Revision Total Hip Arthroplasty with Antiprotrusio Cage: An Intraoperative Masterclass for Acetabular Bone Loss
Key Takeaway
Welcome, fellows, to a critical masterclass on revision total hip arthroplasty utilizing an antiprotrusio cage for severe acetabular bone loss. We'll meticulously navigate comprehensive preoperative planning, precise patient positioning, detailed surgical anatomy, and a granular, step-by-step intraoperative execution. Learn to manage complex defects, identify critical neurovascular structures, and optimize implant stability. We'll also cover essential pearls, pitfalls, and post-operative protocols for successful outcomes in these challenging cases.
Comprehensive Introduction and Patho-Epidemiology
Revision Total Hip Arthroplasty (THA) in the setting of severe acetabular bone loss represents one of the most formidable challenges in reconstructive orthopedic surgery. As the volume of primary joint arthroplasties continues to rise globally, a commensurate increase in revision burden is inevitable. While minor acetabular defects can often be managed with standard hemispherical cementless components, massive bone loss—particularly when it compromises the structural integrity of the anterior and posterior columns—demands a far more sophisticated reconstructive strategy. The antiprotrusio cage, originally popularized by Burch and Schneider, remains a cornerstone in our armamentarium for addressing these catastrophic defects, specifically when a press-fit cementless cup is precluded by an absence of viable host bone for initial stability.
The patho-epidemiology of severe acetabular bone loss is multifactorial. Historically, cemented polyethylene cups subjected to particulate wear debris led to massive osteolysis, often remaining asymptomatic until catastrophic failure and medial migration occurred. Today, we frequently encounter secondary bone stock deficiency resulting from aseptic loosening, chronic periprosthetic joint infection (PJI), recurrent dislocations requiring multiple revisions, or iatrogenic bone loss during the extraction of well-fixed but malpositioned porous-coated components. Furthermore, primary conditions such as severe developmental dysplasia of the hip (DDH), rheumatoid arthritis, or Paget’s disease can predispose a patient to protrusio acetabuli, though these less frequently require a cage unless the bone loss is truly massive and uncontained.
The fundamental biomechanical rationale for the antiprotrusio cage is to bypass the deficient acetabular bone and transfer the loads of weight-bearing directly to the intact host bone of the ilium superiorly and the ischium inferiorly. By spanning the massive defect, the cage protects underlying morselized or structural allograft, allowing for gradual incorporation and reconstitution of the host bone stock over time. This concept of "graft protection" is critical; the cage acts as an internal splint, providing immediate mechanical stability while biological healing occurs beneath it. Unlike highly porous metal augments that rely on biological ingrowth for long-term survival, the cage relies on rigid mechanical fixation, making its precise contouring and stable screw fixation absolutely paramount to the success of the procedure.
As we navigate this masterclass, it is imperative to understand that utilizing an antiprotrusio cage is not a mere salvage procedure, but a definitive, highly technical reconstruction. Every detail, from preoperative templating to the precise contouring of the malleable flanges, carries significant weight. The goal is not simply to fill a void, but to restore the anatomic center of rotation, re-establish appropriate biomechanics, and provide the patient with a durable, pain-free articulation. We will walk through this procedure with the meticulous attention to detail required of an academic reconstructive surgeon, ensuring you are equipped to handle the complexities of massive acetabular deficiency.
Detailed Surgical Anatomy and Biomechanics
A profound understanding of pelvic and acetabular anatomy is non-negotiable when undertaking complex revision THA. The acetabulum is a hemispherical cavity formed by the confluence of the ilium, ischium, and pubis, typically oriented with approximately 45 degrees of inclination and 15 degrees of anteversion relative to the true pelvic plane. In the setting of massive bone loss, these normal anatomical landmarks are frequently distorted, obliterated, or entirely absent, requiring the surgeon to rely on deep pelvic anatomy to orient the reconstruction.
The structural integrity of the acetabulum relies on the anterior and posterior columns, an inverted Y-shaped construct that transfers loads from the lower extremity to the axial skeleton. The anterior column extends from the iliac crest to the pubic symphysis, while the posterior column extends from the dense bone of the sciatic notch down to the ischial tuberosity. Between these columns lies the medial wall, the thinnest portion of the acetabulum. The radiographic "teardrop" represents the confluence of the ischium and the pubis at the inferior aspect of the acetabulum. In cases of severe protrusio or pelvic discontinuity, the continuity between the superior ilium and the inferior ischium/pubis is broken, destabilizing the entire hemipelvis and making standard hemispherical cup fixation impossible.
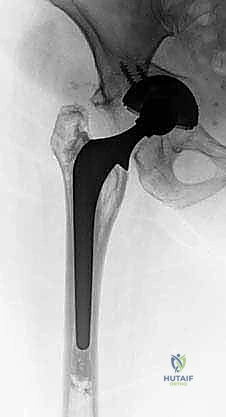
Neurovascular vigilance is the hallmark of a master surgeon in these cases. The proximity of critical structures to the medialized or superiorly migrated acetabulum cannot be overstated. Anteriorly, the external iliac artery and vein lie precariously close to the anterior column and superior pubic ramus. In cases of severe medial migration (medial to Kohler’s line), a fibrous membrane may be the only structure separating a loose implant from these major vessels. Posteriorly, the sciatic nerve exits the greater sciatic notch and runs in close proximity to the posterior column and ischium. When placing the inferior flange of the antiprotrusio cage into the ischium, the trajectory of the fixation screws must be meticulously controlled to avoid penetrating the inner cortex and causing catastrophic sciatic nerve palsy.
Biomechanically, the antiprotrusio cage alters the standard paradigm of acetabular reconstruction. Standard cementless cups require a minimum of 50% host bone contact for reliable initial stability and subsequent osseointegration. When this is unachievable, the cage acts as a load-bearing bridge. The superior flange is secured to the dense cortical bone of the ilium, while the inferior flange is slotted into or screwed onto the ischium. This construct effectively unloads the deficient medial wall and superior dome, transferring the joint reactive forces away from the grafted defects. The polyethylene liner is subsequently cemented into the cage, allowing the surgeon to dial in the exact version and inclination required for stability, independent of the cage's final orientation, thereby optimizing hip biomechanics and abductor tension.
Exhaustive Indications and Contraindications
The decision to utilize an antiprotrusio cage is dictated by the severity of the bone loss and the inability to achieve stable fixation with a hemispherical cementless component. We rely heavily on the Paprosky classification system to categorize these defects and guide our reconstructive algorithm. The cage is primarily indicated for Paprosky Type 3A and Type 3B defects, as well as cases of frank pelvic discontinuity.
Paprosky Type 3A defects are characterized by severe superior migration (greater than 2 cm) with moderate to severe destruction of the superior rim. While the medial wall and ischium are usually present, they may be damaged. In some 3A defects, a jumbo cup with trabecular metal augments may suffice, but if the superior rim cannot support an augment, a cage becomes necessary. Paprosky Type 3B defects involve massive superomedial migration, destruction of the teardrop, and severe ischial damage. In these scenarios, the potential for pelvic discontinuity is exceptionally high. An antiprotrusio cage, often combined with structural allograft or posterior column plating, is the gold standard for bridging this massive defect and restoring pelvic stability.
Contraindications must be strictly observed to prevent devastating failures. The absolute contraindication is an active periprosthetic joint infection. Placing massive amounts of allograft and a large metallic cage in the presence of active sepsis guarantees failure. All infections must be definitively eradicated, typically via a two-stage exchange protocol, before cage reconstruction is attempted. Relative contraindications include inadequate bone stock in the ilium or ischium to support the cage flanges. If the ilium is completely destroyed up to the sacroiliac joint, or if the ischium is entirely absent, alternative salvage procedures, such as a custom triflange acetabular component or a saddle prosthesis, must be considered.
| Indication / Contraindication | Clinical Scenario | Rationale / Management Strategy |
|---|---|---|
| Primary Indication | Paprosky Type 3B Defect | Massive superomedial migration; cage required to bridge defect and protect allograft. |
| Primary Indication | Pelvic Discontinuity | Disruption of anterior/posterior columns; cage acts as internal splint, often with posterior plating. |
| Secondary Indication | Massive Protrusio Acetabuli | Severe medial wall deficiency where impaction grafting alone lacks mechanical support. |
| Absolute Contraindication | Active Periprosthetic Infection | High risk of persistent sepsis; requires two-stage exchange with antibiotic spacer first. |
| Relative Contraindication | Absent Iliac/Ischial Fixation Points | Cage cannot be secured; consider custom triflange implant or alternative salvage. |
| Relative Contraindication | Severe Medical Comorbidities | Prolonged surgical time and blood loss; optimize medically or consider resection arthroplasty. |
Pre-Operative Planning, Templating, and Patient Positioning
Before a scalpel touches the skin, a meticulous preoperative assessment lays the foundation for a successful reconstruction. This intelligence-gathering phase is critical for anticipating intraoperative challenges, formulating a definitive surgical strategy, and ensuring all necessary equipment, allografts, and personnel are available.
The patient's history and physical examination provide the initial clues. We must differentiate intrinsic hip pain from extrinsic sources such as lumbar radiculopathy, spinal stenosis, or vascular claudication. A thorough history helps determine if revision surgery will truly address the patient's chief complaint. Always inquire about previous infections, wound drainage, and pain at rest, which are red flags for septic loosening. "Start-up pain" is a classic indicator of aseptic component loosening. Visual inspection of the skin is crucial; note the location and quality of prior incisions. We require an adequate 6 cm skin bridge between any existing incisions and our planned approach to optimize wound healing and minimize the risk of skin necrosis.
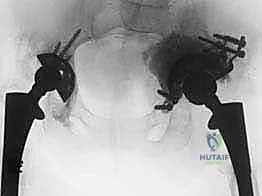
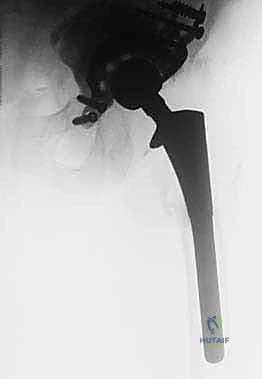
Imaging studies are the roadmap for this complex journey. Plain radiographs, including an AP of the pelvis and AP and true lateral views of the affected hip, are fundamental. These films allow us to classify the bone loss using the Paprosky system and begin our digital templating. However, plain films consistently underestimate the true extent of bone loss. Therefore, a high-resolution CT scan of the pelvis is mandatory. The CT scan provides a precise 3D assessment of the remaining bone stock, the integrity of the columns, and the presence of pelvic discontinuity. Crucially, if a prior implant has migrated medial to Kohler's line, a CT with intravascular contrast is absolutely essential to visualize the proximity of the implant to the external iliac vessels and obturator neurovascular bundle, mitigating the risk of catastrophic hemorrhage during implant extraction. Laboratory studies, including ESR and CRP, are mandatory to rule out subclinical infection; if elevated, a preoperative hip aspiration is required.
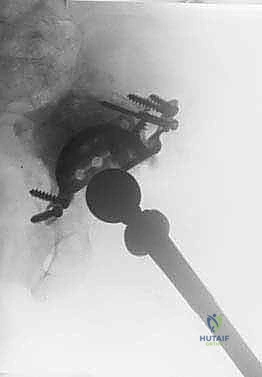
Patient positioning is dictated by the chosen surgical approach and the anticipated need for extensile exposure. For complex revisions requiring an antiprotrusio cage, the lateral decubitus position utilizing a posterior approach is generally preferred. This position offers unparalleled access to the posterior column, the ischium, and the posterior acetabular rim, which are critical areas for cage fixation and potential column plating. The patient must be rigidly secured using a peg board or bean bag to prevent shifting during vigorous reaming or implant extraction. The hip is draped in a wide, sterile fashion, allowing for full range of motion and the potential extension of the incision distally for an extended trochanteric osteotomy (ETO) if required. Intraoperative fluoroscopy must be readily available and positioned to allow for unobstructed AP and lateral views of the hemipelvis without compromising the sterile field.
Step-by-Step Surgical Approach and Fixation Technique
The surgical execution of a cage reconstruction is a highly orchestrated sequence of events. We favor an extensile posterior approach, often combined with an Extended Trochanteric Osteotomy (ETO). The ETO is an invaluable tool in revision THA; it provides direct, straight-line access to the acetabulum, protects the abductor mechanism by reflecting it as a continuous sleeve with the vastus lateralis, and vastly simplifies the removal of a well-fixed or distally subsided femoral stem.
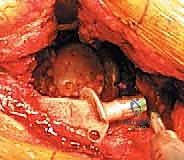
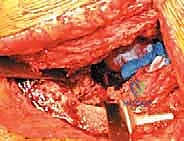
1. Exposure and Component Extraction
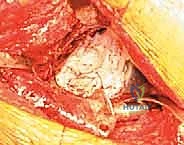
Following the incision and fascial splitting, the posterior structures are identified. If an ETO is not utilized, the external rotators are tagged and released. A thorough capsulectomy is performed to mobilize the proximal femur. The hip is dislocated, and the femoral component is assessed. If the stem is to be retained, it is carefully protected; if it requires revision, it is extracted using appropriate specialized tooling. Attention is then turned to the acetabulum. The removal of the existing acetabular component must be performed with surgical finesse to preserve every millimeter of remaining host bone. Explant systems, curved gouges, and high-speed burrs are utilized to disrupt the bone-implant interface. In cases of severe medial migration, the component is extracted laterally, avoiding any medial leverage that could tear the underlying fibrous membrane and injure the iliac vessels.
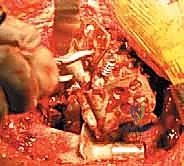
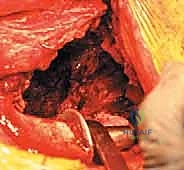
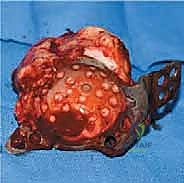
2. Debridement and Defect Assessment
Once the components are removed, a meticulous debridement of all particulate debris, metallosis, and fibrous tissue is performed. The true extent of the bone loss is now revealed. The surgeon must systematically palpate the anterior column, posterior column, superior dome, and ischium. The presence of pelvic discontinuity is assessed by applying traction and rotational forces to the hemipelvis; independent movement of the superior and inferior segments confirms a discontinuity. At this stage, the defect is formally classified, and the preoperative plan is either confirmed or adapted. If a discontinuity is present, consideration is given to plating the posterior column prior to cage insertion to provide initial stability.

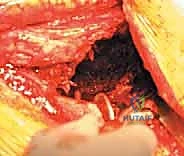
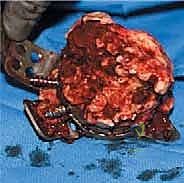
3. Acetabular Preparation and Bone Grafting
The goal of acetabular preparation is not to ream to a hemispherical fit, but merely to remove fibrous tissue and expose bleeding host bone to facilitate graft incorporation. Gentle, reverse reaming or the use of a high-speed burr is preferred. Massive defects are then managed with bone grafting. For contained medial defects, impaction bone grafting is utilized. Cancellous allograft chips (typically 8-10 mm in size) are rigorously washed to remove marrow elements, packed into the defect, and impacted using specialized tamps and reverse reamers to create a dense, stable bed. For uncontained superior or posterior defects, structural allografts (such as a distal femoral or proximal tibial segment) are contoured to fit the void and secured to the host bone with cancellous screws. The structural graft provides mechanical support for the superior flange of the cage.
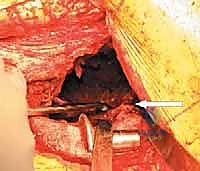
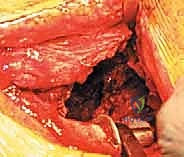
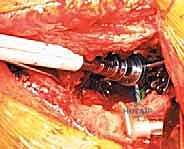
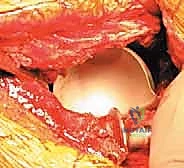
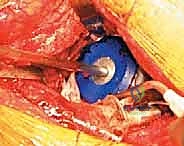
4. Cage Contouring and Insertion
This is the most technically demanding phase of the procedure. The antiprotrusio cage (e.g., Burch-Schneider) must be meticulously contoured to match the patient's specific anatomy. Malleable aluminum templates are used to determine the required bends for the superior (iliac) and inferior (ischial) flanges. The actual titanium or stainless steel cage is then bent using heavy-duty bending irons. Surgical Pearl: Avoid repeated bending of the cage in opposite directions, as this induces metal fatigue and significantly increases the risk of postoperative hardware fracture.
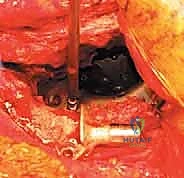

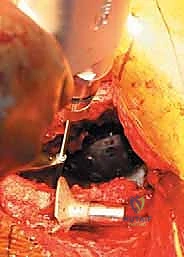
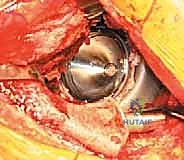
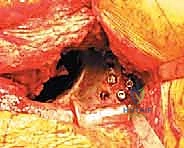
The ischial flange is addressed first. It is either slotted into a prepared cleft in the ischium or secured onto the surface of the ischium with screws. SURGICAL WARNING: When placing screws into the ischium, the sciatic nerve is at extreme risk. The trajectory must be strictly controlled, and finger palpation of the deep ischial surface is recommended to ensure screws do not penetrate the inner cortex. Once the inferior flange is seated, the superior flange is impacted against the ilium and secured with multiple 6.5 mm cancellous screws directed into the dense bone of the sciatic buttress and superior ilium. The cage must achieve absolute, rigid stability; any micro-motion will lead to graft failure and subsequent cage loosening.
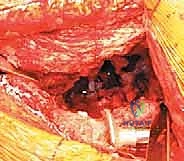
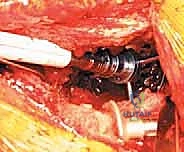
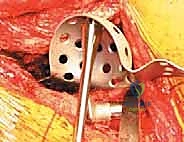

5. Cementation of the Polyethylene Liner
With the cage rigidly fixed, the final step is cementing an all-polyethylene liner into the cage shell. This step allows the surgeon to independently adjust the version and inclination of the articulation, regardless of the cage's spatial orientation. A highly cross-linked polyethylene liner is selected. The inner surface of the cage is thoroughly dried. High-viscosity bone cement is mixed and applied to the cage. The liner is then pressurized into the cement mantle, aiming for an optimal orientation of 40-45 degrees of inclination and 15-20 degrees of anteversion. The hip is reduced, and stability, leg length, and offset are meticulously checked before final closure.
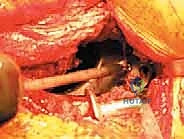
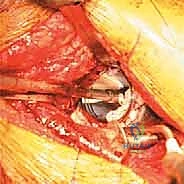
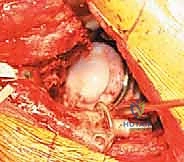
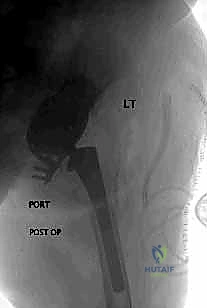
Complications, Incidence Rates, and Salvage Management
Revision THA with an antiprotrusio cage is a high-stakes endeavor associated with a significant complication profile. The extensive exposure, massive bone grafting, and prolonged operative times inherently increase the risk of adverse events. A thorough understanding of these complications and their salvage management is essential for the reconstructive surgeon.
Infection remains one of the most devastating complications, with rates reported between 3% and 8% in complex revisions. The presence of massive avascular allograft and a large metallic implant creates an ideal environment for bacterial colonization. Prophylactic measures, including meticulous dead-space management, copious irrigation, and the use of antibiotic-loaded bone cement, are critical. If a deep periprosthetic joint infection occurs, aggressive management is required. Suppressive antibiotics are rarely successful; definitive treatment necessitates a two-stage exchange arthroplasty, involving complete hardware and graft removal, placement of an articulating or static antibiotic spacer, and a subsequent re-revision once the infection is eradicated.
Instability and dislocation are also distressingly common, with incidence rates ranging from 5% to 15%. This is driven by the alteration of the hip center of rotation, compromised abductor musculature (especially if multiple prior approaches were used), and potential impingement from retained hardware or structural grafts. Meticulous attention to restoring offset, leg length, and proper liner version during the cementation phase is the best prevention. If recurrent
