Adjacent Segment Degeneration: Your Next Spine Case Solved
Key Takeaway
For anyone wondering about Adjacent Segment Degeneration: Your Next Spine Case Solved, Posterior ligamentous disruption is the strongest indicator of instability in thoracolumbar burst fractures, overriding traditional radiographic parameters. This often necessitates surgical intervention, which, in the long term, can contribute to adjacent segment degeneration. Noncontiguous spinal fractures are found in approximately 15% of such cases, emphasizing comprehensive evaluation for these complex injuries.
Welcome to this week’s Grand Rounds. I am presenting a highly complex, multi-layered clinical scenario that bridges the gap between acute orthopedic trauma and long-term spine survivorship. While the immediate threat to our patient is a catastrophic structural failure of the thoracolumbar junction, the overarching theme of our discussion today—and the reason for our title, "Adjacent Segment Degeneration: Your Next Spine Case Solved"—is that the decisions we make in the trauma bay and the operating room tonight will directly dictate whether this patient returns to our clinic in five years with adjacent segment disease.
We will deconstruct a classic, yet perilous, L1 burst fracture with posterior ligamentous complex (PLC) disruption. We will dismantle outdated dogma, specifically the "50-50-25 rule," explore the high incidence of noncontiguous spine fractures, and detail the meticulous surgical execution required to stabilize the spine, protect the neural elements, and restore sagittal balance to prevent future adjacent segment degeneration.
Detailed Patient Presentation and Mechanism of Injury
Our patient is a 45-year-old previously healthy male who was brought to the Level 1 trauma bay after sustaining a high-energy fall from the roof of his two-story home while cleaning his gutters. Emergency Medical Services reported an estimated fall height of approximately 15 to 20 feet, with the patient landing primarily on his feet before collapsing backward onto his buttocks. Upon arrival, he was immobilized on a rigid backboard with a cervical collar in place. His chief complaint was excruciating, unremitting lower back pain that was exacerbated by any truncal movement.
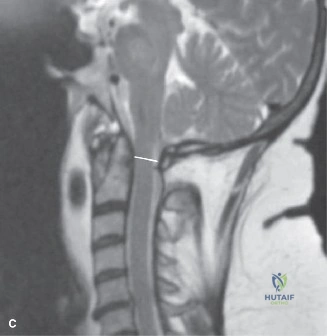
The mechanism of injury here is paramount to understanding the resulting fracture pattern. A fall from height generating an axial load, combined with a sudden flexion moment as the torso collapses forward over the pelvis, places immense stress on the thoracolumbar junction (T11-L2). This region is highly susceptible to injury due to the biomechanical transition from the rigid, kyphotic thoracic spine (supported by the rib cage) to the mobile, lordotic lumbar spine. The axial vector drives the nucleus pulposus through the vertebral endplate, causing the vertebral body to explode outward—the classic burst fracture. Simultaneously, the flexion moment exerts massive tensile forces on the posterior elements, jeopardizing the posterior ligamentous complex.
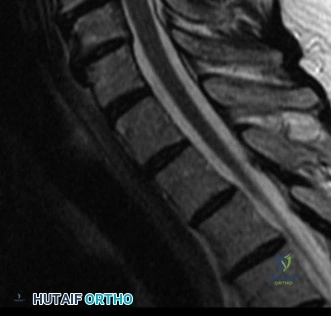
It is critical to recognize that high-energy axial loading injuries rarely occur in isolation. As trauma surgeons, we must maintain a high index of suspicion for associated injuries. The energy transferred through the calcaneus, up the lower extremities, and into the axial skeleton frequently results in concomitant calcaneus fractures, tibial plateau fractures, or pelvic ring disruptions. Furthermore, the sudden deceleration can cause visceral injuries, particularly to the kidneys, spleen, or bowel. In this patient, primary ATLS survey revealed a hemodynamically stable individual, but secondary survey required meticulous attention to the bilateral hindfeet and the abdomen to rule out these classic associated trauma patterns.
Comprehensive Clinical Examination Findings
In the trauma bay, a rigorous and systematic physical examination is the cornerstone of our initial assessment. Following the clearance of his airway, breathing, and circulation, the patient underwent a careful log-roll maneuver to inspect the posterior torso. Inspection revealed significant ecchymosis and soft tissue swelling over the thoracolumbar junction. Palpation elicited exquisite tenderness directly over the spinous processes of T12, L1, and L2. More importantly, a distinct, palpable step-off and widening of the interspinous distance between T12 and L1 was noted. This physical finding is a massive red flag, clinically highly suggestive of a posterior tension band failure and disruption of the interspinous ligaments.
A comprehensive neurological examination was performed and documented according to the American Spinal Injury Association (ASIA) Impairment Scale. Despite the severe bony injury, the patient demonstrated full 5/5 motor strength in all key myotomes of the bilateral lower extremities, including hip flexion (L2), knee extension (L3), ankle dorsiflexion (L4), great toe extension (L5), and ankle plantarflexion (S1). Sensation to light touch and pinprick was completely intact across all dermatomes. Crucially, a digital rectal examination confirmed normal resting sphincter tone and intact voluntary perianal sensation, confirming sacral sparing. The bulbocavernosus reflex was present. The patient was classified as ASIA E.
However, an ASIA E status in the setting of this specific fracture pattern does not equate to a benign clinical course. The presence of a lamina fracture—which we will discuss in the imaging section—in conjunction with significant canal compromise places the neural elements (the conus medullaris and cauda equina) at extreme risk for delayed or iatrogenic injury. The initial intact neurological exam is a baseline; it dictates that our primary surgical goal is the preservation of this function. Any deterioration in his neurological status would mandate an immediate, emergent decompression.
Advanced Imaging and Diagnostics
Radiographic and Computed Tomography Evaluation
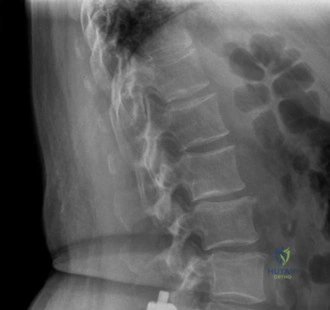
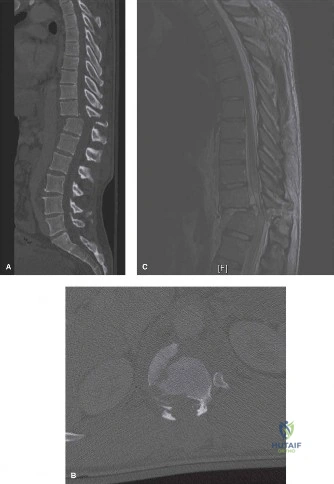
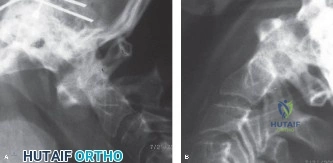
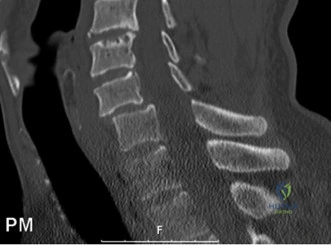
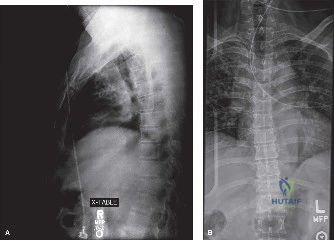
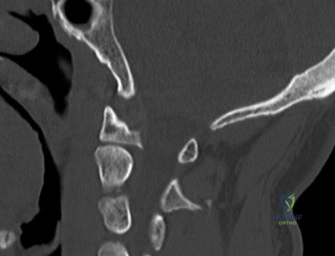
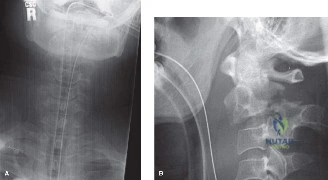
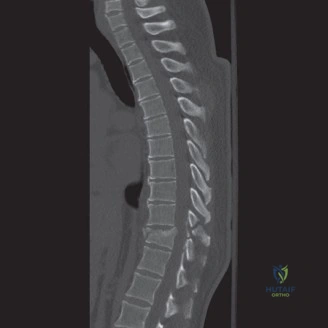
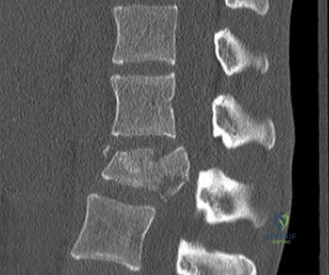
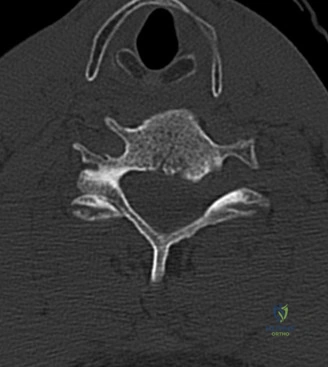
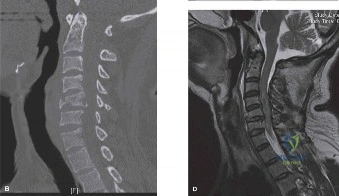
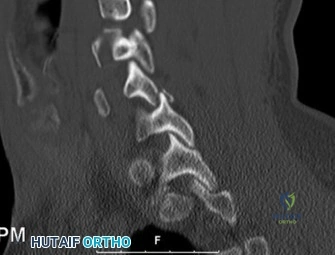
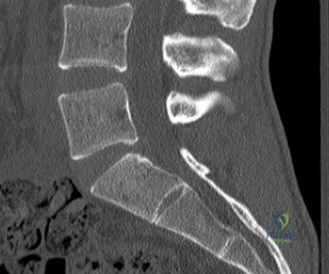
Initial trauma radiographs demonstrated a loss of anterior and middle column height at L1, with a focal kyphotic deformity. However, plain films are vastly insufficient for definitive surgical planning in thoracolumbar trauma. A high-resolution, fine-cut Computed Tomography (CT) scan of the entire spine was obtained. The CT images confirmed an L1 burst fracture with severe comminution of the vertebral body. Sagittal and axial reconstructions revealed 50% canal compromise secondary to a large retropulsed bone fragment originating from the posterosuperior aspect of the L1 vertebral body. Furthermore, the CT demonstrated 25 degrees of segmental kyphosis measured from the superior endplate of T12 to the inferior endplate of L1.
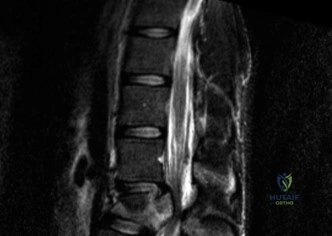
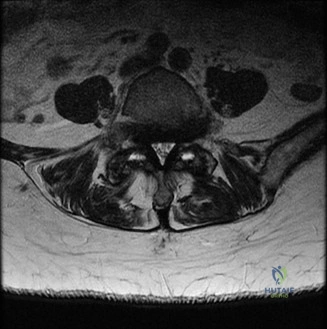
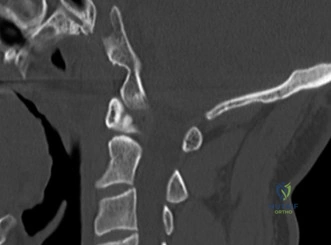
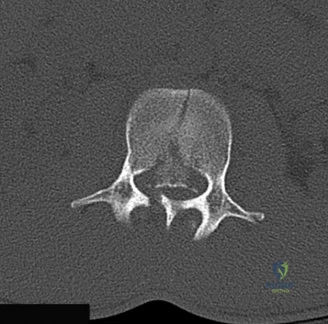
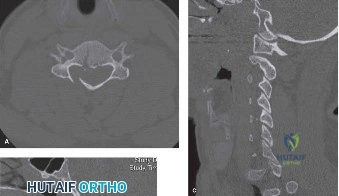
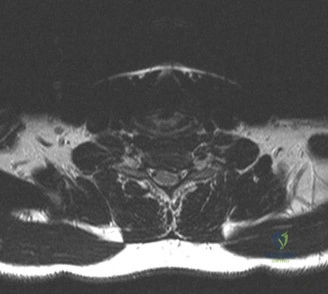
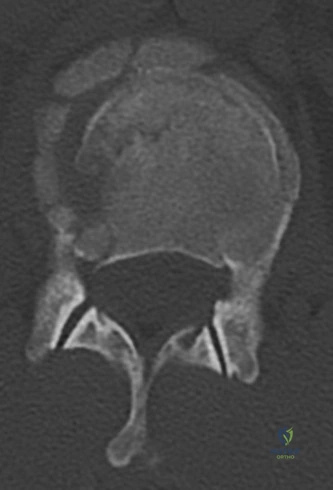
A critical finding on the axial CT slices was a vertical, split fracture propagating through the L1 lamina. This is a highly significant morphological feature. A lamina fracture in the setting of a burst fracture with retropulsion strongly correlates with a dural tear and potential entrapment of the cauda equina nerve roots. When the vertebral body bursts posteriorly, the pedicles are driven outward, and the lamina fractures as the spinal canal attempts to expand to accommodate the retropulsed bone. If the dura is lacerated, nerve roots can herniate through the dural defect and become incarcerated in the laminar fracture site.
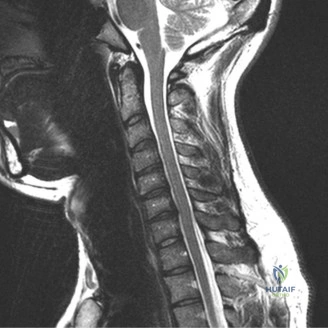
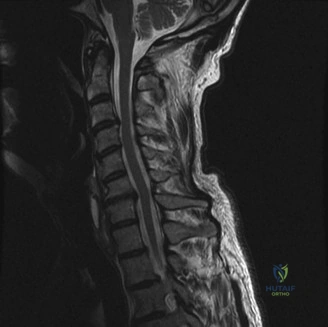
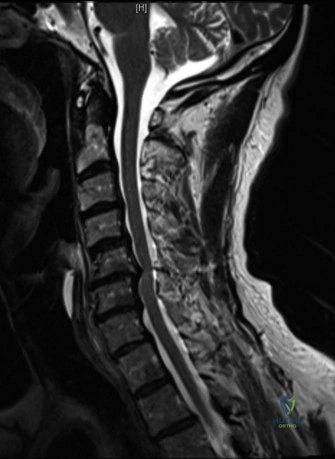
Magnetic Resonance Imaging and the Posterior Ligamentous Complex
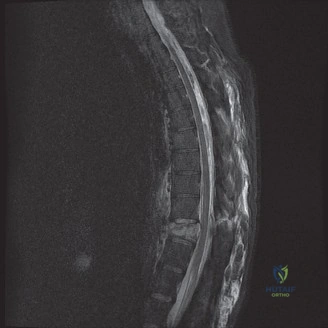
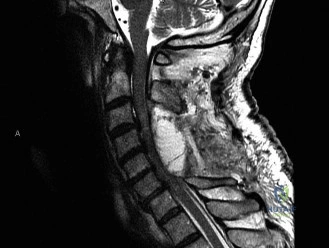
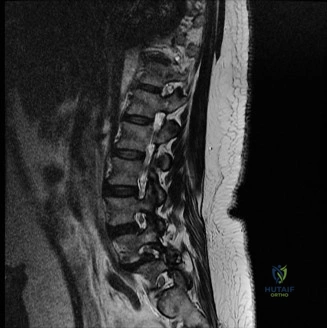
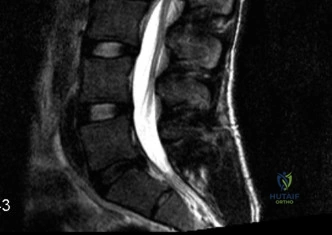
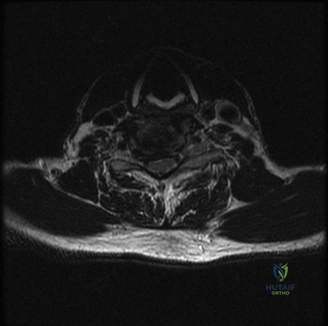
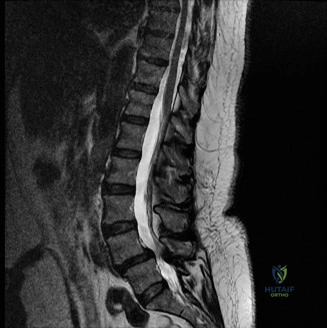
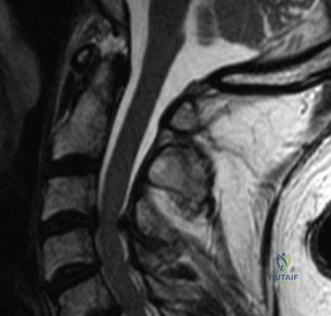
To definitively assess the integrity of the soft tissue stabilizers and the neural elements, a Magnetic Resonance Imaging (MRI) scan without contrast was performed. Historically, textbooks propagated the "50-50-25 rule," suggesting that a burst fracture was inherently unstable if it exhibited >50% canal compromise, >50% loss of vertebral body height, or >25 degrees of kyphosis. Modern spine trauma surgery has largely debunked this rigid radiographic dogma. We now understand that these bony metrics alone do not dictate mechanical instability. The true arbiter of stability is the Posterior Ligamentous Complex (PLC).
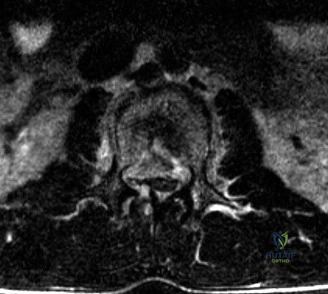
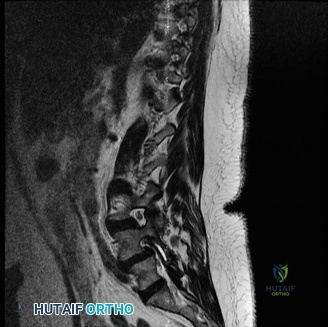
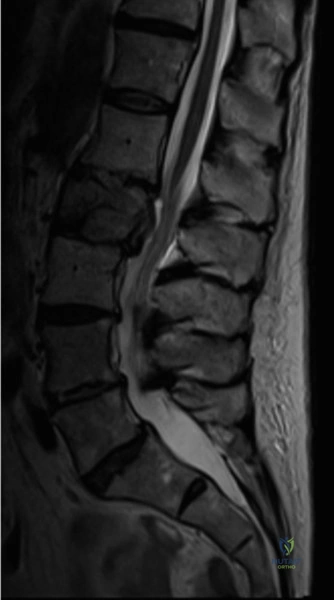
The MRI, particularly the Short Tau Inversion Recovery (STIR) and T2-weighted sagittal sequences, provided the definitive diagnosis. The images demonstrated profound hyperintensity and discontinuity of the ligamentum flavum, the interspinous ligaments, and the supraspinous ligaments at the T12-L1 level. The facet joint capsules were also disrupted, indicated by fluid within the joints. This complete failure of the PLC means the posterior tension band is gone. Regardless of the bony parameters, this spine cannot resist physiological flexion loads. If treated non-operatively, this injury will inevitably lead to progressive kyphosis, delayed neurological deficit, and intractable pain.
Screening for Noncontiguous Fractures
A frequently tested and clinically vital concept in spine trauma is the incidence of noncontiguous spinal fractures. When a patient presents with a primary spinal fracture, what is the rate of finding a second, separate fracture at a non-adjacent level? The literature reports this rate to be between 10% and 22%, with 15% being the most commonly cited average. This high incidence mandates that the entire neuroaxis—from the occiput to the sacrum—be imaged and scrutinized. In our patient, the whole-spine CT protocol ruled out any cervical or additional thoracic/lumbar fractures, but failing to screen the entire spine is a classic pitfall that leads to missed injuries and devastating outcomes.
Exhaustive Differential Diagnosis
When evaluating a thoracolumbar spinal injury, the differential diagnosis must be systematically categorized based on the mechanism of injury, the columns involved (Denis three-column theory), and the ultimate stability of the spine. The following table delineates the primary differential diagnoses considered for this patient.
| Diagnosis | Mechanism of Injury | Structural Involvement | Stability & Clinical Implications |
|---|---|---|---|
| Compression Fracture | Mild to moderate axial load with flexion. | Failure of the anterior column only. Middle and posterior columns remain intact. | Generally stable. Rarely associated with neurological deficits. Treated non-operatively with bracing and mobilization. |
| Burst Fracture (Stable) | Pure axial load. | Failure of anterior and middle columns. Posterior column (PLC) remains intact. | Potentially stable depending on morphology. If PLC is intact and patient is neurologically intact, can often be treated in a TLSO brace. |
| Burst Fracture (Unstable) | Axial load with significant flexion/rotation moment. | Failure of anterior, middle, and posterior columns (PLC disruption). | Our Patient's Diagnosis. Highly unstable. Loss of posterior tension band leads to progressive kyphosis. Requires surgical stabilization. |
| Flexion-Distraction (Chance) | Flexion around an anterior axis (e.g., lap belt injury). | Tension failure of posterior and middle columns; compression or hinge at anterior column. | Highly unstable in flexion. High association with intra-abdominal visceral injuries. Requires surgical stabilization (usually posterior compression construct). |
| Fracture-Dislocation | Massive shear, torsion, or translation forces. | Disruption of all three columns with translation or subluxation of the vertebral bodies. | Extremely unstable. Highest rate of complete neurological transection. Requires emergent surgical reduction and rigid multi-segmental fixation. |
Differentiating between a stable burst fracture and an unstable burst fracture is the crux of this case. The presence of 50% canal compromise and 25 degrees of kyphosis might tempt an inexperienced surgeon to operate based purely on radiographic appearance. However, as discussed, it is the MRI confirmation of the PLC disruption that shifts this diagnosis from a potentially non-operative stable burst to an unequivocally unstable injury requiring intervention.
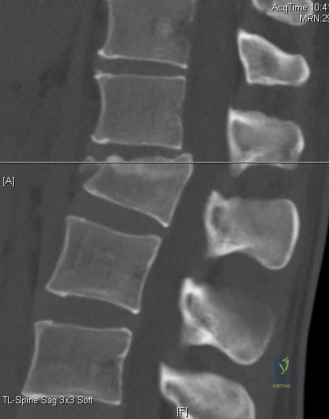
Furthermore, we must rule out a true flexion-distraction (Chance) injury. While our patient has posterior ligamentous disruption, a Chance fracture typically involves a bony or purely ligamentous horizontal split extending from posterior to anterior, often without the severe comminution and retropulsion seen in a burst fracture. Our patient's profound anterior and middle column comminution confirms the primary axial burst mechanism, augmented by a flexion moment that destroyed the PLC.
Complex Surgical Decision Making and Classifications
To standardize our decision-making, we utilize the Thoracolumbar Injury Classification and Severity (TLICS) score. This system evaluates three distinct categories: morphology of the injury, integrity of the posterior ligamentous complex, and neurological status. For our patient, the morphology is a burst fracture, yielding 2 points. The neurological status is intact, yielding 0 points. However, the MRI confirmed definitive disruption of the PLC, yielding 3 points. The total TLICS score is 5. A score of 4 or greater is a definitive indication for surgical intervention.
We also apply the AOSpine Thoracolumbar Classification System. This injury is classified as a Type A4 (complete burst fracture involving both endplates) combined with a Type B2 (posterior tension band disruption / bony or ligamentous failure). The presence of the B2 component dictates the need for posterior stabilization. The decision now pivots to the type of surgical intervention. Options include a custom-molded thoracolumbar orthosis (TLSO), anterior corpectomy and fusion, laminectomy without fusion, or instrumented posterior fusion.
Let us dissect these options. A TLSO is contraindicated; a brace cannot restore a disrupted posterior tension band, and the patient will inevitably collapse into severe kyphosis. Laminectomy alone is an absolute historical error; removing posterior bony elements in a spine that already has a disrupted PLC and a compromised anterior column will cause catastrophic, immediate iatrogenic destabilization. An anterior corpectomy and strut grafting is an excellent operation for clearing the canal, but it involves significant morbidity (thoracotomy/retroperitoneal approach) and does not directly address the primary posterior tension band failure.
Therefore, the gold standard, definitive treatment for this specific injury pattern is an instrumented posterior fusion. By placing pedicle screws above and below the fractured level, we can utilize ligamentotaxis to partially reduce the retropulsed fragment, restore vertebral height, and rigidly recreate the posterior tension band. This is where the concept of preventing Adjacent Segment Degeneration (ASD) enters our operative planning. If we fuse this patient in 25 degrees of segmental kyphosis, we will create a flatback deformity. The adjacent unfused segments (particularly L2-L3 and L3-L4) will be forced into hyperlordosis to compensate, leading to accelerated facet arthropathy, disc degeneration, and eventual adjacent segment failure. Our surgical goal is not just stabilization, but the meticulous restoration of regional sagittal alignment.

Step-by-Step Surgical Technique and Intervention
The patient is brought to the operating room and intubated on the stretcher. Total Intravenous Anesthesia (TIVA) is utilized to facilitate intraoperative neuromonitoring (Somatosensory Evoked Potentials and Motor Evoked Potentials). The patient is carefully log-rolled onto a radiolucent Jackson spinal table with chest and hip pads. Proper positioning is the first step in reduction; simply extending the hips and allowing the abdomen to hang free can induce lordosis and utilize the anterior longitudinal ligament to partially reduce the kyphotic deformity via ligamentotaxis.
A standard midline posterior approach is utilized, extending from T11 to L3 to allow for a "two-up, two-down" construct (T11, T12, L2, L3). Subperiosteal dissection is performed meticulously to expose the spinous processes, laminae, and transverse processes. Care is taken at the L1 level; given the known lamina fracture, the dissection here must be exceedingly gentle to avoid plunging into the spinal canal and injuring the dura or neural elements.
Pedicle screws are placed using anatomic landmarks and fluoroscopic guidance (or robotic/navigation assistance if available). At the thoracolumbar junction, the entry point is typically at the intersection of the pars interarticularis, the midpoint of the transverse process, and the lateral border of the superior articulating facet. We place 6.5mm or 7.5mm polyaxial pedicle screws at T11, T12, L2, and L3. We generally avoid placing screws into the fractured L1 pedicles unless the fracture pattern specifically allows for short-segment fixation with index-level screws, but in a highly comminuted A4 burst, bypassing the index level provides a more robust biomechanical construct.
Before rod placement, we must address the neural canal. Because of the lamina fracture and the 50% canal compromise, a direct posterior decompression (laminectomy) of L1 is performed. We carefully remove the fractured lamina. As suspected, a small dural tear is identified where the fractured bone edge lacerated the thecal sac. This is repaired primarily with 4-0 Nurolon and augmented with a dural sealant. By performing the laminectomy, we decompress the canal and remove the risk of nerve root entrapment during our subsequent reduction maneuvers.
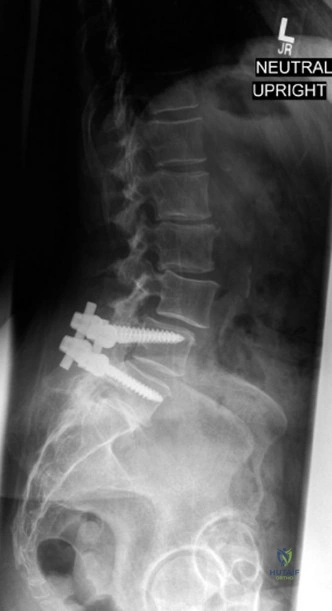
The final, critical step is rod contouring and reduction. To prevent future Adjacent Segment Degeneration, the titanium rods must be contoured to match the patient's ideal pelvic incidence and lumbar lordosis. The rods are seated into the proximal screws. Using reduction towers and careful cantilever forces, the rods are seated into the distal screws. This maneuver actively corrects the 25-degree kyphotic deformity, restoring normal sagittal alignment. The construct is cross-linked if necessary, and a robust posterolateral decortication and bone grafting (using local autograft from the laminectomy and allograft) is performed to ensure a solid arthrodesis.
Strict Post-Operative Protocol and Rehabilitation Stages
Post-operatively, the patient is transferred to the Surgical Intensive Care Unit for close neurological and hemodynamic monitoring. The head of the bed can be elevated, and the patient is allowed to log-roll immediately. Because we have achieved rigid internal fixation, a post-operative TLSO brace is generally not required, though some surgeons may utilize a soft corset for patient comfort and proprioceptive feedback.
Early mobilization is the key to preventing complications such as deep vein thrombosis, pulmonary embolism, and atelectasis. Physical and occupational therapy are consulted on post-operative day one. The patient is assisted out of bed and begins ambulation. Chemical DVT prophylaxis (e.g., low molecular weight heparin) is initiated 24 hours post-operatively, assuming no expansion of epidural hematoma is suspected and the dural repair is secure.
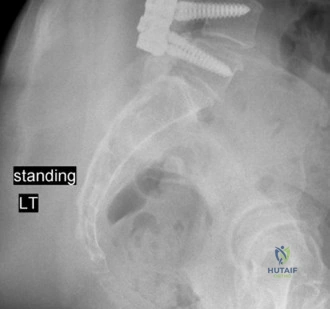
Radiographic follow-up includes upright AP and lateral plain films before discharge to verify the maintenance of sagittal alignment and hardware integrity. The patient is discharged home or to acute inpatient rehabilitation depending on their functional mobility.
Long-term follow-up at 6 weeks, 3 months, 6 months, and 1 year will focus on assessing fusion mass consolidation and monitoring for any signs of hardware failure. More importantly, long-term surveillance (2 to 5 years post-op) will focus on the adjacent segments. By having meticulously restored the sagittal vertical axis (SVA) and regional lordosis during the index procedure, we have minimized the abnormal shear and compressive forces on the T10-T11 and L3-L4 discs, drastically reducing the patient's risk of developing Adjacent Segment Degeneration requiring revision surgery.
High-Yield Clinical Pearls and Pitfalls
To synthesize this complex case, here are the high-yield takeaways that you must master for both your clinical practice and your board examinations:
- The 15% Rule: Always remember that the rate of noncontiguous spine fractures in high-energy trauma is approximately 15% (ranging from 10-22%). A complete radiographic survey of the entire spine is mandatory. Missing a secondary cervical fracture in a lumbar burst patient is a devastating, indefensible error.
- Death of the 50-50-25 Rule: Do not rely solely on plain radiographic parameters (50% canal compromise, 50% height loss, 25 degrees kyphosis) to determine stability. These metrics can exist in a stable spine.
- The PLC is Paramount: The true determinant of biomechanical stability in a thoracolumbar burst fracture is the integrity of the Posterior Ligamentous Complex. MRI is the gold standard for evaluating the interspinous ligaments, ligamentum flavum, and facet capsules.
- Lamina Fractures Predict Dural Tears: A vertical split fracture through the lamina in the setting of a burst fracture is highly correlated with dural lacerations and entrapped nerve roots. Proceed with extreme caution during posterior exposure and strongly consider a decompressive laminectomy before reduction.
- Sagittal Balance Prevents ASD: The primary long-term complication of thoracolumbar fusions is Adjacent Segment Degeneration. Treating the acute fracture is only half the battle; contouring your rods to restore normal lumbar lordosis and regional sagittal balance is the ultimate prophylactic measure against future adjacent segment failure.