Complications of Distal Radius Fractures: Prevention, Biomechanics, and Surgical Management
Key Takeaway
Distal radius fractures present a broad spectrum of potential complications, ranging from malunion and hardware failure to tendon rupture and complex regional pain syndrome (CRPS). Overall complication rates vary from 6% to 80%. Successful management requires a profound understanding of wrist biomechanics, meticulous surgical technique—particularly regarding the watershed line during volar plating—and evidence-based postoperative protocols, including Vitamin C prophylaxis, to optimize patient outcomes and mitigate long-term morbidity.
INTRODUCTION TO DISTAL RADIUS COMPLICATIONS
The management of distal radius fractures has evolved significantly with the advent of locked volar plating and fragment-specific fixation; however, the type and frequency of complications remain highly variable across reported series. In a comprehensive literature review, McKay et al. demonstrated that overall complication rates range dramatically from 6% to 80%, with rates of posttraumatic arthritis spanning from 7% to 65%.
As orthopedic surgeons, mitigating these risks requires a profound understanding of carpal kinematics, meticulous surgical execution, and vigilant postoperative care. Complications can occur regardless of the management strategy chosen—operative or nonoperative—but the sequelae of specific complications can be significantly lessened by prompt, problem-specific intervention.
Incidence of Specific Complications
Based on aggregated clinical data, the incidence of complications following distal radius fractures can be stratified as follows:
* Arthritis/Arthrosis: 7% – 65%
* Loss of Motion: 0% – 31%
* Hardware Complications: 1.4% – 26%
* Nerve Compression/Neuritis: 0% – 17%
* Complex Regional Pain Syndrome (CRPS): 0.3% – 35%
* Osteomyelitis: 4% – 9%
* Dupuytren Contracture: 2% – 9%
* Tendon Rupture/Tenosynovitis: 0% – 12%
* Delayed Union/Nonunion: 0.7% – 4%
* Radioulnar Synostosis: 0% – 1.3%
MALUNION AND POSTTRAUMATIC ARTHRITIS
Jupiter and Fernandez identified malunion—presenting with either an intraarticular step-off or an extraarticular deformity—as the most frequent complication following distal radius fractures. The reported incidence of distal radial malunion is approximately 17%, occurring more frequently after nonoperative management than operative osteosynthesis.
Biomechanics of Deformity
The most common extraarticular deformities include:
1. Shortening (Loss of Radial Height): Alters the load distribution across the radiocarpal and ulnocarpal joints. Normal variance dictates that 80% of axial load is transmitted through the radius and 20% through the ulna. Radial shortening of just 2.5 mm can shift this ratio to 60:40, leading to ulnocarpal impaction syndrome and degenerative tears of the triangular fibrocartilage complex (TFCC).
2. Loss of Volar Tilt (Dorsal Angulation): Normal volar tilt is approximately 11 degrees. Dorsal angulation beyond neutral shifts the center of rotation dorsally, increasing load on the dorsal radiocarpal ligaments and predisposing the patient to midcarpal instability and dorsal intercalated segment instability (DISI).
3. Loss of Radial Inclination: Normal inclination is 22 degrees. Loss of inclination compromises the tethering effect of the radioscaphocapitate ligaments, leading to ulnar translation of the carpus.
Clinical Pearl: Intraarticular step-offs greater than 2 mm are highly predictive of early-onset posttraumatic radiocarpal arthrosis. Anatomic reduction of the articular surface is paramount, particularly in young, high-demand patients.
NONUNION
Nonunion of distal radial fractures is exceptionally rare, occurring in fewer than 1% of patients. Paradoxically, it is reported to be more frequent after operative treatment than nonoperative treatment, often due to iatrogenic devascularization or mechanical failure.
Predisposing Risk Factors
- Biological Factors: Open fractures, severe comminution, deep infections, pathological lesions (e.g., giant cell tumors, metastatic disease), and soft tissue interposition.
- Mechanical Factors: Inadequate internal fixation, excessive distraction utilizing an external fixator (spanning the radiocarpal joint too aggressively), and concomitant fractures of the distal ulna that destabilize the forearm axis.
HARDWARE AND TENDON COMPLICATIONS
Tendon complications represent a significant source of iatrogenic morbidity, most frequently observed after locked volar plating. Flexor tendon ruptures have been reported in up to 12% of patients treated with this modality.
Flexor Tendon Impingement and the Watershed Line
The "watershed line" is a transverse ridge marking the most volar margin of the distal radius, where the joint capsule originates. Flexor tendons (specifically the flexor pollicis longus [FPL] and the flexor digitorum profundus [FDP] to the index finger) lie in intimate contact with the bone at this level.
Complications arise when:
* The plate is placed too distal, crossing the watershed line.
* The plate is lifted off the bone due to inadequate contouring.
* Prominent screw heads abrade the traversing tendons.
To mitigate these risks, Rhee et al. outlined several critical measures:
1. Placement of volar plates strictly proximal to the watershed line.
2. Meticulous closure of the pronator quadratus over the volar plate to serve as a biological interpositional graft.
3. Use of shorter unicortical screws or smooth pegs in the most distal locking holes.

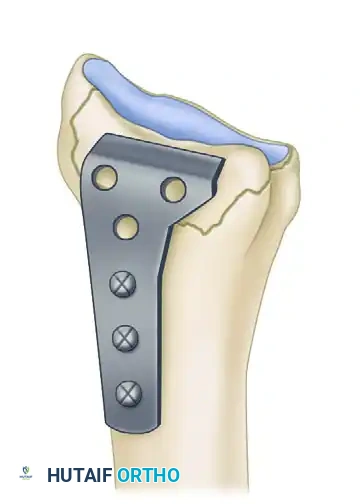
The L-plate provides a volar buttress to the volar rim of the lunate facet, yet allows fixation to the subcutaneous radial side of the proximal fragment, minimizing tendon abrasion.
Extensor Tendon Complications
Extensor tendon ruptures (most commonly the extensor pollicis longus [EPL]) occur due to dorsal screw penetration. The EPL tendon is particularly vulnerable as it acutely angles around Lister's tubercle.
Surgical Warning: Standard AP and lateral fluoroscopic views are insufficient to detect dorsal screw penetration. A dorsal tangential view (skyline view of the dorsal cortex) is mandatory during volar plating to ensure screws do not protrude into the dorsal extensor compartments.
Furthermore, Hanel et al. noted that dorsal distraction plates left in place for longer than 16 weeks had an overall complication rate of 21%, compared to 8.5% when removed earlier, primarily due to extensor tendon adhesions and hardware prominence.
SURGICAL TECHNIQUE: AVOIDING COMPLICATIONS
Proper surgical technique is the primary defense against complications. The frequency of complications has been shown to decrease inversely with increased surgeon experience.
Patient Positioning and Setup
- Positioning: The patient is placed supine with the operative arm extended on a radiolucent hand table.
- Tourniquet: A well-padded pneumatic tourniquet is applied to the proximal arm and inflated to 250 mmHg (or 100 mmHg above systolic pressure) after exsanguination.
- Fluoroscopy: The C-arm is positioned parallel to the table, entering from the head or the contralateral side, allowing for unobstructed AP, lateral, and tangential views.
The Modified Henry Approach (Volar)
- Incision: A longitudinal incision is made over the flexor carpi radialis (FCR) tendon, extending proximally from the wrist crease.
- Superficial Dissection: The FCR tendon sheath is incised. The tendon is retracted ulnarly. Crucial Step: Ulnar retraction of the FCR protects the palmar cutaneous branch of the median nerve, which lies in the subcutaneous tissue ulnar to the FCR.
- Deep Dissection: The floor of the FCR sheath is incised to access the deep compartment. The radial artery is identified and gently retracted radially.
- Pronator Quadratus Elevation: The pronator quadratus (PQ) muscle is identified. An L-shaped incision is made along its radial and distal borders. The PQ is elevated subperiosteally from radial to ulnar, exposing the fracture site.
- Reduction and Fixation: The fracture is reduced using manual traction, volar translation, and provisional K-wires. The volar locking plate is applied.
Fragment-Specific Fixation
In cases of severe intraarticular comminution where a single volar plate cannot capture all articular fragments (e.g., a free dorsal ulnar die-punch fragment), fragment-specific fixation is indicated.
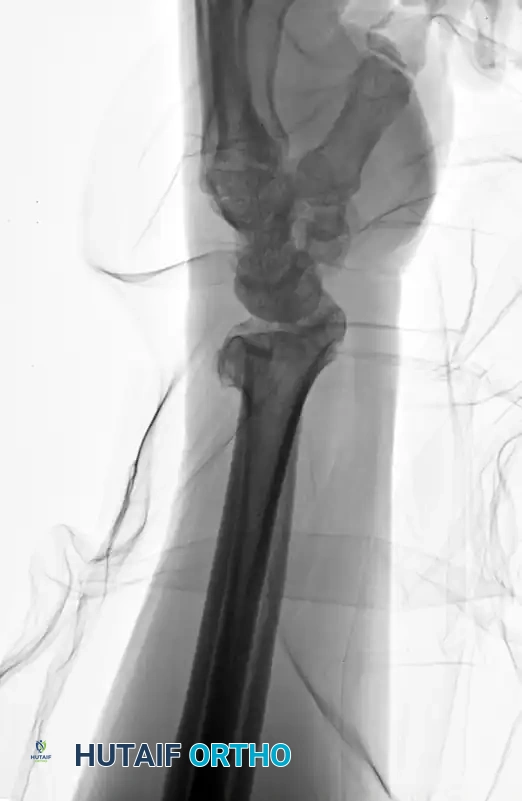
Preoperative AP radiograph demonstrating a highly comminuted, unstable distal radius fracture.
Preoperative Lateral radiograph highlighting severe dorsal comminution and loss of volar tilt.
Fragment-specific systems utilize low-profile, wire-form plates and small-fragment screws to independently address the radial column, intermediate column, and ulnar corner. This modular approach allows for rigid osteosynthesis of complex fracture patterns while minimizing the bulk of a single large implant.
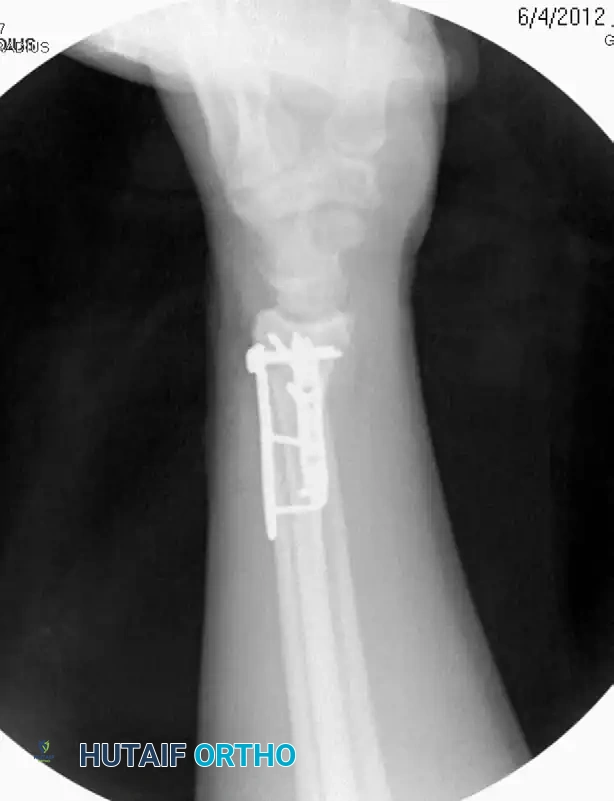
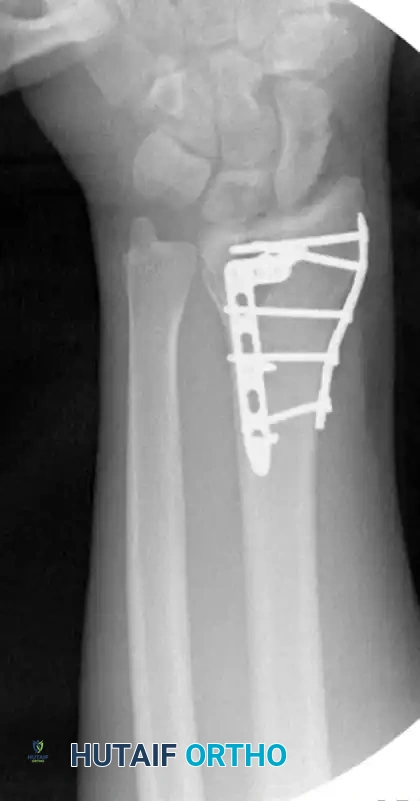
Postoperative AP radiograph demonstrating anatomic restoration of radial height and inclination utilizing fragment-specific fixation.
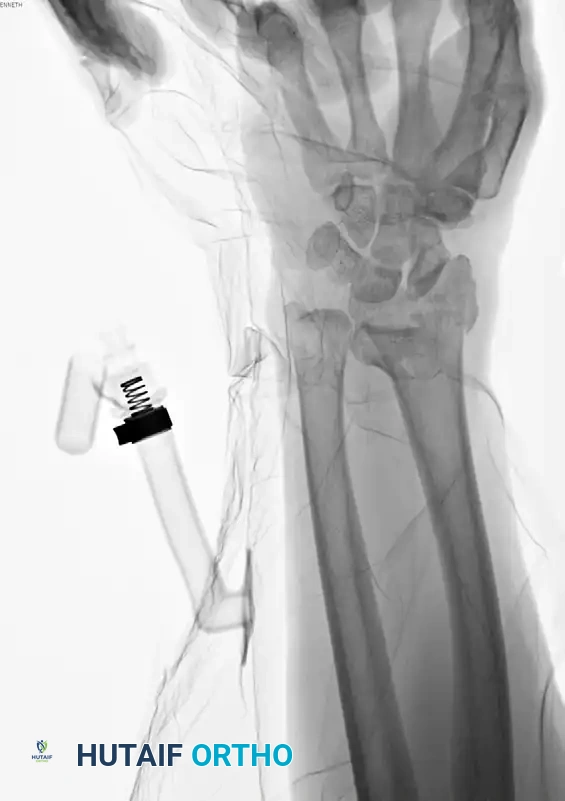
Postoperative Lateral radiograph confirming restoration of volar tilt and congruent radiocarpal articulation.
NEUROLOGICAL COMPLICATIONS
Nerve injuries complicate up to 17% of distal radius fractures. The median nerve is the most frequently injured due to its close proximity to the fracture site and its rigid confinement within the carpal canal.
Acute vs. Delayed Carpal Tunnel Syndrome (CTS)
- Acute CTS: Occurs immediately following high-energy, severely comminuted fractures. It is driven by acute hematoma, fracture displacement into the canal, or massive soft tissue swelling. Management: Requires immediate surgical decompression (carpal tunnel release) alongside fracture stabilization.
- Delayed Median Neuropathy: Presents weeks to months post-injury. It is associated with malunion, residual palmar displacement of fracture fragments, nerve impingement by exuberant callus formation, or prolonged immobilization in extreme positions.
- Prevention: Immobilization with the wrist in excessive flexion (the historical Cotton-Loder position of >20 degrees flexion) and extreme ulnar deviation must be strictly avoided, as this exponentially increases carpal tunnel pressure and compromises median nerve microcirculation.
Injury to the radial sensory nerve and ulnar nerve is less common (0% to 10%) but can occur iatrogenically during percutaneous pinning or external fixation pin placement.
COMPLEX REGIONAL PAIN SYNDROME (CRPS)
CRPS (formerly Reflex Sympathetic Dystrophy) is a devastating complication characterized by disproportionate pain, hyperalgesia, sudomotor changes (edema, sweating), and trophic skin changes. It occurs most commonly in elderly patients and those with underlying psychological or psychiatric conditions, with reported rates ranging from 8% to 35%.
Prophylaxis and Management
A landmark randomized, controlled, multicenter study involving 416 patients determined that prophylactic administration of Vitamin C (500 mg daily for 50 days) significantly reduces the prevalence of CRPS following distal radius fractures.
Evidence-Based Guideline: The American Academy of Orthopaedic Surgeons (AAOS) clinical practice guidelines for distal radial fractures list Vitamin C prophylaxis as having "adequate evidence to support a moderately strong endorsement."
If CRPS develops, early recognition is critical. Management requires a multidisciplinary approach including aggressive hand therapy (stress loading protocols), neuropathic pain modulators (gabapentin, pregabalin), and potentially sympathetic nerve blocks.
COMPARTMENT SYNDROME
Compartment syndrome of the forearm or hand associated with distal radial fractures is rare, occurring in approximately 1% of patients. It is primarily seen in younger patients subjected to high-energy crush injuries or severe polytrauma.
Diagnosis is primarily clinical, characterized by pain out of proportion to the injury, pain with passive stretch of the digits, and tense, woody compartments. If compartment pressures exceed 30 mmHg or are within 30 mmHg of the diastolic blood pressure (ΔP < 30), emergent volar and dorsal fasciotomies are mandated to prevent irreversible ischemic contracture (Volkmann's contracture).
POSTOPERATIVE PROTOCOLS AND REHABILITATION
The ultimate goal of distal radius fracture management is the restoration of painless, functional range of motion. Postoperative protocols must balance the need for fracture stability with the prevention of soft tissue adhesions.
- Phase I (0-2 Weeks): The wrist is immobilized in a bulky dressing or a removable volar splint. Immediate active range of motion (AROM) of the fingers, thumb, elbow, and shoulder is initiated to prevent stiffness and reduce edema.
- Phase II (2-6 Weeks): Suture removal occurs at 10-14 days. If rigid internal fixation was achieved, the patient may begin gentle, therapist-directed AROM of the wrist (flexion, extension, pronation, supination). Splinting is continued between exercise sessions.
- Phase III (6-12 Weeks): Radiographic union is typically evident. Passive range of motion (PROM) and progressive strengthening exercises are introduced. Return to heavy manual labor or contact sports is generally restricted until 12 weeks postoperatively.
By adhering to strict biomechanical principles, utilizing appropriate surgical approaches, and maintaining vigilance for early signs of complications, orthopedic surgeons can navigate the complexities of distal radius fractures and ensure optimal functional recovery for their patients.
You Might Also Like