Mastering Juvenile Bunion Correction: A Mitchell Osteotomy Intraoperative Guide
Key Takeaway
This masterclass guides fellows through the Mitchell Bunionectomy for juvenile hallux valgus. We cover essential anatomy, detailed preoperative planning, and precise intraoperative steps from incision to fixation. Emphasis is placed on protecting neurovascular structures, achieving accurate bone cuts, and preventing complications like avascular necrosis. Learn critical pearls, pitfalls, and comprehensive postoperative management to ensure optimal patient outcomes in pediatric foot surgery.
Comprehensive Introduction and Patho-Epidemiology
Juvenile hallux valgus (JHV) represents one of the most challenging deformities encountered by the orthopedic foot and ankle surgeon. Unlike adult-acquired hallux valgus, which is frequently driven by degenerative changes, footwear choices, and progressive ligamentous attenuation, the juvenile variant is fundamentally a structural and biomechanical anomaly rooted in genetic predisposition. The management of this condition requires a profound understanding of the growing foot, as the presence of open physes dictates our surgical algorithms and limits our armamentarium. The Mitchell osteotomy, particularly with modern modifications, remains a powerful distal metatarsal osteotomy for correcting moderate deformities in the skeletally immature patient, specifically designed to bypass the proximal physis while achieving multiplanar correction.
The patho-epidemiology of juvenile hallux valgus is heavily skewed toward a familial inheritance pattern, with maternal transmission being the most frequently documented etiology. Studies indicate that up to 70% to 90% of adolescent patients presenting with symptomatic hallux valgus have a positive family history. The deformity is characterized by a complex interplay of anatomical variants, most notably metatarsus primus varus (an increased intermetatarsal angle), an oblique medial cuneiform-first metatarsal articulation, and hypermobility of the first ray. Furthermore, the juvenile bunion is rarely associated with degenerative joint disease at the first metatarsophalangeal (MTP) joint, a stark contrast to the adult population. Instead, the primary complaints are pain over the medial eminence, difficulty with shoe wear, and cosmetic concerns that can significantly impact the psychosocial well-being of the adolescent patient.
Understanding the biomechanical derangement is critical for executing a successful correction. As the first metatarsal drifts into varus, the hallux is driven into valgus by the extrinsic forces of the shoe and the altered mechanical vectors of the intrinsic musculature. The adductor hallucis becomes a primary deforming force, tethering the proximal phalanx laterally and exacerbating the lateral subluxation of the sesamoid apparatus. Concurrently, the abductor hallucis slips plantar-laterally, losing its ability to stabilize the medial joint space and instead acting as an intrinsic pronator of the great toe. This dynamic imbalance creates a vicious cycle of progressive deformity that conservative measures—such as wide toe-box shoes and orthotics—can only accommodate, but never correct.
Surgical intervention in this demographic is not merely about cosmesis; it is a profound reconstructive effort to restore the intricate biomechanics of the first ray, prevent early-onset osteoarthritis, and improve the patient's functional capacity. The Mitchell osteotomy, a distal step-cut osteotomy, is particularly advantageous in this context. By performing the osteotomy at the distal metaphyseal-diaphyseal junction, the surgeon safely avoids the proximal physis of the first metatarsal. The step-cut design provides inherent stability against dorsal displacement, while allowing for lateral translation to correct the intermetatarsal angle and plantar translation to compensate for the inevitable shortening of the metatarsal, thereby mitigating the risk of postoperative transfer metatarsalgia.
Detailed Surgical Anatomy and Biomechanics
Mastery of the first ray anatomy is the absolute prerequisite for safe and effective execution of the Mitchell osteotomy. The first ray is not an isolated osseous structure but a highly coordinated functional unit comprising the first metatarsal, the medial cuneiform, the proximal and distal phalanges, and a complex network of capsuloligamentous and musculotendinous stabilizers. In the juvenile patient, the osteology is uniquely defined by the presence of growth plates. The physis of the first metatarsal is located proximally, whereas the physes of the lesser metatarsals are distal. Similarly, the physis of the proximal phalanx is located at its base. This anatomical reality strictly contraindicates proximal osteotomies (such as the Lapidus or proximal crescentic osteotomies) in patients with significant remaining growth, as iatrogenic physeal arrest can lead to devastating shortening and secondary deformities.
The soft tissue envelope surrounding the first MTP joint undergoes predictable pathological changes in the presence of hallux valgus. Medially, the joint capsule and the medial collateral ligament become chronically attenuated and redundant, failing to resist the lateral drift of the hallux. Laterally, the soft tissues become severely contracted. The adductor hallucis tendon, inserting on the lateral base of the proximal phalanx and the fibular sesamoid, exerts an unopposed lateral pull. The sesamoid complex, deeply embedded within the tendons of the flexor hallucis brevis, subluxates laterally beneath the metatarsal head. This lateral shift of the sesamoids displaces the flexor hallucis longus and extensor hallucis longus tendons laterally, transforming these powerful stabilizers into active bowstrings that further drive the hallux into valgus and pronation.
Neurovascular preservation is a paramount concern during the surgical approach. The dorsal medial sensory nerve, a terminal branch of the superficial peroneal nerve, courses superficially across the dorsomedial aspect of the first MTP joint. It provides critical sensory innervation to the medial aspect of the hallux. Iatrogenic injury to this nerve during the initial incision or subsequent retraction is a notorious complication, resulting in painful neuromas, paresthesias, or localized anesthesia that can overshadow an otherwise perfect osseous correction. The surgeon must employ meticulous blunt dissection in the subcutaneous plane to identify and mobilize this nerve out of the surgical field.
Equally critical is the vascular supply to the first metatarsal head, which is notoriously precarious. The primary arterial perfusion arises from an extracapsular arterial ring supplied by the first dorsal metatarsal artery and the first plantar metatarsal artery. Crucially, the majority of the blood supply enters the metatarsal head via the lateral and plantar-lateral capsular attachments. Extensive lateral soft tissue stripping, particularly when combined with an intracapsular distal osteotomy, severely compromises this vascular network, precipitating avascular necrosis (AVN) of the metatarsal head. The Mitchell osteotomy mitigates this risk by relying on indirect lateral release (via the lateral translation of the capital fragment) rather than aggressive direct lateral capsular stripping, thereby preserving the vital lateral vascular tether.
Exhaustive Indications and Contraindications
Patient selection is the cornerstone of successful juvenile bunion surgery. Not all adolescent bunions require, or will benefit from, surgical intervention. The decision to operate must be predicated on a thorough clinical evaluation, radiographic analysis, and a deep understanding of the patient's skeletal maturity and functional demands. The classical presentation involves a highly active adolescent—often female, between the ages of 12 and 16—complaining of intractable pain over the medial eminence that limits participation in sports and dictates footwear modifications.
The primary indication for a Mitchell osteotomy in this population is a symptomatic, moderate hallux valgus deformity (Intermetatarsal Angle [IMA] between 12 and 18 degrees, and a Hallux Valgus Angle [HVA] between 25 and 40 degrees) in a patient with an open proximal first metatarsal physis. The pain must be localized to the MTP joint or the medial eminence and must have proven refractory to a dedicated trial of conservative management, including shoe wear modification, orthoses, and activity modification. Furthermore, the patient must demonstrate a congruent or subluxated MTP joint without evidence of severe degenerative changes, which are exceedingly rare in this age group but must be ruled out.
Contraindications must be rigorously respected to avoid catastrophic failures and high recurrence rates. Absolute contraindications include asymptomatic deformities, regardless of their radiographic severity. Operating on a painless juvenile bunion for purely cosmetic reasons is strongly discouraged due to the inherent risks of surgery and the high propensity for recurrence in the growing foot. Severe deformities (IMA > 20 degrees) typically exceed the corrective capacity of a distal osteotomy and may require delaying surgery until skeletal maturity allows for a proximal or diaphyseal procedure.
Furthermore, patients with underlying neuromuscular disorders (e.g., cerebral palsy, Charcot-Marie-Tooth disease) or generalized ligamentous laxity (e.g., Marfan syndrome, Ehlers-Danlos syndrome) represent poor candidates for isolated distal osteotomies. In these populations, the deforming forces are systemic and persistent, leading to almost guaranteed recurrence unless arthrodesis or more extensive soft tissue balancing is performed.
| Category | Indications for Mitchell Osteotomy | Contraindications for Mitchell Osteotomy |
|---|---|---|
| Clinical | Symptomatic pain over medial eminence | Asymptomatic deformity (cosmetic only) |
| Conservative Care | Failure of >6 months non-operative treatment | Inadequate trial of conservative management |
| Radiographic | Moderate deformity (IMA 12°-18°, HVA 25°-40°) | Severe deformity (IMA > 20°, HVA > 40°) |
| Skeletal Status | Open proximal first metatarsal physis | Closed physes (proximal procedures preferred) |
| Joint Status | Congruent or mildly subluxated MTP joint | Degenerative joint disease (Hallux rigidus) |
| Systemic | Normal neuromuscular tone | Spasticity, neuromuscular disease, hyperlaxity |
Pre-Operative Planning, Templating, and Patient Positioning
Thorough preoperative planning is the blueprint for intraoperative success. This begins with obtaining high-quality, weight-bearing radiographs of the foot, including anteroposterior (AP), lateral, and oblique views. Non-weight-bearing films are virtually useless for assessing the true magnitude of a dynamic forefoot deformity. On the AP radiograph, the surgeon must meticulously measure the Intermetatarsal Angle (IMA), the Hallux Valgus Angle (HVA), and the Distal Metatarsal Articular Angle (DMAA). The DMAA is particularly critical in juvenile bunions, as an increased angle indicates an abnormal, laterally directed orientation of the articular cartilage. If the DMAA is significantly elevated, a simple translation osteotomy may not suffice, and a biplanar osteotomy incorporating a medial closing wedge may be required to render the articular surface perpendicular to the mechanical axis of the first ray.
Templating the osteotomy on digital or physical radiographs allows the surgeon to anticipate the exact location of the bone cuts and the required magnitude of lateral translation. The Mitchell osteotomy is inherently a shortening procedure due to the resection of bone required to create the step-cut and the width of the saw blade. Therefore, the surgeon must calculate the anticipated shortening and plan for concomitant plantar translation of the capital fragment to maintain the weight-bearing capacity of the first metatarsal head. Failure to template and execute this plantarflexion will inevitably transfer the biomechanical load to the lesser metatarsals, resulting in intractable postoperative transfer metatarsalgia.
Patient positioning and operating room setup must be standardized to ensure efficiency and optimal visualization. The patient is placed supine on the operating table. A bump may be placed under the ipsilateral hip to internally rotate the leg, bringing the foot into a perfectly neutral position, pointing straight toward the ceiling. This neutral alignment is vital for accurately assessing the rotational alignment of the hallux intraoperatively. A well-padded pneumatic tourniquet is applied to the proximal thigh or calf to provide a bloodless surgical field, which is essential for identifying fine neurovascular structures and executing precise osseous cuts.
Fluoroscopy is an indispensable tool during this procedure. The C-arm should be positioned on the contralateral side of the patient, draped sterilely, and brought into the field to confirm the starting point of the osteotomy relative to the physis and the articular surface. Before making the skin incision, the surgeon must ensure that both true AP and lateral fluoroscopic views can be obtained effortlessly without compromising the sterile field. A prophylactic intravenous antibiotic, typically a first-generation cephalosporin, is administered within one hour prior to tourniquet inflation.
Step-by-Step Surgical Approach and Fixation Technique
The surgical approach begins with a meticulously planned dorsomedial incision. Starting just distal to the first MTP joint, the incision extends proximally for approximately 5 to 6 centimeters, curving gently to follow Langer's lines over the medial aspect of the first metatarsal shaft. Immediately upon breaching the dermis, the surgeon must transition to blunt dissection. The dorsal medial sensory nerve is highly vulnerable in this superficial layer. Using Metzenbaum scissors or a hemostat, the subcutaneous tissues are gently spread to identify the nerve. Once isolated, it is carefully mobilized and retracted dorsally using a vessel loop, ensuring it remains protected throughout the entirety of the procedure.
Following nerve protection, attention is turned to the joint capsule. A distally based Y-shaped capsuloperiosteal incision is employed. The longitudinal stem of the "Y" is centered over the medial metatarsal shaft, while the diverging arms extend distally toward the dorsal and plantar margins of the MTP joint. This specific geometry creates a robust, distally based flap that provides excellent exposure of the medial eminence and will later be utilized for a strong medial capsulorrhaphy. A periosteal elevator is used to sharply reflect the capsule, exposing the hypertrophic medial eminence and the articular surface of the metatarsal head.
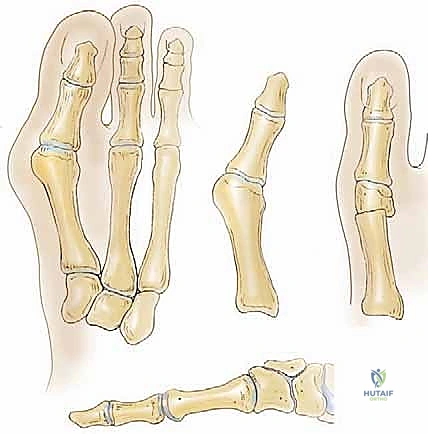
The first osseous maneuver is the resection of the medial eminence. Utilizing an oscillating saw, the cut is initiated at the sagittal groove (the groove of Clark)—the demarcation between the articular cartilage and the exostosis. The saw blade is directed proximally and slightly medially, perfectly parallel to the medial border of the foot. It is a critical pitfall to angle this cut laterally, as doing so will inadvertently resect a portion of the functional articular surface, narrowing the metatarsal head and compromising joint congruency. The resected bone is removed, and the raw cancellous surface is smoothed with a rasp.
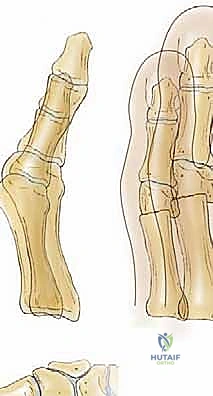
The defining feature of the Mitchell procedure is the double step-cut osteotomy. The first cut is made at the distal metaphyseal-diaphyseal junction, safely distal to the proximal physis. This cut is oriented perpendicular to the longitudinal axis of the metatarsal. Crucially, this is an incomplete cut; the saw blade penetrates only the medial two-thirds of the metatarsal shaft, intentionally leaving the lateral one-third of the cortex intact.
The second cut is made parallel to, and approximately 3 to 5 millimeters proximal to, the first cut. This second cut is complete, passing entirely through the medial, central, and lateral cortices of the metatarsal shaft. The bone segment between these two cuts is carefully excised. This creates a proximal metatarsal shaft with a lateral cortical "step" or "beak," and a free distal capital fragment.

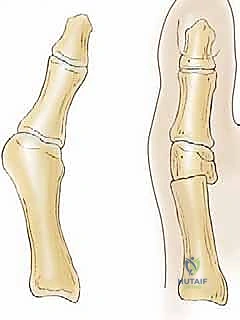
The capital fragment is then manually translated laterally. The lateral step of the proximal shaft acts as a physical buttress, preventing the capital fragment from displacing medially and providing profound intrinsic stability against dorsal migration. Concurrently, the capital fragment must be manually displaced plantarly by 2 to 3 millimeters to compensate for the longitudinal shortening caused by the bone resection. This lateral and plantar translation corrects the metatarsus primus varus and restores the weight-bearing mechanics of the first ray.
Fixation is achieved while holding the capital fragment in its newly corrected position. Traditionally, heavy non-absorbable sutures were passed through drill holes, but modern techniques favor rigid fixation. Two smooth Kirschner wires (typically 0.062 inch) or a single cannulated compression screw can be directed from the dorsal-proximal metatarsal shaft, across the osteotomy site, and into the plantar-distal capital fragment.
Once rigid fixation is confirmed fluoroscopically, the medial capsulorrhaphy is performed. The distally based Y-flap is advanced proximally and sutured under tension to the periosteum of the metatarsal shaft with the hallux held in neutral alignment. This imbrication eliminates medial laxity and reinforces the correction. The skin is closed in layers, and a bulky, compressive soft dressing is applied to hold the toe in the corrected position.
Complications, Incidence Rates, and Salvage Management
Despite meticulous surgical technique, the Mitchell osteotomy carries a distinct profile of potential complications, particularly in the demanding juvenile population. The most devastating complication is avascular necrosis (AVN) of the first metatarsal head. Because the osteotomy is performed in the distal metaphysis, and the primary blood supply enters laterally, excessive lateral soft tissue stripping or aggressive lateral capsular release can completely devascularize the capital fragment. The incidence of AVN is reported to be between 1% and 3%. Management of AVN ranges from prolonged non-weight-bearing in early stages to joint-destructive procedures, such as MTP arthrodesis, if severe collapse and secondary arthritis occur.
Recurrence of the hallux valgus deformity is the most frequent complication in juvenile patients, with literature citing recurrence rates as high as 30% to 40% when surgery is performed prior to skeletal maturity. Recurrence is driven by continued physeal growth, failure to adequately correct a high DMAA, or underlying hypermobility that was not addressed. Salvage for symptomatic recurrence usually necessitates waiting until skeletal maturity and performing a more powerful proximal procedure, such as a Lapidus arthrodesis or a proximal crescentic osteotomy, to definitively stabilize the first ray.
Transfer metatarsalgia is a direct mechanical consequence of first metatarsal shortening without adequate plantar translation. The Mitchell osteotomy inherently shortens the first ray by 3 to 5 millimeters. If the capital fragment is allowed to heal in a dorsiflexed position, or if it is not translated plantarly, the weight-bearing load during the push-off phase of gait is transferred to the second and third metatarsal heads. This results in intractable plantar pain and hyperkeratotic lesions. Salvage management begins with custom orthotics featuring a metatarsal pad; however, refractory cases may require a Weil osteotomy of the lesser metatarsals or a corrective plantarflexion osteotomy of the first metatarsal.
| Complication | Estimated Incidence | Etiology / Risk Factors | Salvage / Management Strategy |
|---|---|---|---|
| Avascular Necrosis (AVN) | 1% - 3% | Excessive lateral soft tissue stripping; disruption of lateral vascular tether | NWB for early stages; MTP Arthrodesis for late collapse |
| Recurrence of Deformity | 15% - 40% | Continued physeal growth; unaddressed hypermobility; undercorrection | Delay until skeletal maturity, then Lapidus or proximal osteotomy |
| Transfer Metatarsalgia | 5% - 15% | Excessive shortening; dorsal elevation of capital fragment | Custom orthotics; Weil osteotomies of lesser metatarsals |
| Hallux Varus (Overcorrection) | 2% - 5% | Excessive lateral translation; over-tightening of medial capsule | Soft tissue release; Extensor hallucis brevis transfer; Arthrodesis |
| Nerve Injury (Neuroma) | 3% - 7% | Iatrogenic transection or traction of dorsal medial sensory nerve | Gabapentinoids; targeted injections; surgical excision and burying |
Phased Post-Operative Rehabilitation Protocols
The postoperative rehabilitation following a Mitchell osteotomy is a carefully orchestrated process designed to protect the osseous healing while preventing debilitating stiffness of the first MTP joint. The protocol is divided into four distinct phases, heavily dependent on radiographic evidence of consolidation and the patient's clinical progression. Patient compliance in the juvenile population is notoriously variable, making thorough preoperative counseling regarding the postoperative restrictions absolutely essential.
Phase 1: Maximum Protection (Weeks 0 to 2)
Immediately following surgery, the patient is placed in a bulky, compressive dressing and a rigid postoperative shoe or a controlled ankle motion (CAM) boot. The primary goal during this phase is to control edema, manage pain, and protect the osteotomy site. The patient is strictly instructed to remain non-weight-bearing or heel-weight-bearing only, utilizing crutches or a knee scooter. Elevation of the operative extremity above the level of the heart is critical to minimize swelling, which can compromise wound healing. At the two-week mark, the patient returns to the clinic for suture removal and the first postoperative radiographic assessment to confirm the maintenance of fixation and alignment.
Phase 2: Protected Weight-Bearing and Early Motion (Weeks 2 to 6)
If the two-week radiographs demonstrate stable alignment without displacement, the patient transitions to progressive weight-bearing in the rigid postoperative shoe. The rigid sole is crucial, as it prevents dorsiflexion of the forefoot, thereby neutralizing the bending moments across the osteotomy site. If Kirschner wires were used for fixation and left protruding through the skin, they are typically removed in the clinic between 4 and 6 weeks postoperatively. During this phase, gentle, passive range of motion (ROM) exercises of the first MTP joint are initiated. The surgeon or physical therapist instructs the patient to manually dorsiflex and plantarflex the hallux to prevent capsular adhesions, taking care not to force the motion beyond the onset of pain.
Phase 3: Restoring Function and Strength (Weeks 6 to 12)
At the six-week mark, new radiographs are obtained. If clinical and radiographic evidence of robust callus formation and osseous union is present, the patient is transitioned out of the rigid shoe and into a supportive, wide-toebox athletic shoe. Physical therapy becomes more aggressive during this phase. Active and active-assisted ROM exercises are emphasized to restore the critical windlass mechanism of the foot. Strengthening exercises targeting the intrinsic foot musculature, particularly the flexor hallucis brevis and the abductor hallucis, are implemented. Gait training is initiated to correct any compensatory movement patterns developed during the period of restricted weight-bearing.
Phase 4: Return to High-Impact Activity (Months 3 to 6)
The final phase focuses on returning the adolescent athlete to their baseline level of activity. By 12 weeks, the osteotomy should be fully consolidated. Patients are cleared to begin low-impact cardiovascular exercises, such as stationary cycling and swimming. Progression to high-impact activities, including running, jumping, and cutting sports, is allowed gradually between 3 and 6 months postoperatively, contingent upon the complete resolution of pain, full restoration of MTP joint motion, and symmetrical lower extremity strength. The patient is strongly advised to continue wearing supportive footwear and to avoid narrow, restrictive shoes to minimize the extrinsic forces that could contribute to recurrence.
Summary of Landmark Literature and Clinical Guidelines
The evolution of the Mitchell osteotomy is deeply rooted in the historical literature of orthopedic foot and ankle surgery. Originally described by C.L. Mitchell and colleagues in 1958, the procedure was designed as a distal metatarsal osteotomy specifically aimed at correcting hallux valgus while preserving the MTP joint. Mitchell's original description elegantly detailed the double step-cut technique, emphasizing the importance of the lateral cortical hinge to provide stability and the lateral displacement of the capital fragment to reduce the intermetatarsal angle. This seminal paper established the foundation for distal osteotomies in the treatment of mild to moderate bunion deformities.
Over the decades, the procedure has undergone several critical modifications to address its inherent complications, most notably transfer metatarsalgia. Hawkins and colleagues highlighted the biomechanical necessity of plantarflexing the capital fragment to compensate for the inevitable shortening caused by the bone resection. Later, Stevens introduced modifications to the fixation techniques, advocating for more rigid internal fixation to prevent dorsal malunion, which was a frequent cause of failure in early iterations of the procedure. These modifications transformed the Mitchell osteotomy from a procedure with unpredictable outcomes into a highly reliable tool in the surgeon's armamentarium.
In the context of juvenile hallux valgus, the literature is dominated by the work of Coughlin and others, who have extensively documented the high recurrence rates associated with surgical intervention in the skeletally immature foot. Coughlin's long-term follow-up studies demonstrated that while distal osteotomies like the Mitchell can provide excellent short-term correction, the persistence of underlying hypermobility and continued physeal growth often lead to recurrence of the deformity. Consequently, modern clinical guidelines strongly advocate for delaying surgical intervention in juvenile bunions until the patient is at or near skeletal maturity, whenever clinically feasible.
Current consensus dictates that the Mitchell osteotomy remains a highly effective, albeit technically demanding, procedure for the adolescent patient with an open proximal physis, moderate deformity, and intractable pain. However, the surgeon must approach this procedure with a profound respect for the complex pathoanatomy, a meticulous surgical technique to preserve vascularity, and a clear understanding of the biomechanical imperatives of the first ray. Only through rigorous adherence to these principles can the orthopedic surgeon hope to master the juvenile bunion correction and achieve lasting, functional outcomes for this challenging patient population.
