Myositis Ossificans: A Challenging Orthopedic Oncology Case & Diagnostic Pitfalls
Key Takeaway
Myositis ossificans, a benign ossifying lesion, is often mistaken for soft tissue sarcoma. Differentiating it relies on a detailed history of trauma, clinical presentation, and critical imaging findings like the "zone phenomenon" on CT scans – a mature peripheral ossification with a less dense center. MRI helps characterize soft tissue components, guiding accurate diagnosis and preventing unnecessary interventions.
Patient Presentation and History
Mechanism of Injury and Initial Clinical Course
A 28-year-old male, a recreational athlete with no significant past medical history, presented to the Orthopedic Trauma clinic complaining of persistent and progressive pain and swelling in his left anterior thigh. The patient sustained a high-energy direct blunt trauma to the anterior aspect of the left thigh during a collision in a rugby match approximately three months prior to the current presentation. The impact was localized to the vastus intermedius and rectus femoris region. Initially, the injury was classified clinically as a severe quadriceps contusion. The patient managed the acute phase conservatively utilizing standard protocols including rest, ice, compression, and elevation, alongside a brief course of over-the-counter non-steroidal anti-inflammatory drugs.
Over the subsequent three to four weeks, the initial ecchymosis and superficial soft tissue tenderness resolved, and the patient attempted a gradual return to sport. However, at approximately six weeks post-injury, the clinical trajectory deviated from the expected natural history of a simple muscle contusion. The patient reported the insidious onset of a new, palpable, firm mass developing deep within the anterior muscle belly. This mass gradually increased in size over the ensuing weeks and became progressively painful, particularly during eccentric quadriceps loading and deep knee flexion.
Progression of Symptoms and Systemic Review
The pain was characterized as a deep, unrelenting, aching sensation that did not radiate along specific dermatomal or peripheral nerve pathways. The discomfort was mechanically exacerbated by physical activity, specifically running and stair climbing, and was only partially ameliorated by rest. Notably, the patient reported an increasing mechanical block to terminal knee flexion, severely limiting his athletic participation and eventually interfering with activities of daily living.
A comprehensive review of systems was negative for constitutional symptoms. The patient explicitly denied any history of fevers, chills, night sweats, unexplained weight loss, or generalized fatigue, which are critical historical data points when evaluating a rapidly enlarging soft tissue mass. Furthermore, the patient reported no prior history of orthopedic trauma to the affected extremity, no personal or family history of metabolic bone diseases, connective tissue disorders, or primary musculoskeletal malignancies. He denied any history of spontaneous bleeding diatheses or anticoagulant utilization.
Pathophysiological Context of the Presentation
The clinical timeline presented by this patient is the hallmark of myositis ossificans traumatica, a form of heterotopic ossification characterized by the aberrant formation of non-neoplastic bone and cartilage within skeletal muscle and adjacent soft tissues following mechanical trauma. The pathophysiology involves a complex inflammatory cascade initiated by the initial hematoma and muscle necrosis. Local tissue hypoxia, combined with the release of inflammatory cytokines and bone morphogenetic proteins from injured skeletal muscle and infiltrating macrophages, stimulates the inappropriate differentiation of resident mesenchymal stem cells into osteoprogenitor cells. The classic temporal presentation—trauma followed by a latent period, subsequent mass formation, and progressive mechanical restriction—requires a high index of suspicion to avoid the catastrophic misdiagnosis of a malignant soft tissue or bone sarcoma.
Clinical Examination Findings
Inspection of the Extremity
On physical examination of the left lower extremity, the patient was observed in both the standing and supine positions. Inspection of the left thigh revealed a subtle but distinct asymmetry compared to the contralateral limb. A localized, firm fullness was visually apparent in the anteromedial aspect of the middle third of the thigh, approximately 10 centimeters proximal to the superior pole of the patella. The overlying cutaneous tissue was entirely normal; there was no evidence of erythema, induration, superficial venous engorgement, or cutaneous tethering. The skin integrity was intact with no prior surgical scars or sinus tracts. Muscle bulk of the vastus medialis obliquus and vastus lateralis appeared symmetrical bilaterally, with no gross evidence of disuse atrophy or fasciculations, suggesting intact gross motor innervation.
Palpation and Soft Tissue Assessment
Palpation was performed meticulously to assess the characteristics of the mass and its relationship to surrounding anatomical structures. Examination revealed a firm, woody, well-circumscribed mass measuring approximately 6 by 4 centimeters in its axial and sagittal dimensions. The mass was deeply situated, appearing to originate within the vastus intermedius muscle belly, deep to the rectus femoris. It was exquisitely tender to direct, deep palpation.
The mass exhibited no mobility in the transverse or longitudinal planes, feeling firmly fixed to the surrounding muscular architecture. However, with the quadriceps relaxed, the mass could be slightly translated independently of the underlying femoral diaphysis, suggesting a lack of direct periosteal or cortical continuity, a critical finding when differentiating from parosteal osteosarcoma or sessile osteochondroma. There was no palpable crepitus, fluctuance, or pulsatility. Minimal localized warmth was appreciated directly over the mass compared to the surrounding soft tissue, consistent with the hyperemic phase of heterotopic bone formation.
Range of Motion and Functional Deficits
A comprehensive assessment of the active and passive range of motion of the left hip and knee was conducted. Hip range of motion, including flexion, extension, internal rotation, and external rotation, was symmetric to the contralateral side and entirely pain-free, ruling out referred pathology from the coxofemoral joint.
Knee kinematics, however, were significantly altered. Active and passive knee flexion was strictly limited to 90 degrees, compared to 140 degrees on the uninjured contralateral side. Attempted flexion beyond 90 degrees elicited a firm, mechanical end-feel accompanied by severe, localized pain over the anterior thigh mass, indicative of a tethering effect within the extensor mechanism. Knee extension was full and symmetric (0 degrees); however, resisted terminal knee extension (quadriceps isometric contraction) provoked sharp pain at the site of the mass. The Ely test was positive, demonstrating rectus femoris tightness and localized pain, further localizing the pathology to the anterior compartment musculature.
Neurological and Vascular Assessment
A detailed distal neurological examination was performed to rule out compressive neuropathy or compartment syndrome. Sensation was intact to light touch and pinprick across the L2 through S1 dermatomes, including the distributions of the saphenous, superficial peroneal, deep peroneal, sural, and tibial nerves. Motor strength testing demonstrated 5/5 power in the hip flexors (L2-L3), hamstrings (L5-S1), tibialis anterior (L4), extensor hallucis longus (L5), and gastrocnemius-soleus complex (S1). Quadriceps strength (L3-L4) was technically 5/5, although testing was limited by pain inhibition.
Vascular examination revealed palpable, bounding, and symmetric femoral, popliteal, dorsalis pedis, and posterior tibial pulses. Capillary refill in the distal digits was brisk, occurring in under two seconds. The compartments of the leg and thigh were soft and compressible, with no clinical indications of acute or chronic exertional compartment syndrome.
Imaging and Diagnostics
Radiographic Evaluation
The diagnostic workup for suspected myositis ossificans relies heavily on the temporal evolution of radiographic findings, which mirror the histological maturation of the heterotopic bone. Initial plain radiographs of the left femur and knee (anteroposterior and lateral projections) obtained in the emergency department immediately following the initial trauma were entirely unremarkable. They demonstrated normal osseous architecture with no evidence of acute fracture, periosteal reaction, or abnormal soft tissue radiodensities.
Follow-up radiographs obtained at six weeks post-injury, coinciding with the clinical emergence of the palpable mass, revealed subtle, amorphous, flocculent calcifications within the soft tissues of the anterior thigh. These early calcifications were ill-defined and lacked a distinct trabecular pattern, representing the early osteoid formation phase.
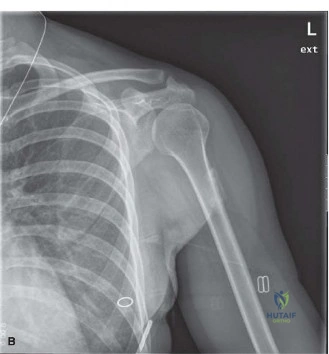
Figure 1: Initial radiograph demonstrating early, ill-defined soft tissue calcification within the quadriceps muscle, approximately 6 weeks post-trauma.
By the twelve-week mark, repeat radiographs demonstrated a dramatic evolution. The lesion exhibited a highly organized pattern of ossification characterized by a distinct, mature, radiodense peripheral rim surrounding a more radiolucent, immature center. This centrifugal pattern of maturation is the classic radiographic "zone phenomenon" that is virtually pathognomonic for myositis ossificans. Crucially, orthogonal radiographic views confirmed a distinct radiolucent cleft separating the ossified mass from the underlying femoral cortex, with absolutely no evidence of cortical destruction, endosteal scalloping, or aggressive periosteal reactions (such as Codman's triangle or sunburst appearance), which strongly militated against a primary malignant bone tumor.
Computed Tomography Findings
To further characterize the lesion, delineate its exact anatomical relationship to the neurovascular bundle, and confirm the diagnosis, a non-contrast Computed Tomography scan of the left thigh was obtained. The CT scan is considered the gold standard imaging modality for demonstrating the zonal phenomenon, particularly in the intermediate stages of maturation where plain radiographs may remain equivocal.

Figure 2: Advanced imaging demonstrating the distinct zonal maturation pattern, with peripheral cortical bone formation and a central radiolucent core, confirming the benign nature of the heterotopic ossification.
The axial, coronal, and sagittal CT reconstructions revealed a well-circumscribed, ovoid soft tissue mass localized entirely within the vastus intermedius muscle. The scan exquisitely demonstrated the peripheral rim of mature cortical bone surrounding a central region of lower attenuation, corresponding to immature osteoid and cellular fibrous tissue. The CT scan definitively confirmed the presence of an intact fascial plane and a clear radiolucent cleft between the ossified mass and the anterior femoral cortex, ruling out parosteal osteosarcoma, which typically arises from the periosteum and exhibits a broad-based attachment to the underlying bone with central, rather than peripheral, maturation.
Magnetic Resonance Imaging Characteristics
While CT is optimal for evaluating the pattern of mineralization, Magnetic Resonance Imaging was utilized to assess the extent of surrounding soft tissue edema and to definitively rule out soft tissue sarcoma. The MRI findings in myositis ossificans are highly dependent on the chronological stage of the lesion and can be notoriously deceptive in the early, acute phase.
In this patient's subacute to chronic presentation (12 weeks), the MRI demonstrated a well-defined intramuscular mass. On T1-weighted sequences, the lesion exhibited a peripheral rim of low signal intensity corresponding to the mature cortical bone, with a central area of intermediate signal intensity. On T2-weighted and Short Tau Inversion Recovery sequences, the mature peripheral rim remained hypointense, while the central core demonstrated heterogeneous hyperintensity, reflecting ongoing cellular activity and immature osteoid.
Importantly, the extensive, ill-defined surrounding muscle edema that characterizes the early, hyperemic phase of myositis ossificans—which can easily be misconstrued as the peritumoral edema of a high-grade soft tissue sarcoma—had largely resolved. The mass was contained entirely within the epimysium of the vastus intermedius, with no neurovascular invasion or joint involvement.
Histological Evaluation and Biopsy Considerations
A critical decision in the diagnostic algorithm of this case was the deliberate avoidance of an early tissue biopsy. The histological appearance of myositis ossificans, much like its radiographic appearance, evolves over time and is defined by the "Zones of Ackerman."
If a biopsy is performed during the early, highly active phase (weeks 2 to 6), the central zone of the lesion consists of rapidly proliferating, highly pleomorphic spindle cells with frequent mitotic figures. This hypercellular, disorganized stroma is virtually indistinguishable from an extraskeletal osteosarcoma or a high-grade soft tissue sarcoma. Misinterpretation of this early histology has historically led to catastrophic, inappropriate radical resections or amputations.
As the lesion matures, it develops three distinct histological zones: an inner zone of cellular, fibroblastic tissue; an intermediate zone of immature osteoid and cartilage; and an outer zone of mature, lamellar trabecular bone. Because the clinical history, physical examination, and the classic centrifugal maturation pattern observed on serial radiographs and CT scans were definitively concordant with myositis ossificans, a biopsy was deemed not only unnecessary but potentially hazardous due to the risk of diagnostic confusion and the potential to seed the surrounding tissue, exacerbating the heterotopic ossification.
Differential Diagnosis
The presentation of a rapidly enlarging, painful soft tissue mass in a young adult necessitates a broad and carefully considered differential diagnosis. The primary objective is to differentiate benign, reactive processes from primary malignant bone or soft tissue sarcomas. The following table outlines the key differentiating features of the most critical pathologies in this diagnostic algorithm.
| Pathology | Clinical Presentation | Radiographic Hallmarks | Histological Features |
|---|---|---|---|
| Myositis Ossificans | History of trauma, painful mass, mechanical restriction. Young athletes. | Centrifugal maturation (zonal phenomenon). Peripheral mature bone, radiolucent center. Cleft separating from bone. | Zones of Ackerman. Peripheral mature lamellar bone, intermediate osteoid, central cellular stroma. |
| Extraskeletal Osteosarcoma | Painful, enlarging mass. Often no trauma history. Older demographic (50+). | Centripetal maturation. Central dense ossification with an ill-defined, immature, radiolucent periphery. | Highly pleomorphic malignant spindle cells producing malignant osteoid. High mitotic rate throughout. |
| Parosteal Osteosarcoma | Slow-growing, painless mass. Posterior distal femur most common. | Broad-based attachment to the underlying cortex. Central dense ossification. "String sign" occasionally seen. | Low-grade malignant spindle cells in a fibrous stroma with well-formed woven bone trabeculae. |
| Soft Tissue Sarcoma (e.g., Synovial) | Painless or painful enlarging mass. Deep to fascia. | Soft tissue mass, often without significant calcification (though synovial sarcoma can calcify). Bone erosion possible. | Varies by subtype. Synovial sarcoma shows biphasic (epithelial and spindle cell) or monophasic patterns. |
| Osteochondroma (Sessile) | Painless mass, mechanical symptoms. Often discovered incidentally. | Cortical and medullary continuity with the host bone. Cartilage cap (seen on MRI). | Mature trabecular bone covered by a benign hyaline cartilage cap. |
Extraskeletal Osteosarcoma
Extraskeletal osteosarcoma is a highly malignant mesenchymal tumor that produces osteoid but occurs entirely within the soft tissues, without primary bone involvement. While it can present as a rapidly enlarging mass, it typically affects an older demographic (patients over 50 years of age). Radiographically, it is the exact inverse of myositis ossificans. Extraskeletal osteosarcoma exhibits a "centripetal" pattern of ossification, where the central portion of the tumor is densely mineralized and mature, while the peripheral advancing edge remains radiolucent, ill-defined, and highly aggressive. This distinction is the single most important radiographic parameter in differentiating the two entities.
Parosteal Osteosarcoma
Parosteal osteosarcoma is a low-grade, surface-based osteosarcoma that typically arises from the periosteum of the metaphysis of long bones, most classically the posterior aspect of the distal femur. Unlike myositis ossificans, which is separated from the host bone by a distinct radiolucent cleft of normal muscle tissue, parosteal osteosarcoma has a broad-based, sessile attachment to the underlying cortex. Over time, it can invade the medullary canal. The ossification pattern is dense and central, lacking the organized peripheral rim seen in myositis ossificans.
Soft Tissue Sarcoma
High-grade soft tissue sarcomas, such as undifferentiated pleomorphic sarcoma or synovial sarcoma, must always be considered in the differential of a deep intramuscular mass. While synovial sarcomas can exhibit stippled calcifications in up to 30% of cases, they do not form the organized, trabecular bone pattern seen in heterotopic ossification. MRI is crucial here; sarcomas typically demonstrate heterogeneous signal intensity, extensive peritumoral edema, and central necrosis, and they lack the distinct low-signal peripheral rim of mature bone on T1 and T2 sequences.
Surgical Decision Making and Classification
Indications for Operative Intervention
The management of myositis ossificans is predominantly non-operative, focusing on symptomatic relief, physical therapy, and allowing the lesion to naturally mature and, in many cases, spontaneously resorb over several years. Operative intervention is strictly reserved for specific, refractory clinical scenarios.
In this patient's case, the indications for surgical excision were clearly met. The primary indication was the severe, persistent mechanical block to knee flexion (limited to 90 degrees) that had plateaued despite an exhaustive course of conservative management and physical therapy. This mechanical tethering of the vastus intermedius severely restricted his functional capacity and precluded his return to athletic activities. Secondary indications included chronic, localized pain caused by the mass impinging on surrounding muscle fibers during contraction, and the psychological burden of a persistent, large thigh mass. Excision is also indicated if the mass causes neurovascular compression, though this was not present in our patient.
Timing of Surgical Excision
The timing of surgical resection is arguably the most critical variable in the operative management of myositis ossificans. Premature excision of an immature, metabolically active lesion is associated with an unacceptably high rate of massive, aggressive recurrence, often resulting in a larger and more debilitating mass than the original lesion.
Surgical intervention must be delayed until the heterotopic bone has reached complete metabolic and radiographic maturity. Clinically, this is indicated by the cessation of local pain at rest and a plateau in the size of the mass. Radiographically, maturity is confirmed by the presence of a well-defined, dense cortical rim and a clear trabecular pattern on plain films and CT scans.
Metabolic maturity can be assessed via laboratory and advanced imaging modalities. Serum alkaline phosphatase levels, which are often elevated during the active osteogenic phase, must return to normal baseline levels. Furthermore, a Technetium-99m methylene diphosphonate three-phase bone scan can be utilized; a maturing lesion will demonstrate progressively decreasing radiotracer uptake, and surgery should ideally be deferred until the scan shows minimal to no active uptake compared to the contralateral side. In this patient, surgery was scheduled at 9 months post-injury, at which point serial imaging confirmed complete cortical maturation, and serum alkaline phosphatase had normalized.
Prophylactic Measures Against Recurrence
Given the inherent risk of recurrence following the excision of heterotopic bone, perioperative prophylactic measures are paramount. The two primary modalities are pharmacological prophylaxis and localized radiation therapy.
Pharmacological prophylaxis typically involves the administration of non-steroidal anti-inflammatory drugs, specifically Indomethacin. Indomethacin acts as a potent non-selective cyclooxygenase inhibitor, thereby blocking the synthesis of Prostaglandin E2. PGE2 is a critical mediator in the differentiation of mesenchymal stem cells into osteoblasts. The standard protocol involves Indomethacin 75 mg sustained-release daily, or 25 mg three times daily, initiated within 24 hours post-operatively and continued for three to six weeks.
Alternatively, or in conjunction with NSAIDs for high-risk cases, localized external beam radiation therapy can be employed. A single fraction of 700 to 800 centigray administered to the operative bed within 24 to 48 hours post-operatively is highly effective in preventing the proliferation and differentiation of osteoprogenitor cells. For this patient, given his young age, athletic demands, and the large size of the lesion, we opted for a combined approach utilizing post-operative Indomethacin for four weeks.
Surgical Technique and Intervention
Patient Positioning and Anesthesia
The patient was brought to the operating theater and placed in the supine position on a standard radiolucent operating table. General endotracheal anesthesia was induced to ensure complete muscle relaxation, which is critical for mitigating tension on the extensor mechanism during the deep dissection and retraction.
A high thigh tourniquet was placed but not initially inflated, reserved for utilization only in the event of uncontrollable hemorrhage, as continuous assessment of tissue perfusion and meticulous hemostasis are critical in preventing post-operative hematoma formation, a known catalyst for recurrent heterotopic ossification. The left lower extremity was sterilely prepped and draped in the standard orthopedic fashion, allowing for full, unhindered manipulation of the hip and knee joints throughout the procedure.
Surgical Approach to the Anterior Thigh
An anterior approach to the femur was utilized to access the vastus intermedius. A longitudinal incision, approximately 12 centimeters in length, was made over the anteromedial aspect of the thigh, centered directly over the palpable mass. Subcutaneous tissues were sharply dissected down to the level of the fascia lata.
The fascia lata was incised longitudinally in line with the skin incision. The interval between the rectus femoris and the vastus medialis was identified. Using blunt dissection, the rectus femoris was carefully mobilized and retracted laterally, exposing the underlying vastus intermedius fascia. Care was taken to identify and protect the descending branches of the lateral circumflex femoral artery and the motor branches of the femoral nerve innervating the vastus musculature, which course through the proximal aspect of this interval.
Tumor Resection and Soft Tissue Management
Upon exposure of the vastus intermedius, the muscle fibers appeared stretched and draped over the underlying mass. A longitudinal myotomy was performed through the epimysium and muscle fibers of the vastus intermedius directly over the apex of the mass.
The heterotopic bone was encased in a thick, fibrous pseudocapsule. Meticulous dissection was carried out utilizing electrocautery and blunt elevators to separate the pseudocapsule from the surrounding healthy muscle tissue. It is imperative to perform an extracapsular, marginal excision, removing the mass entirely intact. Breaching the pseudocapsule or leaving behind fragments of the heterotopic bone significantly increases the risk of recurrence.
The mass was found to be densely adherent to the deep fibers of the vastus intermedius but, as predicted by the preoperative imaging, had no structural continuity with the periosteum of the anterior femur. The mass was circumferentially freed and delivered from the wound en bloc. The excised specimen was a hard, ovoid structure measuring 6.5 x 4.2 x 3.8 centimeters, and was immediately sent for definitive histopathological analysis to confirm the benign nature of the lesion and rule out any malignant transformation.
Hemostasis and Closure Techniques
Following the extirpation of the mass, a substantial dead space remained within the vastus intermedius muscle belly. Meticulous hemostasis was achieved using bipolar electrocautery and the application of topical hemostatic agents (e.g., oxidized regenerated cellulose) to the raw muscle surfaces. Preventing the formation of a post-operative hematoma is the single most critical surgical step in preventing recurrent myositis ossificans.
To manage the dead space, the vastus intermedius muscle edges were carefully approximated using interrupted figure-of-eight absorbable sutures (e.g., #1 Vicryl), ensuring a tension-free closure that would not restrict future muscle excursion. A closed-suction drain was placed deep within the muscle bed and brought out through a separate, laterally based stab incision to evacuate any residual post-operative bleeding.
The rectus femoris was allowed to fall back into its anatomical position. The fascia lata was closed continuously with a heavy absorbable suture. The subcutaneous tissues were closed in layers, and the skin was approximated using a running subcuticular closure. A sterile, compressive dressing was applied from the toes to the proximal thigh to minimize third-spacing and edema.
Post Operative Protocol and Rehabilitation
