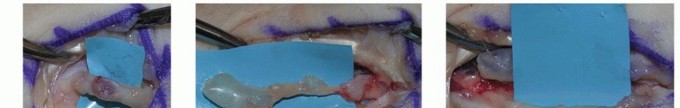
Operative Management of Nail Bed Pathologies and Tumors
Key Takeaway
Surgical management of nail unit pathologies requires a profound understanding of perionychial anatomy. This guide details evidence-based operative interventions for onychocryptosis, subungual exostosis, and nail bed neoplasms. Mastery of techniques such as chemical matrixectomy, wedge resection, and meticulous tumor excision ensures optimal functional outcomes while minimizing recurrence rates and iatrogenic nail dystrophy in orthopedic and podiatric practice.
Introduction to Nail Unit Pathologies
The surgical management of nail unit pathologies encompasses a broad spectrum of conditions, ranging from the ubiquitous onychocryptosis (ingrown toenail) to rare, limb-threatening malignancies such as subungual melanoma. A profound understanding of the perionychial anatomy, embryology, and biomechanics is paramount for the orthopedic surgeon. The nail unit is a complex appendage comprising the nail plate, nail bed (sterile matrix), germinal matrix, eponychium, paronychium, and hyponychium.
Historically, surgical interventions for nail pathologies were fraught with high recurrence rates and severe postoperative nail dystrophy. However, advancements in microsurgical techniques, chemical ablation, and a better understanding of the germinal matrix's role in nail genesis—pioneered by authors such as Zook, Hashimoto, and Lewis—have revolutionized the operative approach. This chapter details the evidence-based surgical management of common and neoplastic nail bed disorders.
Surgical Anatomy and Biomechanics of the Perionychium
To execute precise surgical interventions, the surgeon must master the microanatomy of the nail unit. The nail plate is a keratinized structure produced primarily by the germinal matrix, which extends proximally beneath the eponychial fold. The lunula, the visible white crescent at the base of the nail, represents the distal extent of the germinal matrix.
The sterile matrix lies distal to the lunula and is tightly adherent to the periosteum of the distal phalanx. While it does not contribute significantly to the longitudinal growth of the nail plate, it is responsible for the nail's adherence and adds a minor degree of thickness.
Clinical Pearl: Any surgical excision or trauma involving the germinal matrix will result in a permanent defect or absence of the corresponding longitudinal segment of the nail plate. Conversely, damage to the sterile matrix typically results in non-adherence of the nail plate (onycholysis) or localized deformity.
The vascular supply to the nail unit is robust, derived from the terminal branches of the proper palmar/plantar digital arteries, which form a rich anastomotic arcade within the superficial dermis. This vascularity explains the propensity for subungual hematomas following blunt trauma and necessitates meticulous hemostasis during tumor excisions.
Onychocryptosis (Ingrown Toenail)
Onychocryptosis is one of the most common pathologies encountered in foot and ankle surgery. It is characterized by the penetration of the lateral or medial edge of the nail plate into the adjacent paronychial soft tissue, leading to a cascade of inflammation, infection, and granulation tissue formation (hypertrophy of the unguilabia).
Etiology and Biomechanics
The etiology is multifactorial, encompassing improper nail trimming techniques, constricting footwear, hyperhidrosis, and underlying biomechanical abnormalities of the foot. Claeys (1983) demonstrated that altered ground reaction forces during pathological gait can exacerbate lateral pressure on the hallux, predisposing patients to recurrent onychocryptosis.
Indications for Operative Intervention
Conservative management (warm soaks, cotton wisp elevation, oral antibiotics) is reserved for mild, non-infected cases. Surgical intervention is indicated for:
* Recurrent onychocryptosis failing conservative measures.
* Presence of severe paronychia with abscess formation.
* Chronic granulation tissue with significant hypertrophy of the nail fold.
Surgical Techniques for Onychocryptosis
1. Partial Nail Avulsion with Chemical Matrixectomy (Phenolization)
Chemical matrixectomy using 88% phenol is the gold standard for recurrent ingrown toenails, offering a recurrence rate of less than 5% when performed correctly.
Surgical Steps:
1. Anesthesia and Preparation: Administer a digital block using 1% or 2% lidocaine without epinephrine. Apply a digital tourniquet (e.g., a Penrose drain) at the base of the toe to ensure a bloodless field, as blood deactivates phenol.
2. Nail Avulsion: Use a Freer elevator to separate the eponychium from the nail plate. Longitudinally split the offending border of the nail plate (approximately 2-3 mm wide) using an English anvil nail splitter or straight hemostat. Grasp the spicule with a hemostat and avulse it with a gentle rolling motion toward the midline to ensure the proximal matrix horn is removed intact.
3. Curettage: Vigorously curette the lateral matrix horn to remove any residual germinal tissue and granulation debris.
4. Phenol Application: Apply 88% phenol to the germinal matrix using a sterile cotton-tipped applicator. Massage the applicator into the matrix pocket for three consecutive applications of 30 to 60 seconds each.
5. Neutralization: Flush the area copiously with isopropyl alcohol to neutralize the phenol and wash away necrotic debris.
6. Closure: Release the tourniquet. Apply a non-adherent dressing and a mild compressive wrap.
Surgical Warning: Prolonged application of phenol or failure to thoroughly neutralize it can lead to severe chemical burns, periostitis, or delayed wound healing. Ensure the tourniquet is fully released prior to final dressing application.
2. Wedge Resection (Winograd Procedure)
Originally described by Winograd in 1929, this technique involves the surgical excision of the offending nail border, the underlying matrix, and the hypertrophic paronychial tissue. It is particularly useful when severe hypertrophy of the nail fold is present.
Surgical Steps:
1. Following digital block and exsanguination, make a longitudinal incision through the nail plate and bed, approximately 3 mm from the affected margin, extending proximally through the eponychium.
2. Make a second elliptical incision in the hypertrophic paronychial skin, connecting proximally and distally with the first incision to create a wedge.
3. Excise the wedge of tissue en bloc down to the periosteum of the distal phalanx. It is critical to visually confirm the complete removal of the germinal matrix horn.
4. Suture the remaining paronychial skin to the edge of the nail plate/bed using interrupted 3-0 or 4-0 non-absorbable sutures.
Subungual Exostosis
Subungual exostosis is a benign osteocartilaginous tumor that typically arises from the dorsomedial aspect of the distal phalanx, most commonly in the hallux. It presents as a painful, firm subungual mass that elevates the nail plate, often leading to secondary onycholysis and ulceration.
Surgical Excision
The definitive treatment is surgical excision. The approach depends on the location and size of the lesion.
* Direct Transungual Approach: If the nail plate is already detached or severely deformed, partial or total nail avulsion is performed. A longitudinal incision is made directly over the exostosis through the sterile matrix. The exostosis is excised flush with the normal contour of the distal phalanx using a rongeur or a small osteotome. The sterile matrix is then meticulously repaired with 6-0 absorbable sutures to prevent postoperative nail deformity.
* Fish-Mouth (Periungual) Approach: For distally located lesions, a transverse incision is made at the hyponychium. The sterile matrix is elevated dorsally, and the exostosis is resected. This approach preserves the integrity of the nail bed.
Neoplasms of the Nail Unit
Tumors of the nail unit, though relatively rare, require a high index of suspicion. Benign lesions include glomus tumors, periungual fibromas (often associated with tuberous sclerosis), and pyogenic granulomas. Malignant lesions include squamous cell carcinoma and subungual melanoma.
Glomus Tumors
Glomus tumors are benign hamartomas of the neuromyoarterial glomus body, responsible for thermoregulation. They classically present with a triad of symptoms: severe paroxysmal pain, pinpoint point tenderness (Love's pin test), and cold hypersensitivity. MRI is the imaging modality of choice for preoperative localization.
Subungual Melanoma and the Hutchinson Sign
Subungual melanoma is a rare but highly lethal malignancy, accounting for a significant percentage of melanomas in patients with darker skin phototypes. It often presents as a longitudinal melanonychia (a pigmented band in the nail plate).
A pathognomonic clinical feature of subungual melanoma is the Hutchinson sign, defined as the extension of periungual pigmentation onto the proximal or lateral nail folds (eponychium or paronychium).
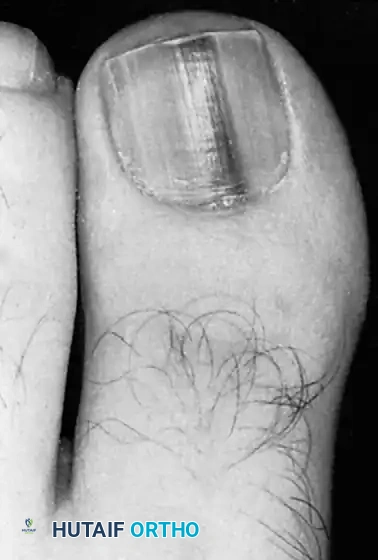
Fig. 84-31 Hutchinson sign. Band of pigmented tissue associated with subungual melanoma. (From Tomczak RL: Embryology of the nail unit. In Myerson MS, ed: Foot and ankle disorders, Philadelphia, 2000, Saunders; courtesy of Elvin Zook, MD.)
Clinical Pearl: Any new, widening, or heterogeneously pigmented longitudinal melanonychia, especially in a single digit of an adult, mandates a full-thickness biopsy of the nail matrix to rule out melanoma.
Surgical Technique 84-14: Excision of Subungual Neoplasms
The following technique details the meticulous excision of a subungual tumor (such as a glomus tumor or a localized benign neoplasm). The primary goals are complete tumor extirpation, preservation of the nail matrix, and minimization of postoperative nail dystrophy.
Preoperative Preparation
- Anesthesia: Administer a comprehensive digital block using a long-acting local anesthetic (e.g., 0.5% bupivacaine mixed with 1% lidocaine).
- Exsanguination: Exsanguinate the digit using an Esmarch bandage or a sterile glove finger cut at the tip.
- Tourniquet: Apply a digital tourniquet at the base of the digit. A completely bloodless field is absolute mandatory; even a single drop of blood can obscure a small glomus tumor or the delicate margins of the germinal matrix.
Surgical Approach and Excision
- Nail Plate Management: Depending on the tumor's location, perform either a partial or total nail plate avulsion. Use a Freer elevator to gently separate the nail plate from the underlying sterile and germinal matrix.
- Matrix Incision: For tumors located beneath the sterile matrix, make a longitudinal incision directly over the mass. If the tumor is beneath the proximal nail fold (germinal matrix), make bilateral oblique incisions at the corners of the eponychium to reflect the proximal nail fold dorsally, exposing the germinal matrix.
- Tumor Extirpation:
- Excise the tumor (which usually is well encapsulated) with a small knife (e.g., a #15 or #67 Beaver blade) or a fine curet.
- Utilize surgical loupe magnification (minimum 2.5x to 3.5x) to ensure complete removal of the capsule while sparing the surrounding healthy matrix tissue.
- For glomus tumors, inspect the bony floor of the distal phalanx; occasionally, the tumor causes pressure erosion into the bone, requiring gentle curettage of the bony crater.
Hemostasis and Closure
- Tourniquet Release: Release the digital tourniquet prior to closure to identify any active bleeding vessels.
- Hemostasis: Control bleeding with bipolar electrocautery.
> Surgical Warning: Strictly avoid the use of monopolar electrocautery within the nail bed. Monopolar energy causes widespread thermal necrosis to the delicate matrix cells, virtually guaranteeing severe, irreversible postoperative nail dystrophy. - Wound Closure:
- Carefully reapproximate the edges of the nail bed (sterile or germinal matrix) using 6-0 absorbable sutures (e.g., chromic gut or Vicryl Rapide) on a spatulated micro-needle.
- Close the external wound (eponychial fold or paronychial skin margins) in one layer with nylon interrupted suture.
- Nail Plate Replacement: If the avulsed nail plate is intact and free of disease, it can be cleaned, fenestrated (to allow hematoma drainage), and reinserted into the eponychial fold. This acts as a biological splint, maintains the eponychial space, and reduces postoperative pain. Secure the nail plate with a single distal suture or Steri-Strips.
Postoperative Management and Protocols
Meticulous postoperative care is essential to ensure optimal healing and prevent complications such as infection or recurrence.
- Immediate Postoperative Care: Apply a non-adherent dressing (e.g., Adaptic or Xeroform) directly over the surgical site, followed by sterile gauze and a mildly compressive cohesive bandage. The patient must keep the extremity strictly elevated above heart level for the first 48 to 72 hours to minimize throbbing pain and edema.
- Wound Care: The initial dressing is typically removed at 48 to 72 hours. Patients are instructed to perform daily warm water and Epsom salt soaks (if chemical matrixectomy was performed) or to keep the wound clean and dry (if primary closure was utilized).
- Suture Removal: Nylon sutures used for skin closure are removed at 10 to 14 days postoperatively. Absorbable sutures in the nail bed are left to dissolve.
- Return to Activity: Patients may bear weight as tolerated in a rigid-soled postoperative shoe immediately following surgery. Return to normal footwear and athletic activities is generally permitted within 2 to 4 weeks, depending on the extent of the resection and wound healing.
Complications
Complications following nail bed surgery include:
1. Recurrence: The most common complication of onychocryptosis surgery, usually due to inadequate removal or incomplete chemical ablation of the lateral matrix horn.
2. Infection: Postoperative paronychia requires prompt treatment with oral antibiotics covering skin flora (e.g., Cephalexin) and local wound care.
3. Nail Dystrophy: Iatrogenic damage to the germinal matrix, excessive thermal injury, or failure to accurately repair the sterile matrix can lead to split nails, pterygium formation, or complete loss of the nail plate.
4. Epidermal Inclusion Cysts: Can occur if fragments of the nail matrix or epithelium are buried within the soft tissue during closure.
You Might Also Like