Proximal Femoral Varus Osteotomy with 90-Degree Blade Plate: An Intraoperative Masterclass
Key Takeaway
Join us in the operating theater for a masterclass on proximal femoral varus osteotomy using a 90-degree blade plate. We'll meticulously cover patient selection, comprehensive preoperative planning, intricate surgical anatomy, and a granular, real-time breakdown of every intraoperative step. Learn essential pearls, avoid common pitfalls, and understand critical postoperative management for optimal patient outcomes. This guide is designed for surgical fellows seeking to master this complex procedure.
Comprehensive Introduction and Patho-Epidemiology
The Proximal Femoral Varus Osteotomy (PFVO) employing a 90-degree fixed-angle blade plate remains one of the most powerful, versatile, and enduring procedures in the armamentarium of the reconstructive and pediatric orthopedic surgeon. While newer modular implant systems and locking plates have entered the market, the 90-degree blade plate offers unparalleled biomechanical stability, rigid internal fixation, and a highly predictable union rate when executed with precision. This procedure is fundamentally designed to reorient the proximal femur in the coronal, sagittal, and axial planes simultaneously, addressing complex three-dimensional deformities with a single, elegant mechanical solution. By altering the proximal femoral geometry, the surgeon profoundly influences the mechanical environment of the hip joint, directly impacting long-term joint survival, functional kinematics, and patient quality of life.
Understanding the patho-epidemiology driving the need for this procedure is critical for appropriate patient selection. The normal development of the proximal femur is a dynamic process governed by the mechanical forces exerted across the hip joint during weight-bearing and muscular contraction. In the typically developing child, the femoral neck-shaft angle (NSA) steadily decreases from approximately 150 degrees at birth to a mature angle of 120 to 135 degrees. Concurrently, femoral anteversion decreases from roughly 40 degrees to 10-15 degrees. However, in the presence of altered neuromuscular tone—such as in cerebral palsy, myelomeningocele, or spinal muscular atrophy—the lack of normal, balanced muscular forces and delayed or absent weight-bearing disrupts this physiological remodeling. The result is a persistent coxa valga and excessive femoral anteversion, a combination that biomechanically drives the femoral head laterally and anteriorly out of the acetabulum.
This lateral migration is quantified radiographically using the Reimers Migration Percentage (RMP). As the RMP increases beyond 33%, the risk of progressive subluxation accelerates, eventually culminating in a painful, rigid, and dislocated hip if left untreated. The PFVO directly counters this pathophysiology. By varusizing the proximal femur, the procedure medializes the femoral shaft relative to the head, improves the articular containment within the acetabular dome, and optimizes the abductor moment arm. Furthermore, the derotational component of the osteotomy corrects the excessive anteversion, centering the femoral head within the true acetabulum during the normal stance phase of gait. Beyond neuromuscular dysplasia, this procedure is equally critical in the management of developmental dysplasia of the hip (DDH), Legg-Calvé-Perthes disease, and post-traumatic or congenital coxa valga, making mastery of this technique an absolute prerequisite for any surgeon managing complex hip pathology.
Detailed Surgical Anatomy and Biomechanics
A profound, three-dimensional understanding of proximal femoral anatomy is non-negotiable for the safe and effective execution of a 90-degree blade plate osteotomy. The proximal femur is not merely a cylinder of bone; it is a complex, anisotropic structure engineered to withstand massive bending and torsional loads. The primary osseous landmarks dictate our surgical orientation. The greater trochanter serves as the lateral pillar, its tip normally aligning with the center of the femoral head. In pathologic coxa valga, the trochanter may sit relatively distal, altering the resting length and tension of the abductor musculature. The lesser trochanter, located posteromedially, is the robust insertion site for the iliopsoas tendon. During a varus osteotomy, particularly a medial closing wedge, the spatial relationship of the lesser trochanter is altered, which can profoundly affect hip flexion mechanics and may necessitate a concurrent psoas tenotomy to prevent postoperative flexion contractures.
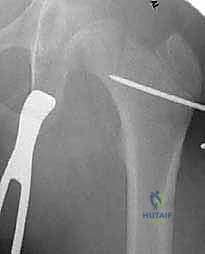
Perhaps the most critical internal anatomical structure for this specific procedure is the calcar femorale. This dense, vertically oriented plate of cortical bone arises from the posteromedial aspect of the femoral shaft and radiates proximally into the posterior portion of the femoral neck. The calcar acts as the primary compressive strut of the proximal femur. When utilizing a 90-degree blade plate, the seating chisel and the subsequent blade must be driven precisely into the femoral neck without violating the medial or inferior calcar. If the blade breaches the calcar, the structural integrity of the fixation is catastrophically compromised, massively increasing the risk of mechanical failure, blade cut-out, and nonunion. The surgeon must utilize multi-planar fluoroscopy to ensure the trajectory of the guidewire remains strictly within the cancellous bone of the neck, superior to the calcar.
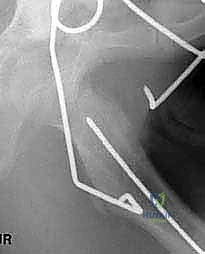
From a soft-tissue perspective, the direct lateral approach requires meticulous navigation of muscular intervals and neurovascular boundaries. The fascia lata must be divided longitudinally to expose the vastus lateralis. The vastus lateralis is then elevated subperiosteally from its origin at the vastus ridge and the linea aspera. This elevation must be performed with strict adherence to the subperiosteal plane to minimize hemorrhage from the perforating branches of the profunda femoris artery, which arborize heavily in the posterior aspect of the lateral femur. Proximally, the surgeon must respect the insertion of the gluteus medius and minimus on the greater trochanter. Iatrogenic injury to these abductors will result in an intractable Trendelenburg gait, negating the biomechanical advantages gained by the osteotomy. Furthermore, while the sciatic nerve is protected posteriorly by the intact musculature, excessive retraction or poor prone positioning can induce neuropraxia.
Exhaustive Indications and Contraindications
The decision to proceed with a Proximal Femoral Varus Osteotomy must be rooted in a rigorous clinical and radiographic evaluation. The primary goal is the preservation of the hip joint through the optimization of biomechanics and the reduction of focal articular contact pressures. In the pediatric population, the most frequent indication is the spastic hip subluxation associated with cerebral palsy. In these patients, a Reimers Migration Percentage exceeding 40-50% in a hip with preserved articular cartilage is an absolute indication for a varus derotational osteotomy (VDRO), often combined with a pelvic osteotomy (e.g., Dega or San Diego) if acetabular dysplasia is concurrently present. The varus angulation directly improves containment, while the derotation corrects the intoeing gait and anterior uncoverage driven by excessive femoral anteversion.
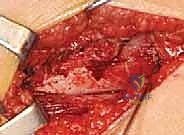
In Legg-Calvé-Perthes disease, the indication for a varus osteotomy is predicated on the concept of "containment." During the fragmentation and early reossification phases, the necrotic femoral head is highly susceptible to lateral extrusion and subsequent plastic deformation (coxa magna). By placing the femur into varus, the vulnerable anterolateral portion of the femoral head is rotated deeply into the acetabulum, utilizing the spherical acetabulum as a biological mold to ensure the head heals concentrically. In young adults, a varus osteotomy may be indicated for early degenerative joint disease secondary to mild dysplasia or coxa valga, provided there is congruency of the joint in abduction and internal rotation on functional radiographs.

However, the procedure is not without strict contraindications. Performing a varus osteotomy in a hip that is incongruent in the proposed functional position will accelerate, rather than delay, arthrosis. Severe osteopenia, often seen in non-ambulatory patients with profound neuromuscular involvement, is a relative contraindication, as the bone may not support the massive localized forces exerted by the blade plate, leading to catastrophic hardware failure. Active infection, uncorrectable coagulopathy, and the absence of functional abductor musculature (which would render the biomechanical correction useless) are absolute contraindications.
| Category | Indications | Contraindications |
|---|---|---|
| Neuromuscular | Spastic subluxation (CP, Spina Bifida), RMP > 40%, progressive coxa valga. | Profound osteopenia precluding hardware fixation, rigid fixed dislocation without salvageable cartilage. |
| Developmental | DDH with residual coxa valga/anteversion, symptomatic acetabular dysplasia (often combined with pelvic osteotomy). | Incongruent joint in the planned position of correction (abduction/internal rotation). |
| Idiopathic/Vascular | Perthes disease (Herring B/B-C) in fragmentation phase requiring containment. | Late-stage Perthes with healed, fixed severe deformity (hinge abduction). |
| Degenerative | Early osteoarthritis secondary to coxa valga, preserved cartilage space, congruent joint. | Advanced bone-on-bone osteoarthritis, inflammatory arthropathies (e.g., Rheumatoid Arthritis). |
| Systemic/Local | Post-traumatic malunion (valgus/extension/rotational deformity). | Active local or systemic infection, severe medical comorbidities precluding anesthesia. |
Pre-Operative Planning, Templating, and Patient Positioning
The success of a 90-degree blade plate osteotomy is definitively determined before the patient ever enters the operating theater. Meticulous preoperative planning and radiographic templating form the absolute blueprint for the procedure. The clinical examination must rigorously assess the patient's rotational profile. The trochanteric prominence test (Craig's test) is utilized in the prone position to estimate femoral anteversion. The degree of internal and external rotation is documented; a patient with 80 degrees of internal rotation and 10 degrees of external rotation clearly demonstrates excessive anteversion requiring surgical derotation. Furthermore, the surgeon must assess for fixed adduction or flexion contractures, which may necessitate concurrent soft tissue releases to allow the varusized femur to rest neutrally without placing excessive tension on the osteotomy site.

Radiographic templating requires a high-quality, true anteroposterior (AP) radiograph of the pelvis. Crucially, to accurately measure the true neck-shaft angle, the radiograph must be taken with the hips internally rotated to neutralize the patient's inherent anteversion. If the radiograph is taken with the legs externally rotated, the neck-shaft angle will appear artificially valgus. Once a true AP is obtained, the surgeon determines the desired postoperative neck-shaft angle. The trigonometric calculation for the guidewire insertion angle is elegant but requires absolute precision: The angle of the guidewire relative to the femoral shaft is equal to the angle of the blade plate (90 degrees) minus the desired degrees of varus correction. For example, if a patient has a preoperative NSA of 150 degrees and the surgeon desires a postoperative NSA of 120 degrees, the required varus correction is 30 degrees. Therefore, the guidewire must be inserted at an angle of 60 degrees to the anatomical axis of the femoral shaft (90° - 30° = 60°).
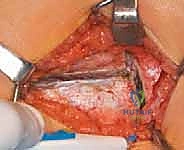
Patient positioning is a critical variable that directly influences the ease and accuracy of the procedure. While some surgeons prefer the supine position on a radiolucent table, the prone position with the operative leg draped free offers distinct, insurmountable advantages, particularly for complex derotational corrections. Prone positioning provides unparalleled access to the posterior aspect of the vastus lateralis, facilitating a cleaner, less hemorrhagic approach. More importantly, it replicates the position of the clinical examination for femoral anteversion. With the knee flexed to 90 degrees, the tibia acts as a perfect goniometer, allowing the surgeon to visually and precisely dial in the exact amount of derotation prior to final plate fixation. The patient must be carefully padded, with chest rolls to ensure uninhibited ventilation and all bony prominences protected to prevent decubitus ulcers or neuropraxia. The C-arm must be positioned to allow unhindered, rapid transition between AP and lateral fluoroscopic views of the proximal femur.
Step-by-Step Surgical Approach and Fixation Technique
The intraoperative execution of this procedure demands a symphony of anatomical respect, mechanical precision, and rigorous fluoroscopic verification. Every step builds upon the integrity of the previous one; a minor angular deviation during guidewire placement will compound into a massive geometric error upon final fixation.
Incision and Deep Dissection
The procedure commences with a robust longitudinal lateral incision centered over the greater trochanter, extending distally along the femoral shaft to accommodate the planned length of the side plate. The subcutaneous tissues are divided in line with the skin incision, taking care to achieve meticulous hemostasis using electrocautery. The fascia lata is identified and incised longitudinally. At this juncture, the vastus lateralis muscle belly is exposed.
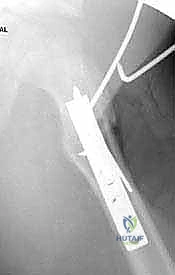
Using a Cobb elevator or electrocautery, the vastus lateralis is meticulously elevated from its posterior origin at the linea aspera and its proximal origin at the vastus ridge. This dissection must remain strictly subperiosteal. Violating the muscle belly will result in significant hemorrhage from the perforating vessels. As the muscle is reflected anteriorly, Bennett or Hohmann retractors are carefully placed circumferentially around the proximal femur. These retractors serve a dual purpose: they provide unparalleled visualization of the lateral cortex and act as a physical barrier, protecting the surrounding neurovascular structures and soft tissues from the oscillating saw and drill bits.
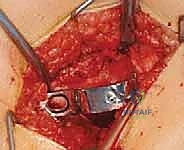
Guidewire Insertion and Anatomical Orientation
This is arguably the most critical step of the entire operation. A 2.0mm or 2.5mm threaded guidewire is selected. The entry point is dictated by the patient's skeletal maturity; in a skeletally mature patient, the entry is directly through the lateral aspect of the greater trochanter. In a skeletally immature patient, the entry point must be carefully plotted just distal to the greater trochanteric apophysis to avoid iatrogenic growth arrest.
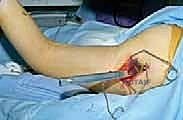
Using an angled guide (e.g., a 60-degree or 70-degree triangle based on the preoperative templating), the guidewire is driven into the femoral neck. The trajectory must be verified continuously in two orthogonal planes using fluoroscopy. On the AP view, the wire must traverse the center of the femoral neck, resting safely superior to the dense calcar femorale. On the lateral view, the wire must be perfectly centered within the anterior-posterior diameter of the neck to avoid anterior or posterior cortical breach.
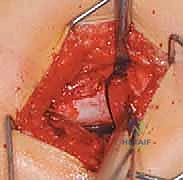
The Seating Chisel: Preparation for the Blade
Once the primary guidewire is perfectly positioned, a second, parallel derotation wire is often placed proximally to control the proximal fragment during the osteotomy. The lateral cortex is then opened using a drill or a small router over the primary guidewire to prevent the seating chisel from splintering the lateral cortex upon entry.
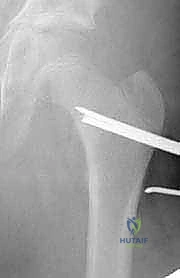
The seating chisel, which perfectly matches the profile of the blade plate, is introduced over the guidewire. The rotational alignment of the chisel is paramount; the handle of the chisel must be perfectly parallel to the longitudinal axis of the femoral shaft in the sagittal plane to ensure the side plate will eventually sit flush against the lateral cortex. The chisel is advanced under strict fluoroscopic guidance. The surgeon must feel the dense, high-pitched resonance of the mallet strikes, indicating solid purchase in the cancellous bone, without the sudden loss of resistance that signifies a cortical breach.
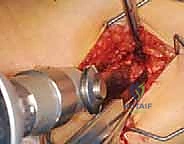
Executing the Osteotomy
With the track for the blade created, the chisel is removed, and the blade plate is temporarily inserted to verify the track. Once confirmed, the blade plate is removed, and the osteotomy is performed. The level of the osteotomy is typically at or just proximal to the lesser trochanter.
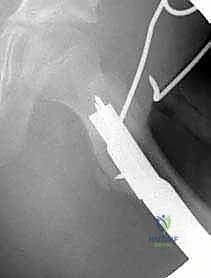
Using a reciprocating or oscillating saw, a transverse cut is made perpendicular to the femoral shaft. Continuous saline irrigation is mandatory during this step to prevent thermal necrosis of the bone, which would profoundly inhibit osteogenesis and lead to nonunion. In cases requiring significant varusization, a medially based closing wedge may be resected to prevent excessive lateral translation of the proximal fragment and to control leg length discrepancy.
Implantation of the 90-Degree Blade Plate
The proximal fragment is mobilized, and the definitive 90-degree blade plate is inserted into the pre-cut track in the femoral neck. The blade must be seated completely until the shoulder of the plate rests flush against the lateral cortex of the proximal fragment.
At this stage, the distal fragment (the femoral shaft) is manipulated. By abducting the leg, the lateral cortex of the distal fragment is brought into contact with the side plate of the implant. This maneuver forcefully closes the osteotomy site and imparts the planned varus angulation.
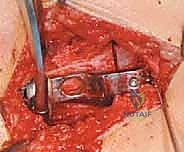
Derotation and Final Fixation
If derotation is required, it is performed at this juncture. With the patient prone and the knee flexed to 90 degrees, the tibia is used as a lever. The distal fragment is externally rotated relative to the internally fixed proximal fragment until the desired degree of anteversion is achieved.
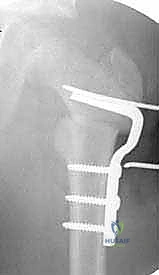
Once the coronal and axial alignments are perfected, a bone clamp is used to secure the side plate to the distal femoral shaft. Axial compression is then applied across the osteotomy site. This is typically achieved using an articulated tension device attached to the distal end of the plate, or by utilizing dynamic compression holes within the plate itself. Absolute rigid compression is essential for primary bone healing.
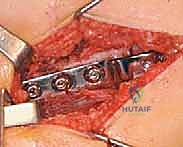
Finally, bicortical screws are placed through the side plate into the distal fragment. Meticulous layered closure over a suction drain concludes the procedure, ensuring the vastus lateralis is securely reapproximated to its origin to prevent postoperative hematoma and muscle herniation.
Complications, Incidence Rates, and Salvage Management
Despite meticulous technique, the Proximal Femoral Varus Osteotomy carries a defined risk profile. Complications can range from minor transient neuropraxias to catastrophic hardware failures requiring complex revision arthroplasty or repeat osteotomy. A profound understanding of these risks is necessary for immediate intraoperative recognition and postoperative management.
The most dreaded mechanical complication is blade cut-out or loss of fixation. This almost invariably stems from technical error during the operation—specifically, violating the superior or anterior/posterior cortex of the femoral neck with the seating chisel, or placing the blade too inferiorly, breaching the calcar femorale. If the calcar is violated, the plate loses its structural support and will toggle under physiological loading, leading to varus collapse and nonunion. Incidence of hardware failure in modern series is relatively low (2-5%) when performed by experienced surgeons, but it spikes dramatically in patients with severe osteopenia or when rigid postoperative weight-bearing restrictions are non-compliant.

Avascular necrosis (AVN) of the femoral head is a devastating biological complication. While more common in proximal femoral osteotomies performed for DDH
