Complex Intra-Articular Distal Humerus Fracture: Diagnostic & Surgical Challenges

Key Takeaway
Complex comminuted intra-articular distal humerus fractures are diagnosed through detailed clinical examination for pain, deformity, and neurovascular status. Imaging is critical: X-rays reveal fracture patterns, while CT scans with 3D reconstructions precisely delineate fragment size, displacement, articular involvement, and bone loss, guiding comprehensive pre-operative planning for these high-energy elbow traumas.
Patient Presentation and History
Good morning, everyone. Today, we'll delve into a complex elbow trauma case, focusing on the diagnostic and surgical challenges of a comminuted intra-articular distal humerus fracture.
Our patient is a 58-year-old right-hand dominant male who presented to the emergency department after a fall from a height of approximately 8 feet while working on a ladder. He landed directly on his outstretched right arm. He reported immediate, severe pain, inability to move his elbow, and noticeable deformity.
His medical history includes well-controlled hypertension and Type 2 Diabetes Mellitus, managed with oral hypoglycemics. He denies any history of osteoporosis or prior elbow injuries. He is an active, independent individual, working as a carpenter, which places significant functional demands on his upper extremities. He is a non-smoker and reports occasional alcohol consumption. The mechanism of injury suggests high-energy trauma, necessitating a thorough evaluation for associated injuries.
Clinical Examination
Upon presentation, the patient was in significant distress from pain.
- Inspection: The right elbow presented with gross swelling, significant ecchymosis extending proximally to the distal humerus and distally into the forearm. There was a palpable deformity around the elbow joint, particularly evident posteriorly. The skin overlying the joint was intact, without any open wounds, tenting, or signs of impending compartment syndrome.
- Palpation: Diffuse tenderness was elicited over the entire distal humerus, olecranon, and radial head. Palpation revealed crepitus with any attempt at passive motion, indicating significant bony disruption. The medial and lateral epicondyles were difficult to delineate due to swelling and comminution.
- Range of Motion (ROM): Both active and passive range of motion of the elbow were severely limited and exquisitely painful. The patient guarded against any movement. Attempts at gentle flexion and extension yielded only a few degrees of motion, and pronation/supination were similarly restricted.
- Neurological Assessment: A meticulous neurological examination was performed given the proximity of major nerves to the elbow joint. Sensation was intact to light touch in all dermatomes of the hand and forearm, including the median (thumb, index, middle finger radial aspect), ulnar (little finger, ring finger ulnar aspect), and radial nerve distributions (dorsal first web space). Motor function was difficult to assess accurately due to pain, but gross motor power for wrist flexion, extension, and finger movements appeared preserved. Specifically, intrinsic hand muscles (ulnar nerve) and wrist extensors (radial nerve) could be gently tested and showed no gross deficits. However, the ulnar nerve was identified as being particularly at risk in this type of injury, necessitating careful monitoring.
- Vascular Assessment: Radial and ulnar arterial pulses at the wrist were palpable, strong, and symmetrical compared to the contralateral limb. Capillary refill in all digits was brisk, less than 2 seconds. No signs suggestive of arterial compromise or evolving compartment syndrome were observed, although serial assessments were planned.
Imaging and Diagnostics
Following the initial clinical assessment, imaging studies were promptly obtained to characterize the injury.
- X-rays:
- Antero-posterior (AP) and lateral views of the elbow were the initial radiographs. These revealed a highly comminuted, intra-articular distal humerus fracture.
- The AP view demonstrated significant disruption of both the medial and lateral columns of the distal humerus, with a clear supracondylar component and extension into the trochlea and capitellum. The fracture line extended into the coronoid fossa and olecranon fossa.
- The lateral view showed posterior displacement and angulation of the distal fragments relative to the humeral shaft, establishing the presence of a complete articular disruption with a supracondylar extension.
Based on the plain radiographs, this injury is classified as an AO/OTA type 13C3 fracture, denoting a complete, multi-fragmentary articular and multi-fragmentary metaphyseal fracture. To adequately formulate a surgical plan, a fine-cut Computed Tomography (CT) scan with 3D reconstructions was obtained. The CT scan is critical for identifying coronal shear fragments of the capitellum and trochlea, assessing the exact degree of articular comminution, and determining the bone stock available for screw purchase in the distal fragments.
Introduction and Epidemiology
Distal humerus fractures account for approximately 2 to 6 percent of all fractures and nearly 30 percent of all elbow fractures. They present a bimodal epidemiological distribution. The first peak occurs in young males, typically resulting from high-energy trauma such as motor vehicle collisions, falls from height, or sports-related injuries. The second peak involves older females, usually secondary to low-energy falls on an outstretched hand, exacerbated by underlying osteopenia or osteoporosis.
The management of complex intra-articular distal humerus fractures remains one of the most demanding challenges in orthopedic trauma surgery. The primary objective is to restore an anatomically congruent articular surface, re-establish the structural relationship between the articular block and the humeral diaphysis, and achieve fixation stable enough to permit immediate postoperative mobilization. The elbow joint is notoriously unforgiving; prolonged immobilization invariably leads to debilitating arthrofibrosis. Therefore, the surgical construct must adhere to the principles of absolute stability for the articular surface and rigid fixation for the metaphyseal-diaphyseal junction.
Surgical Anatomy and Biomechanics
A profound understanding of distal humeral anatomy is a prerequisite for successful surgical reconstruction. The distal humerus can be conceptualized as a triangle or a "tie-arch" structure, consisting of a medial column, a lateral column, and the articular block (the "tie" that connects the two columns distally).
Osteology and Articular Geometry
The medial column diverges from the shaft at approximately 45 degrees and terminates at the medial epicondyle. It is non-articular and serves as the origin for the flexor-pronator mass and the medial collateral ligament (MCL). The lateral column diverges at approximately 20 degrees, terminating at the lateral epicondyle, providing the origin for the extensor-supinator mass and the lateral collateral ligament (LCL) complex.
The articular block is composed of the trochlea medially and the capitellum laterally. The trochlea is a spool-shaped structure covered by hyaline cartilage over 300 degrees of its surface, articulating with the greater sigmoid notch of the ulna. This deep, highly congruent ulnohumeral articulation is the primary stabilizer of the elbow. The capitellum is a hemispherical structure projecting anteriorly, articulating with the radial head to facilitate pronation and supination while sharing valgus loads.
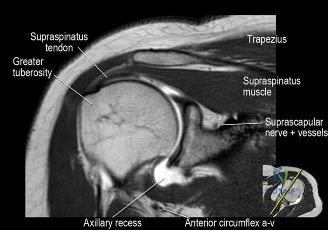
Neurovascular Proximity
The ulnar nerve courses posterior to the medial intermuscular septum and passes through the cubital tunnel, directly posterior to the medial epicondyle. It is at extreme risk during both the initial trauma and subsequent surgical exposure. The radial nerve pierces the lateral intermuscular septum approximately 10 centimeters proximal to the lateral epicondyle, transitioning from the posterior to the anterior compartment. Proximal extension of lateral column plating places the radial nerve at significant risk.
Biomechanical Considerations
Biomechanically, the elbow transmits significant forces. Even simple activities of daily living generate forces across the joint reaching up to three times body weight. The radiocapitellar joint absorbs approximately 60 percent of axial loads in full extension, while the ulnohumeral joint dominates load transfer in flexion. The surgical construct must neutralize bending, torsional, and axial sheer forces. The "tie-arch" must be rigidly reconstructed; failure to adequately secure the articular block to both columns results in catastrophic construct failure and nonunion.
Indications and Contraindications
The decision-making process for distal humerus fractures hinges on patient age, functional demands, bone quality, and fracture morphology. While open reduction and internal fixation (ORIF) is the gold standard for displaced fractures in physiologically active patients, alternative strategies must be considered for specific demographics.
| Management Strategy | Indications | Contraindications |
|---|---|---|
| Non-Operative Management | Truly non-displaced fractures (rare); Patients with severe medical comorbidities rendering them unfit for anesthesia; Severe dementia with inability to comply with rehabilitation. | Displaced intra-articular fractures; Open fractures; Vascular compromise; Floating elbow injuries. |
| Open Reduction and Internal Fixation | Displaced intra-articular fractures (AO/OTA Type B and C); Supracondylar fractures (AO/OTA Type A) with displacement; Open fractures; Concomitant neurovascular injury requiring exploration. | Extreme osteoporotic bone where stable fixation is impossible; Severe overlying soft tissue compromise (relative contraindication, may require staged management). |
| Total Elbow Arthroplasty | Elderly patients (>65 years) with severe comminution (Type C3) and osteoporotic bone; Pre-existing advanced elbow osteoarthritis or inflammatory arthropathy; Unreconstructible articular shear fractures in low-demand patients. | Young, high-demand patients; Active regional infection; Neuromuscular dysfunction (e.g., flail arm); Lack of adequate soft tissue coverage. |
Pre Operative Planning and Patient Positioning
Thorough preoperative planning is critical for minimizing intraoperative delays and ensuring optimal outcomes.
Templating and Equipment Selection
High-resolution CT imaging is utilized to map the fracture fragments. The surgeon must anticipate the need for specific implants, including anatomically pre-contoured distal humerus plates. Currently, both parallel and orthogonal plating systems are widely utilized. The choice often depends on fracture morphology; however, biomechanical studies suggest parallel plating offers superior resistance to torsional forces in highly comminuted bicolumnar fractures. Headless compression screws (ranging from 1.5 mm to 3.0 mm) must be available for osteochondral shear fragments.
Patient Positioning
The patient is typically placed in the lateral decubitus position, though the prone position is a viable alternative.
1. Lateral Decubitus: The patient is rolled onto the uninjured side. A beanbag is used for stabilization. The injured arm is draped free and placed over a padded post or an L-bar, allowing the elbow to flex past 90 degrees. This position affords excellent access to the posterior aspect of the elbow and allows gravity to assist with fracture reduction.
2. Tourniquet Application: A sterile high-arm tourniquet is applied to maximize the surgical field while maintaining hemostasis. The arm is exsanguinated, and the tourniquet is inflated to appropriate pressures (typically 250 mmHg).
Detailed Surgical Approach and Technique
Surgical reconstruction of a complex AO/OTA 13C3 fracture demands a systematic, step-wise approach. The overarching goal is "inside-out" reconstruction: first assembling the articular block, then rigidly securing this block to the humeral diaphysis.
Posterior Skin Incision and Superficial Dissection
A universal posterior midline incision is utilized. The incision begins approximately 10 cm proximal to the olecranon tip, curving slightly laterally around the olecranon to avoid placing the scar directly over the bony prominence, and extends 5 cm distally over the ulnar crest. Full-thickness fasciocutaneous flaps are elevated medially and laterally to protect the cutaneous vascular supply.
Ulnar Nerve Identification and Mobilization
The first critical deep step is the identification and protection of the ulnar nerve. The nerve is located proximally along the medial border of the triceps and traced distally into the cubital tunnel. The overlying Osborne's fascia and the arcuate ligament of the flexor carpi ulnaris (FCU) are divided. The nerve is mobilized circumferentially and protected with a vessel loop. Care must be taken to preserve the extrinsic longitudinal vascular supply to the nerve to prevent ischemic neuropathy. Whether the nerve is left transposed anteriorly or returned to the epicondylar groove at the end of the procedure remains a subject of debate, though anterior subcutaneous transposition is favored if the hardware impinges on the cubital tunnel.
Deep Surgical Approach and Osteotomy
For a highly comminuted C3 fracture, an olecranon osteotomy provides unparalleled exposure of the distal humeral articular surface.

A chevron-shaped osteotomy is preferred over a transverse osteotomy as it provides greater intrinsic stability and a larger surface area for healing.
1. The bare area of the greater sigmoid notch is identified.
2. A pre-drilled hole is created in the proximal ulna to facilitate later repair with a 6.5 mm or 7.3 mm partially threaded cancellous screw or a tension band construct.
3. An oscillating saw is used to initiate the apex-distal chevron osteotomy, stopping just short of the articular cartilage.
4. An osteotome is used to complete the cut through the subchondral bone and cartilage, creating a rough surface that interdigitates perfectly upon reduction.
5. The olecranon fragment, along with the attached triceps mechanism, is reflected proximally, exposing the entire distal humerus.
Articular Reconstruction and Provisional Fixation
The joint is cleared of hematoma and loose debris. The articular fragments (trochlea and capitellum) are identified, reduced anatomically, and provisionally stabilized with smooth Kirschner wires (K-wires). If coronal shear fragments are present, they are reduced and fixed using countersunk headless compression screws placed from anterior to posterior, or posterior to anterior, ensuring the screw heads do not violate the articular surface. The goal is to convert a complex C-type fracture into a simpler metaphyseal A-type fracture by recreating the "spool" of the distal humerus.
Bicolumnar Definitive Fixation
Once the articular block is reconstructed, it is reduced onto the humeral shaft. Provisional fixation is achieved with crossed K-wires. Definitive fixation requires dual plating.

The O'Driscoll principles of parallel plating are highly recommended for C3 fractures:
1. Every screw in the distal fragment should pass through a plate.
2. Screws should engage a fragment on the opposite side that is fixed to a plate.
3. As many screws as possible should be placed in the distal fragments.
4. Each screw should be as long as possible.
5. Screws should engage the subchondral bone of the articular fragments.
6. Plates should be applied to achieve compression at the supracondylar level.
7. The plates must be strong enough to resist bending forces.
Pre-contoured anatomical locking plates are applied to the medial and lateral columns. The medial plate is positioned on the medial ridge, curving around the medial epicondyle. The lateral plate is positioned directly laterally or slightly posteriorly on the lateral column. The construct is sequentially compressed. Locking screws are utilized in the distal articular block to provide fixed-angle stability, which is crucial in osteoporotic bone, while non-locking screws can be used in the diaphysis to draw the bone to the plate and achieve dynamic compression.
Finally, the olecranon osteotomy is reduced and secured using either a heavy intramedullary compression screw combined with a tension band wire, or a dedicated proximal ulna locking plate. The wound is irrigated, the ulnar nerve is addressed (transposed or left in situ), and the layers are closed meticulously over a suction drain.
Complications and Management
The surgical management of distal humerus fractures is fraught with potential complications. Anticipation, meticulous technique, and early recognition are paramount for minimizing morbidity.
| Complication | Estimated Incidence | Etiology and Pathophysiology | Prevention and Salvage Strategies |
|---|---|---|---|
| Ulnar Neuropathy | 10% - 25% | Direct trauma, intraoperative traction, hardware impingement, or postoperative perineural fibrosis. | Prevention: Meticulous exposure, avoiding excessive traction, prophylactic anterior transposition if hardware is prominent. Salvage: EMG/NCS evaluation; surgical neurolysis and submuscular transposition if symptoms persist. |
| Heterotopic Ossification (HO) | 5% - 15% | High-energy trauma, delayed surgery, traumatic brain injury, aggressive passive manipulation. | Prevention: Prophylactic Indomethacin or single-dose localized radiation in high-risk patients. Gentle tissue handling. Salvage: Surgical excision once the HO is mature (typically 6-12 months post-injury) and bone scans show decreased metabolic activity. |
| Nonunion / Implant Failure | 2% - 10% | Inadequate fixation rigidity, failure to restore the medial/lateral columns, poor bone stock, infection. | Prevention: Adherence to parallel plating principles, maximizing screw purchase in the articular block. Salvage: Revision ORIF with autologous bone grafting; conversion to Total Elbow Arthroplasty (TEA) in elderly patients. |
| Elbow Stiffness (Arthrofibrosis) | 15% - 30% | Prolonged postoperative immobilization, capsular contracture, articular incongruity. | Prevention: Rigid fixation allowing immediate active ROM. Avoidance of prolonged splinting. Salvage: Aggressive physical therapy, static progressive splinting; open or arthroscopic capsular release for refractory cases. |
| Olecranon Osteotomy Nonunion | 1% - 5% | Inadequate compression across the osteotomy site, thermal necrosis from the saw blade. | Prevention: Chevron osteotomy, robust tension band or plate fixation. Salvage: Revision fixation with bone grafting; excision of the proximal fragment and triceps advancement if the fragment is small. |
Post Operative Rehabilitation Protocols
The success of distal humerus fracture reconstruction is heavily dependent on the postoperative rehabilitation protocol. The primary goal is to prevent arthrofibrosis while protecting the osteosynthesis construct.
Phase I: Immediate Postoperative (Days 0-14)
The patient is placed in a well-padded posterior splint in 60 to 90 degrees of flexion immediately following surgery to allow for soft tissue rest and edema control. However, this splint is removed on postoperative day 2 or 3 to initiate physical therapy.
* Active and active-assisted range of motion (AAROM) for elbow flexion and extension is initiated under the guidance of a physical therapist.
* Pronation and supination exercises are also commenced.
* Passive stretching is strictly contraindicated during this phase to prevent heterotopic ossification and hardware failure.
* Gravity-assisted extension exercises are encouraged.
Phase II: Intermediate (Weeks 2-6)
Sutures are removed at two weeks.
* The patient progresses with active ROM.
* If extension is lagging, a dynamic or static progressive extension splint may be fabricated for nighttime use, provided the fracture fixation is deemed absolutely rigid.
* Strengthening exercises are avoided to prevent excessive stress on the metaphyseal-diaphyseal junction.
Phase III: Late Rehabilitation (Weeks 6-12+)
Radiographic evaluation is performed at 6 weeks to assess callus formation and fracture consolidation.
* Once clinical and radiographic signs of union are present, isometric strengthening is initiated, progressing to isotonic exercises.
* Maximum medical improvement regarding range of motion is typically achieved between 6 and 12 months postoperatively. A functional arc of motion (30 degrees of extension to 130 degrees of flexion) is the clinical target.
Summary of Key Literature and Guidelines
The evolution of distal humerus fracture management has been heavily influenced by robust biomechanical and clinical research.
The seminal work by O'Driscoll et al. fundamentally shifted the paradigm of fixation towards parallel plating. Their biomechanical studies demonstrated that parallel plates, linked by screws through the articular block, create an architecturally stable "arch" that is significantly more resistant to torsional and bending forces compared to traditional orthogonal (90-90) plating, particularly in the presence of supracondylar comminution. The AO/OTA guidelines now heavily emphasize these bicolumnar parallel plating principles for C-type fractures.
Conversely, clinical studies by Sanchez-Sotelo and the Mayo Clinic group have validated the use of pre-contoured orthogonal plating systems, showing excellent clinical outcomes when meticulous articular reduction and column compression are achieved. The consensus in contemporary literature is that both parallel and orthogonal constructs are clinically viable, provided the fundamental principles of stable bicolumnar fixation are respected.
For the elderly demographic, the Cobb and Morrey studies, alongside subsequent multicenter randomized trials (e.g., McKee et al.), have established Total Elbow Arthroplasty (TEA) as a primary treatment modality for displaced, comminuted distal humerus fractures in patients over 65 years of age. These studies demonstrate that TEA yields more predictable early functional outcomes and lower reoperation rates compared to ORIF in osteoporotic bone, where the risk of hardware failure and nonunion is unacceptably high.
In conclusion, the management of complex intra-articular distal humerus fractures remains a highly technical endeavor. Success requires precise preoperative planning, meticulous surgical execution utilizing advanced bicolumnar fixation techniques, and early, aggressive rehabilitation to restore functional elbow kinematics.
