Spondylodiscitis: Deciphering the next course of action
Key Takeaway
Your ultimate guide to Spondylodiscitis: Deciphering the next course of action starts here. For spondylodiscitis without neurological deficits, epidural abscess, or gross deformity, and with positive blood cultures for methicillin-sensitive *S. aureus*, the next course of action involves infectious disease consultation to optimize antibiotic therapy. Vancomycin is unnecessary; a more appropriate antibiotic should be selected based on sensitivity. Surgical debridement and fusion are generally not indicated at this time.
Comprehensive Introduction and Patho-Epidemiology
Pyogenic spondylodiscitis represents a formidable challenge in the realm of orthopedic spine surgery, characterized by a concurrent infection of the intervertebral disc and the adjacent vertebral bodies. The incidence of this condition has seen a steady trajectory upward over the past two decades, largely driven by an aging population, an increasing prevalence of systemic comorbidities such as diabetes mellitus, expanding use of immunosuppressive therapies, and the rising rates of intravenous drug utilization. The clinical presentation is notoriously insidious, often leading to delayed diagnosis, significant morbidity, and, in severe cases, devastating neurological compromise or structural spinal collapse.
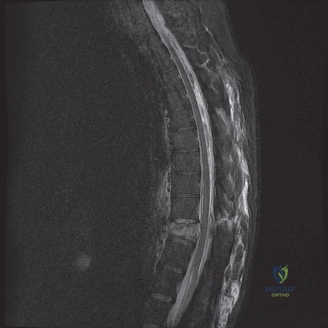
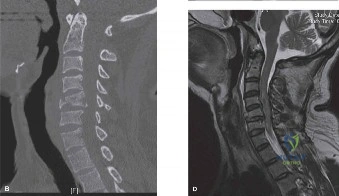
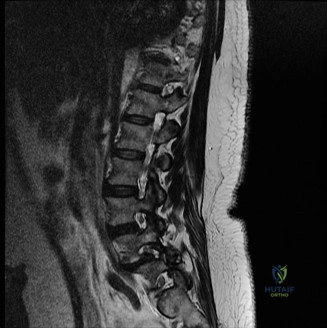
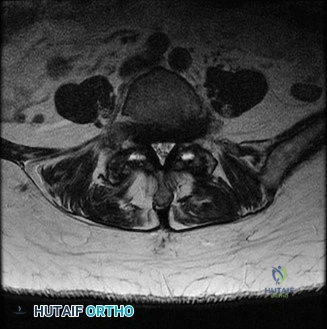
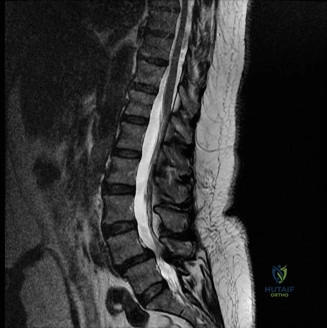
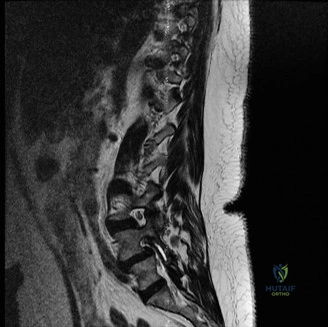
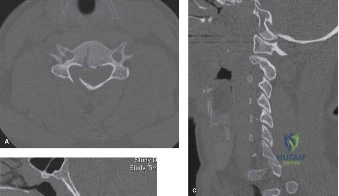
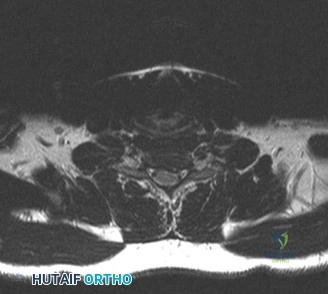
To contextualize the decision-making algorithm, consider the classic presentation of a middle-aged patient with multiple medical comorbidities. A paradigmatic case involves a 48-year-old obese female (Body Mass Index of 43) with poorly controlled diabetes mellitus who presents with severe, unrelenting low back pain, fevers, and chills. Advanced imaging, specifically magnetic resonance imaging (MRI), typically demonstrates discitis involving the L4–5 disc space with adjacent osteomyelitis of the L4 and L5 vertebral bodies. Crucially, in many early or medically responsive cases, there is an absence of epidural abscess formation, and standing radiographs reveal relatively normal sagittal and coronal alignment. When such a patient is neurologically intact—lacking saddle anesthesia, bowel/bladder incontinence, or upper motor neuron signs—the immediate clinical imperative shifts from urgent surgical decompression to aggressive pathogen identification and targeted antimicrobial therapy.
The pathogenesis of spondylodiscitis typically involves hematogenous dissemination of bacteria, though direct inoculation (e.g., post-procedural) and contiguous spread from adjacent soft tissue infections also occur. In the adult population, the subchondral endplate is the primary site of bacterial seeding due to the sluggish blood flow in the terminal arterial arcades. From the endplate, the infection rapidly breaches the avascular intervertebral disc, utilizing it as a nutrient-rich sanctuary shielded from the host immune response, before extending into the contiguous vertebral body.
Microbiologically, Staphylococcus aureus remains the undisputed dominant pathogen, accounting for over half of all cases. Blood cultures are an indispensable diagnostic tool and should be drawn immediately upon presentation, ideally before the initiation of empiric antibiotics. Blood cultures can identify the responsible organism in up to 85% of cases. If cultures return positive for methicillin-sensitive Staphylococcus aureus (MSSA), empiric broad-spectrum coverage such as vancomycin must be rapidly de-escalated to targeted therapy (e.g., cefazolin or nafcillin) to optimize bactericidal efficacy and minimize toxicity. The integration of an infectious disease consultation is paramount in these early stages to dictate the precise antimicrobial regimen, duration, and monitoring parameters.
Detailed Surgical Anatomy and Biomechanics
A profound understanding of the vascular anatomy and regional biomechanics of the lumbar spine is essential for comprehending both the pathophysiology of spondylodiscitis and the principles governing its surgical management. The arterial supply to the lumbar vertebrae arises from the paired segmental lumbar arteries, which branch from the abdominal aorta. These segmental arteries give rise to metaphyseal arteries that form extensive, tortuous capillary networks immediately adjacent to the cartilaginous endplates. In adults, the intervertebral disc is entirely avascular; the terminal arterial arcades end abruptly at the subchondral bone. This anatomical arrangement creates a low-flow hemodynamic environment that is highly conducive to bacterial lodging during transient bacteremic episodes.
Venous drainage of the spinal column is equally critical to the infectious process. Batson’s venous plexus is a complex, valveless network of epidural and paravertebral veins that communicates freely with the pelvic and abdominal venous systems. Because these veins lack valves, any physiological maneuver that increases intra-abdominal or intra-thoracic pressure (such as the Valsalva maneuver) can precipitate retrograde venous flow. This mechanism explains the frequent association between pelvic infections (e.g., urinary tract infections, prostatitis) and subsequent lumbar spondylodiscitis.
From a biomechanical perspective, the L4-L5 motion segment is subjected to some of the highest compressive and shear forces in the human body. The anterior column (comprising the anterior longitudinal ligament, anterior two-thirds of the vertebral body, and anterior annulus fibrosus) bears approximately 80% of the axial load in a healthy spine. When pyogenic osteomyelitis destroys the subchondral endplates and the intervening disc, the anterior column loses its structural integrity.
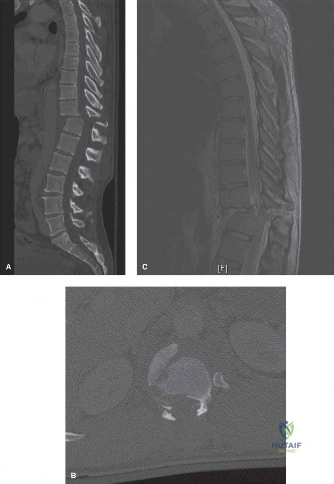
This structural compromise leads to pathological load transfer to the posterior elements (facets and pars interarticularis). As the anterior column collapses under the weight of the trunk, the spine inevitably drifts into a focal kyphotic deformity. This kyphosis not only alters global sagittal balance—requiring increased energy expenditure for standing and walking—but also narrows the neuroforamina and spinal canal, potentially compressing the exiting and traversing nerve roots. Therefore, any surgical intervention must not only eradicate the infectious nidus but also meticulously reconstruct the anterior weight-bearing column to restore physiological lordosis and biomechanical stability.
Exhaustive Indications and Contraindications
The management of spondylodiscitis requires a delicate balance between conservative antimicrobial therapy and aggressive surgical intervention. The default approach for a neurologically intact patient with stable spinal alignment and a known pathogen is non-operative. As demonstrated in our paradigmatic case of the 48-year-old diabetic female with MSSA bacteremia, the absence of neurological deficits, epidural abscess, or gross deformity dictates that medical management is the absolute next best step.
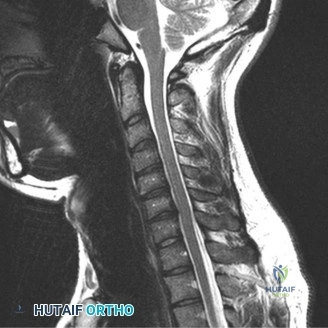
Surgical debridement and instrumented fusion are explicitly not indicated in the acute setting unless specific failure criteria are met. However, the surgeon must remain vigilant, as the clinical picture can deteriorate rapidly. The primary indications for surgical intervention include the development of a progressive neurological deficit, the presence of a symptomatic epidural abscess causing neural compression, progressive spinal deformity (kyphosis or translation) leading to mechanical instability, intractable pain unresponsive to rigid orthosis and analgesia, or failure of medical management (persistent bacteremia or rising inflammatory markers despite appropriate culture-directed antibiotics).
Diagnostic Biopsy Protocols
When blood cultures are negative or deemed unreliable, a CT-guided percutaneous needle biopsy of the disc space or vertebral body is the mandatory next step before committing to long-term empiric antibiotics. Empiric antibiotics should ideally be withheld in the hemodynamically stable patient until deep tissue cultures are obtained. If the initial CT-guided biopsy is non-diagnostic, a second percutaneous biopsy or an open/endoscopic incisional biopsy may be warranted.
| Clinical Scenario | Intervention Strategy | Rationale |
|---|---|---|
| Neurologically intact, known pathogen (MSSA), stable alignment | Intravenous antibiotics (targeted), rigid orthosis, ID consult | High success rate with medical management; surgery poses unnecessary risk. |
| Negative blood cultures, stable patient | Withhold antibiotics, perform CT-guided biopsy | Essential to isolate pathogen to avoid lifelong suppressive therapy or treatment failure. |
| Progressive motor deficit or Cauda Equina Syndrome | Emergent surgical decompression and stabilization | Mechanical compression by epidural abscess or bone fragments requires immediate relief to salvage function. |
| Progressive focal kyphosis (>15 degrees) or translation | Surgical debridement, anterior column reconstruction, posterior fusion | Restores sagittal balance and prevents delayed neurological compromise and intractable mechanical back pain. |
| Intractable pain despite rigid bracing and appropriate IV antibiotics | Surgical stabilization (often percutaneous or minimally invasive) | Micro-instability at the infected segment drives pain; rigid internal fixation halts this process. |
Contraindications to surgery include severe medical comorbidities precluding general anesthesia, multi-organ failure (unless the spinal infection is the direct source of sepsis and source control is life-saving), and patient refusal. In cases of profound obesity (e.g., BMI > 40) and poorly controlled diabetes, surgical complication rates (especially surgical site infections and wound dehiscence) skyrocket, further reinforcing the necessity of exhausting medical management whenever safely possible.
Pre-Operative Planning, Templating, and Patient Positioning
When surgical intervention becomes unavoidable, meticulous pre-operative planning is the cornerstone of a successful outcome. Advanced imaging is non-negotiable. An MRI with and without gadolinium contrast is the gold standard for defining the extent of the epidural abscess, the degree of neural compression, and the involvement of adjacent paraspinal musculature (e.g., psoas abscess). T1-weighted images typically show hypointense signals in the infected marrow, while T2-weighted and STIR sequences reveal hyperintense fluid and edema in the disc space and vertebral bodies. Gadolinium enhancement highlights the vascularized inflammatory phlegmon and the capsule of any abscesses.
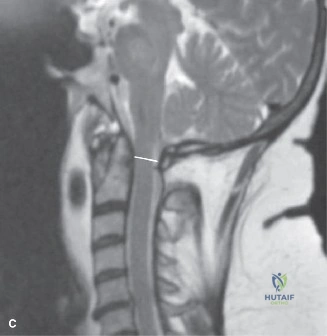
In addition to MRI, a fine-cut computed tomography (CT) scan is essential for evaluating bony destruction. CT allows the surgeon to assess bone stock for pedicle screw purchase and to template the size of the interbody cages required for anterior column reconstruction. Upright standing radiographs (if the patient can tolerate them) or full-length supine films are necessary to evaluate global spinal alignment and regional kyphosis.

Pre-operative medical optimization requires a multidisciplinary approach. The infectious disease team must ensure peak serum bactericidal levels of antibiotics perioperatively. The internal medicine or endocrinology team must aggressively manage blood glucose levels, as hyperglycemia drastically impairs neutrophil function and wound healing. In our 48-year-old diabetic patient, maintaining a perioperative hemoglobin A1c below 7.5% and acute glucose levels between 140-180 mg/dL would be critical if she required surgery.
Patient positioning depends entirely on the chosen surgical approach. For a posterior-only approach (e.g., transforaminal lumbar interbody fusion [TLIF] or posterior column osteotomy), the patient is positioned prone on a radiolucent Jackson table. Care must be taken to pad all bony prominences, allow the abdomen to hang free (to decrease venous pressure and epidural bleeding), and optimize cervical alignment. If an anterior approach is selected (e.g., anterior lumbar interbody fusion [ALIF] or lateral transpsoas approach), the patient is positioned supine or in the lateral decubitus position, respectively. Fluoroscopic localization prior to incision is mandatory to confirm the correct pathological level.
Step-by-Step Surgical Approach and Fixation Technique
The surgical strategy for lumbar spondylodiscitis typically involves radical debridement of the infected tissue, decompression of the neural elements, and rigid mechanical stabilization. While combined anterior-posterior approaches were historically the gold standard, modern spinal instrumentation and techniques have made posterior-only approaches highly effective for the majority of cases, particularly in the mid-to-lower lumbar spine.
Posterior Decompression and Debridement
The procedure begins with a standard midline longitudinal incision, extending at least one level above and below the infected segment. Subperiosteal dissection exposes the posterior elements. Pedicle screws are inserted into the healthy vertebrae adjacent to the infection. In cases of severe endplate destruction, fixation should extend two levels above and two levels below the pathology to ensure adequate biomechanical stability.
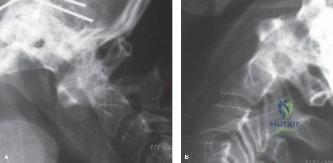
Once instrumentation is placed, a wide laminectomy is performed at the affected level. The ligamentum flavum is excised, exposing the thecal sac and traversing nerve roots. If an epidural abscess is present, it is meticulously evacuated using gentle suction and blunt dissectors. The nerve roots are then mobilized medially to access the infected disc space via a transforaminal approach.
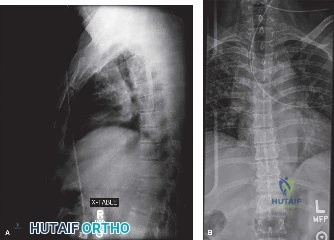
A radical discectomy is performed. All necrotic disc material, infected cartilaginous endplates, and sequestered bone must be aggressively removed using curettes, pituitary rongeurs, and high-speed burrs until punctate bleeding from healthy cancellous bone is encountered. This aggressive debridement is critical for eradicating the bacterial biofilm and providing a vascularized bed for subsequent fusion. Copious irrigation with sterile saline (often several liters) is employed to mechanically wash out residual bacterial load.
Anterior Column Reconstruction
Following debridement, a large void is left in the anterior column. To restore disc height, correct kyphosis, and provide structural support, an interbody device must be inserted. Historically, autologous tricortical iliac crest bone graft was the gold standard. However, structural allografts and titanium cages have been proven safe and highly effective even in the setting of active pyogenic infection, provided that the debridement is thorough and the patient is maintained on appropriate culture-directed antibiotics.
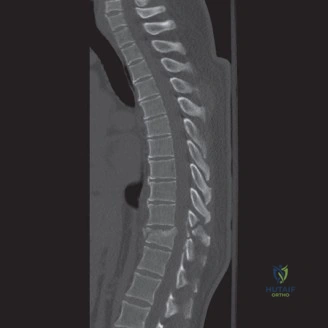
Titanium is particularly advantageous as it resists bacterial colonization better than stainless steel and provides excellent immediate structural support. The cage is packed with autograft (harvested from the laminectomy or iliac crest) or advanced osteoconductive matrices. Once the cage is impacted into the disc space, the pedicle screws are connected with titanium rods, and compression is applied across the construct to lock the interbody graft in place and restore lumbar lordosis. A posterolateral decortication and fusion are then performed using remaining bone graft.
Complications, Incidence Rates, and Salvage Management
Surgical treatment of spondylodiscitis is fraught with potential complications, particularly given the medically fragile nature of the patient population. The presence of systemic infection, combined with the extensive nature of the surgical exposure, creates a high-risk environment for both immediate and delayed adverse events.
Hardware failure and pseudarthrosis remain significant concerns. The infected bone is often osteoporotic due to local hyperemia and disuse, increasing the risk of pedicle screw pullout or subsidence of the interbody cage. If subsidence occurs but alignment remains acceptable and the infection clears, it can often be observed. However, catastrophic failure requires revision surgery, potentially extending the construct or utilizing cement-augmented pedicle screws.
Recurrent or persistent infection is a dreaded complication. This can manifest as persistent drainage, rising inflammatory markers, or new epidural fluid collections. Management involves immediate return to the operating room for irrigation and debridement, exchange of modular hardware components, and consultation with infectious disease for broadening or altering the antimicrobial regimen.
| Complication | Estimated Incidence | Prevention and Salvage Management |
|---|---|---|
| Hardware Loosening / Pullout | 8 - 15% | Prevention: Multi-level fixation, utilize large diameter/length screws, consider cement augmentation in severe osteoporosis. Salvage: Revision with extension of construct. |
| Pseudarthrosis | 10 - 20% | Prevention: Radical debridement to bleeding bone, use of robust autograft, rigid fixation. Salvage: Revision bone grafting, optimization of metabolic factors (Vitamin D, PTH analogs). |
| Recurrent Surgical Site Infection | 5 - 12% | Prevention: Copious intraoperative irrigation, tension-free closure, strict glycemic control (HbA1c < 7.5%). Salvage: Serial I&D, vacuum-assisted closure (VAC), prolonged IV antibiotics. |
| Incidental Durotomy | 4 - 8% | Prevention: Meticulous dissection, especially when epidural tissues are inflamed and adherent. Salvage: Primary watertight suture repair, fibrin glue, flat bed rest for 24-48 hours. |
| Adjacent Segment Disease | 15 - 25% (Long-term) | Prevention: Preservation of adjacent facet capsules, restoration of physiological lumbar lordosis. Salvage: Extension of fusion to the adjacent symptomatic level. |
Neurological injury, while rare, can occur during the mobilization of inflamed, friable nerve roots or during the insertion of instrumentation. Continuous intraoperative neuromonitoring (somatosensory evoked potentials and spontaneous/triggered electromyography) is highly recommended to mitigate this risk.
Phased Post-Operative Rehabilitation Protocols
Whether managed medically or surgically, the rehabilitation and long-term care of the spondylodiscitis patient require a structured, phased approach. The primary goals are the eradication of the infection, the promotion of spinal fusion (either spontaneous autofusion in medical management or surgical arthrodesis), and the restoration of functional mobility.
Phase 1: Acute Management and Immobilization (Weeks 0–6)
During the first six weeks, the patient is typically maintained on intravenous antibiotics. A peripherally inserted central catheter (PICC) line is placed prior to discharge. Immobilization is a critical adjunct, particularly for medically managed patients. A rigid thoracolumbosacral orthosis (TLSO) or a custom-molded rigid lumbar brace is employed whenever the patient is out of bed. It is imperative to note that a simple elastic lumbar corset is entirely inadequate; it provides symptomatic warmth but zero biomechanical restriction. Rigid orthoses restrict gross motion, thereby decreasing micro-motion at the infected segment, alleviating mechanical pain, and facilitating the early stages of bony consolidation.
During this phase, physical therapy focuses on bed mobility, safe transfers, and ambulation with assistive devices. Inflammatory markers—specifically the erythrocyte sedimentation rate (ESR) and C-reactive protein (CRP)—along with a complete blood count (CBC), are monitored weekly or biweekly. CRP is highly responsive and should begin trending downward within days of appropriate therapy, whereas ESR may lag for several weeks.
Phase 2: Transition and Consolidation (Weeks 6–12)
At the 6-week mark, a critical clinical inflection point is reached. As illustrated in the clinical vignette, if the patient demonstrates a favorable clinical response—diminished back pain, stable neurological exam, no radiographic evidence of progressive vertebral collapse, and normalization of WBC, ESR, and CRP—the infectious disease team will typically recommend transitioning from intravenous to highly bioavailable oral antibiotics.
Crucially, antibiotics are not stopped at 6 weeks. The standard of care for vertebral osteomyelitis dictates a total of 12 weeks of continuous antimicrobial therapy to prevent relapse. Oral agents with excellent bone penetration, such as fluoroquinolones, linezolid, or specific beta-lactams, are utilized. The rigid brace is gradually weaned as tolerated, and physical therapy advances to gentle core stabilization exercises, avoiding extreme flexion or extension.
Phase 3: Long-Term Follow-Up and Functional Restoration (Months 3–12)
Upon completion of the 12-week antibiotic course, a final set of inflammatory markers is drawn. Advanced imaging (MRI or CT) is generally not required at the end of treatment if the patient is asymptomatic and markers are normal, as MRI can show persistent marrow edema for many months despite microbiological cure. Radiographs are obtained to assess for spontaneous fusion or the integrity of surgical hardware. The patient is advanced to an unrestricted, progressive resistance training program to rebuild paraspinal musculature and improve cardiovascular endurance.
Summary of Landmark Literature and Clinical Guidelines
The contemporary management of spondylodiscitis is heavily guided by the Infectious Diseases Society of America (IDSA) Clinical Practice Guidelines for the Diagnosis and Treatment of Native Vertebral Osteomyelitis in Adults. These guidelines strongly endorse the initial non-operative approach for neurologically intact patients, emphasizing the critical role of blood cultures and, if necessary, image-guided biopsies prior to antibiotic administration.
The IDSA guidelines also cement the standard duration of antimicrobial therapy at a minimum of 6 weeks, though most orthopedic and infectious disease specialists advocate for a total of 12 weeks (often split between IV and PO) for pyogenic spine infections, particularly when extensive endplate destruction is present. The transition to oral therapy at 6 weeks is supported by robust literature demonstrating non-inferiority to prolonged IV courses, provided the pathogen is susceptible to highly bioavailable oral agents and the patient's inflammatory markers have normalized.
Surgically, landmark biomechanical and clinical studies over the past decade have revolutionized the approach to anterior column reconstruction in the setting of infection. Historically, the use of metallic implants in an infected field was considered taboo. However, extensive retrospective and prospective cohorts have now definitively shown that titanium interbody cages can be safely placed into an actively infected disc space following radical debridement. Titanium's ability to integrate with host bone and its resistance to biofilm formation make it a superior alternative to structural allograft, which carries a higher risk of serving as a necrotic nidus for persistent infection.
Ultimately, deciphering the next course of action in spondylodiscitis requires a nuanced synthesis of the patient's clinical stability, neurological status, radiographic findings, and microbiological data. By adhering to rigorous diagnostic protocols and reserving surgical intervention for specific, evidence-based indications, the orthopedic surgeon can navigate this complex pathology to achieve high rates of infection eradication and functional recovery.
