Percutaneous Distal Metatarsal Osteotomy: Surgical Technique & Evidence
Key Takeaway
The percutaneous distal metatarsal osteotomy is a minimally invasive technique for correcting mild to moderate hallux valgus. By utilizing a specialized micromotorized burr and fluoroscopic guidance, surgeons can achieve extra-articular deformity correction with minimal soft tissue disruption. While proponents cite rapid recovery and high union rates, careful patient selection is paramount due to reported risks of osteonecrosis and malunion. This guide details the precise surgical steps, biomechanical principles, and postoperative protocols.
Comprehensive Introduction and Patho-Epidemiology
The evolution of foot and ankle surgery has undergone a radical paradigm shift over the last two decades, moving progressively toward minimally invasive surgery (MIS). At the forefront of this revolution is the percutaneous distal metatarsal osteotomy (PDMO), a specialized, technically demanding procedure designed to correct hallux valgus deformities through millimeter-length incisions. Originally conceptualized and popularized by pioneers in European orthopaedic centers—most notably Bosch, Magnan, and De Prado—this simple linear subcapital osteotomy aims to achieve the robust structural correction historically reserved for traditional open procedures, such as the Chevron or Scarf osteotomies, while profoundly mitigating the iatrogenic soft tissue trauma inherent to extensive surgical exposures.
Hallux valgus is a complex, three-dimensional deformity characterized not merely by medial deviation of the first metatarsal and lateral deviation of the hallux, but also by coronal plane pronation of the first ray and sagittal plane elevation. The pathophysiology is multifactorial, involving a genetic predisposition, ligamentous laxity, and exacerbation through constrictive footwear. As the first metatarsal drifts medially, the sesamoid apparatus remains tethered to the second metatarsal via the transverse metatarsal ligament, resulting in relative lateral subluxation of the sesamoids. The percutaneous distal metatarsal osteotomy addresses this pathoanatomy by allowing a controlled, extra-articular lateral translation of the metatarsal head, effectively reducing the intermetatarsal angle (IMA) and realigning the articular surface over the sesamoid complex without requiring extensive capsulotomies.
The epidemiological burden of hallux valgus is substantial, affecting approximately 23% of adults aged 18 to 65 years and over 35% of adults over the age of 65, with a pronounced predilection for the female demographic. The socioeconomic impact, driven by pain, altered gait mechanics, and the inability to wear standard footwear, drives a massive volume of surgical interventions annually. The appeal of the percutaneous approach lies in its potential to dramatically reduce this burden. Proponents cite significant advantages: minimal soft tissue dissection, preservation of the crucial vascular supply to the metatarsal head, abbreviated operative times, and the feasibility of performing the procedure entirely under regional ankle-block anesthesia in an outpatient setting.
However, the procedure remains shrouded in significant controversy within the academic orthopaedic community. The literature presents a stark dichotomy of clinical outcomes. While European series have reported patient satisfaction rates exceeding 90% with high union rates, prominent North American foot and ankle surgeons have reported unacceptable complication profiles. These critical reports cite devastating instances of osteonecrosis (avascular necrosis of the metatarsal head), intractable nonunions, severe malunions leading to transfer metatarsalgia, and rapid recurrence of the deformity. Consequently, the percutaneous distal metatarsal osteotomy is universally acknowledged to possess a notoriously steep learning curve. It demands an exceptional three-dimensional spatial awareness of forefoot anatomy, a profound understanding of extra-articular biomechanics, and absolute mastery of intraoperative fluoroscopic imaging.
Detailed Surgical Anatomy and Biomechanics
A profound comprehension of the osteology and vascular anatomy of the first ray is the absolute prerequisite for executing a percutaneous distal metatarsal osteotomy safely. The first metatarsal is unique among the metatarsals, possessing an independent epiphyseal growth plate proximally and bearing a significantly higher load during the terminal stance phase of gait. The vascular supply to the first metatarsal head is notoriously precarious, forming the anatomical basis for the fear of iatrogenic avascular necrosis. The primary extraosseous arterial supply is derived from the first dorsal metatarsal artery, the first plantar metatarsal artery, and the superficial branch of the medial plantar artery. These vessels form a dense capsular anastomotic network. By utilizing a percutaneous approach that intentionally avoids formal capsulotomy and extensive periosteal stripping, the surgeon theoretically preserves this delicate extracapsular vascular arborization, providing a biologic rationale for the procedure's viability despite the subcapital nature of the bone cut.
The soft tissue envelope surrounding the first metatarsophalangeal (MTP) joint is equally critical to the biomechanical success of this procedure. The medial collateral ligament, the lateral collateral ligament, the adductor hallucis insertion, and the plantar plate/sesamoid complex dictate the stability of the joint. In traditional open surgery, lateral soft tissue releases (e.g., modified McBride) are routinely performed. In contrast, the percutaneous technique relies heavily on the integrity of the lateral soft tissue hinge. When the metatarsal head is translated laterally following the osteotomy, the intact lateral capsule and adductor tendon act as a tether, preventing excessive displacement and providing a dynamic tension band that compresses the osteotomy site once weight-bearing is initiated.
The biomechanics of the correction rely entirely on the concept of "guiding the correction" using a strategically placed intramedullary Kirschner wire (K-wire) and the intact soft tissue envelope. Unlike open procedures that utilize rigid internal fixation (such as crossed interfragmentary screws or locking plates) to achieve absolute stability, the percutaneous technique embraces the concept of relative stability. The osteotomy is performed in the subcapital region, strictly perpendicular to the diaphyseal axis in the sagittal plane. By physically translating the capital fragment laterally, the intermetatarsal angle is mechanically reduced. The K-wire, inserted extraperiosteally along the proximal phalanx, acts as a joystick to manipulate the head and subsequently serves as an intramedullary strut to hold the lateral translation.
Achieving three-dimensional correction requires meticulous manipulation of the capital fragment prior to final K-wire advancement. The exact dorsal-plantar entry point of the K-wire dictates the sagittal plane translation of the metatarsal head. If the metatarsal head requires plantar translation to increase its weight-bearing load and prevent transfer metatarsalgia to the lesser rays, the wire must engage the head more dorsally. Conversely, for dorsal translation, the wire should engage more plantarly. Furthermore, because the high-speed burr removes approximately 2 to 3 millimeters of bone (the kerf), the surgeon can induce a slight relative lengthening or shortening of the metatarsal by altering the frontal plane obliquity of the cut, a critical maneuver to maintain the harmonious cascade of the metatarsal parabola.
Exhaustive Indications and Contraindications
Careful, uncompromising patient selection is the fundamental cornerstone of success in percutaneous forefoot surgery. The procedure is not a universal panacea for all hallux valgus deformities, and extending its use beyond established parameters is the primary driver of the catastrophic complications reported in the literature. The ideal candidate is a patient with a mild to moderate, symptomatic hallux valgus deformity that has failed exhaustive conservative management (e.g., orthotics, shoe modification, non-steroidal anti-inflammatory medications). The deformity must be manually reducible, indicating a flexible soft tissue envelope and the absence of severe, rigid degenerative changes within the first MTP joint.
Clinical evaluation must include a rigorous assessment of the entire lower extremity kinetic chain. The surgeon must evaluate the first tarsometatarsal (TMT) joint for clinical hypermobility in the sagittal plane. If profound hypermobility is present, a distal osteotomy will inevitably fail, and the patient requires a proximal fusion (Lapidus procedure). Additionally, the first MTP joint must be assessed for crepitus and restricted range of motion indicative of hallux rigidus; performing a joint-sparing osteotomy in the presence of advanced arthritis will exacerbate joint pain due to altered joint kinematics. Finally, the Silfverskiöld test must be performed to rule out isolated gastrocnemius contracture, which can drive forefoot overload and predispose the patient to recurrence or transfer lesions.
Radiographic parameters are equally stringent. Standardized, weight-bearing anteroposterior (AP), lateral, and sesamoid axial radiographs are mandatory. The primary indications include an intermetatarsal angle (IMA) of less than 15 degrees and a hallux valgus angle (HVA) of less than 30 to 35 degrees. The distal metatarsal articular angle (DMAA) must also be scrutinized; while mild elevations can be addressed by rotating the capital fragment, severe DMAA abnormalities are better managed with open, biplanar osteotomies. Patients with high surgical risk for open procedures—such as those with mild, controlled vascular compromise or dermatological conditions where extensive incisions might fail to heal—represent a unique subset where the percutaneous approach offers distinct advantages, provided severe ischemia is ruled out.
Absolute contraindications must be strictly respected to avoid limb-threatening complications. Severe hallux valgus deformities (IMA > 15°, HVA > 40°) cannot be adequately corrected with a simple linear translation without risking the metatarsal head falling completely off the diaphyseal fragment. Active local or systemic infection, severe peripheral arterial disease (ABI < 0.5), and profound peripheral neuropathy (Charcot neuroarthropathy) are absolute contraindications. Furthermore, the percutaneous distal metatarsal osteotomy should generally be avoided as a revision surgery for previously failed hallux valgus corrections, as the altered anatomy and scarred soft tissue planes drastically increase the risk of neurovascular injury and avascular necrosis.
| Category | Indications for Percutaneous Osteotomy | Contraindications for Percutaneous Osteotomy |
|---|---|---|
| Deformity Severity | Mild to moderate Hallux Valgus | Severe Hallux Valgus (IMA > 15°, HVA > 40°) |
| Radiographic Parameters | IMA < 15°, HVA < 30°, Normal/Mild DMAA | IMA > 15°, HVA > 40°, Severe DMAA abnormality |
| Joint Status | Congruent or reducible MTP joint, no arthritis | First TMT hypermobility, Hallux Rigidus (OA) |
| Vascular/Neurologic | Intact pedal pulses, normal sensation | Severe PAD, active ischemia, peripheral neuropathy |
| Surgical History | Primary surgical intervention | Revision of prior failed HV surgery |
| Patient Factors | Compliant with strict post-op taping/shoe protocols | Non-compliant, active infection, severe osteoporosis |
Pre-Operative Planning, Templating, and Patient Positioning
Pre-operative planning for a percutaneous distal metatarsal osteotomy is a highly quantitative exercise. The surgeon must utilize digital templating software on weight-bearing radiographs to precisely calculate the required lateral translation of the metatarsal head. As a general biomechanical rule, 1 millimeter of lateral translation of the capital fragment correlates to approximately 1 degree of intermetatarsal angle correction. The surgeon must measure the diaphyseal width at the planned subcapital osteotomy site; the translation must never exceed 50% to 60% of the diaphyseal width to ensure adequate bone-to-bone contact for stable union. If the required translation exceeds this threshold, the patient is not a candidate for a distal percutaneous procedure.
Anesthetic planning is a critical component of the operative workflow. The procedure is exceptionally amenable to regional anesthesia, which avoids the systemic risks of general anesthesia and provides profound, long-lasting postoperative analgesia. A comprehensive ankle block—targeting the posterior tibial, deep peroneal, superficial peroneal, sural, and saphenous nerves—is the gold standard. Alternatively, a popliteal sciatic nerve block combined with a saphenous nerve block can be utilized. The use of a pneumatic calf tourniquet is at the surgeon's discretion; however, many percutaneous surgeons prefer to operate without a tourniquet. The absence of a tourniquet allows the continuous flow of blood to act as a heat sink, further mitigating the risk of thermal necrosis during high-speed burring, and allows immediate assessment of digital perfusion.
Patient positioning must be meticulously executed to facilitate unhindered fluoroscopic access, as the procedure relies entirely on real-time radiographic feedback. The patient is placed supine on a radiolucent operating table. A specialized below-the-knee wedge bracket or a custom foam ramp is utilized to allow exactly 90 degrees of knee flexion. This specific positioning places the plantar aspect of the foot firmly and flatly onto the image intensifier detector or table, simulating a plantigrade, weight-bearing posture.
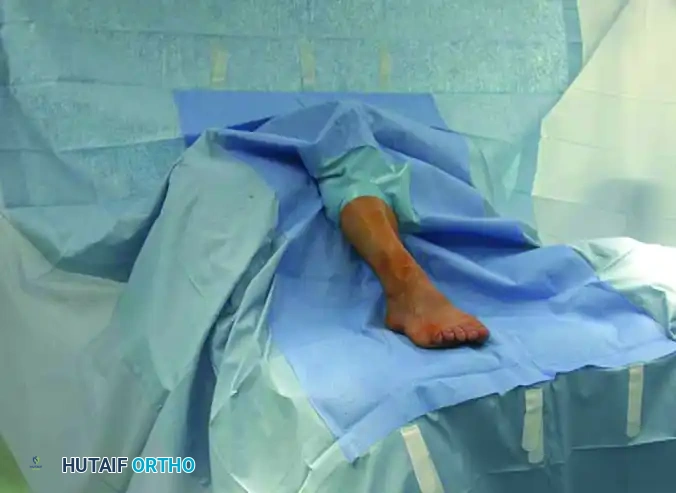
The operating room layout must be optimized for ergonomics and radiation safety. The fluoroscopic image intensifier (C-arm) is brought in from the contralateral side of the patient, positioned so that the arc can effortlessly rotate between true anteroposterior and true lateral projections without striking the table or the patient's contralateral leg. The primary surgeon stands directly in front of the patient at the distal end of the table. This distal position affords the surgeon an unobstructed, axial line of sight down the first ray, facilitating accurate assessment of coronal plane rotation and sagittal alignment, while simultaneously allowing easy manipulation of the C-arm monitor and foot pedal.
Step-by-Step Surgical Approach and Fixation Technique
Kirschner Wire Trajectory and Initial Placement
The initial and arguably most critical step of the procedure involves the strategic placement of the 2.0-mm Kirschner wire. This wire will eventually capture, manipulate, and stabilize the osteotomized metatarsal head. The entry point is meticulously identified at the medial-plantar aspect of the distal phalanx, immediately adjacent to the medial corner of the hallux nail.
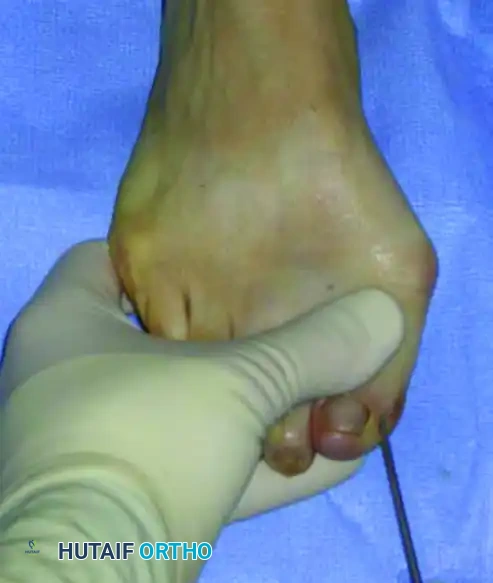
The surgeon must strictly avoid penetrating the distal corner or the germinal matrix of the nail. Transfixing the nail matrix is a severe technical error that can lead to excruciating postoperative pain, permanent nail dystrophy, or devastating skin sloughing while the wire remains in situ. The wire is advanced proximally under fluoroscopic guidance. It is an absolute biomechanical imperative that the wire is placed in an extraperiosteal position along the medial aspect of the proximal phalanx and the medial capsule of the MTP joint.
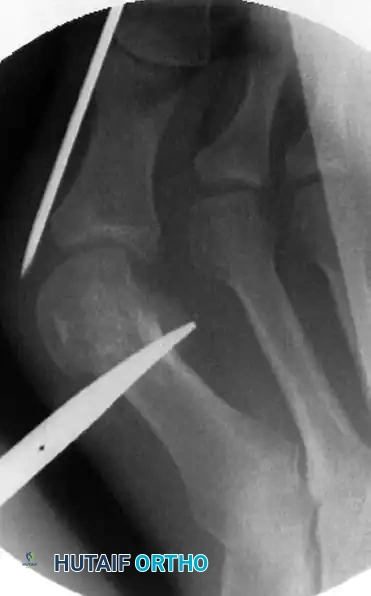
If the wire is inadvertently passed subperiosteally or intracapsularly, it will tether the soft tissues and completely prohibit the lateral displacement of the capital fragment later in the procedure. The wire must be centered exactly midway between the dorsal and plantar cortices of the great toe in the lateral plane to correctly engage the geometric center of the metatarsal head. The wire is driven until it firmly and deeply engages the medial aspect of the metatarsal head. Firm engagement is critical; loss of bony contact during the high-vibration osteotomy will result in an uncontrolled, free-floating capital fragment that is exceedingly difficult to recapture percutaneously.
Skin Incision and Soft Tissue Preparation
Once the K-wire is securely anchored in the metatarsal head, the surgeon identifies the optimal site for the percutaneous portal. This point is typically located approximately 1 cm proximal to the engaged tip of the K-wire, corresponding to the subcapital neck of the first metatarsal. A micro-incision, measuring precisely 3 to 5 millimeters, is created using a #15 or #64 Beaver blade.
The incision must be carried directly and bluntly down to the bone, sharply incising the periosteum only upon direct bony contact. To avoid transecting the dorsal medial cutaneous nerve or the plantar medial neurovascular bundle, the surgeon must ensure the incision remains strictly in the longitudinal midline (the equator) of the medial metatarsal neck. Once the periosteum is breached, a small periosteal elevator or specialized sharp scissors are introduced through the portal.
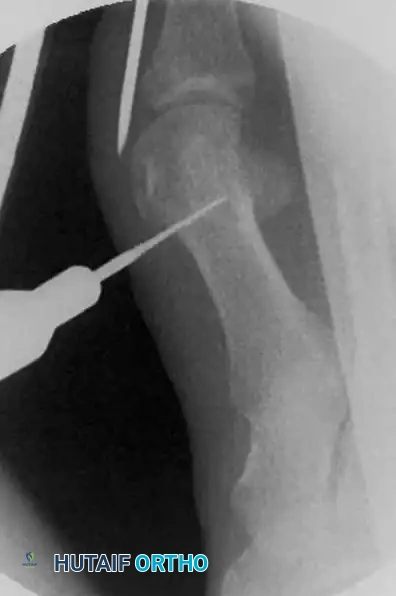
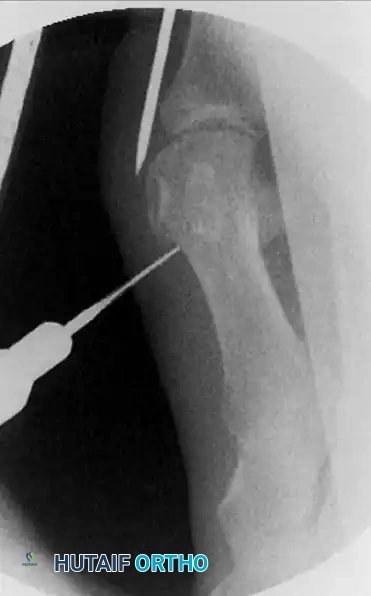
The instrument is used to aggressively detach the periosteum circumferentially around the planned osteotomy site, sweeping both dorsally and plantarly. This step is not merely for exposure; it creates a vital "safe working chamber." By elevating the delicate soft tissues, the joint capsule, and the adjacent neurovascular structures away from the bone, the surgeon protects them from being entangled or lacerated by the high-torque motorized bone cutter.
Osteotomy Execution and Thermal Management
The osteotomy is executed utilizing a specialized 2.33-mm-diameter micromotorized Shannon or Lindemann bone cutter (e.g., Aesculap, Tuttlingen, Germany). This specific burr is engineered for aggressive side-cutting, operating at a high torque but strictly low speed (typically under 5,000 RPM) to minimize the generation of thermal energy. The burr is introduced through the established working chamber to the subcapital region. Before activating the motor, the surgeon must verify the exact level and trajectory of the planned cut using orthogonal fluoroscopy.
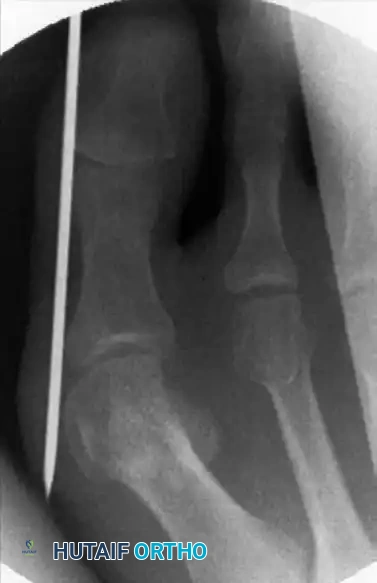
The geometry of the osteotomy is paramount. In the sagittal plane, the cut must be strictly perpendicular to the long axis of the first metatarsal shaft to prevent inadvertent dorsal or plantar translation during lateral shift. In the frontal plane, the surgeon introduces a slight mediolateral obliquity. Because the burr removes a 2 to 3 mm kerf of bone, this slight inclination facilitates relative lengthening (to prevent transfer lesions) or shortening (to decompress the joint) of the metatarsal as dictated by the preoperative templating.
The execution of the cut utilizes a specialized corticotomy technique. The surgeon drills the medial cortex first, then advances the tip of the burr into the medullary canal. From within the canal, the lateral cortex is drilled from inside out.
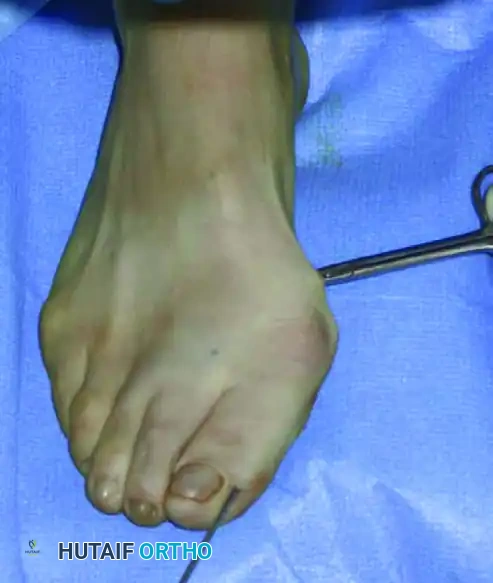
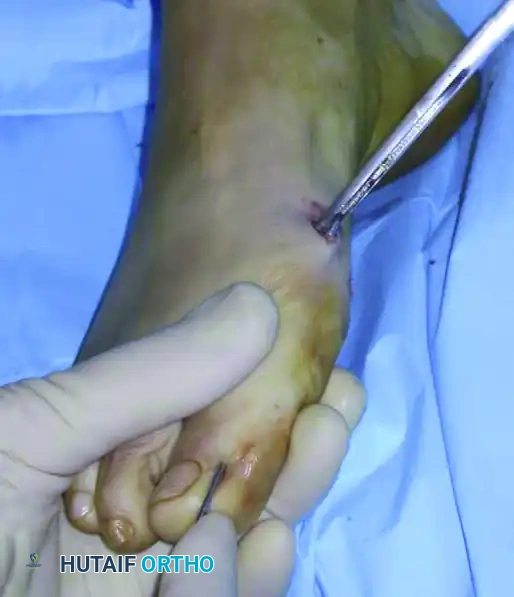
Throughout this entire process, continuous, copious cold saline irrigation directly onto the burr shaft is mandatory. Failure to irrigate will cause catastrophic thermal necrosis of the bone—leading directly to nonunion or avascular necrosis—and thermal burns to the skin edges, leading to wound breakdown. The bone cutter is kept in the same medial entry hole, pivoting in a sweeping motion to drill multiple holes circumferentially until the cut is complete. The surgeon confirms completion by manually stressing the hallux; a palpable and visible "give" indicates the metatarsal head is fully mobile.
Deformity Correction and Intramedullary Fixation
With the osteotomy complete and the capital fragment mobilized, the surgeon proceeds to deformity correction. The metatarsal head must be translated laterally to reduce the intermetatarsal angle. A specially designed grooved intramedullary instrument (e.g., Tecres, Verona, Italy) is inserted through the incision, traversing the osteotomy site, and advanced deep into the medullary canal of the proximal first metatarsal diaphysis.
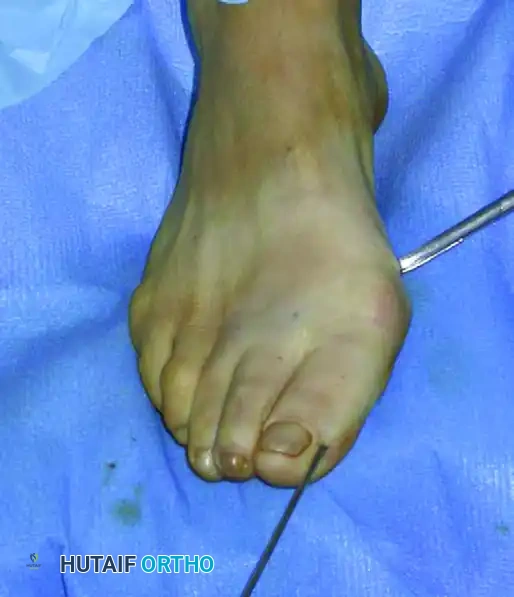
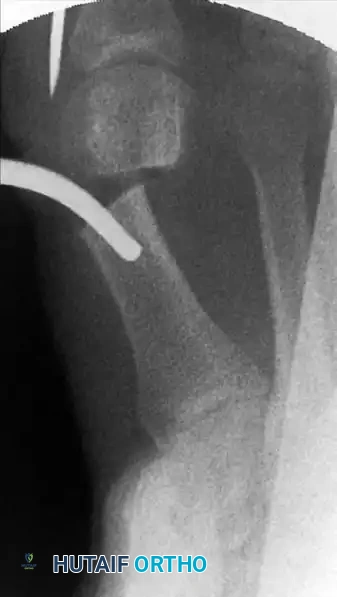
The previously placed K-wire, which is still anchored in the metatarsal head, is now advanced manually. The surgeon visualizes or tactilely feels the proximal tip of the wire engaging directly into the groove of the intramedullary instrument.

To execute the correction, the grooved instrument is used as a powerful mechanical lever. The surgeon levers the proximal handle of the instrument distally, which physically pushes the metatarsal head segment laterally. Simultaneously, the surgeon's opposite hand (holding the hallux and the distal end of the K-wire) is used to tilt, derotate, and control the sagittal alignment of the metatarsal head.
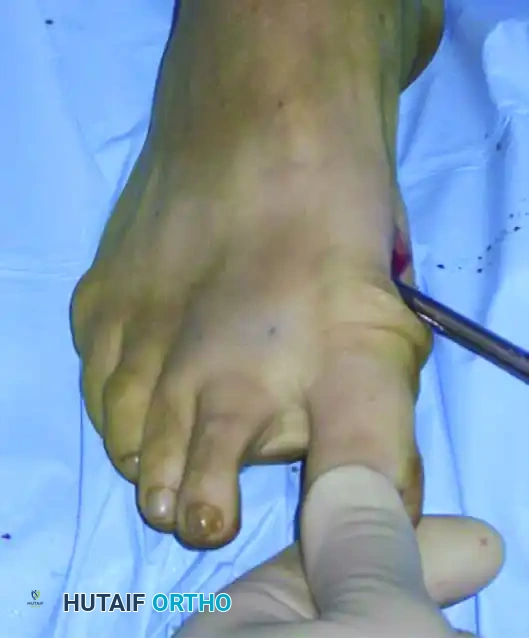
This translation must be performed gradually. Over-aggressive or jerky translation can cause the metatarsal head to completely disengage and "fall off" the diaphyseal fragment into the first intermetatarsal space. Once satisfactory lateral translation and axial alignment are achieved, the K-wire is driven forcefully from distal to proximal, passing out of the metatarsal head and deep into the medullary canal of the proximal metatarsal shaft or into the subchondral bone of the medial cuneiform to lock the correction in place.
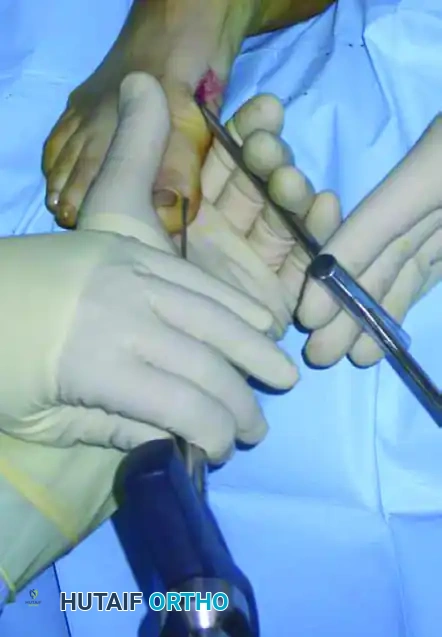
Final confirmation of the correction, translation percentage, and hardware placement is obtained with true orthogonal fluoroscopic views. Satisfactory correction is generally achieved when the medial aspect of the metatarsal head is perfectly flush with the lateral cortex of the metatarsal shaft.
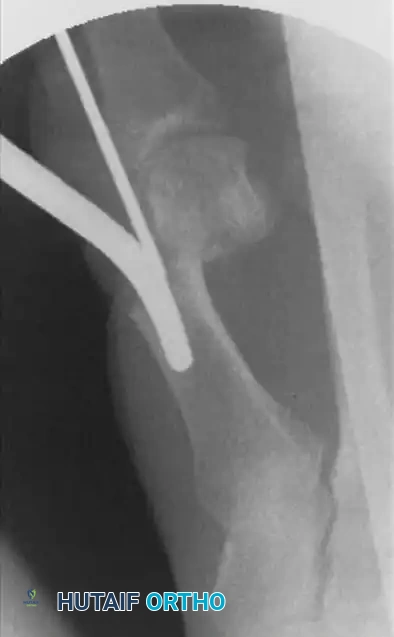
The K-wire is then cut outside the skin and heavily bent to prevent proximal migration. The micro-incision is thoroughly irrigated to remove bone debris and closed with a single non-absorbable suture or simple sterile adhesive strips.
Complications, Incidence Rates, and Salvage Management
As highlighted by the conflicting literature, surgeons must be acutely aware of the potentially devastating complications associated with the percutaneous distal metatarsal osteotomy. The procedure's reliance on indirect visualization and relative stability makes it highly unforgiving of technical errors. The steep learning curve is not a mere anecdotal warning; it is a well-documented phenomenon where early case series by inexperienced surgeons demonstrate complication rates exceeding 30%.
Osteonecrosis (avascular necrosis) of the metatarsal head is the primary and most feared concern raised by critics. While the percutaneous approach theoretically spares the capsular blood supply, overly aggressive burring, failure to use copious cold saline irrigation, or inadvertent laceration of the plantar lateral arterial network during periosteal stripping can severely compromise the head's vascularity. Incidence rates vary wildly, from 0% in expert European series to as high as 7% in early North American reports. Diagnosis requires a high index of suspicion and MRI confirmation if progressive pain and radiographic collapse occur. Salvage of advanced AVN almost uniformly requires a first MTP joint arthrodesis, often necessitating structural bone grafting to restore length.
Nonunion and malunion represent significant biomechanical failures. A single K-wire provides vastly inferior biomechanical stability compared to the crossed screws or locking plates utilized in open procedures. Non-compliant premature weight-bearing, failure of the external taping splint, or excessive thermal necrosis at the osteotomy site can lead to loss of fixation. Dorsal elevation of the metatarsal head is the most common malunion, leading to
