Knee Synovial Chondromatosis: A Detailed Clinical & Advanced Imaging Diagnostic Case Study

Key Takeaway
Synovial chondromatosis in the knee is diagnosed through a combination of detailed patient history (pain, swelling, mechanical symptoms), thorough physical examination (palpable loose bodies, limited ROM), and advanced imaging. Radiographs reveal calcified loose bodies, CT offers detailed delineation, and MRI is crucial for identifying non-calcified nodules and assessing synovial proliferation, forming a complete diagnostic picture.
Welcome to this Orthopedic Grand Rounds presentation. Today, we will dissect a highly complex and clinically fascinating case of Primary Synovial Chondromatosis of the knee. This condition, characterized by the benign metaplasia of synovial connective tissue into cartilaginous nodules, presents unique diagnostic and therapeutic challenges. The insidious nature of the disease often leads to delayed diagnosis, by which time significant secondary mechanical damage to the articular cartilage may have occurred. We will review the patient presentation, deconstruct the clinical examination, analyze the advanced imaging modalities required for surgical templating, and detail the operative intervention necessary to eradicate the metaplastic tissue while preserving joint kinematics.
Patient Presentation and History
A 45-year-old male presented to the Orthopedic Oncology clinic with a 12-month history of progressive right knee pain, swelling, and mechanical symptoms. He reported intermittent locking and clicking, particularly with squatting or pivoting movements, leading to a feeling of instability. The pain was initially insidious in onset, dull and aching, primarily localized to the medial and patellofemoral compartments, but had recently escalated in intensity to a constant 7/10 on the Visual Analog Scale, exacerbated by activity and partially relieved by rest and over-the-counter analgesics. He denied any specific traumatic event that initiated the symptoms, although he recalled a minor twisting injury to the knee approximately 18 months prior, which resolved spontaneously after a few weeks of RICE therapy.
His past medical history was unremarkable, with no known comorbidities such as diabetes, hypertension, or inflammatory arthropathies. He reported no previous knee surgeries or significant prior injuries. His social history included working as an office manager, which involved prolonged sitting and occasional light recreational sports like cycling. He was a non-smoker and consumed alcohol occasionally. Family history was negative for any connective tissue disorders or bone/soft tissue tumors.
The patient noted several episodes of sudden, intense pain accompanied by a transient inability to fully extend the knee, which would spontaneously resolve after a few minutes, suggesting intra-articular loose bodies acting as a mechanical fulcrum within the joint space. He also reported a gradual increase in the size of the knee joint itself, despite minimal effusion at times. This discrepancy between perceived joint volume and aspiratable fluid is a hallmark of synovial proliferative disorders, where the bulk is solid metaplastic tissue rather than simple synovial fluid accumulation. The chronicity of his symptoms, combined with the escalating mechanical blocks, indicates a progressive intra-articular space-occupying pathology that has outpaced conservative management strategies.
Clinical Examination Findings
Inspection of the Knee Joint
On inspection, the right knee appeared mildly swollen with noticeable quadriceps muscle atrophy compared to the contralateral limb, specifically involving the vastus medialis obliquus. This rapid atrophy is indicative of chronic nociceptive inhibition secondary to capsular distension and intra-articular pathology. There was no overt erythema or warmth, effectively lowering the probability of an acute septic process or crystalline arthropathy. The skin appeared intact, with no scars, sinuses, or masses visibly protruding through the retinaculum. A mild genu valgum deformity was noted, consistent bilaterally, suggesting a baseline biomechanical alignment rather than a pathological deviation secondary to unilateral joint destruction.
Palpation and Joint Line Assessment
Palpation revealed a mild effusion, with a positive patellar tap test. However, the fluid wave was less pronounced than the gross visual swelling would suggest, reinforcing the suspicion of synovial hypertrophy or solid intra-articular bodies. There was diffuse tenderness along the medial joint line and patellofemoral facets. Crepitus was elicited throughout the range of motion, distinct from the typical fine crepitus of chondromalacia; it presented as a coarse, clunking sensation. Notably, several firm, mobile, non-tender nodules, approximately 0.5 to 1.5 cm in diameter, were palpable within the suprapatellar pouch and medial parapatellar regions. This "bag of marbles" sensation is highly specific for intra-articular loose bodies. No localized warmth or pulsatile masses were appreciated.
Range of Motion and Kinematic Evaluation
Active range of motion of the right knee was significantly limited due to pain and mechanical blockage, measuring 15 degrees to 105 degrees of flexion, compared to a normal physiological range of 0 degrees to 140 degrees. Passive range of motion mirrored the active findings, with a firm, almost bony end-feel on terminal extension and flexion. This firm end-feel, as opposed to a boggy or springy block typical of a displaced meniscal tear, strongly suggests the interposition of calcified or ossified bodies within the intercondylar notch or posterior recesses. Patellar tracking was within normal limits, though severe patellofemoral crepitus was evident during the active arc of motion.
Special Tests for Ligamentous and Meniscal Integrity
Meniscal examination revealed mild tenderness on palpation of the medial joint line. McMurray's test was equivocal; while a click was appreciated, it was impossible to differentiate a true meniscal clunk from the displacement of a cartilaginous loose body during the provocative maneuver. Ligamentous stability assessment demonstrated no varus or valgus instability at 0 degrees or 30 degrees of flexion, indicating intact collateral ligaments. Lachman and anterior/posterior drawer tests were negative, confirming the structural integrity of the cruciate ligaments. Dial test was negative, ruling out posterolateral corner deficiency.
Neurological and Vascular Assessment
Distal neurovascular status was completely intact. Popliteal and dorsalis pedis pulses were strong and symmetric bilaterally. Capillary refill was brisk at less than two seconds. Sensation was intact to light touch and pinprick in all dermatomes distal to the knee, including the saphenous, deep peroneal, superficial peroneal, sural, and tibial nerve distributions. Motor strength was graded 5/5 in all major muscle groups of the lower extremity, including dorsiflexion and plantarflexion, although pain limited the patient's maximal effort during resisted quadriceps contraction.
Imaging and Diagnostics
Plain Radiography Findings
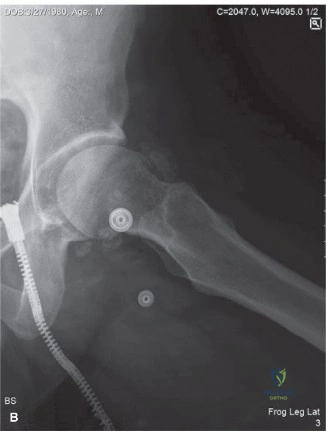
Initial radiographs of the right knee, including anteroposterior, lateral, skyline, and weight-bearing views, demonstrated multiple, well-circumscribed, oval or curvilinear radiopacities within the joint space, varying in size from a few millimeters to approximately 1.5 cm. These calcified loose bodies were most concentrated in the suprapatellar pouch, the medial and lateral gutters, and the posterior recesses of the knee.
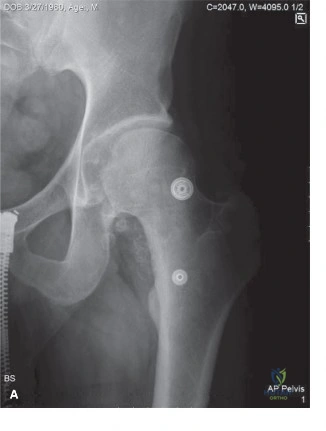
The radiographic pattern exhibited the classic "ring-and-arc" chondroid mineralization, pathognomonic for hyaline cartilage matrices that have undergone endochondral ossification. Importantly, the underlying joint space was relatively preserved, with minimal osteophyte formation or subchondral sclerosis. This lack of advanced degenerative joint disease is a critical radiographic differentiator, suggesting that the loose bodies are the primary pathology (Primary Synovial Chondromatosis) rather than secondary osteochondral fragments resulting from advanced osteoarthritis or neuropathic arthropathy. Extrinsic scalloping of the anterior femoral cortex was noted, a secondary sign of chronic pressure erosion from the hyperplastic synovial masses.
Computed Tomography Applications
To further delineate the osseous anatomy and precisely map the anatomical distribution of the calcified bodies, a non-contrast Computed Tomography scan of the right knee was obtained.
The CT scan provided excellent spatial resolution, confirming the presence of over fifty distinct ossified nodules. The multiplanar reconstructions were instrumental in identifying loose bodies sequestered within the tight confines of the posteromedial and posterolateral compartments, areas notoriously difficult to assess on standard radiographs and challenging to access during arthroscopy. Furthermore, the CT scan clearly demonstrated the pressure erosions along the non-weight-bearing surfaces of the femoral condyles. These erosions exhibited sclerotic margins, confirming their chronic, benign nature, and effectively ruling out the permeative, destructive bone lesions associated with malignant processes such as synovial sarcoma or high-grade chondrosarcoma.
Magnetic Resonance Imaging Characteristics
Magnetic Resonance Imaging is the gold standard for evaluating synovial pathology and was essential in this case to assess the extent of uncalcified chondromata, synovial hypertrophy, and the integrity of the articular cartilage.

The MRI protocol included T1-weighted, T2-weighted fat-suppressed, and proton density sequences. The findings revealed massive distension of the joint capsule by a lobulated, complex intra-articular effusion containing innumerable loose bodies. On T1-weighted images, the uncalcified cartilaginous nodules appeared isointense to skeletal muscle. On T2-weighted fat-suppressed sequences, these uncalcified nodules demonstrated high signal intensity, characteristic of the high water content within hyaline cartilage, while the calcified or ossified central portions appeared as distinct signal voids (hypointense).
The synovium itself was markedly thickened and demonstrated prominent frond-like projections. Following the administration of intravenous gadolinium contrast, there was avid enhancement of the thickened synovium, confirming active synovial proliferation and hypervascularity, while the chondral bodies themselves remained non-enhancing. The articular cartilage showed focal areas of grade II and grade III chondromalacia, particularly on the medial femoral condyle and the central ridge of the patella, likely representing secondary mechanical wear from the abrasive action of the loose bodies. The menisci and cruciate ligaments were confirmed to be structurally intact.
Differential Diagnosis
The presentation of a monoarticular arthropathy with multiple intra-articular loose bodies requires a rigorous differential diagnosis to distinguish between benign reactive processes, primary neoplastic conditions, and secondary degenerative phenomena.
| Diagnostic Entity | Pathophysiology | Radiographic Hallmark | MRI Characteristics | Clinical Demographics |
|---|---|---|---|---|
| Primary Synovial Chondromatosis | Benign metaplasia of synovial tissue into hyaline cartilage nodules. | Multiple, uniform "ring-and-arc" calcifications. Preserved joint space. | Lobulated intra-articular masses. Uncalcified bodies are T2 hyperintense. Synovial enhancement. | 3rd to 5th decade. Male predominance. Monoarticular (knee most common). |
| Secondary Synovial Chondromatosis | Fragmentation of articular cartilage/osteophytes due to underlying joint destruction. | Varied size/shape of bodies. Advanced joint space narrowing, osteophytes, sclerosis. | Degenerative cartilage loss, subchondral edema, meniscal maceration. Fewer, larger loose bodies. | Older patients (>60 years). History of advanced osteoarthritis or trauma. |
| Pigmented Villonodular Synovitis | Benign, locally aggressive fibrohistiocytic proliferation of the synovium. | Soft tissue swelling. Usually no calcifications. Extrinsic bone erosions. | "Blooming artifact" on gradient-echo sequences due to hemosiderin deposition. T1/T2 hypointense nodules. | 3rd to 4th decade. Monoarticular. Recurrent hemarthrosis. |
| Synovial Chondrosarcoma | Malignant transformation of primary synovial chondromatosis or de novo malignancy. | Rapidly enlarging soft tissue mass. Permeative bone destruction. Cortical breakthrough. | Heterogeneous signal. Extensive marrow infiltration. Extra-articular soft tissue extension. | Rare. Suspect if rapid clinical deterioration or recurrence after adequate synovectomy. |
Differentiating Primary from Secondary Disease
The critical distinction in this case lies between Primary and Secondary Synovial Chondromatosis. Secondary disease is vastly more common and occurs when fragments of degraded articular cartilage or osteophytes shed into the joint space and are subsequently nourished by synovial fluid, allowing them to grow. Radiographically, secondary disease is characterized by a few, asymmetrically sized loose bodies in the setting of severe, end-stage osteoarthritis. Our patient, however, presents with dozens of relatively uniform loose bodies and a remarkably well-preserved joint space, confirming the diagnosis of Primary Synovial Chondromatosis.
Ruling out Pigmented Villonodular Synovitis
Pigmented Villonodular Synovitis must also be considered in a middle-aged patient with a chronic, monoarticular, swollen knee. However, PVNS typically presents with recurrent hemarthrosis and lacks the dense, calcified bodies seen on our patient's radiographs. Furthermore, the MRI in PVNS is characterized by extensive hemosiderin deposition, which creates a classic "blooming artifact" on gradient-echo sequences—a feature entirely absent in our patient's imaging.
Surgical Decision Making and Classification
Primary Synovial Chondromatosis is classically described by the Milgram Classification, which divides the disease process into three distinct pathophysiological stages:
* Milgram Stage I: Active synovial disease with proliferation and metaplasia, but no loose bodies have detached into the joint space.
* Milgram Stage II: Transitional phase characterized by active synovial proliferation concurrent with the presence of detached, free-floating cartilaginous or osteocartilaginous loose bodies.
* Milgram Stage III: Late phase where the synovial disease has burned out (inactive synovium), but multiple loose bodies remain within the joint cavity, continuing to grow via nourishment from the synovial fluid.
Based on the MRI findings of active, enhancing synovial hypertrophy combined with dozens of detached loose bodies, our patient is classified as having Milgram Stage II disease.
Rationale for Operative Intervention
Non-operative management for Milgram Stage II Primary Synovial Chondromatosis is generally ineffective and not recommended. The intra-articular bodies act as abrasive third bodies, functioning much like sand in a bearing. If left untreated, the continuous mechanical grinding will inevitably lead to accelerated secondary osteoarthritis, eventually necessitating total joint arthroplasty. Furthermore, the mechanical blocks to extension and flexion severely limit the patient's functional capacity and quality of life.
Therefore, the surgical indication is absolute. The goals of surgery are twofold: first, the meticulous extraction of all intra-articular loose bodies to eliminate the mechanical block and halt the abrasive cartilage wear; and second, a comprehensive anterior and posterior synovectomy to eradicate the metaplastic tissue and minimize the risk of disease recurrence.
Arthroscopic versus Open Approach
The decision between an all-arthroscopic approach versus an open arthrotomy depends on the size of the loose bodies, the extent of extra-articular involvement, and the surgeon's facility with advanced arthroscopic techniques in the posterior compartments of the knee. Given that the largest bodies in this patient measured approximately 1.5 cm, they are amenable to arthroscopic extraction. An arthroscopic approach offers the advantages of decreased postoperative morbidity, faster rehabilitation, and superior visualization of the posterior recesses compared to a standard anterior arthrotomy. We elected to proceed with a comprehensive arthroscopic loose body removal and subtotal synovectomy, with the patient consented for a possible open posterior arthrotomy if arthroscopic clearance proved insufficient.
Surgical Technique and Intervention
Preoperative Planning and Patient Positioning
The patient was brought to the operating theater and placed supine on the operating table. General endotracheal anesthesia was induced. A high-thigh tourniquet was applied to the right lower extremity, and the leg was placed in a standard arthroscopic leg holder, allowing for full, unencumbered manipulation of the knee from 0 to 120 degrees of flexion. The contralateral leg was placed in a well-padded gynecological stirrup to protect against deep vein thrombosis and nerve compression. A meticulous surgical prep and drape were performed. The tourniquet was inflated to 250 mmHg following exsanguination with an Esmarch bandage.
Arthroscopic Diagnostic Sweep and Anterior Compartment Clearance
Standard anterolateral and anteromedial portals were established adjacent to the patellar tendon. Upon insertion of the arthroscope, an immediate egress of viscous, amber-colored synovial fluid was noted, accompanied by the spontaneous extrusion of several small cartilaginous bodies.
The diagnostic sweep revealed a hyperemic, grossly hypertrophic synovium with multiple frond-like villi and embedded cartilaginous nodules, confirming the Milgram Stage II diagnosis. The suprapatellar pouch was massively distended and packed with dozens of loose bodies ranging from 5 mm to 15 mm.
We established a superolateral outflow portal to manage fluid dynamics and allow for the insertion of a large-bore cannula. Using a combination of an arthroscopic grasper and a motorized 4.5 mm aggressive shaver, the loose bodies were systematically extracted. Care was taken to avoid crushing the cartilaginous bodies during extraction, as fragmentation can lead to retained micro-fragments that may seed recurrent disease. Following the clearance of the loose bodies from the suprapatellar pouch, medial gutter, and lateral gutter, a thorough anterior synovectomy was performed. A radiofrequency ablation wand was utilized to achieve hemostasis and ablate the residual metaplastic synovial tissue down to the capsular layer.
Posterior Compartment Access and Posteromedial Posterolateral Portals
The most critical and technically demanding aspect of this procedure is the clearance of the posterior compartments. Failure to address the posterior recesses is the leading cause of early recurrence in synovial chondromatosis.
The arthroscope was passed through the intercondylar notch, navigating between the posterior cruciate ligament and the medial femoral condyle (the "over-the-top" view) to visualize the posteromedial compartment. As anticipated from the preoperative CT scan, a cluster of ossified bodies was sequestered within the posteromedial recess.
To access this area safely, a posteromedial portal was established under direct intra-articular trans-illumination. An 18-gauge spinal needle was used to localize the precise entry point, ensuring a safe trajectory posterior to the medial collateral ligament and anterior to the saphenous nerve and vein. A small incision was made, and a blunt trocar was used to enter the capsule. Through this portal, a grasping forceps was introduced, and six large loose bodies were successfully extracted. A localized posteromedial synovectomy was then performed using a curved shaver blade.
The process was repeated for the posterolateral compartment. The arthroscope was passed lateral to the anterior cruciate ligament to visualize the posterolateral recess. A posterolateral portal was established under trans-illumination, anterior to the biceps femoris tendon and the common peroneal nerve. Several smaller loose bodies were extracted from the popliteal hiatus, and a posterolateral synovectomy was completed.
Specimen Extraction and Intraoperative Pathology
A total of 64 distinct osteocartilaginous bodies were extracted during the procedure. The largest measured 1.6 cm in maximal diameter. Representative samples of the hypertrophic synovium and several loose bodies were sent for routine histopathological analysis. Intraoperative frozen sections were not deemed necessary as the macroscopic appearance was classic for benign synovial chondromatosis, and preoperative imaging showed no evidence of aggressive osseous invasion.
Following complete clearance, the joint was copiously irrigated with 9 liters of normal saline to ensure no micro-fragments remained. The tourniquet was deflated, and meticulous hemostasis was achieved using the radiofrequency wand. The portals were closed with non-absorbable monofilament sutures, and a sterile compressive dressing was applied.
Post Operative Protocol and Rehabilitation
Immediate Postoperative Phase
The patient was discharged on the day of surgery with a hinged knee brace locked in extension for ambulation to protect the portal sites and minimize postoperative hemarthrosis. Weight-bearing was permitted as tolerated with the use of crutches. Cryotherapy was aggressively utilized to manage edema and pain. Deep vein thrombosis prophylaxis consisted of early mobilization and oral aspirin 81 mg twice daily for two weeks.
Intermediate Rehabilitation Phase
At the two-week postoperative visit, the portal sutures were removed. The wounds were clean, dry, and intact. The patient reported a complete resolution of the preoperative mechanical locking. Active and passive range of motion exercises were initiated, with an immediate goal of achieving 0 to 90 degrees of flexion. The hinged brace was unlocked to allow full motion during physical therapy. Stationary cycling with low resistance was introduced to promote synovial fluid circulation and cartilage nutrition.
Advanced Strengthening and Return to Activity
By six weeks postoperatively, the patient had regained full, symmetric range of motion (0 to 135 degrees). Physical therapy transitioned to closed-kinetic-chain strengthening exercises, focusing on quadriceps and hamstring co-contraction to rebuild the atrophied vastus medialis obliquus. Proprioceptive training and balance exercises were incorporated. The patient was cleared to return to his occupation as an office manager without restrictions. Return to higher-impact recreational activities was delayed until 12 weeks postoperatively to allow for complete capsular healing and resolution of the joint effusion. Routine clinical and radiographic follow-up is scheduled at 6 months, 1 year, and annually thereafter to monitor for disease recurrence.
Clinical Pearls and Pitfalls
- Mandatory Advanced Imaging: Plain radiographs are insufficient for surgical templating in synovial chondromatosis. A preoperative CT or MRI is absolutely critical to identify sequestered loose bodies in the posterior compartments and popliteal hiatus.
- The Posterior Compartment Pitfall: The most common technical error in the surgical management of this disease is the failure to establish posteromedial and posterolateral portals. Attempting to clear the posterior recesses solely from anterior portals via the intercondylar notch is inadequate and virtually guarantees disease recurrence.
- Synovectomy Extent: While a complete synovectomy is theoretically ideal to prevent recurrence, it is technically impossible and carries a high risk of postoperative arthrofibrosis. A meticulous subtotal synovectomy, focusing on grossly abnormal tissue and completely clearing all loose bodies, provides the best balance between recurrence prevention and functional outcome.
- Malignant Transformation: Although exceedingly rare (estimated at less than 5%), malignant transformation to synovial chondrosarcoma can occur. A high index of suspicion must be maintained if a patient presents with rapid clinical deterioration, multiple recurrences despite adequate surgical clearance, or imaging demonstrating permeative cortical destruction or extra-articular soft tissue mass extension. All excised tissue must be submitted for formal histopathological evaluation.
- Cartilage Preservation: During arthroscopic extraction, avoid using excessive force or overly aggressive shaver settings that could inadvertently score or damage the underlying articular cartilage. The primary goal is joint preservation; iatrogenic chondral injury defeats the purpose of the intervention.
