Thoracolumbar Spine Injuries: A Comprehensive Guide to Diagnosis, Surgical Anatomy, & Management Decisions
Key Takeaway
Surgical intervention for thoracolumbar spine injuries is typically indicated for unstable fractures requiring decompression of neural elements, restoration of spinal alignment, and stable fixation. Key factors include fracture morphology, neurological status, and especially disruption of the posterior ligamentous complex (PLC), which signifies mechanical instability predisposing to neurological deterioration and progressive kyphosis.
Introduction and Epidemiology
Thoracolumbar spine injuries represent a significant and often complex challenge in orthopedic trauma, necessitating a nuanced understanding of their pathology, biomechanics, and clinical implications. These injuries typically involve the segments from T11 to L2, a transitional zone that experiences considerable biomechanical stress due to its kyphotic-to-lordotic transition and changes in rib cage support. The potential for catastrophic neurological deficits, long-term pain, and functional impairment underscores the critical importance of accurate diagnosis and appropriate management.
Epidemiologically, thoracolumbar spine injuries disproportionately affect young, active males, with high-energy trauma being the predominant etiology. Motor vehicle accidents account for the majority of cases, followed by falls from height, sports injuries, and acts of violence. The incidence of these injuries varies globally but remains a leading cause of spinal cord injury. Approximately 50 to 60 percent of all spinal fractures occur in the thoracolumbar region.
Classification systems provide standardized frameworks for describing fracture morphology, assessing stability, and guiding treatment decisions. While historically the focus was on bony integrity, contemporary understanding emphasizes the critical role of the posterior ligamentous complex in spinal stability. The central dilemma in managing these injuries revolves around distinguishing between stable injuries amenable to non-operative treatment and unstable injuries requiring surgical stabilization or decompression to prevent neurological deterioration, correct deformity, and facilitate rehabilitation. This distinction is paramount and forms the cornerstone of effective patient care.
Pathophysiology of Thoracolumbar Trauma
The pathophysiology of thoracolumbar trauma is dictated by the mechanism of energy transfer. Axial loading typically results in burst fractures, where the intervertebral disc is driven into the vertebral body, causing centrifugal failure of the endplate and retropulsion of bone fragments into the spinal canal. Flexion-distraction injuries, classically associated with lap-belt use in motor vehicle collisions, create tension across the posterior and middle columns, leading to bony or ligamentous failure (Chance fractures). Fracture-dislocations involve complex multi-planar forces, including shear, rotation, and translation, invariably resulting in severe instability and a high incidence of complete neurological deficits.
Secondary injury mechanisms begin immediately following the initial mechanical insult. Ischemia, excitotoxicity, lipid peroxidation, and the inflammatory cascade exacerbate spinal cord damage. This highlights the urgency of restoring spinal alignment and decompressing the neural elements in the setting of incomplete neurological deficits to mitigate secondary cord injury.
Surgical Anatomy and Biomechanics
A thorough understanding of the surgical anatomy and biomechanics of the thoracolumbar spine is fundamental for any surgeon managing these complex injuries. The thoracolumbar junction (T10-L2) is a zone of transition from the rigid thoracic spine, supported by the rib cage, to the more mobile lumbar spine. This area is subjected to significant stress and is thus highly susceptible to injury.
Osteology and Transition Zone Dynamics
Anatomically, each vertebral segment comprises an anterior vertebral body, posterior vertebral arch (pedicles, laminae, transverse and spinous processes), and articular processes forming the facet joints. The spinal canal houses the spinal cord, which typically terminates as the conus medullaris between T12 and L2, transitioning to the cauda equina inferiorly. The precise level of the conus is clinically critical, as injuries above this level can result in upper motor neuron lesions, while those below affect lower motor neurons.
The facet joints transition from a coronal orientation in the thoracic spine (limiting flexion-extension but allowing rotation) to a sagittal orientation in the lumbar spine (allowing flexion-extension but restricting rotation). This abrupt change in facet morphometry at the thoracolumbar junction concentrates torsional and shear forces, predisposing this specific region to failure under high-energy loading.
Ligamentous Stability and Vascular Supply
Crucial to spinal stability are the robust ligamentous structures:
* Anterior Longitudinal Ligament: Resists extension.
* Posterior Longitudinal Ligament: Resists flexion and prevents disc herniation posteriorly.
* Ligamentum Flavum: Connects adjacent laminae, contributing to elastic recoil.
* Interspinous and Supraspinous Ligaments: Resisted flexion and rotation, forming the primary components of the Posterior Ligamentous Complex.
* Facet Joint Capsules: Provide stability and guide motion.
The vascular supply to the spinal cord derives from the paired segmental arteries, with the critical artery of Adamkiewicz (typically arising between T9-L2 on the left side) supplying the anterior spinal artery in the thoracolumbar region. Injury to this vessel during anterior approaches or via massive trauma can lead to devastating anterior cord syndrome, characterized by bilateral loss of motor function and pain/temperature sensation with preserved dorsal column function.
Biomechanical Classification Models
Biomechanically, the Denis Three-Column Theory remains a foundational concept for understanding spinal stability:
1. Anterior Column: Anterior Longitudinal Ligament, anterior two-thirds of the vertebral body and annulus fibrosus.
2. Middle Column: Posterior Longitudinal Ligament, posterior one-third of the vertebral body, and posterior annulus fibrosus.
3. Posterior Column: Posterior bony arch (pedicles, facets, laminae, spinous processes) and the Posterior Ligamentous Complex.
According to Denis, disruption of two or more columns indicates biomechanical instability. While foundational, modern practice relies heavily on the Thoracolumbar Injury Classification and Severity Score and the AOSpine Thoracolumbar Spine Injury Classification System.

The Load-Sharing Classification (McCormack) is also critical for surgical decision-making, particularly when determining if a short-segment posterior construct will fail. It evaluates the amount of damaged vertebral body, the spread of the fragments, and the degree of kyphosis correction. A high score (greater than 6) suggests a high risk of anterior column failure with short-segment posterior-only fixation, indicating the need for an anterior column reconstruction or long-segment posterior fixation.
Indications and Contraindications
The decision to proceed with surgical intervention in thoracolumbar trauma requires a synthesis of fracture morphology, neurological status, and patient-specific physiological factors. The primary goals of surgery are to decompress neural elements, restore spinal alignment, achieve mechanical stability, and facilitate early mobilization.
Clinical Decision Making Frameworks
The Thoracolumbar Injury Classification and Severity Score provides a validated, point-based system to guide operative versus non-operative management. It assesses three categories: injury morphology, integrity of the Posterior Ligamentous Complex, and neurological status. A score of 3 or less typically warrants non-operative management, a score of 5 or more is a strong indication for surgery, and a score of 4 represents an equivocal zone where surgeon preference and patient factors dictate management.
The AOSpine classification further refines this by categorizing injuries into Type A (compression), Type B (tension band disruption), and Type C (translation or displacement), combined with patient-specific modifiers and neurological grading. Type B and C injuries universally require surgical stabilization due to inherent multi-planar instability.
| Parameter | Operative Indications | Non Operative Indications |
|---|---|---|
| Neurological Status | Progressive neurological deficit, incomplete cord syndrome, cauda equina syndrome | Neurologically intact, complete cord injury (relative depending on stability) |
| Biomechanics | Disrupted Posterior Ligamentous Complex, translation or shear injury, >30 degrees kyphosis, >50% loss of vertebral height | Intact Posterior Ligamentous Complex, isolated anterior column compression, stable burst fractures |
| TLICS Score | Score > 4 | Score < 4 |
| AOSpine Class | Type B (tension band failure), Type C (translation) | Type A1, A2, A3 (without neuro deficit or severe kyphosis) |
| Polytrauma | Need for early mobilization to manage pulmonary or systemic injuries | Isolated injury amenable to bracing and early ambulation |
Contraindications to surgery are generally relative and primarily involve severe patient comorbidities that preclude general anesthesia, profound hemodynamic instability (damage control orthopedics may dictate delayed definitive fixation), or active systemic infection. In cases of complete spinal cord injury (ASIA A) present for greater than 48-72 hours, the indication for decompression is debated, though stabilization for nursing care and rehabilitation remains a valid indication.
Pre Operative Planning and Patient Positioning
Meticulous preoperative planning is essential for optimizing outcomes and minimizing intraoperative complications. This begins with a comprehensive primary and secondary survey adhering to Advanced Trauma Life Support protocols, recognizing that thoracolumbar fractures are frequently associated with concomitant intra-abdominal, pulmonary, and closed head injuries.
Advanced Imaging Modalities
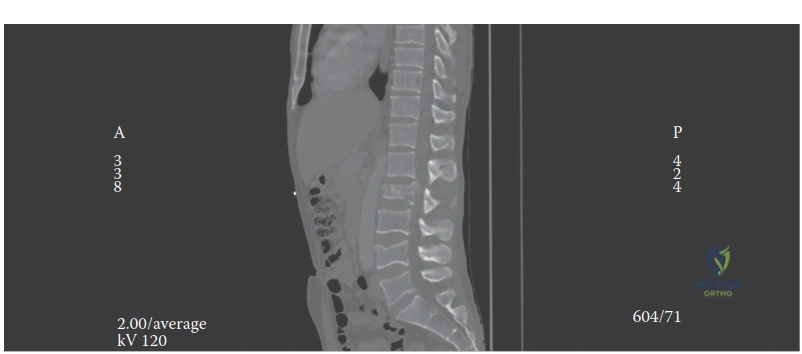
Standard anteroposterior and lateral radiographs provide an initial assessment of alignment and gross fracture morphology. However, thin-slice computed tomography with sagittal and coronal reconstructions is the gold standard for defining bony anatomy, facet subluxation, and the extent of canal compromise.
Magnetic Resonance Imaging is indispensable for evaluating the integrity of the Posterior Ligamentous Complex, intervertebral discs, and the spinal cord itself. Short Tau Inversion Recovery sequences are particularly sensitive for detecting ligamentous edema and epidural hematomas. MRI is strictly indicated in any patient with a neurological deficit, suspected tension-band injury not clearly visible on CT, or when the TLICS score is equivocal.
Neuromonitoring and Operating Room Setup
Intraoperative neuromonitoring, utilizing Somatosensory Evoked Potentials and Motor Evoked Potentials, is highly recommended during the surgical management of thoracolumbar trauma, particularly during reduction maneuvers and instrumentation. Baseline signals should be obtained prior to positioning.
Patient positioning is critical. For posterior approaches, the patient is placed prone on a radiolucent Jackson spinal table. This table allows the abdomen to hang free, decreasing intra-abdominal pressure and thereby reducing epidural venous engorgement and intraoperative blood loss. The Jackson table also facilitates postural reduction of burst fractures through the application of extension forces. Care must be taken to pad all bony prominences to prevent pressure necrosis and to ensure the eyes are free from pressure to avoid ischemic optic neuropathy.
Detailed Surgical Approach and Technique
The choice of surgical approach—posterior, anterior, or combined—depends on the fracture morphology, the location of neural compression, and the surgeon's expertise. Posterior approaches are the workhorse of thoracolumbar trauma due to their familiarity, versatility, and lower morbidity compared to open anterior approaches.
Posterior Midline Approach and Decompression
The standard posterior midline approach involves a longitudinal incision centered over the fractured vertebra, extending proximally and distally to incorporate the planned instrumented levels. Subperiosteal dissection of the paraspinal musculature is performed laterally to the tips of the transverse processes in the thoracic spine and the lateral aspect of the pars interarticularis in the lumbar spine. Meticulous hemostasis is maintained using bipolar electrocautery.
Decompression is indicated for patients with incomplete neurological deficits and anterior canal compromise. While direct anterior decompression via a corpectomy is biomechanically ideal for massive anterior retropulsion, a transpedicular decompression or costotransversectomy can be performed from a posterior approach. This involves resecting the pedicle of the fractured level to access the anterior epidural space, allowing the surgeon to tamp retropulsed bone fragments anteriorly away from the thecal sac using specialized reverse-angle curettes.
Pedicle Screw Instrumentation Principles
Pedicle screw fixation provides rigid three-column control. The entry point for thoracic pedicle screws is generally at the intersection of the bisected transverse process and the lateral margin of the superior articular facet. In the lumbar spine, the entry point is at the intersection of the pars interarticularis, the midpoint of the transverse process, and the lateral border of the superior articular process.
Preparation of the pedicle involves a burr or awl to breach the cortex, followed by a pedicle probe to navigate the cancellous channel into the vertebral body. The trajectory must respect the sagittal and axial angulation of the specific vertebral level. The integrity of the pedicle walls is confirmed using a ball-tipped feeler probe (sounding the pedicle) to ensure no medial, lateral, superior, or inferior breaches have occurred.
Following screw placement, rods are contoured to restore physiological sagittal alignment. Reduction of kyphotic deformity can be achieved through cantilever forces applied to the rods, compression across the posterior elements (in the setting of an intact anterior column), or ligamentotaxis. Ligamentotaxis relies on an intact posterior longitudinal ligament to pull retropulsed bone fragments out of the canal when distraction forces are applied across the pedicle screws.
Anterior Thoracoabdominal Approaches
Anterior approaches are indicated for severe burst fractures with significant canal compromise and incomplete neurological deficits that cannot be adequately addressed posteriorly, or for cases requiring extensive anterior column reconstruction (Load-Sharing Score > 6).
The approach typically involves a left-sided thoracotomy or thoracoabdominal incision, depending on the level. The diaphragm may need to be incised circumferentially at its peripheral attachment to access the thoracolumbar junction. Segmental vessels are ligated at the mid-vertebral body level to mobilize the great vessels and preserve collateral blood supply to the spinal cord. A corpectomy is performed by excising the adjacent discs and the fractured vertebral body, followed by reconstruction using an expandable titanium cage or structural allograft, supplemented by an anterior plate or dual-rod system.
Minimally Invasive Surgical Techniques
Minimally invasive surgery for thoracolumbar trauma is gaining traction, particularly for neurologically intact patients with unstable fractures (e.g., flexion-distraction injuries or Type B fractures). Percutaneous pedicle screw fixation utilizes fluoroscopy or intraoperative navigation to place hardware through small stab incisions, minimizing paraspinal muscle crush injury, reducing blood loss, and accelerating postoperative recovery. However, MIS techniques offer limited ability for direct decompression and rely heavily on postural reduction.
Complications and Management
Surgical management of thoracolumbar injuries carries a substantial risk profile. Complications can be categorized into intraoperative events, early postoperative issues, and late-onset failures. Anticipation and prompt management are critical for mitigating long-term morbidity.
Intraoperative and Postoperative Challenges
Incidental durotomies (dural tears) occur frequently, especially when decompressing highly comminuted burst fractures with sharp retropulsed fragments. Primary repair using 4-0 or 5-0 non-absorbable suture is the gold standard. If primary repair is impossible, augmented closure with muscle/fascia patches, dural substitutes, and fibrin sealants is utilized. A subfascial drain is generally avoided or placed to gravity rather than suction to prevent a continuous cerebrospinal fluid fistula.
Hardware malposition is a significant risk, particularly medial pedicle breaches which can injure the spinal cord or nerve roots. Intraoperative neuromonitoring alerts and intraoperative 3D fluoroscopy (O-arm) or navigation are essential tools to detect and revise malpositioned screws before leaving the operating room.
| Complication | Estimated Incidence | Prevention and Salvage Strategies |
|---|---|---|
| Pedicle Screw Malposition | 5% - 15% (Freehand) | Use intraoperative navigation or 3D fluoroscopy. Salvage: Immediate intraoperative revision; if delayed and symptomatic, return to OR for revision. |
| Incidental Durotomy | 3% - 10% | Meticulous dissection around retropulsed fragments. Salvage: Primary repair, dural sealants, bed rest for 48 hours post-op. |
| Surgical Site Infection | 2% - 8% | Preoperative antibiotics, copious irrigation, intrawound vancomycin powder. Salvage: Serial surgical debridement, targeted IV antibiotics, retention of hardware until fusion occurs. |
| Hardware Failure or Pullout | 1% - 5% | Avoid short-segment fixation in highly comminuted fractures (high Load-Sharing score). Salvage: Extension of fusion construct, addition of anterior column support. |
| Post Traumatic Kyphosis | 5% - 20% | Adequate anterior column reconstruction, robust posterior tension band restoration. Salvage: Corrective osteotomies (e.g., Pedicle Subtraction Osteotomy) and revision instrumentation. |
Late complications include pseudoarthrosis (failure of fusion) and adjacent segment disease. Pseudoarthrosis presents with recrudescent axial pain and hardware failure (rod fracture or screw loosening). Management requires revision surgery with decortication, robust bone grafting (autograft or biologics like rhBMP-2), and extension or reinforcement of the instrumentation construct.
Post Operative Rehabilitation Protocols
The immediate postoperative phase focuses on hemodynamic stability, pain control, and early mobilization. The traditional paradigm of prolonged bed rest has been universally abandoned due to the unacceptable rates of deep vein thrombosis, pulmonary embolism, atelectasis, and deconditioning.
Mobilization and Orthotic Management
Patients who have undergone rigid internal fixation are typically mobilized out of bed on postoperative day one. The use of a Thoracolumbosacral Orthosis following surgical stabilization is highly debated. Historically, a TLSO was routinely prescribed; however, modern pedicle screw constructs offer sufficient biomechanical rigidity that bracing is often unnecessary, serving primarily as a tactile reminder for the patient to avoid extreme bending or twisting. If a brace is utilized, it is generally worn when out of bed for 6 to 12 weeks.
Deep vein thrombosis prophylaxis is paramount. Mechanical prophylaxis (pneumatic compression devices) is initiated immediately. Chemical prophylaxis (e.g., Low Molecular Weight Heparin) is typically started 24 to 48 hours postoperatively, provided there is no evidence of expanding epidural hematoma or ongoing active bleeding.
Physical therapy focuses on transfers, ambulation, and isometric core strengthening. Active range of motion exercises for the spine are generally restricted until radiographic evidence of early bony union is observed, typically around the 8 to 12-week mark.
Summary of Key Literature and Guidelines
The management of thoracolumbar trauma has evolved significantly, driven by landmark clinical trials and the development of validated classification systems. Evidence-based practice requires familiarity with these foundational studies.
Landmark Studies in Thoracolumbar Trauma
The seminal work by Denis in 1983 established the three-column biomechanical model, which, despite its age, remains a conceptual cornerstone for understanding spinal stability. McCormack et al. introduced the Load-Sharing Classification in 1994, fundamentally changing how surgeons evaluate the necessity of anterior column support in burst fractures, thereby reducing the incidence of posterior hardware failure.
The shift toward standardized, reproducible treatment algorithms was solidified by Vaccaro et al. with the introduction of the Thoracolumbar Injury Classification and Severity Score in 2005. This system successfully integrated morphological, biomechanical, and neurological data into a single actionable score. Subsequently, the AOSpine Knowledge Forum Trauma, also led by Vaccaro and colleagues, published the AOSpine Thoracolumbar Spine Injury Classification System in 2013, which refined morphological descriptions and improved inter-observer reliability worldwide.
Regarding the operative versus non-operative debate for stable burst fractures, the randomized controlled trial by Wood et al. (Journal of Bone and Joint Surgery, 2003) is arguably the most influential. The study demonstrated that for neurologically intact patients with stable thoracolumbar burst fractures, there was no significant long-term difference in functional outcomes, pain, or return to work between those treated with surgical stabilization and those managed non-operatively with bracing. This study heavily influenced modern guidelines, cementing non-operative management as the standard of care for TLICS < 4 burst fractures without posterior ligamentous complex disruption.
Contemporary literature continues to explore the boundaries of minimally invasive surgery, the timing of decompression in spinal cord injury (e.g., the STASCIS trial emphasizing decompression within 24 hours for cervical trauma, principles of which are increasingly applied to the thoracolumbar spine), and the integration of artificial intelligence in fracture recognition and preoperative planning. Mastery of this evolving literature is essential for the academic orthopedic surgeon committed to delivering optimal care in thoracolumbar spine trauma.
