Complex Elbow Dislocation with PMRRI and Coronoid Fracture: Clinical Presentation & Diagnostic Insights
Key Takeaway
Posteromedial Rotatory Instability (PMRRI) is a complex elbow dislocation, often with an anteromedial coronoid fracture (O'Driscoll Type III). Diagnosis involves clinical assessment for post-reduction instability and critical CT imaging. CT scans precisely define fracture morphology, essential for accurate orthopedic diagnosis and guiding optimal surgical management plans.
Introduction and Epidemiology
Clinical Presentation and History
A 48-year-old male, a recreational basketball player, presented to the emergency department following a fall during a game. He reported falling directly onto an outstretched left upper extremity, landing with his elbow in slight flexion, valgus, and forearm supination. He experienced immediate, severe pain and deformity of the left elbow, with an inability to move the limb. There was no direct impact to the head or other body parts. His medical history was significant for well-controlled hypertension and a remote history of shoulder arthroscopy, but no prior elbow injuries or surgeries. He denied any neurological deficits or numbness prior to the injury.
Clinical Examination Findings
Upon arrival, the patient was in acute distress with significant pain.
* Inspection: Gross deformity of the left elbow was evident, consistent with a posterior dislocation. Marked swelling was present globally, most pronounced posteromedially, and ecchymosis was developing rapidly. The skin overlying the medial epicondyle appeared stretched but intact, without signs of tenting or impending compromise.
* Palpation: Tenderness was exquisite over the medial epicondyle, olecranon, and the proximal ulna. The ulnar nerve sulcus was tender, but the nerve itself was not palpable as entrapped. A palpable defect was noted posteriorly between the olecranon and the distal humerus.
* Range of Motion: Actively and passively, ROM was severely restricted due to pain and mechanical block. The elbow was held in approximately 30-40 degrees of flexion. Any attempt at supination or pronation was exquisitely painful and limited.
* Neurological Assessment: Sensation to light touch was intact in all dermatomes (C5-T1). Motor function was intact, although limited by pain, with full wrist and finger flexion/extension, and gross elbow flexion/extension power present in a limited arc. Specifically, ulnar nerve function (FCU, FDP ulnar half, intrinsic hand muscles) was assessed and found to be grossly intact.
* Vascular Assessment: Radial and ulnar pulses were 2+ bilaterally and symmetrically. Capillary refill was brisk in all digits. No pallor or paresthesia was reported distally.
Initial Imaging and Diagnostics
Initial imaging focused on plain radiographs to confirm dislocation and assess for associated fractures.
- Plain Radiographs:
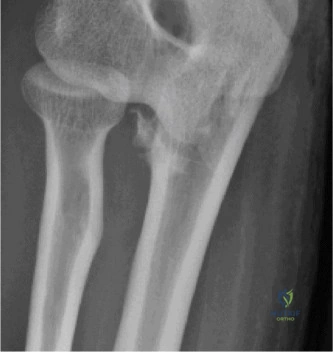
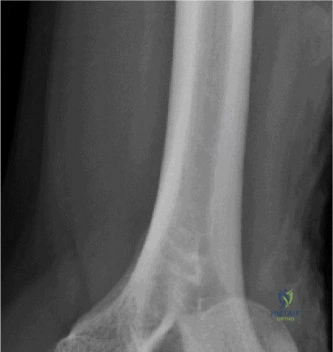
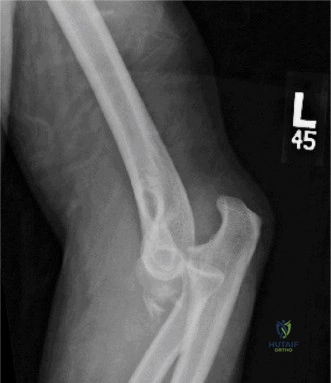
- Anteroposterior and lateral views of the elbow demonstrated a posteromedial dislocation of the ulna relative to the humerus.
- A significant fracture of the anteromedial coronoid process was clearly visible on the lateral view, displacing proximally.
- No obvious radial head fracture or olecranon fracture was identified on these initial views.
- The trochlea appeared to be displaced laterally relative to the coronoid fracture fragment.
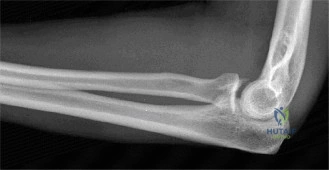
Following initial radiographs, a closed reduction attempt was made in the emergency department under conscious sedation. The elbow was gently reduced, confirmed by post-reduction radiographs. However, despite reduction, the elbow remained grossly unstable, particularly with valgus stress and supination, demonstrating persistent posteromedial subluxation. This finding strongly suggested significant ligamentous and bony disruption.
- Computed Tomography Scan:
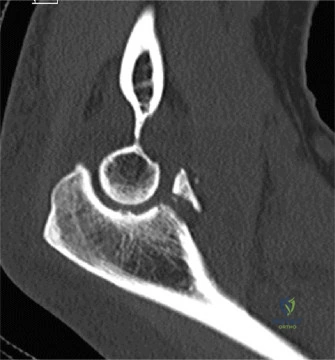
- Given the post-reduction instability and the suspected coronoid fracture, a CT scan of the elbow was obtained to delineate the fracture morphology, displacement, and identify any other subtle bony injuries.
- The CT confirmed a large, comminuted fracture of the anteromedial facet of the coronoid process (O'Driscoll Type III), involving more than 50% of the anteromedial facet and extending towards the sublime tubercle, confirming the diagnosis of varus posteromedial rotatory instability.
Epidemiological Context of Posteromedial Rotatory Instability
Varus posteromedial rotatory instability represents a distinct and highly challenging subset of complex elbow dislocations. Unlike the classic "terrible triad" injury, which is driven by a valgus, axial, and supinating force resulting in radial head and transverse coronoid fractures, varus posteromedial rotatory instability is generated by an axial load combined with varus stress and pronation. This mechanism drives the anteromedial facet of the coronoid process into the medial trochlea, resulting in a shear fracture of the anteromedial facet, accompanied by avulsion or rupture of the lateral collateral ligament complex.
Epidemiologically, these injuries are less common than standard posterolateral rotatory instability patterns but carry a significantly higher morbidity if missed. They frequently occur in middle-aged individuals following a fall on an outstretched hand. Failure to recognize the anteromedial facet fracture and the associated lateral ligamentous incompetence invariably leads to rapid onset post-traumatic arthrosis, joint subluxation, and profound functional impairment.
Surgical Anatomy and Biomechanics
Osteology of the Proximal Ulna and Coronoid
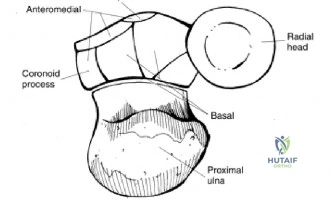
The coronoid process is the keystone of elbow stability, functioning as the primary anterior bony buttress against posterior translation of the ulna. Anatomically, the coronoid is divided into the tip, the body, the anterolateral facet, and the anteromedial facet. The anteromedial facet is particularly critical for varus stability. It lacks cartilaginous coverage at its most medial aspect and serves as the insertion site for the anterior bundle of the medial collateral ligament at the sublime tubercle.
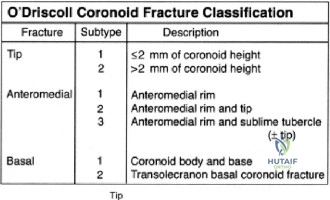
When evaluating coronoid fractures, the O'Driscoll classification provides a vital anatomical framework. Type 1 fractures involve the transverse tip. Type 2 fractures involve the anteromedial facet and are subdivided based on the involvement of the sublime tubercle. Type 3 fractures involve the basal coronoid. Varus posteromedial rotatory instability is uniquely associated with Type 2 (anteromedial facet) fractures. Because the anterior bundle of the medial collateral ligament attaches to the sublime tubercle, a fracture propagating through this region compromises both bony congruency and medial ligamentous restraint.
Ligamentous Restraints and the Lateral Collateral Ligament Complex
The lateral collateral ligament complex is the primary restraint to varus and posterolateral rotatory stress. It consists of the radial collateral ligament, the lateral ulnar collateral ligament, the annular ligament, and the accessory lateral collateral ligament. The lateral ulnar collateral ligament originates from the isometric point on the lateral epicondyle and inserts on the supinator crest of the ulna.
In the setting of varus posteromedial rotatory instability, the lateral collateral ligament complex is invariably disrupted. The mechanism of injury dictates that the lateral structures fail first under tension as the elbow is forced into varus. Once the lateral collateral ligament complex tears, the elbow joint hinges open laterally, driving the medial trochlea into the anteromedial coronoid, resulting in the characteristic shear fracture.
Biomechanics of Varus Posteromedial Rotatory Instability
Understanding the biomechanics of this injury pattern is paramount for successful surgical reconstruction. The elbow joint relies on a highly congruent ulnohumeral articulation. When the anteromedial facet is fractured, the medial column loses its bony support. Concurrently, the lateral collateral ligament deficiency eliminates the lateral tension band.
During active elbow flexion and extension, especially in pronation, gravitational and muscular forces normally stabilize the joint. However, in the varus posteromedial rotatory instability elbow, the absent anteromedial buttress allows the medial trochlea to subluxate posteriorly and medially. If the surgeon only repairs the lateral collateral ligament without restoring the anteromedial coronoid buttress, the lateral repair will inevitably fail under the sheer biomechanical stress of the medial column collapse. Therefore, anatomic restoration of the anteromedial facet is non-negotiable.
Indications and Contraindications
The management of complex elbow dislocations involving the anteromedial facet and lateral collateral ligament complex requires aggressive surgical intervention in the vast majority of cases. Non-operative management is reserved for an exceedingly narrow subset of patients.
| Clinical Scenario | Operative Indication | Non-Operative Indication |
|---|---|---|
| Anteromedial Facet Fracture | Displaced >2mm, involvement of sublime tubercle, any associated mechanical block or subluxation. | Truly non-displaced fractures with a perfectly concentric joint on dynamic fluoroscopy (rare). |
| LCL Complex Tear | Gross varus instability, persistent subluxation after closed reduction, associated with coronoid fracture. | Isolated sprains without functional instability or bony injury. |
| Ulnar Neuropathy | Progressive motor or sensory deficit, entrapment in the joint space. | Transient neuropraxia resolving post-reduction (relative, may still require surgery for bony injury). |
| Patient Factors | Active individuals, high functional demands, medically optimized. | Severe medical comorbidities precluding anesthesia, non-ambulatory patients with minimal upper extremity demands. |
Contraindications to immediate surgical intervention include active superficial or deep soft tissue infection, profound medical instability (e.g., polytrauma with hemodynamic shock), or severe overlying soft tissue compromise (e.g., massive fracture blisters) requiring a delay for soft tissue resuscitation. In cases of severe soft tissue compromise, a spanning external fixator may be applied temporarily.
Pre Operative Planning and Patient Positioning
Advanced Imaging and Templating
Following the initial clinical evaluation and plain radiography, a multidetector Computed Tomography scan with 3D reconstructions is mandatory. The anteromedial facet fracture is notoriously difficult to fully characterize on standard AP and lateral radiographs due to overlap of the radial head and the complex native anatomy of the proximal ulna.
Preoperative templating must focus on the size and comminution of the anteromedial fragment. Small, highly comminuted fragments may not be amenable to standard screw fixation and will require suture lasso techniques or specialized mini-fragment buttress plating. The surgeon must ensure availability of 2.0mm and 2.4mm locking plate sets, headless compression screws, and robust suture anchors for ligamentous repair.
Anesthesia and Patient Positioning
Surgery is typically performed under general anesthesia. A regional interscalene or supraclavicular nerve block is highly recommended for postoperative pain control, provided a thorough preoperative neurological examination has been documented.
The patient is positioned supine on the operating table. A non-sterile tourniquet is applied high on the brachium. The arm is draped free and positioned either across the chest or on a radiolucent hand table. The "arm across the chest" position is highly advantageous for addressing the lateral side of the elbow, as gravity assists in opening the lateral joint space. Conversely, resting the arm on a hand table provides excellent access to the medial aspect of the elbow for coronoid fixation. Many surgeons prefer a dynamic setup where the arm can be moved between the chest and the hand table throughout the procedure.
A sterile tourniquet may be utilized if proximal extension of the incision is anticipated, though a standard high-arm tourniquet is usually sufficient. Fluoroscopy must be positioned to allow for orthogonal views of the elbow without compromising the sterile field.
Detailed Surgical Approach and Technique
The surgical management of varus posteromedial rotatory instability requires a dual-incision approach or a single posterior midline incision with large medial and lateral fasciocutaneous flaps. Given the distinct medial and lateral pathology, dual incisions (a direct medial approach and a direct lateral approach) minimize the risk of large flap necrosis and provide direct orthogonal access to the respective pathologies.
Medial Approach and Coronoid Fixation
The anteromedial facet fracture must be addressed first. Restoring the medial bony column provides a stable foundation against which the lateral ligamentous complex can be tensioned.
- Incision and Superficial Dissection: A medial incision is made centered over the medial epicondyle, extending distally along the sublime tubercle. Care is taken to identify and protect the medial antebrachial cutaneous nerve branches.
- Ulnar Nerve Management: The ulnar nerve is identified proximally in the cubital tunnel and decompressed. Depending on the surgeon's preference and the extent of distal dissection required, the nerve is either protected in situ or routinely transposed anteriorly to prevent iatrogenic injury during plate placement.
- Deep Dissection and Internervous Planes: The flexor-pronator mass is identified. Two primary deep approaches can be utilized: the over-the-top approach (Hotchkiss) or the FCU split approach (Taylor and Scham). For anteromedial facet fractures, splitting the two heads of the flexor carpi ulnaris provides direct, unparalleled access to the sublime tubercle and the anteromedial coronoid.
- Fracture Preparation and Reduction: The fracture hematoma is evacuated. The anteromedial facet fragment is mobilized. Often, the anterior bundle of the medial collateral ligament remains attached to this fragment. The fragment is anatomically reduced using dental picks or a small pointed reduction forceps.
- Fixation Strategy: Fixation is achieved using a pre-contoured anteromedial coronoid buttress plate. The plate is positioned on the anteromedial surface of the proximal ulna, buttressing the fragment against the metaphysis. Distal fixation is achieved with bicortical screws, while proximal fixation into the coronoid fragment may utilize locking screws or, if the fragment is too small, sutures passed through the plate and around the capsuloligamentous insertion.
Lateral Approach and Ligamentous Repair
Once the medial column is rigidly stabilized, attention is turned to the lateral side to address the lateral collateral ligament complex avulsion.
- Incision and Superficial Dissection: A lateral incision is made from the lateral supracondylar ridge extending distally toward the radial head.
- Internervous Plane: The Kocher interval (between the anconeus and the extensor carpi ulnaris) is developed. This plane is relatively avascular and provides direct access to the lateral capsule and the lateral ulnar collateral ligament footprint.
- Identification of Pathology: The lateral collateral ligament complex is typically found avulsed from its humeral origin on the lateral epicondyle. The joint space is irrigated, and any intra-articular debris or osteochondral loose bodies are removed.
- Ligament Repair: The isometric point on the lateral epicondyle is identified (at the center of capitellar curvature). A bleeding bony bed is prepared using a rongeur or burr. Suture anchors (typically 3.5mm or 4.75mm, depending on bone quality) are placed at the isometric origin. Krackow or locking whipstitches are placed through the avulsed lateral ulnar collateral ligament and radial collateral ligament.
- Tensioning and Tying: The elbow is placed in 30 to 40 degrees of flexion and full pronation. Pronation closes the lateral joint space and relaxes the lateral ligamentous structures. The sutures are tied, securing the ligament complex back to its anatomical footprint.
Final Intraoperative Assessment
Following fixation and repair, the elbow must be assessed fluoroscopically and clinically for stability.
* The joint should be taken through a full range of motion.
* A "hanging arm" test or varus/valgus stress testing under fluoroscopy confirms concentric reduction.
* There should be no opening of the lateral joint line on varus stress, and the ulnohumeral joint must remain perfectly concentric.
* 
Complications and Management
Surgical management of complex elbow dislocations is fraught with potential complications. The elbow is highly prone to stiffness, and the proximity of major neurovascular structures increases the risk of iatrogenic injury.
| Complication | Incidence | Etiology and Management Strategy |
|---|---|---|
| Post-Traumatic Stiffness | High (>50%) | Etiology: Capsular contracture, prolonged immobilization, heterotopic ossification. Management: Prevention is key via early active ROM. If refractory after 6 months, consider arthroscopic or open arthrolysis and capsular release. |
| Heterotopic Ossification | 10-20% | Etiology: Severe soft tissue trauma, delayed surgery, central nervous system injury. Management: Prophylaxis with Indomethacin or single-dose radiation in high-risk patients. Surgical excision must be delayed until bone is metabolically mature (typically 6-12 months). |
| Ulnar Neuropathy | 5-15% | Etiology: Initial trauma, traction during medial approach, implant prominence, perineural fibrosis. Management: Routine intraoperative decompression. If postoperative symptoms persist, EMG/NCS evaluation followed by revision neurolysis and submuscular transposition may be required. |
| Recurrent Instability | <5% | Etiology: Failure to recognize or adequately fix the anteromedial facet, non-isometric LCL repair, patient non-compliance. Management: Revision surgery with robust bony fixation, ligamentous reconstruction using autograft (e.g., palmaris longus), or hinged external fixation. |
| Hardware Prominence | 10-15% | Etiology: Subcutaneous nature of the proximal ulna, especially medial plates. Management: Hardware removal after radiographic union (typically >9-12 months post-op) if causing significant soft tissue irritation. |
Post Operative Rehabilitation Protocols
The paramount goal of postoperative rehabilitation following fixation of a varus posteromedial rotatory instability pattern is to balance the protection of the surgical repair with the prevention of devastating elbow stiffness.
Phase I: Immediate Postoperative Period (0 to 2 Weeks)
The patient is typically immobilized in a well-padded posterior splint with the elbow at 90 degrees of flexion and the forearm in neutral to slight pronation. Pronation is critical as it protects the lateral collateral ligament repair by utilizing the intact medial soft tissue hinge and the newly reconstructed anteromedial bony buttress to close the lateral joint space.
During this phase, strict elevation is enforced to minimize edema. Active range of motion of the shoulder, wrist, and digits is initiated immediately to prevent distal edema and maintain tendon glide.
Phase II: Early Active Motion (2 to 6 Weeks)
At the two-week mark, the surgical incisions are inspected, and sutures are removed. The posterior splint is transitioned to a hinged elbow brace.
- Motion Protocol: The brace is unlocked to allow active and active-assisted range of motion in flexion and extension. Extension may be blocked at 30 degrees initially if there are concerns regarding the robustness of the lateral repair, gradually advancing by 10 degrees per week.
- Forearm Rotation: Pronation and supination are performed with the elbow flexed to 90 degrees. Supination combined with extension must be strictly avoided, as this is the primary mechanism of posterolateral subluxation and places maximal stress on the lateral collateral ligament repair.
- Shoulder Positioning: Patients are instructed to avoid shoulder abduction combined with internal rotation (the "pushing up from a chair" position), as this imparts a massive varus force across the elbow joint.
Phase III: Strengthening and Normalization (6 to 12 Weeks)
Radiographs are obtained at 6 weeks to confirm maintenance of reduction and assess fracture healing. Once early union is evident and the joint remains concentric, the hinged brace is discontinued.
- Progressive Loading: Passive stretching is initiated to address residual flexion or extension deficits. Isometric strengthening begins, progressing to isotonic exercises for the biceps, triceps, and forearm musculature.
- Return to Activity: Light functional activities are permitted. Heavy lifting, contact sports, and activities imparting significant varus/valgus stress are restricted until at least 4 to 6 months postoperatively, contingent upon full radiographic union and restoration of dynamic joint stability.
Summary of Key Literature and Guidelines
The understanding and management of varus posteromedial rotatory instability have evolved significantly over the past two decades, driven by landmark biomechanical and clinical studies.
- O'Driscoll et al. (2003): This foundational paper redefined the classification of coronoid fractures. O'Driscoll identified the critical biomechanical role of the anteromedial facet, demonstrating that fractures in this region (Type 2) are distinct from transverse tip fractures. The study highlighted that the anteromedial facet is the primary restraint to varus stress and that its loss leads to rapid joint subluxation.
- Doornberg and Ring (2006): This clinical series clearly delineated the varus posteromedial rotatory instability pattern from the terrible triad. The authors demonstrated that patients with anteromedial facet fractures and lateral collateral ligament tears face a high rate of rapid post-traumatic osteoarthritis if treated non-operatively or with isolated ligamentous repair. They established the absolute necessity of rigidly fixing the anteromedial facet.
- Sanchez-Sotelo et al. (2005): This work focused on the surgical approaches and fixation techniques for complex coronoid fractures. It popularized the use of contoured mini-fragment plates applied directly to the anteromedial surface of the ulna, proving superior biomechanical stability compared to isolated screw fixation or suture lasso techniques for larger fragments.
- Pollock et al. (2009): A biomechanical study that quantified the forces across the elbow joint, confirming that the lateral collateral ligament is the primary restraint to varus stress, but it functions in a codependent relationship with the anteromedial coronoid. If the coronoid is deficient, the forces on the lateral collateral ligament exceed its ultimate tensile strength, leading to inevitable repair failure.
