ABOS Board Review: Pediatric Orthopedics, Bone Tumors & Skeletal Dysplasias | Part 6
Key Takeaway
This ABOS board review covers essential pediatric orthopedic pathology, including septic arthritis, osteomyelitis in infants, benign bone tumor (osteoblastoma) characteristics, and a comprehensive overview of skeletal dysplasias. Learn about their clinical presentation, radiographic features, and management strategies for spinal and hip complications. Part 6 focuses on critical diagnostic and treatment principles.
ABOS Board Review: Pediatric Orthopedics, Bone Tumors & Skeletal Dysplasias | Part 6
Comprehensive 100-Question Exam
00:00
Start Quiz
Question 1
A 15-year-old boy presents with chronic, dull back pain that is not completely relieved by NSAIDs. Imaging reveals a 3 cm expansile, partially sclerotic lesion in the posterior elements of L3.
Based on the clinical and radiographic findings, which of the following is true regarding this pathology?
Explanation
Question 2
A 17-year-old girl undergoes biopsy of a solitary bone lesion. The photomicrograph is shown below.
The presence of loose fibrovascular connective tissue intermixed with irregular osteoid and normal-appearing mitotic figures most strongly supports which diagnosis?
Explanation
Question 3
A 2-week-old neonate presents with pseudoparalysis of the right lower extremity and crying upon diaper changes. Ultrasound confirms a significant hip effusion.
What is the most appropriate next step in management?
Explanation
Question 4
A 6-month-old infant with achondroplasia is noted to have brisk deep tendon reflexes and sleep apnea. What is the most common cause of mortality in this patient population during infancy?
Explanation
Question 5
Which of the following is the primary mechanism of action for the class of medications most commonly used to reduce fracture risk in pediatric patients with Osteogenesis Imperfecta?
Explanation
Question 6
A 16-year-old male presents with a 6-month history of chronic, dull back pain that is not completely relieved by NSAIDs. Radiographs reveal an expansile, lytic lesion in the posterior elements of L3.
What is the most likely diagnosis?
Explanation
Question 7
A biopsy is taken from a 3 cm expansile lesion in the posterior elements of the cervical spine. Histological analysis reveals loose fibrovascular connective tissue intermixed with irregular osteoid and plump osteoblasts.
Which of the following is a primary characteristic distinguishing this condition from osteoid osteoma?
Explanation
Question 8
A 5-month-old infant presents with frontal bossing, rhizomelic shortening of the limbs, and midface hypoplasia. Which of the following describes the genetic etiology of this condition?
Explanation
Question 9
A 12-year-old boy presents with a painful mass on his distal femur. Radiographs show a permeative, diaphyseal lesion with an 'onion-skin' periosteal reaction. Which chromosomal translocation is most classically associated with this tumor?
Explanation
Question 10
A 3-week-old neonate presents with fever, irritability, and a pseudoparalysis of the right lower extremity. Ultrasound reveals a hip joint effusion.
What is the most appropriate next step in management?
Explanation
Question 11
A 7-year-old girl is evaluated for recurrent long bone fractures after minimal trauma. She has blue sclerae and mild hearing loss. This condition is primarily caused by a defect in which of the following?
Explanation
Question 12
A 9-year-old boy sustains a minor fall and presents with arm pain. Radiographs reveal a centrally located, lytic metaphyseal lesion in the proximal humerus with a 'fallen leaf' sign. Aspiration yields clear, yellow fluid. What is the most likely diagnosis?
Explanation
Question 13
A newborn presents with severe bilateral clubfeet, 'hitchhiker' thumbs, and cystic swelling of the external ears (cauliflower ears). Which of the following genes is mutated in this condition?
Explanation
Question 14
Which of the following clinical features most accurately differentiates an osteoblastoma from an osteoid osteoma?
Explanation
Question 15
A 14-year-old male presents with knee pain. Radiographs show a well-circumscribed, eccentrically placed, lytic lesion in the distal femoral epiphysis with a thin sclerotic rim. Histological examination shows mononuclear cells and areas of 'chicken-wire' calcification. What is the diagnosis?
Explanation
Question 16
An 8-year-old boy presents with a waddling gait and bilateral knee and hip pain. Radiographs reveal delayed ossification and irregularity of multiple epiphyses. Spine radiographs are completely normal. Mutation in which gene is most likely responsible?
Explanation
Question 17
A 15-year-old girl presents with a rapidly growing mass on her distal femur. Biopsy reveals malignant spindle cells producing delicate, lace-like osteoid matrix. What is the most common subtype of this tumor?
Explanation
Question 18
A 6-year-old boy presents with a solitary, 'punched-out' lytic skull lesion. Biopsy reveals cells with grooved nuclei (coffee-bean appearance) and eosinophils. Immunohistochemistry will likely be positive for which of the following markers?
Explanation
Question 19
A child born with normal length and facial features develops severe short stature and a waddling gait by age 3. Radiographs demonstrate small, irregular epiphyses and platyspondyly with anterior tongue-like projections of the vertebral bodies. Which of the following is the most likely diagnosis?
Explanation
Question 20
A 12-year-old boy with Multiple Hereditary Exostoses (MHE) is monitored for malignant transformation. Which anatomical location of an osteochondroma carries the highest risk of malignant transformation into a secondary chondrosarcoma?
Explanation
Question 21
An incidental finding on a knee radiograph of a 14-year-old male shows an eccentrically located, multilobulated lucent lesion with a sclerotic rim in the distal femoral metaphysis. Histology from a similar lesion typically shows spindle cells in a storiform pattern with foamy histiocytes. What is the most appropriate management?
Explanation
Question 22
A newborn presents with delayed closure of the cranial sutures, wormian bones, and absent clavicles. What gene mutation is associated with this syndrome?
Explanation
Question 23
An 11-year-old boy presents with fever, focal distal femur pain, and elevated inflammatory markers. Radiographs show a permeative diaphyseal lesion. Biopsy shows sheets of small round blue cells. Immunohistochemistry is strongly positive for CD99. Which of the following is the most important component of the initial treatment algorithm for this condition?
Explanation
Question 24
A 4-year-old child presents with a severe limb length discrepancy. Radiographs show complete destruction and absence of the capital femoral epiphysis and femoral neck on the right side.
This is the classic sequela of which untreated infantile condition?
Explanation
Question 25
A 19-year-old undergoes curettage of a 3.5 cm expansile lesion in the posterior elements of T12. Grossly, the tissue is a hemorrhagic, gritty, purplish-red friable mass.
What is the recommended standard surgical treatment for this benign but locally aggressive lesion?
Explanation
Question 26
A 16-year-old male presents with persistent mid-back pain not completely relieved by NSAIDs and a new-onset painful structural scoliosis. Radiographs of the spine are evaluated.
What is the most appropriate definitive management for the most likely diagnosis?
Explanation
Question 27
A 19-year-old female undergoes biopsy of an expansile lytic lesion in the posterior elements of L3.
The histology demonstrates irregular osteoid trabeculae in a vascular connective tissue stroma with prominent osteoblasts. What is the most likely diagnosis?
Explanation
Question 28
A child with short stature, frontal bossing, and rhizomelic limb shortening is evaluated. Radiographs show narrowing of the interpedicular distances in the lumbar spine. Which of the following describes the underlying molecular defect?
Explanation
Question 29
A newborn presents with short-limbed dwarfism, bilateral rigid clubfeet, "hitchhiker" thumbs, and cystic swelling of the pinnae. What is the primary pathophysiologic defect in this condition?
Explanation
Question 30
A 14-year-old boy presents with right knee pain. Radiographs reveal a well-circumscribed, eccentrically located lytic lesion with a thin sclerotic rim within the proximal tibial epiphysis. Histology shows mononuclear cells with grooved nuclei and "chicken-wire" calcifications. Which immunohistochemical marker is characteristically positive in this tumor?
Explanation
Question 31
A 10-year-old girl presents with a permeative lytic lesion in the femoral diaphysis with an "onion-skin" periosteal reaction. A biopsy confirms Ewing sarcoma. Which of the following cytogenetic abnormalities is most commonly associated with this tumor?
Explanation
Question 32
A 3-year-old child presents with a painless waddling gait.
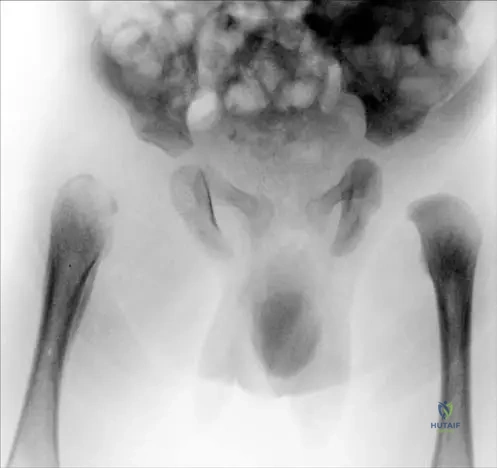
AP pelvis radiograph demonstrates a decreased femoral neck-shaft angle, a vertically oriented physis, and a distinct triangular bone fragment in the inferior femoral neck. What radiographic measurement is the primary determinant for surgical intervention in this condition?
Explanation
Question 33
A 15-year-old boy has a biopsy-proven high-grade intramedullary osteosarcoma of the distal femur without distant metastasis. What is the standard treatment protocol for this patient?
Explanation
Question 34
A 6-year-old child with normal intelligence, corneal clouding, and severe platyspondyly presents with progressive cervical myelopathy. Radiographs reveal severe odontoid hypoplasia and atlantoaxial instability. What is the accumulated metabolite in this syndrome?
Explanation
Question 35
A 7-year-old girl is evaluated for delayed dental eruption and abnormal shoulder mobility, allowing her to touch her shoulders together anteriorly. Radiographs show absent clavicles and delayed closure of cranial sutures. What is the mutated gene responsible for this condition?
Explanation
Question 36
A 4-year-old child with recurrent fractures, blue sclerae, and dentinogenesis imperfecta is treated with intravenous pamidronate. What is the primary mechanism of action of this medication in treating this condition?
Explanation
Question 37
A 16-year-old boy presents with a painful rigid scoliosis that is poorly relieved by NSAIDs. Radiographs and CT show a 3.5 cm expansile, radiolucent lesion in the posterior elements of L3. Histology reveals woven bone trabeculae rimmed by prominent osteoblasts without nuclear atypia. What is the most appropriate definitive management?
Explanation
Question 38
A biopsy from a symptomatic lytic bone lesion in the distal femur of a 14-year-old reveals the provided histology, showing loose fibrovascular connective tissue intermixed with irregular osteoid. Which of the following features most reliably differentiates this lesion clinically from an osteoid osteoma?
Explanation
Question 39
A 3-week-old neonate presents with pseudoparalysis of the right leg and crying with diaper changes. There is no fever, but CRP is significantly elevated. Ultrasound reveals a hip effusion. If this neonatal septic arthritis (coxitis) is diagnosed late and untreated, what is the most severe classical long-term orthopedic complication?
Explanation
Question 40
A 6-year-old boy is evaluated for short stature, a waddling gait, and a barrel chest. Radiographs demonstrate delayed ossification of the capital femoral epiphyses, coxa vara, and platyspondyly. Ophthalmic examination reveals high myopia. A mutation in which of the following genes is most likely responsible?
Explanation
Question 41
The image demonstrates the gross curettage specimen of a primary bone tumor excised from the posterior elements of a 17-year-old's cervical spine. The tumor typically presents with dull pain that is not completely relieved by NSAIDs. Which of the following best describes the classical radiographic finding of this condition?
Explanation
Question 42
A 4-year-old girl with frontal bossing, midface hypoplasia, and rhizomelic shortening of the upper and lower extremities is being evaluated in the clinic. Her parents are of normal stature. Which of the following describes the pathophysiologic mechanism of the genetic mutation in this patient?
Explanation
Question 43
A 17-year-old male presents with chronic dull, aching back pain that is not completely relieved by NSAIDs. Imaging shows a 2.5 cm expansile lytic lesion in the posterior elements of L3.
What is the most likely diagnosis?
Explanation
Question 44
A biopsy is taken from a painful expansile lesion in the C2 lamina. Histology demonstrates the following features.
Which histologic finding is most characteristic of this condition?
Explanation
Question 45
A 2-week-old neonate presents with asymmetric skin folds, pseudoparalysis of the right leg, and pain with passive hip motion.
Ultrasound confirms a large joint effusion consistent with septic arthritis. Which pathogen is most uniquely common in this specific age group compared to older children?
Explanation
Question 46
A 4-year-old child with rhizomelic short stature, frontal bossing, and trident hands is diagnosed with achondroplasia. Which of the following best describes the underlying genetic defect?
Explanation
Question 47
Which of the following radiographic findings is most characteristic of an aggressive osteoblastoma rather than conventional osteosarcoma?
Explanation
Question 48
An infant is placed in a Pavlik harness for developmental dysplasia of the hip. At the 2-week follow-up, the parents report the infant is no longer actively kicking the right leg. Physical examination reveals absent active knee extension on the affected side. What is the most likely cause?
Explanation
Question 49
A 5-year-old boy presents with disproportionate short stature, normal facies, and joint laxity. Radiographs demonstrate delayed epiphyseal ossification and platyspondyly with anterior tongue-like projections. What is the most likely diagnosis?
Explanation
Question 50
A 12-year-old obese boy presents with a left slipped capital femoral epiphysis (SCFE). Which of the following is an absolute indication for prophylactic in situ pinning of the contralateral, asymptomatic hip?
Explanation
Question 51
During the Ponseti method for treating idiopathic clubfoot, the very first step in casting manipulation addresses which component of the deformity?
Explanation
Question 52
A 10-year-old girl presents with a rapidly enlarging mass over her proximal humerus. Radiographs show an eccentric, expansile, purely lytic lesion. MRI demonstrates multiple fluid-fluid levels. What is the most appropriate definitive surgical management after biopsy confirms an active aneurysmal bone cyst (ABC)?
Explanation
Question 53
In Legg-Calvé-Perthes disease, the Herring Lateral Pillar classification is most reliably applied at what stage of the disease to predict the ultimate deformity?
Explanation
Question 54
A 6-year-old child is evaluated for a severe limp and limb length discrepancy. History is significant for a prolonged neonatal intensive care unit stay for sepsis. Radiographs demonstrate complete absence of the femoral head and neck, as seen in the provided late-stage example. What is this specific sequela of neonatal septic arthritis called?
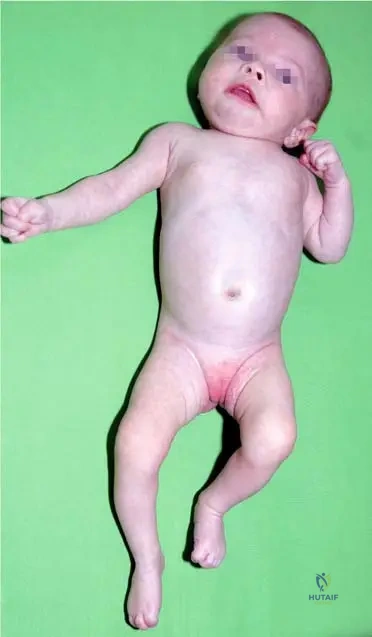
Explanation
Question 55
A 16-year-old male presents with dull, aching pain in his cervical spine. Radiographs and MRI demonstrate an expansile 3.5 cm lesion in the posterior elements of C4.
During curettage, the lesion appears hypervascular and granular. Which of the following best describes the distinguishing features of this lesion compared to an osteoid osteoma?

Explanation
Question 56
A 3-week-old infant presents with fever, irritability, and pseudoparalysis of the right leg. Ultrasound confirms a large hip effusion.
If surgical drainage is delayed, what is the most severe and irreversible complication according to the Choi classification?

Explanation
Question 57
A 4-year-old child with disproportionate short stature, frontal bossing, and rhizomelic shortening of the limbs is diagnosed with achondroplasia. Which of the following accurately describes the molecular pathogenesis of this condition?
Explanation
Question 58
A 7-year-old boy with blue sclerae, dentinogenesis imperfecta, and multiple prior fractures is started on intravenous pamidronate. What is the primary mechanism of action of this medication in the treatment of Osteogenesis Imperfecta?
Explanation
Question 59
A biopsy from a diaphyseal femur lesion in an 11-year-old boy reveals sheets of uniform, small, round, blue cells. Molecular testing is positive for a t(11;22)(q24;q12) translocation. Which of the following fusion proteins is most likely driving this malignancy?
Explanation
Question 60
A 12-year-old boy with Multiple Hereditary Exostoses (MHE) is evaluated for a rapidly growing, painful lesion on his proximal humerus. Mutations in EXT1 and EXT2 genes are implicated in MHE. These genes normally encode enzymes responsible for the synthesis of which molecule?
Explanation
Question 61
A patient presents with absent clavicles, delayed closure of cranial sutures, and supernumerary teeth. Which transcription factor is primarily mutated in this syndrome?
Explanation
Question 62
Which of the following clinical and genetic findings uniquely characterize Diastrophic Dysplasia compared to other short-limb dysplasias?
Explanation
Question 63
A 9-year-old girl sustains a pathologic fracture through a proximal humerus lesion. Radiographs demonstrate a centrally located, lytic metaphyseal lesion with a "fallen leaf" sign. Which of the following best describes the natural history of this lesion if left untreated?
Explanation
Question 64
Aneurysmal bone cysts (ABCs) can occur as primary lesions or secondary to other bone tumors. Primary ABCs have been shown to be true neoplasms driven by a specific genetic rearrangement. Which gene is typically upregulated due to translocation in primary ABCs?
Explanation
Question 65
A 10-year-old boy undergoes knee radiographs following minor trauma, revealing an incidental, eccentric, cortically based, multiloculated lucent lesion in the distal femoral metaphysis. He is completely asymptomatic. What is the most appropriate management?
Explanation
Question 66
A 5-year-old child presents with waddling gait and disproportionate short stature. Unlike patients with achondroplasia, this child has normal craniofacial features. Radiographs show delayed epiphyseal ossification and irregular, fragmented metaphyses. A mutation in which gene is most likely responsible?
Explanation
Question 67
A 6-year-old boy with Morquio Syndrome (Mucopolysaccharidosis Type IV) is scheduled for elective bilateral osteotomies for severe genu valgum. Preoperatively, which of the following evaluations is absolutely critical to prevent catastrophic neurologic injury during intubation?
Explanation
Question 68
A 14-year-old girl presents with precocious puberty, café-au-lait macules with irregular 'coast of Maine' borders, and multiple lytic bone lesions with a ground-glass appearance. Histologic examination of the bone lesions would most likely reveal:
Explanation
Question 69
A 15-year-old boy complains of chronic knee pain. Radiographs demonstrate a well-circumscribed, eccentrically located, lytic lesion exclusively within the proximal tibial epiphysis. Biopsy reveals mononuclear cells with longitudinal nuclear grooves and areas of "chicken-wire" calcification. What is the diagnosis?
Explanation
Question 70
Spondyloepiphyseal Dysplasia Congenita (SEDC) is a disproportionate short-trunk dwarfism. Patients frequently present with severe coxa vara. Which genetic mutation is primarily responsible for SEDC?
Explanation
Question 71
A 4-year-old boy presents with a painful, solitary lytic lesion of the skull. A biopsy demonstrates sheets of cells with indented nuclei intermixed with eosinophils. Immunohistochemistry is positive for CD1a and S-100. Electron microscopy of these cells would most likely show:
Explanation
Question 72
A 13-year-old girl is diagnosed with high-grade intramedullary osteosarcoma of the distal femur. Which of the following is considered the most significant adverse prognostic factor at the time of initial diagnosis?
Explanation
Question 73
During curettage of a suspected benign spinal lesion in a 20-year-old female, the surgeon notes the gross appearance shown in the provided atlas image.
The tissue is red, granular, and heavily bleeding. Histologic analysis is ordered. Which feature is crucial to differentiate this lesion (osteoblastoma) from a well-differentiated osteosarcoma?

Explanation
Question 74
A 2-year-old boy presents with anterolateral bowing of the left tibia. Radiographs reveal sclerosis and a narrowing of the medullary canal at the apex of the bow. Which of the following systemic conditions is most strongly associated with this finding?
Explanation
Question 75
A 16-year-old male presents with localized cervical spine pain. Radiographs reveal a 3.5 cm expansile, radiolucent lesion in the posterior elements of C4.
Which of the following characteristics most reliably differentiates this lesion from an osteoid osteoma?

Explanation
Question 76
A 2-year-old boy presents with disproportionate short stature, rhizomelic shortening, and frontal bossing. Radiographs show narrowing of the interpedicular distances in the lumbar spine. Which of the following gene mutations is the primary cause of this condition?
Explanation
Question 77
A 19-year-old female undergoes curettage for an expansile, painful lesion in the posterior elements of T12. The gross pathological specimen is shown.
Histological analysis shows rich vascularity and prominent osteoblasts surrounding irregular osteoid. What is the most common potential complication if this lesion is treated with standard intralesional curettage alone?

Explanation
Question 78
A 4-week-old infant was diagnosed with neonatal septic arthritis of the hip. Treatment was delayed for several days prior to surgical drainage. A follow-up radiograph one year later shows complete absence of the proximal femoral epiphysis and neck.
This severe structural loss is primarily the result of which of the following pathophysiologic mechanisms?
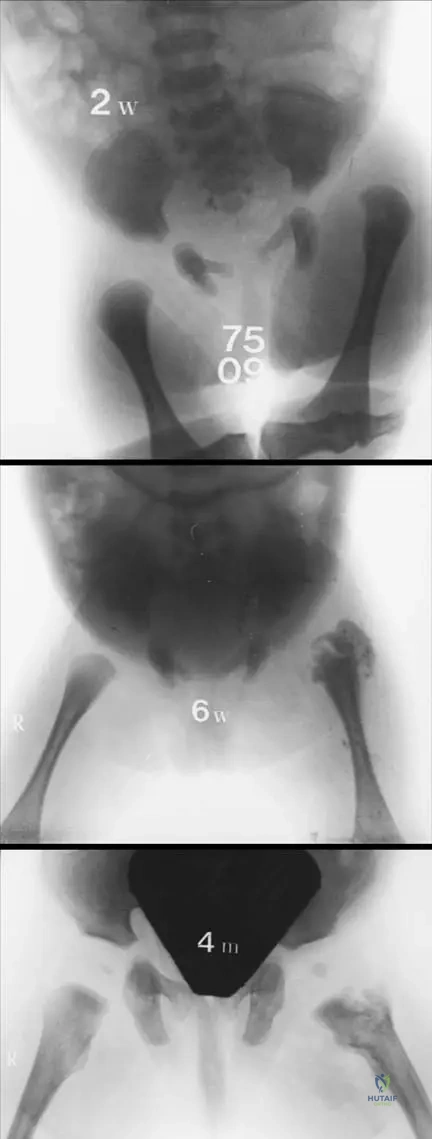
Explanation
Question 79
A 6-year-old child presents with a femoral shaft fracture after a minor mechanical fall. Physical examination reveals blue sclerae and mild hearing loss. Radiographs show generalized osteopenia and thin cortices. Which of the following represents the underlying molecular defect in this patient's condition?
Explanation
Question 80
A 22-year-old man presents with chronic, non-mechanical lower back pain. Imaging shows an expansile 3 cm lytic lesion of the L4 pedicle. A biopsy is performed, and the photomicrograph is shown below.
Which of the following features is most characteristic of this lesion's microscopic appearance?

Explanation
Question 81
A 12-year-old boy presents with multiple painless, bony prominences around his knees, ankles, and shoulders. Radiographs reveal multiple osteochondromas pointing away from the joint lines. He is diagnosed with Multiple Hereditary Exostoses (MHE). Which of the following genes is most likely mutated, and what is the estimated risk of malignant transformation in his lifetime?
Explanation
Question 82
A 16-year-old boy presents with painful scoliosis. Radiographs demonstrate an expansile lesion in the posterior elements of the lumbar spine.
What is the characteristic scoliotic curve pattern associated with this type of lesion?

Explanation
Question 83
An 18-year-old male undergoes curettage of a 3.5 cm posterior spinal lesion. The gross specimen demonstrates hemorrhagic, gritty red tissue.
Based on the gross appearance and size of the lesion, what is the most likely diagnosis?

Explanation
Question 84
A 3-week-old infant is brought to the emergency department for pseudoparalysis of the right leg. Ultrasound confirms a large hip effusion.
Diagnostic aspiration yields frankly purulent fluid. In addition to Staphylococcus aureus, which pathogen is uniquely highly prevalent in this specific age group?
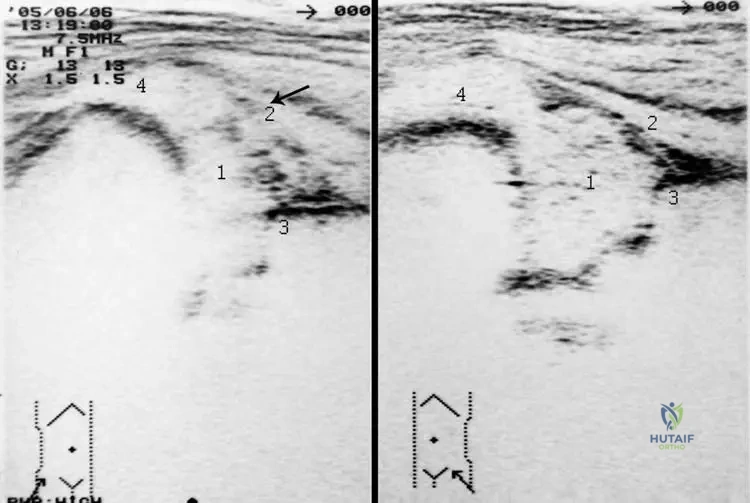
Explanation
Question 85
In the surgical treatment of neonatal septic arthritis of the hip, an anterior approach (Smith-Petersen) is often preferred for open arthrotomy and drainage. Which internervous plane is utilized in this surgical approach?
Explanation
Question 86
A 4-year-old boy presents with rhizomelic short stature, frontal bossing, midface hypoplasia, and trident hands. Which genetic mutation is responsible for his condition?
Explanation
Question 87
A 5-year-old child presents with a history of recurrent long bone fractures after minimal trauma, blue sclerae, and dentinogenesis imperfecta. What is the underlying biochemical defect in this disorder?
Explanation
Question 88
A 14-year-old male presents with chronic knee pain. Radiographs reveal a 2 cm well-circumscribed, lytic lesion in the distal femoral epiphysis with a sclerotic margin. Biopsy shows polyhedral mononuclear cells and "chicken wire" calcifications. What is the diagnosis?
Explanation
None
