Operative Management of Mammalian Bite Injuries to the Hand and Upper Extremity
Key Takeaway
Mammalian bite injuries to the hand, particularly human clenched-fist injuries, represent surgical emergencies due to the high risk of deep space infection, septic arthritis, and osteomyelitis. Successful management dictates a high index of suspicion, meticulous surgical debridement, copious irrigation, and targeted antimicrobial therapy. This guide details the pathoanatomy, microbiology, and step-by-step operative protocols required to prevent devastating functional morbidity following human, canine, and feline bite wounds.
Comprehensive Introduction and Patho-Epidemiology
Mammalian bite injuries to the hand and upper extremity represent a ubiquitous yet highly treacherous subset of musculoskeletal trauma, demanding an uncompromising, evidence-based surgical approach. Accounting for millions of emergency department visits globally each year, these injuries possess a disproportionately high potential for devastating functional morbidity. The unique and unforgiving anatomy of the hand—characterized by superficial articulations, delicate extensor mechanisms, complex synovial sheaths, and relatively avascular deep fascial spaces—renders it exceptionally vulnerable to rapidly progressive, deep space infections following penetrating trauma. When the integumentary envelope is breached by a mammalian tooth, a highly virulent, polymicrobial inoculum is forcefully injected into these closed spaces, bypassing the body's primary immunological barriers.
The patho-epidemiology of mammalian bites is intrinsically linked to the specific oral flora of the offending species, dictating the clinical trajectory and the requisite antimicrobial strategy. Dog bites are the most prevalent, comprising approximately 80% to 90% of all reported animal bites. The canine jaw is capable of exerting immense mechanical force—frequently exceeding 400 pounds per square inch (psi). Consequently, canine bites typically present as a heterogeneous amalgamation of deep puncture wounds, ragged lacerations, severe crush injuries, and frank tissue avulsions. The hallmark pathogen in canine bites is Pasteurella multocida, a fastidious gram-negative coccobacillus isolated in up to 50% of cases, which rapidly induces an intense, localized inflammatory response. Furthermore, Capnocytophaga canimorsus, another canine oral commensal, poses a catastrophic threat of overwhelming sepsis, disseminated intravascular coagulation (DIC), and purpura fulminans, particularly in asplenic, cirrhotic, or immunocompromised hosts.
Feline bites, while statistically less common (accounting for 5% to 15% of mammalian bites), carry a paradoxically higher rate of clinical infection, with incidence rates ranging from 50% to an astonishing 80%. The feline mechanism of injury involves sharp, highly slender, needle-like dentition that effortlessly penetrates deep into joints, periosteum, and flexor tendon sheaths. These wounds often present as deceptively small, punctate lesions that rapidly seal over, trapping the inoculum in an anaerobic environment. Pasteurella multocida is isolated in 70% to 80% of feline bites, frequently precipitating severe pain, aggressive erythema, and purulent tenosynovitis within a mere 12 to 24 hours of inoculation. The rapid onset of symptoms is pathognomonic for feline-induced Pasteurella infections and requires emergent surgical evaluation.
Human bite injuries, conversely, are universally regarded by hand surgeons as the most dangerous of all mammalian bites due to the profound virulence of human saliva and the deceptive mechanisms of injury. Human saliva harbors over 600 distinct species of bacteria, with microbial concentrations reaching a staggering $10^8$ organisms per milliliter. Infections are virtually always polymicrobial, featuring a synergistic blend of aerobes (such as Staphylococcus aureus and Streptococcus viridans) and aggressive anaerobes (Peptostreptococcus, Bacteroides, and Fusobacterium). Of critical importance is Eikenella corrodens, a gram-negative, facultative anaerobe present in up to 30% of human bite infections. Eikenella acts synergistically with other aerobic organisms to accelerate tissue necrosis and osteocartilaginous destruction. Crucially, E. corrodens exhibits intrinsic resistance to first-generation cephalosporins, macrolides, and clindamycin, rendering standard empiric cellulitis therapy profoundly inadequate and highlighting the necessity for specialized, culture-directed antimicrobial regimens alongside aggressive surgical debridement.
Detailed Surgical Anatomy and Biomechanics
To fully comprehend the pathophysiology of mammalian bite injuries, the orthopedic surgeon must possess an intimate understanding of the intricate functional anatomy and biomechanics of the hand, particularly the dorsal apparatus and the metacarpophalangeal (MCP) joints. The dorsal integument of the hand is exceptionally thin and pliable, lacking the robust subcutaneous adipose tissue that protects the palmar surface. Immediately deep to this fragile dermal layer lies the extensor mechanism, the dorsal joint capsules, and the periosteum of the metacarpals and phalanges. Because these critical structures are virtually subcutaneous, even relatively superficial mammalian bites can easily violate the synovial spaces, inoculating the joint or tendon sheath with highly virulent oral flora.
The "Clenched-Fist Injury" (CFI), colloquially known as the "fight bite," represents the quintessential biomechanical disaster of the upper extremity. The injury typically occurs when a patient strikes an opponent's tooth with a closed fist, most frequently impacting the dorsal aspect of the third or fourth MCP joint. The pathophysiology of the CFI is entirely dictated by the biomechanics of the extensor apparatus during the strike. At the exact moment of impact, the MCP joint is in a state of maximal flexion (approximately 80 to 90 degrees). In this position, the extensor digitorum communis (EDC) tendon and the sagittal bands are pulled tightly over the metacarpal head, and the dorsal joint capsule is maximally taut. The opponent's incisor acts as a contaminated trocar, penetrating the skin, piercing the stretched extensor tendon, violating the dorsal joint capsule, and ultimately striking the articular cartilage or metacarpal head, thereby depositing a concentrated bolus of polymicrobial human saliva directly into the intra-articular space.
The true treachery of the CFI manifests immediately following the impact. When the patient subsequently relaxes the hand and extends the fingers, the anatomical layers undergo significant longitudinal translation. The skin glides proximally, the extensor tendon retracts proximally by up to 15 to 20 millimeters, and the joint capsule shifts. This differential excursion completely misaligns the initial puncture tracts through the various tissue layers. Consequently, a highly effective, physiological "one-way valve" is created. The contaminated intra-articular space is completely sealed off from the external environment, trapping the virulent bacteria within the avascular, nutrient-rich synovial fluid. This closed-space phenomenon rapidly establishes an anaerobic environment, precipitating exponential bacterial proliferation, enzymatic degradation of the articular cartilage, and fulminant septic arthritis.
Beyond the dorsal MCP joints, mammalian bites frequently compromise the complex network of deep fascial spaces and synovial sheaths within the hand. Feline bites to the palmar aspect of the digits are notorious for penetrating the flexor tendon sheaths, leading to acute purulent flexor tenosynovitis. The synovial sheaths provide an uninterrupted, avascular highway for purulent exudate to track proximally into the hand. Infections of the index, middle, and ring fingers can rupture into the midpalmar or thenar spaces, while infections of the thumb and small finger can track proximally via the radial and ulnar bursae, respectively, potentially communicating via the space of Parona in the distal forearm. Understanding these anatomical conduits is absolutely paramount for the surgeon, as it dictates the necessity for extensive, multi-compartmental surgical exploration and decompression.
Exhaustive Indications and Contraindications
The decision to proceed with operative intervention in the setting of mammalian bite injuries is governed by the mechanism of injury, the offending species, the anatomical location of the bite, and the time elapsed since inoculation. Conservative management of deep bite wounds to the hand is fraught with peril and frequently culminates in irreversible functional loss. The threshold for surgical exploration must remain exceedingly low, particularly in the context of human clenched-fist injuries and deep feline punctures.
Absolute indications for emergent surgical exploration and debridement include any clinical evidence of established deep space infection. This encompasses septic arthritis (characterized by severe pain with micromotion of the joint, joint effusion, and periarticular erythema), purulent flexor tenosynovitis (manifesting as Kanavel's four cardinal signs: fusiform swelling, flexed resting posture, extreme tenderness along the flexor sheath, and excruciating pain with passive extension), and deep fascial space abscesses. Furthermore, any clenched-fist injury presenting more than 24 hours post-injury must be considered infected and requires formal operative arthrotomy, regardless of the subtlety of the overlying skin puncture. Radiographic evidence of retained foreign bodies (such as radiopaque tooth fragments) or associated fractures with cortical violation also mandates immediate surgical intervention.
Relative indications for surgery include early presentations (less than 12 to 24 hours) of deep puncture wounds, particularly those overlying joints or tendon sheaths, where the depth of penetration cannot be definitively ascertained via local wound exploration in the emergency department. While some highly compliant patients with early, superficial canine lacerations may be managed with aggressive emergency department irrigation and close outpatient follow-up, any ambiguity regarding capsular or sheath violation necessitates formal exploration in the operating theater.
Contraindications to immediate operative intervention are exceedingly rare but must be considered in the context of the patient's overall physiological stability. Hemodynamic instability or profound systemic shock secondary to overwhelming sepsis (e.g., Capnocytophaga bacteremia) may necessitate initial medical resuscitation, broad-spectrum intravenous antimicrobial therapy, and stabilization in the intensive care unit prior to definitive surgical debridement, though source control remains a critical component of resuscitation. Additionally, purely superficial abrasions or scratches that definitively do not breach the dermis or involve deep structures can be safely managed non-operatively with local wound care and prophylactic antibiotics.
| Indication Category | Specific Clinical Scenarios | Surgical Rationale |
|---|---|---|
| Absolute Indications | Septic arthritis of any hand/wrist joint | Prevent irreversible chondrolysis and joint destruction. |
| Absolute Indications | Purulent flexor tenosynovitis (Kanavel's signs) | Prevent tendon necrosis, rupture, and proximal spread. |
| Absolute Indications | Deep space abscess (thenar, midpalmar, hypothenar) | Evacuate purulence, decompress fascial compartments. |
| Absolute Indications | Clenched-Fist Injury (CFI) presenting > 24 hours | High probability of sealed intra-articular infection. |
| Absolute Indications | Retained foreign body (e.g., tooth fragment) | Remove nidus for persistent infection and foreign body reaction. |
| Absolute Indications | Concomitant open fracture (e.g., metacarpal neck) | Debride bone, prevent osteomyelitis, stabilize fracture. |
| Relative Indications | Early (< 24h) deep puncture over a joint/tendon | Prophylactic exploration to rule out capsular/sheath violation. |
| Relative Indications | Severe canine crush injury with devitalized tissue | Excise necrotic muscle/fat to prevent secondary infection. |
| Contraindications | Purely superficial epidermal abrasions/scratches | No deep space involvement; amenable to local wound care. |
| Contraindications | Hemodynamic instability (requires resuscitation first) | Delay definitive orthopedic surgery until medically optimized for anesthesia, though bedside source control may be needed. |
Pre-Operative Planning, Templating, and Patient Positioning
Thorough pre-operative planning is the cornerstone of successful surgical management of mammalian bite injuries. The clinical evaluation must begin with a high index of suspicion, as patients—particularly those with clenched-fist injuries—frequently provide deceptive histories due to embarrassment, intoxication, or fear of legal repercussions. They may attribute the dorsal MCP laceration to a fall against a wall or a crush injury. The astute orthopedic surgeon must adhere to the fundamental axiom: Any laceration over the dorsal aspect of the metacarpophalangeal joint must be treated as a human bite until definitively proven otherwise.
Physical examination requires meticulous attention to anatomical detail. The surgeon must actively assess for erythema, induration, calor, and lymphangitis tracking proximally up the forearm. The extensor mechanism must be evaluated for extensor lag, which may indicate a complete or partial laceration of the EDC tendon or sagittal band rupture. Crucially, the wound must be examined with the patient's hand placed in the exact position of injury (typically full fist flexion). Only by recreating the biomechanics of the strike can the surgeon visualize the true extent of the capsular penetration and the alignment of the puncture tracts.
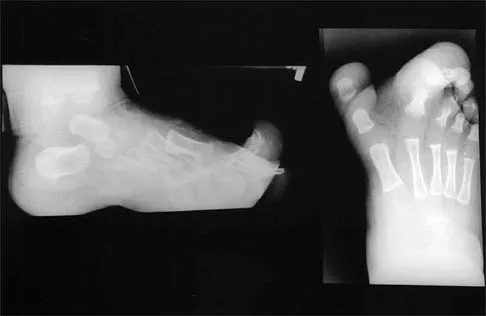
Radiographic evaluation is absolutely mandatory for all mammalian bite injuries to the hand. Standard posteroanterior, lateral, and oblique radiographs must be scrutinized. The surgeon is actively evaluating for three primary pathologies: 1) Concomitant fractures, most notably the "boxer's fracture" (metacarpal neck fracture) which frequently accompanies a CFI; 2) Cortical violations, indentations, or periosteal reactions that indicate direct dental impact on the bone; and 3) Retained radiopaque foreign bodies, particularly human or animal tooth fragments, which can be surprisingly subtle and easily obscured by the complex overlapping osseous anatomy of the hand. In cases of delayed presentation with suspected deep space abscesses, advanced imaging such as ultrasonography or contrast-enhanced Magnetic Resonance Imaging (MRI) may be utilized to delineate the extent of fluid collections, though imaging should never delay emergent surgical exploration in a clinically obvious infection.
Pre-operative laboratory workup should include a complete blood count (CBC) with differential, erythrocyte sedimentation rate (ESR), and C-reactive protein (CRP) to establish a baseline for monitoring therapeutic response. Blood cultures should be obtained in patients exhibiting systemic signs of toxicity (fevers, chills, tachycardia).
Patient positioning and anesthesia are critical components of the operative plan. The procedure is optimally performed under regional anesthesia, specifically a brachial plexus block (supraclavicular or axillary), which provides excellent intra-operative analgesia and beneficial post-operative sympathetic blockade, enhancing peripheral perfusion. General anesthesia is reserved for uncooperative patients, pediatric populations, or cases requiring extensive proximal exploration. The patient is positioned supine with the affected extremity extended on a radiolucent hand table. A proximal pneumatic arm tourniquet is applied. Crucially, exsanguination of the limb prior to tourniquet inflation must be performed via simple gravity elevation for 3 to 5 minutes rather than using an Esmarch bandage. Compressive exsanguination with an Esmarch bandage is strictly contraindicated in the setting of infection, as it risks forcefully extruding purulent material and bacteria proximally into uncompromised fascial planes and the systemic circulation.
Step-by-Step Surgical Approach and Fixation Technique
The operative management of mammalian bites, particularly the human clenched-fist injury, requires a meticulous, systematic approach focused on aggressive debridement, copious irrigation, and the absolute avoidance of primary closure.
1. Incision and Exposure
The surgeon must never rely solely on the traumatic puncture wound for access, as it provides wholly inadequate visualization of the deep structures. For a dorsal MCP joint injury, the puncture wound should be extended longitudinally or via a lazy-S incision. The lazy-S approach is preferred as it prevents the formation of a restrictive linear scar contracture over the joint. Full-thickness skin flaps are carefully elevated and retracted using fine skin hooks or self-retaining retractors, preserving the delicate dorsal venous network and the terminal branches of the radial and ulnar sensory nerves.
2. Tendon Inspection and Arthrotomy
Once the superficial tissues are retracted, the extensor apparatus is meticulously inspected. The finger must be passively flexed by the assistant to recreate the exact position of injury. This maneuver is critical; it brings the lacerated portion of the extensor tendon or sagittal band—which had retracted proximally during extension—directly into the operative field. If the dorsal joint capsule has been violated, the traumatic arthrotomy is formally extended longitudinally to expose the articular surface.
3. Debridement and Joint Exploration
The intra-articular space is systematically inspected. Any macroscopic purulence, fibrinous exudate, or hematoma is evacuated and sent for immediate aerobic, anaerobic, and fungal cultures. The laboratory must be specifically alerted to hold cultures for prolonged periods to isolate fastidious organisms like Eikenella corrodens and Pasteurella multocida. The articular cartilage and metacarpal head are inspected for osteochondral defects or embedded tooth fragments. All necrotic, macerated, and devitalized tissue—including frayed tendon edges, damaged capsule, and non-viable skin margins—must be sharply excised until healthy, bleeding tissue is encountered.
4. High-Volume Irrigation
Following thorough sharp debridement, the wound and joint space undergo high-volume, low-pressure irrigation. A minimum of 3 to 5 liters of normal saline is utilized. Low-pressure irrigation (e.g., via a bulb syringe or gravity tubing) is vastly superior to high-pressure pulsatile lavage in the hand, as high-pressure systems can inadvertently dissect delicate fascial planes and drive particulate matter and bacteria deeper into the synovial sheaths.
5. Management of Concomitant Fractures (Fixation Technique)
If the bite injury is associated with a metacarpal fracture (e.g., a highly contaminated boxer's fracture), the management of the bone becomes a complex clinical challenge. Internal fixation with plates and screws is generally contraindicated in the acute setting of a grossly contaminated bite wound due to the unacceptably high risk of deep implant-associated osteomyelitis. If the fracture is relatively stable, it may be managed non-operatively with splinting once the soft tissue infection is cleared. However, if the fracture is grossly unstable, shortened, or malrotated, temporary skeletal stabilization is required. This is optimally achieved using percutaneous Kirschner wires (K-wires) placed away from the primary zone of injury, or via a mini-external fixator. Definitive internal fixation, if necessary, is strictly delayed until the wound is clean, granulating, and all clinical signs of infection have resolved.
6. Wound Management and Closure Strategy
The most critical tenet of mammalian bite surgery is this: Never primarily close a human bite wound, a deep feline puncture, or a severely contaminated canine crush injury. Primary closure of these wounds is a catastrophic error that virtually guarantees the development of a closed-space infection. The joint capsule, the extensor tendon laceration, and the skin must be left completely open. The wound is packed loosely with saline-moistened gauze or a non-adherent dressing (e.g., Xeroform) to allow for continuous egress of fluid and secondary intention healing. In select cases with massive tissue defects, negative pressure wound therapy (NPWT) may be applied, provided there is no active purulence or exposed articular cartilage. Tendon repairs are strictly delayed; attempting to primarily repair an EDC tendon in a contaminated bed will inevitably lead to infection and rupture.
Complications, Incidence Rates, and Salvage Management
Failure to adhere to the rigorous surgical principles outlined above, or delayed presentation by the patient, can lead to a cascade of catastrophic complications. The avascular nature of the flexor tendon sheaths and articular cartilage means that once infection is established, tissue destruction is rapid and often irreversible.
Septic arthritis is the most feared complication, leading to rapid chondrolysis mediated by bacterial proteases and the host's own lysosomal enzymes. If the articular cartilage is destroyed, the joint cannot be salvaged in its native form. Osteomyelitis frequently occurs when the tooth penetrates the periosteum, particularly in feline bites, or as a sequela of neglected septic arthritis. Tendon rupture is a common complication of purulent flexor tenosynovitis, resulting from both the enzymatic degradation of the collagen matrix and the ischemic necrosis caused by increased pressure within the closed synovial sheath.
In immunocompromised patients, diabetics, or those with peripheral vascular disease, localized infections can rapidly progress to necrotizing fasciitis, gangrene, and systemic sepsis, ultimately necessitating digital, ray, or even proximal limb amputation to save the patient's life.
| Complication | Estimated Incidence (Untreated/Delayed) | Pathophysiology | Salvage Management Strategy |
|---|---|---|---|
| Septic Arthritis | 30% - 50% (in CFIs) | Bacterial proteases and host enzymes cause rapid articular cartilage degradation. | Serial operative debridements; eventual joint arthrodesis or arthroplasty (delayed). |
| Osteomyelitis | 10% - 20% | Direct bacterial inoculation into bone or contiguous spread from joint/soft tissue. | Radical bone debridement, prolonged IV antibiotics, possible bone grafting or ray amputation. |
| Tendon Rupture | 15% - 25% (in tenosynovitis) | Ischemic necrosis from sheath pressure and enzymatic collagen degradation. | Two-stage tendon reconstruction (Hunter rod) after complete eradication of infection. |
| Stiffness / Contracture | 50% - 70% | Adhesion formation between tendon, capsule, and skin; prolonged immobilization. | Intensive hand therapy, dynamic splinting, eventual surgical tenolysis/capsulotomy. |
| Amputation | < 5% (Higher in diabetics) | Uncontrollable necrotizing infection, gangrene, or overwhelming systemic sepsis. | Ray resection or proximal amputation to achieve definitive source control and save life. |
| Systemic Sepsis (e.g., Capnocytophaga) | Rare but highly lethal | Hematogenous dissemination of virulent flora, leading to DIC and multi-organ failure. | ICU admission, vasopressors, massive broad-spectrum IV antibiotics, emergent source control. |
Phased Post-Operative Rehabilitation Protocols
The post-operative management of mammalian bite injuries represents a delicate balancing act between allowing the inflamed, infected tissues to heal and preventing the profound stiffness and tendon adhesions that inevitably follow hand trauma. A phased, meticulously monitored rehabilitation protocol is essential for optimizing functional outcomes.
Phase I: Immobilization and Infection Control (Days 0 to 3)
Immediately following surgery, the hand is placed in a bulky, compressive soft tissue dressing and immobilized in a custom orthosis in the "safe position" (intrinsic-plus position). This posture—wrist extended 20 to 30 degrees, MCP joints flexed 70 to 90 degrees, and interphalangeal (IP) joints fully extended—places the collateral ligaments of the MCP joints under maximal tension, preventing shortening and subsequent extension contractures. The limb must be strictly elevated above the level of the heart to minimize dependent edema, which exacerbates pain and impedes microvascular perfusion. During this phase, culture-directed intravenous antibiotics are administered. Empiric therapy typically involves a beta-lactamase inhibitor combination (e.g., Ampicillin-sulbactam) to cover aerobes, anaerobes, Eikenella, and Pasteurella.
Phase II: Early Active Motion and Wound Care (Days 3 to 14)
If the clinical trajectory is favorable—evidenced by resolving erythema, decreasing edema, and absence of purulent drainage—the dressing is taken down at 48 to 72 hours. The wound is inspected, and if clean, daily hydrotherapy or gentle washing with soap and water is initiated. Crucially, early active range-of-motion (ROM) exercises are commenced out of the splint. Active tendon gliding is paramount to prevent the extensor or flexor tendons from adhering to the adjacent bone or skin flaps. Passive ROM is generally avoided initially to prevent undue stress on the fragile healing tissues. The patient is transitioned to culture-specific oral antibiotics (e.g., Amoxicillin-clavulanate) for a total course of 7 to 14 days, depending on the severity of the initial infection.
Phase III: Delayed Closure and Functional Restoration (Weeks 2 to 6)
By the second or third week, the open wounds should demonstrate a healthy, robust bed of granulation tissue. Depending on the size of the defect, the wound may be allowed to heal entirely by secondary intention, which often yields surprisingly functional and cosmetically acceptable results in the hand. Alternatively, delayed primary closure or the application of a split-thickness skin graft may be performed if the defect is excessively large. Once the wound is closed or fully epithelialized, aggressive hand therapy is initiated. This includes dynamic splinting to address any residual contractures, scar massage, and progressive strengthening exercises. If an extensor tendon was lacerated and left unrepaired during the index procedure, a delayed reconstruction or secondary repair is considered only after the soft tissue envelope is completely stable, supple, and free of any latent infection—typically 3 to 6 months post-injury.
Summary of Landmark Literature and Clinical Guidelines
The modern operative management of mammalian bite injuries is built upon a foundation of landmark microbiological studies and evolving surgical paradigms. Historically, human bite infections were associated with abysmal outcomes, often resulting in widespread amputation. The seminal work by Kanavel in the early 20th century delineated the anatomical fascial spaces and synovial sheaths of the hand, providing the anatomical roadmap necessary for understanding how infections propagate and how they must be surgically decompressed. Kanavel's four cardinal signs of flexor tenosynovitis remain the gold standard for clinical diagnosis to this day.
In the realm of microbiology, the landmark studies by Goldstein and Talan in the 1980s and 1990s revolutionized our understanding of bite flora. Goldstein's exhaustive culturing of human and animal bite wounds definitively established the polymicrobial nature of these injuries and highlighted the critical, synergistic roles of fastidious organisms like Eikenella corrodens and Pasteurella multocida. Their work directly led to the paradigm shift away from traditional penicillin or cephalosporin monotherapy toward the universal adoption of beta-lactam/beta-lactamase inhibitor combinations (e.g., Amoxicillin-clavulanate) as the gold standard empiric therapy.
Current clinical guidelines endorsed by the Infectious Diseases Society of America (IDSA) and the American Society for Surgery of the Hand (ASSH) strongly codify the principles outlined in this chapter. The guidelines unequivocally mandate the avoidance of primary closure for human bites, deep puncture wounds, and clinically infected wounds. Furthermore, they emphasize the necessity of tetanus prophylaxis and the careful consideration of rabies post-exposure prophylaxis (PEP) in accordance with local epidemiological data. The literature consistently reinforces that while antimicrobial therapy is a vital adjunct, it is never a substitute for prompt, aggressive, and meticulous surgical debridement in the management of complex mammalian bite injuries to the upper extremity.
