Exploring Every Approach to the Cervical: A Surgeon's Guide
Key Takeaway
Here are the crucial details you must know about Exploring Every Approach to the Cervical: A Surgeon's Guide. An approach to the cervical spine involves surgical access, primarily categorized as anterior (C3-T1) or posterior (C1-C7). These procedures address conditions like spinal canal stenosis, herniated discs, tumors, or instability. Indications for an anterior approach to the cervical spine include decompression, fusion, stabilization, or disc replacement, aimed at alleviating neurological symptoms or correcting deformities.
Comprehensive Introduction and Patho-Epidemiology
The surgical management of the cervical spine represents one of the most dynamic and anatomically demanding frontiers in modern orthopedic surgery. Historically, the treatment of cervical pathology was limited to posterior non-instrumented fusions and prolonged immobilization. However, the advent of the Smith-Robinson anterior approach in the mid-20th century, coupled with the exponential evolution of posterior segmental instrumentation, has fundamentally revolutionized our armamentarium. Today, cervical spine surgery demands a profound, three-dimensional understanding of neurovascular anatomy, biomechanics, and the natural history of degenerative, traumatic, and neoplastic conditions.
Epidemiologically, the burden of cervical spine disease is shifting dramatically. With an increasingly aging global population, the incidence of cervical spondylotic myelopathy (CSM)—the most common cause of spinal cord dysfunction in adults over the age of fifty—has surged. Concurrently, high-velocity trauma, ossification of the posterior longitudinal ligament (OPLL), and metastatic disease present complex reconstructive challenges that require the surgeon to be equally adept at anterior, posterior, and combined approaches. The decision-making process is no longer merely about decompression; it is intricately tied to the restoration of global sagittal alignment, the preservation of adjacent segment kinematics, and the minimization of iatrogenic morbidity.
The fundamental goal of any cervical approach is the safe and adequate exposure of the pathology while mitigating risks to the visceral axis, the major vascular conduits, and the neural elements. This chapter serves as a definitive, high-yield guide to the myriad approaches to the cervical spine. It meticulously details the anterior subaxial approach (C3-T1), the posterior subaxial approach (C2-C7), the highly specialized posterior upper cervical approach (C1-C2), and the application of halo vest fixation. By synthesizing classic anatomical principles with contemporary evidence-based guidelines, this text aims to equip the orthopedic surgeon, fellow, and resident with the cognitive and technical framework required to navigate the cervical spine safely and effectively.
Detailed Surgical Anatomy and Biomechanics
A masterful cervical surgeon must possess an encyclopedic knowledge of the fascial layers, muscular planes, and neurovascular relationships of the neck. Anteriorly, the neck is compartmentalized by the deep cervical fascia, which is divided into the superficial investing, pretracheal, and prevertebral layers. The anterior approach (Smith-Robinson) capitalizes on the avascular internervous plane between the visceral axis (trachea and esophagus, invested by the pretracheal fascia) medially, and the carotid sheath (common carotid artery, internal jugular vein, and vagus nerve) laterally. The longus colli muscles, lying on the anterior surface of the vertebral bodies, serve as the ultimate landmark for midline orientation and safe retractor placement.
The Recurrent Laryngeal Nerve (RLN) demands specific anatomical reverence. The right RLN branches from the vagus nerve, looping under the right subclavian artery, and ascends obliquely across the operative field to reach the tracheoesophageal groove. Its variable and higher crossing makes it inherently more susceptible to iatrogenic traction injury during right-sided anterior approaches. Conversely, the left RLN loops under the aortic arch and ascends vertically within the protected tracheoesophageal groove, rendering a left-sided approach theoretically safer for the nerve, though surgeon handedness and pathology location often dictate the side of the approach. Furthermore, the sympathetic chain lies laterally on the longus colli; aggressive lateral dissection can result in Horner’s syndrome.
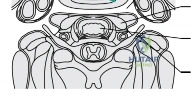
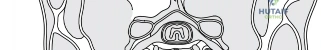
Posteriorly, the anatomy is defined by the robust nuchal ligament and the complex layering of the paraspinal musculature (trapezius, splenius capitis, semispinalis capitis, and cervicis). The posterior approach relies on maintaining a strict midline avascular plane to minimize blood loss and muscle denervation. In the upper cervical spine (C1-C2), the vertebral artery (V3 segment) is the most critical structure. It exits the C2 foramen transversarium, courses laterally to enter the C1 foramen, and then loops medially over the posterior arch of C1 within the vertebral artery groove (sulcus arteriosus) before piercing the posterior atlanto-occipital membrane.
Cervical Biomechanics and Kinematics
Understanding the clinical and radiological range of motion (ROM) is paramount for both diagnosis and surgical planning. The cervical spine is divided biomechanically into the upper (occipitocervical and atlantoaxial) and lower (subaxial, C3-C7) segments. The atlantoaxial joint (C1-C2) is responsible for approximately 50% of total cervical axial rotation, while the subaxial spine provides the majority of flexion, extension, and lateral bending.
The clinical and radiological range of motion parameters are defined as follows:
- Flexion: Clinical total is 45°. Radiologically, the upper spine (C1-C2) contributes 15°, while the lower spine (C3-C7) contributes 40°.
- Extension: Clinical total is 55°. Radiologically, the upper spine contributes 15°, and the lower spine contributes 25°.
- Lateral Bending: Clinical total is 40°. The upper spine contributes 0°, while the lower spine contributes a massive 50°.
- Axial Rotation: Clinical total is 70°. The upper spine is the primary driver here, contributing 40°, with the lower spine contributing 45°.
Position of Arthrodesis
When performing a fusion, the spatial orientation of the construct is critical to prevent late deformity and adjacent segment degeneration. The overarching principle is to maintain the native sagittal contour (cervical lordosis) and strictly avoid local iatrogenic kyphosis.
1. During anterior interbody fusion surgery (ACDF), the structural bone graft or artificial interbody cage selected must be wedge-shaped, featuring a greater anterior vertebral height compared to the posterior height. This forces the adjacent endplates into a lordotic alignment.
2. During posterior fusion and stabilization procedures, the titanium or cobalt-chrome rods must be meticulously contoured into a lordotic shape prior to securing the set screws, thereby using the instrumentation to pull the spine into physiological alignment.
Exhaustive Indications and Contraindications
The decision to approach the cervical spine anteriorly, posteriorly, or via a combined 360-degree approach hinges on the location of the compressive pathology, the sagittal alignment of the spine, the number of levels involved, and the presence of instability. The anterior approach is generally favored for ventral pathology, particularly when cervical kyphosis is present, as it allows for direct decompression of the anterior column and simultaneous restoration of lordosis through structural grafting.
Indications for the anterior approach (C3-T1) include anterior decompression for spinal canal or foraminal stenosis presenting as myelopathy, radiculopathy, or profound neurological deficit. It is the gold standard for herniated discs arising from degenerative or traumatic causes, ventral osteophyte complexes, and anterior bony element fractures. Furthermore, it is indicated for degenerative subluxation, excision of anterior tumors, drainage of prevertebral infections, and addressing congenitally narrow canals. In cases of OPLL, anterior corpectomy or discectomy is highly effective, though it carries a higher risk of dural tears. Additionally, the anterior approach is utilized for Cervical Disc Replacement (CDR) in carefully selected patients with degenerative disc disorders lacking facet arthropathy or instability.

Conversely, the posterior approach is typically reserved for multilevel disease (typically >3 levels), dorsal compressive pathology (such as ligamentum flavum hypertrophy), or when the patient has preserved cervical lordosis. It is also the primary route for addressing C1-C2 instability (e.g., odontoid fractures, transverse ligament ruptures, rheumatoid atlantoaxial subluxation). Halo vest fixation, while less common in the modern era of rigid internal fixation, remains a vital tool for definitive non-operative management of specific upper cervical trauma or as an adjunct to internal fixation in highly unstable scenarios.
| Approach / Technique | Primary Indications | Absolute Contraindications | Relative Contraindications |
|---|---|---|---|
| Anterior (ACDF/Corpectomy) | Ventral disc herniation, anterior osteophytes, kyphotic deformity, anterior trauma, CDR. | Active anterior neck infection, severe uncorrectable coagulopathy. | Prior anterior neck radiation, previous severe dysphagia, massive multilevel OPLL. |
| Posterior (Laminectomy/Fusion) | Multilevel stenosis (>3 levels), maintained lordosis, dorsal compression, C1-C2 instability. | Fixed cervical kyphosis (without combined anterior release). | Poor bone quality (for lateral mass screws), previous extensive posterior muscle resection. |
| Posterior (Laminoplasty) | Multilevel myelopathy with preserved lordosis, OPLL. | Kyphosis, severe axial neck pain, gross instability. | Rheumatoid arthritis, severe facet arthropathy. |
| Halo Vest Fixation | Occipital condyle fractures, specific C1/C2 fractures (e.g., Type II odontoid in young patients), adjunctive stability. | Severe skull fractures, overriding cranial trauma, severe soft tissue scalp injury. | Elderly patients (high risk of respiratory failure/falls), barrel-chest deformity. |
Pre-Operative Planning, Templating, and Patient Positioning
Meticulous preoperative planning is the bedrock of successful cervical spine surgery. Imaging must include high-quality orthogonal plain radiographs to assess global alignment, dynamic flexion-extension views to rule out occult instability, and advanced cross-sectional imaging. MRI is mandatory for evaluating neural element compression, cord signal changes (myelomalacia), and soft tissue integrity. Thin-slice CT with sagittal and coronal reconstructions is critical for evaluating bony anatomy, particularly the course of the vertebral arteries, facet joint morphology, and the presence of OPLL or osteophytes.

Positioning for the Anterior Approach
For the anterior approach, the patient is positioned supine on a radiolucent table. A transverse shoulder roll is placed vertically between the scapulae to allow the shoulders to fall posteriorly, naturally extending the neck and enhancing lordosis. The head is supported on a foam donut. For lower cervical levels (C6-T1), visualization is often obstructed by the clavicles and shoulders. To mitigate this, bilateral shoulder traction using heavy adhesive tape pulled distally and secured to the foot of the bed is employed. Alternatively, Gardner-Wells tongs or a halter traction system can be used to stabilize the head and provide gentle axial traction. The chin should be slightly rotated away from the side of the approach to stretch the SCM and open the surgical corridor.
Positioning for the Posterior Approach
For posterior subaxial and upper cervical approaches, the patient is typically positioned prone. The head is rigidly secured using a Mayfield cranial tong system. The neck is positioned in a "military tuck" (slight flexion to open the posterior elements, but maintaining neutral global alignment to avoid fusing the patient in kyphosis). The table is placed in reverse Trendelenburg (head up) to decrease venous engorgement in the epidural space, significantly reducing intraoperative bleeding. All pressure points, particularly the eyes, face, and ulnar nerves, must be meticulously padded and checked.

Halo Vest Application Principles
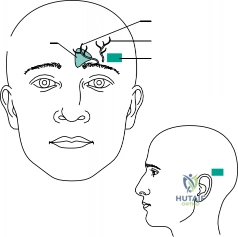
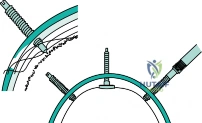
When applying a halo vest, positioning and pin placement are critical. The anterior pins must be placed in the "safe zone" of the frontal bone: lateral to the supraorbital nerve and artery (lateral to the middle third of the eyebrow), below the equator of the skull, and above the orbital rim. Posterior pins are placed diagonally opposite the anterior pins, typically 1-2 cm superior to the ear, clearing the mastoid process. Pins are tightened in opposing pairs to a standard torque of 8 inch-pounds in adults (less in children, depending on skull thickness).
Step-by-Step Surgical Approach and Fixation Technique
Anterior Approach to the Cervical Spine (C3-T1)
The anterior approach utilizes a transverse incision (often hidden in a natural skin crease for cosmesis) for 1-2 level pathology, or a longitudinal incision along the anterior border of the SCM for extensive multilevel disease. After incising the skin and subcutaneous tissue, the platysma is divided in line with the skin incision. The superficial layer of the deep cervical fascia is incised anterior to the SCM.
Blunt dissection is then utilized to develop the plane between the carotid sheath laterally and the visceral axis medially. The omohyoid muscle may be mobilized or divided depending on the level (it typically crosses at C6). The prevertebral fascia is then incised over the midline, exposing the longus colli muscles. The sympathetic chain, located on the lateral third of the longus colli, must be protected. The longus colli are elevated subperiosteally to allow for the placement of self-retaining retractors under the muscle edges, preventing slippage and protecting the esophagus and carotid sheath.
Following discectomy and decompression of the uncinate processes and posterior longitudinal ligament, the cartilaginous endplates are removed using curettes and burrs, preserving the subchondral bone to prevent graft subsidence. A wedge-shaped structural graft or cage is impacted into the disc space to restore height and lordosis. An anterior cervical plate is then applied, ensuring the screws do not violate the adjacent disc spaces.

Posterior Approach to the Lower Cervical Spine (C2-C7)
A strict midline longitudinal incision is made through the skin and subcutaneous tissues down to the nuchal ligament. Using electrocautery, an avascular dissection is performed straight down to the spinous processes. Subperiosteal dissection of the paraspinal musculature is carried out laterally to expose the laminae and the lateral masses. Dissection must not proceed lateral to the lateral margin of the lateral masses to avoid injuring the vertebral artery and exiting nerve roots.
For lateral mass screw fixation, the Magerl or Roy-Camille techniques are most commonly utilized. In the Magerl technique, the entry point is 1 mm medial and 1 mm superior to the center of the lateral mass. The trajectory is 25 degrees outward (lateral) and parallel to the facet joint (approximately 25-30 degrees cephalad). This trajectory safely avoids the vertebral artery anteriorly and the nerve root inferiorly. Following screw placement, decompression via laminectomy or laminoplasty can be safely performed without compromising the fixation points.
Posterior Approach to the Upper Cervical Spine (C1-C2)
The upper cervical spine demands extreme precision. The posterior arch of C1 is exposed, taking care not to dissect more than 1.5 cm lateral to the midline to avoid the vertebral artery in the sulcus arteriosus. The C2 spinous process, laminae, and pars interarticularis are exposed.

The Harms technique (C1 lateral mass screws combined with C2 pedicle or pars screws) is the modern workhorse for atlantoaxial instability. For C1, the C2 nerve root is mobilized inferiorly, and the entry point is at the center of the posterior aspect of the C1 lateral mass. The trajectory is straight anterior and slightly medial. For C2 pedicle screws, the entry point is in the cranial and medial quadrant of the C2 isthmus, with a trajectory directly medial (20-30 degrees) and cephalad (20 degrees), guided by preoperative CT templating to navigate the narrow pedicle and avoid the high-riding vertebral artery.
Complications, Incidence Rates, and Salvage Management
Surgical intervention in the cervical spine is fraught with potential complications, ranging from transient functional deficits to catastrophic neurovascular injury. A profound understanding of these risks, their incidence, and mitigation strategies is essential for informed consent and intraoperative safety.
Dysphagia: This is the most common complication following anterior cervical surgery. The incidence is remarkably high, reported at approximately 50% in the short term (within the first few weeks) and lingering at around 10% in the long term. It is significantly more common in multilevel surgeries, prolonged retraction times, revision surgeries, and in older patients. The etiology is multifactorial, involving esophageal edema, hematoma, denervation, and mechanical irritation from high-profile anterior plates. This complication can be actively reduced by keeping retraction time to an absolute minimum (periodically releasing retractors), utilizing smooth-contour retractors, selecting lower-profile titanium plates, ensuring meticulous tissue handling, and achieving absolute hemostasis. Deflating and re-inflating the endotracheal tube cuff after retractor placement also reduces pressure on the recurrent laryngeal nerve and esophageal mucosa.
Recurrent Laryngeal Nerve (RLN) Injury: The incidence of RLN injury is approximately 0.2% to 1%, though subclinical vocal cord paresis may be higher. It produces paralysis of one side of the vocal cord, leading to dysphonia (hoarseness of the voice), airway problems, and a high risk of aspiration pneumonia. As previously detailed, this is anatomically more common in right-sided approaches due to the variable and oblique course of the right RLN. If bilateral anterior surgery is planned (e.g., a staged revision), an ENT evaluation of the vocal cords is mandatory prior to the second stage; operating on the contralateral side in the presence of an unrecognized unilateral palsy can result in bilateral cord paralysis, necessitating an emergency tracheostomy.
C5 Palsy: This is a well-documented complication following both anterior and posterior cervical decompressions, with an incidence ranging from 5% to 10%. It typically presents as delayed-onset weakness of the deltoid and biceps muscles, often without sensory loss or pain. The exact etiology is debated but is largely attributed to the "tethering effect"—the posterior shift of the spinal cord following decompression places traction on the short, horizontally oriented C5 nerve roots. Most cases resolve spontaneously over 6 to 12 months with conservative management and physical therapy.
| Complication | Estimated Incidence | Primary Prevention Strategy | Salvage / Management |
|---|---|---|---|
| Dysphagia | 50% short-term; 10% long-term | Intermittent retractor release, low-profile plates, deflate ET cuff. | Diet modification, speech therapy, rarely hardware removal. |
| RLN Palsy | 0.2% - 1.0% | Left-sided approach (debatable), avoid sharp dissection in tracheoesophageal groove. | ENT referral, vocal cord injection, speech therapy. |
| Vertebral Artery Injury | <0.5% | Pre-op CT templating, strict adherence to lateral mass/pedicle trajectories. | Direct tamponade, avoid bilateral injury, endovascular coiling/stenting. |
| Esophageal Perforation | <0.1% | Blunt dissection, smooth retractors, avoid over-penetration of drills/screws. | Immediate intraoperative repair, muscle flap, NPO, broad-spectrum IV antibiotics. |
| C5 Palsy | 5% - 10% | Avoid excessive posterior cord drift (limit width of laminectomy), prophylactic foraminotomy. | Physical therapy, time (majority recover within 12 months). |
Phased Post-Operative Rehabilitation Protocols
The postoperative rehabilitation of the cervical spine patient must be meticulously tailored to the specific surgical approach, the quality of the patient's bone, and the biomechanical stability of the construct. The overarching goal is to protect the neural elements and the developing fusion mass while preventing adjacent segment stiffness and muscular atrophy.

Phase 1: Protection and Healing (Weeks 0-4)
In the immediate postoperative phase, the primary focus is on wound healing, pain control, and protection of the instrumentation. For standard 1-2 level ACDFs with rigid plating, a soft cervical collar is often utilized merely for patient comfort and proprioceptive feedback, rather than structural support. However, for multilevel posterior reconstructions, corpectomies, or patients with osteopenia, a rigid orthosis (e.g., Aspen or Miami J collar) is mandated for 4 to 6 weeks. Patients are instructed on strict swallowing precautions (soft diet initially) and are taught log-rolling techniques for bed mobility. Lifting is strictly restricted to less than 5-10 pounds.
Phase 2: Weaning and Isometric Strengthening (Weeks 4-8)
As the initial soft tissue healing progresses, the patient is gradually weaned from the cervical orthosis. Physical therapy is initiated with a focus on gentle, pain-free active range of motion (ROM). Passive stretching by a therapist is generally avoided to prevent undue stress on the hardware. Isometric strengthening of the cervical paraspinal and deep neck flexor muscles is introduced. Upright standing radiographs (AP, Lateral, and sometimes dynamic flexion-extension views) are obtained around the 6-week mark to assess hardware integrity, maintenance of lordosis, and early signs of bridging trabecular bone.
Phase 3: Dynamic Stabilization and Return to Function (Weeks 8-12+)
During this phase, therapy progresses to dynamic stabilization exercises, proprioceptive training, and upper extremity strengthening. Cardiovascular conditioning is increased. Return to work and sport criteria are highly individualized. Sedentary work may be resumed as early as 2-4 weeks, whereas heavy manual labor or contact sports require a minimum of 3-6 months, definitive radiographic evidence of solid arthrodesis, and full, painless recovery of motor strength.
Halo Vest Specific Rehabilitation
Patients managed in a halo vest require highly specialized care. Pin sites must be cleaned daily using half-strength hydrogen peroxide or chlorhexidine to prevent pin tract infections. The torque of the pins must be checked by the surgeon at 24 hours, 48 hours, and then weekly for the first month to prevent loosening. The vest itself must be kept dry, and skin integrity beneath the vest must be monitored closely to prevent decubitus ulcers. The halo is typically maintained for 10 to 12 weeks, followed by a transition to a rigid cervical collar for an additional 4 weeks as the musculature rehabilitates.
Summary of Landmark Literature and Clinical Guidelines
The evolution of cervical spine surgery is deeply rooted in landmark peer-reviewed literature that continues to dictate modern clinical guidelines. The original description of the anterior cervical discectomy and fusion by Smith and Robinson in 1958 remains the foundational text for the anterior approach, establishing the safety of the internervous plane and the efficacy of structural tricortical iliac crest grafting.
A critical concept in cervical spine surgery is the development of Adjacent Segment Disease (ASD). The landmark longitudinal study by Hilibrand et al. (1999) demonstrated that symptomatic adjacent segment disease occurs at a rate of approximately 2.9% per year following ACDF, with survivorship free of ASD being roughly 75% at 10 years. This literature spurred the development and rigorous FDA investigational device exemption (IDE) trials for Cervical Disc Replacement (CDR). Long-term data (7-10 year follow-ups) from trials comparing ACDF to CDR (e.g., Mobi-C, ProDisc-C) have shown that CDR is statistically non-inferior, and in some parameters superior, to ACDF for 1- and 2-level disease, specifically highlighting lower rates of secondary surgical interventions at adjacent levels.
Furthermore, guidelines from the Cervical Spine Research Society
