Complex Calcaneal Fracture: Clinical Presentation, Advanced Imaging & Sanders IIIBC Classification Case Study
Key Takeaway
A Sanders Type IIIBC calcaneal fracture is a severe intra-articular heel bone fracture with extensive comminution, often resulting from high-energy axial loads. Diagnosis involves detailed clinical examination for swelling, ecchymosis, and pain, complemented by plain X-rays (evaluating Bohler's/Gissane's angles) and definitive CT scans to classify articular involvement and guide surgical planning.
Patient Presentation and History
A 38-year-old male, previously fit and healthy, presented to the emergency department following a 10-foot fall from a ladder onto both feet. He immediately experienced severe bilateral heel pain, rendering him unable to bear weight. The mechanism of injury was a direct axial load through the lower extremities.
His medical history was unremarkable, with no known comorbidities such as diabetes, peripheral vascular disease, or osteopenia, which are crucial considerations in fracture healing and surgical planning. He is an active smoker, consuming approximately 15 pack-years. Social history includes employment as a construction worker, highlighting the significant functional implications of lower extremity injury. There were no reported allergies and he was not on any regular medications.
Upon initial assessment, specific inquiry was made regarding other potential injuries, especially those associated with high-energy axial loading. This included symptoms referable to the lumbar spine, which is crucial given the incidence of concomitant spinal fractures (up to 10-15% in calcaneal fractures), as well as injuries to the talus, pilon, or contralateral foot. The patient denied any back pain, loss of sensation, or motor weakness.
Mechanism of Injury and Biomechanics
The biomechanics of this injury pattern involve a high-energy axial load where the body weight is driven downward while the ground reaction force is transmitted upward through the heel. In this scenario, the lateral process of the talus acts as a wedge, driving into the crucial angle of Gissane of the calcaneus. This sheer force typically creates a primary fracture line extending from the proximal-medial aspect to the distal-lateral aspect of the calcaneus, dividing the bone into an anteromedial fragment (the "constant" fragment, which remains attached to the talus via the strong interosseous talocalcaneal and deltoid ligaments) and a posterolateral fragment (the tuberosity).
The secondary fracture lines dictate the specific fracture pattern, such as joint depression or tongue-type configurations, depending on the position of the foot (dorsiflexion versus plantarflexion) at the moment of impact. The energy dissipation through the cancellous bone of the calcaneal body results in significant comminution, loss of calcaneal height, increase in calcaneal width, and varus deformity of the tuberosity due to the unresisted pull of the Achilles tendon and the medial orientation of the sustentaculum tali.
Demographics and Comorbidities
While the patient lacks systemic metabolic conditions like diabetes or osteopenia, his 15 pack-year smoking history is a critical prognostic factor. Nicotine induces vasoconstriction, increases platelet aggregation, and decreases cellular oxygenation due to carbon monoxide competitive binding with hemoglobin. In the context of calcaneal fractures, smoking significantly increases the risk of devastating postoperative wound complications, including marginal flap necrosis, deep infection, and subsequent osteomyelitis. Studies, notably the landmark trial by Buckley et al., have demonstrated that smokers with displaced intra-articular calcaneal fractures often have poorer outcomes following operative intervention compared to non-smokers, making the decision to proceed with open reduction and internal fixation (ORIF) highly nuanced in this demographic.
Occupational and Social History
The patient's occupation as a construction worker necessitates prolonged standing, walking on uneven surfaces, and heavy lifting. A malunited calcaneal fracture resulting in loss of calcaneal height, increased heel width, subtalar arthritis, and subfibular impingement would severely compromise his ability to return to his previous level of employment. This occupational demand strongly weighs in favor of anatomical restoration of the subtalar joint and calcaneal morphology, despite the elevated soft tissue risks associated with his smoking status.
Clinical Examination Findings
Initial examination revealed significant swelling and ecchymosis extending from the hindfoot into the midfoot bilaterally, more pronounced on the left. The skin over both heels, particularly the lateral aspects, appeared tense and shiny, raising concerns for impending fracture blisters and soft tissue compromise. Mondor's sign (hematoma extending to the sole of the foot) was present on the left. No open wounds were observed, and there were no signs of gross deformity, though the normal calcaneal contour was lost due to swelling.
Palpation elicited exquisite tenderness over the calcaneal tuberosity and along the lateral aspect of both calcanei. Crepitus was present on gentle manipulation of the left hindfoot. The Achilles tendon was intact bilaterally, and the integrity of the fibula, tibia, and talus was assessed by careful palpation to rule out associated fractures.
Gross range of motion of the ankle and subtalar joint was severely limited due to pain and swelling, preventing a precise assessment. Both feet were held in a position of slight dorsiflexion due to muscle spasm.
Neurological assessment revealed intact sensation in the distribution of the sural, superficial peroneal, deep peroneal, tibial, and saphenous nerves bilaterally. Motor function of the ankle dorsiflexors, plantarflexors, invertors, and evertors was limited by pain but appeared grossly intact when resisted. Distal pulses (dorsalis pedis and posterior tibial) were strong and symmetric bilaterally, and capillary refill was prompt. Compartment pressures were not overtly elevated, but the presence of significant swelling mandated close monitoring for potential compartment syndrome, particularly in the midfoot. Close attention was paid to the skin integrity, noting areas of blanching with pressure, indicative of potential flap compromise if an immediate surgical approach were contemplated.
Soft Tissue Inspection and Compartment Evaluation
The presence of Mondor's sign—a plantar ecchymosis extending along the plantar fascia—is pathognomonic for a calcaneal fracture and indicates significant deep hematoma tracking along fascial planes. The tense, shiny skin on the lateral hindfoot indicates severe interstitial edema. The "wrinkle test" was negative on the left side, meaning the skin could not be pinched into fine wrinkles, signifying that the swelling had exceeded the elastic capacity of the dermis. Proceeding with an extensile lateral approach in the presence of a negative wrinkle test carries an unacceptably high risk of postoperative wound dehiscence.
Compartment syndrome of the foot, while less common than in the leg, is a limb-threatening complication associated with high-energy crush injuries and calcaneal fractures. The foot contains nine distinct fascial compartments (medial, lateral, superficial, adductor, four interosseous, and the calcaneal compartment). The calcaneal compartment, containing the quadratus plantae muscle, is particularly vulnerable in this injury pattern. While overt signs of compartment syndrome (pain out of proportion, pain with passive stretch of the toes) were absent, the threshold for intracompartmental pressure monitoring must remain low during the initial observation period.
Palpation and Structural Assessment
Loss of calcaneal height and increased calcaneal width are the clinical hallmarks of a displaced intra-articular calcaneal fracture. The lateral displacement of the tuberosity and the lateral wall blowout often lead to subfibular impingement, where the peroneal tendons become compressed between the lateral malleolus and the widened calcaneal lateral wall. Palpation inferior to the lateral malleolus elicited severe pain, consistent with this lateral wall expansion. The Achilles tendon was palpated to ensure continuity, as avulsion fractures of the calcaneal tuberosity can occasionally masquerade as standard intra-articular fractures but require entirely different, often emergent, surgical management to prevent posterior skin necrosis.
Neurological and Vascular Integrity
A meticulous neurological examination is paramount, specifically evaluating the sural nerve and the posterior tibial nerve. The sural nerve courses posterior to the lateral malleolus and is at risk from the initial trauma, the lateral wall blowout, and subsequent surgical approaches. The posterior tibial nerve, coursing through the tarsal tunnel on the medial aspect, can be tethered or compressed by the medial displacement of the sustentaculum tali or extensive medial hematoma. Baseline documentation of intact two-point discrimination in these nerve distributions is essential for postoperative comparison. Vascular integrity, confirmed by palpable dorsalis pedis and posterior tibial pulses, ensures adequate perfusion, though microvascular compromise to the lateral calcaneal angiosome remains a primary concern due to the patient's smoking history and injury-induced edema.
Imaging and Diagnostics
Initial imaging commenced with plain radiographs of both feet and ankles, and a focused lumbar spine series to exclude associated injuries.
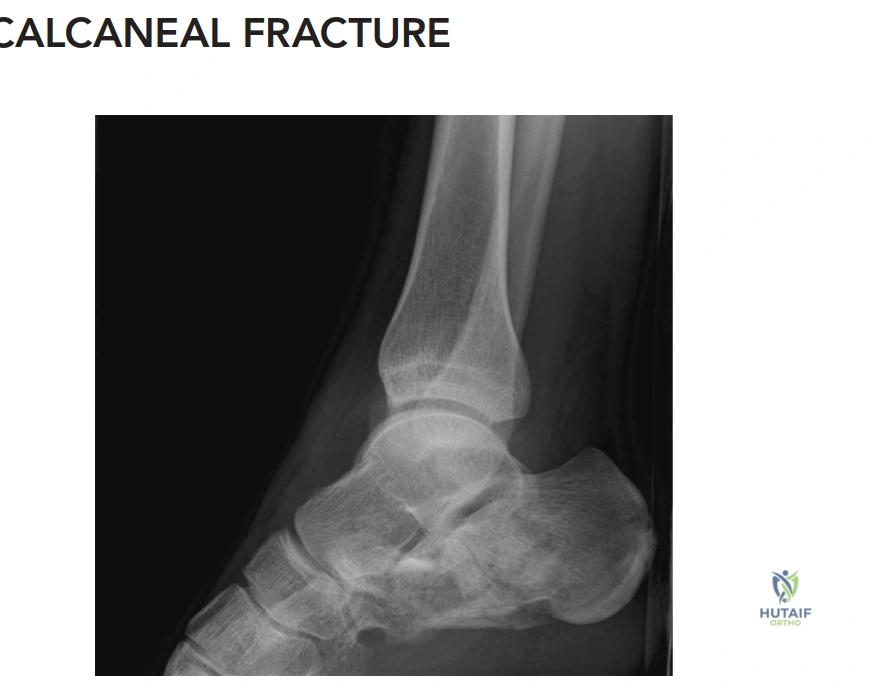
X-ray Findings (Left Calcaneus):
* Lateral View: Demonstrated a significant decrease in Bohler's angle (measured at 5 degrees, normal 20-40 degrees), indicative of substantial collapse of the posterior facet and loss of calcaneal height. Gissane's angle (Crucial angle) was increased to 140 degrees (normal 100-120 degrees), reflecting the disruption of the lateral process of the talus and the primary fracture line. There was clear evidence of a tongue-type fracture pattern with extension into the subtalar joint. Loss of calcaneal length and significant posterior facet depression were also evident.
* Axial (Harris) View: Revealed significant lateral wall blowout, increased heel width, and varus angulation of the calcaneal tuberosity. The primary fracture line separating the sustentacular fragment from the tuberosity was visible, confirming the intra-articular nature of the injury.
Standard Radiographic Evaluation
In addition to the lateral and Harris axial views, an anteroposterior (AP) view of the foot is necessary to evaluate the calcaneocuboid joint for anterior process extension, which occurs in approximately 60% of intra-articular calcaneal fractures. Broden's views were also obtained. These are specialized radiographs taken with the leg internally rotated 40 degrees and the x-ray beam angled cephalad at 10, 20, 30, and 40 degrees. Broden's views are historically utilized to visualize the posterior facet of the subtalar joint from posterior to anterior, aiding in the assessment of articular congruity. While largely supplanted by computed tomography (CT) for preoperative planning, Broden's views remain highly valuable for intraoperative fluoroscopic assessment of posterior facet reduction.
Advanced Computed Tomography Analysis
Computed Tomography (CT) without contrast is the gold standard for evaluating calcaneal fractures, providing a three-dimensional understanding of the fracture morphology, articular comminution, and fragment displacement. Fine cuts (1-2 mm) in the axial, coronal, and sagittal planes are mandatory.
- Coronal Plane: Essential for evaluating the posterior facet of the subtalar joint. This plane allows for the application of the Sanders classification system. It clearly demonstrates the number of articular fragments, the location of the fracture lines relative to the posterior facet, the degree of articular step-off, and the medial-lateral widening of the calcaneus.
- Axial Plane: Optimal for assessing the calcaneocuboid joint involvement, the degree of lateral wall blowout, and the integrity of the sustentaculum tali. It also visualizes the primary fracture line extending from posteromedial to anterolateral.
- Sagittal Plane: Best for evaluating the loss of calcaneal height, the depression of the posterior facet into the cancellous body, and the overall length of the calcaneus. It clearly differentiates between joint depression and tongue-type fracture patterns based on the exit point of the secondary fracture line.

The CT analysis of the left calcaneus revealed a highly comminuted posterior facet. The coronal cuts demonstrated three distinct articular fragments with fracture lines located centrally and laterally within the posterior facet, consistent with a Sanders Type IIIBC classification. The sagittal cuts confirmed a tongue-type variant where the secondary fracture line exited posteriorly through the tuberosity, rather than superiorly just behind the posterior facet (which would indicate a joint depression type). Significant comminution of the anterior process with extension into the calcaneocuboid joint was also noted.
Preoperative Templating and Planning
Preoperative templating involves utilizing the CT data to plan the surgical approach, reduction sequence, and fixation construct. In this Sanders IIIBC pattern, the presence of a central articular fragment (the "B" fragment) requires meticulous elevation and provisional fixation to the medial "constant" sustentacular fragment before addressing the lateral "C" fragment. The templating process dictates the need for a low-profile, anatomically contoured perimeter plate to buttress the lateral wall and support the elevated posterior facet. The length of the screws required to capture the sustentaculum tali from the lateral cortex is estimated using the axial CT cuts, ensuring adequate purchase in the dense bone of the constant fragment without penetrating the medial soft tissues and endangering the neurovascular bundle.
Differential Diagnosis
When evaluating high-energy axial load injuries to the hindfoot, a comprehensive differential diagnosis is essential to ensure no concomitant or alternative injuries are overlooked. The clinical presentation of severe heel pain, swelling, and inability to bear weight is shared among several distinct pathologies.
Diagnostic Considerations in Axial Load Injuries
| Diagnosis | Mechanism of Injury | Key Clinical Findings | Radiographic Hallmark |
|---|---|---|---|
| Intra-articular Calcaneal Fracture | Axial load (fall from height, MVC). Talar lateral process acts as a wedge. | Severe heel pain, widened heel, decreased height, Mondor's sign, varus tuberosity. | Decreased Bohler's angle, increased Gissane's angle, posterior facet disruption on CT. |
| Talar Body/Neck Fracture | Hyperdorsiflexion with axial load. | Deep ankle/hindfoot pain, profound swelling, potential skin tenting (talar neck). | Disruption of talar contours, subtalar/tibiotalar incongruity, Hawkin's sign (prognostic). |
| Tibial Pilon Fracture | High-energy axial load driving the talus into the distal tibial plafond. | Distal leg swelling, gross ankle instability, severe soft tissue compromise, fracture blisters. | Distal tibial metaphyseal comminution with intra-articular extension into the ankle joint. |
| Extra-articular Calcaneal Fracture | Twisting, avulsion (Achilles), or direct direct blow. | Localized tenderness (e.g., anterior process, tuberosity), less severe overall hindfoot swelling. | Intact posterior facet. Fracture lines isolated to tuberosity, anterior process, or medial process. |
| Subtalar Dislocation | High-energy inversion or eversion stress. | Gross deformity of the hindfoot (medial or lateral shift), skin tenting, locked joint. | Disruption of the talocalcaneal and talonavicular joints with preserved tibiotalar alignment. |
In this clinical scenario, the presence of a widened heel, decreased calcaneal height, and profound localized tenderness over the lateral calcaneus strongly pointed toward a calcaneal fracture. The definitive diagnosis and differentiation from extra-articular variants or talar injuries were confirmed via the comprehensive radiographic and CT evaluation, which clearly delineated the intra-articular Sanders IIIBC pattern.
Surgical Decision Making and Classification
The management of displaced intra-articular calcaneal fractures remains one of the most debated topics in orthopedic trauma. The decision to proceed with operative versus non-operative management requires a careful balancing of the functional benefits of anatomical restoration against the significant risks of soft tissue complications.
Sanders Classification System
The Sanders classification is the most widely utilized and prognostically relevant system for intra-articular calcaneal fractures. It is based on the coronal CT cuts at the widest point of the posterior facet of the talus. The posterior facet is divided into three potential fracture lines (A, B, and C), creating four potential articular pieces (lateral, central, medial, and sustentacular).
- Type I: Non-displaced articular fractures (regardless of the number of fracture lines).
- Type II: Two-part articular fractures (one fracture line). Subdivided into IIA, IIB, IIC based on the location of the primary line.
- Type III: Three-part articular fractures (two fracture lines) with a centrally depressed fragment. Subdivided into IIIAB, IIIAC, and IIIBC.
- Type IV: Four-part or highly comminuted articular fractures.
Our patient presents with a Sanders Type IIIBC fracture. This indicates two fracture lines through the posterior facet: one located centrally (B) and one located laterally (C), resulting in three distinct articular fragments. This is a highly complex pattern. The central fragment is often deeply impacted into the cancellous body of the calcaneus, requiring significant manipulation for elevation and reduction. The prognosis for Type III fractures is inherently worse than Type II, with a higher incidence of post-traumatic subtalar arthritis regardless of the quality of surgical reduction.
Essex Lopresti Classification
While the Sanders system guides operative planning based on articular comminution, the Essex-Lopresti classification, based on lateral radiographs or sagittal CT cuts, describes the overall fracture morphology and the exit point of the secondary fracture line.
- Joint Depression Type: The secondary fracture line exits superiorly, just posterior to the posterior facet. The tuberosity fragment remains separate from the posterior facet.
- Tongue Type: The secondary fracture line exits posteriorly through the calcaneal tuberosity. The posterior facet remains attached to the posterior tuberosity fragment.
Our patient exhibits a tongue-type variant. This distinction is critical for reduction maneuvers. In a tongue-type fracture, the entire posterior facet and tuberosity unit can often be manipulated via a Schanz pin placed percutaneously into the posterior tuberosity (the Essex-Lopresti maneuver). Plantarflexion of the pin elevates the posterior facet, while varus/valgus manipulation corrects the coronal alignment.
Indications for Operative Intervention
The primary goals of operative intervention are to restore calcaneal height, length, and width, correct varus deformity of the tuberosity, decompress the subfibular space, and anatomically reduce the posterior facet of the subtalar joint.
Absolute indications for surgery include open fractures and fractures with severe soft tissue compromise threatening skin viability (e.g., severe tongue-type fractures tenting the posterior skin). Relative indications, which apply to this patient, include displaced intra-articular fractures in young, active individuals.
The decision-making process in this specific case is complicated by the patient's smoking history. The Buckley trial (JBJS 2002), a landmark prospective randomized controlled trial comparing operative versus non-operative management of calcaneal fractures, demonstrated that while young, healthy, non-workers' compensation patients had significantly better outcomes with surgery, patients who smoked or were receiving workers' compensation had outcomes that were not significantly different from, or were worse than, those managed non-operatively. Furthermore, smokers had a drastically higher rate of wound complications.
However, given the patient's age (38), occupation (construction worker requiring prolonged weight-bearing and agility), and the severe displacement of the Sanders IIIBC pattern, non-operative management would almost certainly result in a severe malunion. This malunion would manifest as a shortened, widened heel with profound subfibular impingement, obligate varus gait, and rapid-onset post-traumatic subtalar arthritis, likely necessitating a complex corrective subtalar arthrodesis with bone block distraction in the future.
Therefore, after extensive counseling regarding the elevated risks of wound necrosis, infection, and potential need for subsequent soft tissue coverage procedures (including free tissue transfer), the decision was made to proceed with Open Reduction and Internal Fixation (ORIF). To mitigate the soft tissue risk, surgery must be delayed until the swelling has completely subsided and the "wrinkle test" is positive, typically 10 to 21 days post-injury.
Surgical Technique and Intervention
The surgical execution for a Sanders IIIBC calcaneal fracture demands meticulous preoperative planning, precise soft tissue handling, and a rigid adherence to a sequential reduction strategy. Given the patient's smoking history, the viability of the lateral soft tissue flap is the paramount concern throughout the procedure.
Patient Positioning and Setup
The patient is positioned in the lateral decubitus position on a radiolucent Jackson table, with the operative extremity facing upward. All bony prominences are meticulously padded to prevent iatrogenic nerve palsies. A pneumatic tourniquet is applied to the proximal thigh. The contralateral leg is flexed at the hip and knee to allow for unobstructed lateral fluoroscopic imaging. The fluoroscopy machine (C-arm) is positioned to enter from the anterior aspect of the patient, allowing for seamless transition between lateral, axial (Harris), and Broden's views without requiring repositioning of the limb. A bump is placed under the operative leg to ensure it is parallel to the floor, facilitating accurate intraoperative radiographic assessment.
Surgical Approach and Soft Tissue Handling
An extensile lateral approach is utilized. This approach provides unparalleled visualization of the lateral wall, posterior facet, and calcaneocuboid joint. The incision is meticulously planned to respect the vascular angiosomes of the hindfoot, specifically the lateral calcaneal artery, a terminal branch of the peroneal artery.
The incision begins 2-3 cm proximal to the tip of the lateral malleolus, just anterior to the Achilles tendon. It extends distally in a straight line to the junction of the plantar and lateral skin (glabrous line), then curves gently anteriorly toward the base of the fifth metatarsal.
A strict "no-touch" technique is employed for the soft tissue flap. The incision is carried sharply down to bone in a single sweep, avoiding any subcutaneous undermining or creation of split-thickness planes. A full-thickness subperiosteal flap is elevated, encompassing the skin, subcutaneous tissue, sural nerve, and peroneal tendons. The flap is elevated off the lateral wall of the calcaneus, exposing the subtalar joint and the calcaneocuboid joint.
To retract the flap without causing crush injury to the microvasculature, self-retaining retractors are strictly avoided. Instead, three 1.6 mm Kirschner wires (K-wires) are driven into the lateral talus, the talar neck, and the cuboid. The full-thickness flap is then gently retracted superiorly and held in place by bending the K-wires over the soft tissue. This technique eliminates continuous point pressure on the flap edges, significantly reducing the risk of postoperative marginal necrosis.
Fracture Reduction Sequence
The reduction of a highly comminuted Sanders IIIBC fracture must follow a logical, step-wise progression, working from the known (the constant fragment) to the unknown (the displaced lateral fragments).
- Tuberosity Reduction: A 5.0 mm Schanz pin is inserted percutaneously from posterior to anterior into the dense bone of the calcaneal tuberosity fragment. Using this pin as a joystick, axial traction is applied to restore calcaneal length. The tuberosity is then translated medially and rotated out of varus to restore the mechanical axis of the hindfoot. Once length and alignment are restored, the tuberosity is provisionally pinned to the constant sustentacular fragment using a heavy (2.0 mm) K-wire directed from the posterolateral tuberosity into the anteromedial sustentaculum tali.
- Posterior Facet Elevation: With the tuberosity reduced, attention is turned to the subtalar joint. In a Sanders IIIBC pattern, the central "B" fragment is often deeply impacted into the cancellous void. A periosteal elevator or a Freer is used to gently disimpact and elevate the central and lateral articular fragments. The articular surface is reconstructed from medial to lateral, using the intact medial facet of the talus as a template.
- Provisional Articular Fixation: Once the posterior facet is anatomically reduced, it is provisionally held with subchondral K-wires directed from lateral to medial, capturing the sustentacular fragment. Intraoperative Broden's views and lateral fluoroscopy are utilized to confirm articular congruity and the restoration of Bohler's angle.
- Lateral Wall Reduction: The lateral wall blowout is reduced, decompressing the subfibular space. The lateral wall fragments are often highly comminuted and act as a cortical shell over the cancellous void created by the elevation of the posterior facet.
Internal Fixation Construct
Following provisional reduction, definitive fixation is achieved utilizing a low-profile, anatomically contoured calcaneal perimeter plate. The primary biomechanical goal of the plate is to act as a lateral buttress, maintaining the restored calcaneal height, length, and neutral alignment of the tuberosity, while supporting the elevated posterior facet.
The plate is positioned over the lateral wall. Strategic screw placement is critical.
* Sustentacular Screws: The most critical screws are placed through the plate, just inferior to the posterior facet, directed from lateral to medial into the dense bone of the sustentaculum tali. These screws (typically 3.5 mm cortical or locking screws) secure the lateral construct to the constant medial fragment. Absolute care must be taken to ensure these screws are of appropriate length; over-penetration medially can tether the flexor hallucis longus (FHL) tendon or injure the posterior tibial neurovascular bundle.
* Tuberosity Screws: Screws are placed into the posterior tuberosity to maintain the correction of varus and length.
* Anterior Process Screws: Screws are directed into the anterior process, extending toward the calcaneocuboid joint, to complete the perimeter fixation.
* Subchondral Support: Additional lag screws may be placed outside the plate, directly through the subchondral bone of the posterior facet, to provide absolute stability to the articular reduction.
Given the significant cancellous void created by the elevation of the depressed articular fragments, the use of bone graft or bone graft substitutes (e.g., calcium phosphate cement or cancellous allograft) is often debated. While structural support can be beneficial, studies have shown that rigid perimeter plating alone is often sufficient to
