Operative Management of Chronic Ankle and Proximal Tibiofibular Joint Dislocations
Key Takeaway
The management of chronic, unreduced ankle dislocations and proximal tibiofibular joint instability presents a formidable challenge in orthopedic surgery. This comprehensive guide details the pathoanatomy, biomechanics, and step-by-step surgical approaches required to address these complex deformities. Emphasis is placed on meticulous preoperative planning, soft tissue balancing, and rigid fixation to restore joint congruency and optimize functional outcomes in both idiopathic and posttraumatic presentations.
INTRODUCTION TO CHRONIC LOWER EXTREMITY DISLOCATIONS
The management of old, unreduced dislocations of the lower extremity, specifically those involving the tibiotalar (ankle) joint and the proximal tibiofibular joint (PTFJ), requires a profound understanding of regional biomechanics, soft-tissue contractures, and altered pathoanatomy. Unlike acute injuries, chronic dislocations are complicated by severe soft-tissue contracture, capsular scarring, osteopenia, and articular cartilage degradation. This chapter provides an exhaustive, evidence-based framework for the operative management of these complex and often debilitating conditions.
CHRONIC UNREDUCED ANKLE DISLOCATIONS
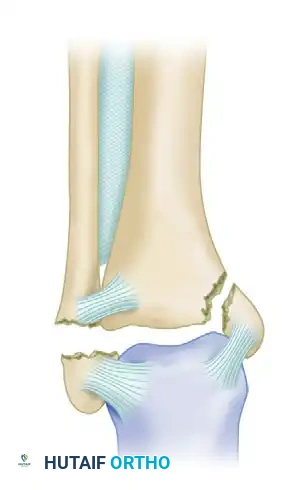
An old, unreduced dislocation of the ankle without an associated fracture is an exceedingly rare clinical entity. The inherent stability of the ankle mortise is provided by the congruent osseous architecture of the tibial plafond and the talar dome, augmented by the robust medial deltoid ligament complex, the lateral collateral ligaments, and the distal tibiofibular syndesmosis. Consequently, the type, direction, and severity of an ankle dislocation are almost universally dictated by the pattern of associated osseous failure.
Pathoanatomy and Injury Patterns
The direction of the talar displacement relative to the tibia defines the dislocation. In chronic settings, the surrounding soft tissues adapt to the deformed position, making delayed reduction a formidable surgical challenge.
- Anterior Dislocations: These are typically the result of forced dorsiflexion combined with axial loading. An anterior dislocation is almost always complicated by a shear or impaction fracture of the anterior margin of the distal articular surface of the tibia (anterior plafond).
- Posterior Dislocations: The most common variant, posterior dislocations occur via forced plantarflexion and axial loading. They are usually complicated by a fracture of the distal tibia, specifically involving the posterior margin (posterior malleolus) and a portion of the metaphysis, or they present as a classic trimalleolar fracture-dislocation.
- Lateral Dislocations: These require significant disruption of the medial structures (deltoid ligament or medial malleolus) and the syndesmosis. A lateral dislocation is usually complicated by a lateral malleolar or bimalleolar fracture.
Clinical Pearl: In chronic unreduced ankle dislocations, the articular cartilage of the talus undergoes rapid degeneration due to abnormal pressure distributions and lack of synovial fluid nourishment. Preoperative counseling must include the high likelihood of post-traumatic osteoarthritis and the potential future need for tibiotalar arthrodesis.
Preoperative Evaluation and Planning
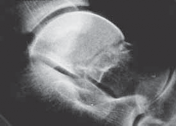
Advanced imaging is mandatory. Weight-bearing radiographs (if tolerated) provide a baseline, but a fine-cut Computed Tomography (CT) scan with 3D reconstructions is essential to delineate the fracture morphology, identify intra-articular loose bodies, and assess bone stock. Magnetic Resonance Imaging (MRI) may be utilized to evaluate the integrity of the articular cartilage and the degree of soft-tissue interposition, particularly the posterior tibial tendon or the peroneal tendons, which can become incarcerated in the joint space.
Surgical Management of the Unreduced Ankle
The primary goal of surgery is to achieve a concentric, stable reduction of the talus within the mortise, restore fibular length, and reconstruct the ligamentous restraints.
Patient Positioning and Anesthesia
The patient is placed supine on a radiolucent operating table. A bump is placed under the ipsilateral hip to internally rotate the leg, bringing the lateral malleolus forward. General anesthesia or a robust regional block is employed, and a thigh tourniquet is applied.
Surgical Approaches
A dual-incision technique is frequently required to address both medial and lateral pathology, as well as to clear the gutters of fibrotic tissue.
- Direct Lateral Approach: Centered over the fibula, extending distally toward the base of the fifth metatarsal. This allows access to the lateral malleolus, the anterolateral joint capsule, and the syndesmosis.
- Anteromedial or Posteromedial Approach: Depending on the location of the incarcerated structures and the medial malleolar fracture. An anteromedial approach allows visualization of the medial gutter and the deltoid ligament.
Step-by-Step Surgical Technique
- Soft Tissue Release and Debridement: The most critical step in a chronic dislocation is mobilizing the joint. The anterolateral and anteromedial capsules are often heavily scarred. A meticulous capsulectomy is performed. The medial and lateral gutters must be cleared of all fibrotic tissue.
- Addressing Contractures: In posterior dislocations, the Achilles tendon and posterior capsule are severely contracted. A percutaneous or open Tendo-Achilles Lengthening (TAL) or a Strayer procedure (gastrocnemius recession) is almost universally required to allow the talus to translate anteriorly.
- Joint Reduction: Once the soft tissues are released, longitudinal traction is applied. A Schanz pin can be placed into the neck of the talus or the calcaneus to act as a "joystick" to assist in manipulating the talus back into the mortise.
- Fracture Fixation:
- Fibular Length: The fibula must be out to length and anatomically rotated. This is the cornerstone of ankle stability. Rigid plate osteosynthesis is performed.
- Posterior Malleolus: If a large posterior malleolar fragment is present, it should be reduced and fixed, either via a posterolateral approach with a buttress plate or via anterior-to-posterior lag screws, to restore the posterior restraint of the ankle.
- Medial Malleolus: Fixed with partially threaded cancellous screws or a tension band construct.
- Syndesmotic Stabilization: Chronic dislocations often feature a grossly unstable syndesmosis. After anatomic reduction of the fibula into the incisura fibularis, the syndesmosis is stabilized using two quadricortical syndesmotic screws or dynamic suture button constructs.
- Ligamentous Reconstruction: If the deltoid or lateral collateral ligaments are irreparably attenuated, primary repair augmented with suture tape or allograft reconstruction may be necessary to restore coronal plane stability.
Surgical Warning: Aggressive soft tissue stripping around the talar neck must be avoided to minimize the risk of avascular necrosis (AVN) of the talus, a devastating complication in chronic fracture-dislocations.
Postoperative Protocol
- 0-2 Weeks: The patient is placed in a bulky Jones dressing with a posterior splint in neutral dorsiflexion. Strict non-weight-bearing (NWB) status is maintained.
- 2-6 Weeks: Sutures are removed. The patient is transitioned to a short-leg cast or a rigid fracture boot, remaining NWB.
- 6-12 Weeks: Progressive weight-bearing is initiated based on radiographic evidence of fracture healing. Active range of motion (ROM) exercises begin.
- 3-6 Months: Aggressive physical therapy focusing on proprioception, peroneal strengthening, and gait mechanics.
THE PROXIMAL TIBIOFIBULAR JOINT (PTFJ)
The proximal tibiofibular joint is a diarthrodial synovial joint that plays a subtle but critical role in the biomechanics of the lower extremity. It dissipates torsional stresses applied at the ankle, absorbs lateral tibial bending moments, and transmits approximately one-sixth of the static weight-bearing load.
Anatomy and Biomechanics
The joint is stabilized by the anterior and posterior superior tibiofibular ligaments, the interosseous membrane, the biceps femoris tendon, and the lateral collateral ligament (LCL) of the knee. The common peroneal nerve courses intimately around the fibular neck, making it highly vulnerable during both injury and surgical intervention.
Ogden Classification of PTFJ Instability
Ogden's seminal work categorized PTFJ subluxations and dislocations into distinct clinical entities, primarily dividing them into idiopathic and posttraumatic types.
Idiopathic Subluxation
The idiopathic type occurs primarily in preadolescent or adolescent children, with a higher prevalence in females. It is frequently associated with generalized ligamentous laxity (e.g., Ehlers-Danlos or Marfan syndrome). Interestingly, it can also manifest in patients in their late 40s and 50s as secondary soft-tissue restraints attenuate with age.
- Clinical Presentation: Patients typically complain of lateral knee pain, a "popping" sensation, or a feeling of instability, particularly during activities involving knee flexion and tibial internal rotation.
- Management: Idiopathic subluxation is almost exclusively treated nonoperatively. Because it appears to be a self-limited condition in young patients, surgical intervention is strongly discouraged. Initial treatment consists of activity modification, physical therapy focusing on biceps femoris and popliteus strengthening, and occasionally, a brief period of cast immobilization if acutely symptomatic.
Posttraumatic Dislocation
Posttraumatic dislocations are high-energy injuries, often seen in equestrians, paratroopers, and athletes. Ogden further classified these based on the direction of displacement:
* Type I: Subluxation (excessive translation without complete dislocation).
* Type II: Anterolateral dislocation (most common, usually from a fall on a flexed knee with the foot inverted).
* Type III: Posteromedial dislocation (often associated with direct trauma and high risk of peroneal nerve injury).
* Type IV: Superior dislocation (invariably associated with high-energy tibial shaft fractures or severe ankle syndesmotic disruptions).
Surgical Management of Chronic PTFJ Instability
Surgery is indicated in older patients or posttraumatic cases where the subluxation/dislocation becomes chronic, exquisitely painful, and refractory to prolonged immobilization and physical therapy.
Surgical Options
The surgical management of chronic PTFJ instability is controversial, with three primary techniques described in the literature:
- Fibular Head Resection:
- Indications: Chronic, painful arthrosis of the PTFJ without gross knee instability.
- Technique: A lateral approach is utilized. The common peroneal nerve is meticulously identified and neurolysed. The fibular head is resected oblique to the shaft.
- Critical Step: The LCL and the biceps femoris tendon, which insert on the fibular head, must be carefully detached and rigidly reattached to the lateral tibial metaphysis (usually via suture anchors or a bone tunnel) to prevent catastrophic posterolateral rotatory instability (PLRI) of the knee.
- Proximal Tibiofibular Arthrodesis:
- Indications: Chronic instability in high-demand patients.
- Technique: The articular cartilage of the PTFJ is denuded down to bleeding subchondral bone. The joint is reduced and fixed with two fully threaded cancellous lag screws.
- Pitfall: Arthrodesis of the PTFJ eliminates the normal proximal-distal excursion of the fibula during ankle dorsiflexion. This can lead to secondary ankle pain, restricted ankle motion, and eventual syndesmotic failure. Therefore, some authors recommend a concomitant excision of a small segment of the fibular shaft (a distal fibulectomy) to decouple the ankle from the fused PTFJ, though this is highly morbid.
- Ligamentous Reconstruction:
- Indications: Chronic instability where joint preservation is desired.
- Technique: Various techniques exist, including rerouting a slip of the biceps femoris tendon through a drill hole in the lateral tibia, or utilizing a free tendon allograft (e.g., semitendinosus) routed in a figure-of-eight fashion between the fibular head and the lateral tibial tubercle (Gerdy's tubercle) to recreate the anterior and posterior superior tibiofibular ligaments.
Pitfall: Failure to identify, protect, and neurolyse the common peroneal nerve during any surgical approach to the proximal tibiofibular joint is the most common cause of devastating postoperative morbidity (foot drop). The nerve must be visualized and protected throughout the entirety of the procedure.
Postoperative Protocol for PTFJ Surgery
- 0-2 Weeks: The knee is immobilized in a hinged knee brace locked in extension. The patient is restricted to toe-touch weight-bearing (TTWB).
- 2-6 Weeks: Passive and active-assisted ROM is initiated, typically limiting flexion to 90 degrees to protect the ligamentous reconstruction or LCL reattachment. Weight-bearing is gradually advanced.
- 6-12 Weeks: Full weight-bearing is permitted. The brace is discontinued. Strengthening focuses on the hamstrings, quadriceps, and peroneal musculature.
- Return to Play: Typically permitted at 4 to 6 months postoperatively, contingent upon the restoration of symmetric knee stability and the absence of lateral joint line pain.
CONCLUSION
The operative management of chronic, unreduced dislocations of the ankle and proximal tibiofibular joint demands meticulous surgical execution. In the ankle, success hinges upon aggressive soft-tissue mobilization, anatomic restoration of the fibula, and rigid stabilization of the mortise. In the proximal tibiofibular joint, the surgeon must carefully balance the need for stability against the biomechanical consequences of arthrodesis, all while maintaining absolute vigilance over the common peroneal nerve. Through strict adherence to these evidence-based principles, orthopedic surgeons can salvage function and mitigate the long-term sequelae of these severe lower extremity deformities.
📚 Medical References
- Ankle dislocation without fracture: an on-fi eld perspective, Clin J Sport Med 16:269, 2006.
- Ramasamy P, Ward A: Distal tibiofi bular joint dislocation with an intact fi bula: a classifi cation system, Injury 34:862, 2003.
- Shaik MM, Tandon T, Agrawal Y, et al: Medial and lateral rotatory dislocations of the ankle after trivial trauma—pathomechanics and results of two cases, J Foot Ankle Surg 45:346, 2006.
- Uyar M, Tan A, Isler M, et al: Closed posteromedial dislocation of the tibiotalar joint without fracture in a basketball player, Br J Sports Med 38:342, 2004.
- Patella Ahmad CS, Stein BE, Matuz D, et al: Immediate surgical repair of the medial patellar stabilizers for acute
You Might Also Like