Recurrent Anterior Shoulder Instability in Elite Athletes: A Diagnostic Case Study
Key Takeaway
Diagnosing recurrent anterior shoulder instability, especially in athletes like rugby players, involves a thorough clinical exam, including apprehension and relocation tests. Crucial imaging includes CT for quantifying glenoid bone loss and Hill-Sachs lesions, and MRA to assess labral tears and capsular laxity. These findings guide precise surgical planning for return to sport.
Patient Presentation and History
A 28-year-old male professional rugby player presented to our clinic with recurrent right shoulder instability. His initial injury occurred approximately 18 months prior during a rugby tackle, resulting in a traumatic anterior glenohumeral dislocation. This was reduced in the emergency department, followed by a period of sling immobilization for three weeks and supervised physiotherapy. Despite adherence to the rehabilitation protocol, he experienced three further episodes of anterior dislocation over the subsequent 12 months, all during sporting activities involving abduction and external rotation. The most recent episode, three weeks prior to presentation, spontaneously reduced but left him with persistent apprehension and an inability to return to sport.
He reports significant pain with overhead activities and a constant fear of re-dislocation. He denies any paresthesia, weakness, or neurovascular symptoms. There is no personal or family history of generalized ligamentous laxity or connective tissue disorders. His past medical history is unremarkable, and he takes no regular medications. He is a non-smoker and consumes alcohol socially. His primary goal is to return to elite-level rugby.
Mechanism of Injury and Biomechanical Considerations
The initial traumatic event involved a high-energy collision characteristic of elite rugby, specifically a tackle where the right arm was forced into extreme abduction, external rotation, and extension. This position places maximal stress on the anterior band of the inferior glenohumeral ligament (IGHL) complex. When the applied force exceeds the tensile strength of the capsulolabral complex, catastrophic failure occurs, typically resulting in the detachment of the anteroinferior labrum from the glenoid rim—the classic Bankart lesion.
In this patient's case, the high-energy nature of the initial trauma, combined with the compressive forces generated by the surrounding musculature during the dislocation event, resulted in an impaction fracture of the posterosuperior humeral head against the dense cortical bone of the anterior glenoid rim. This created a Hill-Sachs lesion, while simultaneously causing a shear fracture or attritional wear of the anterior glenoid rim, leading to a bony Bankart lesion. The subsequent recurrent dislocations over the following 12 months exacerbated this osseous deficiency, leading to a progressive loss of the anterior glenoid articular arc and deepening of the humeral head defect, establishing a highly unstable biomechanical environment.
Natural History and Recurrence Risk Factors
The natural history of traumatic anterior shoulder instability in young, high-demand athletes is characterized by an exceptionally high rate of recurrence when managed non-operatively. Literature suggests that athletes under the age of 20 have recurrence rates approaching 90%, and those in their twenties, particularly those engaged in contact sports like rugby, face recurrence rates between 60% and 80%. The failure of supervised physiotherapy in this patient underscores the structural nature of his pathology; dynamic stabilizers (rotator cuff and periscapular musculature) are insufficient to compensate for significant osseous and capsuloligamentous defects in the setting of high-velocity, sport-specific loads.
Clinical Examination Findings
Upon inspection, the right shoulder demonstrated no obvious deformity, swelling, or ecchymosis. There was no visible muscle atrophy of the deltoid or rotator cuff musculature. Previous surgical scars were absent.
Palpation revealed mild tenderness over the anterior aspect of the glenohumeral joint and the coracoid process. There was no warmth or effusion.
Active range of motion was significantly limited by apprehension, particularly with abduction greater than 90 degrees and external rotation greater than 60 degrees. Passive range of motion was full, but apprehension was elicited at the end-range of abduction and external rotation. Internal rotation was full and pain-free.
Provocative Testing and Instability Assessment
Specific stability tests were performed to isolate the vectors of instability and assess the integrity of the capsulolabral structures:
- Apprehension Test: Strongly positive at 90 degrees of abduction and maximal external rotation. This elicited significant apprehension and a guarding response, indicating insufficiency of the anterior band of the IGHL and probable engagement of a Hill-Sachs lesion over a deficient anterior glenoid rim.
- Relocation Test (Fowler Sign): Positive. The application of a posteriorly directed force on the proximal humerus stabilized the joint, centering the humeral head within the glenoid fossa, and immediately relieved the patient's apprehension, allowing for further external rotation.
- Surprise Test (Anterior Release Test): Positive. Sudden release of the posterior pressure during the relocation test reproduced the patient's severe apprehension and pain, highly specific for anterior instability.
- Load and Shift Test: Demonstrated increased anterior translation (Grade II, humeral head rides over the glenoid rim but spontaneously reduces) compared to the contralateral shoulder, with a palpable clunk upon reduction. Posterior and inferior translation were symmetrical and within normal limits (Grade I).
- Sulcus Sign: Negative, indicating no significant inferior capsular laxity or coracohumeral ligament insufficiency.
- Jobe Relocation Test for Posterior Instability: Negative.
- O'Brien Active Compression Test and Speed Test: Negative, decreasing the likelihood of concomitant superior labral anterior-posterior (SLAP) tears or long head of the biceps tendon pathology.
- Acromioclavicular Joint Compression Test: Negative.
Neurological and Vascular Evaluation
A comprehensive neurovascular examination is mandatory in the setting of recurrent instability to rule out traction neurapraxia, particularly of the axillary and musculocutaneous nerves. Distal pulses (radial, ulnar) were palpable and symmetrical. Capillary refill was less than two seconds. Sensation in the axillary nerve distribution (lateral shoulder badge area), musculocutaneous nerve (lateral forearm), radial, ulnar, and median nerve distributions was intact and symmetrical to the contralateral side. Motor strength was graded 5/5 in all upper extremity muscle groups tested, including the deltoid, biceps brachii, and triceps brachii, although apprehension limited full effort during resisted external rotation. The Beighton score was 0/9, effectively ruling out generalized ligamentous hyperlaxity as a contributing factor to his instability.
Imaging and Diagnostics
Initial plain radiographs obtained in the emergency department at the time of the first dislocation confirmed an anterior glenohumeral dislocation. Post-reduction films showed concentric reduction.
For the current presentation, a new series of standard shoulder radiographs was obtained, including a True Anteroposterior (Grashey view), an Axillary view, and a Scapular Y view.
The Grashey view demonstrated an intact overall glenoid contour but raised high clinical suspicion for a blunting of the anterior-inferior aspect, suggestive of chronic osseous wear. The Axillary view, crucial for evaluating the anterior glenoid rim and posterior humeral head, confirmed a bony Bankart lesion and revealed a moderate Hill-Sachs lesion on the posterior-superior aspect of the humeral head.
Advanced Cross Sectional Imaging CT and MRI
To accurately quantify the degree of bone loss and assess the soft tissue envelope, advanced cross-sectional imaging was indicated.
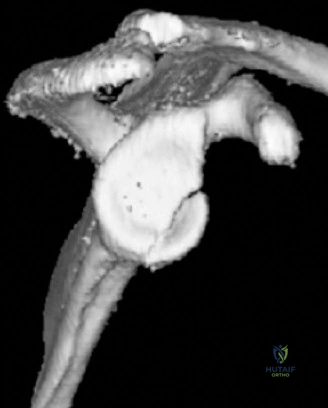
A non-contrast computed tomography (CT) scan with 3D reconstruction with digital subtraction of the humeral head was obtained. This is the gold standard for quantifying glenoid bone loss. Utilizing the best-fit circle method (Pico method) on the en face view of the sagittal reconstructed glenoid, the inferior glenoid circle was drawn based on the intact posterior and inferior margins. The missing anterior chord was measured, revealing a 22% anterior glenoid bone loss. This quantitative measurement is a critical inflection point in surgical decision-making, as it exceeds the generally accepted subcritical threshold of 13.5% to 15%, beyond which soft tissue stabilization alone is associated with unacceptably high failure rates.
Furthermore, the CT scan allowed for detailed evaluation of the Hill-Sachs lesion. The defect was measured for its depth, width, and volume. More importantly, the location of the Hill-Sachs lesion was evaluated in the context of the glenoid track paradigm.

The Glenoid Track Paradigm Application
The glenoid track is defined as the contact zone of the glenoid on the humeral head during maximum abduction and external rotation. The width of this track is approximately 83% of the intact glenoid width. However, in the presence of anterior glenoid bone loss, the glenoid track is narrowed by the exact width of the bony defect.
In this patient, the intact glenoid width was estimated at 28 mm. The 22% bone loss equated to a 6.1 mm defect. The native glenoid track (83% of 28 mm = 23.2 mm) was reduced by 6.1 mm, resulting in a functional glenoid track of 17.1 mm. The Hill-Sachs interval (the distance from the medial margin of the Hill-Sachs lesion to the medial margin of the rotator cuff footprint) was measured at 21 mm. Because the Hill-Sachs interval (21 mm) was greater than the functional glenoid track (17.1 mm), the lesion was classified as an "off-track" Hill-Sachs lesion. An off-track lesion will engage the anterior glenoid rim during abduction and external rotation, acting as a fulcrum to lever the humeral head out of the joint, guaranteeing failure of an isolated arthroscopic Bankart repair.
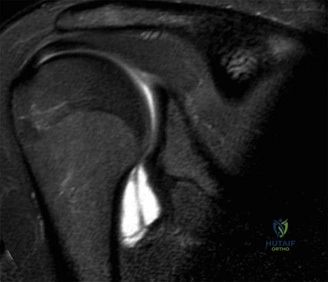
Magnetic Resonance Arthrography Evaluation
Magnetic Resonance Arthrography (MRA) was also performed to evaluate the capsulolabral complex, rotator cuff, and articular cartilage. The MRA confirmed the complete avulsion of the anterior-inferior labrum with a periosteal sleeve avulsion, but without significant medial displacement (ruling out an ALPSA lesion). The anterior band of the IGHL was attenuated but remained attached to the humeral neck, ruling out a Humeral Avulsion of the Glenohumeral Ligament (HAGL) lesion. The rotator cuff tendons were intact, and there was no evidence of significant chondral delamination or osteoarthritis (Kellgren-Lawrence Grade 0).
Differential Diagnosis
When evaluating a young athlete with recurrent shoulder instability, it is imperative to differentiate between traumatic structural instability, atraumatic multidirectional instability, and specific capsuloligamentous avulsion variants, as the surgical management differs drastically.
| Differential Diagnosis | Pathophysiology and Mechanism | Key Clinical Findings | Imaging Characteristics |
|---|---|---|---|
| Traumatic Anterior Instability with Bony Bankart (Working Diagnosis) | High-energy trauma (abduction/external rotation) causing failure of the anterior-inferior capsulolabral complex and fracture/attrition of the anterior glenoid rim. | Unidirectional anterior instability. Positive apprehension/relocation tests. History of distinct traumatic dislocation event. | MRI: Anteroinferior labral tear. CT: Anterior glenoid bone loss (>15-20%) and concomitant Hill-Sachs lesion. |
| Multidirectional Instability MDI | Atraumatic or microtraumatic etiology. Generalized capsular redundancy and altered neuromuscular control. Often associated with generalized hyperlaxity. | Instability in multiple planes (anterior, posterior, inferior). Positive sulcus sign. Positive Beighton score. Lack of a single major traumatic event. | MRI: Increased capsular volume, patulous inferior pouch. Absence of discrete labral tears or significant bone loss. |
| Humeral Avulsion of Glenohumeral Ligament HAGL | Traumatic hyperabduction and external rotation. The IGHL complex tears at its humeral insertion rather than the glenoid origin. | Similar presentation to Bankart tears. Persistent anterior instability despite previous successful labral repair. | MRI Arthrography: "J-sign" or "U-sign" indicating contrast extravasation into the axillary pouch due to avulsion of the IGHL from the humeral neck. |
| Anterior Labroligamentous Periosteal Sleeve Avulsion ALPSA | Traumatic anterior dislocation where the torn anteroinferior labrum and intact anterior scapular periosteum strip and displace medially and inferiorly on the glenoid neck. | High rate of recurrence. Often heals in a medially displaced position, resulting in an incompetent anterior bumper. | MRI: Medially displaced labrum scarred down to the anterior glenoid neck. Absence of a discrete cleft between the labrum and the glenoid rim. |
| Posterior Glenohumeral Instability | Axial load to an adducted, flexed, and internally rotated arm (e.g., blocking in American football, seizures, electrocution). | Posterior shoulder pain. Positive Jerk test and Kim test. Decreased external rotation if locked posterior dislocation is present. | MRI: Posterior labral tear (Reverse Bankart), reverse Hill-Sachs lesion (McLaughlin lesion) on the anteromedial humeral head. |
Surgical Decision Making and Classification
The surgical decision-making process in this case is driven by the patient's demographic profile, the chronicity of the instability, the specific sport he plays, and the objective quantification of his osseous defects.
Instability Severity Index Score Application
The Instability Severity Index Score (ISIS), developed by Boileau et al., is a validated preoperative scoring system used to predict the risk of recurrence following an isolated arthroscopic Bankart repair. The score is calculated out of 10 points:
* Age under 20 years at the time of surgery (2 points) - Patient is 28 (0 points)
* Participation in competitive sports (2 points) - Yes (2 points)
* Participation in contact/forced overhead sports (1 point) - Rugby (1 point)
* Shoulder hyperlaxity / Anterior/inferior hyperlaxity (1 point) - No (0 points)
* Hill-Sachs lesion visible on AP radiograph in external rotation (2 points) - Yes (2 points)
* Loss of sclerotic contour of the anterior glenoid on AP radiograph (2 points) - Yes (2 points)
This patient's ISIS score is 7 out of 10. A score greater than 3 suggests an unacceptably high recurrence rate (up to 70%) with arthroscopic soft-tissue stabilization alone. A score of 7 heavily mandates a bone-block augmentation procedure.
Critical Bone Loss and the Bipolar Defect
Historically, glenoid bone loss greater than 20% to 25% was considered the absolute indication for a bony augmentation procedure. However, recent biomechanical and clinical outcome studies have shifted this paradigm toward a "subcritical" bone loss threshold of 13.5% to 15%, particularly in high-demand contact athletes. At 22% glenoid bone loss, this patient is well beyond both the subcritical and critical thresholds.
Furthermore, the patient presents with a bipolar bone defect—both a glenoid defect and a humeral head defect (Hill-Sachs). The application of the glenoid track concept confirmed an "off-track" lesion. While an arthroscopic Bankart repair combined with a Remplissage procedure (capsulotenodesis of the infraspinatus into the Hill-Sachs defect) can convert an off-track lesion to an on-track lesion, this approach is contraindicated in the setting of >15% glenoid bone loss. Remplissage addresses the humeral side but does not restore the articular arc of the glenoid, which is critical for stability in a contact athlete.
Rationale for Open Latarjet Procedure
Given the 22% glenoid bone loss, the off-track Hill-Sachs lesion, the high ISIS score, and the patient's occupation as an elite rugby player, an open Latarjet procedure (coracoid transfer) is the gold standard intervention.
The Latarjet procedure provides a "triple-blocking effect" as described by Patte:
1. Bone Block Effect: The transferred coracoid process extends the anterior-posterior width of the glenoid, restoring the articular arc and converting the off-track Hill-Sachs lesion back to an on-track lesion.
2. Sling Effect: The conjoint tendon (short head of the biceps and coracobrachialis), which remains attached to the transferred coracoid, acts as a dynamic muscular sling across the anterior-inferior capsule when the arm is abducted and externally rotated, physically blocking anterior translation of the humeral head.
3. Capsular Repair Effect: The stump of the coracoacromial (CA) ligament, left attached to the coracoid graft, is sutured to the native anterior capsule, reconstructing the capsulolabral complex.
Alternative bone block procedures, such as the Eden-Hybinette (iliac crest bone graft) or distal tibial allograft, were considered. However, these procedures only provide a static bone block without the dynamic sling effect of the conjoint tendon, which is highly beneficial in collision athletes. Therefore, the open Latarjet procedure was selected as the definitive treatment plan.
Surgical Technique and Intervention
The patient was medically cleared and optimization was confirmed. Regional anesthesia was achieved via an interscalene nerve block, followed by the induction of general anesthesia.
Patient Positioning and Preparation
The patient was positioned in the modified beach-chair position with the head secured and the operative arm draped free, resting on an articulating arm positioner. Care was taken to ensure the medial border of the scapula was supported but the posterior glenohumeral joint was free to allow for posterior pressure during reduction and graft positioning. A standard surgical timeout was performed. Prophylactic intravenous antibiotics (Cefazolin 2g) were administered prior to incision.
Deltopectoral Approach and Coracoid Harvest
A 5 to 7 cm longitudinal incision was made starting from the tip of the coracoid process extending distally toward the axillary fold. Subcutaneous tissues were dissected, and the deltopectoral interval was identified by the cephalic vein. The vein was mobilized laterally with the deltoid to preserve its venous drainage, and the interval was developed. The clavipectoral fascia was incised, exposing the conjoint tendon and the coracoid process.
The coracoacromial (CA) ligament was identified and sharply detached from its acromial insertion, leaving a generous 1 cm stump attached to the lateral aspect of the coracoid for later capsular repair. The pectoralis minor tendon was identified at its insertion on the medial aspect of the coracoid. To maximize the length of the coracoid graft, the pectoralis minor was sharply elevated off the bone.
The coracoid process was then prepared for osteotomy. The inferior surface of the coracoid was cleared of soft tissue, taking extreme care to identify and protect the musculocutaneous nerve, which typically enters the conjoint tendon 3 to 5 cm distal to the coracoid tip. A specialized angled oscillating saw was used to perform the osteotomy at the base (the "knee") of the coracoid, yielding a graft approximately 2.5 to 3 cm in length.
Graft Preparation
The harvested coracoid graft was meticulously prepared on the back table. The inferior surface of the coracoid (which would become the articular surface) was decorticated using a high-speed burr to expose bleeding cancellous bone, optimizing the environment for osseous union. Two drill holes (typically 4.0 mm) were placed centrally along the longitudinal axis of the graft, spaced 1 cm apart, using a specialized drill guide to ensure parallel trajectory. Top hats (cannulated washers) were inserted into the drill holes to prevent screw head cut-out during final fixation.
Subscapularis Approach and Glenoid Preparation
Attention was returned to the glenohumeral joint. The subscapularis muscle was managed via a muscle-splitting approach rather than a tenotomy to preserve the integrity of the tendon, which is crucial for early rehabilitation and return to sport in athletes. A horizontal split was created at the junction of the middle and inferior thirds of the subscapularis muscle belly. The split was maintained with a self-retaining retractor (e.g., a modified Gelpi or Fukuda retractor).
The underlying anterior joint capsule was identified. A vertical capsulotomy was performed near the glenoid rim. The joint was inspected, confirming the massive anterior labral tear and significant bony deficiency. The anterior glenoid neck was thoroughly prepared. All remnant labral tissue and periosteum were excised, and the anterior glenoid neck was decorticated with a high-speed burr and osteotomes to create a flat, bleeding cancellous bone bed to match the prepared surface of the coracoid graft. Perfect congruency between the graft and the glenoid neck is paramount to prevent non-union.
Graft Positioning and Fixation Construct
The coracoid graft was introduced through the subscapularis split. Positioning of the graft is the most critical step of the procedure. The graft must be placed perfectly flush with the articular cartilage of the glenoid. If the graft is placed too laterally (proud), it will cause rapid and severe glenohumeral osteoarthritis. If placed too medially, it will fail to restore the articular arc and the bone block effect will be lost. Furthermore, the graft must be positioned inferiorly, strictly below the equator of the glenoid (typically between the 2 o'clock and 5 o'clock positions for a right shoulder), to effectively block the dislocation vector.
Once optimal positioning was achieved and temporarily held with K-wires, the graft was fixed to the native glenoid using two 3.75 mm partially threaded cannulated titanium malleolar screws. The screws were directed strictly parallel to the articular surface to avoid joint penetration. Compression across the osteotomy site was confirmed visually and tactilely.
Capsulolabral Reconstruction and Closure
Following rigid fixation of the bone block, the capsular repair was performed. The native anterior capsule was repaired to the stump of the CA ligament that was preserved on the coracoid graft using high-strength non-absorbable sutures. This effectively renders the bone graft extra-articular, preventing direct contact between the humeral head cartilage and the raw cancellous bone of the graft during the healing phase, and restores the anterior capsular tension.
The subscapularis split was allowed to close naturally; no sutures were placed in the muscle belly to avoid tethering. The deltopectoral interval was irrigated copiously. Subcutaneous tissues were closed in layers with absorbable sutures, and the skin was closed with a subcuticular running suture. A sterile dressing and a shoulder immobilizer sling were applied in the operating room.
Post Operative Protocol and Rehabilitation
The postoperative rehabilitation following a Latarjet procedure is heavily dependent on the protection of the subscapularis split and the osseous union of the coracoid graft. The protocol is divided into distinct, progressive phases.
Phase 1 Immediate Postoperative Immobilization Weeks 0 to 4
The primary goal of this phase is to protect the surgical construct, manage pain and inflammation, and promote initial tissue healing.
* Immobilization: The patient is strictly immobilized in a sling with an abduction pillow for 4 weeks, removing it only for hygiene and specific exercises.
* Range of Motion: Passive range of motion (PROM) is initiated immediately but strictly limited. Forward flexion is limited to 90 degrees. External rotation is strictly limited to neutral (0 degrees) to protect the subscapularis split and the anterior capsular repair. Internal rotation is allowed to the chest.
* Strengthening: Grip strengthening, active wrist/elbow ROM, and gentle submaximal isometric exercises for the deltoid and periscapular musculature are encouraged. No active internal rotation is permitted.
Phase 2 Intermediate Range of Motion Weeks 5 to 8
The focus shifts to restoring full passive and active-assisted range of motion while continuing to protect the healing bone graft. Radiographs are obtained at 6 weeks to assess graft position and early signs of union.
* Immobilization: The sling is discontinued at 4 to 5 weeks.
* Range of Motion: Progression to full active-assisted and active range of motion (AROM) in all planes. External rotation is gradually progressed, aiming for 30 to 40 degrees by week 6, and full ER by week 8.
* Strengthening: Initiation of light isotonic strengthening for the rotator cuff and periscapular stabilizers. Closed kinetic chain exercises are introduced to enhance proprioception and joint stability. Scapular dyskinesia, common after prolonged immobilization, is aggressively addressed with targeted motor control exercises.
Phase 3 Strengthening and Neuromuscular Control Weeks 9 to 16
Assuming radiographic evidence of coracoid graft incorporation, the rehabilitation becomes more aggressive, focusing on strength, power, and dynamic stability.
* Range of Motion: Full, symmetric AROM should be achieved.
* Strengthening: Progressive resistance exercises for all shoulder girdle musculature. Emphasis is placed on the subscapularis, which was violated during the approach, and the dynamic stabilizers. Plyometric exercises (e.g., medicine ball throws) are introduced late in this phase to train the stretch-shortening cycle.
Phase 4 Advanced Sport Specific Rehabilitation and Return to Play Months 4 to 6
The final phase bridges the gap between clinical rehabilitation and the demands of elite-level rugby.
* Sport-Specific Drills: Introduction of contact progressions, tackling mechanics, and sport-specific agility drills.
* Return to Play Criteria: Return to competitive rugby is not time-based alone but criterion-based. The patient must demonstrate:
1. Radiographic confirmation of complete coracoid graft union.
2. Full, pain-free range of motion.
3. Isokinetic strength testing demonstrating at least 90% strength of the rotator cuff and deltoid compared to the uninjured contralateral side.
4. Successful completion of a functional testing algorithm (e.g., Closed Kinetic Chain Upper Extremity Stability Test).
5. Psychological readiness and absence of apprehension during
