Mastering Thoracolumbar Surgery: Full Operative Planning

Key Takeaway
This article provides essential research regarding Mastering Thoracolumbar Surgery: Full Operative Planning. Operative planning full for thoracolumbar spine surgery encompasses a comprehensive approach. It includes a full history and examination, complete spine radiographs with bending films, and whole spine MRI. This crucial stage also involves multidisciplinary team review, detailed anaesthetic and medical workup, lung function tests, and arranging cord monitoring and an intensive care unit bed for optimal patient care.
Comprehensive Introduction and Patho-Epidemiology
The surgical management of the thoracolumbar spine represents one of the most complex, high-stakes, and rapidly evolving domains within orthopedic surgery. Historically, the treatment of spinal deformity, trauma, and degenerative conditions was limited by rudimentary instrumentation and an incomplete understanding of global spinopelvic biomechanics. The paradigm shift from unsegmental distraction constructs, such as Harrington rods, to modern segmental pedicle screw fixation has revolutionized our ability to achieve rigid stabilization and three-dimensional deformity correction. This chapter provides an exhaustive, highly technical overview of thoracolumbar surgery, focusing on operative planning, surgical execution, and the management of complex spinal pathologies.


Epidemiologically, surgical interventions in the thoracolumbar spine are most frequently indicated for adolescent idiopathic scoliosis (AIS), adult spinal deformity (ASD), degenerative spondylolisthesis, spinal trauma, and primary or metastatic oncologic resections. The global burden of adult spinal deformity is particularly notable, with prevalence rates estimated at up to 68% in populations over the age of 60. As life expectancy increases, orthopedic spine surgeons are increasingly tasked with managing severe degenerative kyphoscoliosis in elderly patients who often present with concomitant osteoporosis, cardiopulmonary comorbidities, and rigid, fixed deformities. Understanding the natural history of these conditions is paramount; while AIS primarily threatens coronal balance and cosmetic appearance, adult degenerative scoliosis frequently results in severe sagittal imbalance, debilitating axial back pain, and neurogenic claudication.

The decision to operate on the thoracolumbar spine must be grounded in a meticulous understanding of the patient's patho-epidemiology and a clear definition of surgical goals. The primary objectives of surgical intervention remain the decompression of neural elements, the restoration of global spinopelvic harmony, and the achievement of a solid, durable arthrodesis. Achieving these goals requires an intimate knowledge of spinal anatomy, advanced imaging modalities, and a versatile surgical armamentarium capable of addressing both anterior and posterior column deficiencies. Furthermore, the surgeon must be acutely aware of the systemic impact of major spinal surgery, optimizing the patient pre-operatively to mitigate the inherent risks of extensive blood loss, prolonged anesthesia, and massive fluid shifts.


Detailed Surgical Anatomy and Biomechanics
Thoracic Spine Osteology and Ligamentous Complex
The thoracic spine is uniquely characterized by its inherent stability and relative rigidity, primarily conferred by the articulating rib cage and the coronal orientation of the facet joints. The costovertebral and costotransverse articulations act as a robust anterior and lateral buttress, significantly limiting axial rotation and lateral bending compared to the cervical and lumbar regions. The pedicles of the thoracic spine are morphologically distinct; they are narrower, exhibit greater morphological variability, and have a more medial angulation in the upper thoracic spine (T1-T3) that gradually transitions to a more sagittal orientation in the lower thoracic spine (T10-T12). The medial wall of the thoracic pedicle is substantially thicker than the lateral wall, a critical anatomical feature that directs inadvertently errant pedicle screws laterally into the rib head rather than medially into the spinal canal.

The ligamentous complex of the thoracic spine, comprising the anterior longitudinal ligament (ALL), posterior longitudinal ligament (PLL), ligamentum flavum, and interspinous/supraspinous ligaments, functions as a critical tension band. The ALL is firmly adherent to the anterior vertebral bodies and intervertebral discs, providing significant resistance to hyperextension. The ligamentum flavum in the thoracic region is thinner than in the lumbar spine but remains a vital landmark during posterior decompression and pedicle cannulation. Understanding the tension-band effect of these posterior elements is essential when planning posterior column osteotomies (e.g., Ponte or Smith-Petersen osteotomies), which rely on the resection of the ligamentum flavum and facet capsules to mobilize the thoracic spine for sagittal and coronal correction.
Lumbar Spine and Spinopelvic Parameters
The lumbar spine is engineered for load-bearing and multi-planar mobility, characterized by massive vertebral bodies, thick intervertebral discs, and sagittally oriented facet joints that permit extensive flexion and extension while restricting axial rotation. The pedicles of the lumbar spine are large, ovoid, and directed slightly medially and caudally, making them ideal anchors for robust transpedicular fixation. The transition from the rigid thoracic spine to the mobile lumbar spine at the thoracolumbar junction (T11-L2) creates a biomechanical stress riser, making this region highly susceptible to traumatic fractures and adjacent segment degeneration following long fusions.


A profound understanding of spinopelvic parameters is non-negotiable for the modern spine surgeon. The pelvis acts as the foundational base for the spinal column, and its morphology dictates the required lumbar lordosis (LL) for any given patient. Pelvic Incidence (PI) is a fixed anatomical parameter, while Pelvic Tilt (PT) and Sacral Slope (SS) are dynamic positional parameters (PI = PT + SS). The fundamental goal of adult spinal deformity correction is to restore the mathematical relationship between the spine and the pelvis, specifically aiming for a PI-LL mismatch of less than 10 degrees, a PT of less than 20 degrees, and a Sagittal Vertical Axis (SVA) of less than 5 cm. Failure to respect these biomechanical imperatives inevitably leads to construct failure, proximal junctional kyphosis (PJK), and debilitating postoperative sagittal imbalance.


Neurovascular Considerations
The neurovascular anatomy of the thoracolumbar spine demands meticulous surgical respect. The thoracic spinal cord occupies a relatively large proportion of the spinal canal, leaving a narrow "safe zone" for surgical manipulation. The vascular supply to the thoracic cord is famously tenuous, relying heavily on segmental medullary arteries. The most critical of these is the Artery of Adamkiewicz (Arteria Radicularis Magna), which typically arises from a left-sided intercostal or lumbar artery between T9 and L1 in 75% of individuals. Injury to this vessel during anterior approaches or via overzealous bipolar cauterization of segmental vessels can precipitate catastrophic anterior spinal artery syndrome, presenting as irreversible paraplegia with loss of pain and temperature sensation.


Anterior approaches to the lumbar spine require navigation of the great vessels. The abdominal aorta bifurcates at the L4-L5 disc space, while the inferior vena cava (IVC) is formed by the confluence of the common iliac veins at the L5 vertebral body. The left common iliac vein is particularly vulnerable during anterior exposures of L4-L5, as it courses directly across the disc space. Additionally, the superior hypogastric sympathetic plexus drapes over the anterior aspect of the L5-S1 disc space; iatrogenic injury to this plexus during anterior lumbar interbody fusion (ALIF) can result in retrograde ejaculation in males, a complication that must be explicitly discussed during the informed consent process.
Exhaustive Indications and Contraindications
Clinical Decision Making in Deformity and Degeneration
The indications for surgical intervention in the thoracolumbar spine are multifaceted, depending heavily on the patient's age, symptomatology, and the natural history of the underlying disease process. In adolescent idiopathic scoliosis (AIS), surgery is universally indicated for severe deformity (Cobb angle > 50 degrees) or documented curve progression in a skeletally immature patient. In the adult population, indications shift from purely structural progression to symptomatic relief. Surgery is indicated for neurogenic claudication or radicular pain associated with structural pathology (e.g., degenerative spondylolisthesis or rotatory subluxation) that has failed exhaustive conservative measures, including physical therapy, pharmacological management, and targeted epidural steroid injections.
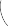

Severe sagittal or coronal imbalance resulting in intractable axial back pain and an inability to maintain an upright posture is a primary indication for complex deformity correction. Patients with flatback syndrome, often a sequela of previous iatrogenic lumbar fusions without adequate lordosis, require extensive reconstructive procedures, frequently involving three-column osteotomies. Furthermore, progressive neurological deficits, cauda equina syndrome, and unstable traumatic fractures (e.g., burst fractures with significant canal compromise and posterior ligamentous complex injury) represent absolute indications for urgent or emergent surgical decompression and stabilization.


Absolute and Relative Contraindications
Surgical intervention is contraindicated in patients whose physiological status precludes the safe administration of general anesthesia or the physiological insult of major surgery. Severe, unoptimized cardiopulmonary disease, active systemic infection, and uncorrectable coagulopathies are absolute contraindications. Relative contraindications require nuanced clinical judgment and extensive preoperative optimization. Severe osteoporosis (T-score < -2.5) significantly increases the risk of hardware pullout, subsidence, and proximal junctional failure (PJF). In these cases, preoperative anabolic therapy (e.g., teriparatide) and intraoperative techniques such as cement augmentation of pedicle screws are strongly recommended.
| Category | Absolute Contraindications | Relative Contraindications |
|---|---|---|
| Medical/Systemic | Active systemic or surgical site infection; Uncorrectable coagulopathy; ASA Class V | Poorly controlled diabetes (HbA1c > 7.5%); Severe malnutrition; Active nicotine use |
| Bone Quality | Non-viable bone stock for fixation (e.g., severe radiation necrosis) | Severe osteoporosis requiring pre-op anabolic therapy; Chronic steroid use |
| Neurological | Complete, irreversible paraplegia > 48 hours (for decompression purposes) | Progressive neurodegenerative disorders (e.g., ALS) complicating rehab |
| Psychosocial | Inability to consent; Active, untreated severe psychiatric illness | Poor compliance history; Lack of social support for postoperative rehabilitation |

Pre-Operative Planning, Templating, and Patient Positioning
Advanced Imaging and Spinopelvic Templating
The foundation of successful thoracolumbar surgery lies in exhaustive preoperative planning. Standard imaging protocols must include full-length, free-standing 36-inch orthogonal radiographs to accurately assess global coronal and sagittal balance. The use of EOS low-dose biplanar imaging has become the gold standard, allowing for simultaneous assessment of the spine, pelvis, and lower extremities, which is crucial for identifying compensatory mechanisms such as pelvic retroversion, hip extension, and knee flexion. Magnetic Resonance Imaging (MRI) is mandatory to evaluate the neural elements, assess disc hydration, and identify central, lateral recess, or foraminal stenosis.

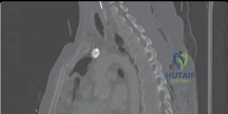
High-resolution computed tomography (CT) with multiplanar reconstruction is essential for evaluating bone stock, identifying facet arthropathy, and planning pedicle screw trajectories. In cases of severe deformity or revision surgery, CT-based 3D templating software allows the surgeon to simulate osteotomies, calculate the exact degree of correction required to achieve spinopelvic harmony, and pre-contour rods. The surgeon must meticulously calculate the required Lumbar Lordosis (LL) based on the patient's Pelvic Incidence (PI), plan the upper and lower instrumented vertebrae (UIV and LIV) to avoid ending the construct at the apex of a kyphotic curve, and determine the necessity of pelvic fixation.

Anesthetic Considerations and Neuromonitoring
Thoracolumbar reconstruction is physiologically demanding, often associated with massive blood loss and significant fluid shifts. Multidisciplinary preoperative optimization involving anesthesiology and internal medicine is critical. A robust blood conservation strategy must be employed, including the preoperative administration of erythropoietin and iron, intraoperative cell salvage (Cell Saver), and the systematic use of antifibrinolytics such as Tranexamic Acid (TXA). TXA is typically administered as a loading dose (10-50 mg/kg) followed by a continuous infusion, significantly reducing both intraoperative and postoperative hemorrhagic losses.


Multimodal intraoperative neuromonitoring (IONM) is the standard of care for complex thoracolumbar surgery. This includes Somatosensory Evoked Potentials (SSEPs) to monitor the dorsal columns, Transcranial Motor Evoked Potentials (TcMEPs) for the anterior corticospinal tracts, and spontaneous/triggered Electromyography (sEMG/tEMG) for individual nerve root function. The anesthesia team must utilize total intravenous anesthesia (TIVA) without neuromuscular blockade to ensure reliable MEP signals. Any significant degradation in neuromonitoring signals demands an immediate, algorithmic response: increasing mean arterial pressure (MAP > 85 mmHg), correcting anemia or hypovolemia, releasing traction or deformity correction maneuvers, and ruling out technical hardware complications.

Optimal Patient Positioning
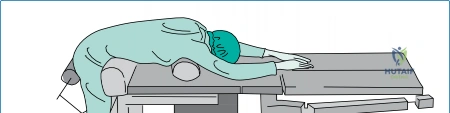
Patient positioning is a critical, yet often underappreciated, phase of the surgical procedure. For posterior approaches, the patient is typically positioned prone on an open-frame Jackson table. This specialized table allows the abdomen to hang freely, reducing intra-abdominal pressure, thereby decreasing venous engorgement of the epidural Batson's plexus and minimizing intraoperative bleeding. The hips should be extended to maximize lumbar lordosis during positioning, particularly when in-situ fusion is planned.

Meticulous attention must be paid to pressure points. The face must be supported with a specialized foam prone-view mask, ensuring the eyes are completely free of pressure to prevent catastrophic perioperative visual loss (POVL), typically caused by ischemic optic neuropathy. The arms are abducted to less than 90 degrees and slightly flexed to prevent brachial plexus stretch injuries. All bony prominences, including the ulnar nerves, iliac crests, and patellae, must be heavily padded. The surgical team must confirm that the breasts and male genitalia are free from compression before the sterile prep begins.


Step-by-Step Surgical Approach and Fixation Technique
Posterior-Only Approach and Pedicle Screw Instrumentation
There is an overwhelming and increasing trend towards posterior-only surgery for the management of thoracolumbar pathologies. The posterior approach provides excellent access to the posterior column, neural elements, and pedicles for robust three-column fixation. The procedure begins with a precise midline incision, followed by subperiosteal dissection of the paraspinal musculature off the spinous processes, laminae, and facet joints. Meticulous hemostasis using bipolar electrocautery and bone wax is maintained throughout the exposure. The dissection must extend laterally to the tips of the transverse processes in the thoracic spine and the lateral pars/transverse processes in the lumbar spine to provide an adequate bed for the posterolateral fusion mass.

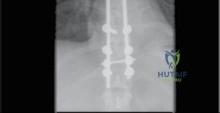
Pedicle screw instrumentation forms the biomechanical foundation of modern constructs. The freehand technique relies on precise anatomical landmarks: the intersection of the pars interarticularis, the superior articular facet, and the transverse process. The cortex is burred, and a pedicle probe is advanced with tactile feedback to ensure an intraosseous trajectory. The tract is then palpated with a ball-tipped probe to confirm five intact bony walls (medial, lateral, superior, inferior, and anterior). Alternatively, stereotactic navigation and robotic-assisted placement are increasingly utilized, particularly in cases of severe rotational deformity, revision surgery with obscured landmarks, or minimally invasive (MIS) approaches. These technologies significantly enhance the accuracy of screw placement, reducing the risk of neurological injury and biomechanical failure.


Anterior Approaches and Interbody Fusion Techniques
While posterior surgery dominates, anterior approaches remain indispensable for specific indications. A thorough, complete discectomy is only possible with an anterior approach; thus, very stiff, rigid curves may benefit significantly from an anterior release prior to posterior instrumentation. Furthermore, thoracolumbar and lumbar curves are frequently treated with anterior instrumentation, especially if there is no compensatory or structural thoracic curve. Anterior Lumbar Interbody Fusion (ALIF), Oblique Lumbar Interbody Fusion (OLIF), and Lateral Lumbar Interbody Fusion (LLIF) allow for the placement of massive interbody cages spanning the apophyseal ring.


These anterior and lateral techniques provide unparalleled indirect decompression of the neural foramina through restoration of disc height, maximize the surface area for arthrodesis, and offer powerful tools for correcting sagittal and coronal deformities via hyperlordotic cages and sectioning of the ALL. The anterior approach to the thoracic spine, typically via a thoracotomy or video-assisted thoracoscopic surgery (VATS), allows for the resection of rib heads and complete excision of the intervertebral discs, mobilizing the anterior column for subsequent posterior correction. However, these approaches carry unique morbidity, including pulmonary complications, intercostal neuralgia, and the risk of great vessel injury.


Deformity Correction Maneuvers and Pelvic Fixation
Once the spine is instrumented and mobilized via facetectomies or osteotomies, deformity correction is executed. Techniques include rod translation, where the spine is pulled to a pre-contoured rod; cantilever reduction, utilizing the rod as a lever arm to reduce kyphosis; and direct vertebral derotation (DVD), which applies torsional forces to correct the rotational component of scoliosis. In cases of severe, rigid deformity, three-column osteotomies are required. Pedicle Subtraction Osteotomies (PSO) can provide 30-40 degrees of sagittal correction at a single level, while Vertebral Column Resections (VCR) are reserved for the most severe, fixed, and angular deformities, offering complete dissociation of the spinal column for massive realignment.

Posterior instrumentation allows for robust fixation to the pelvis, which is a massive advantage—and often a strict requirement—in long fusions in the elderly, patients with severe sagittal imbalance, and non-walking patients with neuromuscular-type curves. Stopping a long construct at L5 is associated with unacceptably high rates of L5-S1 disc degeneration, pseudarthrosis, and hardware failure. Pelvic fixation is most commonly achieved using S2-Alar-Iliac (S2AI) screws or traditional iliac screws. S2AI screws offer the advantage of remaining in line with the lumbar construct, eliminating the need for bulky offset connectors and reducing implant prominence, which is particularly beneficial in thin, malnourished patients.

Complications, Incidence Rates, and Salvage Management
Neurological and Vascular Complications
Thoracolumbar surgery carries a significant risk profile that must be explicitly discussed with the patient. The overall mortality rate is approximately 0.03%, primarily driven by cardiopulmonary events in elderly patients undergoing massive reconstructive procedures. Neurological deficit is the most feared complication; the incidence of complete neurological deficit (paraplegia) is 0.03%, while incomplete deficits (radiculopathy, transient weakness) occur in approximately 1.5% of cases. Neurological injury can result from direct trauma via errant pedicle screws, over-distraction of the spinal cord during deformity correction, or ischemic injury secondary to hypotension or vascular sacrifice.
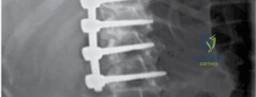
Vascular complications, while rare, can be catastrophic. Damage to major vessels, such as the aorta or inferior vena cava, primarily occurs during anterior approaches or via over-penetration of pedicle screws breaching the anterior vertebral cortex. Immediate recognition and vascular surgery consultation are imperative. Additionally, damage to the sympathetic chain during anterior thoracic or lumbar approaches can result in Horner's syndrome or sympathectomy-induced temperature dysregulation in the lower extremities, respectively.
Mechanical Failure and Pseudarthrosis
Mechanical complications remain a persistent challenge, with revision surgery required in approximately 5% of cases. Failure to achieve complete curve correction or failure to restore spinopelvic parameters inevitably leads to abnormal biomechanical loading and subsequent construct failure. Proximal Junctional Kyphosis (PJK) and Proximal Junctional Failure (PJF) are particularly prevalent in adult
Clinical & Radiographic Imaging Archive