Middle-Third Clavicle Fractures: An Exhaustive Review of Anatomy, Pathophysiology, and Management
Key Takeaway
Middle-third clavicle fractures are frequent traumas exhibiting specific displacement patterns. While non-operative historically, operative fixation is now favored for significantly displaced or comminuted cases to reduce symptomatic malunion and nonunion. Thorough neurovascular assessment and biomechanical understanding are crucial for optimizing patient outcomes.
Introduction and Epidemiology
Middle-third clavicle fractures represent a substantial portion of orthopedic trauma, accounting for 2-10% of all fractures and 45-80% of all clavicle fractures. The clavicle is the most commonly fractured bone in the adult population. Its subcutaneous location and biomechanical role as a strut connecting the axial skeleton to the upper extremity render it vulnerable to injury. These fractures exhibit a bimodal distribution, with a high incidence in young, active males due to high-energy trauma and in elderly females often associated with osteoporosis and low-energy falls.

The mechanism of injury is typically a direct blow to the superior aspect of the shoulder, or an indirect force transmitted through the arm during a fall onto an outstretched hand. Associated injuries, though uncommon for isolated midshaft fractures, can include scapular fractures, rib fractures, pneumothorax, brachial plexus injury, or subclavian vessel compromise. This is particularly true in high-energy trauma or highly displaced fractures. A thorough neurovascular examination is paramount in the initial assessment.
Historically, the vast majority of middle-third clavicle fractures were managed non-operatively with good results. However, growing evidence highlighting higher rates of malunion and symptomatic nonunion, particularly in significantly displaced and comminuted fractures, has shifted the treatment paradigm towards operative fixation for select indications. This document aims to provide an exhaustive academic review of the classification, treatment rationale, and strategies for optimizing outcomes in middle-third clavicle fractures.
Fracture Classification Systems
Accurate classification is essential for guiding treatment and standardizing research. The Allman classification divides the clavicle into thirds, with Group I representing middle-third fractures. The Robinson classification provides a more granular prognostic framework for midshaft fractures (Type 2). Within Robinson Type 2, injuries are subdivided based on displacement and comminution. Type 2A represents non-displaced fractures, while Type 2B represents displaced fractures. Type 2B is further subdivided into 2B1 (simple or single butterfly fragment) and 2B2 (comminuted or segmental). This distinction is critical, as Robinson Type 2B2 fractures carry a significantly higher risk of nonunion when managed non-operatively.
Surgical Anatomy and Biomechanics
The clavicle is a unique S-shaped long bone, acting as a strut that maintains the length of the shoulder girdle and provides attachment for numerous muscles and ligaments. Its subcutaneous position along its entire length makes it susceptible to direct trauma and allows for easy palpation of fracture deformities.
Bony Anatomy
The clavicle has a medial sternal end, a middle third shaft, and a lateral acromial end. The middle third is the thinnest and most acutely curved portion, predisposing it to fracture. The medial third is round and articulates with the manubrium via the sternoclavicular joint. The middle third is typically prismatic, becoming flatter laterally. It lacks a medullary canal, instead containing cancellous bone and trabeculae, which has implications for intramedullary nailing. The lateral third is flat and articulates with the acromion via the acromioclavicular joint.
Muscular Attachments and Displacement Forces
Crucial muscle attachments dictate the classic displacement patterns observed in midshaft fractures. The sternocleidomastoid originates from the medial clavicle and sternum, inserting onto the mastoid process. Its unopposed pull on the medial fracture fragment causes superior and posterior displacement. The pectoralis major originates from the medial clavicle and sternum, contributing to medial fragment stability but also driving shortening.
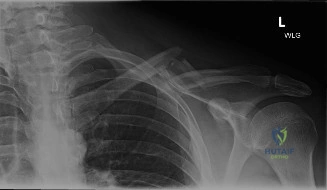
The deltoid originates from the lateral clavicle and acromion. Its weight, combined with the mass of the upper extremity, exerts a strong inferior force on the lateral fragment. The trapezius provides superior support to the lateral fragment, though its effect is invariably overwhelmed by the deltoid and arm weight in displaced fractures. The subclavius muscle originates from the first rib and inserts onto the inferior surface of the clavicle, offering a critical anatomical buffer that protects underlying neurovascular structures from fracture spikes and iatrogenic injury during drilling.
Ligamentous Attachments
The primary ligamentous stabilizers for midshaft fractures are the coracoclavicular ligaments and the costoclavicular ligament. Comprising the conoid and trapezoid ligaments, the coracoclavicular ligaments connect the clavicle to the coracoid process, providing primary vertical stability to the acromioclavicular joint and the lateral clavicle. The costoclavicular ligament anchors the medial clavicle to the first rib, resisting superior displacement forces.
Neurovascular Proximity
The neurovascular anatomy in the vicinity of the middle-third clavicle demands meticulous surgical technique. The subclavian artery and vein, along with the cords and divisions of the brachial plexus, lie directly posterior and inferior to the middle third of the clavicle. The distance between the posterior cortex of the clavicle and the subclavian vein can be as little as 10 to 15 millimeters. Furthermore, the supraclavicular nerves descend over the clavicle to provide sensation to the anterior chest wall. These cutaneous branches are highly variable and are frequently encountered during surgical approaches, requiring careful mobilization to prevent postoperative chest wall numbness or painful neuroma formation.
Indications and Contraindications
The decision to proceed with operative versus non-operative management hinges on patient-specific factors, fracture morphology, and the risk profile for nonunion or symptomatic malunion. Non-operative management remains the gold standard for non-displaced or minimally displaced fractures, utilizing a sling for comfort followed by progressive range of motion. However, operative osteosynthesis is increasingly favored for specific morphological criteria that predict failure of conservative care.
Operative Versus Non Operative Decision Matrix
| Management Strategy | Indications | Relative Contraindications |
|---|---|---|
| Non-Operative | Non-displaced fractures | High-demand overhead athletes |
| Minimal displacement under 100 percent | Polytrauma requiring early weight bearing | |
| Shortening less than 1.5 cm | Impending skin compromise | |
| Pediatric patients | Floating shoulder variants | |
| Operative Fixation | 100 percent displacement | Active surgical site infection |
| Shortening greater than 2.0 cm | Severe medical comorbidities high anesthesia risk | |
| Z-type comminution Robinson 2B2 | Non-ambulatory patients with low functional demand | |
| Open fractures | Poor soft tissue envelope | |
| Impending skin necrosis tenting | Extreme osteopenia precluding hardware purchase | |
| Associated neurovascular injury | ||
| Floating shoulder double disruption |
Absolute indications for surgery include open fractures, vascular compromise requiring repair, and progressive neurologic deficit. Relative indications, which form the bulk of surgical volume, center on fracture displacement and shortening. Extensive literature demonstrates that shortening greater than 2 centimeters and complete fracture displacement are independent predictors of nonunion and poor functional outcomes, including decreased shoulder endurance and altered scapular kinematics.
Pre Operative Planning and Patient Positioning
Thorough preoperative planning ensures appropriate implant selection and minimizes intraoperative complications. Standard imaging includes an anteroposterior view and a 15 to 30 degree cephalic tilt view to accurately assess superior-inferior displacement. A computed tomography scan is rarely required for isolated midshaft fractures but is invaluable for assessing severe comminution, evaluating medial or lateral extension, or ruling out associated scapular neck fractures in suspected floating shoulder injuries.

Patient Positioning and Setup
The patient is typically placed in a beach chair position with the head of the bed elevated 30 to 45 degrees. This position utilizes gravity to assist in reducing the inferiorly displaced lateral fragment. Alternatively, a supine position with a bump placed between the scapulae can be utilized to allow the shoulders to fall posteriorly, aiding in the restoration of clavicular length.
The head and neck must be secured in a neutral position to avoid excessive traction on the contralateral brachial plexus. The operative arm is prepped and draped free to allow for intraoperative manipulation, which is often necessary to achieve reduction. Fluoroscopy must be brought in from the contralateral side or the head of the bed. The surgeon must confirm that orthogonal views of the entire clavicle can be obtained without obstruction before initiating the incision.
Implant Selection
Surgeons must choose between superior and anteroinferior plating, as well as between pre-contoured locking plates, reconstruction plates, and intramedullary devices. Pre-contoured locking plates offer superior biomechanical stability in comminuted fractures and osteoporotic bone. Superior plating provides a biomechanically advantageous tension band construct against the inferior pull of the arm, but carries a higher risk of hardware prominence. Anteroinferior plating utilizes longer screws in the anterior-to-posterior plane, directs drills away from the subclavian vessels, and generally results in less hardware irritation, though it may be more technically challenging to contour in specific fracture patterns.
Detailed Surgical Approach and Technique
Surgical fixation of middle-third clavicle fractures is predominantly performed via open reduction and internal fixation utilizing plate osteosynthesis. The approach must balance adequate exposure for reduction with the preservation of the soft tissue envelope and periosteal blood supply.
Incision and Superficial Dissection
Two primary incision strategies exist. The traditional approach utilizes a longitudinal incision centered directly over the palpable fracture deformity. Alternatively, a supraclavicular or bikini incision follows the Langer lines of the neck, providing a superior cosmetic outcome.
Following skin incision, the subcutaneous tissues are sharply dissected. The platysma muscle is identified and incised in line with the skin incision. Subplatysmal flaps are elevated to expose the underlying clavipectoral fascia. Meticulous attention must be paid to identifying and protecting the supraclavicular nerve branches. These nerves course perpendicular to the clavicle. Whenever possible, they should be mobilized and retracted using vessel loops. If a branch is encased in scar tissue or unavoidably transected, the proximal stump should be buried in local muscle to prevent painful neuroma formation.
Deep Dissection and Fracture Reduction
The clavipectoral fascia is incised longitudinally over the superior or anteroinferior aspect of the clavicle, depending on the planned plating surface. Periosteal stripping must be strictly minimized to preserve the vascularity of the fracture fragments, particularly in the presence of comminution. Butterfly fragments should not be stripped of their soft tissue attachments.

Reduction is achieved through a combination of manual traction on the arm, direct manipulation of the fragments with bone reduction forceps, and elevation of the lateral fragment. In cases of severe shortening, a lamina spreader or a push-pull screw technique can be utilized to restore length. For simple oblique or spiral fractures, anatomic reduction and provisional fixation with a lag screw can convert the fracture into a stable construct prior to neutralization plating.
Plate Application and Fixation
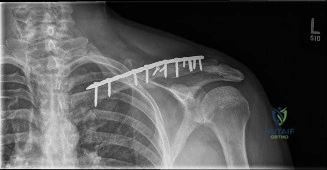
Once provisional reduction is achieved, the selected plate is applied. If a superior plate is chosen, it is positioned on the superior surface of the clavicle. Pre-contoured plates often require minor adjustments using bending irons to perfectly match the patient's unique anatomy. At least three bicortical screws, providing a minimum of six cortices of purchase, must be placed on each side of the fracture.
Drilling must be performed with extreme caution. The drill should be directed carefully, and an oscillating drill attachment or drill stops should be used to prevent plunging through the far cortex and injuring the underlying subclavian vessels or brachial plexus. The use of a blunt retractor or a periosteal elevator placed inferior to the clavicle can provide a physical barrier during drilling and screw measurement.
In comminuted fractures where anatomic reduction of intermediate fragments is impossible or requires excessive soft tissue stripping, bridge plating is the technique of choice. The plate is secured to the main medial and lateral fragments, spanning the comminuted zone to maintain length, alignment, and rotation while preserving the fracture hematoma.
Intramedullary Fixation Alternatives
For specific fracture patterns, particularly simple transverse or short oblique midshaft fractures without significant comminution, intramedullary fixation with titanium elastic nails represents a viable alternative. This minimally invasive technique involves introducing the nail through a small entry portal at the medial or lateral clavicle and advancing it across the fracture site under fluoroscopic guidance. While offering cosmetic advantages and potentially faster time to union due to relative stability, intramedullary nailing is contraindicated in severely comminuted fractures due to the inability to maintain length and rotation.
Closure
Following final fluoroscopic confirmation of reduction and hardware placement, the surgical site is copiously irrigated. The clavipectoral fascia is meticulously closed over the hardware to provide soft tissue coverage and minimize hardware prominence. The platysma is repaired as a distinct layer, followed by subcutaneous and subcuticular skin closure.
Complications and Management
While operative fixation of middle-third clavicle fractures yields high union rates and excellent functional outcomes, it is not without risks. Surgeons must be adept at recognizing and managing both early and late complications.

Common Complications and Salvage Strategies
| Complication | Estimated Incidence | Etiology and Risk Factors | Management and Salvage Strategy |
|---|---|---|---|
| Hardware Prominence | 10 to 30 percent | Subcutaneous anatomy superior plating | Hardware removal after radiographic union typically 12 to 18 months |
| Supraclavicular Nerve Injury | 10 to 25 percent | Iatrogenic transection or traction | Observation gabapentinoids neuroma excision and proximal burial |
| Nonunion | 1 to 5 percent | Infection inadequate fixation smoking | Revision open reduction internal fixation with autologous bone grafting |
| Infection | 1 to 4 percent | Poor soft tissue envelope hematoma | Irrigation and debridement suppressive antibiotics hardware retention until union if stable |
| Adhesive Capsulitis | 2 to 5 percent | Prolonged immobilization lack of rehab | Aggressive physical therapy intra-articular corticosteroid injections manipulation under anesthesia |
| Neurovascular Injury | Under 1 percent | Plunging drill bits sharp fracture spikes | Immediate vascular or neurosurgical consultation and repair |
| Implant Failure | 1 to 2 percent | Premature weight bearing nonunion | Revision osteosynthesis with robust construct and bone grafting |
Hardware prominence is the most frequent complication following plate osteosynthesis, often necessitating a secondary procedure for implant removal. Patients should be counseled preoperatively regarding this possibility. Symptomatic nonunion, while significantly reduced with operative management compared to non-operative treatment of displaced fractures, still occurs. Atrophic nonunions require revision surgery with decortication, rigid internal fixation, and the application of autologous bone graft, typically harvested from the iliac crest. Hypertrophic nonunions, indicating adequate biology but inadequate mechanical stability, generally respond well to revision with a more rigid construct alone.
Infection is a devastating complication that requires aggressive management. Superficial infections may be treated with oral antibiotics, but deep infections necessitate urgent surgical irrigation and debridement. If the fixation remains stable, the hardware should be retained until fracture union occurs, supported by culture-directed suppressive antibiotic therapy. If the fixation is loose, the hardware must be removed, the infection cleared, and the fracture subsequently stabilized, potentially requiring a staged procedure.
Post Operative Rehabilitation Protocols
A structured rehabilitation protocol is vital for restoring shoulder kinematics and preventing stiffness while protecting the surgical construct. Rehabilitation is generally divided into distinct phases based on biological healing timelines.
Phase One Immediate Post Operative to Two Weeks
During the initial two weeks, the primary goals are pain control, wound healing, and prevention of distal edema. The patient is placed in a standard shoulder sling. Pendulum exercises are initiated immediately. Active range of motion of the elbow, wrist, and hand is highly encouraged to prevent stiffness and promote venous return. Active shoulder motion and lifting are strictly prohibited.
Phase Two Two to Six Weeks
As soft tissue healing progresses, the focus shifts to restoring passive and active-assisted range of motion. The sling is gradually weaned for activities of daily living but may be worn in public or during sleep for protection. Supine forward elevation and external rotation exercises are introduced. Pulleys and wand exercises can be utilized. Active lifting remains restricted to the weight of a coffee cup. Radiographs are typically obtained at the six-week mark to assess callus formation.
Phase Three Six to Twelve Weeks
Upon radiographic evidence of progressive union, active range of motion is fully integrated. Isotonic strengthening of the rotator cuff and periscapular stabilizers begins. Resistance band exercises are highly effective in this phase. The patient is permitted to increase lifting weight progressively, guided by pain and functional tolerance.
Phase Four Return to Sport and Heavy Labor
Return to contact sports or heavy manual labor is generally restricted until clinical and radiographic union is absolute, typically between three and four months postoperatively. Premature return to high-impact activities risks catastrophic hardware failure or peri-implant fracture. A functional assessment demonstrating symmetric shoulder strength and full, pain-free range of motion is required before clearance for unrestricted activity.
Summary of Key Literature and Guidelines
The paradigm shift toward operative management of displaced middle-third clavicle fractures is heavily supported by robust level-one evidence.
The landmark 2007 multicenter randomized controlled trial by the Canadian Orthopaedic Trauma Society remains a cornerstone of modern clavicle fracture management. This study compared non-operative treatment with plate fixation for completely displaced midshaft clavicle fractures. The authors demonstrated that operative fixation resulted in significantly lower rates of nonunion and symptomatic malunion. Furthermore, the operative cohort exhibited superior functional outcomes, as measured by DASH and Constant scores, at all time points up to one year, along with an accelerated return to work and sport.
Subsequent literature by Robinson and colleagues further defined the risk factors for nonunion in non-operatively managed fractures. They identified advancing age, female gender, complete displacement, and the presence of severe comminution as independent predictors of failure. This prognostic data is invaluable during shared decision-making with patients in the clinic.
Recent meta-analyses comparing intramedullary nailing to plate osteosynthesis for midshaft fractures have shown comparable union rates and functional outcomes between the two modalities. However, plating remains the more versatile option, capable of addressing complex comminution and significant length discrepancies that are unsuited for intramedullary devices.
Current academic consensus advocates for an individualized approach. While absolute indications for surgery are rare, the relative indications of displacement greater than 100 percent and shortening greater than 2 centimeters warrant a strong recommendation for operative intervention in the active patient to optimize long-term shoulder mechanics and minimize the risk of nonunion. Continuous refinement of implant design, particularly the development of anatomically pre-contoured plates, and a deeper understanding of supraclavicular nerve anatomy continue to drive down complication rates and improve patient outcomes in the surgical management of these common injuries.
