ABOS Orthopedic Board Review: Bone Dysplasias, HO, GCRG, Gorham's Disease | Part 23
Key Takeaway
Orthopedic Board Review Part 23 covers key topics including metaphyseal dysplasia (Schmid, McKusick), heterotopic ossification (prophylaxis, excision, risk factors), giant cell reparative granuloma (jaw lesions, pathology, treatment), and Gorham's disease (vanishing bone, vascular pathology). This section provides essential knowledge for ABOS exam preparation.
ABOS Orthopedic Board Review: Bone Dysplasias, HO, GCRG, Gorham's Disease | Part 23
Comprehensive 100-Question Exam
00:00
Start Quiz
Question 1
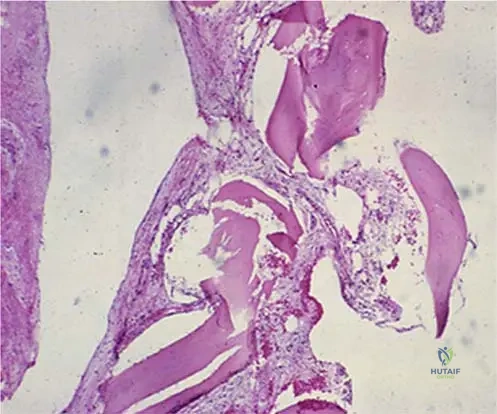
A 14-year-old boy presents with progressive shoulder pain and weakness. Radiographs show complete osteolysis of the clavicle and acromion without reactive bone formation.
Biopsy is likely to show which of the following histopathologic features?
Explanation
Question 2
A 65-year-old male with a history of severe Brooker class IV heterotopic ossification following a right total hip arthroplasty (THA) is scheduled for a left THA. Which of the following is the most effective prophylactic regimen for this high-risk patient?
Explanation
Question 3
A 15-year-old female presents with a radiolucent, expansile lesion in the proximal phalanx of her index finger. Biopsy shows spindle cells in a fibrous stroma with focal hemorrhage, clustered multinucleated giant cells, and reactive bone formation. Laboratory tests (serum calcium, PTH) are completely normal. What is the most likely diagnosis?
Explanation
Question 4
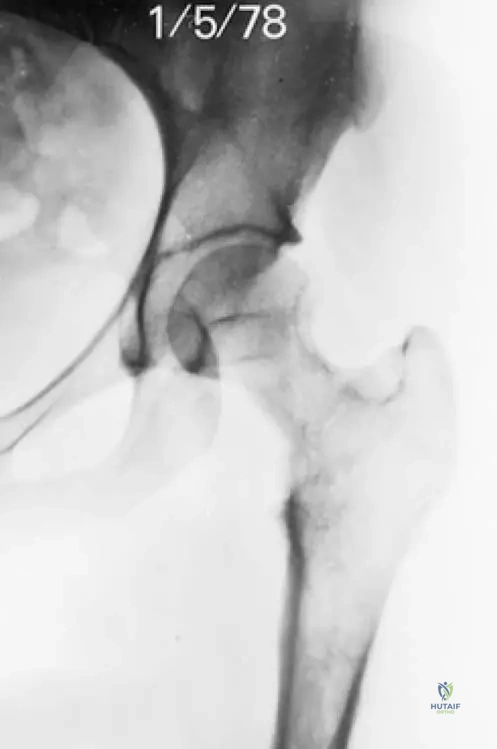
A 22-year-old asymptomatic male undergoes knee radiographs following mild trauma, revealing an 'Erlenmeyer flask' deformity of the distal femurs and proximal tibias without marked cortical thickening.
What is the most likely genetic defect associated with this condition?
Explanation
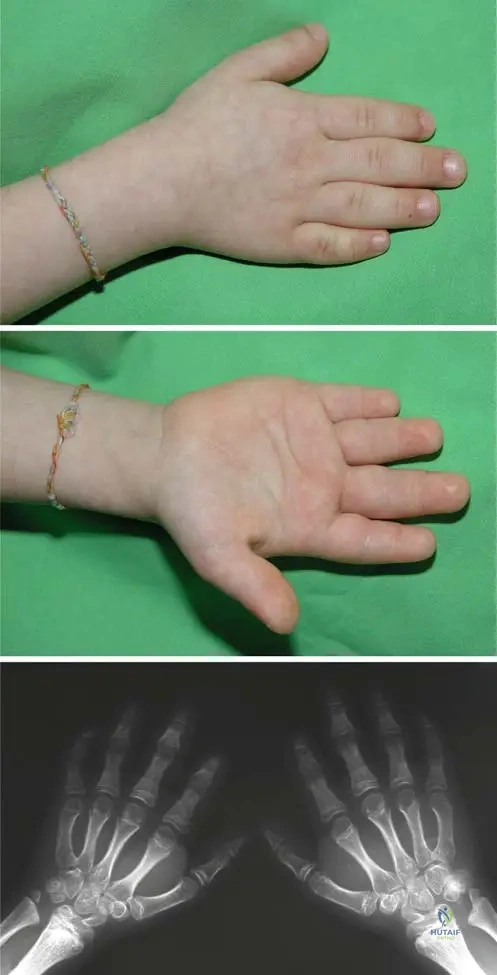
Question 5
A 28-year-old male is diagnosed with Gorham-Stout disease involving the thoracic spine and ribs.
He develops sudden onset dyspnea. What is the most common life-threatening complication associated with his condition?
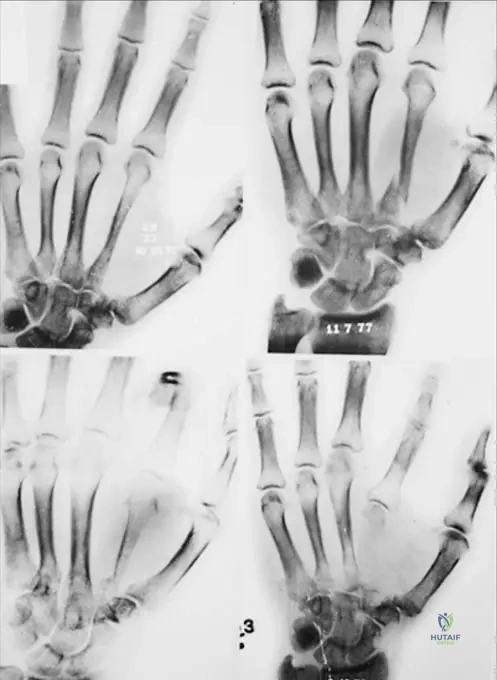
Explanation
Question 6
A 4-year-old child presents with painful soft tissue swellings on her back and a congenital malformation of her great toes. Which of the following gene mutations is most likely responsible for her condition?
Explanation
Question 7
A 35-year-old male sustained a severe traumatic brain injury 8 months ago and developed massive heterotopic ossification around his right hip. Which of the following is considered the most reliable radiographic indicator of heterotopic ossification maturity prior to surgical excision?
Explanation
Question 8
A 5-year-old boy presents with short trunk dwarfism, a barrel chest, a waddling gait, and high myopia. Radiographs show delayed ossification of the femoral heads and flattening of the vertebral bodies. A mutation in which collagen type is associated with this condition?
Explanation
Question 9
A 12-year-old girl is noted to have excessive mobility of her shoulders, allowing her to touch them together anteriorly. Radiographs show hypoplastic clavicles and delayed closure of the cranial sutures. What transcription factor is mutated in this disorder?
Explanation
Question 10
A 10-year-old child presents with bilateral knee and hip pain after activity. Radiographs reveal delayed, fragmented, and irregular ossification centers of the femoral heads and knees, but the spine is radiographically normal. A defect in which of the following proteins is most commonly implicated?
Explanation
Question 11
A 45-year-old female presents with progressive osteolysis of her left hemipelvis and proximal femur, diagnosed as Gorham-Stout disease.
Alongside surgical stabilization, which pharmacological agent has shown the most efficacy in slowing the osteolytic process?

Explanation
Question 12
A newborn is noted to have short limbs, rigid clubfeet, 'hitchhiker' thumbs, and cystic swelling of the external ears. Radiographs reveal short, thick tubular bones. What is the underlying pathogenesis of this condition?
Explanation
Question 13
A 25-year-old male presents with progressive shoulder weakness and a dull ache. Radiographs show extensive resorption of the humeral head and glenoid without a sclerotic margin or periosteal reaction.
Biopsy reveals thin-walled, endothelium-lined vascular channels replacing bone. What is the most likely diagnosis?

Explanation
Question 14
A 45-year-old male sustained a severe traumatic brain injury and an associated acetabular fracture. To prevent heterotopic ossification (HO) following open reduction internal fixation, which of the following regimens is most appropriate while minimizing fracture nonunion risk?
Explanation
Question 15
A 15-year-old presents for evaluation of genu valgum. Radiographs demonstrate marked symmetric widening of the distal femoral and proximal tibial metaphyses with cortical thinning, giving an "Erlenmeyer flask" deformity.
The patient is otherwise asymptomatic with normal intelligence. Which genetic mutation is most commonly associated with this condition?

Explanation
Question 16
A 22-year-old female presents with a slowly enlarging, painless swelling over her mandible. Radiographs show a multilocular radiolucent lesion. Histology reveals fibrous stroma with focal hemorrhage, hemosiderin, and clustered multinucleated giant cells around hemorrhagic areas. What is the most likely diagnosis?
Explanation
Question 17
A 30-year-old male with a complete T6 spinal cord injury from an accident 3 months ago develops sudden swelling, warmth, and restricted range of motion in his right hip. Deep vein thrombosis is ruled out. Serum alkaline phosphatase is significantly elevated. What is the most sensitive early imaging modality to confirm the suspected diagnosis?
Explanation
Question 18
A 14-year-old boy with known Gorham's disease of the thoracic spine and ribs develops sudden-onset respiratory distress.
Chest radiograph reveals a large pleural effusion. What is the most likely nature of this effusion and its pathogenesis?

Explanation
Question 19
A newborn presents with micromelic dwarfism, cleft palate, "hitchhiker" thumbs, and bilateral clubfeet. Radiographs reveal flattened, irregular cervical vertebrae. Which gene mutation is responsible for this condition?
Explanation
Question 20
A 12-year-old boy presents with delayed tooth eruption, hypermobility of the shoulders allowing them to meet in the midline, and a wide, flat skull. Which transcription factor is mutated in this condition?
Explanation
Question 21
A 34-year-old presents with a painful swelling in the 3rd metacarpal. X-rays show a lytic, expansile lesion in the metaphysis. Blood tests reveal normal calcium, phosphorus, and PTH levels. Biopsy shows spindle cells with grouped multinucleated giant cells and zones of reactive bone formation. Which condition must be ruled out before confirming GCRG?
Explanation
Question 22
A 6-year-old child presents with waddling gait and joint pain. Radiographs show delayed, irregular ossification of the capital femoral epiphyses bilaterally, but normal spine radiographs. Which gene is most commonly mutated in the autosomal dominant form of this disorder?
Explanation
Question 23
Following a total hip arthroplasty, a patient's 6-month follow-up pelvic radiograph demonstrates heterotopic ossification with bone islands extending between the pelvis and proximal femur, leaving less than 1 cm of space between opposing bone surfaces. What is the Brooker classification for this HO?
Explanation
Question 24
A 32-year-old male with confirmed Gorham-Stout disease of the left femur is experiencing progressive, massive osteolysis despite conservative care.
Which of the following medical treatments has shown efficacy in slowing the osteolytic process in this disease?

Explanation
Question 25
A 4-year-old child presents with short stature, bowlegs, and a waddling gait. Radiographs reveal flared, irregular metaphyses but normal epiphyses and spine. Laboratory studies show normal calcium, phosphorus, and alkaline phosphatase. Which collagen gene is typically mutated?
Explanation
Question 26
A 2-year-old boy with achondroplasia presents for evaluation. His parents are concerned about his prominent forehead and spinal curvature. On exam, he has a thoracolumbar kyphosis. What is the expected natural history of this spinal deformity?
Explanation
Question 27
During evaluation of a lytic lesion in the distal phalanx of a 28-year-old patient, histological review shows fibroblasts, areas of hemorrhage, and multinucleated giant cells that are small and clustered irregularly. Which feature is most helpful to differentiate GCRG from true Giant Cell Tumor of Bone (GCTB)?
Explanation
Question 28
A 29-year-old patient sustained a severe elbow trauma and developed heterotopic ossification, resulting in functional ankylosis. Surgical excision is planned. To minimize recurrence, what is the best indicator that the HO is "mature" and ready for resection?
Explanation
Question 29
A 5-year-old male presents with short trunk dwarfism, a barrel chest, and coxa vara. He has normal intelligence and normal-sized hands and feet. Radiographs show flattened vertebral bodies and delayed ossification of the epiphyses. Which structure's underlying defect is responsible for this condition?
Explanation
Question 30
What is the primary histological feature driving the massive osteolysis seen in Gorham-Stout disease?
Explanation
Question 31
A 15-year-old male presents with progressive osteolysis of his clavicle and ribs consistent with Gorham's disease. What is the most common life-threatening complication associated with this specific anatomic involvement?

Explanation
Question 32
A 24-year-old patient presents with genu valgum. Radiographs reveal widening of the metaphyses of the long bones, yielding an 'Erlenmeyer flask' deformity, while the diaphyses are of normal thickness. Which of the following is true regarding this condition?

Explanation
Question 33
Which of the following histopathological features most reliably differentiates a Giant Cell Reparative Granuloma (GCRG) from a true Giant Cell Tumor (GCT) of bone?
Explanation
Question 34
Indomethacin is frequently used as prophylaxis against heterotopic ossification (HO) following acetabular fracture fixation. What is its primary mechanism of action in this context?
Explanation
Question 35
A patient is scheduled for surgical excision of heterotopic ossification around the elbow following a severe traumatic brain injury. To prevent recurrence, prophylactic radiation therapy is planned. What is the optimal timing for administering this radiation dose?
Explanation
Question 36
A 30-year-old male presents with chronic shoulder pain and weakness. Radiographs demonstrate complete resorption of the humeral head and glenoid without any signs of reactive bone formation or sclerosis.
What is the expected initial laboratory profile?

Explanation
Question 37
Achondroplasia is the most common form of short-limbed dwarfism. Which of the following best describes the genetic pathophysiology of this condition?
Explanation
Question 38
A 6-year-old boy presents with short stature, waddling gait, and joint pain. Radiographs reveal delayed, irregular ossification of the capital femoral epiphyses bilaterally. To differentiate between Multiple Epiphyseal Dysplasia (MED) and Spondyloepiphyseal Dysplasia (SED), which radiographic finding is most diagnostic of SED?
Explanation
Question 39
A 35-year-old male developed severe heterotopic ossification (HO) of the right hip following a traumatic brain injury and prolonged coma. According to classical orthopedic teaching, what is the most reliable indicator that the HO is mature enough for safe surgical excision?
Explanation
Question 40
A newborn is evaluated for severe limb shortening. Exam reveals a 'hitchhiker thumb', bilateral clubfeet, and cystic swelling of the external ears (cauliflower ears). What is the underlying biochemical defect in this condition?
Explanation
Question 41
A 16-year-old female presents with swelling in her right middle finger after a jamming injury 3 months ago. Radiographs show a lytic, expansile lesion in the diaphysis of the proximal phalanx without cortical breakthrough. Biopsy reveals spindle cells and giant cells grouped around hemorrhagic foci. Which of the following is true?
Explanation
Question 42
A 14-year-old male presents with unusually hypermobile shoulders, allowing him to touch them together anteriorly. He has a broad forehead and retained deciduous teeth. Which gene mutation is responsible for his condition?
Explanation
Question 43
A 24-year-old male presents with progressive shoulder pain and weakness over two years. Serial radiographs demonstrate progressive 'vanishing' of the proximal humerus without a distinct mass.
A biopsy is performed. What is the expected predominant histologic finding?

Explanation
Question 44
A 25-year-old female presents with a lytic, expansile lesion in the 2nd metacarpal. Biopsy demonstrates a spindle cell background with clustered, irregularly distributed multinucleated giant cells centered around areas of hemorrhage. Laboratory workup reveals normal serum calcium and parathyroid hormone levels. What is the most likely diagnosis?
Explanation
Question 45
A 55-year-old male undergoes a right total hip arthroplasty. He has a history of severe Brooker class IV heterotopic ossification (HO) following a previous left THA. Which of the following is the most appropriate pharmacologic prophylaxis to prevent HO in this patient?
Explanation
Question 46
A 12-year-old boy presents with genu valgum. Radiographs reveal the following deformity.
What is the primary pathophysiological defect underlying this classic Erlenmeyer flask appearance?

Explanation
Question 47
A 19-year-old patient is diagnosed with Gorham-Stout disease affecting the clavicle, scapula, and upper ribs. Which of the following is a potentially fatal complication uniquely associated with this disease location?
Explanation
Question 48
A 4-year-old child is evaluated for progressive stiffness and painful soft tissue swellings. Physical examination reveals bilateral hallux valgus and uniquely shortened great toes. Radiographs show early ectopic bone formation in the paraspinal muscles. What is the underlying genetic mutation?
Explanation
Question 49
Which of the following histological or molecular features best distinguishes a giant cell reparative granuloma (GCRG) of a metacarpal from a true giant cell tumor (GCT) of bone?
Explanation
Question 50
A 32-year-old male with a severe traumatic brain injury develops rigid ankylosis of his right elbow secondary to heterotopic ossification (HO). When planning surgical excision, which of the following is considered the most reliable indicator that the HO is mature enough for resection?
Explanation
Question 51
A 38-year-old female presents with intractable pelvic pain and progressive deformity. Radiographs demonstrate massive osteolysis of the left hemipelvis.
Which of the following statements is true regarding the natural history of this disease?

Explanation
Question 52
A 7-year-old girl is noted to have delayed closure of her fontanelles, prominent frontal bossing, and hypermobility of her shoulders, allowing them to be apposed in the midline. Which transcription factor is mutated in this condition?
Explanation
Question 53
A child with diastrophic dysplasia presents for routine orthopedic follow-up. He exhibits the classic features of short-limbed dwarfism, cauliflower ears, and hitchhiker thumbs. Which spinal deformity must be closely monitored due to its potential for rapid progression and neurologic compromise?
Explanation
Question 54
A 6-year-old child presents with a waddling gait and bilateral hip pain. Radiographs demonstrate delayed and irregular ossification of the capital femoral epiphyses bilaterally. To differentiate Multiple Epiphyseal Dysplasia (MED) from Spondyloepiphyseal Dysplasia (SED), which radiographic feature is most specific to MED?
Explanation
Question 55
A 5-year-old boy presents with short stature, coxa vara, and pronounced bowing of the lower extremities. Laboratory tests (calcium, phosphorus, alkaline phosphatase, and Vitamin D) are completely normal. Radiographs show widened, irregular metaphyses but normal epiphyses. What is the genetic mutation responsible for the Schmid type of this dysplasia?
Explanation
Question 56
A 15-year-old male presents with progressive shoulder pain and weakness. Radiographs demonstrate the 'vanishing bone' appearance seen here.
What is the primary histological feature of this disease process?

Explanation
Question 57
A 45-year-old man undergoes surgical excision of heterotopic ossification (HO) about the elbow. He is prescribed a single dose of 700 cGy radiation postoperatively. What is the mechanism by which this therapy prevents HO recurrence?
Explanation
Question 58
A 22-year-old female presents with a lytic lesion in the proximal phalanx of her ring finger. Biopsy reveals multinucleated giant cells arranged irregularly around areas of prominent hemorrhage, separated by a spindle-cell fibrous stroma. Which of the following is the most likely diagnosis?
Explanation
Question 59
Which of the following genes is mutated in Schmid type metaphyseal chondrodysplasia?
Explanation
Question 60
A 19-year-old patient with known Gorham-Stout disease of the thoracic spine and ribs develops sudden respiratory distress.
What is the most common life-threatening complication associated with this specific anatomical involvement?

Explanation
Question 61
Which of the following patient profiles is at the highest risk for developing heterotopic ossification following a total hip arthroplasty?
Explanation
Question 62
A 10-year-old asymptomatic child undergoes knee radiographs following minor trauma, revealing an 'Erlenmeyer flask' deformity of the distal femurs.
History reveals early dental caries and genu valgum. What is the most likely diagnosis?

Explanation
Question 63
When planning the surgical excision of heterotopic ossification (HO) following a traumatic brain injury, which of the following is the most reliable clinical and radiographic indicator that the HO is mature enough for resection?
Explanation
Question 64
A 35-year-old patient undergoes a biopsy of an expansile, lytic lesion in the third metacarpal. Pathology reports findings consistent with a Giant Cell Reparative Granuloma. What laboratory workup is mandatory to rule out a mimicking systemic condition?
Explanation
Question 65
A 6-month-old infant with a known FGFR3 mutation presents with failure to thrive, apnea, and hypotonia. What is the most common cause of mortality in this patient population during infancy?
Explanation
Question 66
Which of the following medical treatments has shown efficacy in managing the progressive osteolysis and lymphatic abnormalities seen in Gorham-Stout disease?
Explanation
Question 67
A 40-year-old man who sustained a severe traumatic brain injury 4 months ago develops progressively decreasing range of motion in his right elbow due to neurogenic heterotopic ossification (HO). When is the most appropriate timing to surgically resect the HO?
Explanation
Question 68
A 25-year-old male presents with progressive shoulder pain and weakness. Radiographs demonstrate progressive dissolution of the proximal humerus without reactive bone formation, as shown in the image.
What is the most common life-threatening complication if this disease process involves the ribs or thoracic spine?

Explanation
Question 69
A 45-year-old male with a history of ankylosing spondylitis undergoes a primary total hip arthroplasty. He is scheduled for prophylactic radiation therapy to prevent heterotopic ossification. What is the optimal dose and timing for this intervention?
Explanation
Question 70
A 4-year-old child presents with short stature, a waddling gait, and bowing of the lower extremities. Radiographs show flaring and irregularity of the metaphyses with normal epiphyses and spine. Genetic testing reveals a mutation in the COL10A1 gene. What is the most likely diagnosis?
Explanation
Question 71
A 22-year-old female presents with a lytic, expansile lesion in the first metatarsal. Biopsy shows a fibroblastic stroma with focal hemorrhage, hemosiderin deposition, and multinucleated giant cells clustered around the areas of hemorrhage. Serum calcium, phosphorus, and PTH are normal. Which of the following is true regarding this condition?
Explanation
Question 72
A 6-month-old infant is evaluated for rhizomelic short stature, frontal bossing, and midface hypoplasia. Radiographs reveal narrowing of the interpedicular distances in the lumbar spine. Which of the following represents the underlying cellular defect in this condition?
Explanation
Question 73
A 30-year-old female experiences spontaneous resorption of her mandible over several years. Biopsy of the affected area is most likely to demonstrate which of the following?
Explanation
Question 74
The radiograph of a 5-year-old child with short stature demonstrates metaphyseal flaring and lucencies, as shown in the image.
If this patient has McKusick type metaphyseal chondrodysplasia (cartilage-hair hypoplasia), which of the following systemic manifestations is most commonly associated?

Explanation
Question 75
Following a severe traumatic brain injury and subsequent open reduction internal fixation of an acetabular fracture, a 35-year-old male develops significant stiffness in the affected hip. Radiographs reveal bone bridging the pelvis and the proximal femur, resulting in apparent hip ankylosis. According to the Brooker classification, what grade is this heterotopic ossification?
Explanation
Question 76
A 16-year-old boy has an expansile, osteolytic lesion in the distal phalanx of his thumb. Biopsy confirms a giant cell reparative granuloma. What is the most appropriate initial surgical management?
Explanation
Question 77
A 7-year-old girl presents with short stature, a waddling gait, and joint laxity. Unlike achondroplasia, her facial features are completely normal. Radiographs reveal delayed, fragmented epiphyseal ossification centers and irregular metaphyses. Which of the following genes is most likely mutated in this patient?
Explanation
Question 78
A newborn is noted to have short-limbed dwarfism, bilateral clubfeet, "hitchhiker" thumbs, and cystic swelling of the external ears. Radiographs show a short, thick first metacarpal. What is the underlying genetic mutation for this condition?
Explanation
Question 79
Which of the following patient scenarios carries the highest risk for developing heterotopic ossification following a total hip arthroplasty if prophylactic measures are not utilized?
Explanation
Question 80
A 12-year-old girl presents with progressive left clavicular pain. Radiographs reveal massive osteolysis of the clavicle, as shown in the image.
Laboratory evaluation is completely normal, with no evidence of infection or malignancy. Which of the following best describes the pathophysiologic mechanism of this disease?

Explanation
Question 81
A 24-year-old male presents with progressive upper extremity weakness and a 'vanishing' appearance of his humerus on radiographs.
Which of the following is the hallmark histologic finding of this condition?

Explanation
Question 82
A 45-year-old male with a history of severe heterotopic ossification (HO) is scheduled to undergo a total hip arthroplasty. A single fraction of 700 cGy radiation is planned for prophylaxis. What is the primary mechanism by which radiation prevents HO?
Explanation
Question 83
A 5-year-old child presents with short stature and a waddling gait. Radiographs are shown below.
Genetic testing is most likely to reveal a mutation in which of the following genes?

Explanation
Question 84
A 16-year-old female presents with an expansile, radiolucent lesion in her first metacarpal. Biopsy reveals a spindle cell stroma, reactive bone formation, and multinucleated giant cells clustered primarily around areas of hemorrhage. Serum calcium, phosphorus, and parathyroid hormone levels are normal. Which of the following is the most likely diagnosis?
Explanation
Question 85
A 21-year-old male with confirmed Gorham-Stout disease involving the clavicle, scapula, and upper ribs is admitted to the intensive care unit. Which of the following is the most common life-threatening complication associated with this specific anatomic pattern of the disease?
Explanation
Question 86
A 30-year-old male sustained a severe traumatic brain injury and subsequently developed clinically significant heterotopic ossification (HO) ankylosing his right elbow. When evaluating the optimal timing for surgical excision of the HO, which of the following is the most reliable indicator that the bone is mature enough to minimize recurrence?
Explanation
Question 87
A 35-year-old female presents with severe groin pain and the progressive radiographic changes shown below.
In addition to bisphosphonates, which of the following medical therapies specifically targeting the mTOR pathway has proven effective in arresting this condition?

Explanation
Question 88
A 10-year-old boy presents with a prominent forehead, delayed eruption of adult teeth, and the ability to touch his shoulders together anteriorly. Radiographs confirm hypoplastic clavicles. This condition is caused by a mutation in a gene that is critical for the differentiation of which of the following cell types?
Explanation
Question 89
A 45-year-old male sustains an acetabular fracture requiring open reduction and internal fixation. The surgeon plans to prescribe indomethacin for heterotopic ossification prophylaxis. Which of the following is the most significant musculoskeletal risk associated with this therapy?
Explanation
Question 90
When distinguishing a Giant Cell Reparative Granuloma (GCRG) from a Giant Cell Tumor (GCT) of bone pathologically, which of the following histological features strongly favors a diagnosis of GCRG?
Explanation
Question 91
A 4-year-old girl is diagnosed with the most common form of short-limb dwarfism. Her parents are of average height. The underlying mutation results in an abnormality in which specific zone of the physis?
Explanation
Question 92
A 16-year-old male presents with progressive swelling and pain in his left forearm. Radiographs demonstrate near-complete osteolysis of the radius. Biopsy confirms Gorham-Stout disease. Which of the following serum laboratory profiles (Calcium, Phosphorus, Alkaline Phosphatase) is most characteristic of this condition?
Explanation
Question 93
A 60-year-old female presents with restricted hip range of motion 1 year after a right total hip arthroplasty. Radiographs reveal heterotopic ossification extending from the pelvis to the proximal femur, leaving a radiolucent gap of 0.5 cm between the opposing bone surfaces. According to the Brooker classification, what is the grade of her heterotopic ossification?
Explanation
None
