Revision Hip Success: Unpacking The Case Title Acetabular Grafting
Key Takeaway
This article provides essential research regarding Revision Hip Success: Unpacking The Case Title Acetabular Grafting. Acetabular impaction grafting, detailed in this case title, treats a loosened hip replacement with a large acetabular bone defect. The procedure reconstructs the acetabulum using metallic meshes and morselized bone allograft, followed by cementing a new cup. This restores hip function for patients experiencing groin pain and walking restrictions, such as a 78-year-old female.
Patient Presentation and History
History of Present Illness
We present the case of an 82-year-old male, independent in his activities of daily living, who presented with progressively worsening right hip pain, instability, and an antalgic limp over the past 18 months. He underwent a primary cementless total hip arthroplasty on the right side 15 years prior for debilitating primary osteoarthritis. The index procedure utilized a standard titanium porous-coated hemispherical cup with a highly cross-linked polyethylene liner and a proximally porous-coated tapered titanium femoral stem. His initial post-operative course was uneventful, and he enjoyed excellent, pain-free function for over a decade, maintaining a high level of low-impact activity.
His current pain is described as a dull, aching sensation localized primarily to the deep anterior groin and lateral peritrochanteric region. This pain is significantly exacerbated by weight-bearing, prolonged standing, and dynamic activities. Notably, he reports a mechanical sensation of "giving way" or frank instability, particularly when transitioning from a seated to a standing position, or when traversing uneven terrain. He denies any antecedent acute trauma, falls, fevers, chills, night sweats, or other systemic symptoms that would immediately raise suspicion for an acute infectious etiology.
The insidious onset of these symptoms over an 18-month period is highly characteristic of progressive particulate disease leading to macrophage-induced osteolysis and subsequent aseptic loosening of the implant. The generation of submicron polyethylene wear debris initiates a foreign body response, activating macrophages which release pro-inflammatory cytokines such as Tumor Necrosis Factor-alpha, Interleukin-1, and Interleukin-6. This cascade ultimately stimulates osteoclastogenesis via the RANK/RANKL pathway, leading to progressive periprosthetic bone resorption.
Past Medical and Surgical History
The patient's past medical history is significant for well-controlled essential hypertension, hyperlipidemia, and early-stage chronic kidney disease. He is a non-smoker and has no history of diabetes mellitus, inflammatory arthropathies, or immunosuppression. His surgical history is limited to the aforementioned right total hip arthroplasty and a remote appendectomy in his youth.
Preoperative Optimization and Functional Status
Prior to the onset of his current symptoms, the patient was a community ambulator without assistive devices. Currently, he is reliant on a single-point cane for longer distances to offload the affected extremity and mitigate the abductor lurch. Given his age and mild renal impairment, preoperative optimization required careful coordination with the internal medicine and anesthesiology services. His medications, including an ACE inhibitor and a statin, were managed per standard perioperative protocols. A comprehensive preoperative anesthesia assessment deemed him an appropriate candidate for revision arthroplasty under regional anesthesia (spinal) to minimize pulmonary complications, reduce intraoperative blood loss, and mitigate the risk of postoperative delirium common in the octogenarian population.
Clinical Examination Findings
Inspection and Gait Analysis
On initial physical examination, the patient was observed ambulating with a pronounced antalgic gait and a positive Trendelenburg sign on the right side. The uncompensated Trendelenburg gait indicates significant mechanical disadvantage or frank failure of the right hip abductor mechanism (gluteus medius and minimus). In the setting of acetabular component migration, the center of rotation of the hip is frequently displaced superiorly and medially. This medialization shortens the abductor moment arm, rendering the abductor musculature biomechanically inefficient and unable to maintain a level pelvis during the single-leg stance phase of gait.
A measurable leg length discrepancy of approximately 2 cm was noted, with the right lower extremity appearing shorter. This shortening is consistent with the superior migration of the acetabular component into the ilium. Skin integrity around the previous posterolateral surgical incision was entirely intact, well-healed, and without any clinical signs of erythema, induration, localized warmth, or sinus tract formation. There was no palpable mass or significant soft tissue fluctuance to suggest an adverse local tissue reaction or large fluid collection.
Palpation and Range of Motion Assessment
Palpation elicited moderate tenderness over the greater trochanter, likely secondary to abductor fatigue and secondary trochanteric bursitis, as well as deep tenderness in the anterior groin region, a classic sign of acetabular pathology. Active and passive range of motion of the right hip was severely restricted and elicited significant pain, particularly at the extremes of motion.
Goniometric measurements revealed flexion limited to 70 degrees, abduction to 10 degrees, adduction to 0 degrees, internal rotation to 5 degrees, and external rotation to 10 degrees. The patient demonstrated profound guarding and significant pain with axial loading of the limb (the anvil test) and with the Stinchfield test (resisted active straight leg raise), further confirming mechanical loosening and micromotion of the components under load.
Neurological and Vascular Evaluation
A meticulous neurological assessment revealed intact sensation to light touch and pinprick in the L2 through S1 dermatomal distributions bilaterally. Motor strength was 5/5 in the bilateral lower extremities for hip flexion (iliopsoas), extension (gluteus maximus), knee flexion (hamstrings), knee extension (quadriceps), ankle dorsiflexion (tibialis anterior), and ankle plantarflexion (gastrocnemius-soleus complex). The abductor strength on the right was difficult to isolate purely due to pain inhibition but was clinically weak (graded 3/5) compared to the contralateral side.
Distal pulses, including the femoral, popliteal, dorsalis pedis, and posterior tibial arteries, were palpable, bounding, and symmetrical bilaterally. Capillary refill was brisk (less than 2 seconds) in all digits. No clinical signs of deep vein thrombosis, such as calf swelling, erythema, or a positive Homan's sign, were noted.
Imaging and Diagnostics
Plain Radiographic Evaluation
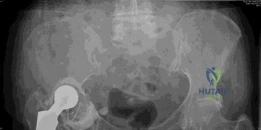
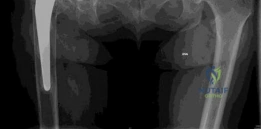
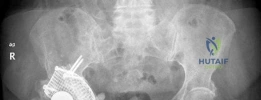
Initial plain radiographs, including an anteroposterior pelvis and cross-table lateral of the right hip, were obtained and meticulously reviewed. The AP pelvis demonstrated severe superior and medial migration of the cementless acetabular component. The hemispherical cup was definitively loose, exhibiting progressive, contiguous periprosthetic radiolucent lines exceeding 2 mm across all three DeLee and Charnley zones. This pattern is the radiographic hallmark of aseptic loosening driven by particulate osteolysis.

There was evidence of extensive acetabular bone loss, particularly localized to the superior dome (ilium) and the medial wall. The medial migration of the component resulted in violation of the Kohler line (ilioischial line), confirming the presence of protrusio acetabuli. The teardrop, a critical radiographic landmark representing the inferior aspect of the acetabular fossa, appeared attenuated but not completely obliterated.
Conversely, the femoral component appeared well-fixed and stable radiographically. There was no evidence of subsidence, pedestal formation at the distal tip, or significant periprosthetic radiolucencies in the Gruen zones. The proximal porous coating appeared to have robust osteointegration, and the diaphyseal fit remained isthmic.
Advanced Imaging Modalities
Given the complexity of the acetabular defect and the planned revision, advanced imaging was mandated to precisely quantify the volumetric bone loss and evaluate the integrity of the anterior and posterior columns. A multi-detector Computed Tomography scan of the pelvis with metal artifact reduction sequence protocols was obtained.
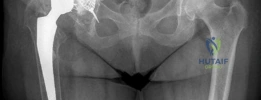
The coronal CT reconstructions provided a definitive assessment of the medial wall defect and the extent of superior migration. The imaging confirmed a severe cavitary defect extending into the ilium, with a focal segmental defect of the superior rim. The medial wall was critically thin, with focal areas of complete absence, allowing the medial aspect of the cup to protrude into the true pelvis. Importantly, the CT scan confirmed that despite the severe osteolysis, the anterior and posterior columns remained in continuity, ruling out a complete pelvic discontinuity.
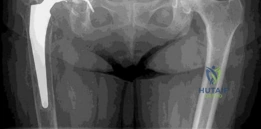
Three-dimensional surface-rendered CT reconstructions were utilized for preoperative templating and spatial orientation of the defect. These 3D models are invaluable for visualizing the exact geometry of the remaining host bone and for determining the appropriate size and shape of structural allografts or highly porous metal augments required to restore the anatomic center of rotation.
Laboratory Diagnostics and Infection Rule Out
A rigorous protocol to rule out periprosthetic joint infection is mandatory in all revision arthroplasty scenarios, regardless of the clinical presentation. Initial serological markers, including the erythrocyte sedimentation rate and C-reactive protein, were drawn. Both inflammatory markers returned well within normal physiological limits (ESR 12 mm/hr, CRP 0.4 mg/dL).
Despite the negative serology, a fluoroscopically guided aspiration of the right hip joint was attempted to obtain synovial fluid for cell count, differential, and cultures. The aspiration yielded a "dry tap," returning no fluid despite multiple passes and saline lavage attempts. Given the completely benign clinical presentation, the absence of systemic inflammatory signs, the normal serological markers, and the classic radiographic appearance of wear-induced osteolysis, the diagnosis of periprosthetic joint infection was deemed highly unlikely. The definitive preoperative diagnosis was established as aseptic mechanical loosening of the acetabular component secondary to massive periacetabular osteolysis.
Differential Diagnosis
The presentation of a painful total hip arthroplasty years after the index procedure requires a systematic and exhaustive differential diagnosis. While aseptic loosening is the most common cause of late failure, other catastrophic etiologies must be systematically excluded to prevent inappropriate surgical intervention.
| Diagnostic Entity | Clinical Presentation Hallmarks | Radiographic Findings | Laboratory and Aspiration Findings |
|---|---|---|---|
| Aseptic Loosening (Particulate Disease) | Insidious onset of pain, start-up pain, progressive limp, mechanical instability. No systemic signs. | Eccentric wear of polyethylene liner, progressive radiolucent lines (>2mm) in multiple zones, endosteal scalloping, component migration. | Normal ESR/CRP. Synovial fluid WBC < 3,000 cells/µL, PMN < 80%. Cultures negative. |
| Periprosthetic Joint Infection | Constant pain (rest and night pain), acute or subacute onset, possible fevers/chills, localized warmth, erythema, or draining sinus. | Periosteal reaction, rapid focal osteolysis, early component loosening without significant wear, soft tissue swelling. | Elevated ESR/CRP. Synovial WBC > 3,000 cells/µL, PMN > 80%. Positive Alpha-defensin. Positive cultures. |
| Periprosthetic Fracture | Acute onset of severe pain following a specific traumatic event or minor fall. Inability to bear weight immediately. | Visible cortical disruption, acute subsidence or angulation of the component, displaced bone fragments. | Normal inflammatory markers unless concomitant infection exists. Aspiration typically reveals hemarthrosis. |
| Adverse Local Tissue Reaction | Groin pain, palpable soft tissue mass, spontaneous dislocation, abductor weakness out of proportion to pain. Often seen in Metal-on-Metal or modular necks. | Large cystic or solid soft tissue masses on MARS MRI. Often minimal bony osteolysis initially. | Elevated serum Cobalt and Chromium levels. Normal ESR/CRP. Aspiration shows aseptic lymphocyte-dominated vasculitis-associated lesion. |
Surgical Decision Making and Classification
Acetabular Defect Classification
Accurate classification of the acetabular bone loss is the cornerstone of preoperative planning and dictates the reconstructive strategy. The Paprosky classification system is the most widely utilized and validated framework for evaluating acetabular defects in revision total hip arthroplasty. It relies on specific radiographic landmarks: the superior dome, the medial wall (Kohler's line), the teardrop, and the ischium.
Based on the preoperative plain radiographs and advanced CT imaging, this patient's defect was classified as a severe Paprosky Type IIIA defect.
* Superior Migration: The component had migrated superiorly greater than 3 cm, indicating severe loss of the superior dome and structural support.
* Medial Migration: The component had breached Kohler's line, indicating a deficient medial wall and protrusio.
* Ischial Osteolysis: Moderate osteolysis was present extending into the ischium.
* Teardrop Integrity: The teardrop was attenuated but remained partially intact, differentiating this from a Type IIIB defect (where the teardrop is completely obliterated, and severe ischial lysis is present).
* Pelvic Discontinuity: The CT scan confirmed intact anterior and posterior columns, ruling out a Paprosky Type IV defect.
Implant Selection and Grafting Strategy
The primary goals of revision acetabular reconstruction are to achieve rigid initial stability of the new component, restore the anatomic center of rotation, restore host bone stock, and provide a construct that allows for long-term biological fixation.
For a Paprosky Type IIIA defect with significant superior and medial cavitary loss, combined with a superior segmental rim defect, a standard hemispherical cup alone is insufficient. Achieving an isthmic fit on host bone is impossible without excessively superiorizing the center of rotation, which would result in persistent abductor weakness and limb length discrepancy.
The selected surgical strategy prioritized "Acetabular Grafting" to restore bone stock, utilizing a combination of particulate morselized allograft for the contained cavitary medial defects and a highly porous titanium structural augment to address the uncontained superior segmental rim defect.
- Morselized Allografting (Impaction Bone Grafting): The medial protrusio defect acts as a contained cavitary void. Utilizing the principles popularized by the Slooff-Ling technique, this void will be tightly packed with morselized cancellous allograft. This technique restores medial bone stock, lateralizes the new component to the anatomic center of rotation, and provides a biological scaffold for host bone creeping substitution.
- Highly Porous Metal Augment: The superior segmental defect requires structural support. Historically, bulk structural allografts (e.g., femoral head allografts) were utilized. However, these are associated with high rates of late resorption and collapse. Modern highly porous metals (tantalum or highly porous titanium) offer a trabecular structure that mimics cancellous bone, providing an excellent coefficient of friction for initial mechanical stability and a highly osteoconductive environment for rapid biological ingrowth.
- Highly Porous Hemispherical Shell: A multi-hole, highly porous titanium revision shell will be utilized. This allows for the placement of multiple trans-acetabular screws to achieve rigid initial fixation against the host bone and the structural augment.
Rationale for Femoral Component Retention
The preoperative radiographic assessment indicated a well-fixed, biologically integrated cementless femoral stem. Extracting a well-fixed porous-coated stem is a highly morbid procedure, often requiring an extended trochanteric osteotomy or a transfemoral approach, which significantly increases surgical time, blood loss, and the risk of periprosthetic fracture, particularly in an 82-year-old patient.
Therefore, the decision was made to retain the femoral stem. The modularity of the trunnion allows for the exchange of the femoral head. By utilizing various neck lengths and offset options, we can fine-tune the leg length and soft tissue tension after the acetabular center of rotation has been restored. Careful intraoperative inspection of the trunnion for signs of fretting or corrosion (trunnionosis) is mandatory before placing a new modular head.
Surgical Technique and Intervention
Patient Positioning and Surgical Approach
The patient was brought to the operating theater and placed in the lateral decubitus position on a standard radiolucent operating table. Rigid pelvic positioners were utilized at the anterior superior iliac spine and the sacrum to ensure the pelvis remained perfectly orthogonal to the floor, a critical step for accurate assessment of component version and inclination during the reconstruction. Bony prominences were meticulously padded, and an axillary roll was placed to protect the brachial plexus.
A standard posterolateral approach to the hip was utilized, incorporating the previous surgical incision. The incision was extended proximally and distally to ensure adequate exposure for a complex revision. The tensor fasciae latae and gluteus maximus fascia were incised in line with the skin incision. The gluteus maximus fibers were bluntly split.
Deep exposure revealed significant scar tissue and pseudocapsule formation. The sciatic nerve was carefully identified, neurolysed from surrounding scar tissue, and protected throughout the procedure without placing it under undue tension. The short external rotators and the posterior capsule, which were heavily scarred, were sharply excised to expose the posterior aspect of the greater trochanter and the proximal femur.
Component Explantation and Defect Preparation
The hip was carefully dislocated posteriorly. The modular highly cross-linked polyethylene liner was found to be severely worn eccentrically, with evidence of complete wear-through at the superior dome, leading to metal-on-metal articulation between the femoral head and the titanium shell. The femoral head was removed from the trunnion. The trunnion was carefully inspected and found to be pristine, without evidence of significant corrosion or deformation.
Attention was then turned to the acetabulum. The loose titanium shell was surrounded by a massive volume of reactive, granulomatous tissue characteristic of particulate disease.
The shell was easily extracted with minimal force using an explantation instrument, confirming the preoperative diagnosis of complete aseptic loosening. Following extraction, an aggressive and meticulous debridement of all granulomatous tissue, fibrous membranes, and necrotic bone was performed using curettes and a high-speed burr. This step is critical; all soft tissue must be removed to expose bleeding, viable host bone to facilitate biological ingrowth into the new implants and graft material.
Acetabular Reconstruction and Bone Grafting
Following debridement, the true extent of the Paprosky IIIA defect was visualized. The medial wall was profoundly deficient, and a large superior segmental defect was present.
The medial cavitary defect was addressed first. Fresh frozen morselized cancellous allograft was prepared on the back table.

The graft was washed with pulsatile lavage to remove marrow elements and lipids, reducing the immunogenic payload and enhancing osteoconductivity. The morselized graft was then introduced into the medial defect. Reverse reaming (running the reamer in reverse) was utilized to impact the graft material tightly into the cavitary void, consolidating it and essentially "neo-medializing" the medial wall to prevent further protrusio of the trial components.
Once the medial wall was reconstituted with impacted graft, the superior segmental defect was addressed. A trial highly porous titanium augment was selected and positioned to fill the superior void and restore the structural integrity of the acetabular rim. The augment was provisionally fixed with K-wires.
A trial hemispherical shell was then introduced. The goal was to achieve a "press-fit" against the inferior host bone (ischium and pubis) and the superiorly placed metal augment, ensuring the center of rotation was restored to its anatomic position (inferior and lateral compared to the preoperative state).
Final Component Implantation and Stability Assessment
Once the optimal size and position of the augment and shell were determined via trialing, the definitive implants were opened. The highly porous titanium augment was secured to the superior host ilium using two 6.5 mm partially threaded cancellous screws directed into the dense bone of the sciatic buttress.
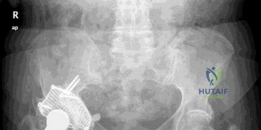
A layer of bone cement (polymethylmethacrylate) was applied to the interface between the augment and the definitive multi-hole highly porous titanium revision shell to create a monolithic construct. The definitive shell was then impacted into place, achieving excellent initial scratch fit against the host bone and the augment.
To ensure rigid mechanical stability, multiple 6.5 mm trans-acetabular screws were placed through the shell. Screw trajectory was strictly confined to the posterior-superior and posterior-inferior quadrants (the safe zones of Wasielewski) to avoid catastrophic injury to the external iliac vessels and the obturator neurovascular bundle. Excellent cortical purchase was achieved in the ilium and ischium.
Following secure fixation of the acetabular construct, a highly cross-linked polyethylene liner was impacted into the shell. Attention was returned to the retained femoral stem. Trialing with various modular heads was performed. A +4 mm offset ceramic head was selected to optimize soft tissue tension, restore leg length, and maximize the abductor moment arm.
The hip was reduced, and stability was rigorously tested. The hip was stable in 90 degrees of flexion with 45 degrees of internal rotation, and stable in full extension with external rotation. Leg lengths were assessed clinically via the Shuck test and by comparing the relationship of the greater trochanter to the center of the femoral head, confirming restoration of symmetric limb length. The wound was irrigated copiously, and a meticulous layered closure was performed over a deep subfascial drain.
Post Operative Protocol and Rehabilitation
Inpatient Management and Immediate Postoperative Care
The patient's immediate postoperative course was managed in the surgical step-down unit due to his advanced age and the complexity of the procedure. Intravenous antibiotics (Cefazolin) were administered for 24 hours prophylactically. Deep vein thrombosis prophylaxis was initiated with low molecular weight heparin (Enoxaparin) given his high-risk profile, transitioning to oral Apixaban upon discharge for a total of 35 days.
Pain management utilized a multimodal approach, including scheduled acetaminophen, NSAIDs (with careful monitoring of renal function), Gabapentin, and judicious use of oral opioids for breakthrough pain. The subfascial drain was removed on postoperative day one when output fell below 30 cc per shift.
Weight Bearing Restrictions and Physical Therapy
Rehabilitation following complex acetabular reconstruction with structural augments and impaction bone grafting requires a delicate balance between preventing stiffness and protecting the initial mechanical fixation to allow for biological ingrowth.
The patient was restricted to toe-touch weight-bearing (approximately 20 lbs of pressure) on the operative extremity for the first 6 weeks postoperatively. This protected weight-bearing phase is critical to prevent early micromotion at the implant-bone interface, which could lead to fibrous encapsulation rather than osseointegration of the highly porous metals, and to prevent subsidence of the impacted allograft.
Physical therapy focused on early mobilization out of bed, isometric quadriceps and gluteal sets, and gentle active-assisted range of motion within the constraints of standard posterior hip precautions (no flexion past 90 degrees, no adduction past midline, no internal rotation).
Long
Clinical & Radiographic Imaging