How We Tackled Massive Bone Loss in a Revision Hip Arthroplasty
Key Takeaway
We review everything you need to understand about How We Tackled Massive Bone Loss in a Revision Hip Arthroplasty. A Paprosky IIIB defect signifies severe acetabular massive bone loss, typically seen in revision total hip arthroplasty. It's characterized by >3 cm superior migration of the hip center, significant ischial osteolysis exceeding 15mm, violation of Kohler's line, and obliteration of the teardrop. This complex defect often requires specialized reconstruction due to the extensive bony compromise.
Introduction and Epidemiology
Revision total hip arthroplasty in the setting of massive bone loss represents one of the most formidable challenges in adult reconstructive surgery. As the volume of primary total hip arthroplasty procedures continues to rise globally, coupled with expanding indications for younger, more active patients, the cumulative burden of revision arthroplasty is increasing proportionately. Massive bone loss in these scenarios is typically multifactorial, arising from particulate wear debris-induced osteolysis, aseptic loosening, recurrent instability, periprosthetic joint infection, periprosthetic fractures, or iatrogenic bone loss during the extraction of well-fixed primary components.
The epidemiology of revision hip arthroplasty indicates a shift toward more complex reconstructions. While early revisions are often necessitated by instability or infection, late revisions are predominantly driven by aseptic loosening and progressive osteolysis, which silently compromise the structural integrity of the acetabular columns and the femoral diaphysis. Managing these massive defects requires a comprehensive understanding of reconstructive options, ranging from highly porous metal augments and cup-cage constructs to modular fluted tapered stems and proximal femoral replacements. The primary goals remain consistent across all techniques: achieving rigid initial fixation, restoring the anatomic center of rotation, optimizing the abductor lever arm, and establishing a biological environment conducive to long-term host bone ingrowth or stable fibrous encapsulation.
Surgical Anatomy and Biomechanics
A profound understanding of the altered surgical anatomy and biomechanics in the multiply revised hip is paramount for achieving a successful outcome. Massive bone loss distorts standard anatomical landmarks, rendering conventional surgical navigation unreliable and increasing the risk of neurovascular injury.
Acetabular Considerations
The acetabulum is a hemispherical construct supported by the anterior and posterior columns, which converge at the superior dome. In the setting of massive bone loss, the superior dome and the medial wall are frequently compromised. The anterior column extends from the iliac wing to the pubic symphysis, while the posterior column extends from the sciatic notch to the ischial tuberosity.

Biomechanically, the native hip center of rotation is located approximately 15 to 20 millimeters superior to the teardrop and 30 millimeters lateral to Kohler’s line. Superior and lateral migration of the hip center—common in uncontained Paprosky Type III defects—dramatically increases joint reactive forces, diminishes the abductor moment arm, and predisposes the construct to accelerated wear, impingement, and dislocation. Restoration of the anatomic center of rotation is critical to normalize the biomechanical environment. When placing highly porous metal augments or custom triflange components, the surgeon must intimately understand the trajectory of the superior gluteal neurovascular bundle, which exits the sciatic notch and is at risk during superior screw placement, and the obturator neurovascular bundle, which is at risk during inferior dissection or screw placement into the ischium.
Femoral Considerations
The proximal femur relies on the integrity of the calcar, the greater trochanter, and the diaphyseal isthmus for load transfer. Massive femoral bone loss often eradicates the metaphyseal cancellous bone, precluding standard metaphyseal-engaging implants. Consequently, the biomechanical burden of fixation is transferred distally to the diaphyseal cortical bone.
The femoral isthmus provides the most reliable site for initial mechanical stability. Modular fluted tapered titanium stems rely on a scratch fit within this diaphyseal bone, utilizing longitudinal flutes to resist torsional forces and a tapered geometry to resist axial subsidence. The biomechanical principle of diaphyseal bypass dictates that the stem must achieve a minimum of 4 to 6 centimeters of scratch fit distal to the most distal defect or osteotomy site. Failure to achieve this bypass length exponentially increases the risk of early subsidence and mechanical failure. Furthermore, the preservation or reconstruction of the greater trochanter is essential for maintaining abductor tension; nonunion or migration of the trochanter severely compromises gait mechanics and increases dislocation risk.
Indications and Contraindications
The decision to proceed with complex revision arthroplasty for massive bone loss must be carefully weighed against the patient's physiological age, medical comorbidities, and functional demands.
| Clinical Scenario | Recommended Operative Strategy | Non Operative or Salvage Strategy |
|---|---|---|
| Aseptic Loosening with Paprosky IIIA Acetabular Defect | Hemispherical highly porous cup with superior augment. | Observation if asymptomatic and non-progressive. |
| Pelvic Discontinuity with Viable Host Bone | Cup-cage construct or custom triflange acetabular component (CTAC) with bone grafting. | Resection arthroplasty (Girdlestone) if medically unfit for prolonged surgery. |
| Paprosky IIIB Femoral Defect (Metaphyseal and Diaphyseal Loss) | Modular fluted tapered stem with extended trochanteric osteotomy (ETO). | Suppressive bracing (rarely effective), wheelchair mobilization if non-ambulatory. |
| Paprosky IV Femoral Defect (Extensive Diaphyseal Loss) | Proximal femoral replacement (megaprosthesis) or Allograft-Prosthesis Composite (APC). | Resection arthroplasty or amputation in extreme, unsalvageable cases. |
| Massive Bone Loss with Active Periprosthetic Joint Infection | Two-stage exchange: Explantation, antibiotic spacer, followed by definitive reconstruction. | Chronic antibiotic suppression or permanent resection arthroplasty. |
| Severe Medical Comorbidities (ASA IV) with Asymptomatic Osteolysis | Close radiographic surveillance. | Avoidance of surgery; activity modification. |
Contraindications to definitive single-stage reconstruction include active, uncontrolled periprosthetic joint infection, severe medical comorbidities precluding prolonged anesthesia, and inadequate soft tissue coverage. Relative contraindications include profound neurological deficits (e.g., severe Parkinson's disease or complete abductor paralysis) where the risk of recurrent instability may outweigh the benefits of reconstruction, prompting consideration for constrained liners or dual mobility bearings.
Pre Operative Planning and Patient Positioning
Meticulous preoperative planning is the cornerstone of successful revision arthroplasty. The complexity of massive bone loss dictates that the surgeon must anticipate multiple reconstructive scenarios and have the necessary modular implants, augments, and allograft materials available in the operating theater.
Clinical Evaluation and Imaging
The clinical evaluation must assess the patient's ambulatory status, leg length discrepancy, abductor strength, and neurovascular status. Previous operative notes and implant records are critical for identifying the existing components and planning for appropriate extraction tooling.
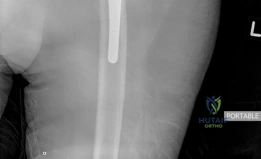
Radiographic evaluation begins with high-quality orthogonal views of the pelvis and the entire femur. However, plain radiographs consistently underestimate the true extent of osteolysis and bone loss. Therefore, a computed tomography (CT) scan with Metal Artifact Reduction Sequence (MARS) is mandatory for evaluating massive defects. CT imaging allows for precise quantification of remaining host bone, assessment of column integrity, and identification of pelvic discontinuity.

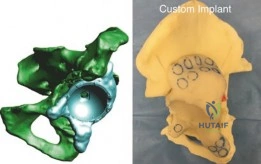
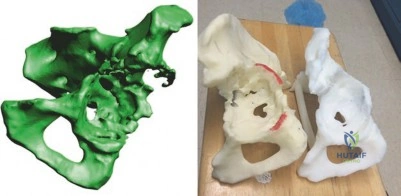
In cases of severe distortion, three-dimensional (3D) reconstruction and physical 3D-printed models are invaluable. These models facilitate tactile preoperative planning, allowing the surgeon to trial augment placement, determine the optimal trajectory for fixation screws, and design Custom Triflange Acetabular Components (CTAC) if standard modular options are deemed insufficient.
Classification Systems
Accurate classification of bone loss guides the reconstructive strategy. The Paprosky classification remains the most widely utilized system.
For the acetabulum:
* Type I: Minimal deformity, intact rim.
* Type II: Distorted hemisphere but intact columns (IIA: superior bone loss, IIB: superior and lateral, IIC: medial).
* Type III: Severe bone loss with compromised columns. Type IIIA features superior and lateral migration ("up and out") with an intact teardrop. Type IIIB features medial and superior migration ("up and in") with teardrop obliteration and high risk of pelvic discontinuity.
For the femur:
* Type I: Minimal metaphyseal loss.
* Type II: Extensive metaphyseal loss, intact diaphysis.
* Type IIIA: Metaphyseal loss, diaphyseal damage but >4 cm of intact isthmus for fixation.
* Type IIIB: Metaphyseal loss, diaphyseal damage with <4 cm of intact isthmus.
* Type IV: Extensive metaphyseal and diaphyseal loss, completely non-supportive isthmus.
Patient Positioning
The patient is typically placed in the lateral decubitus position on a radiolucent operative table. Rigid pelvic fixation using peg boards or specialized pelvic positioners is critical to maintain the anatomic orientation of the pelvis during aggressive reaming and component impaction. The operative field must be draped widely to allow for extensile approaches, including distal extension for a transfemoral approach or proximal extension for iliac wing exposure. Fluoroscopy must be readily available and easily positioned to confirm component alignment and diaphyseal engagement intraoperatively.
Detailed Surgical Approach and Technique
The execution of revision hip arthroplasty with massive bone loss requires a systematic, stepwise approach encompassing safe exposure, meticulous component extraction, aggressive debridement, and rigid reconstruction.
Surgical Approach and Exposure
While the direct anterior or anterolateral approaches can be utilized for selected revisions, the posterior approach is the workhorse for massive bone loss due to its extensile nature. The incision incorporates the previous surgical scar when possible, extending proximally toward the posterior superior iliac spine and distally along the femoral shaft.
The gluteus maximus is split in line with its fibers. The sciatic nerve must be identified and protected throughout the procedure, particularly in cases of medialized acetabular components or extensive scar tissue. A meticulous capsulectomy is performed to mobilize the proximal femur.
When dealing with well-fixed distal stems or severe proximal femoral deformity, an Extended Trochanteric Osteotomy (ETO) is frequently indicated. The ETO provides unparalleled, direct, extensile exposure to the acetabulum while facilitating the safe extraction of cemented or porous-coated stems. A controlled osteotomy is created from the posterior border of the greater trochanter, extending distally into the diaphysis. The length of the osteotomy is determined preoperatively, typically ranging from 12 to 15 centimeters, ensuring it bypasses the distal extent of the existing implant. The osteotomized fragment, retaining the insertions of the gluteus medius and vastus lateralis, is reflected anteriorly, preserving its vascular supply and ensuring a robust envelope for subsequent healing.
Acetabular Reconstruction Techniques
Following component extraction, the acetabulum is aggressively debrided of all fibrous tissue, granuloma, and particulate debris to expose bleeding host bone. The true extent of the defect is then assessed and compared to the preoperative Paprosky classification.
For Paprosky Type II and IIIA defects, hemispherical highly porous metal cups (tantalum or highly porous titanium) are the gold standard. These materials possess a high coefficient of friction, providing excellent initial scratch fit, and a high porosity that mimics cancellous bone, promoting rapid and extensive biological ingrowth. Reaming is performed to maximize contact with viable host bone, often requiring a "jumbo cup" technique.
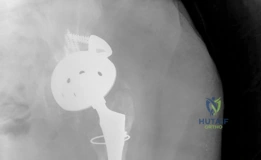
When superior or posterosuperior segmental defects preclude stable cup seating, highly porous metal augments are utilized. These augments are available in various shapes (e.g., buttress, shim, half-moon) and sizes. The defect is sequentially milled or reamed to match the geometry of the augment. The augment is then rigidly fixed to the host bone using multiple cancellous screws. The primary acetabular shell is subsequently impacted into the reconstructed cavity and cemented to the augment, creating a monolithic construct.
In the presence of Paprosky IIIB defects or pelvic discontinuity (a complete separation of the superior and inferior hemipelvis), the reconstructive complexity escalates significantly. The goal is to bridge the discontinuity and achieve stable fixation in both the ilium and the ischium/pubis.
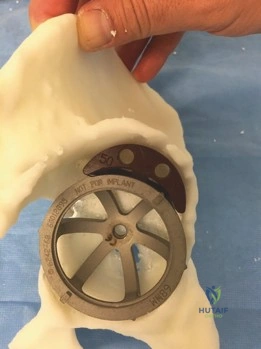
Options for pelvic discontinuity include:
1. Cup Cage Constructs: A highly porous hemispherical cup is impacted into the defect and fixed with screws. An ilioischial cage is then contoured and placed over the cup, spanning the discontinuity. The cage is secured to the ilium proximally and the ischium distally. A polyethylene liner is then cemented into the cage. This technique relies on the cage for immediate mechanical stability while allowing the underlying porous cup to achieve biological ingrowth.
2. Custom Triflange Acetabular Components (CTAC): For the most severe, uncontained defects where modular augments or cages are insufficient, a CTAC is designed based on the patient's preoperative CT scan. The implant features flanges that extend onto the ilium, ischium, and pubis, allowing for screw fixation into optimal host bone corridors. While highly effective, CTACs require significant lead time for manufacturing and are expensive.
3. Impaction Bone Grafting: In younger patients with cavitary defects, massive allograft impaction grafting combined with a cemented polyethylene cup and a supportive mesh can restore bone stock. However, this technique is technically demanding and carries a higher risk of early mechanical failure in massive uncontained defects.
Femoral Reconstruction Techniques
Femoral reconstruction is dictated by the integrity of the diaphysis. Once the acetabulum is reconstructed, attention turns to the femur.
For Paprosky Type II and IIIA defects, where the metaphyseal bone is absent but the diaphyseal isthmus is intact, modular fluted tapered titanium stems are the implant of choice. These stems feature a distally fluted geometry that engages the diaphyseal cortex, providing rotational stability, and a 2-to-3-degree taper that provides axial stability via a wedge effect.
The diaphysis is sequentially reamed until cortical chatter is achieved, indicating engagement of the dense cortical bone. The proximal body is then selected independently to restore leg length, offset, and version. This modularity is crucial for optimizing hip biomechanics independent of distal diaphyseal fixation. It is imperative that the stem achieves a minimum of 4 to 6 centimeters of scratch fit distal to any defect or the distal extent of an ETO to prevent subsidence.
For Paprosky Type IIIB defects, the isthmus is compromised, making diaphyseal engagement unpredictable. In these instances, longer, curved modular stems that bypass the deficient isthmus and engage the distal femoral metaphysis or even the epiphyseal scar may be required.
In the most extreme cases (Paprosky Type IV), where the entire proximal and mid-diaphyseal femur is destroyed, a proximal femoral replacement (megaprosthesis) is indicated. This involves resection of the compromised bone and replacement with a massive modular oncologic-style prosthesis. While this provides immediate stability and allows for early mobilization, it sacrifices host bone stock and relies entirely on the mechanical interface of the distal stem, carrying a higher long-term risk of aseptic loosening. An alternative is an Allograft-Prosthesis Composite (APC), where a structural proximal femoral allograft is utilized in conjunction with a long cemented or cementless stem. APCs theoretically restore bone stock and allow for biological reattachment of the abductor mechanism, but they are associated with high rates of allograft nonunion, resorption, and infection.
If an ETO was performed, it is reduced around the proximal body of the revision stem and secured using multiple heavy-duty cerclage cables. The cables must be tensioned appropriately to provide rigid fixation of the osteotomy fragment, facilitating osseous union while preventing trochanteric escape.
Complications and Management
Revision hip arthroplasty for massive bone loss is fraught with potential complications. The surgeon must be vigilant in both prevention and management.
| Complication | Estimated Incidence | Pathophysiology and Risk Factors | Management and Salvage Strategies |
|---|---|---|---|
| Dislocation and Instability | 10% - 25% | Abductor deficiency, altered center of rotation, incorrect component version, ETO nonunion. | Closed reduction. If recurrent, revision to a dual mobility bearing or constrained acetabular liner. Trochanteric advancement if abductors are avulsed. |
| Aseptic Loosening / Subsidence | 5% - 15% | Failure to achieve adequate distal diaphyseal scratch fit, inadequate bone grafting, biological failure of ingrowth. | Revision of the loose component. Use of larger diameter stems, longer diaphyseal bypass, or transition to proximal femoral replacement. |
| Periprosthetic Joint Infection (PJI) | 3% - 10% | Prolonged operative time, massive dead space, extensive soft tissue stripping, allograft use. | Acute: Debridement, antibiotics, and implant retention (DAIR). Chronic: Two-stage exchange arthroplasty with articulating spacer. |
| Intraoperative Periprosthetic Fracture | 4% - 12% | Aggressive diaphyseal reaming, impaction of oversized stems, osteoporotic host bone. | Bypass the fracture with a longer stem (minimum 2 cortical diameters distal). Supplement with cerclage cables or strut allografts. |
| Sciatic Nerve Palsy | 2% - 6% | Excessive lengthening, direct retractor trauma, hematoma compression, thermal injury from cement. | Remove compressive hematomas. Ankle-foot orthosis (AFO) for foot drop. Often requires prolonged observation; recovery is variable and often incomplete. |
| Extended Trochanteric Osteotomy Nonunion | 1% - 5% | Inadequate cable tension, devascularization of the fragment, premature weight-bearing. | Observation if asymptomatic. If associated with abductor weakness or instability, revision cable fixation with bone grafting. |
Instability remains the most frequent complication. The use of dual mobility articulations has significantly reduced the dislocation rate in complex revisions by increasing the jump distance and the effective head size. Constrained liners are reserved as a salvage option due to their restricted range of motion and higher risk of transmitting forces to the cup-bone interface, potentially leading to premature acetabular loosening.
Post Operative Rehabilitation Protocols
Rehabilitation following complex revision arthroplasty with massive bone loss must be highly individualized, balancing the need for early mobilization to prevent medical complications (e.g., deep vein thrombosis, pneumonia) with the necessity of protecting the tenuous mechanical fixation and allowing for biological ingrowth.
In cases where rigid initial fixation is achieved with highly porous metals and modular tapered stems, patients may be allowed touch-down weight-bearing (TDWB) or partial weight-bearing (PWB) for the first 6 to 8 weeks. Progression to full weight-bearing as tolerated (WBAT) is contingent upon radiographic evidence of early incorporation and the absence of subsidence.
If an Extended Trochanteric Osteotomy (ETO) was performed, active abduction is strictly prohibited for a minimum of 6 to 8 weeks to prevent displacement of the osteotomy fragment. Patients are instructed in passive and active-assisted range of motion exercises within a safe zone.
In extreme cases involving massive structural allografts or tenuous pelvic discontinuity reconstructions, strict non-weight-bearing status may be enforced for up to 12 weeks. Deep vein thrombosis prophylaxis is mandatory, typically utilizing low molecular weight heparin or direct oral anticoagulants, adjusted for the patient's renal function and bleeding risk.
Summary of Key Literature and Guidelines
The evolution of techniques for managing massive bone loss is well-documented in the orthopedic literature. A thorough understanding of these landmark studies is essential for evidence-based practice.
- Paprosky and Sporer (2003): The foundational texts detailing the Paprosky classification system for both acetabular and femoral defects. These studies established the algorithm linking specific defect patterns to reconstructive strategies, fundamentally shifting the paradigm from cemented allograft reconstructions to cementless, biologically active fixation.
- Berry et al. (Mayo Clinic Registry): Extensive long-term data on the survivorship of highly porous metal cups and augments. Their work demonstrated that trabecular metal components significantly reduce the rate of aseptic loosening in severe acetabular defects compared to traditional titanium mesh and structural allograft techniques.
- Richards et al. (Modular Tapered Stems): Biomechanical and clinical studies validating the use of modular fluted tapered titanium stems. The literature confirms that achieving a minimum of 4 cm of diaphyseal scratch fit is critical for preventing subsidence and achieving long-term survivorship in Paprosky IIIA and IIIB femoral defects.
- American Academy of Orthopaedic Surgeons (AAOS) Clinical Practice Guidelines: The AAOS emphasizes the necessity of preoperative MARS MRI or CT imaging for accurate defect assessment. Furthermore, recent consensus statements strongly advocate for the use of dual mobility bearings in revision scenarios with a high risk of instability, particularly when the abductor mechanism is compromised or an ETO has been utilized.
- DeBoer et al. (Pelvic Discontinuity): Landmark papers evaluating the efficacy of cup-cage constructs versus Custom Triflange Acetabular Components. The literature suggests that while cup-cages offer excellent mid-term results and intraoperative flexibility, CTACs provide superior long-term mechanical stability in the most severe, uncontained pelvic discontinuities, albeit at a higher cost and with requisite manufacturing delays.
