High-Energy Pelvic Ring Injury: A Comprehensive Case Study of APC III with Vertical Shear
Key Takeaway
An APC III pelvic ring injury is an unstable, high-energy trauma with complete pubic symphysis and posterior sacroiliac complex disruption, often with vertical shear. Diagnosis involves clinical assessment for instability, initial AP, Inlet, Outlet radiographs, and CT scans to define specific fracture patterns like sacral involvement and displacement, especially in hemodynamically unstable cases.
Patient Presentation and History
A 38-year-old male presented to the Level I Trauma Center following a high-energy motor vehicle versus pedestrian incident. He was struck directly from the side while crossing an intersection by an SUV traveling at an estimated 80 kilometers per hour. Bystanders reported he was thrown approximately 15 meters and landed on the hard asphalt. He arrived hemodynamically unstable, with a Glasgow Coma Scale of 10 (E2V3M5) due to presumed traumatic brain injury and profound hypovolemic shock.
Initial Advanced Trauma Life Support primary survey revealed a patent airway, labored breathing with a respiratory rate of 28 breaths per minute, and diminished breath sounds on the right hemithorax with dullness to percussion highly suggestive of a massive hemothorax. Concurrently, the trauma team noted bilateral open tibia and fibula fractures, classified as Gustilo-Anderson IIIA on the left and IIIB on the right. Initial vital signs demonstrated a blood pressure of 70/40 mmHg and a heart rate of 130 beats per minute, indicating Class IV hemorrhagic shock.
Pelvic assessment during the primary survey demonstrated gross mechanical instability upon gentle palpation of the anterior superior iliac spines, with significant external rotation of both lower extremities indicating an "open book" morphology. Rectal examination revealed a normal sphincter tone but gross blood on the examining finger, immediately raising the suspicion for an open pelvic ring injury via a rectal mucosal tear. While no obvious perineal hematoma was noted in the first few minutes of evaluation, significant crepitus was palpable over the symphysis pubis and the right sacroiliac joint. Past medical history was significant for hypertension controlled with an angiotensin-converting enzyme inhibitor and a 15-pack-year smoking history.
Primary Survey and Resuscitation Protocol
Given the profound hemodynamic instability, a massive transfusion protocol was immediately initiated with a 1 to 1 to 1 ratio of packed red blood cells, fresh frozen plasma, and platelets. Tranexamic acid was administered intravenously within the first hour of injury. A right-sided thoracostomy tube was placed, immediately draining 800 milliliters of frank blood, which stabilized the respiratory status.
Simultaneously, a commercial pelvic binder was applied centered strictly over the greater trochanters to achieve temporary reduction of the pelvic volume and promote a tamponade effect within the retroperitoneal space. The application of the binder resulted in a transient improvement in mean arterial pressure to 65 mmHg. Due to the persistent shock state and the high suspicion of retroperitoneal hemorrhage from the pelvic venous plexus and potentially arterial sources, the trauma surgery team was activated for potential pre-peritoneal pelvic packing versus emergent angioembolization.
Clinical Examination Findings
Following initial resuscitation, endotracheal intubation for airway protection, and chest tube insertion for the hemothorax, a more detailed secondary survey was performed in the trauma bay.
Inspection of the Pelvis and Extremities
Gross asymmetry of the pelvis was evident despite the temporary binder application. There was apparent widening of the inter-iliac distance. Both lower extremities remained externally rotated, with the right lower extremity demonstrating significant proximal migration, suggesting a vertical shear component in addition to the anteroposterior compression. No obvious open pelvic wounds were visible on the anterior abdominal wall or flanks, but extensive, rapidly expanding ecchymosis was developing over the perineum, scrotum, and right flank extending towards the iliac crest.
A significant Morel-Lavallée lesion was suspected over the right greater trochanteric and gluteal region due to a palpable, fluctuant mass indicative of a closed degloving injury and hemolymphatic fluid collection. Inspection of the lower extremities confirmed an open Gustilo-Anderson IIIA fracture of the left distal tibia and fibula with significant soft tissue stripping but adequate periosteal coverage. The right lower extremity exhibited an open Gustilo-Anderson IIIB fracture of the mid-shaft tibia and fibula with segmental bone loss, extensive road debris contamination, and exposed diaphyseal bone devoid of periosteum.
Palpation and Mechanical Stability Assessment
Gentle anterior-posterior compression and lateral compression maneuvers had initially confirmed significant mechanical instability. It is a critical orthopedic trauma principle that once pelvic instability is identified, repeated mechanical testing is strictly contraindicated to prevent disruption of any forming retroperitoneal clot and to avoid exacerbating hemorrhage. The pelvic binder was left in place. Tenderness was elicited over the pubic symphysis, bilateral iliac wings, and profoundly over the right sacroiliac joint and sacrum.
The abdomen was distended and diffusely tender but lacked rigid peritonitis, though assessment was limited by the patient's intubated status. Palpable tenderness was noted directly over the pubic symphysis.
Genitourinary and Rectal Examination
Gross blood on the initial rectal exam persisted. A high-riding prostate was not definitively appreciated due to massive soft tissue swelling and hematoma formation in the perineum, but urethral integrity was highly questioned. Blood was noted at the urethral meatus. Consequently, transurethral catheterization was deferred pending a retrograde urethrogram. Vaginal examination was not applicable given the patient's gender. The presence of rectal blood mandated a general surgery consultation for evaluation of a rectal tear and consideration of an emergent diverting loop colostomy to prevent catastrophic pelvic sepsis.
Neurological and Vascular Assessment
Peripheral vascular examination revealed weak but palpable dorsalis pedis and posterior tibial pulses bilaterally, assessed via Doppler ultrasound due to the severe hypotension. Capillary refill was delayed to greater than 3 seconds in both feet.
Due to the patient's altered mental status, sedation, and intubation, a comprehensive neurological exam was deferred. However, gross motor function was assessed by noxious stimuli prior to deep sedation, revealing some withdrawal from painful stimuli in the left lower extremity but minimal response in the right lower extremity. This discrepancy raised immediate concern for a lumbosacral plexus injury, specifically involving the L5 and S1 nerve roots on the right side, which are highly susceptible to traction injuries in vertical shear and severe anteroposterior compression pelvic ring disruptions. Anal sphincter tone was noted to be intact on repeat rectal exam after initial shock resolution, suggesting preservation of the lower sacral roots (S2 through S4).
Imaging and Diagnostics
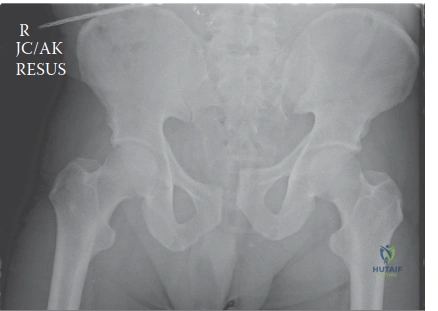
Radiographic evaluation began in the trauma bay with a portable anteroposterior radiograph of the pelvis and a portable chest radiograph. The AP pelvis radiograph revealed a catastrophic disruption of the pelvic ring. There was a pubic symphyseal diastasis measuring approximately 6 centimeters, complete disruption of the right sacroiliac joint with 3 centimeters of cephalad migration of the right hemipelvis, and widening of the left sacroiliac joint anteriorly.

Following initial stabilization and application of the pelvic binder, the patient was transported to the computed tomography suite. A comprehensive trauma protocol CT scan was performed, including a non-contrast CT of the head and cervical spine, followed by a CT angiography of the chest, abdomen, and pelvis with venous phase imaging.
Computed Tomography Findings
The CT scan provided a detailed anatomical map of the osseous and soft tissue injuries.
- Anterior Ring: The symphyseal diastasis was confirmed. There were no associated rami fractures. The bladder was displaced posteriorly by a large retropubic hematoma (space of Retzius).
- Posterior Ring: Axial and coronal reconstructions demonstrated a complete, highly unstable right-sided sacroiliac joint disruption. The anterior and posterior sacroiliac ligaments, as well as the sacrospinous and sacrotuberous ligaments, were completely avulsed. The right ilium was translated superiorly and posteriorly relative to the sacrum. The left sacroiliac joint demonstrated anterior widening with intact posterior ligaments, consistent with a severe open-book injury on that side.
- Vascular Assessment: CT angiography revealed a prominent arterial blush in the right greater sciatic notch, highly suspicious for active extravasation from the superior gluteal artery. A secondary blush was noted in the pre-peritoneal space adjacent to the pubic symphysis, likely originating from the obturator artery or the corona mortis.
- Soft Tissue: The CT confirmed a large, multi-loculated fluid collection over the right greater trochanter extending into the subcutaneous tissues of the flank, confirming the clinical suspicion of a massive Morel-Lavallée lesion.
Additional Diagnostic Procedures
A retrograde urethrogram was performed by the urology service in the trauma bay, which demonstrated a partial disruption of the membranous urethra with extravasation of contrast. A suprapubic catheter was subsequently placed under ultrasound guidance to achieve urinary diversion. A rigid proctoscopy performed by the general surgery team identified a 3-centimeter full-thickness longitudinal tear in the anterior rectal wall, confirming the diagnosis of an open pelvic fracture.
Differential Diagnosis
The evaluation of a high-energy pelvic ring injury requires precise classification to guide both resuscitation and definitive surgical management. The primary differentials revolve around the vector of force applied to the pelvis, which dictates the predictable pattern of ligamentous and osseous failure.
| Classification | Mechanism of Injury | Anterior Ring Injury | Posterior Ring Injury | Hemodynamic Risk |
|---|---|---|---|---|
| Anteroposterior Compression Type III | Direct anterior to posterior crushing force. | Symphyseal diastasis or vertical rami fractures. | Complete disruption of anterior and posterior SI ligaments, sacrospinous, and sacrotuberous ligaments. | Extremely High. Massive venous plexus and potential arterial disruption (internal iliac branches). |
| Vertical Shear | Axial loading force to one hemipelvis (e.g., fall from height, severe upward force). | Symphyseal diastasis or vertical rami fractures. | Complete vertical translation of the hemipelvis. Disruption of all posterior ligaments. | Extremely High. High association with superior gluteal artery injury and lumbosacral plexus traction. |
| Lateral Compression Type III | Lateral force causing internal rotation of one hemipelvis, with contralateral external rotation (windswept pelvis). | Transverse rami fractures (ipsilateral) and symphyseal diastasis or rami fractures (contralateral). | Posterior crush/impaction (ipsilateral) and complete SI disruption (contralateral). | Moderate to High. Risk of visceral injury from bony spicules; retroperitoneal bleeding present but often tamponades better than APC. |
| Combined Mechanical Injury | Complex combination of vectors, often high-energy polytrauma. | Variable, highly comminuted. | Variable, often multidirectional instability. | High. Unpredictable bleeding patterns and severe associated injuries. |
In this clinical scenario, the patient exhibits a classic Combined Mechanical Injury pattern, specifically an Anteroposterior Compression Type III with a superimposed Vertical Shear component on the right side. The profound symphyseal widening indicates the APC vector, while the 3-centimeter cephalad migration of the right hemipelvis confirms the complete vertical instability characteristic of a shear injury.
Surgical Decision Making and Classification
The management of this patient requires a multidisciplinary approach, balancing the immediate life-threatening hemorrhage with the need for long-term mechanical stability of the pelvic ring. The Young-Burgess classification system categorizes this as an APC III / Vertical Shear variant, while the Tile classification system would designate this as a Type C1.3 injury (rotationally and vertically unstable, unilateral posterior disruption with contralateral rotational instability).
Damage Control Orthopedics versus Early Total Care
Given the patient's presentation in Class IV hemorrhagic shock, elevated lactate, base deficit, and coagulopathy, Early Total Care (ETC) is absolutely contraindicated. The patient is physiologically exhausted and falls into the "in extremis" or "borderline" category according to the clinical grading scales for polytrauma. Therefore, the principles of Damage Control Orthopedics must be strictly applied.
The immediate goals of DCO in this patient are:
1. Arrest retroperitoneal hemorrhage.
2. Provide temporary mechanical stability to the pelvic ring to assist in clot formation.
3. Manage the open fracture contamination to prevent overwhelming sepsis.
4. Divert the fecal stream due to the open rectal injury.
Phased Surgical Strategy
Phase 1: Emergent Damage Control Intervention
The presence of arterial blush on the CT angiogram necessitates immediate intervention. The surgical decision was made to proceed emergently to the hybrid operating room for pelvic angiography and embolization, followed immediately by pre-peritoneal pelvic packing and external fixation. The general surgery team would perform a diverting loop sigmoid colostomy, and the orthopedic team would perform emergent irrigation and debridement of the bilateral open tibia fractures.
Phase 2: Resuscitation and Optimization
Following the damage control procedures, the patient will be transferred to the Surgical Intensive Care Unit for correction of coagulopathy, acidosis, and hypothermia (the lethal triad).
Phase 3: Definitive Reconstruction
Once physiologically optimized (typically days 3 to 7 post-injury), the patient will return to the operating room for definitive internal fixation of the anterior and posterior pelvic ring, management of the Morel-Lavallée lesion, and definitive skeletal stabilization of the tibia fractures.
Surgical Technique and Intervention
Phase 1 Damage Control Execution
The patient was transported to the hybrid operating room. Interventional radiology accessed the left common femoral artery. Selective angiography of the right internal iliac artery confirmed active extravasation from the superior gluteal artery. Selective coil embolization was successfully performed. Prophylactic gel-foam embolization of the bilateral obturator arteries was also completed given the massive anterior ring disruption.
Immediately following embolization, a supra-acetabular external fixator was applied. Two 5.0 millimeter Schanz pins were placed percutaneously into the dense bone corridor of the anterior inferior iliac spine, directed towards the posterior superior iliac spine under fluoroscopic guidance (obturator oblique outlet view). A carbon fiber bar construct was utilized to close the pelvic volume, reducing the symphyseal diastasis from 6 centimeters to approximately 2 centimeters. Over-compression was carefully avoided to prevent internal rotation deformity of the hemipelvis.
A midline laparotomy was performed by general surgery. Pre-peritoneal pelvic packing was executed by packing three laparotomy sponges deep into the true pelvis bilaterally, anterior to the bladder and posterior to the pubic symphysis, directly compressing the venous plexus. A diverting loop sigmoid colostomy was matured in the left upper quadrant. Concurrently, the bilateral open tibia fractures underwent radical irrigation with 9 liters of normal saline each, excision of devitalized muscle and bone margins, and application of bridging spanning external fixators.
Phase 2 Definitive Pelvic Reconstruction
On post-injury day 5, the patient's physiology had normalized. Lactic acid was 1.2 mmol/L, and coagulopathy was corrected. The patient was brought to the operating room for definitive fixation.
Patient Positioning and Preparation
The patient was placed supine on a radiolucent Jackson flat table. A bump was placed under the lumbosacral junction to facilitate reduction. The entire abdomen, pelvis, and bilateral lower extremities were prepped and draped in a standard sterile fashion. The supra-acetabular external fixator was left in place temporarily to assist with reduction maneuvers.
Anterior Ring Fixation
A standard Pfannenstiel approach was utilized. A transverse incision was made two fingerbreadths superior to the pubic symphysis. The anterior rectus sheath was incised transversely, and the rectus abdominis muscles were split along the linea alba. The retropubic space of Retzius was accessed, and the previously placed pelvic packs were carefully removed. Hemostasis was achieved.
The pubic symphysis was identified. A specialized pelvic reduction forceps (Jungbluth clamp) was applied using 3.5 millimeter cortical screws placed into the superior pubic rami bilaterally. The external fixator was loosened, and the clamp was tightened to achieve an anatomic reduction of the symphyseal diastasis.
Fixation was achieved using a pre-contoured 6-hole symphyseal plate. Given the severe instability and the vertical shear component, a multi-hole, orthogonal plating construct was deemed necessary. A superior plate was applied utilizing 3.5 millimeter fully threaded cortical screws, ensuring at least two screws engaged the dense bone of the pubic body bilaterally. A secondary anterior plate was placed orthogonally to increase biomechanical rigidity and resist the massive rotational forces.
Posterior Ring Fixation
Attention was then turned to the posterior ring. Due to the complete disruption of the right sacroiliac joint and the vertical shear vector, percutaneous iliosacral screws alone were deemed biomechanically insufficient. A decision was made to perform an open reduction and internal fixation of the right sacroiliac joint combined with percutaneous stabilization of the left side.
An anterior approach to the sacroiliac joint via the lateral window of the ilioinguinal approach was considered, but given the severe posterior displacement, a posterior approach was selected. The patient was carefully repositioned prone. A longitudinal incision was made lateral to the posterior superior iliac spine. The gluteus maximus was elevated to expose the posterior ilium and the disrupted sacroiliac joint.
The vertical translation was reduced using a Schanz pin placed in the posterior ilium as a joystick, combined with longitudinal traction applied to the right lower extremity. Once anatomic reduction of the sacroiliac joint was confirmed via direct visualization and fluoroscopy, two anterior-to-posterior oriented trans-iliac trans-sacral screws were placed.
Using precise fluoroscopic imaging (Inlet, Outlet, and Lateral sacral views), a guide wire was advanced from the right lateral ilium, across the right sacroiliac joint, through the S1 sacral body, and into the left ilium. A 7.3 millimeter fully threaded, cannulated screw was placed. A second 7.3 millimeter screw was placed into the S2 sacral segment. The fully threaded nature of these trans-iliac trans-sacral screws provides maximum thread purchase in the dense cortical bone of the ilium bilaterally, preventing lateral migration and providing superior biomechanical stability against vertical shear forces compared to partially threaded lag screws.
Management of the Morel-Lavallée Lesion
While prone, the massive right trochanteric Morel-Lavallée lesion was addressed. A longitudinal incision was made over the fluctuant area. Approximately 800 milliliters of serosanguinous fluid and liquefied necrotic fat were evacuated. The cavity was aggressively debrided of all non-viable tissue using a curette and pulsed lavage. Sclerodesis was performed using a doxycycline solution, and two large-bore closed suction drains were placed deep into the cavity before meticulous layered closure.
Definitive Skeletal Stabilization of Lower Extremities
The patient was repositioned supine. The bilateral tibial external fixators were removed. Given the severe soft tissue compromise (Gustilo IIIB on the right), intramedullary nailing was deemed high risk for deep infection at this stage. Therefore, definitive management with fine-wire circular external fixators (Ilizarov frames) was selected for both tibias to allow for rigid stabilization, bone transport if necessary for the right-sided bone loss, and unhindered access for soft tissue reconstructive procedures by the plastic surgery team.
Post Operative Protocol and Rehabilitation
The postoperative management of a severe APC III with Vertical Shear injury requires strict adherence to biomechanical constraints and aggressive medical management.
Weight-Bearing Restrictions
The patient was restricted to strict non-weight bearing on the bilateral lower extremities for a minimum of 12 weeks. The severe comminution of the tibias and the catastrophic nature of the pelvic ring disruption necessitate prolonged protection. Mobilization was restricted to bed-to-chair transfers utilizing a mechanical lift.
Deep Vein Thrombosis Prophylaxis
Pelvic ring injuries carry one of the highest risks for venous thromboembolism in orthopedic trauma. Chemical prophylaxis with low-molecular-weight heparin (Enoxaparin 40 mg subcutaneously daily) was initiated 24 hours post-operatively, once the risk of catastrophic retroperitoneal bleeding had sufficiently decreased. This will be continued for a minimum of 4 weeks, transitioning to an oral anticoagulant if dictated by the prolonged immobilization. Mechanical prophylaxis with sequential compression devices was utilized on the uninjured upper extremities.
Urologic and Colorectal Follow-up
The suprapubic catheter will remain in place for 4 to 6 weeks. The urology service will perform a repeat retrograde urethrogram and voiding cystourethrogram to assess urethral healing prior to any consideration of catheter removal or formal urethroplasty. The diverting loop colostomy will be maintained for 3 to 6 months. Reversal will only be considered after complete healing of the rectal tear is confirmed via endoscopy and fluoroscopic enema studies, and the pelvic fractures have achieved solid radiographic union to prevent any risk of late pelvic sepsis.
Radiographic Surveillance
Standard AP, Inlet, and Outlet pelvic radiographs will be obtained at 2 weeks, 6 weeks, 12 weeks, and 6 months post-operatively to monitor for loss of reduction, hardware failure, or delayed union. CT imaging may be utilized at 12 weeks to definitively assess osseous bridging across the sacroiliac joint.
Clinical Pearls and Pitfalls
- Avoid Repeated Mechanical Testing: Once pelvic instability is diagnosed clinically or radiographically, do not repeatedly compress the pelvis. This disrupts the fragile retroperitoneal hematoma and exacerbates potentially lethal hemorrhage.
- Binder Placement is Critical: A pelvic binder must be placed strictly over the greater trochanters, not over the iliac crests. High placement over the crests can paradoxical open the true pelvis or fail to reduce the posterior ring volume.
- Beware the Corona Mortis: During the Pfannenstiel approach and retropubic dissection, meticulous care must be taken to identify and ligate the corona mortis—an anastomotic connection between the external iliac and obturator vessels located on the posterior aspect of the superior pubic ramus. Inadvertent avulsion can lead to massive, difficult-to-control hemorrhage.
- Trans-iliac Trans-sacral Fixation for Vertical Shear: In severe vertical shear injuries, standard unilateral iliosacral screws may fail due to the immense vertical forces. Trans-iliac trans-sacral screws (TITS) utilizing fully threaded screws provide significantly higher biomechanical rigidity by anchoring in the dense cortical bone of the contralateral ilium.
- Vigilance for Lumbosacral Plexus Injury: Vertical shear and massive APC injuries place immense traction on the L5 nerve root (as it drapes over the sacral ala) and the sacral roots. A meticulous neurological exam must be documented as soon as the patient's cognitive status allows, as iatrogenic injury during screw placement must be differentiated from the initial traumatic neuropraxia.
- Mandatory Rectal and Vaginal Exams: Any high-energy pelvic fracture requires a thorough rectal and, in females, vaginal examination. Missing an open pelvic fracture can lead to catastrophic pelvic sepsis and near-certain mortality.
- Morel-Lavallée Lesion Management: Do not ignore closed degloving injuries. If left untreated, they have a high rate of secondary infection and can compromise future surgical incisions. Early recognition, evacuation, debridement, and dead-space management are paramount.
