Advanced Surgical Management of Congenital Ring Syndrome
Key Takeaway
Congenital ring syndrome, also known as amniotic band sequence, presents with circumferential constriction bands, acrosyndactyly, or intrauterine amputations. Surgical management is dictated by the depth of the band and distal vascularity. Emergent release is required for vascular compromise, while staged Z-plasties address severe lymphedema. Advanced reconstruction, including non-vascularized toe phalangeal transfers, restores length and function in amputated digits, requiring meticulous soft tissue handling and rigid Kirschner wire fixation.
Introduction and Pathogenesis
Congenital ring syndrome, frequently referred to in the literature as congenital constriction band syndrome, amniotic band sequence (ABS), Streeter dysplasia, or annular grooves, is a complex congenital anomaly characterized by deep cutaneous creases that encircle a limb or digit. The visual presentation often mimics a string tightly tied around the affected part, leading to varying degrees of distal vascular and lymphatic compromise.
The condition has an estimated incidence of 1 in 15,000 live births and accounts for approximately 2% of all congenital hand anomalies. It predominantly affects the distal extremities, with the central digits of the hand being the most frequently involved.
Etiological Theories
There is no evidence to suggest that congenital ring syndrome is an inherited genetic condition. The exact etiology remains a subject of historical and contemporary debate, primarily divided into two prevailing theories:
- Extrinsic Theory (Kinnier Wilson and Torpin): This is the most widely accepted model. It postulates that early rupture of the amnion leads to the formation of mesodermic fibrous bands. These amniotic bands entangle the developing fetal limbs, causing mechanical constriction, secondary ischemia, and subsequent amputation or deformity.
- Intrinsic Theory (Streeter): Streeter originally proposed that the bands result from a failure of normal embryonic germ plasm development, specifically a localized failure of subcutaneous tissue formation, similar to the embryogenesis of normal skin creases. He suggested that hemorrhages in the distal rays lead to the formation of amniotic adhesions in utero.
There is general consensus that these malformations occur later in gestation than typical congenital hand anomalies. While most intrinsic hand anomalies develop between the 5th and 7th weeks of gestation, congenital ring syndrome typically occurs after this period. The youngest fetus documented with this specific anomaly was at 10 weeks of gestation.
Clinical Presentation and Classification
The clinical presentation of congenital ring syndrome is highly variable, ranging from mild, superficial cosmetic grooves to severe, limb-threatening constrictions and complete intrauterine amputations.

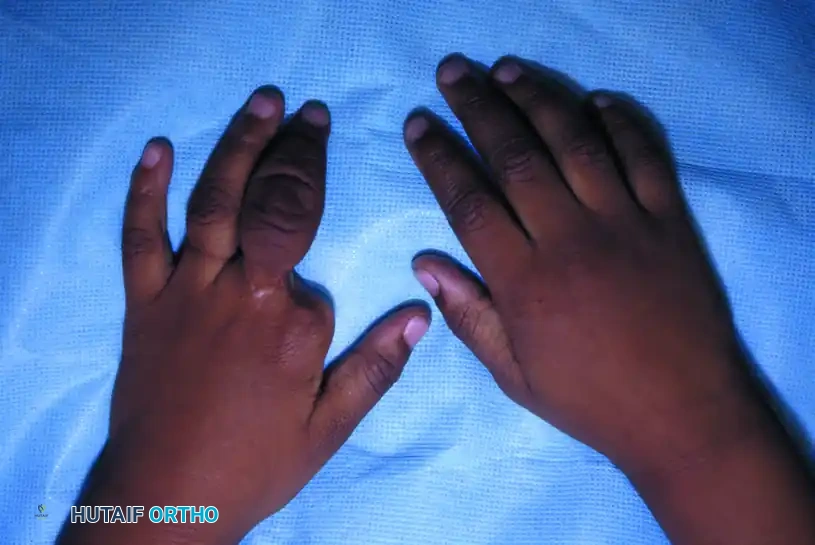
Clinical presentation of congenital ring syndrome demonstrating intrauterine amputation of the index finger and severe lymphedema of the long finger due to a deep proximal constriction band.
Patterson Classification
Patterson systematically categorized the deformities associated with congenital ring syndrome into four distinct types. These types may present in isolation or in any combination within a single patient, but they do not consistently correlate with other intrinsic limb anomalies (such as symphalangism or camptodactyly).
- Type 1: Simple Constriction Rings: These rings usually occur transversely, though occasionally obliquely, around the limb or digit. They are superficial, affecting only the skin and immediate subcutaneous tissue without compromising distal lymphatic or venous drainage.
- Type 2: Deep Rings with Distal Abnormality: These rings penetrate deeply into the fascia, obstructing lymphatic and venous return. This results in significant distal lymphedema, bulbous swelling, and potential vascular compromise.
- Type 3: Fenestrated Syndactyly (Acrosyndactyly): Characterized by the lateral fusion of adjacent digits at their distal ends, with proximal fenestrations (epithelialized clefts) remaining between the intervening skin and soft tissue. This is pathognomonic for amniotic band sequence.
- Type 4: Intrauterine Amputation: The most severe manifestation, where the mechanical constriction leads to complete ischemia and auto-amputation of the distal part. The soft tissues are typically more affected than the bone, which may protrude distally (resembling a guillotine amputation). There are no rudimentary parts distally, and the proximal limb structures are normally developed.
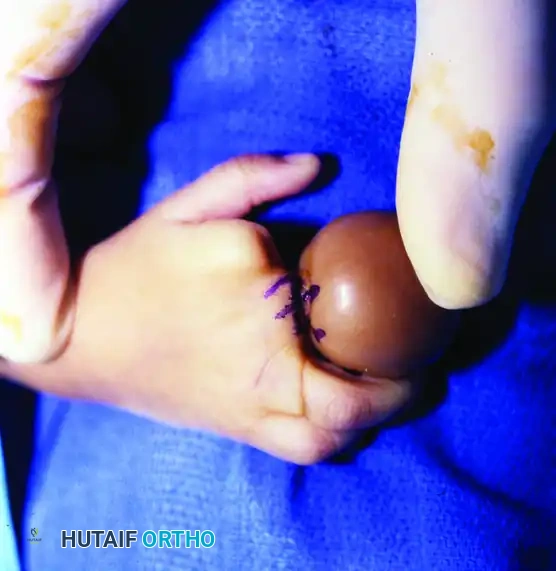
Clinical Pearl: In cases of severe lymphedema (Patterson Type 2), assess capillary refill immediately at birth. If good capillary refill is present despite severe bulbous swelling, surgical intervention can be safely postponed for 1 to 3 months to allow the infant to grow, significantly lessening the anesthetic and surgical risks.
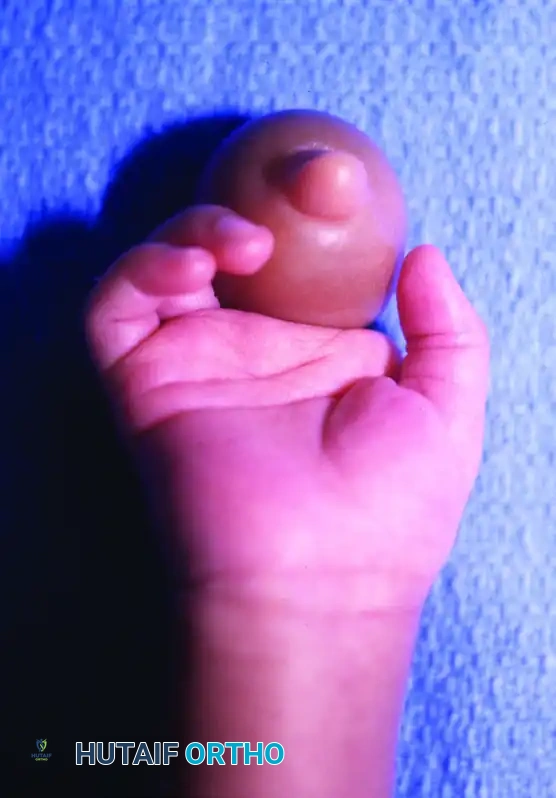
Close-up view of severe distal lymphedema secondary to a deep Patterson Type 2 constriction band. Note the bulbous engorgement of the soft tissues.
Preoperative Evaluation and Imaging
Thorough clinical examination must assess the vascular status of the affected digits. Doppler ultrasound may be utilized to confirm arterial patency in severely edematous digits.
Standard orthogonal radiographs (anteroposterior and lateral) of the affected extremity are mandatory. Radiographs help delineate the extent of bone involvement, identify protruding phalangeal shafts in intrauterine amputations, and reveal characteristic bony deformities caused by the chronic constriction.
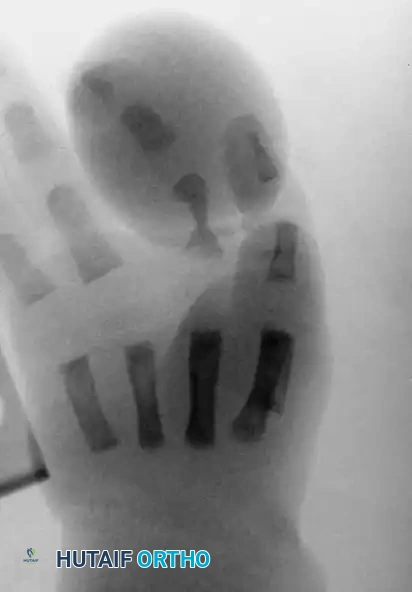
Preoperative radiograph demonstrating the classic "hourglass" deformity of the proximal phalanx, a direct result of chronic osseous remodeling secondary to the overlying soft-tissue constriction band.
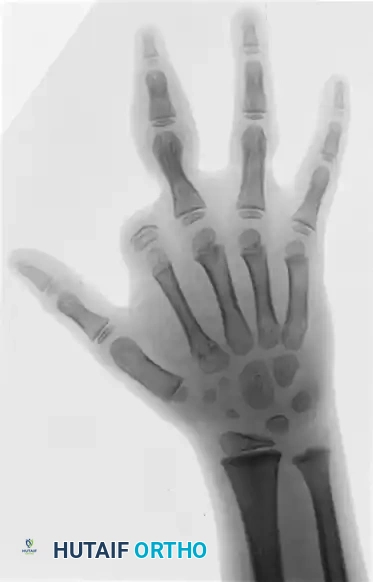
Radiograph illustrating multiple intrauterine amputations (Patterson Type 4) across the digits, with varying levels of phalangeal absence.
Surgical Indications and Timing
The timing of surgical intervention is dictated entirely by the vascular status of the limb or digit:
1. Emergent (Neonatal period): Indicated for deep bands causing acute vascular compromise, cyanosis, or impending necrosis. Immediate release of the band is required to salvage the digit.
2. Urgent/Early (3 to 6 months of age): Indicated for deep bands causing progressive lymphedema without acute ischemia. Early intervention prevents irreversible fibrotic changes in the edematous tissue.
3. Elective (12 to 18 months of age): Indicated for simple, superficial rings (Type 1) causing cosmetic deformity, or for the reconstruction of acrosyndactyly and amputations.
Surgical Warning: Never perform a circumferential excision of a constriction band in a single stage. Circumferential excision disrupts the remaining tenuous superficial venous and lymphatic drainage, risking catastrophic distal necrosis. Always stage the release, addressing 50% of the circumference at a time, separated by 2 to 3 months.
Surgical Techniques
1. Excision and Z-Plasty for Constriction Bands
The gold standard for treating simple and deep constriction rings is the complete excision of the fibrotic band followed by multiple Z-plasties or W-plasties to lengthen the scar and prevent recurrent circumferential contracture.
Step-by-Step Approach:
* Marking: Design multiple Z-plasties along the course of the band. The central limb of the Z-plasty lies within the groove of the band. The limbs should be designed at 60-degree angles to provide optimal lengthening (approximately 73% theoretical length increase) and reorientation of the scar.
* Incision and Excision: Incise along the markings. Meticulously excise the dense, avascular fibrous tissue comprising the band. This tissue often extends down to the deep fascia or even the periosteum.
* Tissue Handling: Preserve all identifiable superficial veins and lymphatic channels. The underlying neurovascular bundles are usually intact but may be displaced or compressed; dissect them free with loupe magnification.
* Flap Transposition: Elevate the triangular flaps as full-thickness skin and subcutaneous flaps. Transpose the flaps to break up the linear constriction.
* Closure: Close the flaps with fine absorbable sutures (e.g., 5-0 or 6-0 chromic gut or fast-absorbing plain gut) to avoid the need for suture removal in a pediatric patient.
Intraoperative photograph showing the precise markings for staged multiple Z-plasties on a digit with a deep constriction band and distal lymphedema.
2. Acrosyndactyly Release
Acrosyndactyly requires careful separation of the distally fused digits. Unlike simple syndactyly, the proximal web space is often partially formed (fenestrated).
* The distal fusion is sharply divided.
* The proximal epithelialized sinus tracts are excised.
* The web space is reconstructed using standard dorsal and volar triangular or rectangular flaps, supplemented by full-thickness skin grafts (usually harvested from the groin) to cover the lateral digital defects.
3. Reconstruction of Intrauterine Amputations: Non-Vascularized Toe Phalanx Transfer
For children presenting with Patterson Type 4 intrauterine amputations, restoring digital length and providing a stable post for pinch is critical for hand function. A non-vascularized toe phalanx transfer is a highly effective technique for reconstructing absent metacarpals or proximal phalanges, particularly when performed in children under 18 months of age, as the transferred phalanx retains significant growth potential.
Surgical Technique for Phalangeal Transfer:
-
Recipient Site Preparation:
- Make a dorsal or mid-lateral incision over the stump of the amputated digit.
- Carefully dissect the soft tissues to create a recipient pouch. Identify and mobilize the remnant flexor and extensor tendons, as well as the digital nerves.
- Expose the distal end of the recipient bone (e.g., the metacarpal head or remnant proximal phalanx). Prepare the bony surface to ensure a flat, bleeding cancellous bed for optimal osteointegration.
-
Donor Site Harvest (Toe):
- The middle phalanx of the third or fourth toe is typically selected to minimize donor site morbidity.
- Make a dorsal longitudinal incision over the selected toe.
- Harvest the phalanx. Crucial Step: The phalanx must be harvested extra-periosteally if the goal is to allow the donor toe to regenerate bone, or with its periosteum intact if maximum growth of the transfer is desired.
-
Transfer and Fixation:
- Introduce a smooth Kirschner wire (K-wire) into the harvested toe phalanx.
- Pass the K-wire in a retrograde manner into the recipient metacarpal (or proximal stump). Surgical Pearl: Ensure the K-wire is passed centrally so that the delicate skin of the recipient pouch is not compromised or placed under undue tension by the pin.
- Align the volar plate and collateral ligament structures of the transferred toe phalanx in a nearly anatomical position over the recipient metacarpal head.
- Because of their secured position with the K-wire, the volar plate and collateral ligaments can be sutured directly to the adjacent soft tissue of the hand, or left to heal to the adjacent tissue bed.
- Center the flexor tendon over the transferred phalanx by suturing it securely to the periosteum or remnant fibrous tissue to provide future dynamic stability.
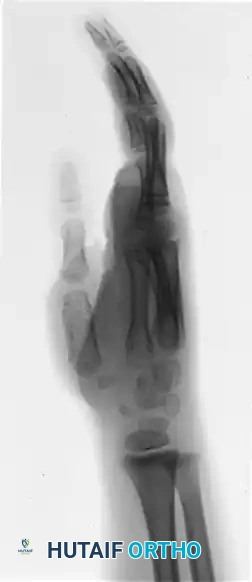
Postoperative radiograph demonstrating the integration of a non-vascularized toe phalanx transfer fixed with a longitudinal Kirschner wire to restore digital length.
- Donor Site Closure:
- Fix the donor toe with a longitudinal K-wire, holding the remaining distal phalanx at an appropriate distance from the metatarsal head to maintain toe length and alignment while the periosteal sleeve regenerates bone.
- Close the skin primarily.
Postoperative Care and Rehabilitation
Meticulous postoperative care is essential for the success of both soft tissue releases and bony reconstructions in congenital ring syndrome.
- Immobilization: Following Z-plasties or phalangeal transfers, the hand is immobilized in a bulky, well-padded long-arm cast. The elbow is flexed to 90 degrees to prevent the cast from slipping off the infant's arm.
- Pin Management: For phalangeal transfers, the K-wires in both the hand and the donor foot are typically left in place for 6 weeks.
- Pin Removal and Therapy: At the 6-week mark, the pins are removed in the clinic. The child is immediately encouraged to actively flex and extend the digits of both the hand and the foot. Formal occupational therapy may be initiated to encourage integration of the reconstructed digits into gross and fine motor play.
- Monitoring: Long-term follow-up is required to monitor the growth of the transferred phalanx, assess for any recurrence of constriction bands (which is rare if completely excised), and evaluate the resolution of lymphedema.
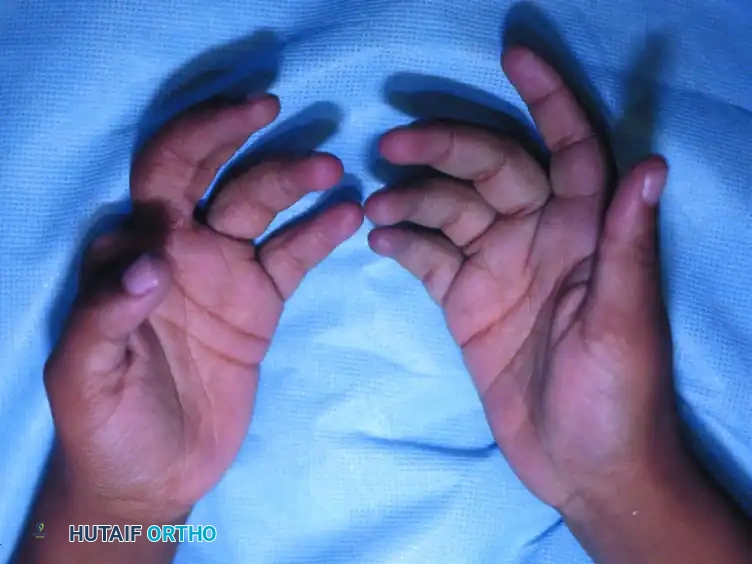
Volar view of the hands at 2 years' follow-up. The lymphedema has completely resolved following staged Z-plasties, and the patient demonstrates excellent active flexion and extension of the reconstructed digits.
Complications and Pitfalls
- Vascular Compromise: The most devastating complication is distal ischemia following a single-stage circumferential release. Always stage the procedure.
- Persistent Lymphedema: Incomplete excision of the deep fibrotic band will result in failure to resolve the distal lymphedema. The band must be excised down to healthy, unscarred tissue.
- Pin Tract Infection: Meticulous pin care is required for phalangeal transfers. Superficial infections usually respond to oral antibiotics, but deep infections may necessitate premature pin removal, risking non-union or malalignment of the transfer.
- Growth Arrest: In non-vascularized transfers, the phalanx may undergo partial resorption or fail to grow at the same rate as the contralateral digits, potentially requiring secondary lengthening procedures later in childhood.
📚 Medical References
You Might Also Like