-impact activities such as sprinting and jumping. This early symptomology was managed conservatively with rest and intermittent cryotherapy, yielding transient symptomatic relief. However, over the preceding eight weeks, the clinical picture evolved significantly. The pain transitioned from activity-dependent to constant, developing a severe nocturnal component that consistently awakened the patient from sleep. This transition to rest pain and night pain is a critical clinical indicator of an aggressive, space-occupying intramedullary process causing endosteal pressure and periosteal stretching. The pain became entirely refractory to maximum recommended doses of over-the-counter non-steroidal anti-inflammatory drugs and acetaminophen.
Concurrently, the patient and his family noted a slowly enlarging, firm, and non-mobile soft tissue mass arising from the anterior and lateral aspects of the distal left thigh. This mass had become markedly more prominent over the four to six weeks prior to presentation. The patient reported a substantial decline in athletic performance, eventually leading to complete cessation of sports participation due to mechanical restriction and severe discomfort during weight-bearing activities.
A comprehensive review of systems was largely unremarkable. The patient denied any history of acute macrotrauma, penetrating injury, or prior surgical interventions to the left lower extremity. There were no constitutional symptoms such as unexplained weight loss, night sweats, cyclical fevers, chills, or generalized malaise, which are often sought to differentiate between infectious etiologies, systemic inflammatory conditions, and various neoplastic processes.
The patient’s past medical history was entirely benign. He had no known congenital anomalies, prior hospitalizations, or chronic medical conditions. He was not taking any prescription medications or supplements. Family history was extensively reviewed and was negative for any hereditary cancer syndromes, such as Li-Fraumeni syndrome or hereditary retinoblastoma, which are known to carry a significant genetic predisposition for the development of osteosarcoma. Furthermore, there was no family history of other sarcomas, early-onset breast carcinomas, or hematological malignancies.
Clinical Examination Findings
The physical examination was conducted with a focus on evaluating the local extent of the disease, assessing the functional deficit, and determining the proximity of the suspected neoplasm to critical neurovascular structures.
General Inspection and Gait Biomechanics
Upon initial observation, the patient demonstrated a profoundly antalgic gait. He exhibited a shortened stance phase on the affected left lower extremity, actively minimizing the duration of axial loading. A noticeable lateral trunk lean over the left hip was observed during the stance phase, a compensatory mechanism to reduce the joint reaction forces across the painful distal femur. Despite the localized pathology, the patient appeared systemically well-nourished and developed appropriately for his stated age, with no evidence of cachexia, jaundice, or pallor that might suggest advanced metastatic disease or profound systemic illness.
Local Inspection of the Left Lower Extremity
Detailed inspection of the left distal thigh and knee revealed a prominent, visually apparent fusiform swelling centered over the distal third of the femoral diaphysis and metaphysis. The mass measured approximately 8 centimeters in the longitudinal axis and 6 centimeters in the transverse axis, extending proximally from the superior pole of the patella.
The integument overlying the mass appeared taut, shiny, and slightly erythematous compared to the contralateral limb. A distinct network of prominent, engorged superficial veins was visible coursing over the anterior and lateral aspects of the mass, indicative of the robust neoangiogenesis and increased regional blood flow characteristic of high-grade sarcomas. There were no cutaneous manifestations of prior trauma, such as ecchymosis, abrasions, or lacerations. Furthermore, there were no sinus tracts, areas of ulceration, or skin necrosis. Mild disuse atrophy was noted in the proximal quadriceps musculature when compared to the right thigh, although the calf musculature remained symmetric.
Palpation and Compartment Assessment
Palpation confirmed the presence of a large, firm, and unyielding mass that was intimately fixed to the underlying osseous structures of the distal femur. The mass elicited moderate to severe point tenderness, particularly along its lateral and anterior borders. The mass was distinctly non-compressible, differentiating it from purely cystic or vascular malformations. Superiorly, the margins of the mass were ill-defined, blending imperceptibly into the surrounding vastus intermedius and vastus lateralis musculature, suggesting extraosseous soft tissue extension. Distally, the mass approached the suprapatellar pouch but appeared to spare the patella itself.
The skin overlying the tumor exhibited a localized increase in temperature, further corroborating the presence of a highly vascularized and metabolically active lesion. Evaluation of the knee joint revealed a small to moderate, tense effusion. A patellar tap test was positive, indicating intra-articular fluid accumulation. This effusion could represent either a sympathetic response to the adjacent metaphyseal inflammation or direct intra-articular extension of the tumor, a critical distinction that dictates the necessity of extra-articular vs intra-articular resection margins during definitive surgical management.
Regional lymph node basins, specifically the superficial and deep inguinal nodes as well as the popliteal nodes, were carefully palpated. No pathological lymphadenopathy was identified, which is consistent with the typical metastatic behavior of osteosarcoma, which preferentially disseminates hematogenously rather than via the lymphatic system.
Range of Motion and Joint Mechanics
Evaluation of the left knee joint kinematics demonstrated a profound restriction in both active and passive range of motion, secondary to pain, mechanical block from the soft tissue mass, and tethering of the extensor mechanism.
Active flexion was severely limited to 0 to 80 degrees, whereas the contralateral asymptomatic knee demonstrated a full, unrestricted arc of motion from 0 to 140 degrees. Active extension revealed an extension lag of -5 degrees. Passive extension to 0 degrees was achievable but elicited severe pain at terminal extension, likely due to tensioning of the anterior joint capsule and the overlying compromised quadriceps expansion. Axial loading of the knee joint, as well as the application of varus, valgus, and rotational stresses, exacerbated the patient's pain, indicating significant structural compromise of the distal femoral metaphysis and imminent risk of pathological fracture.
Neurological and Vascular Assessment
A meticulous neurovascular examination of the left lower extremity was performed, given the close anatomical proximity of the distal femoral mass to the superficial femoral artery as it transitions through the adductor hiatus into the popliteal space.
Motor function was assessed and graded at 5/5 in all major muscle groups of the lower extremity, including hip flexors, extensors, abductors, and adductors, as well as ankle dorsiflexors, plantarflexors, invertors, and evertors. While knee flexion and extension strength were technically intact, testing was limited by patient guarding and pain during anti-gravity movements.
Sensory examination revealed intact light touch, pinprick, and two-point discrimination across all dermatomes from L2 through S1. There were no paresthesias, dysesthesias, or signs of hyperalgesia in the distribution of the saphenous, common peroneal, or tibial nerves.
Vascular assessment demonstrated robust, palpable, and bilaterally symmetrical pulses in the femoral, popliteal, dorsalis pedis, and posterior tibial arteries. Capillary refill in the toes was brisk, occurring in less than two seconds. Despite the significant size of the soft tissue mass, there was no clinical evidence of direct neurovascular compression, compartment syndrome, or distal ischemia.
Imaging and Diagnostics
The diagnostic algorithm for a suspected primary malignant bone tumor requires a systematic and highly coordinated approach, beginning with plain radiography and progressing to advanced cross-sectional imaging, functional staging studies, and ultimately, histological confirmation via biopsy.
Initial Plain Radiography
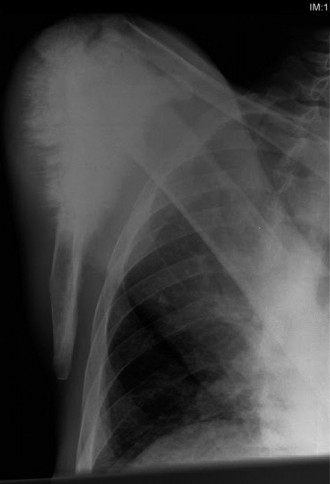
Orthogonal anteroposterior and lateral radiographs of the left distal femur and knee were obtained as the initial imaging modality. These films revealed a highly aggressive, destructive osseous lesion centered within the distal femoral metaphysis, with extension proximally into the diaphyseal region.

The lesion exhibited a mixed lytic and blastic radiographic appearance. The radiolucent (lytic) areas represented aggressive trabecular bone destruction by the proliferating tumor cells, while the radiodense (blastic) areas indicated the production of chaotic, disorganized neoplastic osteoid matrix, a hallmark of osteosarcoma.
Significant cortical destruction was evident, particularly involving the anterior and lateral cortices of the distal femur. The tumor had clearly breached the cortical confines, leading to a massive extraosseous soft tissue extension.
The periosteal reaction was profound and highly characteristic of a rapidly growing malignant process. A prominent "sunburst" or "hair-on-end" periosteal reaction was visualized, caused by the ossification of Sharpey's fibers as the periosteum is rapidly elevated and stretched by the expanding tumor mass. Furthermore, a distinct Codman's triangle was identified along the posteromedial cortex. This radiographic sign represents the triangular area of reactive subperiosteal new bone formed at the advancing edge of the tumor where the periosteum is lifted away from the underlying cortex but has not yet been entirely destroyed.
A large, partially mineralized soft tissue mass was clearly delineated, extending anteriorly into the substance of the quadriceps musculature and laterally into the vastus lateralis. The joint space appeared radiographically preserved, although the true extent of epiphyseal or intra-articular involvement cannot be definitively excluded on plain films alone.
Advanced Cross Sectional Imaging
Following the concerning radiographic findings, urgent advanced imaging was coordinated to precisely define the local anatomical extent of the tumor, assess for neurovascular involvement, and evaluate for synchronous osseous lesions.
Magnetic Resonance Imaging (MRI) of the Left Femur and Knee:
A dedicated, contrast-enhanced MRI of the entire left femur, including the hip and knee joints, was performed. MRI is the gold standard for evaluating the local staging of primary bone sarcomas.
* Intramedullary Extent: T1-weighted sequences demonstrated replacement of the normal hyperintense fatty marrow by a hypointense tumor infiltrate. The intramedullary extent of the tumor was accurately measured to assist in preoperative planning for the proximal osteotomy level.
* Soft Tissue Extension: T2-weighted and Short Tau Inversion Recovery (STIR) sequences highlighted the massive extraosseous soft tissue component, which demonstrated heterogeneous hyperintensity indicative of cellular tumor, necrosis, and peritumoral edema.
* Neurovascular Bundle Assessment: Axial sequences were critical for evaluating the relationship of the tumor to the popliteal artery and vein. In this patient, the tumor was noted to abut the neurovascular bundle posteriorly, but a distinct plane of fat or reactive tissue was preserved, suggesting that the vessels were displaced rather than directly encased or invaded. This finding is paramount for determining the feasibility of a limb-salvage procedure.
* Epiphyseal and Joint Involvement: The MRI confirmed extension of the tumor through the physeal scar into the distal femoral epiphysis. However, the articular cartilage and the cruciate ligaments appeared intact, with no gross evidence of direct tumor extension into the knee joint cavity, despite the presence of a reactive joint effusion.
* Skip Metastases: A coronal STIR sequence of the entire femur was meticulously reviewed to rule out "skip metastases"—synchronous, non-contiguous foci of tumor within the same bone or trans-articularly in the proximal tibia. No skip lesions were identified.
Computed Tomography (CT) of the Left Femur:
A non-contrast CT scan of the distal femur with 3D reconstructions was obtained to further characterize the osseous anatomy, define the extent of cortical destruction, and identify subtle matrix mineralization patterns that might not be fully appreciated on MRI. The CT scan confirmed the aggressive cortical breakthrough and the dense, cloud-like osteoid matrix production characteristic of osteoblastic osteosarcoma.
Systemic Staging Studies
Given the high propensity for hematogenous dissemination, comprehensive systemic staging is mandatory prior to the initiation of any therapeutic intervention.
- Computed Tomography (CT) of the Chest: The lungs are the most common site of metastasis for osteosarcoma. A high-resolution, non-contrast CT of the chest was performed to evaluate for pulmonary nodules. The scan revealed clear lung fields with no evidence of pulmonary metastatic disease.
- Positron Emission Tomography combined with Computed Tomography (PET CT) or Technetium 99m Bone Scan: To assess for distant osseous metastases, a whole-body FDG PET-CT was utilized. The primary lesion in the distal femur demonstrated intense, heterogeneous FDG avidity (high SUVmax), consistent with a highly metabolically active malignancy. No other areas of abnormal radiotracer uptake were identified throughout the axial or appendicular skeleton, confirming localized disease.
Biopsy and Histopathological Diagnosis
The definitive diagnosis of osteosarcoma requires histopathological confirmation. The biopsy of a suspected primary bone tumor is a critical procedure that must be meticulously planned and executed, ideally by the orthopedic oncologist who will perform the definitive resection. Poorly planned biopsies can contaminate neurovascular structures, compromise tissue planes, and convert a limb-salvage candidate into an obligate amputation.
In this case, an image-guided core needle biopsy was performed under conscious sedation.
* Biopsy Principles: The biopsy tract was placed longitudinally along the anterior aspect of the distal thigh, directly in line with the planned extensile surgical approach for the definitive resection. The needle traversed the vastus intermedius, avoiding the vastus medialis and the medial neurovascular bundle. Multiple core samples were obtained from the soft tissue extension and the peripheral osseous margins of the tumor, avoiding the central necrotic core to ensure a high yield of viable diagnostic tissue. Meticulous hemostasis was achieved to prevent a post-biopsy hematoma, which can spread tumor cells along fascial planes.
- Histopathology: The biopsy specimens were evaluated by a specialized musculoskeletal pathologist. Microscopic examination revealed a highly cellular neoplasm composed of pleomorphic, hyperchromatic spindle-shaped and epithelioid cells. The defining diagnostic feature was the presence of malignant cells directly producing fine, lace-like, unmineralized osteoid matrix. Frequent atypical mitotic figures and areas of coagulative necrosis were observed. These findings established a definitive diagnosis of High Grade Conventional Osteoblastic Osteosarcoma.
Differential Diagnosis
The clinical and radiographic presentation of an aggressive, destructive bone lesion in a pediatric or adolescent patient necessitates a focused differential diagnosis. While osteosarcoma is the most likely diagnosis given the classic radiographic features, other malignant and infectious etiologies must be systematically considered and ruled out.
| Differential Diagnosis | Demographics and Clinical Presentation | Radiographic and Imaging Features | Histological and Laboratory Findings |
|---|---|---|---|
| Osteosarcoma | Adolescents and young adults (10-25 years). Bimodal peak (second peak >60 years with Paget's disease). Pain, swelling, night pain. | Metaphyseal location. Mixed lytic/blastic. Sunburst periosteal reaction, Codman's triangle. Osteoid matrix production. | Pleomorphic spindle cells producing malignant osteoid. Elevated Alkaline Phosphatase (ALP) and Lactate Dehydrogenase (LDH) in some cases. |
| Ewing Sarcoma | Children and young adolescents (5-20 years). Pain, swelling. May present with systemic symptoms (fever, weight loss, elevated ESR/CRP) mimicking infection. | Diaphyseal or metadiaphyseal location. Permeative, moth-eaten lytic destruction. "Onion-skin" (lamellated) periosteal reaction. Large soft tissue mass. | Small round blue cells. CD99 positive. t(11;22) chromosomal translocation (EWS-FLI1 fusion gene). |
| Osteomyelitis (Acute/Subacute) | Any age, but common in children. Acute onset pain, fever, erythema, localized warmth. History of recent infection or trauma. | Metaphyseal location. Early x-rays may be normal. Later shows regional osteopenia, lytic destruction, smooth periosteal reaction. Brodie's abscess in subacute cases. | Acute inflammatory infiltrate (neutrophils). Positive tissue cultures (Staphylococcus aureus most common). Elevated WBC, ESR, and CRP. |
| Chondrosarcoma (Primary) | Older adults (>40 years). Rare in pediatric population. Insidious onset of pain and swelling. | Metaphyseal or diaphyseal. Lytic lesion with intralesional "rings and arcs" or "popcorn" calcifications (chondroid matrix). Endosteal scalloping. | Malignant chondrocytes in a hyaline cartilaginous matrix. Permeation of host bone trabeculae. |
| Langerhans Cell Histiocytosis (Eosinophilic Granuloma) | Children and young adults (1-15 years). Localized pain. May have multiple lesions. | Punched-out lytic lesions. Can have a "hole-within-a-hole" appearance (beveled edge). Solid periosteal reaction. | Proliferation of Langerhans cells (grooved nuclei). Eosinophilic infiltrate. CD1a and S100 positive. Birbeck granules on electron microscopy. |
Surgical Decision Making and Classification
The management of high-grade osteosarcoma requires a highly coordinated, multidisciplinary approach involving orthopedic oncology, medical oncology, musculoskeletal radiology, and pathology. Following the definitive histopathological diagnosis and completion of the staging workup, the patient's case was presented at the institutional multidisciplinary sarcoma tumor board.
Staging and Classification
The tumor was classified using the Enneking Surgical Staging System for Musculoskeletal Sarcomas.
* Grade (G): High grade (G2) based on the histopathological presence of pleomorphic cells, high mitotic rate, and necrosis.
* Site (T): Extracompartmental (T2). The tumor had breached the femoral cortex and extended into the surrounding soft tissue compartments of the thigh.
* Metastasis (M): No regional or distant metastasis identified (M0).
Therefore, the patient was staged as Enneking Stage IIB (High grade, extracompartmental, without metastasis). This stage dictates an aggressive, multimodal treatment paradigm.
Multidisciplinary Treatment Protocol
The standard of care for localized, high-grade osteosarcoma involves a sandwich therapy approach: neoadjuvant (preoperative) chemotherapy, followed by definitive local surgical control, and concluding with adjuvant (postoperative) chemotherapy.
Neoadjuvant Chemotherapy:
The patient was initiated on a standard multi-agent neoadjuvant chemotherapy regimen, typically consisting of High-Dose Methotrexate, Doxorubicin (Adriamycin), and Cisplatin (the MAP protocol). The rationale for neoadjuvant chemotherapy is multifaceted:
1. Eradication of Micrometastatic Disease: Osteosarcoma is considered a systemic disease at presentation, with subclinical micrometastases presumed to be present even with negative staging scans. Early systemic therapy targets these micrometastases.
2. Tumor Cytoreduction: Chemotherapy aims to induce tumor necrosis, shrink the soft tissue mass, and potentially facilitate a less morbid limb-salvage procedure by increasing the distance between the tumor capsule and critical neurovascular structures.
3. Assessment of Histologic Response: The degree of tumor necrosis observed in the resected specimen following neoadjuvant chemotherapy is one of the most powerful prognostic indicators for overall survival. A good response is typically defined as greater than 90% tumor necrosis (Huvos Grade III or IV).
Surgical Options and Rationale
Following approximately 10 to 12 weeks of neoadjuvant chemotherapy, the patient underwent restaging MRI and CT scans to evaluate the local and systemic response. The restaging MRI demonstrated a reduction in the peritumoral edema, ossification of the soft tissue mass rim, and no evidence of neurovascular encasement, confirming that the patient remained an excellent candidate for limb-salvage surgery.
The surgical decision-making process involves balancing the absolute requirement for oncologic clearance (achieving negative surgical margins) with the desire to maximize postoperative functional outcome and quality of life. The primary surgical options considered were:
- Transfemoral Amputation: Historically the standard of care, amputation provides definitive local control but results in significant functional and psychological morbidity. In the modern era, amputation is generally reserved for cases where the tumor extensively encases the major neurovascular bundle, making limb salvage impossible without leaving gross residual disease, or in cases of severe infection or pathological fracture with massive soft tissue contamination. Given the clear tissue planes around the popliteal vessels in this patient, amputation was not the primary recommendation.
- Rotationplasty (Van Nes Procedure): This involves an intercalary resection of the distal femur and knee joint, followed by 180-degree external rotation of the tibia and foot, and vascular anastomosis. The ankle joint subsequently functions as a knee joint, allowing for the fitting of a customized below-knee prosthesis. Rotationplasty provides excellent long-term durability, allows for high-impact activities, and avoids the complications associated with massive endoprostheses (e.g., aseptic loosening, deep infection). However, it is associated with significant cosmetic and psychological challenges. This option was discussed extensively with the patient and family, but they opted for endoprosthetic reconstruction.
- Limb Salvage with Distal Femoral Replacement (Megaprosthesis): This is the most common surgical approach for distal femoral osteosarcomas in skeletally mature or near-mature adolescents. It involves an en bloc wide resection of the distal femur, the tumor, the biopsy tract, and a cuff of normal surrounding tissue, followed by reconstruction using a modular metallic endoprosthesis. This approach provides a cosmetically acceptable limb and rapid postoperative mobilization. The primary risks include long-term mechanical failure (aseptic loosening, hinge wear), periprosthetic joint infection, and the potential need for multiple revision surgeries over the patient's lifetime.
Given the patient's age, skeletal maturity (near-closed physes), the lack of neurovascular encasement, and the strong preference of the patient and family for a cosmetically normal-appearing limb, Limb Salvage with Wide En Bloc Resection and Modular Distal Femoral Replacement was selected as the definitive surgical intervention.
Preoperative Templating and Margin Planning
Meticulous preoperative planning is essential. Using the restaging MRI, the proximal extent of the intramedullary tumor was identified. A planned osteotomy site was marked at least 3 centimeters proximal to the most proximal MRI abnormality to ensure a wide osseous margin. The soft tissue margins were planned to include an extrafascial dissection, resecting the vastus intermedius en bloc with the tumor while preserving the vastus medialis and vastus lateralis where they were not directly involved.
Templating for the modular endoprosthesis was performed using calibrated digital radiographs to determine the appropriate stem diameter, stem length, and the size of the articular components required to restore the patient's native joint line and leg length.
Surgical Technique and Intervention
The surgical procedure was performed under general anesthesia with the patient positioned supine on a radiolucent operating table. A non-sterile pneumatic tourniquet was placed as proximally as possible on the left thigh but was not inflated. Tourniquet use in orthopedic oncology is generally avoided during the resection phase to prevent venous stasis and the theoretical risk of forcing tumor emboli into the systemic circulation during limb exsanguination. The tourniquet serves strictly as a life-saving backup in the event of catastrophic hemorrhage from the major vessels.
Surgical Approach and Biopsy Tract Excision
An extensile anteromedial approach to the distal femur was utilized. The skin incision incorporated the previous biopsy tract, utilizing an elliptical incision to excise the tract en bloc with a 1 to 2-centimeter margin of normal skin. The incision was extended proximally along the anterior aspect of the thigh and distally over the medial parapatellar region, ending at the tibial tubercle.
Thick fasciocutaneous flaps were elevated to expose the anterior compartment musculature. The rectus femoris was identified and retracted laterally. The vastus medialis was identified, and the dissection proceeded along the intermuscular septum.
Neurovascular Dissection and Protection
The critical initial step of the deep dissection involved the identification and protection of the superficial femoral artery and vein as they exit the adductor canal (Hunter's canal) and transition into the popliteal space.
The adductor magnus tendon was identified, and the adductor hiatus was opened. The vascular bundle was meticulously dissected free from the posterior aspect of the distal femur and the posterior capsule of the tumor. Vessel loops were placed around the popliteal artery and vein for continuous control and retraction. The sciatic nerve, and its bifurcation into the tibial and common peroneal nerves, were identified in the posterior compartment and protected throughout the procedure. The preservation of a pristine layer of healthy tissue (e.g., epimysium, fat) between the tumor pseudocapsule and the neurovascular structures is paramount to achieving a wide margin.
En Bloc Resection and Margin Assessment
Once the posterior neurovascular structures were safely mobilized and retracted, the anterior and lateral soft tissue dissections were completed. The vastus intermedius, which was intimately involved with the anterior tumor mass, was sacrificed and left attached to the specimen.
Attention was then directed to the proximal osseous margin. Based on preoperative MRI measurements, the planned osteotomy site was identified on the femoral diaphysis. A sterile ruler was used to measure the exact distance from the joint line. The periosteum was circumferentially incised at this level, and a transverse osteotomy was performed using an oscillating sagittal saw.
Following the osteotomy, a sample of the proximal intramedullary canal marrow was obtained using a curette and sent for immediate intraoperative frozen section analysis. The pathologist confirmed the absence of malignant cells in the marrow margin, allowing the procedure to proceed to reconstruction.
Distally, the resection involved an extra-articular or intra-articular approach depending on preoperative imaging. In this case, given the lack of direct joint invasion on MRI but the presence of an effusion, a wide intra-articular resection was performed. The patellar tendon was carefully preserved. The medial and lateral collateral ligaments, as well as the anterior and posterior cruciate ligaments, were transected at their femoral insertions. The posterior joint capsule was incised, and the entire distal femur, encompassing the tumor, the biopsy tract, and the surrounding soft tissue cuff, was delivered en bloc from
You Might Also Like

