Scarf Osteotomy Masterclass: Precision Correction of Hallux Valgus
Key Takeaway
This masterclass guides fellows through the Scarf osteotomy for hallux valgus, detailing comprehensive surgical anatomy, meticulous preoperative planning, and precise intraoperative execution. We cover every micro-step, from incision to hardware fixation, emphasizing neurovascular protection, optimal osteotomy cuts, and fragment displacement. Critical pearls and pitfalls are highlighted, alongside comprehensive postoperative rehabilitation, ensuring a thorough understanding of this versatile procedure.
Welcome, fellows, to the operating theater. Today, we're tackling a symptomatic hallux valgus deformity with a Scarf osteotomy – a truly versatile and powerful technique for first metatarsal correction. This isn't just about moving bone; it's about restoring biomechanics, alleviating pain, and achieving a lasting cosmetic outcome for our patients.
Preoperative Planning: The Blueprint for Success
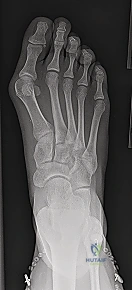
Before we even consider making an incision, our blueprint for this procedure begins with meticulous preoperative planning. We've thoroughly evaluated the patient's weight-bearing anteroposterior (AP) and lateral radiographs of the foot. These images are critical for assessing several key parameters:
- Intermetatarsal Angle (IMA): The primary indication for a Scarf osteotomy is typically a symptomatic hallux valgus with an IMA of less than 20 degrees. We're looking for a stable first metatarsocuneiform joint here; instability might push us towards a fusion.
- Hallux Valgus Angle (HVA): This measures the lateral deviation of the great toe.
- Distal Metatarsal Articular Angle (DMAA): This assesses the orientation of the articular surface of the first metatarsal head. An abnormal DMAA, especially in juvenile hallux valgus, can be corrected effectively with a Scarf.
- Interphalangeal Angle (IPA): If this angle is significantly elevated, it may indicate the need for a concurrent proximal phalangeal osteotomy, such as an Akin osteotomy, to achieve complete correction. We've templated for this possibility.
- Metatarsal Length: We assess for any relative shortening or lengthening that might be required. The Scarf is unique in its ability to allow for shortening, lengthening, rotation, displacement, or even plantarization of the first metatarsal head.
- Joint Congruency: We note the congruency of the first metatarsophalangeal (MTP) joint. While the Scarf is excellent for arthritic hallux valgus not severe enough for a fusion, severe incongruity or advanced arthritis might warrant a different approach.
- Osteophytes: Presence and size of any dorsal or medial osteophytes.
- Medial Eminence: The size of the bony medial eminence, or "bunion," which we will resect.
- Sesamoid Position: The position and condition of the sesamoids under the first metatarsal head. Lateral subluxation is a hallmark of hallux valgus, and their reduction is a key indicator of successful correction.
Today's patient presents with symptomatic hallux valgus, an IMA of 16 degrees, and moderate lateral sesamoid subluxation, making the Scarf osteotomy an ideal choice.
Patient Positioning and Anesthesia
Our patient is positioned supine on the operating table. Crucially, we've placed a sandbag under the ipsilateral buttock. This maneuver internally rotates the hip, ensuring the big toe points directly to the ceiling, providing optimal exposure and alignment for our surgical approach. A thigh tourniquet has been applied high on the thigh, ensuring a bloodless field once inflated. We've also administered prophylactic antibiotics, as per our protocol, to minimize the risk of infection. The foot and ankle are prepped and draped in a sterile fashion, ensuring we have full access to the surgical site and enough room for fluoroscopy.
Surgical Anatomy: Navigating the First Ray
Before we make our incision, let's quickly review the critical anatomy of the first ray.
* Bony Anatomy: We're working on the first metatarsal, extending from its base at the tarsometatarsal (TMT) joint to its head, which articulates with the proximal phalanx. The medial eminence is our primary target for resection.
* Neurovascular Structures:
* Dorsal Medial Cutaneous Nerve: This sensory nerve, a branch of the superficial fibular nerve, runs superficially along the dorsomedial aspect of the foot. It is highly susceptible to injury during skin incision and capsular dissection. We must identify and protect it.
* Plantar Neck Vascular Bundle: This crucial blood supply to the metatarsal head enters the metatarsal neck plantarly. Aggressive plantar dissection or careless retraction can compromise this vascularity, leading to avascular necrosis of the metatarsal head – a devastating complication.
* Muscular Intervals: We'll be working through the subcutaneous tissue and then incising the medial capsule. Later, during the lateral release, we'll address the adductor hallucis muscle's tendinous insertion.
* Ligamentous Structures: The medial collateral ligament of the MTP joint, the lateral collateral ligament, and the suspensory metatarsal-sesamoid ligaments are key stabilizers that contribute to the deformity and will be addressed.
Intraoperative Execution: The Scarf Osteotomy Masterclass
Alright, fellows, let's begin. Scalpel, please.
1. Soft Tissue Release and Bunionectomy
Our first step is to gain meticulous exposure and perform the necessary soft tissue releases.
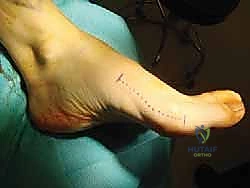
a. Medial Longitudinal Incision:
We begin with a medial longitudinal incision. This incision extends precisely from the palpable first tarsometatarsal (TMT) joint proximally, distally along the medial flare of the first metatarsal, to the medial aspect of the proximal phalanx.

This length is crucial. If we anticipate a concomitant proximal phalangeal osteotomy, such as an Akin, we can extend this incision slightly more distally.
As we deepen the incision through the skin and subcutaneous tissue, be acutely aware of the dorsal medial cutaneous nerve. Use blunt dissection with Metzenbaum scissors to carefully identify and retract this nerve dorsally and protect it throughout the procedure. Any direct trauma or excessive traction can lead to postoperative neuroma or paresthesia.
b. Medial Capsular Incision and Bunionectomy:
Once the nerve is protected, we sharply incise the medial capsule in a single, longitudinal direction. This provides excellent exposure of the medial eminence of the first metatarsal head.
Now, using an oscillating saw, we will resect the medial eminence. The key here is precision: resect it 1 mm medial to the sagittal sulcus.
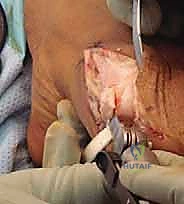
This ensures we remove the prominent bone without over-resecting, which could lead to a postoperative varus deformity of the hallux. Use a small rongeur or rasp to smooth any sharp edges after resection.
c. Metatarsal Shaft Exposure and Plantar Protection:
With the medial eminence resected, we now need to expose the first metatarsal shaft. We achieve this using sharp subperiosteal dissection. This means we stay directly on the bone, meticulously lifting the periosteum and soft tissues.
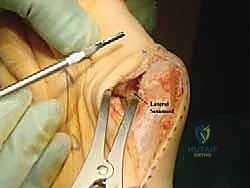
This is a critical step, fellows. As we dissect plantarly, we must take extreme care to protect the plantar neck vascular bundle to the metatarsal head. This bundle provides the primary blood supply. Aggressive dissection or careless retraction in this area can lead to avascular necrosis.
Surgical Warning: Always maintain a subperiosteal plane to shield the plantar neurovascular structures. Use gentle, broad retraction.
For proximal plantar exposure, we use a large Langenbeck retractor to gently protect and retract the plantar flap. This allows us to safely visualize the plantar aspect of the metatarsal without disrupting the crucial plantar blood supply. We identify the tarsometatarsal joint proximally, but there's no need to expose it further.
d. Lateral Release of the First MTP Joint:
Now, let's address the lateral contracture, which is a significant component of the hallux valgus deformity. We'll perform a lateral release of the first metatarsophalangeal joint using an "over the top" technique.
First, introduce a lamina spreader into the first web space. This gently opens the space, providing excellent visualization.
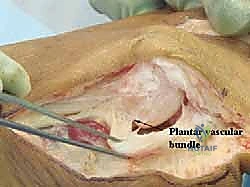
Using a banana blade, which is ideal for its curved profile, we perform sharp dissection to release the contracted structures.
Specifically, we release the tendinous insertion of the adductor hallucis muscle from the fibular sesamoid and the base of the proximal phalanx. We then release the suspensory metatarsal-sesamoid ligaments and make multiple sharp perforations in the lateral capsule at the joint line.
Once these structures are released, apply a varus force to the hallux. This maneuver helps to complete the capsular release and confirm the adequacy of our lateral soft tissue release. If the hallux still resists correction, further capsular perforations may be required.
Surgical Pearl: The "over the top" technique for lateral release is preferred as it avoids a separate incision and typically does not compromise the plantar blood supply. However, if visualization is difficult or the deformity is very severe, a separate first web space incision can be made, but this adds another potential wound.
2. The Scarf Osteotomy: Precision Bone Cuts
Now for the core of the procedure: the Scarf osteotomy itself. This is a Z-shaped osteotomy designed to allow for controlled translation, rotation, and even shortening/lengthening of the first metatarsal.
a. Medial Longitudinal Cut:
We start with the medial longitudinal cut. This cut defines the central axis of our osteotomy.
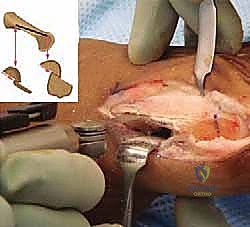
Using a small oscillating saw, begin this cut distally, approximately 5 mm from the articular surface of the metatarsal head and 2 to 3 mm from the dorsal surface of the metatarsal.
The cut then extends proximally, finishing about 5 mm from the tarsometatarsal joint and 2 to 3 mm from the proximal plantar surface of the metatarsal.
Surgical Pearl: The precise geometry of this cut is paramount. The slightly more plantar proximal endpoint allows for a degree of controlled plantarization of the metatarsal head, which can be beneficial in cases of metatarsus primus elevatus.
Crucially, make this longitudinal cut in the same plane as the plantar orientation of the metatarsal.
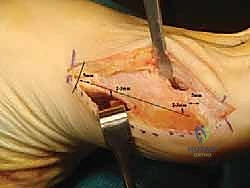
This ensures the osteotomy is stable and allows for predictable displacement. The large Langenbeck retractor, which we used earlier for plantar protection, is invaluable here to help visualize the plantar metatarsal surface and guide the saw blade accurately. Use constant irrigation to prevent thermal necrosis.
b. Transverse Cuts:
Next, we make the two transverse cuts, forming the "Z" shape. These cuts are made at approximately 60 degrees to the longitudinal cut, creating a chevron pattern.
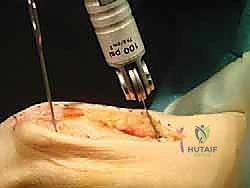
Both transverse cuts are directed proximally. It is absolutely critical to avoid convergence laterally, as this will significantly hinder the ability to translate the fragments. If the cuts converge, the distal fragment will be locked, preventing lateral displacement.
For the distal transverse cut, as you approach the lateral cortex, you'll need to elevate your hand slightly to complete the cut laterally without damaging the surrounding soft tissues.
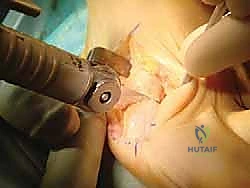
Once both transverse cuts are complete, gently separate the two bone fragments. Do not use excessive force or lever the fragments, as this can cause iatrogenic fracture. If the fragments don't separate easily, it likely means one of the cuts is incomplete. Carefully re-evaluate and repeat the necessary cut, taking care to avoid double cutting, which can shorten the osteotomy unnecessarily. If the lateral capsule is still preventing displacement, a further release from the lateral side may be required.
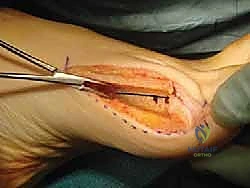
3. Fragment Displacement and Fixation
With the osteotomy complete, we now perform the desired displacement and rotation.
a. Displacement and Rotation:
Using a bone clamp, typically a small pointed reduction clamp, apply it to the distal lateral cortex of the distal fragment.
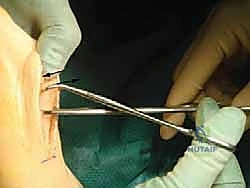
Gently but firmly, translate the distal fragment laterally, guided by our preoperative templating and the desired correction. We can achieve up to two-thirds of lateral displacement while still maintaining a strong lateral strut and excellent bone-to-bone apposition, which is crucial for stability and healing. If rotation is required to address a DMAA, this is also performed at this stage.
Once the desired position is achieved, apply a compression clamp to hold the displacement firmly in place.
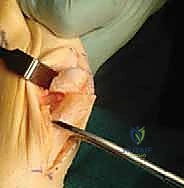
This temporary fixation is vital for precise screw placement.
b. Screw Fixation (Barouk Screws):
We typically use Barouk screws for fixation. These are cannulated, self-tapping screws designed with a long distal thread and a threaded head, which allows for excellent compression and burial of the screw head below the bone surface, minimizing soft tissue irritation.
i. Distal Screw Placement:
We always place the distal screw first.
1. Guidewire Insertion: Pass a guidewire from the proximal fragment obliquely into the metatarsal head.
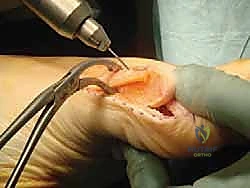
2. Intra-articular Check: It is absolutely critical to directly visualize the guidewire in the joint. We'll retract the capsule and check the articular surface.
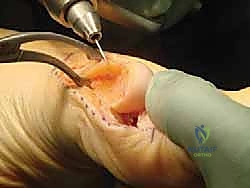
If the guidewire has penetrated the joint, withdraw it and re-insert.
3. Measurement: Once the guidewire is optimally placed, withdraw it until it is flush with the articular surface. This allows for accurate measurement of the required screw length. Our goal is a screw that is at least 4 mm less than the measured amount to avoid intra-articular penetration.
4. Drilling and Countersinking: Drill over the guidewire. Ensure the drill countersink is seated fully to create a recess for the screw head. This prevents inadvertent fracture during screw placement and ensures the head is flush.
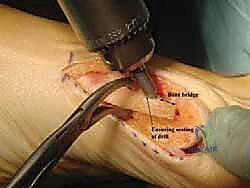
5. Screw Insertion: Insert the Barouk screw, ensuring it achieves good compression across the osteotomy site.
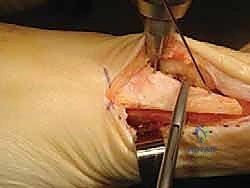
ii. Proximal Screw Placement:
Next, we place the proximal screw.
1. Guidewire Insertion: Place the second guidewire for the proximal screw in the midline, in an oblique direction, aiming to reach the plantar cortex of the distal fragment.
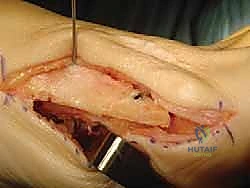
2. Plantar Visualization: Retraction of the plantar tissue, which we already performed for the longitudinal cut, is crucial here. It allows for direct visualization of the guidewire exiting the plantar cortex and ensures accurate placement.
3. Measurement: Measure the guidewire length after confirming its position. This measurement dictates the screw length.
4. Drilling and Countersinking: Drill and countersink as before.
5. Screw Insertion: Insert the proximal Barouk screw. Visually confirm good compression and accurate length, ensuring the screw head is buried and the tip is not prominent plantarly.
Surgical Pitfall: When inserting the proximal screw, be careful not to seat it too deep into the very thin dorsal cortex. This can reduce screw hold and potentially lead to dorsal cortical fracture. Aim for good purchase in the plantar cortex of the distal fragment.
4. Final Adjustments and Closure
a. Resection of Residual Medial Prominence:
After screw fixation, we often find a small residual medial bony protuberance on the medial distal aspect of the dorsal fragment.
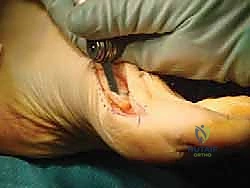
Use a small oscillating saw or rongeur to excise this, ensuring a smooth contour to prevent future soft tissue irritation or recurrence of a "bunion" appearance. Check the osteotomy for stability by gently stressing the fragments.
b. Medial Capsular Imbrication:
Now, we imbricate the medial capsule. Using a strong absorbable suture, such as a 2-0 Vicryl, we repair and tighten the medial capsule. While performing this, hold the hallux in a neutral or slightly abducted position, often with the aid of a surgical swab or gentle traction.
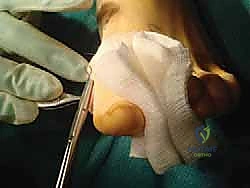
This imbrication helps to maintain the correction, reinforce the medial structures, and prevent recurrence of the valgus deformity.
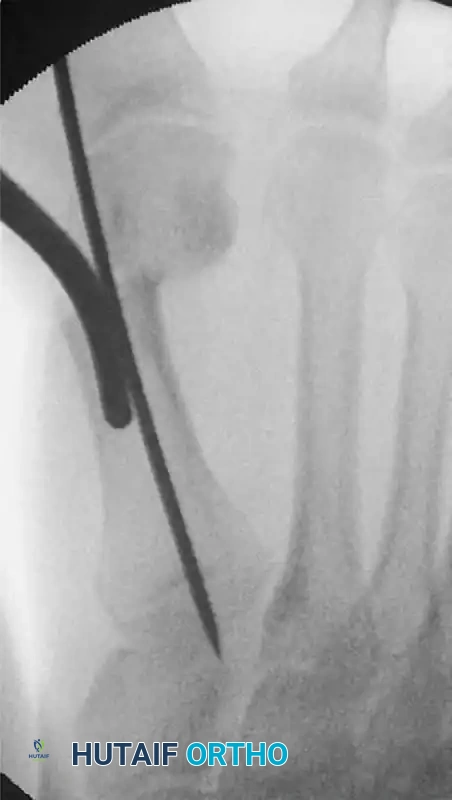
c. Final Radiographic Assessment:
Before closing, we perform a final radiographic assessment using image intensification. We take AP, oblique, and lateral views of the foot, ensuring the foot is flat on the image intensifier plate, mimicking a weight-bearing position.
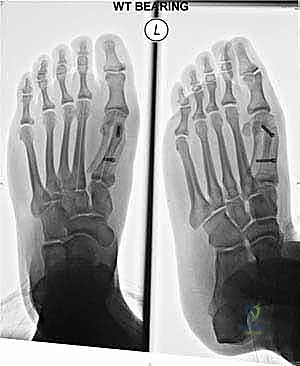
We meticulously check for:
* Reduction of the Intermetatarsal Angle (IMA): Ensure adequate correction.
* Screw Position and Length: Confirm no intra-articular penetration and good bone purchase.
* Relocation of the Sesamoids: Verify they are centered beneath the metatarsal head.
* Overall Alignment: Assess the hallux valgus angle and distal metatarsal articular angle.
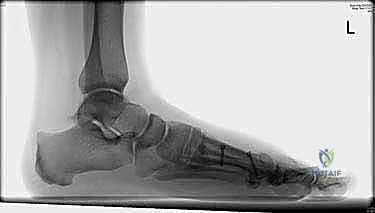
At this point, if the hallux valgus angle remains elevated despite adequate first metatarsal correction, we reassess the need for a concurrent proximal phalangeal osteotomy (Akin osteotomy). This is a distal closing wedge osteotomy of the proximal phalanx, fixed with a small staple or K-wire, to further correct the hallux position.
d. Wound Closure:
Finally, we close the wound in layers. We use a continuous absorbable suture, such as Monocryl, for the subcutaneous layer and a fine Monocryl for the skin closure. Apply a sterile dressing and a forefoot bandage, which is crucial for maintaining the achieved correction and providing gentle compression.
💡 Pearls and Pitfalls: Navigating Challenges
Throughout this procedure, there are several critical points to remember:
- Divergent Transverse Cuts: As discussed, always ensure your transverse cuts diverge laterally, or at least remain parallel. Avoid convergent transverse cuts at all costs, as this creates an hourglass effect that will make displacement impossible and can lead to iatrogenic fracture if forced.
- Rotational Osteotomy for DMAA: If you're using the Scarf to correct a significant distal metatarsal articular angle (DMAA), you may need to excise a small wedge of bone from the proximal, lateral, plantar fragment. This allows for the necessary rotational displacement without impingement onto the second metatarsal. A "shorter" Scarf osteotomy, with less longitudinal extent, can also be employed for DMAA correction.
- Longitudinal Cut Direction: Remember the versatility of the longitudinal cut. By adjusting its plantar orientation, you can achieve a degree of plantarization or dorsiflexion of the metatarsal head as required by the patient's specific biomechanics (e.g., to address metatarsus primus elevatus).
- Double Cutting Transverse Cuts: While tempting if the fragments don't separate easily, double cutting the transverse cuts should be avoided unless absolutely necessary. It can inadvertently shorten the osteotomy, which might be undesirable. However, in cases of very stiff joints or severe hallux valgus deformity where significant shortening is actually beneficial for joint decompression, a controlled double cut might be considered.
- Screw Placement:
- Joint Penetration: Always, always perform direct visualization of the metatarsophalangeal joint to confirm the guidewire and subsequent screw are not intra-articular. This is non-negotiable. Fluoroscopy alone is not sufficient for this granular check.
- Proximal Screw Hold: Take care to avoid seating the proximal screw too deep into the very thin dorsal cortex. While cannulated screws offer good purchase, the dorsal cortex can be fragile. Aim for maximal purchase in the plantar cortex of the distal fragment.
- Proximal Plantar Exposure: This seemingly simple step is vital. A safe and thorough proximal plantar exposure, protecting the vascular supply, allows for:
- Accurate orientation of the longitudinal cut parallel to the plantar surface.
- Clear identification of the flare of the first tarsometatarsal joint, ensuring the proximal transverse cut is not intra-articular.
- Direct visualization of the lateral plantar surface, enabling the surgeon to pass the guidewire for the proximal screw under direct vision and precisely check its length, preventing plantar prominence.
Postoperative Care and Rehabilitation
Our work doesn't end in the OR. Postoperative care is crucial for optimal outcomes.
- Immediate Post-Op: The patient will be discharged home on the day of surgery, provided they are stable and pain is controlled. Strict advice is given to elevate the foot whenever resting for the first 2 weeks to minimize swelling. Patients are typically allowed to bear weight on their heel and lateral forefoot in a hard-soled postoperative shoe. Cast immobilization is generally not required for a well-fixed Scarf osteotomy.
- 2 Weeks Post-Op: The wound is inspected for healing. Any sutures are removed. The hallux is then re-strapped to maintain alignment. Patients are taught simple passive and active toe flexion-extension exercises to prevent stiffness and promote early range of motion.
- 5 Weeks Post-Op: We obtain follow-up radiographs to assess the osteotomy for signs of consolidation. If there is adequate radiographic evidence of healing, the patient is instructed to transition from the hard-soled shoe to a wide, comfortable shoe or sneaker. They are encouraged to progress to full weight-bearing as tolerated.
- Beyond 5 Weeks: Physical therapy may be initiated to address any residual stiffness, gait abnormalities, or muscle weakness. Full return to activity is typically gradual over 3-6 months.
Complication Management
While the Scarf osteotomy is highly effective, complications can occur:
- Wound Dehiscence/Infection: Managed with local wound care, antibiotics, or debridement as needed. Early recognition is key.
- Recurrence of Hallux Valgus: Can result from inadequate soft tissue release, insufficient bony correction, or poor patient compliance with post-op instructions. Revision surgery may be considered.
- Avascular Necrosis (AVN) of the Metatarsal Head: A rare but devastating complication, typically due to compromise of the plantar neck vascular bundle. Prevention through meticulous dissection and gentle retraction is paramount. If AVN occurs, non-weight-bearing and observation may be attempted, but severe cases can lead to collapse and require salvage procedures like arthrodesis or implant arthroplasty.
- Hardware Irritation: Prominent screws can cause pain. If symptomatic, hardware removal can be performed after adequate bone healing (typically 6-12 months).
- Non-union or Delayed Union: Rare with good fixation. If it occurs, prolonged non-weight-bearing, bone stimulation, or revision surgery with bone grafting may be necessary.
- Stiffness/Limited Range of Motion: Managed with aggressive physical therapy.
- Nerve Injury: Damage to the dorsal medial cutaneous nerve can cause numbness or painful neuroma. Initial management is conservative; persistent painful neuromas may require excision.
That concludes our masterclass on the Scarf osteotomy. Remember, precision, anatomical knowledge, and meticulous technique are the hallmarks of a successful outcome. Always prioritize patient safety and functional restoration. Thank you, fellows.
REFERENCES
Strapping of the hallux is discontinued at this time. Delayed union or nonunion is rare with this osteotomy.
-
Barouk LS, Barouk P. The Scarf first metatarsal osteotomy in the correction of hallux valgus deformity. Interact Surg 2007;2:2–11.
-
Berg RP, Olsthoorn PG, Pöll RG. Scarf osteotomy in hallux valgus: a review of 72 cases. Acta Orthop Belg 2007;73:219–223.
-
Crevoisier X, Mouhsine E, Ortolano V, et al. The Scarf osteotomy for the treatment of hallux valgus deformity: a review of 84 cases. Foot Ankle Int 2001;22:970–976.
-
Deenik AR, Pilot P, Brandt SE, et al. Scarf versus chevron osteotomy in hallux valgus: a randomized controlled trial in 96 patients. Foot Ankle Int 2007;28:537–541.
-
Deenik A, van Mameren H, de Visser E, et al. Equivalent correction in Scarf and chevron osteotomy in moderate and severe hallux valgus: a randomized controlled trial. Foot Ankle Int 2008;29:1209–1215.
-
Garrido IM, Rubio ER, Bosch MN, et al. Scarf and Akin osteotomies for moderate and severe hallux valgus: clinical and radiographic results. Foot Ankle Surg 2008;14:194–203.
-
Hammel E, Abi Chala ML, Wagner T. Complications of first ray osteotomies: a consecutive series of 475 feet with first metatarsal Scarf osteotomy and first phalanx osteotomy. Rev Chir Orthop Reparatrice Appar Mot 2007;93:710–719.
-
Jones S, Al Hussainy HA, Ali F, et al. Scarf osteotomy for hallux valgus: a prospective clinical and pedobarographic study. J Bone Joint Surg Br 2004;86B:830–836.
-
Lipscombe S, Molly A, Sirikonda S, et al. Scarf osteotomy for the correction of hallux valgus: midterm clinical outcome. J Foot Ankle Surg 2008;47:273–277.
-
Perugia D, Basile A, Gensini A, et al. The scarf osteotomy for severe hallux valgus. Int Orthop 2003;27:103–106.
OUTCOMES
- The Scarf osteotomy is now a widely used method of correction for hallux valgus; it is particularly popular in Europe. Satisfaction rates range from 88% to 92%, 2,3,8,9 equivalent to those of the chevron osteotomy, 4,5 including patients defined as having severe hallux valgus. In a review of five recent publications 4,6,8–10 the hallux valgus angle was improved on average by 16 degrees (range 11 to 21), the intermetatarsal angle by 6.4 (range 3 to 10), and the AOFAS score by 45 (range 37 to 55).
- A learning curve for performing the Scarf osteotomy has also been noted, with higher complication rates seen in early series. 1
COMPLICATIONS
- The main complication seen is stiffness, which occurs in up to 5% of cases. 7 Other complications include wound problems, infection, undercorrection, overcorrection, fractures, chronic regional pain disorder, and deep vein thrombosis. Delayed union and osteonecrosis are rare complications. Fracture risk can be reduced by preserving the lateral strut when placing the proximal screw and by using a long longitudinal cut.
You Might Also Like