Master ABOS Orthopedic Board Review: Pediatric Infections, Tumors, & Skeletal Dysplasias | Part 6
Key Takeaway
ABOS Pediatric Orthopedics Review Part 6 covers key topics in pediatric orthopedic pathology. It includes newborn septic coxitis, osteomyelitis, benign bone tumors like osteoblastoma, and a wide range of skeletal dysplasias such as achondroplasia, SED, and Morquio syndrome, focusing on their diagnosis, clinical features, and management strategies.
Master ABOS Orthopedic Board Review: Pediatric Infections, Tumors, & Skeletal Dysplasias | Part 6
Comprehensive 100-Question Exam
00:00
Start Quiz
Question 1
A 16-year-old boy presents with back pain. Radiographs reveal an expansile lesion in the spine as shown.
Which of the following is the most likely location of this tumor?
Explanation
Question 2
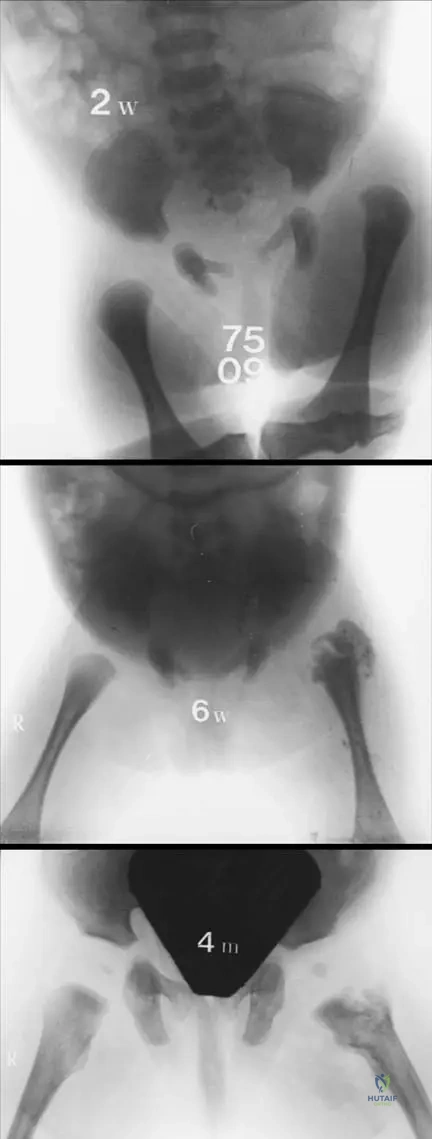
A 2-week-old neonate presents with pseudoparalysis of the right leg and irritability with diaper changes. Ultrasound shows a hip effusion and radiographs reveal subtle changes as shown.
Besides Staphylococcus aureus, which organism is a leading cause of septic arthritis in this age group?
Explanation
Question 3
A 3-year-old boy is diagnosed with Kingella kingae septic arthritis of the knee. What is the most effective method for isolating this fastidious organism from synovial fluid?
Explanation
Question 4
A 14-year-old girl undergoes curettage of a 3.5 cm lytic bone lesion in the distal femur. The histology is shown.
Microscopy reveals loose fibrovascular connective tissue intermixed with irregular osteoid without atypical mitoses. Her pain was poorly relieved by NSAIDs. What is the diagnosis?
Explanation
Question 5
Which of the following gene mutations is responsible for Achondroplasia, resulting in a gain-of-function that inhibits chondrocyte proliferation at the physis?
Explanation
Question 6
A 7-year-old boy presents with fever, swelling, and pain in the midshaft of his femur. Radiographs show a permeative diaphyseal lesion with an onion-skin periosteal reaction. Cytogenetics reveal a t(11;22) translocation. Which fusion gene is associated with this condition?
Explanation
Question 7
A 6-year-old girl with severe short stature, genu valgum, and corneal clouding is evaluated. Radiographs reveal universal platyspondyly and hypoplasia of the odontoid. A urine test is positive for keratan sulfate. What is the most critical orthopedic concern prior to any surgical intervention involving general anesthesia?
Explanation
Question 8
A 13-year-old boy presents with chronic knee pain. Radiographs show an eccentrically located, lytic epiphyseal lesion in the proximal tibia with a sclerotic margin. Biopsy shows mononuclear cells and chicken-wire calcifications. What is the diagnosis?
Explanation
Question 9
A 2-year-old boy with a history of anterolateral tibial bowing develops a pseudoarthrosis after a minor fall. He has multiple cafe-au-lait spots. The underlying genetic mutation affects a protein primarily involved in which of the following cellular pathways?
Explanation
Question 10
A 14-year-old boy presents with chronic, dull back pain. He states the pain is constant and does not significantly improve with ibuprofen. Radiographs are shown.
Which of the following describes the most likely diagnosis?
Explanation
Question 11
A 14-year-old boy presents with progressive back pain that is poorly responsive to NSAIDs. Neurological examination is normal. Radiographs are shown below.
Which of the following characteristics best differentiates this lesion from an osteoid osteoma?
Explanation
Question 12
A 16-year-old girl undergoes intralesional curettage of an expansile 3.5 cm lytic lesion located in the posterior elements of C4. A photomicrograph of the specimen is shown.
What is the most likely diagnosis?
Explanation
Question 13
A 2-week-old neonate presents with asymmetric hip creases, fever, and pseudoparalysis of the right lower extremity. Ultrasound confirms a large hip effusion, and emergent surgical drainage is performed. The clinical image below demonstrates severe sequelae of a missed diagnosis in a similar patient.
What is the most devastating long-term complication of delayed diagnosis of neonatal septic arthritis of the hip?
Explanation
Question 14
A 14-month-old child presents with refusal to bear weight and a knee effusion. Fluid analysis shows a WBC count of 65,000 cells/microL with a negative Gram stain. The suspected organism is a fastidious Gram-negative rod that is part of the normal pediatric respiratory flora. Which method is most critical for isolating the likely causative organism?
Explanation
Question 15
A 4-year-old boy presents with rhizomelic short stature, frontal bossing, and a depressed nasal bridge. The genetic mutation underlying his condition primarily disrupts normal bone growth through which of the following cellular mechanisms?
Explanation
Question 16
An 11-year-old boy presents with severe, deep thigh pain and fever. Radiographs show a permeative diaphyseal lesion with an "onion-skin" periosteal reaction. A core biopsy demonstrates uniform small round blue cells. Which specific genetic translocation is most diagnostic of this malignancy?
Explanation
Question 17
A 5-year-old girl with an established diagnosis of Spondyloepiphyseal Dysplasia congenita (SEDc) presents for a routine orthopedic evaluation. Because of her condition, she is at highest risk for which of the following potentially life-threatening complications?
Explanation
Question 18
A 6-year-old boy presents with short-trunk dwarfism, corneal clouding, and normal intelligence. Radiographs demonstrate severe platyspondyly and odontoid hypoplasia. Urine tests reveal elevated levels of keratan sulfate. This clinical picture is most consistent with a deficiency in which enzyme?
Explanation
Question 19
A 15-year-old boy presents with a rapidly expanding, destructive metaphyseal lesion of the distal femur. MRI reveals large fluid-fluid levels. Histology shows highly pleomorphic, atypical spindle cells producing fine, lace-like osteoid within the septa separating blood-filled spaces. What is the most likely diagnosis?
Explanation
Question 20
A 7-year-old girl from Massachusetts presents with a massive, painless effusion of her right knee. She is afebrile and inflammatory markers are minimally elevated. Joint aspiration yields 45,000 WBCs/microL. After sending synovial fluid for testing, what is the recommended initial management for this likely diagnosis?
Explanation
Question 21
A 9-year-old boy sustains a minimally displaced pathologic fracture through a central, entirely lytic lesion in the proximal humerus metaphysis. A "fallen leaf" sign is present. The lesion abuts the physis. What is the most appropriate management after the fracture has initially healed?
Explanation
Question 22
A 15-year-old boy presents with progressive back pain that awakens him at night and is not relieved by ibuprofen. Imaging shows a 3-cm expansile lytic lesion in the posterior elements of L3. Biopsy reveals the following histology.
What is the most likely diagnosis?
Explanation
Question 23
A 10-day-old neonate presents with fever, irritability, and decreased spontaneous movement of the right lower extremity. On examination, the infant cries with passive range of motion of the right hip. An ultrasound reveals a significant joint effusion. What is the most appropriate next step in management?
Explanation
Question 24
A newborn is noted to have severe short limb dwarfism, rigid bilateral clubfeet, abducted "hitchhiker" thumbs, and cystic swelling of the pinnae. Mutations in which of the following genes or proteins are responsible for this condition?
Explanation
Question 25
An 18-month-old child presents with a limp and low-grade fever. Hip aspiration yields purulent fluid with a normal Gram stain. Routine cultures are initially negative, but growth is eventually achieved using aerobic blood culture vials (BACTEC). What is the most likely causative organism?
Explanation
Question 26
A 6-month-old infant with achondroplasia presents with poor feeding, hypotonia, and episodes of central apnea. Which of the following is the most critical screening study to perform?
Explanation
Question 27
A 17-year-old male presents with chronic neck pain. Radiographs demonstrate an expansile lesion in the posterior elements of C4.
Histologically, the lesion consists of woven bone trabeculae lined by prominent osteoblasts. Which of the following strongly differentiates this lesion from an osteoid osteoma?
Explanation
Question 28
A 9-year-old boy presents with severe thigh pain, high fever, and a swollen, erythematous leg. MRI confirms osteomyelitis of the femur and an adjacent deep venous thrombosis (DVT). Blood cultures grow gram-positive cocci. Which of the following virulence factors is most strongly associated with this severe clinical presentation?
Explanation
Question 29
A 4-year-old child with disproportionate short-trunk dwarfism is evaluated. Radiographs show delayed ossification of the femoral heads, severe coxa vara, and platyspondyly. Ocular examination reveals high myopia. A mutation in which of the following genes is the most likely cause?
Explanation
Question 30
A 6-year-old boy presents with localized back pain. Radiographs show a completely flattened C5 vertebral body (vertebra plana) with intact adjacent disc spaces. Biopsy of the lesion would most likely show cells positive for which of the following markers?
Explanation
Question 31
A 12-year-old boy has a permeative lytic lesion in the femoral diaphysis with an associated "onion-skin" periosteal reaction. Biopsy reveals sheets of uniform small round blue cells. Which of the following chromosomal translocations is most characteristic of this tumor?
Explanation
Question 32
A 3-year-old child presents with a waddling gait and joint hyperlaxity. The child appeared normal at birth but developed disproportionate short-limb dwarfism over the last year. Facial features and intelligence are normal. Radiographs show small, irregular epiphyses and metaphyseal flaring. A mutation in which gene is responsible?
Explanation
Question 33
An 11-year-old girl presents with recurrent episodes of clavicular and tibial pain with mild swelling. Radiographs show lytic and sclerotic changes in the medial clavicle and proximal tibia. Multiple biopsies show chronic inflammation but all bacterial, fungal, and mycobacterial cultures remain sterile. What is the most appropriate initial treatment?
Explanation
Question 34
A 14-year-old boy presents with progressive knee pain. Radiographs reveal a well-circumscribed, eccentrically located lytic lesion with a sclerotic margin, entirely contained within the proximal tibial epiphysis. Histology shows mononuclear cells, osteoclast-like giant cells, and areas of "chicken-wire" calcification. What is the diagnosis?
Explanation
Question 35
A 9-year-old girl from Connecticut presents with a massive, painless effusion of her right knee. She is afebrile and bears weight with a mild limp. Joint fluid aspiration yields 25,000 WBCs/mm3. Serology is positive for Borrelia burgdorferi. What is the most appropriate initial management?
Explanation
Question 36
An 8-year-old boy sustains a minor twisting injury to his arm and complains of shoulder pain. Radiographs show a centrally located, completely radiolucent lesion in the proximal humeral metaphysis extending to the physis. A small fragment of bone is seen resting at the dependent portion of the cyst. What is the most likely diagnosis?
Explanation
Question 37
A 10-year-old boy presents with bilateral knee and hip pain, and a waddling gait. Radiographs show delayed, irregular, and fragmented ossification centers of the capital femoral epiphyses. Lateral knee radiographs demonstrate a "double-layer" patella. Spinal radiographs are entirely normal. What is the most likely diagnosis?
Explanation
Question 38
A 7-year-old girl with homozygous sickle cell disease (HbSS) presents with severe bone pain, high fever, and swelling over the midshaft of her radius. MRI confirms diaphyseal osteomyelitis. While Staphylococcus aureus is highly prevalent, this patient is uniquely at high risk for infection from which of the following organisms?
Explanation
Question 39
A 15-year-old male presents with chronic back pain, which is worse at night and incompletely relieved by NSAIDs. Radiographs reveal an expansile, lytic lesion in the posterior elements of L3.
Based on the clinical presentation and typical radiographic findings shown, what is the most likely diagnosis?
Explanation
Question 40
A 2-week-old neonate presents with pseudoparalysis of the right leg. Ultrasound shows a large hip effusion, and aspiration yields frank pus.
What is the most appropriate surgical approach for emergency drainage of this joint?
Explanation
Question 41
A 5-year-old child with a known diagnosis of achondroplasia is being evaluated. What is the most common cause of early childhood mortality in patients with this condition?
Explanation
Question 42
A 14-year-old boy presents with distal femur pain. Radiographs demonstrate a mixed lytic and sclerotic lesion with a sunburst periosteal reaction. A core needle biopsy is performed. What histologic feature is mandatory for the diagnosis of osteosarcoma?
Explanation
Question 43
A 10-year-old girl is diagnosed with a diaphyseal femur tumor characterized by onion-skin periosteal reaction and CD99-positive small round blue cells. What is the most common cytogenetic translocation associated with this tumor?
Explanation
Question 44
An 18-month-old child presents with a limp, low-grade fever, and refusal to bear weight. Blood labs show CRP 25 mg/L and WBC 11,000/mm3. Standard synovial fluid culture is negative at 48 hours. To isolate the most likely causative organism in this age group, which laboratory technique should have been utilized?
Explanation
Question 45
A 6-year-old child presents with short-trunk dwarfism, corneal clouding, normal intelligence, and marked atlantoaxial instability secondary to odontoid hypoplasia. Which enzyme deficiency is responsible for this condition?
Explanation
Question 46
A newborn presents with short-limbed dwarfism, rigid equinovarus foot deformities, "hitchhiker" thumbs, and cystic swelling of the pinnae (cauliflower ears). What is the underlying genetic mutation for this condition?
Explanation
Question 47
A 19-year-old male with chronic neck pain undergoes biopsy of an expansile lesion in the C4 lamina. Histology is shown below.
Based on the photomicrograph and clinical presentation, what is the most appropriate definitive management?
Explanation
Question 48
A 10-year-old girl is evaluated for a broad skull, delayed fontanelle closure, and the unusual ability to touch her shoulders together anteriorly. Which gene mutation is responsible for her condition?
Explanation
Question 49
A 9-year-old girl presents with multiple recurrent episodes of bone pain and swelling in her clavicle and distal tibia. Labs show a mildly elevated ESR but normal WBC count. Multiple biopsies reveal sterile, non-infectious inflammation. What is the first-line treatment for this condition?
Explanation
Question 50
A 7-year-old boy presents with a lytic skull lesion and back pain due to a collapsed vertebral body (vertebra plana). Biopsy reveals an abundance of distinct histiocytes with grooved nuclei. Which immunohistochemical markers are classically positive in the lesional cells?
Explanation
Question 51
A 6-year-old boy from Connecticut presents with an acute, massive right knee effusion and an intermittent limp. He is afebrile, and the joint aspirate yields 45,000 WBCs/mm3. What diagnostic test sequence is recommended to confirm the suspected diagnosis?
Explanation
Question 52
An 8-year-old boy presents with mild shoulder pain after throwing a baseball. X-rays reveal a centrally located, lytic, slightly expansile lesion in the proximal humerus metaphysis with a visible "fallen leaf" sign. Which of the following is true regarding the management of this lesion?
Explanation
Question 53
A 17-year-old male presents with persistent, dull aching pain in his mid-back that is not reliably relieved by NSAIDs. Imaging shows a 3.5 cm expansile radiolucent lesion in the posterior elements of T10. Biopsy is performed and reveals the following histology:
What is the most likely diagnosis?

Explanation
Question 54
A 15-year-old girl presents with progressive back pain. Radiographs of her spine demonstrate an expansile, predominantly lytic lesion as shown in image A.
If this lesion is confirmed as an osteoblastoma, what is the most common spinal compartment initially involved?

Explanation
Question 55
A 3-week-old neonate presents with a swollen, erythematous right thigh and pseudoparalysis. An ultrasound confirms a hip effusion, and radiographs show early destructive changes in the proximal femur.
What anatomic factor strongly predisposes neonates to concurrent osteomyelitis and septic arthritis of the hip?
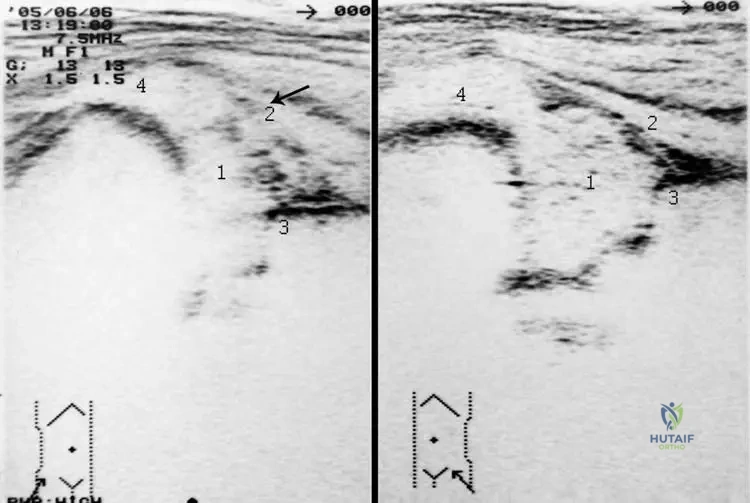
Explanation
Question 56
A 4-year-old boy with achondroplasia presents for a routine orthopedic evaluation. His parents are concerned about his bowing legs and his occasional snoring. Which of the following is the most critical screening evaluation recommended to prevent sudden mortality in this patient population?
Explanation
Question 57
A 9-year-old boy presents with a pathologic fracture of the proximal humerus following a minor fall. Radiographs show a centrally located, completely lytic lesion in the metaphysis that does not breach the cortex, with a small bony fragment settled at the bottom of the cyst. What is the most appropriate initial management after fracture healing?
Explanation
Question 58
A 6-year-old girl with blue sclerae and a history of multiple low-impact fractures is diagnosed with Osteogenesis Imperfecta (OI). Which underlying genetic defect is most commonly responsible for her condition?
Explanation
Question 59
A 7-year-old boy from Connecticut presents with acute right knee swelling and a limp. He is afebrile with a WBC of 9,000/mm³ and an ESR of 30 mm/hr. Joint aspiration yields 45,000 WBCs/mm³ with a predominance of PMNs. What is the most appropriate next step in diagnosis?
Explanation
Question 60
A 12-year-old boy presents with pain and swelling in his mid-thigh. Radiographs show a permeative diaphyseal lesion with an "onion skin" periosteal reaction. Genetic testing reveals a t(11;22) chromosomal translocation. What fusion protein is associated with this specific translocation?
Explanation
Question 61
A 10-year-old girl is evaluated for short stature and delayed primary tooth eruption. On examination, she is able to bring her shoulders together anteriorly. Radiographs reveal absent clavicles and delayed skull ossification. Which transcription factor is mutated in this condition?
Explanation
Question 62
A 5-year-old African American child with homozygous sickle cell disease presents with high fever and severe left arm pain. Radiographs show periosteal elevation of the radial diaphysis. While Staphylococcus aureus remains common, which of the following organisms is disproportionately frequent in this specific patient population?
Explanation
Question 63
An 11-year-old boy presents with night-time right thigh pain that dramatically improves within 30 minutes of taking ibuprofen. Radiographs demonstrate a dense sclerotic lesion in the proximal femur with a 1-cm central radiolucent nidus. What is the most common definitive treatment currently utilized for this condition?
Explanation
Question 64
A 14-year-old boy with a family history of Multiple Hereditary Exostoses (MHE) is evaluated for a rapidly growing bump on his distal femur. What is the approximate lifetime risk of malignant transformation of an osteochondroma in patients with MHE?
Explanation
Question 65
A 9-year-old girl presents with recurrent episodes of bone pain and swelling involving the clavicles and distal tibias. Blood cultures are repeatedly negative, and a bone biopsy reveals sterile, non-specific chronic inflammation. She also has palmoplantar pustulosis. What is the first-line treatment for this condition?
Explanation
Question 66
A 13-year-old girl presents with knee pain. MRI reveals a multiloculated, expansile metaphyseal lesion in the proximal tibia with prominent fluid-fluid levels. Biopsy confirms an Aneurysmal Bone Cyst (ABC). What primary genetic alteration is frequently associated with primary ABCs?
Explanation
Question 67
A 17-year-old male presents with dull, aching back pain that is not relieved by NSAIDs. Radiographs show a 3 cm expansile lesion in the posterior elements of L3. Biopsy reveals the following histology.
What is the most likely diagnosis?

Explanation
Question 68
A 15-year-old girl presents with a painful scoliosis. Radiographs of the spine are obtained as shown.
If this lesion causes a scoliotic deformity, which of the following best describes the typical curve pattern?

Explanation
Question 69
A 3-week-old neonate presents with fever, irritability, and decreased movement of the left lower extremity. Imaging demonstrates a hip effusion.
What is the most appropriate empiric intravenous antibiotic regimen after obtaining aspirates?

Explanation
Question 70
An 8-year-old boy presents with a permeative lytic lesion in the diaphysis of the femur with a prominent periosteal reaction. Biopsy reveals sheets of uniform small round blue cells that are CD99 positive. Which specific chromosomal translocation is most characteristic of this tumor?
Explanation
Question 71
A 14-year-old boy with distal femoral osteosarcoma completes neoadjuvant chemotherapy and undergoes limb-salvage surgery. Which of the following is the most important independent prognostic factor for his long-term survival?
Explanation
Question 72
A 6-year-old girl presents with a limp, precocious puberty, and large, irregular cafe-au-lait spots on her torso. Radiographs show ground-glass appearing expansile lesions in her proximal femur resulting in a "shepherd's crook" deformity. What is the underlying genetic mutation?
Explanation
Question 73
A 9-year-old girl has had intermittent clavicle and distal tibial pain for 6 months. Inflammatory markers are mildly elevated. Multiple bone biopsies yield no bacterial growth and show chronic non-suppurative inflammation. What is the most appropriate first-line treatment?
Explanation
Question 74
A 4-year-old boy with achondroplasia presents with progressive weakness in his upper and lower extremities and sleep apnea. What is the most likely anatomic cause of these new neurologic findings?
Explanation
Question 75
A 6-year-old boy with short-trunk dwarfism, corneal clouding, and normal intelligence is diagnosed with Morquio syndrome (MPS IV). He is at highest risk for developing which of the following orthopedic conditions?
Explanation
Question 76
A 10-year-old boy is brought in for an abnormal shoulder appearance. He has excessive shoulder mobility and can touch his shoulders together anteriorly. Radiographs show complete absence of the clavicles. Which gene is primarily mutated in this condition?
Explanation
Question 77
A 7-year-old boy from Connecticut presents with a massive, painless right knee effusion. He is afebrile, weight-bearing, and has a WBC of 8,000 cells/mcL and an ESR of 25 mm/h. Joint aspiration reveals a WBC count of 45,000/mcL. Gram stain is negative. What is the most appropriate next step in diagnosis?
Explanation
Question 78
A 16-year-old male presents with chronic, dull back pain that is not completely relieved by NSAIDs. Radiographs show a 3 cm expansile lesion in the posterior elements of the lumbar spine. A biopsy is obtained, revealing loose fibrovascular connective tissue intermixed with irregular woven bone trabeculae and active osteoblasts, with no nuclear atypia.
Which of the following statements is true regarding this lesion?


Explanation
Question 79
A 3-week-old premature neonate presents with asymmetric hip creases, irritability, and decreased spontaneous movement of the right lower extremity. Ultrasound reveals a large right hip effusion.
Following diagnostic aspiration that yields purulent fluid, which of the following empiric antibiotic regimens is most appropriate for this patient?

Explanation
Question 80
A 4-year-old child presents with rhizomelic short stature, a prominent forehead, midface hypoplasia, and a diagnosis of achondroplasia. Genetic testing confirms a mutation in the FGFR3 gene. Which of the following spinal manifestations is most likely to become symptomatic and require surgical intervention in adulthood?
Explanation
Question 81
A 12-year-old boy presents with severe, progressive knee pain. Radiographs reveal a mixed lytic and sclerotic lesion in the distal femoral metaphysis with a "sunburst" periosteal reaction and Codman's triangle. Core needle biopsy confirms high-grade, conventional osteosarcoma. Which of the following factors is most predictive of this patient's long-term survival?
Explanation
Question 82
A 6-year-old girl with blue sclerae, dentinogenesis imperfecta, and a history of multiple low-energy long bone fractures is diagnosed with Osteogenesis Imperfecta (OI). She is started on an intravenous bisphosphonate protocol. What is the primary cellular mechanism of action of this medication in the treatment of her condition?
Explanation
Question 83
An 8-year-old boy presents to the emergency department after a minor fall onto his arm. Radiographs demonstrate a pathologic fracture through a centrally located, purely radiolucent lesion in the proximal humeral metaphysis. A radiopaque fragment is noted resting at the dependent portion of the cyst (the "fallen leaf" sign). What is the most appropriate initial management for this presentation?
Explanation
Question 84
A 10-year-old girl presents with a 6-month history of intermittent, multifocal bone pain involving the medial clavicle and bilateral proximal tibias. Laboratory studies show a mildly elevated ESR, but multiple bone biopsies show sterile, non-suppurative inflammation. Radiographs reveal mixed lytic and sclerotic metaphyseal lesions. Which of the following is the most appropriate first-line treatment for this condition?
Explanation
Question 85
A 9-year-old boy is evaluated for unusual shoulder mobility. On examination, he is able to approximate his shoulders in the midline anteriorly. Physical exam also reveals a broad skull, delayed fontanelle closure, and multiple retained deciduous teeth. A mutation in which of the following genes is responsible for this patient's condition?
Explanation
Question 86
A 17-year-old male complains of chronic, dull back pain that is worse at night but has an inconsistent response to NSAIDs. A biopsy is obtained, and the histology demonstrates loose fibrovascular connective tissue intermixed with irregular osteoid and plump osteoblasts.
Which of the following clinical or radiographic features distinguishes this lesion from an osteoid osteoma?

Explanation
Question 87
A 14-year-old male presents with painful scoliosis and back spasms. Radiographs demonstrate an expansile lytic lesion in the posterior elements of L3.
If this lesion is responsible for the patient's scoliosis, what is the expected curve pattern?

Explanation
Question 88
A 4-week-old female is treated for culture-proven septic arthritis of the right hip.
Which unique anatomical factor makes the neonatal hip highly susceptible to permanent avascular necrosis and physeal destruction from this condition?

Explanation
Question 89
A 2-year-old boy with achondroplasia presents for a routine orthopedic evaluation. His parents are concerned about his prominent forehead and bowing legs. What is the most common spinal abnormality requiring surgical intervention in adulthood for patients with this condition?
Explanation
Question 90
An 8-year-old boy presents with an aggressive, permeative diaphyseal lesion in his femur with a classic 'onion-skin' periosteal reaction. A core needle biopsy is performed to confirm the diagnosis. Which immunohistochemical marker is most consistently positive in this specific tumor?
Explanation
Question 91
A 10-year-old girl complains of intermittent proximal tibial pain for 3 months. Laboratory tests show a normal WBC count and a slightly elevated ESR. Radiographs reveal a well-circumscribed lucency in the proximal tibial metaphysis surrounded by a thick sclerotic margin. What is the most likely diagnosis?
Explanation
Question 92
A 5-year-old child presents with a history of recurrent low-energy fractures, blue sclerae, and early-onset hearing loss. Genetic testing confirms Osteogenesis Imperfecta Type I. What is the underlying molecular defect?
Explanation
Question 93
A 12-year-old boy presents with multiple painless, bony bumps over his knees and shoulders. Radiographs show sessile bony projections that are continuous with the medullary cavity of the host bone. Mutations in which of the following genes are responsible for this condition?
Explanation
Question 94
A 6-year-old boy presents with disproportionate short trunk dwarfism, normal intelligence, a barrel chest, and severe coxa vara. Radiographs show significant delay in epiphyseal ossification and platyspondyly. What is the molecular basis of this child's skeletal dysplasia?
Explanation
Question 95
A 7-year-old boy presents with high fever, chills, and an inability to bear weight on his left leg. Examination reveals severe focal tenderness over the distal femur. Which region of the bone is the initial nidus for bacterial seeding in acute hematogenous osteomyelitis in this age group?
Explanation
Question 96
A 9-year-old boy sustains a pathological fracture through a central, lytic lesion in the proximal humerus after throwing a baseball. Radiographs demonstrate the 'fallen leaf' sign. What is the recommended initial management if the cyst remains active and expansile after the fracture heals?
Explanation
Question 97
A 6-year-old girl from Connecticut presents with a massive, painless effusion of the right knee. She had an uncharacterized rash several months prior. Joint aspiration yields 40,000 WBCs with predominantly mononuclear cells. What is the recommended initial serological test to confirm the suspected diagnosis?
Explanation
Question 98
A 4-year-old boy with Morquio syndrome (Mucopolysaccharidosis Type IV) presents for orthopedic evaluation. Before clearing this patient for general anesthesia for a hernia repair, which critical cervical spine abnormality must be urgently ruled out?
Explanation
Question 99
A 14-year-old girl gets an ankle radiograph after a mild sprain. An incidental eccentric, lucent, cortically-based lesion with a scalloped sclerotic border is found in the distal tibial metaphysis. She has no pain at the site. What is the most appropriate management?
Explanation
Question 100
A 4-year-old child presents with a waddling gait, short stature, and significant joint laxity. Unlike classic achondroplasia, the child has normal facial features and head circumference. Radiographs show delayed epiphyseal ossification and irregular, fragmented epiphyses. A mutation in which gene is responsible for this condition?
Explanation
None
