Crack the Case: Bony Bankart Hillsachs Shoulder Injuries
Key Takeaway
Your ultimate guide to Crack the Case: Bony Bankart Hillsachs Shoulder Injuries starts here. Traumatic anterior shoulder instability is common in young athletes, carrying a high recurrence risk. Recurrent episodes significantly increase arthritis risk, mandating aggressive treatment. Comprehensive evaluation for persistent instability often includes assessing for critical bony defects, such as a **bony bankart hillsachs** lesion, which are key determinants for effective management and preventing future dislocations.
Patient Presentation and History
A 28-year-old male, a semi-professional rugby player, presents to the emergency department following a high-energy traumatic anterior shoulder dislocation. The mechanism of injury involved a direct tackle with his arm in an abducted and externally rotated position, resulting in immediate pain, loss of function, and a visibly deformed shoulder. This is his first documented shoulder dislocation. He reports a "clunk" sensation followed by excruciating pain. He was unable to move his arm and supported it with his contralateral limb.
His medical history is unremarkable. He denies any prior shoulder instability, pain, or significant trauma to the affected limb. He is a non-smoker and consumes alcohol socially. There are no known allergies, and he is not on any regular medications. His primary goal is to return to competitive rugby at his pre-injury level.
The biomechanics of this specific injury pattern in collision athletes are well-documented in orthopedic trauma literature. The combination of forced abduction, external rotation, and extension applies maximal tensile stress to the inferior glenohumeral ligament complex and the anteroinferior labrum. When the applied force exceeds the ultimate tensile strength of these static stabilizers, structural failure occurs, often resulting in capsulolabral avulsion and, in high-energy scenarios, osseous failure of the glenoid rim and impaction of the posterolateral humeral head against the dense cortical bone of the anterior glenoid vault. Given the patient's age and participation in a high-demand collision sport, the pre-test probability for significant structural damage, including bipolar bone loss, is exceedingly high.
Clinical Examination Findings
Upon initial inspection in the emergency department, the left shoulder exhibited the classic "shoulder pad" sign, indicative of an anterior glenohumeral dislocation, with prominence of the acromion and flattening of the deltoid contour anteriorly. The humeral head was palpable anteriorly and inferiorly, beneath the coracoid process. Ecchymosis was noted around the shoulder girdle, extending down the upper arm. There was no open wound or obvious skin compromise.
Palpation revealed significant tenderness globally around the glenohumeral joint. The patient guarded against any movement due to severe pain. Distal neurovascular status was assessed immediately. Radial, ulnar, and median pulses were 2+ bilaterally and symmetrically. Capillary refill was brisk in all digits.
Neurological assessment was crucial given the risk of axillary nerve injury. Sensation over the lateral deltoid patch was diminished (hypoesthesia) but not absent, suggesting a neuropraxia. Deltoid contraction was difficult to assess due to pain and guarding, but the patient could weakly abduct the arm against minimal resistance, indicating some axillary nerve sparing. Biceps, triceps, and wrist/finger flexor/extensor strength were intact and symmetric to the contralateral side.
Following initial reduction in the emergency department, which was performed under conscious sedation, the patient's pain significantly improved. Post-reduction examination demonstrated the following:
- Inspection: Normal shoulder contour restored, but swelling and ecchymosis persisted.
- Palpation: Diffuse tenderness around the glenohumeral joint, particularly anteriorly and inferiorly. No crepitus with gentle motion.
- Range of Motion:
- Passive Range of Motion: Forward flexion to 90 degrees (pain-limited), abduction to 70 degrees (pain-limited), external rotation to 0 degrees (markedly limited by apprehension), internal rotation to T8 level (pain-limited).
- Active Range of Motion: Significantly restricted across all planes due to pain and apprehension.
- Special Tests for Instability:
- Apprehension Test: Markedly positive with the arm in abduction and external rotation, reproducing the patient's fear of re-dislocation.
- Relocation Test: Relief of apprehension with posterior translation pressure on the humeral head.
- Load and Shift Test: Demonstrated increased anterior translation (Grade II, 50% translation without subluxation over glenoid rim) with a firm endpoint. Posterior and inferior translation were within normal limits.
- Sulcus Sign: Negative, ruling out significant inferior or multidirectional instability.
- Neurological Assessment Post Reduction: Hypoesthesia in the lateral deltoid patch persisted. Deltoid strength remained 3/5 against gravity, with subjective weakness. Remaining motor and sensory functions were normal. This indicated a persistent, likely neuropraxic, axillary nerve injury, warranting close monitoring and electromyography if no improvement is noted at the six-week interval.
Imaging and Diagnostics
Radiographic Evaluation
Immediate post-reduction radiographs were obtained to confirm concentric reduction and evaluate for osseous pathology. The standard trauma series included a true anteroposterior Grashey view, a scapular Y view, and an axillary lateral view.
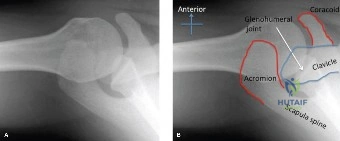
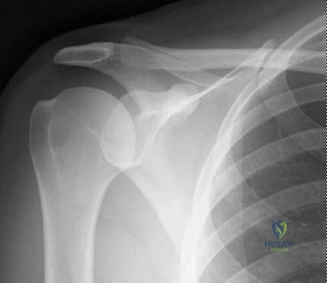
The Grashey view confirmed concentric reduction of the glenohumeral joint with no evidence of superior migration of the humeral head, suggesting an intact rotator cuff. However, close inspection of the anteroinferior glenoid rim revealed a distinct sclerotic line and a small, displaced osseous fragment, pathognomonic for a bony Bankart lesion. Furthermore, an internal rotation anteroposterior view demonstrated a dense vertical line in the superolateral aspect of the humeral head, representing a Hill-Sachs impaction fracture. The axillary lateral view corroborated the presence of the anterior glenoid rim fracture, showing a deficiency in the normal pear-shaped contour of the inferior glenoid.
Advanced Cross Sectional Imaging
Given the radiographic evidence of bipolar bone loss (bony Bankart and Hill-Sachs lesion) in a high-demand collision athlete, a non-contrast computed tomography scan with three-dimensional reconstructions was mandated to precisely quantify the osseous defects.

The CT scan utilizing the Pico surface area method, which involves a best-fit circle drawn on the inferior portion of the glenoid on the en face sagittal view, revealed a 22% anterior glenoid bone loss. The fragment was comminuted and non-reconstructable. Furthermore, axial and coronal reconstructions were utilized to evaluate the Hill-Sachs lesion. The impaction fracture was measured for depth, width, and length.
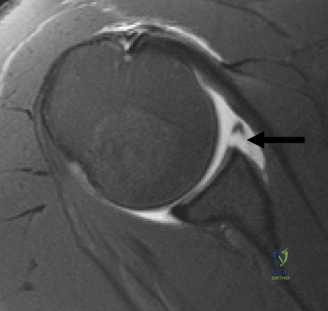
To fully assess the soft tissue envelope, a Magnetic Resonance Arthrogram was subsequently performed. The MRA confirmed a complete avulsion of the anteroinferior capsulolabral complex extending from the 3 o'clock to the 6 o'clock position. The inferior glenohumeral ligament was stripped from the glenoid neck, consistent with an anterior labroligamentous periosteal sleeve avulsion variant. The rotator cuff tendons were contiguous and demonstrated no full-thickness or high-grade partial-thickness tearing. The long head of the biceps tendon was centered within the bicipital groove without evidence of superior labrum anterior and posterior pathology.
Differential Diagnosis
The presentation of acute traumatic anterior shoulder instability requires a comprehensive evaluation to differentiate between isolated soft tissue lesions, complex osseous defects, and associated neurovascular or tendinous injuries. The following table outlines the primary differential diagnoses considered for this patient profile.
| Diagnostic Consideration | Pathophysiology and Mechanism | Key Clinical Findings | Imaging Characteristics |
|---|---|---|---|
| Bipolar Bone Loss Instability | Concomitant bony Bankart (glenoid rim fracture) and Hill-Sachs (humeral head impaction) lesions resulting from high-energy anterior dislocation. | Severe apprehension at lower degrees of abduction/external rotation. High risk of recurrent instability. | 3D CT shows >15-20% glenoid bone loss and an engaging or off-track Hill-Sachs lesion. |
| Isolated Soft Tissue Bankart | Avulsion of the anterior labrum and anterior band of the inferior glenohumeral ligament without significant osseous involvement. | Positive apprehension and relocation tests. Classic presentation in lower-energy dislocations. | MRI/MRA shows labral detachment at the anteroinferior quadrant. CT shows intact glenoid vault. |
| Humeral Avulsion of Glenohumeral Ligament | Avulsion of the inferior glenohumeral ligament complex from its humeral insertion rather than the glenoid origin. | Often presents with significant inferior capsular laxity. Can occur with or without concurrent labral pathology. | MRA demonstrates a "J-sign" with contrast extravasation into the axillary pouch along the humeral neck. |
| Rotator Cuff Tear with Dislocation | Disruption of the rotator cuff tendons (most commonly supraspinatus/infraspinatus in older patients, subscapularis in younger athletes) during dislocation. | Significant weakness in external rotation or elevation post-reduction. "Dead arm" sensation distinct from axillary neuropraxia. | MRI reveals discontinuity of the rotator cuff footprint. Plain films may show superior humeral head migration. |
Surgical Decision Making and Classification
The management of anterior shoulder instability in a young, competitive collision athlete with documented bipolar bone loss represents one of the most challenging paradigms in orthopedic sports medicine. Non-operative management in this demographic yields an unacceptably high recurrence rate, often exceeding 80%, and leads to progressive glenohumeral chondrolysis and further osseous attrition. Therefore, operative intervention is definitively indicated.
The Instability Severity Index Score
To objectify the surgical decision-making process, the Instability Severity Index Score was calculated. This patient scores highly: age under 20 at first dislocation (0 points, as he is 28), participation in competitive sports (2 points), participation in contact/collision sports (1 point), hyperlaxity (0 points), Hill-Sachs lesion visible on AP radiograph (2 points), and glenoid loss visible on AP radiograph (2 points). A score of 7 heavily favors an open bony augmentation procedure over an arthroscopic soft tissue repair, as the failure rate of arthroscopic Bankart repair in patients with an ISIS score greater than 6 approaches 70%.
The Glenoid Track Paradigm
The critical determinant in this case is the interaction between the glenoid bone loss and the humeral head defect, known as the Glenoid Track concept. The glenoid track is defined as the contact zone of the glenoid on the humeral head during maximum abduction and external rotation. It is calculated as 83% of the intact glenoid width minus the measured anterior glenoid bone loss.
If the medial margin of the Hill-Sachs lesion falls outside this calculated track, the lesion is deemed "off-track," meaning it will engage the anterior glenoid rim, levering the humeral head out of the joint. In this patient, the 22% glenoid bone loss significantly narrows the glenoid track. Measurements from the 3D CT confirmed that the medial margin of his Hill-Sachs lesion extended medial to the calculated track, classifying this as an off-track lesion.
An arthroscopic Bankart repair alone in an off-track scenario is biomechanically insufficient and carries a prohibitive risk of failure. While an arthroscopic Bankart combined with a Remplissage (infraspinatus tenodesis into the Hill-Sachs defect) can convert an off-track lesion to an on-track lesion, the magnitude of the glenoid bone loss (22%) in a rugby player mandates restoration of the anterior glenoid arc. Therefore, a Latarjet procedure (coracoid transfer) is the gold standard treatment for this specific clinical presentation.
The Latarjet procedure provides a "triple-blocking" effect:
1. Bone Block Effect: Restores the anteroinferior glenoid articular arc, effectively widening the glenoid track and preventing Hill-Sachs engagement.
2. Sling Effect: The conjoint tendon (short head of biceps and coracobrachialis) acts as a dynamic sling across the anteroinferior capsule when the arm is abducted and externally rotated, resisting anterior translation.
3. Capsular Repair: The capsule is repaired to the stump of the coracoacromial ligament, restoring the static anterior restraint.
Surgical Technique and Intervention
Patient Positioning and Setup
The patient is taken to the operating room and placed in the modified beach chair position after the administration of general anesthesia and an interscalene regional nerve block for postoperative analgesia. The head is secured in a neutral position, ensuring the cervical spine is not hyperextended or laterally flexed. The operative left upper extremity is prepped and draped in a standard sterile fashion, allowing for full, unencumbered manipulation of the arm. A pneumatic arm positioner is utilized to maintain the limb in varying degrees of abduction and rotation throughout the procedure.
Deltopectoral Approach and Coracoid Harvest
A standard deltopectoral incision is made, beginning at the tip of the coracoid process and extending distally and laterally toward the deltoid tuberosity, approximately 7 centimeters in length. The cephalic vein is identified and retracted laterally with the deltoid muscle to preserve its venous drainage, while the pectoralis major is retracted medially. The clavipectoral fascia is incised, exposing the conjoint tendon and the coracoid process.
The coracoacromial ligament is identified and transected approximately 1 centimeter from its coracoid insertion; this stump is meticulously preserved for the later capsular repair. The pectoralis minor tendon is identified on the medial aspect of the coracoid. Using electrocautery, the pectoralis minor is sharply elevated off the medial coracoid.

The coracoid osteotomy is a critical step. A 90-degree oscillating saw is used to perform the osteotomy at the base of the coracoid process, just distal to the coracoclavicular ligaments, ensuring a graft length of at least 2.5 to 3 centimeters. The osteotomized coracoid, with the conjoint tendon still attached, is mobilized. The inferior surface of the coracoid is decorticated using a high-speed burr to expose a flat, bleeding cancellous bone bed. This surface will ultimately interface with the anterior glenoid. Two 3.2-millimeter drill holes are placed centrally in the coracoid graft, spaced approximately 1 centimeter apart, using a specialized drill guide to ensure parallel trajectory.
Glenoid Preparation and Graft Fixation
Attention is then turned to the subscapularis muscle. To expose the anterior capsule and glenoid, a subscapularis split is performed in line with its fibers, typically at the junction of the superior two-thirds and inferior one-third. This split minimizes disruption to the muscular architecture compared to a formal tenotomy and preserves the inferior tendinous band. A self-retaining retractor is placed within the split.
The anterior capsule is incised vertically, and a capsular flap is created. A Fukuda retractor is placed intra-articularly to displace the humeral head posteriorly and laterally, providing excellent visualization of the anteroinferior glenoid. The labral remnants and the small bony Bankart fragment are excised. The anterior glenoid neck, from the 2 o'clock to the 6 o'clock position, is aggressively decorticated with a burr to create a flat, congruent bleeding bone bed that matches the prepared surface of the coracoid graft.
The prepared coracoid graft is passed through the subscapularis split. The graft is positioned flush with the articular cartilage of the glenoid. It is imperative that the graft is not placed proud (lateral) to the cartilage surface, as this will lead to rapid and devastating glenohumeral osteoarthritis. Conversely, if placed too medially, the bone block effect is negated.
Once optimal positioning is confirmed visually and palpably, two 1.5-millimeter guide wires are advanced through the pre-drilled holes in the coracoid and into the glenoid vault, aiming parallel to the articular surface. The glenoid is drilled with a 3.2-millimeter drill, and the lengths are measured. Two 3.75-millimeter partially threaded, cannulated titanium screws are inserted to achieve rigid interfragmentary compression.
Capsular Repair and Closure
Following rigid fixation of the graft, the intra-articular retractors are removed. The arm is taken through a full range of motion under direct visualization to confirm that the humeral head remains concentrically reduced and does not impinge upon the graft during internal rotation. The native anterior capsule is then repaired to the preserved stump of the coracoacromial ligament using non-absorbable sutures. This step re-establishes the anterior capsular restraint and places the bone graft in an extra-articular position, further protecting the humeral articular cartilage.
The subscapularis split is allowed to fall back together and is loosely approximated with absorbable sutures. The deltopectoral interval is irrigated copiously. Subcutaneous tissues are closed with interrupted inverted absorbable sutures, and the skin is closed with a running subcuticular stitch. The patient is placed in a neutral rotation shoulder immobilizer prior to extubation.
Post Operative Protocol and Rehabilitation
The postoperative rehabilitation following a Latarjet procedure is heavily dictated by the need to protect the osseous healing of the coracoid graft and the soft tissue healing of the subscapularis split, while preventing postoperative stiffness. The protocol is divided into four distinct phases.
Phase 1: Maximum Protection (Weeks 0-4)
The primary goal during this phase is to protect the surgical construct and manage pain and inflammation. The patient is strictly immobilized in a sling for four weeks. Pendulum exercises are initiated immediately. Passive range of motion is instituted under the guidance of a physical therapist, with strict limitations: forward flexion is limited to 90 degrees, and external rotation is limited to 0 degrees (neutral) to protect the subscapularis split and avoid tension on the conjoint tendon. Internal rotation is permitted to the chest wall. Active elbow, wrist, and hand range of motion are encouraged.
Phase 2: Moderate Protection and Active Motion (Weeks 4-8)
At four weeks, the sling is discontinued. Active-assisted and active range of motion exercises are initiated. Forward flexion is advanced as tolerated. External rotation is gradually increased by 10 to 15 degrees per week, aiming for symmetric external rotation by week 8. Submaximal isometric exercises for the rotator cuff and deltoid are introduced. Isotonic strengthening of the periscapular stabilizers (rhomboids, trapezius, serratus anterior) is emphasized to establish a stable base for glenohumeral mechanics.
Phase 3: Early Strengthening (Weeks 8-16)
Radiographic evaluation is performed at the 8-week mark to confirm graft incorporation and absence of hardware complications. Once osseous union is progressing satisfactorily, progressive resistive exercises are initiated. Rotator cuff strengthening transitions from isometric to isotonic using resistance bands and light weights. Proprioceptive neuromuscular facilitation exercises are integrated. The focus shifts to restoring dynamic stability and neuromuscular control of the shoulder girdle.
Phase 4: Advanced Strengthening and Return to Sport (Months 4-6)
This phase bridges the gap between clinical rehabilitation and athletic performance. Plyometric exercises and sport-specific drills are introduced. For this rugby player, tackling drills, rucking simulations, and overhead passing mechanics are progressively loaded. Return to competitive collision sports is strictly prohibited until at least 5 to 6 months postoperatively. Criteria for return to play include:
1. Radiographic evidence of complete coracoid graft union.
2. Full, pain-free active range of motion symmetric to the contralateral side.
3. Isokinetic strength testing demonstrating at least 90% strength of the rotator cuff and deltoid compared to the uninjured limb.
4. Successful completion of a functional sport-specific testing protocol without apprehension or compensatory mechanics.
Clinical Pearls and Pitfalls
Pearls for Success
- Graft Positioning is Paramount: The classic "flush" positioning of the coracoid graft cannot be overstated. The graft should be positioned exactly flush with the native glenoid cartilage, or a maximum of 1 millimeter medial to it. Utilizing a smooth elevator to palpate the transition between the graft and the cartilage ensures accurate placement.
- Subscapularis Management: Utilizing a subscapularis split rather than a tenotomy significantly reduces postoperative subscapularis weakness and accelerates the rehabilitation timeline. It also maintains the inferior tendinous band, which provides an additional buttress against anterior translation.
- Screw Trajectory: The screws must be placed parallel to the glenoid articular surface to avoid intra-articular penetration. A trajectory that is too medial risks neurovascular injury in the suprascapular notch, while a trajectory that is too lateral violates the joint space.
Pitfalls and Complications
- Neurological Injury: The musculocutaneous nerve typically enters the coracobrachialis muscle 3 to 5 centimeters distal to the tip of the coracoid. Aggressive distal retraction of the conjoint tendon must be avoided to prevent a traction neuropraxia. The axillary nerve is at risk during inferior capsular release and glenoid preparation; a blunt retractor should always be placed inferiorly to protect it.
- Graft Osteolysis and Non-union: Inadequate decortication of the coracoid or glenoid, or failure to achieve rigid interfragmentary compression, can lead to graft non-union or resorption. Utilizing partially threaded screws to achieve compression is mandatory.
- Overhanging Graft: A graft placed proud (lateral) to the articular surface will act as a mechanical abrasive against the humeral head. This is the most common iatrogenic cause of rapid-onset, severe glenohumeral osteoarthritis following a Latarjet procedure and often necessitates early hardware removal and potential arthroplasty in severe cases.
