Distal Femoral Fracture in Achondroplasia: A Complex Orthopedic Case Study
Key Takeaway
Managing distal femoral fractures in achondroplasia presents unique challenges due to altered bone morphology, including short, bowed femurs and narrow intramedullary canals. Diagnosis involves advanced imaging like CT with 3D reconstruction to understand complex comminution. Pre-operative planning is critical, requiring meticulous templating for appropriately sized implants and addressing specific anatomical variations for successful surgical outcomes.
Patient Presentation and History
Mechanism of Injury and Initial Trauma Resuscitation
A 35-year-old male presented to the Level I trauma center via emergency medical services following a high-energy blunt force trauma. The patient was an unrestrained pedestrian struck by a motor vehicle traveling at an estimated velocity of 40 miles per hour. The primary impact point was the anterolateral aspect of the left lower extremity. Upon arrival in the trauma bay, the patient was evaluated utilizing the Advanced Trauma Life Support protocol. The primary survey revealed a patent airway, unlabored bilateral breath sounds, and hemodynamic stability with a blood pressure of 135/85 mmHg and a heart rate of 92 beats per minute. The Glasgow Coma Scale score was 15. The secondary survey focused on the isolated high-energy injury to the left lower extremity, which demonstrated gross deformity, significant soft tissue swelling, and an inability to bear weight.
Achondroplasia Pathophysiology and Baseline Status
The patient carries a known diagnosis of achondroplasia, the most common form of short-limbed dwarfism, identified during infancy. Achondroplasia is an autosomal dominant genetic disorder caused by a gain-of-function mutation in the fibroblast growth factor receptor 3 gene located on chromosome 4p16.3. This mutation results in the constitutive activation of the receptor, which severely inhibits chondrocyte proliferation and differentiation within the proliferative zone of the physis. Consequently, endochondral ossification is profoundly impaired, leading to the characteristic phenotypic features of rhizomelic limb shortening, macrocephaly, frontal bossing, and midface hypoplasia.
From an orthopedic trauma perspective, the achondroplastic skeleton presents unique biomechanical and anatomic challenges. The long bones, particularly the femurs and humeri, are significantly shortened but possess a normal or increased cortical diameter, resulting in a thick, robust appearance. However, the medullary canals are typically narrow, and the metaphyseal regions exhibit excessive flaring. Furthermore, achondroplastic femurs frequently demonstrate exaggerated anterolateral bowing and altered mechanical axes, which fundamentally change the bending moments and stress distributions across the bone during traumatic loading.
Comorbidities and Preinjury Functional Baseline
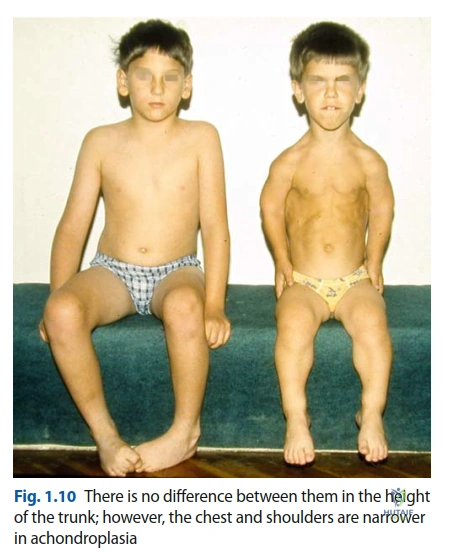
The patient’s medical history was significant for chronic lumbar spinal stenosis, a ubiquitous complication in adult achondroplasia due to congenitally short pedicles, decreased interpedicular distances, and exaggerated lumbar lordosis. This was managed conservatively with targeted physical therapy and non-steroidal anti-inflammatory drugs, without the need for prior surgical decompression. He also had a history of recurrent childhood otitis media resulting in mild conductive hearing loss, related to the altered anatomy of the Eustachian tubes and midface hypoplasia.
Prior to the injury, the patient was an independent, community-dwelling ambulator without the use of assistive devices. He had no history of prior orthopedic surgeries, fragility fractures, or metabolic bone disease. He was a non-smoker and rarely consumed alcohol, optimizing his baseline physiological capacity for tissue healing. His pre-injury knee range of motion was documented in previous clinical records as 0 to 130 degrees of flexion, with a baseline elbow extension deficit of 15 degrees, both of which are standard phenotypic variations within the achondroplastic population.
Clinical Examination Findings
Advanced Trauma Life Support Secondary Survey
Following the primary survey and initial stabilization, a meticulous secondary survey was conducted. The patient exhibited the classic morphologic features of achondroplasia, with a measured stature of 130 centimeters. Inspection of the axial skeleton revealed mild thoracolumbar kyphosis transitioning into a hyper-lordotic lumbar spine. No midline spinal tenderness or step-offs were palpated, and the pelvis was stable to anterior-posterior and lateral compression forces. The bilateral upper extremities and the right lower extremity were entirely unremarkable, demonstrating full baseline range of motion without focal tenderness or deformity.
Orthopedic Assessment of the Distal Femur
Focused examination of the left lower extremity revealed profound pathological alterations. A gross varus deformity was immediately apparent at the level of the distal thigh and knee joint, accompanied by an apparent limb shortening of approximately 4 centimeters compared to the contralateral side. Massive soft tissue swelling and extensive ecchymosis extended from the mid-thigh distally to the proximal tibia, obliterating the normal topographic landmarks of the patella and femoral condyles.
The skin envelope remained intact, with no evidence of open traumatic wounds, abrasions, or degloving injuries (Morel-Lavallée lesions). However, the extreme tension of the soft tissue envelope necessitated close monitoring for impending soft tissue compromise. Palpation elicited exquisite, localized tenderness circumferentially around the distal femur. Palpable crepitus was readily appreciated with minimal manipulation, confirming the presence of a highly unstable, displaced fracture. Active range of motion of the knee was completely absent due to a mechanical block and severe pain inhibition. Passive motion was not attempted to prevent further displacement of fracture fragments and potential iatrogenic neurovascular injury.
Neurovascular and Compartment Syndrome Evaluation
Given the high-energy mechanism and the proximity of the fracture to the popliteal fossa, a rigorous neurovascular assessment was paramount. The popliteal artery is tethered proximally at the adductor hiatus and distally at the soleus arch, making it highly susceptible to traction or transection injuries in the setting of displaced distal femur fractures.
Vascular examination revealed palpable and symmetric dorsalis pedis and posterior tibial pulses. Capillary refill in the distal tufts of the toes was brisk, occurring in less than two seconds. Ankle-brachial indices were deferred given the strong palpable pulses, but the threshold for obtaining a CT angiogram remained low if any vascular asymmetry developed.
Neurological examination assessed the major motor and sensory distributions of the lower extremity. Sensation was intact to light touch and pinprick in the distributions of the superficial peroneal (dorsum of the foot), deep peroneal (first web space), saphenous (medial leg and foot), sural (lateral foot), and tibial (plantar aspect) nerves. Motor function, while limited by pain, demonstrated intact extensor hallucis longus (deep peroneal), tibialis anterior (deep peroneal), peroneus longus and brevis (superficial peroneal), and gastrocnemius-soleus complex (tibial) function.
The fascial compartments of the thigh and leg were palpated to assess for acute compartment syndrome. While the thigh compartments were tense due to fracture hematoma, they were compressible, and the patient did not exhibit pain out of proportion to the injury or pain with passive stretch of the toes. Continuous serial examinations were instituted to monitor for the delayed onset of compartment syndrome.
Imaging and Diagnostics
Plain Radiography Analysis
Initial orthogonal plain radiographs of the left femur and knee were obtained in the trauma bay to delineate the fracture pattern and guide immediate management.

The anteroposterior and lateral projections confirmed a catastrophic, high-energy distal femoral fracture. The images demonstrated a highly comminuted, intra-articular fracture extending from the joint surface proximally into the metaphyseal-diaphyseal junction. A distinct intercondylar split was visible, separating the medial and lateral femoral condyles and disrupting the articular congruity of the patellofemoral and tibiofemoral joints.
The metaphyseal region exhibited severe comminution with multiple intermediate cortical fragments. The overall alignment was grossly distorted, characterized by significant varus angulation, posterior translation of the condylar block (driven by the unopposed pull of the gastrocnemius muscles), and axial shortening. The bone quality appeared robust, consistent with achondroplasia, but the geometric proportions—specifically the wide metaphyseal flare transitioning rapidly into a narrow, bowed diaphysis—were highly abnormal.
Advanced Computed Tomography and Articular Mapping
To comprehensively evaluate the articular involvement and facilitate preoperative templating, a non-contrast Computed Tomography scan of the left distal femur and knee was executed.
The axial, coronal, and sagittal reformats provided critical details regarding the fracture morphology. The CT scan confirmed a Müller AO/OTA 33-C3 classification, denoting a complete articular fracture with multifragmentary metaphyseal and articular comminution.
Crucially, the sagittal reformats revealed a displaced coronal plane fracture of the lateral femoral condyle—a Hoffa fragment (AO/OTA 33-B3). This is a classic finding in high-energy axial load injuries and requires independent, specific fixation strategies (typically anterior-to-posterior interfragmentary screws) to prevent catastrophic articular collapse postoperatively. The CT also mapped the extent of the metaphyseal void, indicating that significant bone loss or impaction had occurred, which would likely necessitate biological augmentation during the reconstruction.
Three Dimensional Reconstruction and Templating
Three-dimensional surface-rendered CT reconstructions were generated to provide a spatial understanding of the fracture fragments and to assist in the conceptualization of the reduction sequence.
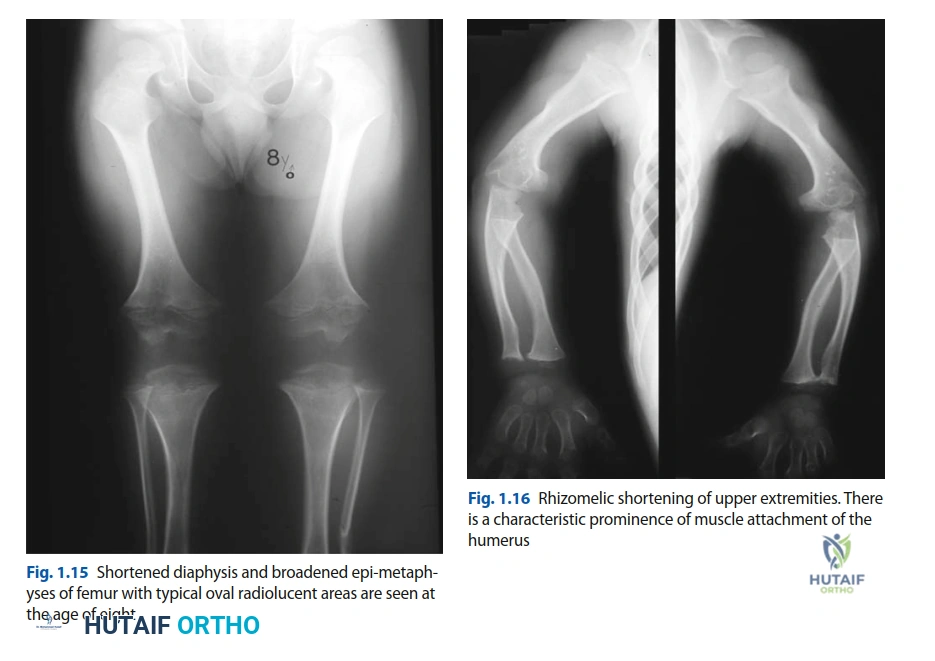
The 3D models vividly illustrated the rotational deformity of the condylar fragments and the severity of the metaphyseal comminution. Preoperative templating in this patient presented an extraordinary challenge. Standard distal femoral locking plates are designed based on the anatomic parameters of the normal adult femur, which features a specific radius of curvature and a gradual metaphyseal flare.
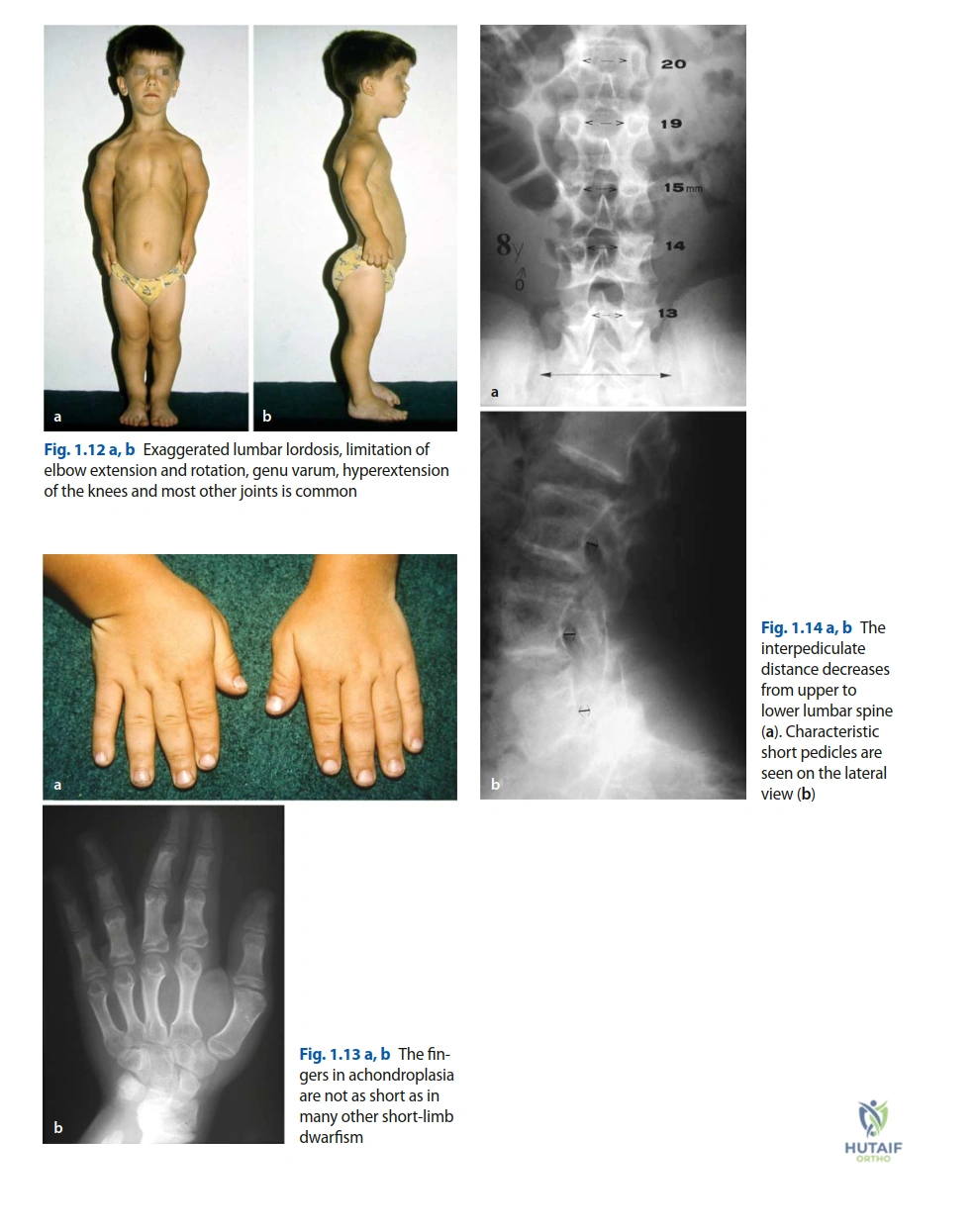
In the achondroplastic femur, the exaggerated anterolateral bow, the abrupt metaphyseal-diaphyseal transition, and the narrow medullary canal render standard off-the-shelf implants geometrically mismatched. Templating software was utilized to overlay various implant options, revealing that standard lateral distal femoral plates would stand off significantly from the diaphyseal cortex if the articular block was reduced anatomically. This necessitated a preoperative plan involving extensive plate contouring, the potential use of shorter, broader plates, or the application of dual plating techniques to achieve stable fixation without inducing iatrogenic malalignment.
Differential Diagnosis
Diagnostic Considerations in High Energy Knee Trauma
When a patient presents with high-energy trauma to the knee and distal thigh, the differential diagnosis must encompass a spectrum of osseous, ligamentous, and vascular injuries. While the plain radiographs definitively diagnosed a distal femoral fracture, the initial clinical presentation of gross deformity, instability, and massive swelling requires the systematic exclusion of other concomitant or alternative pathologies.
| Diagnostic Consideration | Clinical Presentation Profile | Radiographic and Advanced Imaging Findings | Primary Management Strategy |
|---|---|---|---|
| Distal Femoral Intra Articular Fracture AO 33 C3 | Gross deformity of distal thigh, varus/valgus instability, severe localized tenderness, palpable crepitus, inability to bear weight. | Plain films show metaphyseal comminution and intercondylar split. CT confirms articular step-off, Hoffa fragments, and metaphyseal void. | Operative fixation (Dual plating or IM nailing if anatomy permits). Anatomic reduction of articular surface is mandatory. |
| Complex Tibial Plateau Fracture AO 41 C | Swelling localized slightly more distally over the proximal tibia. Joint effusion, varus/valgus instability at the joint line. | Plain films demonstrate depression or splitting of the medial/lateral tibial plateaus. CT required to map articular depression and fragment orientation. | Operative fixation with lateral and/or medial buttress plating. Elevation of depressed articular segments with bone grafting. |
| Traumatic Knee Dislocation KD V | Extreme instability in multiple planes. High risk of spontaneous reduction prior to arrival. High incidence of neurovascular compromise (popliteal artery, peroneal nerve). | Plain films may show asymmetric joint spaces or avulsion fractures (Segond, fibular head). MRI confirms multiligamentous rupture (ACL, PCL, MCL, LCL). | Immediate closed reduction if dislocated. Emergent vascular intervention if ischemic. Staged ligamentous reconstruction post-stabilization. |
| Periprosthetic or Pathologic Fracture | History of prior arthroplasty or known primary malignancy/metastatic disease. May occur with low-energy mechanisms. | Radiographs show fracture propagating around an existing implant or through a lytic/blastic osseous lesion. | Revision arthroplasty, bypass plating, or oncologic resection depending on the underlying etiology and bone stock. |
In this specific case, the definitive radiographic evidence of a highly comminuted distal femoral fracture superseded other primary diagnoses. However, the high-energy nature of the trauma mandated a high index of suspicion for concomitant ligamentous injuries, which are frequently masked by the osseous instability and can only be accurately assessed intraoperatively or postoperatively once skeletal stability is restored.
Surgical Decision Making and Classification
Fracture Classification Systems
The fracture was meticulously classified using the Müller AO/OTA classification system, which categorizes distal femoral fractures based on their anatomical location and the severity of articular and metaphyseal involvement. The distal femur is designated as bone segment 33. Type A fractures are extra-articular; Type B are partial articular (involving only one condyle); and Type C are complete articular fractures, where the articular surface is detached from the diaphysis.
This patient sustained a 33-C3 fracture, the most severe category, characterized by a complete articular fracture with multifragmentary articular and metaphyseal comminution. The presence of a coronal plane Hoffa fragment further complexified the injury pattern. The C3 classification implies a high-energy mechanism, significant soft tissue stripping, and a profoundly challenging surgical reconstruction due to the lack of intact structural landmarks to guide reduction.
Indications for Operative Intervention
Non-operative management of displaced, intra-articular distal femoral fractures is historically associated with catastrophic outcomes, including severe malunion, profound joint stiffness, post-traumatic osteoarthritis, and the systemic complications of prolonged immobilization (deep vein thrombosis, pulmonary embolism, decubitus ulcers, and pneumonia). Therefore, operative intervention is the absolute standard of care for this injury pattern.
The primary surgical objectives are the anatomic restoration of the articular surface to minimize post-traumatic arthrosis, the restoration of mechanical alignment (length, rotation, and angulation) to ensure proper load transfer across the knee joint, and the achievement of stable internal fixation to permit early, active range of motion and functional rehabilitation.
Implant Selection and Biomechanical Considerations
The selection of the optimal fixation construct in an achondroplastic patient with a 33-C3 fracture requires a profound understanding of orthopedic biomechanics. The standard armamentarium for distal femoral fractures includes retrograde intramedullary nails, single lateral locking plates, dual plating constructs, and distal femoral replacement (megaprosthesis).
Retrograde intramedullary nailing was strictly contraindicated in this case. The severe intra-articular comminution and the presence of a Hoffa fragment precluded the safe establishment of a stable entry portal in the intercondylar notch. Furthermore, the narrow medullary canal and the exaggerated anterolateral bowing of the achondroplastic femur would make nail passage impossible without iatrogenic fracture or severe malalignment.
Distal femoral replacement is typically reserved for elderly, low-demand patients with severe osteopenia or pre-existing severe osteoarthritis, allowing for immediate weight-bearing. In a healthy 35-year-old patient, joint preservation is paramount to ensure long-term functional survivorship.
Therefore, plate osteosynthesis was the definitive choice. Historically, single lateral locked plating was the workhorse for these injuries. However, contemporary biomechanical studies have demonstrated that in the presence of severe medial metaphyseal comminution (a medial void), a single lateral plate is subjected to massive cyclic bending moments, leading to a high incidence of varus collapse, plate fatigue failure, and nonunion.
To counteract these biomechanical forces, a dual plating strategy was selected. This involves the application of a robust lateral distal femoral locking plate combined with a medial buttress plate. The dual construct significantly increases the torsional rigidity and axial load-bearing capacity of the fixation, effectively neutralizing the varus bending moments and providing a stable mechanical environment for secondary bone healing in the comminuted metaphyseal segment. The unique challenge remained the geometric mismatch between standard plates and the achondroplastic bone, necessitating intraoperative plate contouring.
Surgical Technique and Intervention
Patient Positioning and Operating Room Setup
The patient was brought to the operating theater and placed in the supine position on a fully radiolucent Jackson flat table. General endotracheal anesthesia was induced, and prophylactic intravenous antibiotics (Cefazolin) were administered prior to incision. A non-sterile tourniquet was placed high on the left proximal thigh to facilitate a bloodless surgical field during the critical articular reduction phase. A bump was placed beneath the ipsilateral hip to internally rotate the leg, neutralizing the natural external rotation of the lower extremity and bringing the patella to a direct anterior zenith. The entire left lower extremity was prepped and draped in a standard sterile fashion, allowing for full, unhindered manipulation of the hip and knee. A sterile bump was positioned beneath the knee to maintain approximately 30 to 40 degrees of flexion, which relaxes the deforming pull of the gastrocnemius muscles on the distal condylar fragments.
Surgical Approaches to the Distal Femur
To address the complex 33-C3 fracture pattern and facilitate dual plating, a dual-incision approach was planned.
First, a standard lateral parapatellar approach was utilized. The incision extended from the lateral aspect of the tibial tubercle, coursing proximally along the lateral border of the patella, and continuing along the anterolateral aspect of the distal thigh. The iliotibial band was incised in line with its fibers. The vastus lateralis was elevated off the lateral intermuscular septum, taking meticulous care to ligate the perforating branches of the profunda femoris artery. The joint capsule was incised, providing excellent visualization of the lateral femoral condyle, the intercondylar notch, and the trochlear groove.
Subsequently, a limited medial subvastus approach was executed to access the medial femoral condyle and the medial metaphysis. A longitudinal incision was made over the medial distal thigh. The fascia overlying the vastus medialis was incised, and the muscle belly was elevated anteriorly and superiorly, exposing the medial periosteum of the distal femur while preserving the adductor magnus insertion at the adductor tubercle.
Articular Reduction and Provisional Fixation
The critical first phase of the operation was the precise, anatomic reconstruction of the articular block. The fracture hematoma was evacuated, and the joint was thoroughly irrigated to remove osteochondral debris. The Hoffa fracture of the lateral femoral condyle was addressed initially. The coronal fracture plane was debrided, and the fragment was anatomically reduced using pointed Weber reduction forceps. Provisional fixation was achieved with multiple 1.6-millimeter Kirschner wires. Definitive fixation of the Hoffa fragment was accomplished utilizing three 3.5-millimeter headless compression screws inserted from anterior to posterior, ensuring the screw heads were countersunk beneath the articular cartilage to prevent patellofemoral impingement.
Following the stabilization of the coronal plane, the sagittal intercondylar split was reduced. The medial and lateral condyles were manipulated using large periarticular reduction forceps. The anatomic restoration of the trochlear groove and the distal articular surface was confirmed visually and fluoroscopically. The condylar block was provisionally held with smooth Steinmann pins. Definitive intercondylar fixation was achieved with two 6.5-millimeter partially threaded cancellous lag screws, inserted from lateral to medial, compressing the condyles together and recreating a solid, unified articular block.
Metaphyseal Diaphyseal Restoration and Plating Strategy
With the articular block reconstituted, the operation transitioned to the metaphyseal-diaphyseal reconstruction. The goal was to restore length, alignment, and rotation without excessively stripping the delicate periosteal blood supply of the comminuted metaphyseal fragments (bridge plating principle).
A pre-contoured titanium lateral distal femoral locking plate was selected. However, as anticipated during preoperative templating, the standard plate geometry clashed with the achondroplastic femur's exaggerated bow and rapid metaphyseal flare. Utilizing heavy-duty plate benders, the diaphyseal portion of the plate was meticulously contoured intraoperatively to match the patient'
