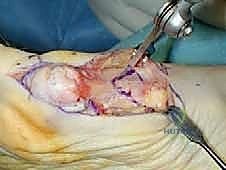
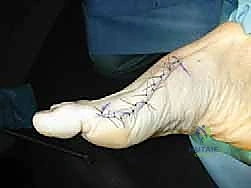
Proximal Chevron Osteotomy with Locking Plate Fixation for Hallux Valgus Correction
Key Takeaway
Join us in the OR for a masterclass on proximal chevron osteotomy with locking plate fixation, a robust technique for significant hallux valgus correction. We'll meticulously cover patient positioning, intricate anatomy, step-by-step intraoperative execution, critical pearls to optimize outcomes, and strategies to manage potential pitfalls. This procedure offers stable fixation, early weight-bearing, and excellent functional results for our patients.
Comprehensive Introduction and Patho-Epidemiology
Pathophysiology of Hallux Valgus
Hallux valgus is not merely an aesthetic concern or a simple exostosis; it is a complex, progressive, three-dimensional deformity of the first ray. The pathology is characterized by lateral deviation and pronation of the hallux, paired with medial deviation and often pronation of the first metatarsal. This divergence results in an increased intermetatarsal angle (IMA) between the first and second metatarsals, leading to subluxation of the first metatarsophalangeal (MTP) joint. As the medial eminence becomes increasingly prominent, it is subjected to chronic friction against footwear, leading to overlying adventitial bursitis and significant pain.
The biomechanical cascade of hallux valgus involves a destabilization of the medial column of the foot. The intrinsic musculature, specifically the abductor hallucis, shifts plantarly, losing its ability to abduct the hallux and instead acting as an anomalous flexor and pronator. Simultaneously, the adductor hallucis and the lateral head of the flexor hallucis brevis (FHB) gain a mechanical advantage, exerting an unopposed lateral and deforming force on the proximal phalanx. The sesamoid complex, tethered to the transverse metatarsal ligament, remains in its anatomical position relative to the second metatarsal, meaning the first metatarsal head effectively subluxates medially off the sesamoid apparatus.
Understanding this three-dimensional derangement is critical for the operating surgeon. Correction cannot simply address the medial eminence; it must restore the anatomical alignment of the first ray, relocate the sesamoid complex beneath the metatarsal head, and rebalance the soft tissues. Failure to address the increased IMA, the lateral soft tissue contracture, or the rotational component of the metatarsal will invariably lead to a high rate of clinical recurrence and patient dissatisfaction.
Evolution of the Proximal Chevron Osteotomy
The surgical management of hallux valgus boasts a rich history, with over 130 distinct procedures described in the orthopedic literature. Distal osteotomies, such as the distal chevron, are highly effective for mild to moderate deformities. However, their capacity for lateral translation is limited by the width of the metatarsal head, making them insufficient for severe deformities with an IMA exceeding 15 degrees. To address these larger angles, surgeons historically relied on proximal osteotomies, such as the closing base wedge osteotomy or the crescentic osteotomy.
While effective at reducing the IMA, traditional proximal osteotomies carried significant inherent risks. Closing wedge osteotomies often resulted in undesirable shortening and dorsal elevation of the first metatarsal, leading to transfer metatarsalgia. Crescentic osteotomies, while preserving length, were notoriously unstable in the sagittal plane and technically demanding to fixate. The proximal chevron osteotomy emerged as a biomechanically superior alternative, combining the intrinsic stability of a V-shaped cut with the powerful corrective potential of a proximal diaphyseal location.
The proximal chevron osteotomy allows for significant lateral translation and angular correction of the distal fragment. By placing the apex of the osteotomy in the proximal metadiaphysis, the surgeon leverages a longer lever arm, achieving a greater reduction of the IMA for every millimeter of lateral translation compared to a distal osteotomy. Furthermore, the V-shaped geometry provides excellent inherent stability against rotational and translational forces, making it an ideal choice for comprehensive bunion correction in moderate to severe cases.
Rationale for Locking Plate Fixation
Historically, the Achilles heel of proximal first metatarsal osteotomies has been the method of fixation. Kirschner wires (K-wires) provided minimal stability, necessitated prolonged periods of non-weight-bearing, and carried a high risk of pin tract infections. Standard lag screws, while an improvement, often failed in osteopenic bone or succumbed to the immense cantilever forces exerted on the first ray during the terminal stance phase of gait, leading to dorsal malunion and transfer lesions.
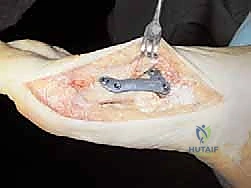
The advent of locking plate technology has revolutionized the execution and postoperative management of the proximal chevron osteotomy. Locking plates function as internal fixators; the screw heads thread directly into the plate, creating a rigid, fixed-angle construct. This design does not rely on friction between the plate and the bone, making it exceptionally reliable in poor-quality cancellous bone and highly resistant to the dorsal elevating forces that plague the first metatarsal.
This enhanced biomechanical stability translates directly to superior clinical outcomes. Locking plate fixation mitigates the risk of fixation failure, delayed union, and malunion. Crucially, it allows for accelerated postoperative rehabilitation protocols. Patients can often be permitted to bear weight early in a protective boot, which significantly reduces the risk of deep vein thrombosis, minimizes disuse osteopenia, and drastically improves patient satisfaction and functional recovery compared to the prolonged immobilization required by historical fixation methods.
Detailed Surgical Anatomy and Biomechanics
Osteology and Articular Geometry
The first metatarsal is the cornerstone of the medial longitudinal arch and the primary load-bearing structure of the forefoot. It articulates proximally with the medial cuneiform at the first tarsometatarsal (TMT) joint, a structurally complex articulation that dictates the mobility of the entire first ray. Distally, the metatarsal head articulates with the proximal phalanx at the MTP joint. The metatarsal shaft is uniquely contoured, exhibiting a dorsal concavity and a plantar convexity, which must be accounted for during osteotomy planning to avoid inadvertent intra-articular extension or cortical breaching.
The metadiaphyseal junction, the target zone for the proximal chevron osteotomy, is characterized by a transition from the dense cortical bone of the diaphysis to the more vascular, cancellous bone of the proximal metaphysis. The cortical thickness varies significantly; the medial and lateral cortices are generally robust, while the dorsal cortex can be surprisingly thin. Surgeons must be acutely aware of this anatomy when directing the saw blade and placing screws, ensuring adequate purchase without causing iatrogenic fractures or troughing.
The plantar aspect of the first metatarsal head features two distinct longitudinal grooves separated by a central ridge known as the crista. These grooves accommodate the medial (tibial) and lateral (fibular) sesamoids. In a hallux valgus deformity, as the metatarsal deviates medially and pronates, the crista is often eroded, and the sesamoids appear laterally subluxated on an AP radiograph. Restoring the metatarsal head over the sesamoid apparatus is a critical radiographic endpoint for a successful proximal chevron osteotomy.
Neurovascular Topography
Meticulous dissection and respect for the neurovascular anatomy are paramount during the medial approach to the first metatarsal. The most critical sensory structure at risk is the medial dorsal cutaneous nerve, a terminal branch of the superficial fibular nerve. This nerve typically courses dorsomedially over the extensor hallucis longus (EHL) tendon and crosses the surgical field obliquely. Injury to this nerve, whether via direct transection, aggressive retraction, or entrapment in scar tissue, can result in a debilitating neuroma or a highly distressing area of numbness over the dorsomedial hallux.
The plantar innervation is supplied by the medial plantar cutaneous nerve, a branch of the tibial nerve. While generally protected by the thick plantar soft tissues during a standard medial approach, aggressive plantar dissection or the placement of overly long plantar-directed screws can irritate or injure these branches. Surgeons must maintain their dissection within the designated fascial planes to avoid encroaching on these sensitive plantar structures.
The vascular supply to the first metatarsal head is robust but vulnerable. The primary blood supply is derived from the first dorsal metatarsal artery and the first plantar metatarsal artery, which form an extracapsular arterial ring around the metatarsal neck before penetrating the bone. While proximal osteotomies carry a lower risk of avascular necrosis (AVN) of the metatarsal head compared to distal osteotomies (which directly threaten the nutrient vessels at the neck), care must still be taken to avoid excessive stripping of the dorsal and lateral periosteum to preserve the delicate vascular network.
Musculotendinous and Capsuloligamentous Structures
The dynamic stability of the first MTP joint relies on a delicate balance of intrinsic and extrinsic musculotendinous forces. The abductor hallucis tendon courses along the medial border of the foot, inserting onto the medial aspect of the proximal phalanx base and the medial sesamoid. In hallux valgus, this tendon subluxates plantarly, losing its abductor moment and contributing to the pronation of the hallux. During the surgical approach, this tendon is often visualized and retracted plantarly; in severe cases, a dorsal relocation may be required during closure.
The adductor hallucis is a powerful deforming force in hallux valgus. Composed of oblique and transverse heads, it inserts onto the lateral base of the proximal phalanx and the lateral sesamoid. Its relentless pull exacerbates the lateral deviation of the toe. The release of this tendon, along with the lateral collateral ligament and the lateral sesamoid suspensory ligament, is an absolute prerequisite for successful deformity correction. Without a thorough lateral release, the proximal osteotomy will be fighting against an unyielding soft tissue tether.
The MTP joint capsule undergoes significant adaptive changes in the presence of a chronic bunion deformity. The medial capsule becomes attenuated, redundant, and mechanically incompetent, while the lateral capsule becomes severely contracted. The surgical strategy must address both sides of this equation: releasing the contracted lateral structures to permit realignment, and performing a robust medial capsulorrhaphy (imbrication) to restore medial stability and hold the corrected position during the critical early phases of biological healing.
Biomechanical Considerations of the First Ray
The first ray functions as a dynamic weight-bearing beam during the stance phase of gait. During terminal stance (heel-off to toe-off), the windlass mechanism is activated; dorsiflexion of the hallux tightens the plantar fascia, elevating the longitudinal arch and locking the midtarsal joints, thereby creating a rigid lever for propulsion. This mechanism exerts tremendous dorsal elevating forces on the first metatarsal head.
If a proximal osteotomy is not rigidly fixated, these ground reaction forces will inevitably lead to dorsal malunion of the distal metatarsal fragment. A dorsally elevated first metatarsal (metatarsus primus elevatus) results in a loss of weight-bearing capacity through the first ray. The load is subsequently transferred laterally to the lesser metatarsal heads, leading to intractable transfer metatarsalgia, stress fractures, and severe patient morbidity.
This biomechanical reality underscores the necessity of locking plate fixation for the proximal chevron osteotomy. The fixed-angle construct neutralizes the cantilever bending forces, ensuring that the metatarsal heals in its anatomically corrected, plantigrade position. Furthermore, the surgeon must be meticulous in their osteotomy execution, ensuring that the plantar limb of the chevron is sufficiently long to resist dorsal displacement and that the overall length of the first ray is preserved to maintain the functional integrity of the forefoot.
Exhaustive Indications and Contraindications
Patient Selection Criteria
The proximal chevron osteotomy is a highly specialized procedure reserved for specific clinical scenarios. The ideal candidate is a patient presenting with a symptomatic, moderate to severe hallux valgus deformity that has failed to respond to extensive conservative measures, including shoe wear modification, orthotics, and anti-inflammatory therapies. Pain should be the primary driving factor for surgery; prophylactic correction of asymptomatic deformities is generally discouraged due to the inherent risks of surgical intervention.
Radiographically, the procedure is indicated for patients with an intermetatarsal angle (IMA) typically ranging from 15 to 20 degrees, and a hallux valgus angle (HVA) exceeding 30 degrees. It is particularly useful in cases where the MTP joint remains congruent or subluxated but reducible, and where a distal osteotomy would not provide sufficient lateral translation to normalize the IMA. The proximal chevron is also an excellent option for revision surgeries where a previous distal procedure has failed to adequately address the magnitude of the deformity.
Careful clinical assessment is required to ensure the patient has adequate bone stock to support a proximal osteotomy and locking plate fixation. While locking plates perform better in osteopenic bone than traditional screws, severe osteoporosis remains a concern. The patient must also possess the cognitive and physical capacity to adhere to a strict, phased postoperative rehabilitation protocol, as premature unprotected weight-bearing can compromise even the most robust fixation construct.
Absolute and Relative Contraindications
Recognizing the contraindications to a proximal chevron osteotomy is just as critical as identifying the indications. Absolute contraindications include the presence of active local or systemic infection, severe peripheral arterial disease compromising the healing potential of the soft tissues and bone, and profound neuroarthropathy (such as Charcot foot), which fundamentally alters the biomechanics and healing capacity of the extremity.
Severe hypermobility of the first tarsometatarsal (TMT) joint is a critical relative—and often absolute—contraindication. If the medial column is profoundly unstable at the TMT level, a proximal osteotomy will fail to address the root cause of the deformity, leading to a near-certain recurrence. In such cases, a first TMT arthrodesis (Lapidus procedure) is the biomechanically appropriate intervention. Similarly, the presence of advanced degenerative joint disease (osteoarthritis) at the first MTP joint contraindicates an osteotomy; these patients are better served by an MTP joint arthrodesis to reliably eliminate pain.
Other relative contraindications include an exceptionally narrow first metatarsal diaphysis, which may preclude safe execution of the osteotomy and hardware placement without iatrogenic fracture. Severe osteoporosis, while partially mitigated by locking plate technology, increases the risk of hardware failure and loss of fixation. Finally, patients with unrealistic expectations, uncontrolled psychiatric conditions, or a history of profound non-compliance with medical directives are poor candidates for this technically demanding reconstructive procedure.
Decision Making Matrix
| Clinical Scenario | Radiographic Findings | Recommended Procedure | Rationale |
|---|---|---|---|
| Mild Deformity | IMA < 13°, HVA < 30° | Distal Chevron Osteotomy | Adequate translation achievable distally; less invasive. |
| Moderate/Severe Deformity | IMA 15°-20°, HVA > 30° | Proximal Chevron Osteotomy | Requires greater translation; proximal location provides longer lever arm. |
| Severe Deformity + TMT Hypermobility | IMA > 20°, Positive Root's Test | Lapidus Procedure (TMT Arthrodesis) | Must stabilize the medial column to prevent recurrence. |
| Deformity + MTP Degeneration | Joint space narrowing, osteophytes | First MTP Arthrodesis | Osteotomy will not relieve arthritic pain; fusion provides definitive relief. |
| Severe Osteoporosis | Cortical thinning, osteopenia | MTP Arthrodesis or Lapidus | High risk of hardware failure and non-union with diaphyseal osteotomies. |
Pre-Operative Planning, Templating, and Patient Positioning
Clinical and Radiographic Assessment
Comprehensive preoperative planning begins in the clinic. A thorough physical examination must assess the vascular status (palpable dorsalis pedis and posterior tibial pulses), neurologic function, and the exact location of the patient's pain. The surgeon must evaluate the range of motion of the first MTP joint, noting any crepitus or restriction that might indicate underlying degenerative changes. Crucially, the stability of the first TMT joint must be assessed manually (Root's test) to rule out hypermobility that would necessitate a Lapidus fusion instead of an osteotomy.
Standardized, weight-bearing radiographs are mandatory. These must include anteroposterior (AP), lateral, and sesamoid axial views. Non-weight-bearing films are virtually useless for surgical planning as they do not accurately represent the dynamic deformity. On the AP view, the surgeon must measure the Hallux Valgus Angle (HVA), the Intermetatarsal Angle (IMA), and the Distal Metatarsal Articular Angle (DMAA). The lateral view is utilized to assess the sagittal alignment of the first ray (Meary's angle) and rule out metatarsus primus elevatus.
The sesamoid axial view is critical for evaluating the coronal plane rotation of the first metatarsal and the degree of sesamoid subluxation. If the metatarsal is significantly pronated, a standard proximal chevron may need to be modified (e.g., incorporating a rotational correction) or an alternative procedure considered. The congruency of the MTP joint must also be evaluated; an incongruent joint requires soft tissue balancing (lateral release and medial reefing) in addition to the bony correction.
Digital Templating and Implant Selection
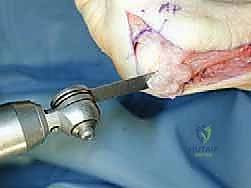
Modern orthopedic surgery relies heavily on digital templating software to ensure precision and optimize outcomes. Using calibrated preoperative radiographs, the surgeon virtually overlays the planned osteotomy. The apex of the proximal chevron is typically planned 1.5 to 2.0 cm distal to the first TMT joint, situated in the metadiaphyseal region. The dorsal and plantar limbs of the V-cut are templated, usually at an angle of 60 to 90 degrees relative to each other, ensuring the plantar limb is sufficiently long to provide sagittal plane stability.
Digital templating allows the surgeon to calculate the exact amount of lateral translation required to reduce the IMA to a normal physiological range (typically less than 9 degrees). The surgeon can virtually translate the distal fragment and assess the resulting alignment. This step is crucial for identifying potential pitfalls, such as excessive translation that might lead to cortical overhang or insufficient bony apposition, which could compromise healing and require a bone graft.
Implant selection is also finalized during this phase. The surgeon templates various low-profile, contoured locking plates designed specifically for proximal metatarsal osteotomies. The plate must be appropriately sized to span the osteotomy site, allowing for at least two locking screws in the proximal fragment and two in the distal fragment. The trajectory of the screws must be planned to ensure bicortical purchase where possible, without penetrating the TMT or MTP joints, and avoiding the plantar neurovascular structures.
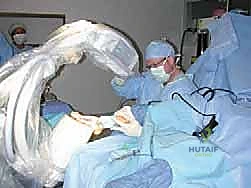
Operating Room Setup and Patient Positioning
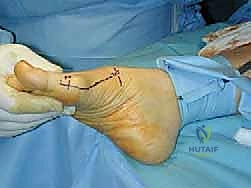
Optimal operating room setup and patient positioning are fundamental to the smooth execution of the procedure. The patient is placed in the supine position on a standard operating table. A small bump (often a rolled blanket or sandbag) is placed under the ipsilateral hip. This slight internal rotation of the lower extremity brings the medial aspect of the foot directly facing the ceiling, optimizing the surgeon's ergonomic access to the surgical site and preventing the leg from externally rotating during the procedure.
A pneumatic thigh tourniquet is applied over copious padding. While an ankle tourniquet is an option, a thigh tourniquet is generally preferred as it provides a wider, more reliable bloodless field and avoids tethering the extrinsic tendons around the ankle, which can interfere with intraoperative assessment of toe alignment. The entire lower extremity, from the toes to the mid-thigh, is prepped and draped in a standard sterile fashion, allowing for visualization of the entire mechanical axis of the leg if necessary.
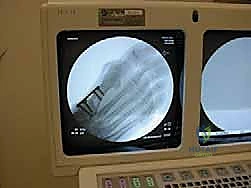
Fluoroscopy is absolutely indispensable for this procedure. The C-arm should be positioned on the contralateral side of the table, draped sterilely, and brought into the field before the incision is made to confirm that unobstructed AP, lateral, and oblique views of the first ray can be obtained without repositioning the patient. The surgeon should verify that the imaging monitor is placed in their direct line of sight. Once the setup is verified, the limb is exsanguinated with an Esmarch bandage, and the tourniquet is inflated to the appropriate pressure (typically 250-300 mmHg).
Step-by-Step Surgical Approach and Fixation Technique
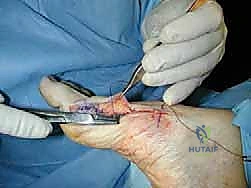
Incision and Soft Tissue Dissection
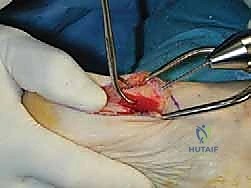
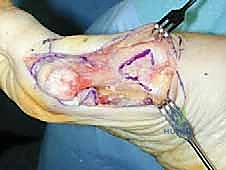
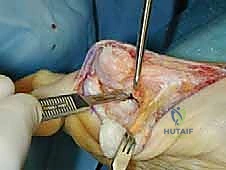
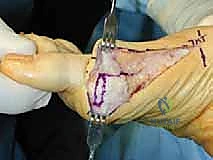
The procedure commences with a meticulously planned single midmedial approach to the first metatarsal. The palpable landmarks—the medial eminence of the metatarsal head and the first TMT joint line—are identified. A longitudinal incision, approximately 6 to 8 cm in length, is sharply executed using a no. 10 blade. The incision is centered over the midline of the medial aspect of the first metatarsal, extending from the proximal metaphysis to just distal to the MTP joint line.
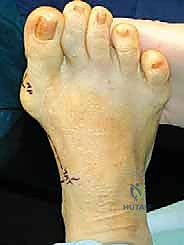
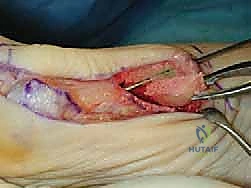
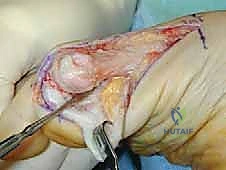
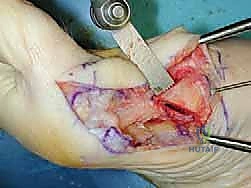
Immediately upon breaching the dermis, the surgeon must exercise extreme caution. The medial dorsal cutaneous nerve frequently crosses the proximal aspect of this surgical field. Subcutaneous dissection should be performed bluntly with Metzenbaum scissors or a hemostat, carefully identifying and gently retracting the nerve either dorsally or plantarly to protect it from the
Clinical & Radiographic Imaging Archive