Skeletal Langerhans Cell Histiocytosis: Orthopedic Diagnosis, Biomechanics & Management
Key Takeaway
Skeletal Langerhans Cell Histiocytosis (LCH) involves osteolytic bone lesions causing structural compromise. Orthopedic implications include pathological fracture risk, spinal instability, and neurological deficits. Management often requires diagnostic biopsy and intervention for fractures, instability, or disabling pain. A multidisciplinary approach is crucial for optimal outcomes.
Introduction and Epidemiology
Langerhans Cell Histiocytosis represents a complex and heterogeneous disorder characterized by the clonal proliferation of CD1a and CD207 positive Langerhans cells, which are typically found in the epidermis and mucosa. While historically regarded as an inflammatory or reactive myeloid condition, contemporary molecular pathology has reclassified Langerhans Cell Histiocytosis as an inflammatory myeloid neoplasm. This paradigm shift is driven by the discovery of recurrent somatic mutations activating the MAPK pathway, most notably the BRAF V600E mutation present in approximately 50 to 60 percent of cases, and MAP2K1 mutations in an additional 15 to 20 percent. The clinical spectrum ranges from solitary, self-limiting eosinophilic granulomas to aggressive, multifocal, multisystem disease with significant morbidity and mortality.
Orthopedic involvement, specifically skeletal Langerhans Cell Histiocytosis, is a common presentation, accounting for 80 to 90 percent of all cases. Any bone can be affected, but common sites include the skull, long bones of the appendicular skeleton including the femur and humerus, vertebrae, and the pelvis. The disease exhibits a bimodal age distribution, with a distinct peak incidence in early childhood between 1 and 4 years of age, and a smaller secondary peak in adulthood between 20 and 40 years. The overall incidence is estimated at 5 to 9 cases per million children per year, classifying it as a rare orphan disease. Males are slightly more affected than females.
The primary concern in orthopedic oncology is the aggressive osteolytic nature of these lesions. This osteolysis compromises cortical and cancellous bone integrity, leading to pathological fractures, severe spinal deformity, and potential neurological deficits. Accurate diagnosis utilizing advanced imaging and histopathological confirmation, followed by appropriate multidisciplinary management involving orthopedic oncologists, pediatric hematologist-oncologists, and radiation oncologists, is paramount to optimize patient outcomes and minimize long-term musculoskeletal sequelae.

Surgical Anatomy and Biomechanics
Skeletal involvement typically manifests as sharply defined osteolytic lesions, representing areas of aggressive bone destruction mediated by the infiltrating Langerhans cells, eosinophils, lymphocytes, plasma cells, and multinucleated macrophages. The specific anatomical and biomechanical considerations are highly dependent on the anatomical location of the lesion and the remaining cortical bone stock.
Common Sites and Structural Implications
Cranial lesions, particularly in the temporal or parietal bones, frequently lead to localized pain, palpable soft tissue masses, and rarely, neurological compromise if there is extension involving the dura mater or significant intracranial mass effect. Radiographically, these lesions appear as classic punched out lytic defects with beveled edges due to unequal destruction of the inner and outer tables of the skull.
Vertebral involvement results in the classic vertebra plana, characterized by severe, uniform collapse of a vertebral body. This typically occurs with sparing of the posterior elements and the adjacent intervertebral discs. This collapse can lead to progressive spinal deformity, primarily segmental kyphosis, intractable back pain, and spinal instability. Neurological deficits due to epidural extension or retropulsion of bone fragments into the spinal canal can occur, although they are clinically less common than the radiographic degree of collapse might suggest. The thoracolumbar junction is the most frequently affected spinal segment.
Diaphyseal or metaphyseal lesions in long bones such as the femur, humerus, and tibia are highly problematic. These lytic defects create significant stress risers within the tubular bone architecture, drastically increasing the risk of pathological fractures, particularly in the weight-bearing lower extremities. Lesions extending greater than 50 percent of the cortical circumference or exceeding 2.5 centimeters in axial diameter are universally considered at high risk for catastrophic mechanical failure.
Pelvic lesions frequently present as large, expansive lytic areas within the ilium, ischium, or pubis, causing deep-seated pain and, in massive lesions, pelvic ring instability. Periacetabular involvement is particularly challenging, as it can lead to hip joint subluxation, accelerated secondary osteoarthritis, and severe functional impairment.
Biomechanical Consequences of Osteolysis
The osteolytic process directly and profoundly compromises the structural integrity of the affected bone. Focal cortical defects concentrate mechanical stresses, significantly reducing the bone tolerance to physiological bending, torsional, and axial loads. The reduction in the area moment of inertia makes the bone highly susceptible to spiral or transverse fractures under minimal trauma.
In weight-bearing bones, extensive lytic lesions diminish the capacity to withstand ground reaction forces and muscle pull, predisposing the patient to acute mechanical collapse. In the axial skeleton, vertebral body destruction shifts the instantaneous axis of rotation, leading to anterior column deficiency and progressive axial instability. While vertebra plana in pediatric Langerhans Cell Histiocytosis often demonstrates remarkable spontaneous remodeling and reconstitution of vertebral height over several years, acute collapse with retropulsion may require urgent surgical intervention if progressive neurological deficit or intractable mechanical instability occurs.
Indications and Contraindications
The management paradigm for skeletal Langerhans Cell Histiocytosis has shifted significantly over the past two decades. Historically treated with aggressive surgical curettage or en bloc resection, the current approach heavily favors minimally invasive techniques, medical management, and observation for asymptomatic lesions. Surgery is now primarily reserved for obtaining diagnostic tissue, preventing impending pathological fractures, stabilizing acute fractures, and decompressing neural elements.
| Clinical Scenario | Operative Indications | Non Operative Indications |
|---|---|---|
| Diagnostic Uncertainty | Open or core needle biopsy required to confirm diagnosis and obtain tissue for molecular profiling (BRAF/MAP2K1). | Classic radiographic appearance in a patient with known, biopsy-proven multisystem LCH. |
| Appendicular Skeleton | Impending pathological fracture (Mirels score > 8), acute displaced fracture, massive cortical destruction (>50% circumference). | Asymptomatic lesions, small lesions (<2.5 cm), lesions responding to systemic chemotherapy or targeted BRAF inhibitors. |
| Axial Skeleton | Progressive neurological deficit, epidural spinal cord compression, severe and progressive kyphotic deformity, spinal instability. | Asymptomatic vertebra plana, stable kyphosis without neurological compromise (high potential for spontaneous remodeling). |
| Pelvis and Acetabulum | Impending protrusion acetabuli, severe structural instability of the pelvic ring. | Contained iliac wing lesions, asymptomatic pubic rami lesions. |
| Craniofacial | Lesions causing severe mass effect, impending visual loss (orbital lesions), or significant dural compromise. | Asymptomatic calvarial lesions, small isolated skull defects. |
Absolute and Relative Contraindications
Absolute contraindications to surgical intervention include the presence of active, uncontrolled systemic infection or severe coagulopathy that cannot be medically optimized. Surgery is also contraindicated if the primary goal is curative wide resection of a solitary bone lesion, as intralesional curettage combined with systemic or local adjuvant therapy has proven equally effective with significantly lower morbidity.
Relative contraindications include operating on highly vascular lesions without prior embolization, or undertaking major reconstructive surgery in patients with aggressive, uncontrolled multisystem disease where systemic targeted therapy (such as Vemurafenib for BRAF V600E mutated LCH) may rapidly shrink the tumor burden and negate the need for extensive orthopedic reconstruction.
Pre Operative Planning and Patient Positioning
Thorough preoperative planning is essential to minimize surgical morbidity and ensure accurate diagnostic yield. The multidisciplinary team must coordinate the timing of biopsy and definitive stabilization, often integrating systemic therapy induction protocols.
Diagnostic Imaging Strategy
Standard orthogonal radiographs remain the initial modality of choice, revealing the classic geographic lytic lesions without sclerotic margins in early phases, and potentially periosteal reaction in later phases. Advanced imaging is mandatory for surgical planning. Magnetic Resonance Imaging with and without intravenous gadolinium contrast is the gold standard for evaluating the extent of intramedullary disease, cortical breakthrough, soft tissue extension, and the proximity of the lesion to neurovascular bundles and physes.
Computed Tomography is highly valuable for assessing residual cortical bone stock, planning the trajectory for core needle biopsies, and evaluating the exact geometry of impending fractures. To stage the disease and identify multifocal skeletal involvement, a whole-body PET-CT or a technetium-99m bone scan combined with a radiographic skeletal survey is required.
Biopsy Principles and Histopathology
Biopsy is the critical first step in management. The biopsy tract must be carefully planned so that it can be excised during future surgical approaches if the lesion proves to be a primary bone sarcoma rather than Langerhans Cell Histiocytosis. Core needle biopsy under fluoroscopic or CT guidance is generally preferred over open biopsy to minimize the risk of iatrogenic fracture and tumor seeding.
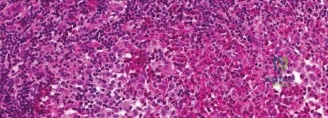
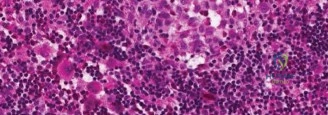
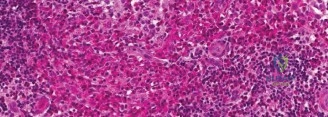
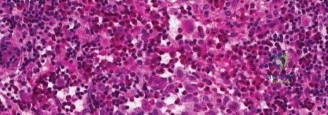
Multiple cores should be obtained and sent fresh for flow cytometry, standard hematoxylin and eosin staining, and comprehensive molecular profiling. The pathologist will look for the characteristic grooved, coffee-bean shaped nuclei of Langerhans cells, admixed with eosinophils. Immunohistochemistry must confirm positivity for CD1a, S100, and Langerin (CD207).
Patient Positioning and Operating Room Setup
Positioning is dictated by the anatomical location of the lesion and the planned surgical intervention. For proximal femoral lesions requiring prophylactic intramedullary nailing, the patient is positioned supine on a radiolucent fracture table with the operative leg placed in traction. This allows for unimpeded intraoperative fluoroscopy in both anteroposterior and lateral planes.
For spinal decompression and posterior stabilization, the patient is positioned prone on a Jackson spinal table with all bony prominences meticulously padded. The abdomen must hang free to decrease epidural venous engorgement and minimize intraoperative blood loss. Neurophysiological monitoring, including Somatosensory Evoked Potentials and Motor Evoked Potentials, is standard setup for any spinal intervention involving deformity correction or decompression.
Detailed Surgical Approach and Technique
Surgical intervention in skeletal Langerhans Cell Histiocytosis requires meticulous technique to achieve adequate intralesional clearance while preserving maximal host bone stock, particularly in the pediatric population where physeal preservation is paramount.
Appendicular Skeleton Curettage and Prophylactic Fixation
For a large, impending pathological fracture of the long bones, the standard approach involves intralesional curettage, local adjuvant treatment, bone grafting, and prophylactic internal fixation.
The surgical approach utilizes standard internervous planes to expose the affected bone. For a distal femoral lesion, a lateral approach elevating the vastus lateralis from the lateral intermuscular septum provides excellent exposure. A cortical window is created using a high-speed burr or osteotomes. The window must be large enough to allow thorough visualization and access to the entire medullary cavity but small enough to avoid creating a massive structural defect.
Aggressive intralesional curettage is performed using varying sizes of angled curettes. The goal is to remove all macroscopic gross tumor tissue. Following curettage, the cavity is treated with a high-speed burr to extend the margin by 1 to 2 millimeters into normal cancellous bone, breaking down the microscopic tumor extensions. While chemical adjuvants like phenol or liquid nitrogen cryotherapy are frequently used in giant cell tumors or chondroblastomas, their use in Langerhans Cell Histiocytosis is less standardized and often avoided in young children due to the risk of adjacent physeal damage or excessive bone necrosis.
The resulting cavitary defect is then packed tightly with bone graft. Autologous cancellous bone graft from the iliac crest remains the gold standard for osteoinduction and osteoconduction, but allograft chips or synthetic bone substitutes (such as calcium phosphate or calcium sulfate cements) are frequently utilized to avoid donor site morbidity.
Finally, prophylactic internal fixation is applied to bypass the stress riser. In the diaphysis, load-sharing intramedullary nails are biomechanically superior. In the metaphysis or in young children with open physes, load-bearing locking plate constructs spanning the entire length of the bone are preferred to protect the structural integrity without violating the growth plates.
Axial Skeleton Decompression and Stabilization
Surgical management of spinal Langerhans Cell Histiocytosis is reserved for severe cases with progressive neurological deficit or gross mechanical instability. The standard technique involves a posterior approach for decompression and instrumented fusion.
A midline longitudinal incision is made, and the paraspinal musculature is elevated subperiosteally to expose the posterior elements of the affected levels and at least two levels above and below. Pedicle screws are inserted under fluoroscopic or navigation guidance. In pediatric patients, care must be taken to accommodate the smaller pedicle morphology.
If epidural tumor extension is causing cord compression, a laminectomy or transpedicular decompression is performed. The tumor tissue is often soft, friable, and highly vascular. Meticulous hemostasis using bipolar electrocautery and hemostatic agents is critical.
Anterior column reconstruction is rarely necessary in Langerhans Cell Histiocytosis. Unlike metastatic carcinoma or multiple myeloma, the vertebra plana in LCH has a remarkable capacity for spontaneous reconstitution over time once the active disease process is halted. Therefore, stabilizing the posterior tension band with rigid rod constructs is usually sufficient to prevent progressive kyphosis while allowing the anterior column to heal and remodel. Posterolateral decortication and application of bone graft complete the fusion process.
Complications and Management
Surgical management of skeletal Langerhans Cell Histiocytosis carries specific risks related to the aggressive nature of the osteolysis, the altered biomechanics of the host bone, and the unique physiological considerations of the pediatric patient population.
| Complication | Estimated Incidence | Prevention and Management Strategies |
|---|---|---|
| Local Recurrence | 10% - 20% | Ensure aggressive mechanical burring during curettage. Manage recurrences with repeat curettage, intralesional corticosteroid injection, or systemic targeted therapy (BRAF inhibitors). |
| Pathological Fracture | 5% - 15% (Post-curettage) | Utilize robust prophylactic internal fixation spanning the entire bone. Restrict weight-bearing until radiographic consolidation of the bone graft is evident. |
| Physeal Arrest | 5% - 10% (Pediatric cases) | Avoid curettage or burring directly against the growth plate. Use intraoperative fluoroscopy to confirm instrument position. Monitor for limb length discrepancy and angular deformity postoperatively. |
| Hardware Failure | < 5% | Select appropriate load-sharing implants. Ensure adequate bone grafting to support the construct. Revise with larger implants and structural allograft if failure occurs. |
| Spinal Deformity Progression | 10% - 15% (Vertebra plana) | Close radiographic surveillance of vertebra plana. Apply rigid posterior instrumentation spanning multiple levels if instability or progressive kyphosis is identified. |
| Infection | 2% - 5% | Strict adherence to sterile technique, prophylactic intravenous antibiotics, and meticulous soft tissue handling. Treat deep infections with aggressive surgical debridement and culture-directed antibiotics. |
In the pediatric population, the most devastating long-term complication is iatrogenic physeal arrest. If the LCH lesion is juxtaphyseal, the surgeon must balance the need for adequate tumor clearance with the preservation of the growth plate. If premature physeal closure occurs, it can lead to significant limb length discrepancy or angular deformity, necessitating complex reconstructive procedures such as epiphysiodesis of the contralateral limb, or distraction osteogenesis using external fixators.
Post Operative Rehabilitation Protocols
Postoperative rehabilitation must be highly individualized, taking into account the anatomical location of the lesion, the extent of bone destruction, the type of surgical stabilization performed, and the patient age and compliance level.
Appendicular Skeleton Rehabilitation
Rehabilitation following curettage and prophylactic fixation of the lower extremity generally follows a phased approach.
Phase 1 focuses on tissue protection and early mobilization. Patients are typically restricted to toe-touch or partial weight-bearing using crutches or a walker for the first 6 to 8 weeks. Continuous passive motion and active-assisted range of motion exercises for adjacent joints are initiated immediately to prevent capsular contracture and maintain cartilage nutrition.
Phase 2 begins once there is radiographic evidence of early bone graft incorporation and callus formation, typically around 8 to 12 weeks. Weight-bearing is progressively advanced to full. The focus shifts to active muscle strengthening, emphasizing the quadriceps, hamstrings, and gluteal musculature to restore dynamic joint stability. Proprioceptive training and closed kinetic chain exercises are introduced.
Phase 3 involves return to full activity and sports. This is generally permitted only after complete radiographic consolidation of the lesion, incorporation of the bone graft, and recovery of at least 90 percent of contralateral limb strength. This process can take 6 to 12 months depending on the initial defect size.
Axial Skeleton Rehabilitation
Following posterior spinal fusion and decompression, patients are mobilized early, often on postoperative day one, to prevent pulmonary complications and deep vein thrombosis. Depending on the rigidity of the fixation construct and the patient bone quality, a custom-molded Thoracolumbosacral Orthosis may be prescribed for 3 to 6 months to provide supplemental external support and limit extreme ranges of motion.
Physical therapy focuses on isometric core strengthening, paraspinal muscle activation, and gait training. High-impact activities, heavy lifting, and contact sports are strictly prohibited until solid arthrodesis is confirmed on dynamic radiographs or computed tomography, which typically requires 6 to 12 months.
Summary of Key Literature and Guidelines
The management of Langerhans Cell Histiocytosis is guided by international consensus protocols, primarily those developed by the Histiocyte Society. The LCH-III and LCH-IV protocols have established clear guidelines for risk stratification and treatment, demonstrating that isolated skeletal lesions often respond excellently to minimal intervention, including observation, intralesional corticosteroid injection, or limited curettage.
Recent academic literature has been revolutionized by the discovery of the BRAF V600E mutation by Badalian-Very et al. in 2010. This landmark finding shifted the classification of LCH to a myeloid neoplasm and opened the door for targeted molecular therapies. Studies evaluating BRAF inhibitors, such as Vemurafenib and Dabrafenib, have shown dramatic and rapid clinical responses in patients with severe, refractory, or multisystem skeletal disease, frequently rendering massive, technically unresectable orthopedic lesions amenable to conservative management or simplified surgical stabilization.
Furthermore, long-term natural history studies on vertebra plana, such as those by Garg et al., have definitively proven the high potential for spontaneous vertebral remodeling in children with LCH. These studies caution against aggressive anterior corpectomy and structural grafting, advocating instead for isolated posterior stabilization only when strict criteria for instability or neurological deficit are met. The contemporary orthopedic surgeon must integrate these molecular advancements and conservative natural history data to provide optimal, evidence-based care for patients with skeletal Langerhans Cell Histiocytosis.
