Shoulder Arthroscopy Masterclass: A Comprehensive Intraoperative Guide
Key Takeaway
This masterclass guides fellows through shoulder arthroscopy, emphasizing meticulous technique and comprehensive understanding. We cover detailed surgical anatomy, precise patient positioning, and step-by-step intraoperative execution from portal creation to systematic diagnostic examination. Learn to identify key structures, manage potential pitfalls, and ensure optimal patient outcomes through expert pearls and post-operative strategies.
Comprehensive Introduction and Patho-Epidemiology
The evolution of shoulder arthroscopy represents one of the most profound paradigm shifts in modern orthopedic surgery. Transitioning from a mere diagnostic adjunct to the definitive therapeutic modality for complex intra-articular and subacromial pathology, arthroscopy has fundamentally altered our approach to the glenohumeral joint. The shoulder is a marvel of biomechanical engineering—a spheroidal, multiaxial articulation that prioritizes an immense range of motion at the direct expense of inherent bony stability. This delicate equilibrium relies heavily on a complex network of capsuloligamentous restraints and dynamic muscular force couples. As orthopedic surgeons, mastering shoulder arthroscopy requires not only exceptional psychomotor skills but also a profound, three-dimensional understanding of this intricate anatomy.
The epidemiological burden of shoulder disorders is staggering, carrying significant socioeconomic implications. Rotator cuff disease exists on a continuum, ranging from mild tendinopathy to massive, irreparable tears, and its prevalence increases exponentially with advancing age. Conversely, glenohumeral instability and superior labral anterior-to-posterior (SLAP) lesions predominantly afflict the younger, athletic demographic. The sheer volume of these pathologies necessitates a highly reproducible, minimally invasive surgical approach that minimizes soft tissue morbidity, accelerates rehabilitation, and optimizes functional outcomes. Arthroscopy fulfills these criteria, but only when executed with meticulous precision.
Diagnostic arthroscopy remains the absolute cornerstone of all advanced shoulder procedures. While high-resolution magnetic resonance imaging (MRI) and MR arthrography provide an excellent preoperative roadmap, they are not infallible. The arthroscope offers the definitive, magnified, real-time visualization of intra-articular and peri-articular structures. More importantly, it permits dynamic assessment and tactile feedback through probing—allowing the surgeon to assess tissue compliance, identify subtle labral detachments, and evaluate the structural integrity of the rotator cuff footprint. Proceeding to a therapeutic intervention without first conducting a rigorous, systematic diagnostic tour is akin to flying blind and frequently leads to missed concomitant pathologies.
The learning curve for advanced shoulder arthroscopy is notoriously steep. It demands a transition from the direct, macroscopic visualization of open surgery to navigating a fluid-filled, confined space via a two-dimensional monitor. Surgeons must develop intuitive triangulation skills, master the management of fluid dynamics to maintain a clear visual field without causing excessive soft tissue extravasation, and become proficient with an array of specialized instrumentation. This masterclass chapter is designed to bridge the gap between foundational knowledge and advanced intraoperative execution, providing a comprehensive guide to navigating the complexities of the arthroscopic shoulder.
Detailed Surgical Anatomy and Biomechanics
Osteology and the Bony Framework
The bony architecture of the shoulder girdle forms the foundation upon which the complex soft tissue envelope operates. The glenoid fossa of the scapula is a shallow, pear-shaped socket that articulates with the humeral head. Its orientation is paramount for stability; it is typically anteverted and features a superior tilt. The articular surface of the glenoid is significantly smaller than that of the humeral head—often likened to a golf ball sitting on a golf tee—which underscores the absolute necessity of robust capsular and muscular stabilizers. The "bare area" of the glenoid, a central region devoid of articular cartilage, is a normal anatomical variant that must not be mistaken for a chondral defect.
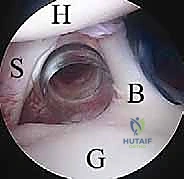
The proximal humerus consists of the spherical articular head, the anatomical neck, and the greater and lesser tuberosities. The humeral head is typically retroverted relative to the epicondylar axis of the distal humerus, a critical factor in understanding both native biomechanics and arthroplasty templating. The relationship between the humeral head and the glenoid dictates the joint's instantaneous center of rotation. Any alteration in this relationship, whether through bone loss (e.g., an engaging Hill-Sachs lesion or a bony Bankart) or soft tissue failure, leads to obligate translation and subsequent instability.
The acromion, a lateral extension of the scapular spine, forms the rigid roof of the subacromial space. Its morphology, famously classified by Bigliani into Type I (flat), Type II (curved), and Type III (hooked), plays a historic, albeit debated, role in the pathogenesis of external subacromial impingement. Anteriorly, the coracoid process—a hook-like projection from the scapula—serves as the "lighthouse of the shoulder." It is the origin for the conjoined tendon (short head of the biceps and coracobrachialis) and the insertion site for the pectoralis minor, making it a critical surgical landmark, yet a notorious danger zone due to its proximity to the brachial plexus and axillary vessels.
The clavicle acts as the sole bony strut connecting the upper extremity to the axial skeleton via the sternoclavicular (SC) joint, while articulating laterally with the acromion at the acromioclavicular (AC) joint. The AC joint is frequently a source of superior shoulder pain due to degenerative arthropathy or distal clavicle osteolysis. Understanding the spatial relationship between the clavicle, acromion, and coracoid is essential for navigating the subacromial space and performing procedures such as distal clavicle excision or coracoacromial ligament release.
Static Stabilizers and Capsuloligamentous Complex
The glenohumeral joint capsule is a redundant, fibrous sac designed to permit a massive arc of motion; however, specific thickenings within this capsule form the glenohumeral ligaments, which serve as the primary static restraints to translation. The superior glenohumeral ligament (SGHL) originates from the superior labrum and courses to the lesser tuberosity. Working in concert with the coracohumeral ligament (CHL), the SGHL forms a critical component of the rotator interval, primarily resisting inferior translation of the humeral head when the arm is adducted and in external rotation.
The middle glenohumeral ligament (MGHL) exhibits significant anatomical variability. It typically originates from the anterosuperior glenoid and inserts medial to the lesser tuberosity, acting as the primary restraint to anterior translation when the arm is abducted to 45 degrees. Surgeons must be acutely aware of normal variants, most notably the Buford complex. This variant is characterized by a thick, cord-like MGHL originating directly from the superior labrum, accompanied by a congenital absence of the anterosuperior labrum. Mistakenly "repairing" a Buford complex to the glenoid rim will result in severe, iatrogenic restriction of external rotation.
The inferior glenohumeral ligament (IGHL) complex is the most robust and biomechanically crucial static stabilizer, functioning much like a hammock suspending the humeral head. It is composed of a distinct anterior band, a posterior band, and an intervening axillary pouch. The anterior band is the primary restraint against anterior translation when the shoulder is positioned in 90 degrees of abduction and maximal external rotation—the classic apprehension position. Conversely, the posterior band resists posterior translation in abduction and internal rotation.
The glenoid labrum is a fibrocartilaginous ring that circumscribes the glenoid rim, effectively deepening the concavity of the socket by up to 50%. It acts as a "chock-block" against humeral head translation and serves as the crucial attachment site for the glenohumeral ligaments and the long head of the biceps tendon. Pathology of the labrum, whether an anterior-inferior detachment (Bankart lesion) or a superior labral tear (SLAP lesion), fundamentally disrupts the tensioning of the capsuloligamentous complex, leading to symptomatic micro- or macro-instability that frequently necessitates arthroscopic repair.
Dynamic Stabilizers and the Rotator Cuff
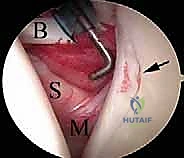
The dynamic stability of the shoulder is governed by the coordinated action of the rotator cuff musculature—the supraspinatus, infraspinatus, teres minor, and subscapularis. These muscles do not function in isolation; rather, they operate as intricate force couples that compress the humeral head into the glenoid concavity during arm elevation. The superior force couple (supraspinatus) initiates abduction, while the anterior (subscapularis) and posterior (infraspinatus, teres minor) force couples balance the humeral head in the transverse plane. Disruption of these force couples, such as in a massive rotator cuff tear, leads to superior migration of the humeral head and altered joint kinematics.
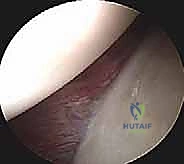
The anatomical footprint of the rotator cuff on the greater and lesser tuberosities is a critical area of focus during arthroscopic repair. The supraspinatus and infraspinatus tendons interdigitate near their insertions, forming a continuous fibrous sheet. Burkhart's concept of the "suspension bridge" describes a thickened band of tissue, the rotator cable, which spans from the coracohumeral ligament to the teres minor, stress-shielding the thinner, more avascular rotator crescent. Understanding this architecture is vital; tears involving the cable significantly alter the biomechanical transmission of forces and require meticulous anatomical restoration.
The subscapularis, the largest and most powerful of the rotator cuff muscles, is a critical anterior stabilizer. It originates from the subscapular fossa and inserts onto the lesser tuberosity. The superior border of the subscapularis forms the inferior boundary of the rotator interval. Arthroscopic evaluation of the subscapularis requires specific maneuvers, such as internal rotation and posterior levering of the humerus, to visualize its insertion. The "comma sign," a distinct arc of tissue representing the avulsed medial sling of the biceps and the superior glenohumeral ligament, is a pathognomonic arthroscopic marker for a retracted upper subscapularis tear.
The long head of the biceps (LHB) tendon is an accessory dynamic stabilizer with a complex, intra-articular yet extrasynovial trajectory. Originating from the supraglenoid tubercle and superior labrum (the biceps anchor), it courses through the joint, exits via the rotator interval, and descends into the bicipital groove. The LHB acts as a humeral head depressor and contributes to anterior stability. However, it is frequently a primary source of anterior shoulder pain due to tenosynovitis, subluxation (often associated with subscapularis tears), or partial tearing. The decision to perform a biceps tenotomy versus tenodesis depends on patient age, activity level, and cosmetic concerns regarding the "Popeye" deformity.
Neurovascular Danger Zones
Navigating the arthroscopic environment requires an acute, constant awareness of the surrounding neurovascular arborization. The axillary nerve is arguably the most vulnerable structure during shoulder arthroscopy. Originating from the posterior cord of the brachial plexus, it traverses the quadrangular space and courses circumferentially around the surgical neck of the humerus, innervating the deltoid and teres minor. It lies precariously close to the inferior joint capsule (approximately 10-15 mm inferior to the glenoid rim). When establishing a lateral or posterior portal, or when performing inferior capsular releases, instruments must be directed superiorly and meticulously controlled to avoid catastrophic denervation of the deltoid.
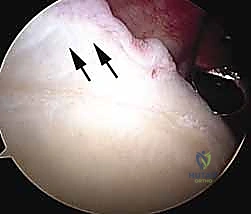
The anterior compartment houses the musculocutaneous nerve, which typically pierces the coracobrachialis muscle 3 to 5 centimeters distal to the tip of the coracoid process. When establishing anterior portals, particularly the standard anterior or anteroinferior portals, the trajectory must always remain lateral to the coracoid process. Venturing medial to the coracoid enters absolute danger territory, placing not only the musculocutaneous nerve at risk but also the entire brachial plexus and the axillary artery and vein. The coracoid serves as the absolute medial boundary for any arthroscopic instrumentation.
The suprascapular nerve provides motor innervation to the supraspinatus and infraspinatus. It courses through the suprascapular notch (beneath the transverse scapular ligament) and then winds around the spinoglenoid notch to reach the infraspinous fossa. The nerve is at risk during extensive posterior capsular releases, during the repair of massive, retracted posterior rotator cuff tears where aggressive medial mobilization is required, or during the placement of posterosuperior portals (e.g., the Port of Wilmington) if the trajectory is directed too medially into the spinoglenoid notch.
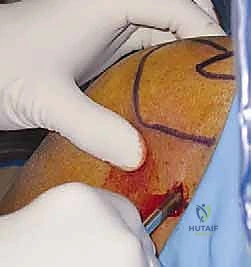
Finally, the cephalic vein, which delineates the deltopectoral interval, must be considered when establishing anterior portals or converting to an open approach. While less catastrophic than a major nerve injury, iatrogenic injury to the cephalic vein can cause troublesome bleeding that obscures the arthroscopic visual field and complicates fluid management. A thorough understanding of these danger zones, coupled with meticulous portal placement utilizing the "outside-in" spinal needle localization technique, is the surgeon's best defense against devastating iatrogenic complications.
Exhaustive Indications and Contraindications
The decision to proceed with shoulder arthroscopy must be rooted in a rigorous clinical evaluation, advanced imaging findings, and the exhaustion of appropriate non-operative modalities. Arthroscopy is not a panacea; it is a highly specific surgical tool indicated for distinct anatomical lesions that have failed conservative management. The surgeon must carefully weigh the patient's physiological age, functional demands, medical comorbidities, and psychological readiness to adhere to a strict, often prolonged, postoperative rehabilitation protocol.
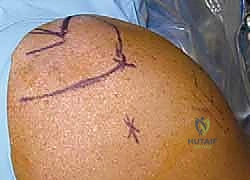
Indications for arthroscopic intervention are broad but well-defined. Full-thickness rotator cuff tears in symptomatic patients, particularly those that are acute or traumatic, are prime indications. Partial-thickness tears that have failed conservative care (e.g., physical therapy, subacromial corticosteroid injections) and involve greater than 50% of the tendon footprint may warrant completion and repair, or in-situ repair. Glenohumeral instability, encompassing acute first-time dislocators in high-demand athletes, recurrent anterior or posterior instability, and multidirectional instability refractory to aggressive physical therapy, are routinely managed arthroscopically with labral repair and capsular plication.
Other robust indications include the management of superior labral anterior-to-posterior (SLAP) lesions, particularly in overhead athletes, though the trend in older populations leans heavily toward biceps tenodesis. Subacromial impingement syndrome refractory to non-operative measures may be addressed via arthroscopic subacromial decompression and acromioplasty, though this is rarely an isolated procedure today. Additionally, arthroscopy is invaluable for the removal of loose bodies, management of synovial diseases (e.g., synovial chondromatosis, pigmented villonodular synovitis), and the treatment of early-stage adhesive capsulitis (frozen shoulder) via capsular release when prolonged conservative management fails.
Contraindications, while fewer, are absolute and must be respected to avoid catastrophic outcomes. Active, untreated local or systemic infection is an absolute contraindication to elective arthroscopy. Advanced glenohumeral osteoarthritis, characterized by significant joint space narrowing, large osteophytes, and subchondral sclerosis, is a contraindication for arthroscopic debridement as a definitive procedure; these patients are appropriately managed with arthroplasty. Severe, unyielding stiffness in the highly inflammatory "freezing" phase of adhesive capsulitis is a relative contraindication, as surgical trauma can exacerbate the fibroproliferative response.
| Category | Indications | Contraindications |
|---|---|---|
| Rotator Cuff | Full-thickness tears, high-grade partial tears (>50%), acute traumatic tears. | Asymptomatic tears, massive irreparable tears without pseudo-paralysis (relative). |
| Instability | Recurrent dislocations, Bankart lesions, symptomatic multidirectional instability. | Voluntary dislocators with underlying psychiatric disorders. |
| Labrum/Biceps | Symptomatic SLAP tears, LHB tenosynovitis/tears, symptomatic internal impingement. | Advanced age with SLAP (prefer tenodesis), asymptomatic variants (Buford). |
| Articular/Synovial | Loose bodies, recalcitrant adhesive capsulitis, synovial chondromatosis, septic arthritis (washout). | Advanced glenohumeral osteoarthritis (bone-on-bone), active overlying cellulitis. |
| Patient Factors | Failure of 3-6 months conservative care, high functional demand, compliant with rehab. | Medical instability for anesthesia, inability to comply with postoperative immobilization. |
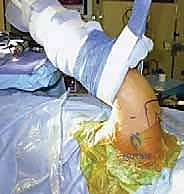
Pre-Operative Planning, Templating, and Patient Positioning
Clinical Evaluation and Advanced Imaging
Surgical success is predicated on meticulous preoperative planning, which begins with a comprehensive history and physical examination. The surgeon must ascertain the mechanism of injury, the chronicity of symptoms, and the precise character of the pain. Night pain and weakness are classic hallmarks of rotator cuff pathology, whereas a sensation of "dead arm" or apprehension in the abducted/externally rotated position points toward anterior instability. A systematic physical exam must include a thorough assessment of active and passive range of motion, cervical spine clearance to rule out radiculopathy, and specific provocative testing (e.g., Neer's and Hawkins for impingement; Jobe's test for supraspinatus; O'Brien's test for SLAP lesions; and the apprehension/relocation test for anterior instability).
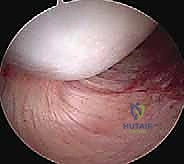
Standard radiographic evaluation is mandatory and should never be bypassed in favor of an MRI. A complete trauma series includes a true anteroposterior (Grashey) view to assess joint space and superior humeral head migration, an axillary lateral view to evaluate glenohumeral congruity and glenoid wear, and a scapular Y view to assess acromial morphology. Specialized views, such as the Stryker notch view for Hill-Sachs lesions or the West Point view for bony Bankart lesions, may be ordered based on clinical suspicion.
Advanced imaging is the final step in the diagnostic workup. High-field MRI without contrast is highly sensitive and specific for evaluating the integrity of the rotator cuff, assessing muscle atrophy (Goutallier classification), and identifying subchondral edema. However, for suspected labral pathology, capsular injuries, or subtle instability patterns, an MR arthrogram is the gold standard. The intra-articular gadolinium distends the joint capsule, beautifully outlining labral tears, SLAP lesions, and capsular avulsions (e.g., HAGL lesions). In cases of significant instability where bone loss is suspected, a 3D computed tomography (CT) scan with digital subtraction of the humeral head is essential for accurately quantifying glenoid bone loss, which dictates whether a soft-tissue stabilization or a bony augmentation (e.
Clinical & Radiographic Imaging Archive