Anterior Instability: How Glenoid Bone Loss Shapes Treatment
Key Takeaway
This article provides essential research regarding Anterior Instability: How Glenoid Bone Loss Shapes Treatment. Glenoid bone loss refers to the reduction of bone from the glenoid, appearing as an identifiable fragment or attritional loss. It is a significant factor contributing to recurrent anterior shoulder instability. For substantial glenoid bone loss, typically over 20%, surgical interventions like a Latarjet procedure are often employed to stabilize the shoulder, influencing treatment decisions.
Introduction and Epidemiology
Anterior shoulder instability represents the most common major joint dislocation encountered in orthopedic practice, disproportionately affecting young, active, and athletic populations. While the classic Bankart lesion—an avulsion of the anteroinferior capsulolabral complex—was historically considered the essential lesion of anterior instability, contemporary orthopedic understanding has shifted dramatically toward the recognition of osseous defects. Glenoid bone loss, often occurring in tandem with humeral head defects (Hill-Sachs lesions) to create bipolar bone loss, fundamentally alters the biomechanical stability of the glenohumeral joint and dictates surgical decision making.
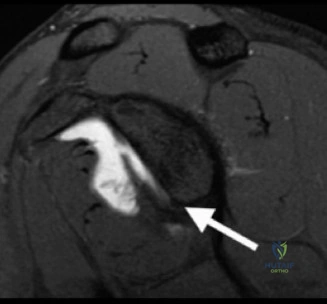
The epidemiology of anterior instability highlights a high recurrence rate, particularly in patients under the age of 20 engaged in contact sports. Recurrence rates following non operative management in this demographic can exceed 80 percent. Even following arthroscopic soft tissue stabilization, recurrence rates remain unacceptably high if critical glenoid bone loss is unrecognized or inadequately addressed. The incidence of significant glenoid bone loss in recurrent instability patients is estimated to be between 20 and 40 percent. The morphology of this bone loss typically manifests as attrition or fracture of the anteroinferior glenoid rim, transforming the normal pear shaped glenoid into an "inverted pear" configuration.
Understanding how glenoid bone loss shapes treatment is paramount for the orthopedic surgeon. The paradigm has evolved from a uniform approach of arthroscopic Bankart repair to a highly individualized algorithm based on precise quantification of osseous defects. The failure to recognize critical or subcritical glenoid bone loss is the leading cause of failed soft tissue stabilization, necessitating a thorough understanding of the pathophysiology, advanced imaging techniques, and complex reconstructive options such as the Latarjet procedure, iliac crest bone grafting, or distal tibial allografting.

Surgical Anatomy and Biomechanics
The glenohumeral joint relies on a complex interplay of static and dynamic stabilizers due to its minimal intrinsic osseous constraint. The glenoid fossa is relatively flat, covering only one quarter to one third of the humeral head articular surface. Static stability is provided by the capsulolabral complex, the negative intraarticular pressure, and the geometry of the articular surfaces. Dynamic stability is governed by the rotator cuff musculature, which compresses the humeral head into the glenoid concavity, and the periscapular muscles that position the glenoid in space.
Glenoid bone loss compromises the concavity compression mechanism. The anteroinferior glenoid acts as a critical buttress against anterior translation when the arm is in the vulnerable position of abduction and external rotation. Loss of bone in this region decreases the articular arc length and reduces the force required to translate the humeral head out of the fossa. Biomechanical studies have demonstrated that a defect of 20 percent of the glenoid width reduces the resistance to anterior translation by over 30 percent.
The concept of the Glenoid Track is essential for understanding bipolar bone loss. The glenoid track is the contact zone of the glenoid on the posterior humeral head as the arm moves through its range of motion. If a Hill-Sachs lesion extends medial to the glenoid track, it is classified as "off track" and will engage the anterior glenoid rim, levering the humeral head out of the joint. Glenoid bone loss narrows the glenoid track, making a previously "on track" Hill-Sachs lesion "off track."
When addressing glenoid bone loss surgically, particularly with the Latarjet procedure, the anatomy of the coracoid process and its attachments must be intimately understood. The coracoid provides origins for the short head of the biceps brachii and the coracobrachialis (the conjoined tendon), and the pectoralis minor, as well as the insertion of the coracoacromial ligament. The Latarjet procedure provides a triple blocking effect
First, the bone block increases the anteroposterior diameter of the glenoid, restoring the articular arc.
Second, the conjoined tendon acts as a dynamic sling across the inferior subscapularis and anteroinferior capsule when the arm is abducted and externally rotated.
Third, the repair of the capsule to the stump of the coracoacromial ligament provides a reinforced static restraint.
The neurovascular anatomy surrounding the coracoid and anterior shoulder is complex and perilous. The musculocutaneous nerve typically enters the conjoined tendon 3 to 8 centimeters distal to the coracoid tip, but anatomical variants exist where it enters much closer. The axillary nerve traverses the inferior capsule and must be protected during capsular release and glenoid exposure.
Indications and Contraindications
The management of anterior instability is dictated by the degree of glenoid bone loss, the presence of an engaging Hill-Sachs lesion, and patient specific risk factors. The Instability Severity Index Score is a validated tool that incorporates age, sport type, level of play, hyperlaxity, and radiographic findings to predict the risk of recurrence following arthroscopic Bankart repair. A score of over 6 points historically suggests an unacceptably high recurrence risk with soft tissue repair alone, prompting consideration for bony augmentation.
Historically, the threshold for critical glenoid bone loss was considered to be 20 to 25 percent of the glenoid width. However, recent literature has identified "subcritical" bone loss—defined as 13.5 to 15 percent—as a significant risk factor for failure in high demand athletes, particularly when combined with an off track Hill-Sachs lesion.
Operative intervention is indicated for recurrent anterior instability, first time dislocations in high risk athletes, and instability associated with significant osseous defects. Contraindications to bony augmentation procedures include active infection, severe medical comorbidities precluding surgery, and voluntary multidirectional instability without a traumatic etiology.
Operative Versus Non Operative Management Strategies
| Management Strategy | Indications | Contraindications |
|---|---|---|
| Non Operative Rehabilitation | First time dislocation in older/low demand patients; Voluntary instability; Multidirectional instability without structural lesions. | Recurrent traumatic instability; High demand collision athletes with structural defects; Engaging Hill-Sachs lesions. |
| Arthroscopic Bankart Repair | Recurrent instability with minimal glenoid bone loss (under 13.5 percent); "On track" Hill-Sachs lesion; Low ISIS score. | Glenoid bone loss over 15 percent; "Off track" Hill-Sachs lesion; High demand collision athletes with poor tissue quality. |
| Arthroscopic Bankart with Remplissage | Subcritical glenoid bone loss (10 to 15 percent) with an "off track" Hill-Sachs lesion; Revision soft tissue stabilization without massive glenoid loss. | Critical glenoid bone loss over 20 percent; Significant stiffness or restricted external rotation preoperatively. |
| Latarjet Procedure | Glenoid bone loss over 15 to 20 percent; Revision of failed Bankart repair; High demand collision athletes with subcritical bone loss. | Massive glenoid bone loss exceeding coracoid dimensions (over 30 percent); Advanced glenohumeral osteoarthritis. |
| Distal Tibial or Iliac Crest Allograft | Massive glenoid bone loss (over 25 to 30 percent); Failed Latarjet procedure with resorbed coracoid graft. | Active infection; Lack of adequate native bone stock for screw fixation. |
Pre Operative Planning and Patient Positioning
Thorough preoperative planning is the cornerstone of successful instability surgery. Standard radiographic evaluation should include a true anteroposterior view in the plane of the scapula (Grashey view), an axillary lateral view, and a Stryker notch view to evaluate for Hill-Sachs lesions. The Bernageau or West Point axillary views can provide additional information regarding the anteroinferior glenoid rim.
Advanced imaging is mandatory when bone loss is suspected. While Magnetic Resonance Imaging or MR Arthrogram is excellent for evaluating the capsulolabral complex, rotator cuff, and cartilage, three dimensional Computed Tomography is the gold standard for quantifying osseous defects.
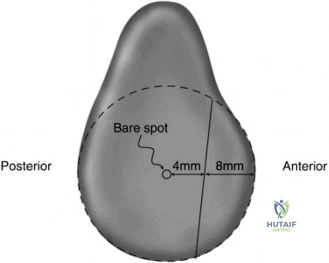
The en face view of the glenoid on 3D CT with the humeral head digitally subtracted allows for precise measurement. The "best fit circle" method is commonly utilized. A circle is drawn matching the contour of the inferior and posterior glenoid, and the area or width of the missing anterior bone is calculated relative to the area or diameter of the circle. The Pico method compares the surface area of the injured glenoid to the contralateral normal glenoid, assuming the contralateral shoulder is uninjured. The humeral head must also be evaluated to calculate the glenoid track, measuring the width of the Hill-Sachs lesion and the intact anterior glenoid bone bridge.
Patient positioning is dictated by the planned surgical procedure. For an arthroscopic Bankart repair or remplissage, the surgeon may choose either the lateral decubitus or the beach chair position based on preference. Lateral decubitus provides excellent visualization and access to the inferior capsule due to longitudinal and lateral traction.
For open bony augmentation procedures such as the Latarjet, the beach chair position is universally preferred. The patient is positioned with the backrest elevated to approximately 45 to 60 degrees. The head is secured in a neutral position to avoid cervical spine hyperextension or lateral flexion, which could place traction on the brachial plexus. The operative arm must be completely free to allow for manipulation, specifically abduction and external rotation, which is critical for exposing the anterior glenoid and managing the subscapularis. A pneumatic arm positioner is highly advantageous for maintaining the limb in precise positions during the coracoid harvest and graft fixation.
Detailed Surgical Approach and Technique
This section will focus on the open Latarjet procedure, as it is the workhorse operation for anterior instability in the setting of significant glenoid bone loss. The procedure demands meticulous dissection, precise osteotomies, and rigid fixation.
Surgical Approach and Coracoid Preparation
A 5 to 7 centimeter incision is made starting at the tip of the coracoid process and extending distally toward the axillary fold, following the deltopectoral groove. The cephalic vein is identified and typically retracted laterally with the deltoid, preserving its major tributaries. The deltopectoral interval is developed, exposing the clavipectoral fascia, which is incised lateral to the conjoined tendon.
The coracoid process is exposed from its tip to its base. The coracoacromial ligament is identified and sectioned approximately 1.5 centimeters from its coracoid insertion, preserving a stump for later capsular repair. The pectoralis minor tendon is released from the medial border of the coracoid. Extreme care must be taken during the medial dissection to avoid injury to the neurovascular bundle.
The coracoid osteotomy is performed using an oscillating saw or a curved osteotome. The cut is made at the "knee" of the coracoid, just distal to the coracoclavicular ligaments, ensuring a graft length of at least 2.5 to 3 centimeters. The graft is then mobilized. The musculocutaneous nerve must be palpated and protected during mobilization. The inferior surface of the coracoid (which will become the articular surface) is decorticated using a burr or saw to expose bleeding cancellous bone. Two drill holes are placed in the graft, typically 1 centimeter apart, using a specialized drill guide.
Subscapularis Management and Joint Exposure
The subscapularis muscle can be managed via a tenotomy, a peel, or a muscle splitting approach. The subscapularis split is currently favored as it preserves the dynamic stabilizing function of the muscle. The split is performed horizontally at the junction of the upper two thirds and lower one third of the muscle belly.
A self retaining retractor is placed within the split to expose the underlying capsule. The capsule is incised vertically. A Fukuda retractor is placed within the joint to retract the humeral head laterally and posteriorly, providing visualization of the anterior glenoid.
Glenoid Preparation and Graft Fixation
The anteroinferior glenoid neck is cleared of all soft tissue and labral remnants. The bone is decorticated with a burr to create a flat, bleeding bed that precisely matches the prepared surface of the coracoid graft. This step is critical for achieving bony union.
The coracoid graft is passed through the subscapularis split. The graft must be positioned perfectly flush with, or slightly medial to (no more than 1 millimeter), the articular cartilage of the glenoid. If the graft is placed too laterally, it will overhang the joint, leading to rapid and devastating glenohumeral osteoarthritis. If placed too medially, it will fail to restore the articular arc and the bony blocking effect will be lost.
Once the graft is provisionally fixed with K-wires, two partially threaded cancellous screws (typically 3.5 or 4.0 millimeters) or cannulated screws are inserted. Compression across the osteotomy site is essential. Biomechanical studies support the use of two screws to prevent rotation of the graft. Alternatively, cortical buttons can be used for fixation, which may reduce the risk of hardware complications.
Capsular Repair and Closure
Following rigid fixation, the capsule is repaired to the preserved stump of the coracoacromial ligament attached to the coracoid graft. This step restores the anterior capsular restraint and makes the graft extra articular, theoretically reducing the risk of arthropathy. The subscapularis split is allowed to close naturally, and the deltopectoral interval is approximated. The skin is closed in a standard layered fashion.
Complications and Management
While the Latarjet procedure is highly effective at preventing recurrent instability, it is technically demanding and associated with a unique set of complications. The overall complication rate ranges from 15 to 30 percent, though the rate of complications requiring revision surgery is significantly lower.
Neurologic injury is a devastating complication. The musculocutaneous nerve is at highest risk during coracoid mobilization and retraction, while the axillary nerve is at risk during inferior capsular release and glenoid exposure. Most nerve palsies are neuropraxias secondary to traction and resolve with observation, but iatrogenic transection requires immediate microsurgical repair.
Graft nonunion or osteolysis occurs when the graft fails to incorporate into the glenoid. Osteolysis is frequently observed at the superior pole of the graft and is thought to be related to stress shielding or lack of mechanical loading. While often asymptomatic, significant osteolysis can lead to recurrent instability.
Hardware complications, such as screw backout or breakage, can cause mechanical symptoms, pain, and cartilage damage. Prominent screws require removal once graft union is confirmed.
Glenohumeral osteoarthritis is a long term complication, primarily driven by lateral graft overhang or over tightening of the anterior structures. Precise graft positioning is the most critical factor in preventing this complication.
Common Complications and Salvage Strategies
| Complication | Estimated Incidence | Prevention and Salvage Strategies |
|---|---|---|
| Neurologic Injury | 1 to 3 percent | Prevention: Direct visualization; avoid excessive medial retraction; release retractors periodically. Salvage: EMG at 6 weeks if no recovery; nerve exploration and grafting if transected. |
| Graft Nonunion | 5 to 10 percent | Prevention: Meticulous decortication of both surfaces; rigid bicolortical compression; smoking cessation. Salvage: Revision fixation with bone grafting; conversion to distal tibial allograft if graft is completely resorbed. |
| Graft Osteolysis | 10 to 20 percent | Prevention: Flush positioning to ensure mechanical loading; use of cortical buttons instead of rigid screws (controversial). Salvage: Often asymptomatic; if instability recurs, revision bony augmentation is required. |
| Hardware Prominence | 5 to 8 percent | Prevention: Countersink screw heads; ensure accurate screw length measurement to avoid posterior prominence. Salvage: Arthroscopic or open hardware removal after CT confirmation of solid bony union. |
| Recurrent Instability | 2 to 5 percent | Prevention: Accurate assessment of bipolar bone loss; proper graft positioning; secure capsular repair. Salvage: Distal tibial allograft; Iliac crest bone block; addressing concurrent capsular laxity. |
| Osteoarthritis | 10 to 15 percent (long term) | Prevention: Avoid lateral graft overhang (graft must be flush or slightly medial); avoid over tightening the subscapularis. Salvage: Conservative management; total shoulder arthroplasty in older, low demand patients. |
Post Operative Rehabilitation Protocols
Rehabilitation following bony augmentation for anterior instability must balance the protection of the osteotomy site and capsular repair with the prevention of postoperative stiffness. The protocol is generally divided into distinct phases based on biological healing timelines.
Phase One Protection and Early Motion
Lasting from surgery until postoperative week four, the primary goal is graft protection. The patient is immobilized in a sling. Pendulum exercises and passive forward elevation up to 90 degrees are initiated immediately. External rotation is strictly limited to neutral to protect the subscapularis split and avoid tension on the coracoid graft via the conjoined tendon. Active elbow, wrist, and hand range of motion are encouraged.
Phase Two Active Assisted Motion
From weeks four to eight, the sling is discontinued. Active assisted range of motion is initiated, progressing to active range of motion as tolerated. Forward elevation is advanced to full. External rotation is gradually increased, aiming for 30 degrees by week six and full range of motion by week eight. Scapular stabilization exercises and closed chain isometric exercises are introduced.
Phase Three Strengthening
Beginning at week eight, provided there is radiographic evidence of early graft incorporation, strengthening exercises are initiated. Rotator cuff and periscapular strengthening are prioritized. Resistance bands and light weights are utilized. The focus is on restoring dynamic stability and muscular endurance. Proprioceptive training is also integrated during this phase.
Phase Four Return to Sport
From months four to six, the focus shifts to sport specific activities. Advanced plyometrics, throwing programs, and contact drills are introduced. Return to collision sports is typically permitted at the six month mark, contingent upon full, painless range of motion, symmetrical strength (at least 90 percent of the contralateral side), and CT confirmation of solid graft union.
Summary of Key Literature and Guidelines
The management of anterior instability with glenoid bone loss is heavily guided by several landmark biomechanical and clinical studies.
The concept of the "inverted pear" glenoid was popularized by Burkhart and De Beer in 2000. Their seminal paper demonstrated that arthroscopic Bankart repair in patients with significant bone loss (defined as the loss of the inferior glenoid contour) resulted in an unacceptable recurrence rate of 67 percent, compared to 4 percent in patients without significant bone loss. This established the absolute necessity of evaluating bone stock prior to soft tissue stabilization.
Balg and Boileau introduced the Instability Severity Index Score in 2007. By assigning point values to risk factors such as age under 20, competitive sports, contact sports, shoulder hyperlaxity, Hill-Sachs lesions on AP radiographs, and loss of glenoid contour, they created a prognostic tool. A score of over 6 points became a widely accepted threshold for recommending a Latarjet procedure over an arthroscopic Bankart repair, standardizing the treatment algorithm.
The Glenoid Track concept, detailed by Di Giacomo, Itoi, and Burkhart in 2014, revolutionized the understanding of bipolar bone loss. They provided a biomechanical framework to determine whether a Hill-Sachs lesion would engage the anterior glenoid rim based on the width of the intact glenoid. This concept shifted the focus from isolated glenoid or humeral defects to the dynamic interplay between the two surfaces, guiding the use of the remplissage procedure for off track lesions with subcritical glenoid bone loss.
More recently, literature by Dickens and colleagues has challenged the traditional 20 percent threshold for critical glenoid bone loss. Their research indicates that "subcritical" bone loss—as low as 13.5 percent—can lead to poor clinical outcomes and recurrent instability in high demand, collision athletes. This has led to a paradigm shift, lowering the threshold for bony augmentation or prompting the routine addition of a remplissage to arthroscopic Bankart repairs in this specific patient population.
In summary, the treatment of anterior shoulder instability is fundamentally shaped by the presence and magnitude of glenoid bone loss. Successful outcomes rely on meticulous preoperative radiographic quantification, strict adherence to evidence based indications, and precise surgical execution of advanced reconstructive techniques.
