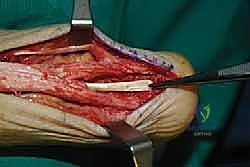
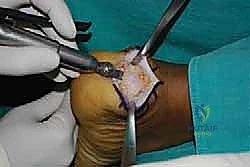
Mastering Insertional Achilles Tendinopathy: A Debridement, Exostectomy, and Reattachment Surgical Masterclass
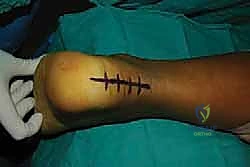
Key Takeaway
This masterclass guides orthopaedic fellows through the surgical management of insertional Achilles tendinopathy. We cover preoperative planning, detailed surgical anatomy, patient positioning, and a step-by-step intraoperative execution of debridement, calcaneal exostectomy, and Achilles reattachment. Critical pearls, potential pitfalls, and comprehensive postoperative rehabilitation protocols are emphasized for optimal patient outcomes.
Comprehensive Introduction and Patho-Epidemiology
Welcome, colleagues and fellows, to the operating theater and this comprehensive masterclass. Today, we are addressing a common yet uniquely challenging and often debilitating condition: insertional Achilles tendinopathy (IAT). This pathology extends far beyond simple posterior heel pain; it represents a complex, multi-factorial interplay of degenerative tendon changes, dynamic bony impingement, and chronic bursal inflammation. Our ultimate surgical objective is to meticulously debride the diseased, non-viable tendon, resect the offending calcaneal prominence (Haglund’s deformity), and securely reattach the healthy Achilles fibers to a biologically prepared bony bed. This is a procedure that demands absolute precision, profound patience, and an intimate, three-dimensional understanding of the local anatomy and biomechanics.
Insertional Achilles tendinopathy must be distinctly differentiated from midsubstance Achilles tendinopathy, as the pathophysiology, patient demographics, and surgical management algorithms are fundamentally different. IAT typically manifests precisely at the tendon's enthesis on the posterior calcaneus. At a histological level, the condition is characterized by angiofibroblastic hyperplasia, mucoid degeneration, and a profound disorganization of the highly structured type I collagen fibers. Rather than an acute inflammatory cascade, we observe a failed healing response. The tendon becomes thickened, fibrotic, and mechanically compromised, often developing intra-substance calcific deposits that further disrupt the normal force transmission from the triceps surae to the foot.
Epidemiologically, insertional Achilles tendinopathy affects a broad spectrum of patients, ranging from elite, high-demand athletes to sedentary, middle-aged individuals. Patients typically present with chronic, activity-related aching or sharp, stabbing pain, which is often severely exacerbated by activities that place the Achilles under stretch, such as walking uphill or ascending stairs. A progressively enlarging, indurated prominence on the posterior heel is a hallmark physical finding, exquisitely tender to direct palpation. Systemic risk factors, including obesity, diabetes mellitus, inflammatory arthropathies, and prior fluoroquinolone use, can significantly accelerate the degenerative process and complicate both nonoperative and operative management. During the clinical evaluation, a negative Thompson's test is standard, confirming the continuity of the tendon and ruling out a complete acute rupture, though the tendon’s structural integrity is undeniably compromised.
Detailed Surgical Anatomy and Biomechanics
Achilles Tendon Complex and Insertion
The Achilles tendon is the largest, thickest, and strongest tendon in the human body, serving as the confluent tendinous extension of the gastrocnemius and soleus muscle bellies. The gastrocnemius, a bi-articular muscle, originates from the medial and lateral femoral condyles, while the mono-articular soleus originates from the posterior aspect of the tibia and fibula. As these muscles converge, their respective fascial contributions intertwine and rotate approximately 90 degrees externally as they descend toward the heel. This rotation results in the gastrocnemius fibers inserting primarily on the lateral and posterior aspects of the calcaneal footprint, while the soleus fibers insert more medially and anteriorly. Understanding this rotational anatomy is critical when performing a central tendon split, as it dictates the fiber orientation you will encounter.
The insertion footprint of the Achilles tendon on the posterior calcaneal tuberosity is expansive, typically measuring approximately 2 cm in width and 2.5 cm in length. Crucially, this insertion is not merely a posterior attachment; it extends distally and wraps around the medial and lateral borders of the calcaneal tuberosity. The most proximal aspect of the posterior calcaneus is devoid of tendon insertion, covered instead by the retrocalcaneal bursa. When performing our exostectomy, we must meticulously respect the true footprint of the tendon, detaching only what is necessary for exposure and debridement, while preserving the medial and lateral expansions to maintain residual stability and augment our final repair.
Calcaneal Osteology and Impingement Mechanics
The osteology of the posterior calcaneus is central to the pathogenesis of IAT. The posterosuperior aspect of the calcaneus frequently presents with a prominent bony ridge, clinically referred to as a Haglund's deformity or "pump bump" when pathologically enlarged. The Achilles tendon inserts distal to this prominence. During ankle dorsiflexion, the anterior aspect of the Achilles tendon is forced against this posterosuperior bony prominence. This repetitive mechanical impingement, analogous to a rope fraying over a sharp rock, induces microtrauma, bursal inflammation, and subsequent tendinosis.
Radiographic parameters, such as the Chauveaux-Liet angle and the Fowler-Philip angle, have historically been used to quantify this prominence, though their clinical utility is often superseded by advanced imaging and intraoperative findings. The calcaneal tuberosity itself consists of a dense cortical shell surrounding a highly trabeculated cancellous core. During the exostectomy, our goal is to resect the offending posterosuperior corner to eliminate impingement while preserving sufficient cortical bone distally to accommodate our suture anchors. Over-resection risks violating the primary weight-bearing trabecular patterns of the heel, potentially leading to catastrophic calcaneal stress fractures.
Bursal Anatomy and Soft Tissue Envelopes
The posterior heel is protected and lubricated by a complex system of bursae and fascial layers. The retrocalcaneal bursa is a true, anatomically constant bursa situated in the recess between the anterior aspect of the distal Achilles tendon and the posterosuperior calcaneal prominence. It serves to reduce friction during ankle motion. In the setting of IAT and Haglund's deformity, this bursa becomes chronically inflamed, hypertrophic, and fibrotic—a condition known as retrocalcaneal bursitis. Complete excision of this bursa is a mandatory step in the surgical procedure to eliminate a primary pain generator and fully expose the bony impingement lesion.
Superficial to the Achilles tendon lies the pre-Achilles (or subcutaneous calcaneal) bursa, located between the skin and the tendon insertion. While less frequently the primary source of pathology, it can become inflamed due to external pressure from footwear. The Achilles tendon itself lacks a true synovial sheath; instead, it is enveloped by a paratenon, a highly vascularized layer of loose connective tissue that provides the majority of the tendon's extrinsic blood supply. Meticulous handling of the paratenon during the surgical approach is vital, as its preservation minimizes postoperative adhesions and optimizes the biological environment for tendon healing.
Neurovascular Topography
Navigating the posterior heel requires a profound respect for the regional neurovascular anatomy. The sural nerve is the most critical structure at risk during a posterior approach. It courses distally along the posterolateral aspect of the calf, piercing the deep fascia to become superficial roughly 10 cm proximal to the calcaneal insertion. It then runs adjacent to the lateral border of the Achilles tendon before curving anteriorly below the lateral malleolus. Injury to the sural nerve, whether through direct transection, aggressive retraction, or inclusion in a suture, can result in devastating neuromas or painful paresthesias along the lateral foot.
Accompanying the sural nerve is the lesser saphenous vein, which must be carefully identified and either protected or formally ligated if it crosses the operative field, as unaddressed venous bleeding can lead to significant postoperative hematomas and subsequent wound breakdown. On the medial side, the posterior tibial neurovascular bundle (comprising the posterior tibial artery, vein, and tibial nerve) lies deep to the deep posterior compartment fascia, behind the medial malleolus. While generally safe during a standard central posterior approach, aggressive deep medial dissection or errant retractor placement can jeopardize these structures. Furthermore, the posterior heel skin relies on a delicate angiosomal blood supply derived from calcaneal branches of both the posterior tibial and peroneal arteries. Minimizing subcutaneous undermining is imperative to prevent skin flap necrosis.
Exhaustive Indications and Contraindications
The decision to proceed with surgical intervention for insertional Achilles tendinopathy must be evidence-based, patient-specific, and strictly reserved for those who have exhausted all viable conservative modalities. Up to 50% of patients, even those with significant radiographic deformities, can achieve symptomatic resolution with a dedicated nonoperative regimen. Initial management mandates activity modification, transitioning from high-impact loading to low-impact alternatives. Biomechanical unloading via heel lifts (typically 1-2 cm) or footwear with an elevated, soft heel counter is essential to decrease tendon tension and reduce impingement against the Haglund's deformity.
A structured physical therapy program is the cornerstone of conservative care. Unlike midsubstance tendinopathy, where aggressive eccentric loading protocols (e.g., the Alfredson protocol) are highly efficacious, insertional tendinopathy requires a modified approach. We strictly advise against aggressive eccentric stretching into dorsiflexion, as this exacerbates the impingement of the tendon against the calcaneus. Instead, eccentric exercises should be performed on flat ground, restricting motion to neutral or slight plantarflexion. Extracorporeal shockwave therapy (ESWT) has demonstrated moderate efficacy in stimulating neovascularization and pain modulation and is a reasonable adjunct. Nonsteroidal anti-inflammatory drugs (NSAIDs) may provide short-term analgesic relief but do not alter the underlying degenerative pathology.
Crucially, corticosteroid injections are generally contraindicated in the management of Achilles tendinopathy. The profound catabolic effect of corticosteroids on collagen synthesis significantly elevates the risk of spontaneous tendon rupture, particularly in an already degenerate tendon. The only highly selective exception is a low-volume, ultrasound-guided injection strictly isolated to the retrocalcaneal bursa, ensuring absolutely no intra-tendinous infiltration, and only in cases where bursitis is the primary driver of pain with minimal tendinosis. Even then, this is performed with extreme caution and thorough patient counseling regarding rupture risks.
| Surgical Indications | Absolute Contraindications | Relative Contraindications |
|---|---|---|
| Failure of 3-6 months of comprehensive nonoperative management. | Active local or systemic infection. | Poorly controlled Diabetes Mellitus (HbA1c > 8.0%). |
| Severe, unrelenting pain significantly limiting activities of daily living. | Severe peripheral arterial disease (inadequate perfusion for wound healing). | Active smoking (significantly increases non-union/wound failure risk). |
| Extensive central calcific tendinosis not amenable to conservative care. | Medically unstable patient unfit for anesthesia. | Chronic, high-dose systemic corticosteroid use (poor tissue quality). |
| Concomitant high-grade partial tearing of the distal Achilles tendon. | Non-ambulatory status prior to symptom onset. | Patient non-compliance or inability to adhere to strict postoperative rehab. |
Pre-Operative Planning, Templating, and Patient Positioning
Advanced Imaging and Pre-Surgical Templating
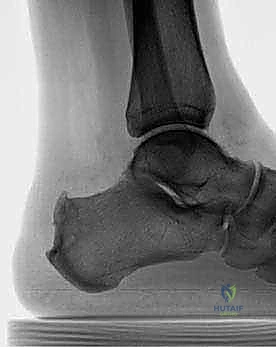
Thorough preoperative planning relies heavily on high-quality imaging. A weight-bearing lateral radiograph of the foot and ankle is the initial standard. We meticulously evaluate the morphology of the calcaneal tuberosity, identifying the Haglund's deformity and assessing the presence, size, and location of intra-tendinous calcifications (enthesophytes). These calcifications often dictate the extent of tendon detachment required for adequate debridement. We mentally template the trajectory of our planned osteotomy, aiming to resect the posterosuperior prominence while preserving the vital plantar and distal cortical bone stock necessary for anchor fixation.
While radiographs confirm the bony anatomy, Magnetic Resonance Imaging (MRI) is indispensable for evaluating the soft tissue envelope. A non-contrast MRI, particularly fluid-sensitive sagittal T2-weighted or STIR sequences, allows us to quantify the extent of intra-substance tendon degeneration, mucoid tearing, and the severity of retrocalcaneal bursitis.
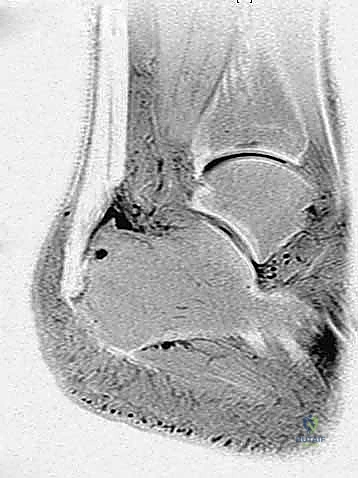
Crucially, the MRI helps us estimate the percentage of viable tendon that will remain after aggressive debridement. If we anticipate that more than 50% of the tendon footprint will be compromised or resected, we must preoperatively plan for and consent the patient for a Flexor Hallucis Longus (FHL) tendon transfer to augment the repair and provide a robust vascularized graft.
Operating Room Setup and Instrumentation
The operating room must be meticulously prepared for both the primary procedure and any potential augmentations. A standard foot and ankle orthopedic tray is required, supplemented with specific instruments for tendon and bone work. A high-speed microsagittal saw and a variety of sharp, curved osteotomes are essential for the calcaneal exostectomy. For tendon reattachment, we utilize a robust suture anchor system. I prefer a double-row configuration using 4.75mm or 5.5mm biocomposite or PEEK anchors loaded with high-tensile strength, ultra-high-molecular-weight polyethylene (UHMWPE) tape or suture.
If an FHL transfer is anticipated, an interference screw system (typically 7mm or 8mm) must be available on the back table. Intraoperative fluoroscopy (a mini C-arm) is absolutely mandatory. It is draped into the sterile field and positioned to provide orthogonal lateral and axial views of the calcaneus. This ensures precise, real-time visualization of the exostectomy trajectory, confirming complete removal of the impingement lesion without compromising the structural integrity of the calcaneal body, and verifying optimal trajectory and depth of the suture anchors.
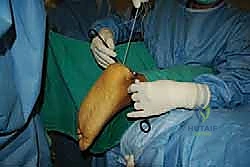
Patient Positioning and Tourniquet Management
Patient positioning is a critical sequence that dictates surgical access and safety. We employ a highly specific protocol to maximize efficiency and minimize neurological risk.
1. Tourniquet Application (Supine): The patient is initially brought into the operating room and placed supine on the stretcher. A well-padded thigh tourniquet is applied high on the operative leg. Applying the tourniquet while supine ensures the patient's lumbar spine is neutral and supported, avoiding the dangerous spinal torsion that often occurs when attempting to lift and rotate the leg of a prone, anesthetized patient.
2. Prone Positioning: Following the induction of general anesthesia or a regional block, the patient is carefully and synchronously log-rolled into the prone position onto the operating table.
3. Padding and Protection: Meticulous attention is paid to pressure points. The chest and iliac crests are supported with gel rolls to allow free abdominal excursion for ventilation and to prevent elevated venous pressures. The arms are positioned on arm boards with the elbows slightly flexed and the ulnar nerves completely free of compression. The knees are slightly flexed with a gel pad under the distal tibia.
4. Foot Positioning: The operative foot is positioned so that it hangs completely free off the distal edge of the operating table. This allows the surgeon unhindered, 360-degree access to the posterior heel and permits full passive plantarflexion and dorsiflexion of the ankle. This dynamic mobility is crucial for assessing the adequacy of the bony resection and for establishing the correct tension on the Achilles tendon during the final reattachment phase.
Step-by-Step Surgical Approach and Fixation Technique
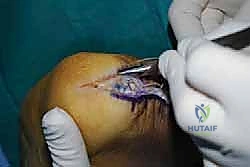
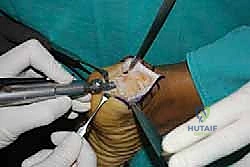
Incision and Deep Dissection
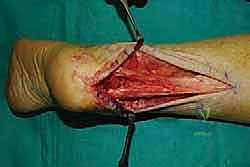
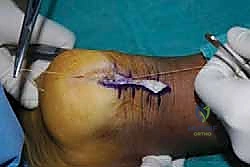
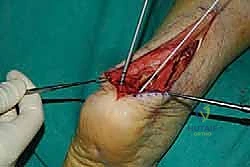
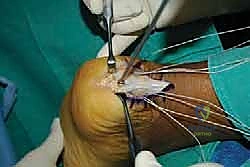
With the limb exsanguinated and the tourniquet inflated, we begin our approach. I utilize a central posterior longitudinal incision, placed directly midline over the Achilles tendon and the palpable calcaneal prominence.

This incision typically measures 6 to 8 centimeters, extending from the healthy proximal tendon down to the superior aspect of the plantar fat pad. The central approach is favored because it provides excellent, direct access to the pathology while inherently protecting the sural nerve laterally and the vascular structures medially, provided we stay strictly in the midline.
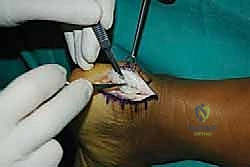
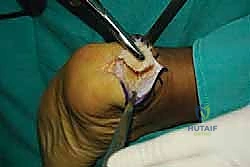
The skin and subcutaneous fat are incised sharply down to the paratenon. We meticulously avoid creating large subcutaneous flaps, as the posterior heel skin is notoriously prone to ischemic necrosis. Instead, we perform a full-thickness dissection directly down to the tendon substance. The paratenon is incised in line with the skin incision. Once the diseased Achilles tendon is visualized, a scalpel is used to make a robust, full-thickness longitudinal split directly down the center of the tendon, extending distally through its insertion onto the calcaneus.
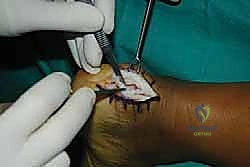
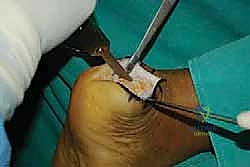
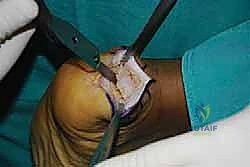
Tendon Detachment and Debridement
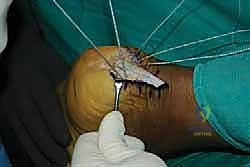
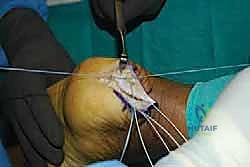
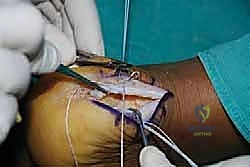
With the central split established, we must now reflect the tendon to expose the underlying pathology. Using a #15 blade or a sharp Cobb elevator, we meticulously elevate the medial and lateral halves of the Achilles tendon off the posterior calcaneus.
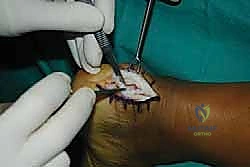
We are creating two distinct, full-thickness tendon slips. It is imperative to perform this elevation as a sharp, full-thickness peel directly off the bone, preserving the structural integrity of the tendon flaps and avoiding intra-substance delamination.
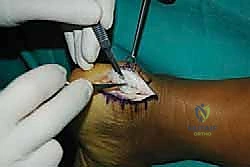
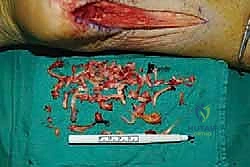
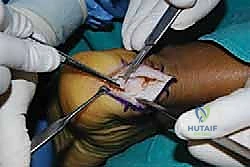
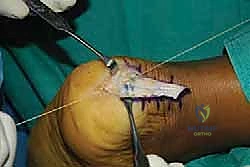
As we elevate these slips, we encounter the central core of the tendon, which is typically the epicenter of the degenerative process. This tissue is often fibrotic, disorganized, and laden with hard, chalky calcific deposits. We perform an aggressive debridement of this central diseased tissue, excising all non-viable tendon and enthesophytes until only healthy, parallel-oriented collagen fibers remain.
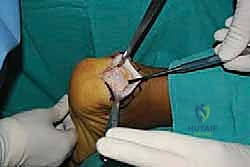
Simultaneously, the hypertrophic, inflamed retrocalcaneal bursa, now fully exposed deep to the tendon, is radically excised using a combination of sharp dissection and a motorized shaver. This clears the space and exposes the posterosuperior aspect of the calcaneus.
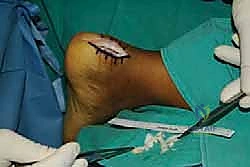
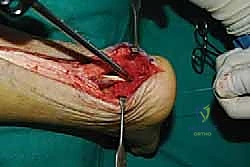
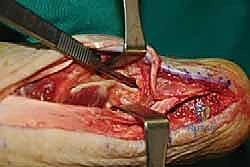
Calcaneal Exostectomy and Bursal Resection
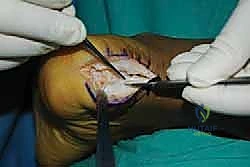
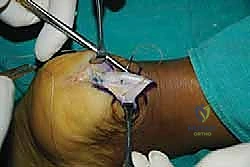
With the tendon slips retracted medially and laterally, the Haglund's deformity is clearly visualized. The goal of the exostectomy is to resect this prominence to eliminate impingement while maintaining a flat, bleeding cancellous bone bed for tendon reattachment.
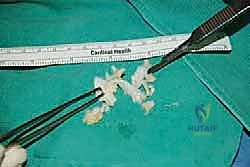
I typically begin by scoring the planned osteotomy line with a bovie electrocautery or a small osteotome. The trajectory should start just proximal to the distal tendon insertion footprint and angle dorsally and anteriorly.
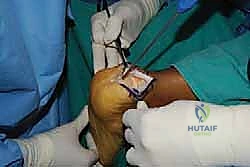
Using a microsagittal saw with a wide blade, the exostectomy is performed. It is crucial to irrigate copiously during sawing to prevent thermal necrosis of the surrounding bone, which could compromise anchor fixation.
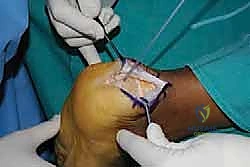
Following the primary saw cut, a rongeur and a rasp are utilized to smooth any sharp cortical edges, particularly at the medial and lateral borders of the resection, to prevent secondary fraying of the repaired tendon.
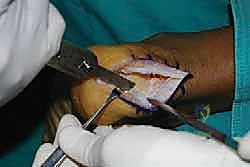
Before proceeding, the C-arm is brought in to obtain a strict lateral radiograph. This confirms that the posterosuperior prominence has been adequately resected, restoring a normal calcaneal contour, and that no residual bony impingement exists when the ankle is passively dorsiflexed.
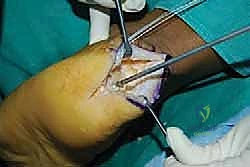
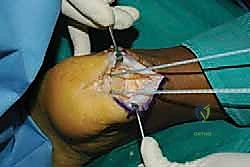
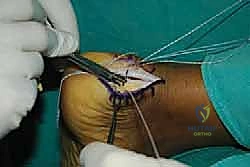
Tendon Reattachment and Augmentation Strategies
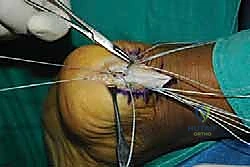
The final, critical phase is securing the healthy tendon back to the prepared calcaneal bed. The choice of fixation depends on the extent of tendon detachment. If less than 50% of the insertion was detached, a robust single-row repair may suffice. However, for extensive detachments, a double-row, suture-bridge technique is biomechanically superior, maximizing the footprint contact area and compression.
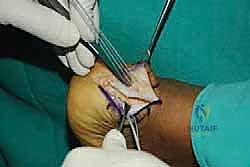
We begin by placing our proximal row of anchors (typically two 4.75mm anchors) into the dense bone at the proximal edge of the resected footprint. The anchors must be inserted at the "deadman's angle" (approximately 45 degrees to the direction of pull) to maximize pullout strength.
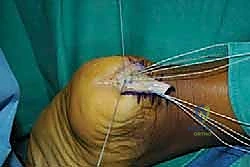
The sutures or tapes from these proximal anchors are then passed through the medial and lateral tendon slips using a self-retrieving suture passing instrument, utilizing a Krackow or locking mattress configuration.
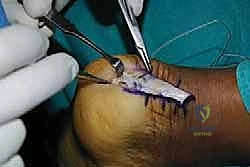
With the ankle held in resting equinus (typically 10-15 degrees of plantarflexion) to match the resting tension of the contralateral side, the sutures are tied, bringing the tendon down flush against the decorticated bone.
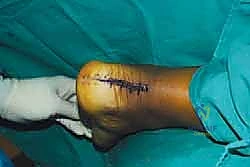
For a double-row repair, the suture tails from the proximal row are then crisscrossed and secured distally using knotless anchors placed at the inferior margin of the footprint, creating a pressurized, broad area of tendon-to-bone contact.
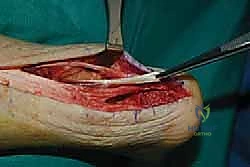
If intraoperative assessment reveals that the residual Achilles tendon is severely attenuated, friable, or if more than 50% of the footprint was resected, an FHL tendon transfer is immediately performed. Through the same posterior incision, deep dissection exposes the deep posterior compartment fascia. The FHL muscle belly is identified, and its tendon is harvested as distally as possible (often requiring a small medial midfoot incision for maximal length). A bone tunnel is drilled in the calcaneus, anterior to the Achilles footprint, and the FHL tendon is passed through and secured with an interference screw while the ankle is held in neutral dorsiflexion, providing both mechanical augmentation and a rich vascular supply to the healing environment.
Complications, Incidence Rates, and Salvage Management
Despite meticulous surgical technique, surgery for insertional Achilles tendinopathy carries a non-trivial risk profile. The most devastating and frequent complications involve the soft tissue envelope. The posterior heel skin has a tenuous blood supply, and excessive retraction, thick flaps, or underlying hematoma can lead to delayed wound healing, wound dehiscence, or frank skin necrosis. Superficial infections can often be managed with oral antibiotics and local wound care, but deep infections extending to the tendon or hardware represent a surgical emergency requiring aggressive serial debridements, hardware removal, and potentially complex soft tissue coverage (e.g., reverse sural artery flap or free tissue transfer).
Neurological complications, primarily involving the sural nerve, are also a significant concern. Sural neuritis or neuroma formation can occur due to direct iatrogenic injury, aggressive retraction, or entrapment within scar tissue. Patients present with burning, hyperesthesia, or numbness along the lateral aspect of the foot. Initial management includes gabapentinoids, desensitization therapy, and targeted nerve blocks. Refractory cases may necessitate surgical exploration, neurolysis, or proximal neurectomy with burial of the nerve stump into muscle.
Mechanical failures, such as anchor pullout or re-rupture of the Achilles tendon, are rare but catastrophic. They typically result from aggressive non-compliance with postoperative weight-bearing restrictions, poor bone quality (osteopenia), or inadequate initial fixation. Salvage of a failed repair is exceedingly complex and almost universally requires a robust tendon transfer (FHL or peroneus brevis) combined with an allograft reconstruction (e.g., Achilles tendon with calcaneal bone block) to restore the biomechanical integrity of the posterior chain.
| Complication | Estimated Incidence | Prevention Strategy | Salvage / Management Algorithm |
|---|---|---|---|
| Wound Dehiscence / Necrosis | 5% - 15% | Meticulous handling, full-thickness flaps, strict immobilization. | Local wound care, negative pressure wound therapy, potential flap coverage. |
| Sural Nerve Injury / Neuroma | 3% - 8% | Central midline incision, blunt lateral dissection, avoid blind suturing. | Gabapentinoids, diagnostic blocks; surgical neurolysis or proximal neurectomy. |
| Deep Infection | 1% - 3% | Pre-op antibiotics, copious irrigation, strict hemostasis. | Urgent operative I&D, hardware removal, IV antibiotics, ID consult. |
| Anchor Pullout / Re-rupture | < 2% | Double-row fixation, FHL transfer if >50% resected, strict rehab adherence. | Revision surgery with FHL transfer and/or Achilles allograft reconstruction. |
| Persistent Pain / Stiffness | 10% - 20% | Complete exostectomy (fluoroscopic verification), aggressive late-phase PT. | Prolonged conservative care, custom orthotics; rarely, revision exostectomy. |
Phased Post-Operative Rehabilitation Protocols
The postoperative rehabilitation following debridement and reattachment of the Achilles tendon is a protracted, highly structured process. Patient education is paramount; they must understand that full recovery and return to baseline athletic activity frequently requires 9 to 12 months. The protocol is divided into distinct biological phases to protect the repair while progressively restoring motion and strength.
Phase 1: Maximum Protection and Immobilization (Weeks 0-2)
Immediately postoperatively, the patient is placed in a bulky, well-padded short leg splint with the ankle immobilized in 15 to
Clinical & Radiographic Imaging Archive