Pediatric Salter-Harris Type IV Distal Femoral Physeal Fracture: A Case Study
Key Takeaway
A Salter-Harris type IV distal femoral physeal fracture involves both the epiphysis and metaphysis, extending through the growth plate. Diagnosis typically begins with clinical presentation and plain radiographs, followed by CT imaging for precise evaluation of articular displacement and surgical planning. Neurovascular assessment is critical due to the high-energy mechanism often associated with these pediatric injuries.
Patient Presentation and History
Trauma Bay Arrival and Primary Survey
A 12-year-old male presented to the Level I trauma center emergency department following a high-energy mechanism of injury. The patient was an unrestrained passenger in a motor vehicle collision, occupying the rear passenger-side seat during a direct lateral impact (T-bone collision) to the right side of the vehicle. Emergency Medical Services reported significant vehicular intrusion and a prolonged extrication time of approximately 30 minutes. Upon arrival at the trauma bay, the patient was evaluated according to Advanced Trauma Life Support protocols. His airway was patent, breathing was unlabored with symmetrical breath sounds, and hemodynamics were stable, demonstrating a normotensive state with age-appropriate resting tachycardia. The Glasgow Coma Scale was 15. There was no reported loss of consciousness, and the primary survey revealed no immediate life-threatening injuries to the cranium, thorax, abdomen, or pelvis.
Secondary Survey and Injury Specifics
During the secondary survey, the patient reported immediate, severe, and unrelenting pain localized to his right distal thigh and knee, accompanied by an absolute inability to bear weight or actively mobilize the extremity. The kinetic energy transfer inherent in a lateral impact mechanism frequently induces significant varus or valgus stress on the lower extremities. In the pediatric population, the ligamentous structures (specifically the medial and lateral collateral ligaments) possess greater tensile strength than the cartilaginous physeal plates, making physeal failure the pathognomonic response to such biomechanical stress.
Demographics and Comorbidities
A comprehensive review of systems and past medical history was obtained from the patient and his legal guardians. The patient’s medical history was entirely unremarkable. There were no known bleeding diatheses, metabolic bone disorders (such as osteogenesis imperfecta or hypophosphatemic rickets), or prior traumatic injuries to the appendicular skeleton. He was not taking any prescription medications and had no known drug allergies.
Skeletal Maturity Assessment
Of critical importance in pediatric orthopedic trauma, the patient was assessed for skeletal maturity. He was clinically prepubescent, corresponding to Tanner Stage II. Based on subsequent skeletal age assessment utilizing the Greulich and Pyle atlas, his bone age was congruent with his chronological age. The distal femoral physis is the most active growth plate in the human body, contributing approximately 70% of the longitudinal growth of the femur and roughly 40% of the overall length of the lower extremity, growing at an average rate of 9 to 10 millimeters per year. Given his skeletal age, he possessed an estimated remaining growth potential of approximately 4 to 5 years, equating to roughly 3.5 to 5.0 centimeters of longitudinal growth remaining from the distal femoral physis alone. This substantial remaining growth potential significantly elevates the clinical stakes regarding anatomical reduction, as any physeal insult or subsequent bar formation could result in profound leg length discrepancy or severe angular deformity.
Clinical Examination Findings
Inspection of the Soft Tissue Envelope
Upon initial localized assessment, the patient was alert, oriented, and in significant distress secondary to the orthopedic injury. Inspection of the right lower extremity revealed marked swelling, extensive ecchymosis, and an obvious structural deformity of the distal femur, specifically a valgus angulatory deformity. The soft tissue envelope was meticulously evaluated. The skin overlying the fracture site was intact, with no evidence of open traumatic wounds, full-thickness abrasions, or degloving injuries. There was no severe tenting of the skin that would indicate impending soft tissue necrosis, though the skin was taut due to the underlying hemarthrosis and fracture hematoma. The knee appeared to be held in a fixed, guarded position of slight flexion, approximately 15 degrees. There was no obvious rotational malalignment of the tibia relative to the femur.
Palpation and Structural Integrity
Palpation was conducted with extreme care to avoid exacerbating patient discomfort while obtaining necessary clinical data. There was exquisite, poorly tolerated tenderness circumferentially around the distal femur. This tenderness was most pronounced over the medial and lateral femoral condyles, as well as the suprapatellar pouch. A distinct, palpable gap and bony step-off were appreciated proximally to the medial aspect of the physis, highly suggestive of a displaced metaphyseal fragment. The knee joint itself was tense, indicative of a massive acute hemarthrosis. Gentle attempts at eliciting crepitus were deferred to prevent further iatrogenic damage to the delicate perichondrial ring of LaCroix and the groove of Ranvier, both of which are critical for appositional physeal growth.
Range of Motion and Joint Stability
Active and passive range of motion of the right knee was severely limited by pain and mechanical block. Flexion was estimated at a maximum of 10 to 20 degrees, and the joint was fixed at 5 degrees of flexion due to involuntary hamstring guarding and capsular distension from the hemarthrosis. Any attempt to mobilize the joint beyond this narrow arc elicited severe apprehension and muscle spasm. Ankle and foot range of motion were preserved, symmetric to the contralateral limb, and entirely pain-free, ruling out concomitant distal kinetic chain injuries. Ligamentous stability testing (varus/valgus stress, Lachman, anterior/posterior drawer) was not formally performed in the acute setting due to the obvious fracture instability and the risk of displacing the physeal fragments further.
Neurological and Vascular Assessment
A rigorous neurovascular examination is paramount in distal femoral fractures due to the intimate anatomical relationship between the distal femur and the neurovascular bundle within the popliteal fossa. Distal neurological examination revealed intact sensation to light touch and pinprick in the distributions of the saphenous, superficial peroneal, deep peroneal, sural, and tibial nerves. Motor function of the extensor hallucis longus, tibialis anterior, gastrocnemius-soleus complex, and flexor hallucis longus was intact and graded at 5/5 strength.
Vascular assessment revealed palpable, strong, and symmetrical dorsalis pedis and posterior tibial pulses compared to the uninjured contralateral limb. Capillary refill in the distal digits was brisk, occurring in under two seconds. However, the popliteal artery is tethered proximally at the adductor hiatus (Hunter's canal) and distally at the fibrous arch of the soleus muscle. Posterior displacement of the distal femoral metaphysis can easily stretch, compress, or lacerate the popliteal artery. Despite the reassuring initial vascular exam, the high-energy mechanism and significant soft tissue swelling mandated a high index of suspicion for intimal tear or delayed vascular compromise. Continuous pulse oximetry on the ipsilateral hallux and serial neurovascular checks were immediately initiated. An Ankle-Brachial Index was calculated at 1.05, ruling out the immediate need for a CT angiogram, though the threshold for advanced vascular imaging remained low.
Imaging and Diagnostics
Plain Radiographic Evaluation
Initial diagnostic imaging consisted of standard orthogonal plain radiographs of the right femur and knee. The anteroposterior and lateral views of the right distal femur clearly demonstrated a Salter-Harris type IV physeal fracture involving the medial femoral condyle. The fracture line initiated at the articular surface of the medial femoral condyle, propagated obliquely through the epiphysis and the physis, and subsequently exited proximally through the medial metaphysis, creating the classic Thurstan Holland fragment.
There was significant displacement of the articular fragment. Radiographic measurements indicated approximately 6 millimeters of vertical displacement and a 4-millimeter articular step-off at the intercondylar notch. On the lateral projection, the epiphysis was displaced posteriorly and medially relative to the metaphysis, a common displacement pattern driven by the pull of the medial gastrocnemius head. There was also a notable valgus angulation of the distal articular block relative to the anatomical axis of the femoral shaft. No other acute bony abnormalities, such as patellar fractures or tibial plateau involvement, were identified. The tibiofemoral joint space appeared maintained, and there were no radiopaque loose bodies visible within the joint capsule.

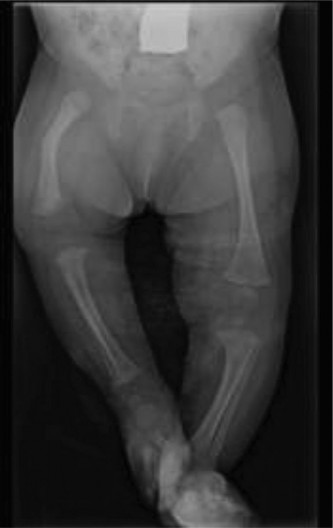
Above: Representative lateral radiograph demonstrating a distal femoral physeal fracture, showing posterior displacement and typical angulation.
Advanced Imaging Indications and Findings
Given the Salter-Harris type IV nature of the injury, which involves the articular surface and physis, a Computed Tomography (CT) scan with 1mm cuts was obtained to further characterize the articular involvement and facilitate preoperative templating. Plain radiographs notoriously underestimate the degree of comminution and articular incongruity in complex physeal injuries.
The CT scan with multiplanar reconstructions (sagittal, coronal, and 3D volume rendering) provided critical anatomical intelligence. The coronal reconstructions confirmed a 4.5-millimeter intra-articular step-off involving the weight-bearing dome of the medial femoral condyle. Furthermore, the axial cuts revealed a degree of rotational malalignment of the epiphyseal fragment that was not fully appreciated on the plain films. The CT scan also confirmed the absence of coronal plane comminution (Hoffa-type fracture extensions) within the epiphyseal fragment, which would have significantly altered the fixation strategy.
Magnetic Resonance Imaging Considerations
While a preoperative Magnetic Resonance Imaging (MRI) scan was not immediately obtained in the emergency setting due to the necessity for urgent surgical intervention, its utility in pediatric distal femur fractures is well-documented. MRI is highly sensitive for identifying concomitant soft tissue derangements, which occur in up to 40% of displaced pediatric distal femoral physeal fractures. These include meniscal entrapment within the fracture site, anterior cruciate ligament avulsions, and medial collateral ligament tears. In this specific case, the decision was made to assess the menisci and cruciate ligaments via direct visualization and intraoperative examination under anesthesia rather than delaying surgical reduction for an MRI.
Differential Diagnosis
When evaluating a pediatric patient with an acute, traumatic hemarthrosis and distal femoral deformity, the differential diagnosis must encompass a spectrum of osseous, physeal, and ligamentous pathologies. Distinguishing between these entities is critical, as the treatment algorithms and long-term prognoses vary significantly.
| Differential Diagnosis | Key Differentiating Clinical Features | Radiographic and Advanced Imaging Findings |
|---|---|---|
| Salter-Harris Type IV Distal Femur Fracture | Severe pain, hemarthrosis, marked instability. Mechanism usually involves axial load with varus/valgus stress. High risk of growth arrest. | Fracture line crosses epiphysis, physis, and metaphysis. Articular step-off present. Best visualized on CT for exact articular mapping. |
| Salter-Harris Type II Distal Femur Fracture | Most common distal femur physeal fracture. Extra-articular. Pain and swelling, but less severe hemarthrosis than Type III/IV unless capsular tear occurs. | Fracture line passes transversely through the physis and exits through the metaphysis (Thurstan Holland fragment). Intact epiphysis. |
| Salter-Harris Type III Distal Femur Fracture | Intra-articular fracture without metaphyseal involvement. High energy trauma. Significant hemarthrosis. | Fracture line passes from articular surface through epiphysis and exits horizontally along the physis. No metaphyseal spike. |
| Osteochondral Fracture of Femoral Condyle | Often associated with patellar dislocation (lateral condyle) or direct impact. Locking or catching mechanical symptoms if fragment is loose. | Plain films may miss small fragments. MRI is gold standard showing cartilage/subchondral bone defect and loose body. |
| Tibial Eminence Avulsion Fracture | Pediatric equivalent of an ACL tear. Positive Lachman test (if pain allows). Hemarthrosis present. | Bony avulsion at the anterior intercondylar area of the tibia. Best seen on lateral radiograph or CT scan. |
| Medial Collateral Ligament Rupture | Valgus stress mechanism. Tenderness over medial joint line and femoral/tibial attachments. Valgus laxity on exam. | Plain films generally normal (possible Pellegrini-Stieda lesion chronically). MRI confirms ligamentous disruption. |
Surgical Decision Making and Classification
Classification Frameworks
The injury was classified primarily using the Salter-Harris classification system, which remains the most universally accepted prognostic and descriptive tool for pediatric physeal fractures. A Salter-Harris Type IV fracture indicates that the fracture line traverses the epiphysis, crosses the cartilaginous physis, and exits through the metaphysis. This creates a completely unstable fragment that includes a portion of the articular surface, the germinal layer of the growth plate, and metaphyseal bone.
Additionally, the Peterson classification of physeal injuries provides further context. This injury aligns with a Peterson Type IV, which is analogous to the Salter-Harris IV but emphasizes the absolute necessity of anatomic reduction to prevent cross-physeal osseous bridging.
Rationale for Operative Intervention
The decision to proceed with urgent operative intervention was absolute and unequivocal. Non-operative management of a displaced Salter-Harris Type IV distal femoral fracture is contraindicated due to several critical biomechanical and biological factors:
- Articular Incongruity: The patient presented with a 4.5-millimeter articular step-off. The intra-articular tolerance for step-off in weight-bearing joints is generally accepted to be less than 2 millimeters. Failure to restore articular congruity leads to altered joint contact mechanics, focal cartilage overloading, and inevitable early-onset post-traumatic osteoarthritis.
- Physeal Bar Formation (Epiphysiodesis): The Salter-Harris Type IV fracture vertically violates all zones of the physis, including the reserve zone and the proliferative zone. If the metaphyseal bone is allowed to heal in direct contact with the epiphyseal bone across the physeal defect, an osseous bridge (physeal bar) will form. Given the patient's significant remaining growth potential (4-5 years), a physeal bar would cause asymmetrical growth arrest, leading to severe progressive valgus deformity and leg length discrepancy. Anatomic reduction minimizes the gap between the disrupted physeal zones, allowing cartilaginous repair rather than osseous bridging.
- Mechanical Instability: The distal femur is subjected to massive deforming forces from the quadriceps, hamstrings, and gastrocnemius muscles. A displaced Type IV fracture is inherently unstable and cannot be maintained in anatomical alignment with closed reduction and cast immobilization alone.
Timing of Surgery
While some pediatric fractures can be treated subacutely, displaced intra-articular physeal fractures of the distal femur warrant urgent intervention. Delaying surgery increases the risk of fracture hematoma organization, soft tissue interposition (specifically periosteum), and further damage to the delicate physeal cartilage during delayed reduction attempts. The patient was optimized and taken to the operating room within 12 hours of presentation.
Surgical Technique and Intervention
Preoperative Planning and Patient Positioning
Preoperative templating was performed utilizing the CT multiplanar reconstructions to determine optimal screw trajectory and length. The goal was to achieve independent compression of the epiphyseal and metaphyseal fracture components without placing hardware across the physis.
The patient was brought to the operating room and placed in the supine position on a fully radiolucent Jackson table to facilitate unimpeded fluoroscopic imaging in multiple planes. General endotracheal anesthesia was administered, supplemented with a regional adductor canal block for postoperative pain control. A non-sterile pneumatic tourniquet was placed high on the proximal thigh. The right lower extremity was prepped and draped in standard sterile fashion. A sterile bump was utilized to allow the knee to rest at approximately 30 degrees of flexion, relaxing the posterior neurovascular structures and the gastrocnemius muscle.
Surgical Approach
Given the medial location of the fracture and the necessity for direct articular visualization, a medial parapatellar arthrotomy was selected. A longitudinal incision was made over the anteromedial aspect of the knee, extending from the superior pole of the patella to the level of the tibial tubercle. Subcutaneous tissues were sharply dissected to expose the medial patellar retinaculum.
The retinaculum and joint capsule were incised, entering the joint space. A massive hemarthrosis, laden with fat globules indicating intra-articular fracture, was immediately evacuated using a combination of suction and copious sterile saline irrigation. This step is critical to visualize the articular surface and assess for osteochondral loose bodies.
Fracture Debridement and Soft Tissue Management
Upon exposure of the medial femoral condyle, the fracture site was identified. Consistent with the literature on pediatric physeal fractures, a significant flap of torn periosteum was found incarcerated within the vertical physeal fracture gap. This periosteal interposition is the primary impediment to closed reduction in these injuries. Using a Freer elevator and a dental pick, the incarcerated periosteum was meticulously extracted from the fracture site and reflected proximally. The fracture edges were gently debrided of organized hematoma, taking extreme care not to curette or damage the exposed cartilaginous physis.
The medial meniscus was inspected and found to be intact and free from entrapment within the fracture line. The anterior and posterior cruciate ligaments were visualized and confirmed to be intact.
Reduction Maneuvers
Reduction of a Salter-Harris IV fracture mandates a sequential approach: anatomical restoration of the articular surface (epiphysis) takes absolute precedence, followed by reduction of the metaphyseal component.
A 5.0-millimeter Schanz pin was placed into the medial epicondylar fragment to serve as a "joystick" for manipulation. Longitudinal traction was applied, and the epiphyseal fragment was derotated and translated anteriorly to match the intact lateral condyle. A large Weber point-to-point reduction clamp was placed with one tine on the non-articular medial epicondyle and the other tine carefully positioned on the intact lateral femoral condyle through a small lateral stab incision. Compression was applied.
Direct visual inspection of the articular cartilage confirmed a perfectly flush anatomical reduction of the joint surface with zero step-off. Fluoroscopy was then brought in to confirm the reduction of the metaphyseal component and the restoration of the anatomical mechanical axis.
Fixation Construct
The fixation strategy aimed for absolute stability to allow early range of motion while strictly avoiding cross-physeal hardware placement.
- Epiphyseal Fixation: Two 1.25-millimeter smooth Kirschner wires were advanced from medial to lateral through the epiphysis, parallel to the joint line and strictly distal to the physis, to provisionally hold the articular reduction. Over these guidewires, two 4.0-millimeter partially threaded cannulated titanium screws were placed. The screws were advanced carefully to ensure the threads fully bypassed the fracture site, allowing for lag compression of the epiphyseal fragment. Washers were utilized to prevent screw head subsidence into the relatively soft pediatric epiphyseal cancellous bone.
- Metaphyseal Fixation: Following epiphyseal stabilization, attention was turned to the metaphyseal Thurstan Holland fragment. A single 4.5-millimeter partially threaded cannulated screw was placed from medial to lateral, parallel to the physis and strictly proximal to it, capturing the metaphyseal spike and compressing it to the intact femoral shaft.
Final fluoroscopic images in the anteroposterior, lateral, and bilateral oblique planes confirmed perfect anatomical reduction, restoration of the joint line, and extra-physeal placement of all hardware. The tourniquet was deflated, and meticulous hemostasis was obtained. The arthrotomy was closed in layers utilizing heavy absorbable suture. The skin was closed with a running subcuticular suture, and a sterile compressive dressing was applied. The limb was placed in a hinged knee brace locked in full extension.
Post Operative Protocol and Rehabilitation
Immediate Postoperative Phase (Weeks 0-4)
The primary goal in the immediate postoperative phase is protection of the biological fixation and soft tissue healing. The patient was admitted for 24 hours of intravenous antibiotics and neurovascular monitoring. He was discharged on postoperative day one.
The rehabilitation protocol mandated strict non-weight-bearing (NWB) status on the operative extremity for a minimum of six weeks. The hinged knee brace was locked in full extension for ambulation with crutches to prevent buckling and protect the metaphyseal fixation from shear forces. However, to prevent intra-articular adhesions and arthrofibrosis, passive range of motion (PROM) was initiated on postoperative day three. A Continuous Passive Motion (CPM) machine was utilized for 4 to 6 hours daily, with an initial arc of motion set from 0 to 30 degrees, progressively increasing by 10 degrees every few days as tolerated by pain and swelling.
Intermediate Phase (Weeks 4-8)
At the four-week postoperative clinic visit, clinical examination and interval radiographs were evaluated. Radiographs demonstrated maintenance of hardware position and early signs of metaphyseal callus formation. The patient remained NWB but was transitioned to active-assisted range of motion (AAROM) and active range of motion (AROM). The brace was unlocked to allow 0 to 90 degrees of flexion during the day. Patellar mobilization exercises were emphasized to prevent patella infera and extensor mechanism tethering.
Advanced Phase (Weeks 8-12 and Beyond)
At eight weeks, definitive radiographic bridging of the metaphyseal fracture was observed. The patient was cleared to begin a progressive partial weight-bearing protocol, advancing 25% of body weight weekly until full weight-bearing was achieved. Physical therapy focused on closed kinetic chain exercises, quadriceps strengthening, and proprioceptive retraining.
Hardware Removal and Long-Term Surveillance
A critical component of the postoperative protocol in pediatric physeal fractures is the timing of hardware removal. Retained hardware, even if placed extra-physeally, can cause localized tethering of the periosteum or act as a mechanical block to normal appositional growth. Therefore, elective hardware removal was planned and executed at 5 months post-injury, once complete osseous consolidation was confirmed.
Long-term surveillance is mandatory. The patient was enrolled in a strict follow-up protocol requiring clinical evaluation and bilateral full-length standing lower extremity radiographs (scanograms) at 6 months, 12 months, and annually thereafter until complete skeletal maturity. This surveillance is designed to detect early signs of physeal bar formation, leg length discrepancy, or angular deformity (valgus/varus drift), which would necessitate timely intervention such as epiphysiodesis of the contralateral limb or corrective osteotomy.
Clinical Pearls and Pitfalls
Surgical and Diagnostic Pearls
- Assume Periosteal Incarceration: In displaced pediatric distal femoral physeal fractures, always assume the periosteum is incarcerated within the fracture gap. Closed reduction attempts are frequently futile and can damage the physis. Early open reduction with direct extraction of the periosteum is the safest and most effective approach.
- Articular Reduction is Paramount: The fundamental rule of Salter-Harris III and IV fractures is that the articular surface must be anatomically reduced under direct visualization. Even a 1-2 millimeter step-off will inevitably lead to early osteoarthritis.
- Independent Fixation Strategy: Utilize an independent fixation strategy. Compress the epiphyseal fragment to the intact epiphysis, and compress the metaphyseal fragment to the intact metaphysis. This restores stability without violating the cartilaginous physis with threaded implants.
- Vascular Vigilance: Maintain a high index of suspicion for popliteal artery injury, particularly with posterior displacement of the metaphysis. A normal initial pulse does not rule out an intimal tear that may thrombose hours later. Serial examinations are non-negotiable
You Might Also Like


