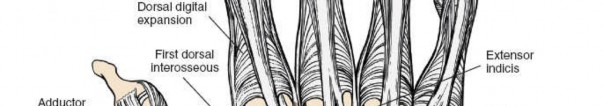
Perioperative Optimization in Hand Surgery: Antibiotic Stewardship, Operating Room Ergonomics, and Surgical Execution
Key Takeaway
Surgical site infections in hand surgery are rare but potentially devastating. Recent large-scale prospective and retrospective studies demonstrate that routine perioperative antibiotic prophylaxis does not significantly reduce infection rates, even in high-risk patients or complex cases. Optimizing operating room ergonomics, establishing standardized surgical routines, and ensuring precise assistant positioning are far more critical for minimizing intraoperative complications and maximizing surgical efficiency.
PERIOPERATIVE OPTIMIZATION IN HAND SURGERY
The successful execution of complex hand and upper extremity surgery relies on a foundation of meticulous perioperative planning, strict adherence to evidence-based protocols, and the optimization of the surgical environment. While the technical prowess of the surgeon is paramount, systemic factors—such as the rational use of perioperative antibiotics and the ergonomic arrangement of the operating room—profoundly influence patient outcomes. Disorganization, fatigue, and outdated clinical dogmas diminish the efficiency of the operating team and compromise surgical precision.
This comprehensive guide delineates the current evidence regarding perioperative antibiotic prophylaxis in hand surgery, establishes gold-standard protocols for operating room ergonomics, and details the execution of fundamental surgical approaches facilitated by optimal team dynamics.
EVIDENCE-BASED PERIOPERATIVE ANTIBIOTIC PROTOCOLS
Although surgical site infections (SSIs) are statistically rare following elective hand surgery, a postoperative infection in this anatomically dense region can be a disastrous complication. The complex interplay of synovial sheaths, fascial spaces, and poorly vascularized structures (such as tendons and articular cartilage) means that even a superficial infection can rapidly progress to deep space infection, tenosynovitis, or osteomyelitis. Such complications cause severe impairment of hand function, drastically delay rehabilitation, and often preclude a timely return to work. Severe infections frequently necessitate multiple surgical debridements and can result in permanent, irreversible biomechanical damage to the hand.
Despite these catastrophic risks, the routine use of perioperative antibiotics for many orthopaedic procedures in the hand remains highly questionable and is increasingly discouraged by modern antibiotic stewardship programs.
Analysis of Current Literature
The paradigm of administering prophylactic antibiotics for all hand surgeries has been challenged by robust clinical data. Two landmark series provide definitive guidance on this issue:
- The Retrospective Cohort (8,850 Patients): A massive retrospective analysis evaluated the efficacy of prophylactic antibiotics across a broad spectrum of hand procedures. The study found absolutely no significant difference in the frequency of surgical site infections between patients who received perioperative antibiotics and those who did not. Crucially, this lack of efficacy persisted even in designated "high-risk" cohorts, including active smokers, patients with poorly controlled diabetes mellitus, and cases involving prolonged operative times.
- The Prospective Randomized Trial (1,340 Patients): A rigorously controlled prospective study corroborated the retrospective findings. It demonstrated no statistically significant difference in infection rates based on antibiotic administration. Furthermore, the study stratified patients by surgical variables and found no difference in infection rates between elective and emergency surgeries, between operations lasting less than 2 hours and those lasting longer, or even between "clean" wounds and "crush/dirty" wounds.
Clinical Pearl: Antibiotic Stewardship
The authors of both major studies, supported by evolving guidelines from the American Society for Surgery of the Hand (ASSH), conclude that antibiotic prophylaxis should not be routinely administered for standard surgery of the hand. Prophylaxis should be strictly reserved for specific, evidence-based indications such as open fractures, human or animal bites, gross purulence, or the implantation of massive foreign bodies (e.g., total wrist arthroplasty), rather than applied as a blanket protocol.
ARRANGEMENT AND ROUTINE IN THE OPERATING ROOM
Because surgical results in the hand depend considerably on the skill, judgment, and precise microscopic work of the surgeon, it is imperative to keep intraoperative distractions to an absolute minimum. Disorganization, physical fatigue, and procedural uncertainty rapidly diminish the efficiency of the operating team and increase the risk of iatrogenic injury.
It is critical for the operating surgeon to establish a standard, unwavering routine that is followed regularly. When a standardized workflow is established, each surgical assistant, scrub nurse, and anesthesiologist can depend on this routine. The activities of the assistants should never be disrupted by the surgeon with irregular, unexpected, or inconsistent demands. A standard routine makes it possible for assistants to anticipate what is expected of them at each micro-step in the operation, allowing them to perform without hesitation, delay, or wasted motion.
The Psychological and Auditory Environment
The operating room should always be maintained as a pleasant, highly focused environment—often referred to as the "sterile cockpit."
With the increasing popularity of Wide Awake Local Anesthesia No Tourniquet (WALANT) techniques, many hand surgery patients are fully conscious during the procedure. If a local or regional anesthetic is being used and the patient is awake, loud noises, dropping of instruments, inappropriate bursts of conversation, or expressions of surgical frustration may severely alarm the patient and must be strictly avoided. Conversely, playing background music of the patient’s choosing has been shown to be highly comforting, reducing intraoperative hypertension and anxiety.
Preoperative Planning and Equipment Standardization
Efficiency on the day of surgery begins weeks in advance. If a complex surgical procedure is being arranged, the surgeon must communicate specific requests regarding special needs to the operating room staff well ahead of time.
- Instrumentation: Advance arrangements for specific micro-instruments, specialized sutures (e.g., 4-0 to 6-0 non-absorbable core sutures for tendon repair), the operating microscope, and specific osteosynthesis implants are mandatory.
- Imaging: Radiology support, including the use of mini C-arm fluoroscopy, must be arranged beforehand. The C-arm should be positioned to enter the field perpendicular to the hand table without disrupting the surgeon's seated position.
- Instrument Tray: The tray holding the basic instruments is typically placed on a Mayo stand or a shelf extending from the operating table, perfectly level with the working surface. The instruments must always be arranged in the exact same order. This standardized spatial arrangement allows the surgeon to develop muscle memory, saving critical time by routinely reaching for instruments without having to look away from the operative field or the microscope.
Surgeon Ergonomics and Biomechanics
Microsurgery and intricate hand surgery require the elimination of physiologic tremor. This is achieved through strict adherence to ergonomic principles.
The operating surgeon usually sits on a firm, comfortable, and highly stable stool, though they may occasionally stand for procedures requiring significant axial force (e.g., reaming a radius).
- Posture: When sitting, the surgeon’s knees should be almost level with the hips, and the feet must rest flat on the floor without strain. The back should be comfortably erect to prevent cervical and lumbar radiculopathy over a long career.
- Arm Support: The working surface of the operating hand table must be exactly at elbow height. This provides a comfortable, solid support for the forearms, which is the primary mechanism for eliminating resting tremor during microvascular anastomosis or nerve coaptation.
- Lighting: Illumination is critical. When the overhead surgical light is directed from above the surgeon’s left shoulder (for a right-handed surgeon), it shines directly onto the operative field, effectively eliminating shadows cast by the surgeon's own hands or instruments.
- Positioning Relative to the Patient: For most procedures, the surgeon should sit on the axillary side of the involved extremity. This allows the anatomy of either the right or left hand to be viewed in the same relative anatomical position, preserving the surgeon's spatial orientation. Some procedures on the dorsum of the hand and wrist (e.g., dorsal wrist ganglion excision or distal radius plating) may be performed more easily from the cephalic side.
Surgical Warning: Anatomical Disorientation
If the surgeon changes sides (moving from the axillary to the cephalic side of the arm board), it is critical to consciously acknowledge the 180-degree change in visual perspective to avoid catastrophic anatomical disorientation, particularly regarding the relationship of neurovascular bundles to flexor tendons.

The Role and Positioning of the Surgical Assistant
The surgical assistant is the unsung hero of complex hand surgery. Seated directly opposite the surgeon, the assistant must view the operative field from a vantage point 8 to 10 cm higher than the surgeon. This height differential allows the assistant a clear line of vision into the wound without having to bend forward, which would obstruct the surgeon’s view or block the overhead lighting.
Although mechanical hand holders (e.g., lead hands or specialized retractor systems) are commercially available, they cannot dynamically respond to the shifting needs of the procedure and are never as effective as a motivated, well-trained human assistant.
The primary duty of the assistant is to hold the patient’s hand absolutely stable, secure, and motionless. By applying precise counter-tension and retracting the adjacent digits, the assistant provides the surgeon with unimpeded access to the operative field.
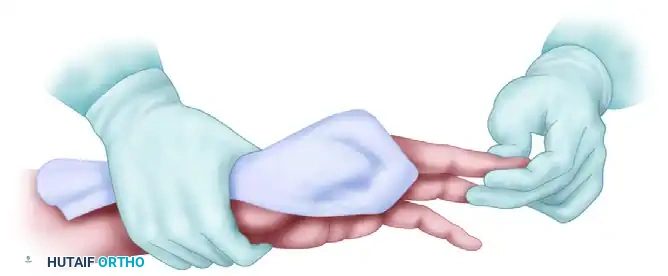
SURGICAL APPROACHES: THE MIDLATERAL DIGITAL INCISION
To illustrate the critical interplay between surgeon ergonomics, assistant positioning, and surgical execution, we examine the midlateral digital incision—a workhorse approach for accessing the flexor tendon sheath, digital nerves, and phalanges without causing volar scar contractures.
Indications
- Flexor tendon repair or tenolysis.
- Digital nerve and artery repair.
- Drainage of flexor tenosynovitis.
- Excision of volar or lateral digital masses.
Step-by-Step Surgical Execution
- Positioning and Retraction: As demonstrated in the ergonomic setup, the assistant grasps the patient's hand, holding the target digit in extension while gently flexing and retracting the adjacent digits out of the surgical field. The assistant's grip must be firm but atraumatic, ensuring the digit does not rotate during the incision.
- Landmark Identification: The surgeon identifies the dorsal and volar flexion creases of the interphalangeal joints. The midlateral line connects the apices of the flexion creases when the finger is fully flexed.
- The Incision: Using a #15 blade, the surgeon makes a longitudinal incision exactly along the midlateral line. The incision must remain dorsal to the volar flexion creases to prevent postoperative flexion contractures.
- Superficial Dissection: The skin is incised down to the subcutaneous fat. The surgeon must immediately identify and preserve the dorsal sensory branches of the digital nerve.
- Deep Dissection (Cleland's and Grayson's Ligaments):
- Grayson’s ligaments (volar to the neurovascular bundle) are carefully divided.
- The neurovascular bundle (digital artery and nerve) is identified and gently retracted volarly using a Ragnell or Senn retractor held by the assistant.
- Cleland’s ligaments (dorsal to the neurovascular bundle) are preserved if possible, or divided if deeper access to the phalanx is required.
- Exposure of the Flexor Sheath: With the neurovascular bundle safely retracted volarly, the surgeon has direct, unimpeded access to the flexor tendon sheath, the cruciform and annular pulleys, and the volar aspect of the phalanges.
Pitfall: Neurovascular Injury
The most common error during a midlateral approach is placing the incision too volarly, directly over the neurovascular bundle. Always err slightly dorsal to the apices of the flexion creases, and ensure the assistant maintains strict rotational control of the digit so the anatomical landmarks remain true.
POSTOPERATIVE PROTOCOLS AND REHABILITATION
The success of hand surgery extends far beyond the operating room. Postoperative protocols must be as rigorously standardized as the intraoperative routine.
- Immediate Postoperative Care: The hand should be dressed with a non-adherent contact layer, followed by fluffed gauze to accommodate postoperative swelling. A well-padded volar or dorsal orthosis is applied depending on the structures repaired (e.g., dorsal blocking splint for flexor tendon repairs).
- Elevation: The patient must be instructed to keep the hand elevated strictly above the level of the heart for the first 48 to 72 hours to minimize edema, which is the primary enemy of hand rehabilitation.
- Infection Monitoring: Despite the omission of routine prophylactic antibiotics, the surgical site must be monitored for signs of pathological erythema, disproportionate pain, or purulent drainage.
- Early Mobilization: Under the guidance of a certified hand therapist (CHT), early protected mobilization protocols (such as early active motion for tendon repairs) should be initiated within 3 to 5 days postoperatively to prevent restrictive adhesion formation and ensure the restoration of optimal hand biomechanics.
You Might Also Like