Anterior Flap Hemipelvectomy: A Masterclass in Oncologic Reconstruction
Key Takeaway
Welcome to an advanced surgical masterclass on anterior flap hemipelvectomy. We'll meticulously navigate this complex oncologic procedure, designed for extensive posterior pelvic and buttock sarcomas. This guide covers detailed anatomy, precise intraoperative execution, critical pearls to avoid pitfalls, and comprehensive postoperative management, ensuring optimal patient outcomes and reconstructive success using the robust anterior myocutaneous thigh flap.
Introduction and Epidemiology
The anterior flap hemipelvectomy represents a critical evolution in orthopedic oncology, serving as a highly modified version of the classic posterior flap hemipelvectomy. Historically, standard hemipelvectomy relied on a posterior skin and fasciocutaneous flap harvested from the gluteal region to close the massive pelvic defect following amputation through the sacroiliac joint and pubic symphysis. However, this classic approach is oncologically contraindicated when managing extensive soft tissue sarcomas of the buttock or primary bone sarcomas of the pelvis with significant posterior extension, as the posterior flap tissues are either directly involved or contaminated by the tumor.
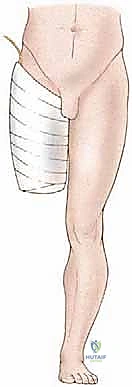
The anterior flap hemipelvectomy resolves this limitation by utilizing a massive, robust myocutaneous flap harvested from the anterior thigh—specifically the quadriceps musculature and overlying integument—pedicled on the superficial femoral vessels. This modification permits the radical en bloc resection of the entire gluteal region, posterior hemipelvis, and involved sciatic nerve, offering a potentially curative surgical option for tumors previously deemed unresectable.
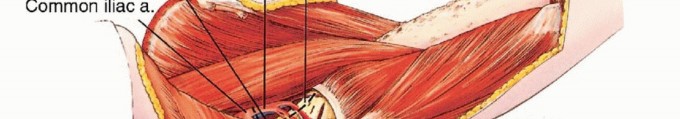
From an epidemiological perspective, pelvic sarcomas present a formidable challenge. Primary bone sarcomas of the pelvis, including chondrosarcoma, osteosarcoma, and Ewing sarcoma, account for approximately ten to fifteen percent of all primary malignant bone tumors. Chondrosarcoma is the most prevalent in adult populations, frequently arising from the periacetabular region or the iliac wing, and is notoriously resistant to both chemotherapy and radiation therapy. Consequently, achieving wide, negative surgical margins (R0 resection) remains the absolute strongest predictor of overall survival and local recurrence-free survival.
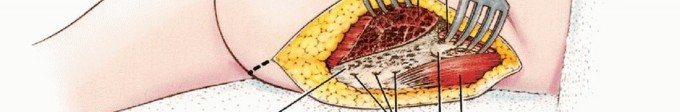
While the modern era of orthopedic oncology heavily favors limb-sparing internal hemipelvectomy, limb salvage is not universally applicable. Tumors that exhibit massive extraosseous extension into the sciatic notch, encase the sciatic nerve, or involve the major pelvic neurovascular bundles preclude functional limb preservation. In these advanced scenarios, external hemipelvectomy is mandated. When the posterior gluteal tissues are compromised by tumor extension, radiation changes, or previous biopsy tracts, the anterior flap hemipelvectomy becomes the definitive oncologic procedure of choice.
Procedure Overview and Oncologic Advantages
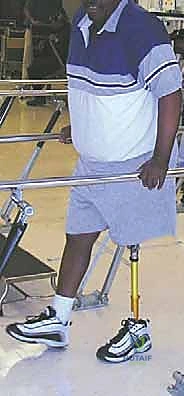
The primary oncologic advantage of the anterior flap hemipelvectomy is the ability to sacrifice the entire buttock compartment, including the gluteal muscles, sciatic nerve, sacrospinous ligaments, sacral alar, and all overlying posterior skin to the midline. The resulting massive posterior defect is obliterated by rotating the anterior myocutaneous flap posteriorly. Because the flap encompasses a large portion of the anterior thigh compartment, it provides a highly vascularized, bulky tissue mass ideal for dead-space management, coverage of exposed viscera, and the creation of a durable, well-padded stump that facilitates future prosthetic fitting. Furthermore, the robust vascularity of the quadriceps flap demonstrates excellent tolerance to postoperative radiation therapy, minimizing the risk of wound dehiscence or ischemic necrosis frequently associated with heavily irradiated traditional flaps.
Surgical Anatomy and Vascular Biomechanics
A profound understanding of the pelvic and lower extremity vascular tree is mandatory for the successful execution of an anterior flap hemipelvectomy. The procedure hinges on the preservation of the anterior vascular pedicle while systematically dismantling the posterior and intrapelvic attachments.
Key Vascular Structures and the Flap Pedicle
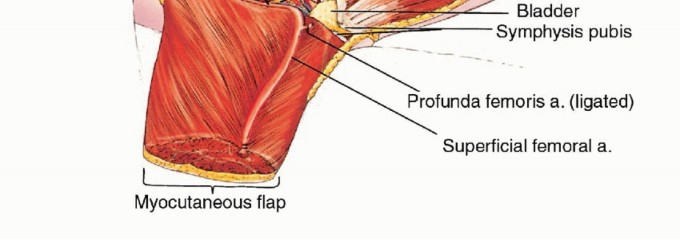
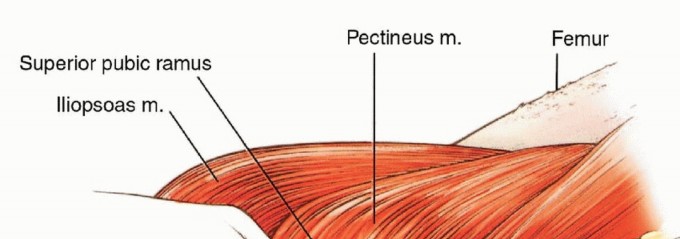
The external iliac vessels exit the pelvis beneath the inguinal ligament to become the common femoral vessels within the femoral triangle. The critical branch in this region is the profunda femoris artery, which arises from the posterolateral aspect of the common femoral artery and dives deep to supply the posterior thigh.
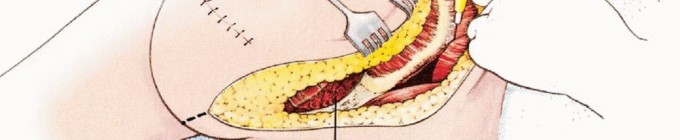
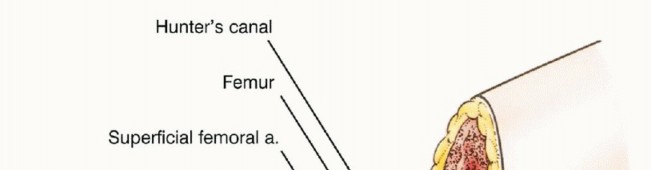
To mobilize the anterior myocutaneous flap, the profunda femoris artery and vein must be meticulously identified, ligated, and divided near their origin. The common femoral and superficial femoral vessels (SFA) must be strictly preserved, as they form the primary vascular pedicle for the flap. The SFA travels deep to the sartorius muscle and enters the adductor canal (Hunter's canal). At the level of the adductor hiatus, the SFA is ligated and divided distally, preventing exsanguination from the amputated extremity while maintaining retrograde and perforator flow to the quadriceps.
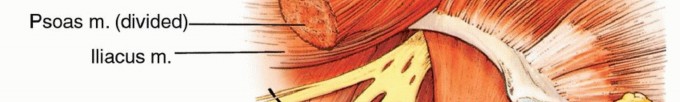
Muscular Vascular Supply
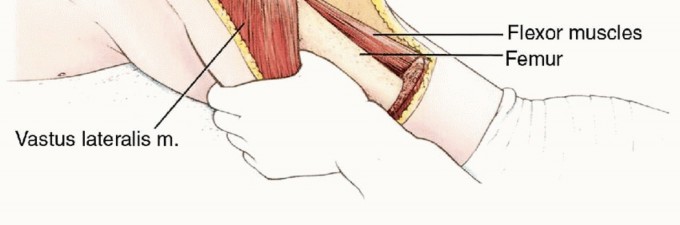
The quadriceps femoris group, the sartorius, and the adductor musculature derive their blood supply from perforating branches of the SFA. Specifically, perforating branches that pass through the intramuscular septum must be carefully managed. The entire anterior and medial muscular compartments of the thigh are elevated en bloc. The descending branch of the lateral femoral circumflex artery (a branch of the profunda) often provides significant supply to the vastus lateralis; therefore, its origin must be evaluated during profunda ligation. In many cases, the flap relies heavily on the muscular branches originating directly from the SFA and retrograde flow through the genicular anastomoses if the distal SFA is ligated low enough.
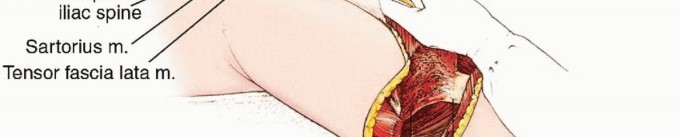
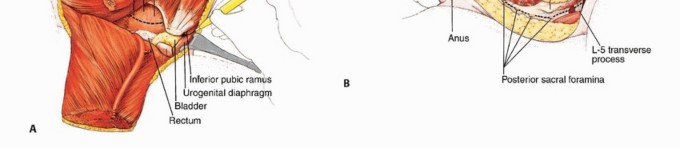
Osteology and Ligamentous Anatomy
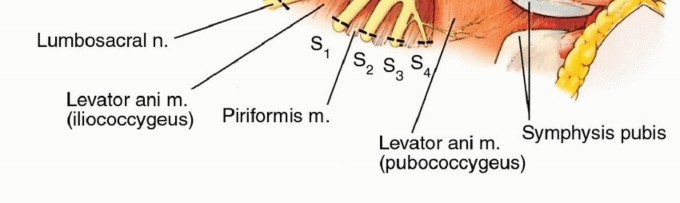
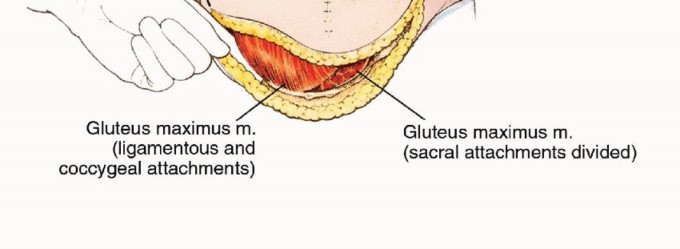
The bony resections required for a classic hemipelvectomy occur at the pubic symphysis anteriorly and the sacroiliac joint posteriorly. However, depending on tumor extent, an extended hemipelvectomy may require an osteotomy through the sacral ala or even the neural foramina. The ligamentous structures stabilizing the hemipelvis—namely the anterior and posterior sacroiliac ligaments, the sacrotuberous ligament, and the sacrospinous ligament—must be systematically divided. The sacrotuberous and sacrospinous ligaments are critical landmarks during the posterior dissection, as the pudendal neurovascular bundle and the sciatic nerve exit the greater and lesser sciatic foramina in close proximity to these structures.
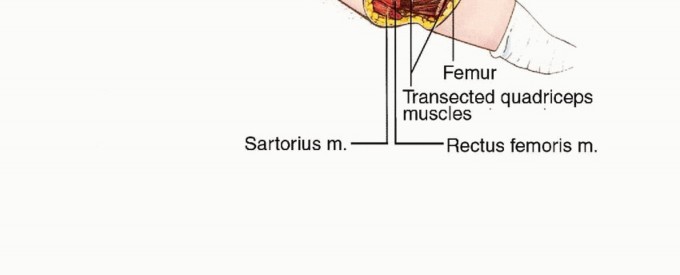
Biomechanics of the Postoperative Pelvis
The biomechanical consequences of a hemipelvectomy are profound. The functional loss of the hemipelvis disrupts the transmission of axial loads from the spine to the lower extremity. Furthermore, the loss of the ischial tuberosity drastically alters seated biomechanics. The remaining hemipelvis and the sacrum must bear the entirety of the patient's seated weight. The massive bulk of the anterior quadriceps flap is biomechanically essential in this regard; it provides a vital cushion over the exposed sacrum and abdominal viscera, preventing pressure ulceration and supporting the structural integrity of the pelvic floor, which is entirely lost on the amputated side.
Indications and Contraindications
The decision to proceed with an anterior flap hemipelvectomy is highly complex and must be made within the context of a multidisciplinary tumor board. The primary goal is oncologic clearance; functional considerations, while important, are secondary to achieving negative margins in high-grade sarcomas.
Oncologic Indications
The classic indication for an anterior flap hemipelvectomy is a massive primary bone sarcoma (e.g., osteosarcoma, Ewing sarcoma, chondrosarcoma) of the ilium or periacetabular region that exhibits massive posterior extraosseous extension into the gluteal musculature, thereby precluding the use of a standard posterior gluteal flap. Additionally, massive high-grade soft tissue sarcomas of the buttock that invade the sciatic notch or involve the proximal posterior thigh are prime indications.
Palliative indications also exist. In cases of fungating, bleeding, or severely painful recurrent tumors of the posterior pelvis where systemic therapy has failed, an anterior flap hemipelvectomy may be performed to achieve local control, eliminate the source of sepsis or hemorrhage, and improve the patient's remaining quality of life.
Contraindications
Absolute contraindications primarily relate to tumor involvement of the anterior compartment. If the tumor extends anteriorly to involve the quadriceps musculature, the overlying anterior skin, or encases the superficial femoral vessels, the anterior flap cannot be utilized safely. In such cases, alternative and highly complex closures, such as free tissue transfer (e.g., latissimus dorsi free flap) combined with a modified amputation, must be considered.
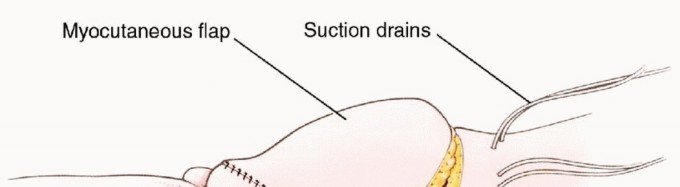
Severe peripheral vascular disease represents a relative, and sometimes absolute, contraindication. If the superficial femoral artery is occluded or severely stenotic, the viability of the anterior flap is compromised. Preoperative vascular imaging is non-negotiable in this patient population.
Summary of Operative Considerations
| Clinical Scenario | Recommended Approach | Rationale |
|---|---|---|
| Posterior Pelvic Sarcoma (Gluteal involvement) | Anterior Flap Hemipelvectomy | Classic posterior flap is oncologically contaminated. Anterior flap provides safe margins and bulk. |
| Anterior Pelvic Sarcoma (Quadriceps/SFA involvement) | Posterior Flap Hemipelvectomy | Anterior flap is contaminated. Standard posterior gluteal flap provides coverage. |
| Massive Tumor involving both Anterior and Posterior Compartments | Hemipelvectomy with Free Flap Coverage | Neither local flap is viable. Requires radical resection and microvascular free tissue transfer (e.g., Latissimus). |
| Iliac Wing Tumor (No sciatic nerve/joint involvement) | Internal Hemipelvectomy (Limb Salvage) | Limb can be preserved if neurovascular bundle and sciatic nerve are free of tumor. |
| Fungating/Bleeding Posterior Pelvic Tumor (Palliative) | Anterior Flap Hemipelvectomy | Removes necrotic burden, controls hemorrhage, provides durable soft tissue coverage for palliation. |
Pre Operative Planning and Patient Positioning
Thorough preoperative planning is the cornerstone of a successful anterior flap hemipelvectomy. The surgical team must possess a precise three-dimensional understanding of the tumor's relationship to the pelvic viscera, the major vascular structures, and the bony pelvis.
Advanced Imaging Protocols
Magnetic Resonance Imaging (MRI) of the entire pelvis and the affected lower extremity is mandatory. T1-weighted, T2-weighted, and post-contrast sequences are utilized to delineate the intraosseous and extraosseous extent of the tumor. The relationship of the tumor mass to the sciatic nerve, the lumbosacral plexus, and the intrapelvic organs (bladder, rectum) must be explicitly mapped.

Computed Tomography Angiography (CTA) is equally critical. The CTA serves a dual purpose: first, it confirms the patency and caliber of the superficial femoral artery and vein, ensuring the anterior flap will be viable; second, it maps the pelvic vascular tree, allowing the surgeon to plan the ligation of the internal iliac vessels and identify any aberrant vascular anatomy (e.g., corona mortis). In highly vascular tumors, preoperative angiographic embolization of the internal iliac artery or specific tumor feeding vessels may be performed 24 to 48 hours prior to surgery to minimize intraoperative blood loss.
Multidisciplinary Optimization
Patients undergoing hemipelvectomy require extensive physiological and psychological optimization. A thorough cardiac and pulmonary evaluation is required given the massive fluid shifts and potential for significant blood loss. Preoperative stoma siting by a wound, ostomy, and continence nurse (WOCN) is advised, even if a bowel or bladder resection is not explicitly planned, as intraoperative findings may necessitate visceral resection. Psychological counseling is imperative to prepare the patient for the profound alteration in body image and functional independence.
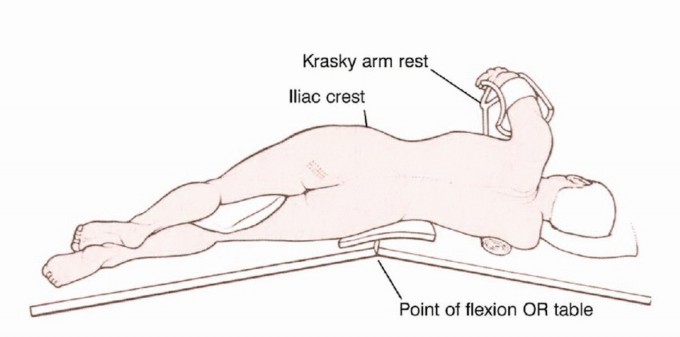
Patient Positioning and Preparation
The patient is typically positioned in a "floppy" lateral decubitus position on a radiolucent operating table. The affected side is elevated to approximately 45 to 60 degrees using a vacuum beanbag. This specific positioning is critical as it allows simultaneous access to the anterior abdomen, the groin, the anterior thigh, and the posterior gluteal and sacral regions without the need for intraoperative repositioning.
A Foley catheter is placed to decompress the bladder and monitor urine output. Wide surgical preparation is performed, extending from the costal margin down to the toes of the affected extremity, and crossing the midline anteriorly and posteriorly. The entire limb is draped free to allow for full manipulation during the osteotomies and flap elevation.
Detailed Surgical Approach and Technique
The surgical execution of an anterior flap hemipelvectomy is a massive, multi-staged undertaking that requires meticulous hemostasis and strict adherence to oncologic planes.
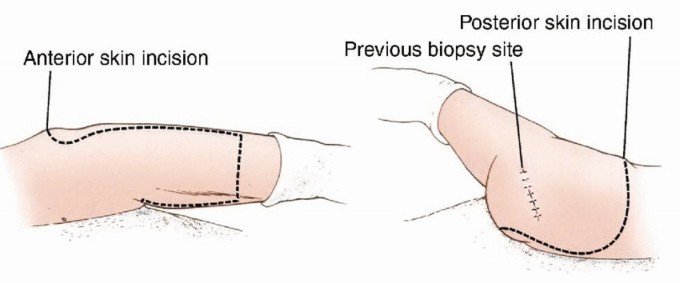
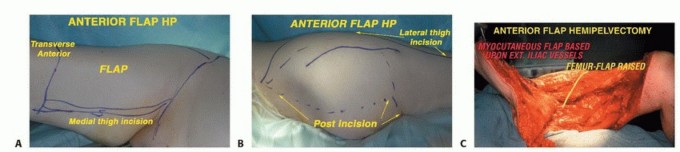
Incision and Flap Design
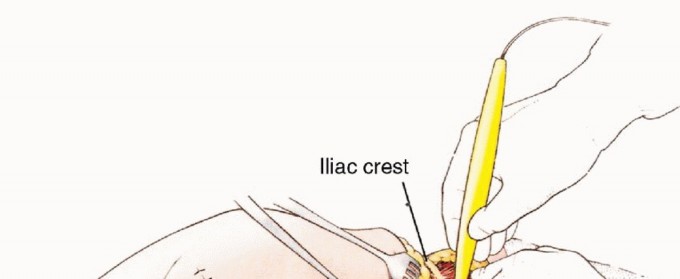
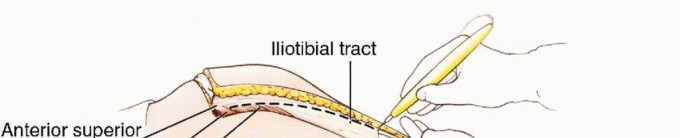
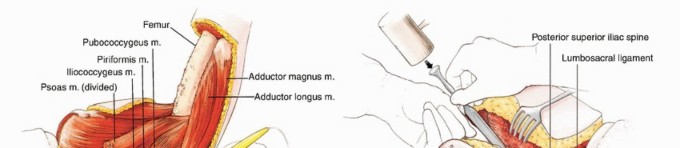
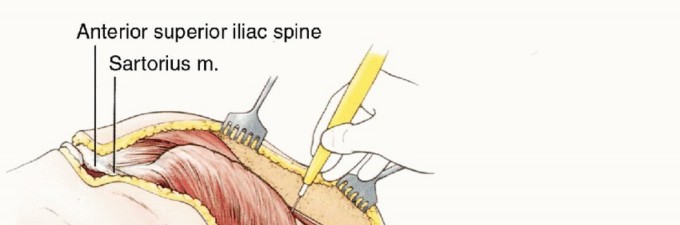
The incision is designed as a massive racket shape. The anterior limb of the incision begins just superior to the anterior superior iliac spine (ASIS), courses medially parallel to the inguinal ligament toward the pubic tubercle, and then extends distally down the anteromedial aspect of the thigh over the course of the superficial femoral vessels. The posterior limb drops from the ASIS, courses posteriorly over the iliac crest, and swoops down to encompass the entire gluteal region, ensuring wide margins around any posterior tumor extension.
Anterior Dissection and Vascular Control
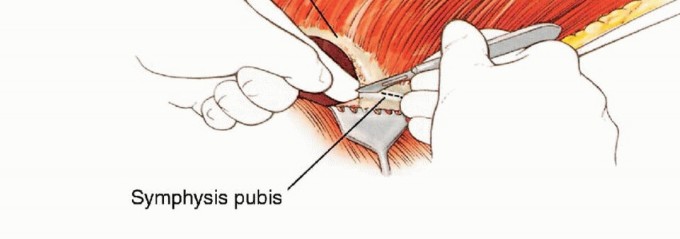
The initial phase of the operation focuses on securing the vascular pedicle. The anterior incision is deepened through the subcutaneous tissues to expose the femoral triangle. The inguinal ligament is identified and can be divided to provide proximal control of the external iliac vessels.
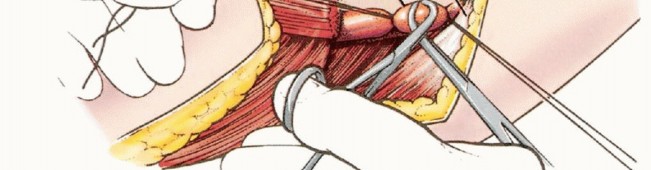
The femoral nerve is identified and divided high in the retroperitoneum or at the level of the inguinal ligament. The common femoral artery and vein are meticulously skeletonized. The dissection proceeds distally to identify the bifurcation of the common femoral artery into the superficial femoral artery (SFA) and the profunda femoris artery.

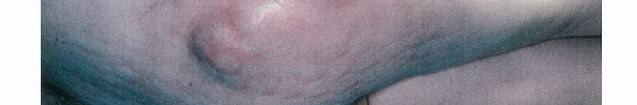
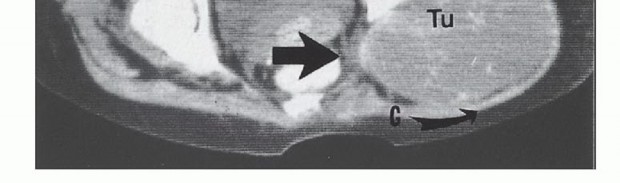




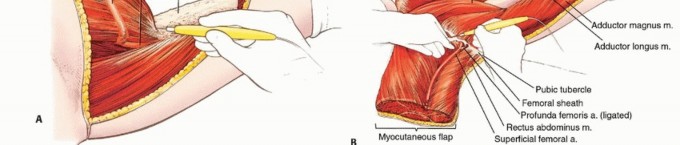

You Might Also Like