ABOS Orthopedic Board Review: Scoliosis, Ankylosing Spondylitis, Bone Tumors & Dysplasias | Part 31
Key Takeaway
This ABOS Orthopedic Board Review covers key topics in spinal deformities like infantile, juvenile, and adolescent scoliosis, Scheuermann's kyphosis, and Ankylosing Spondylitis. It also delves into bone dysplasias such as fibrous dysplasia, enchondromas, osteochondromas, and Ewing's sarcoma, providing essential knowledge for orthopedic surgeons preparing for their board examinations.
ABOS Orthopedic Board Review: Scoliosis, Ankylosing Spondylitis, Bone Tumors & Dysplasias | Part 31
Comprehensive 100-Question Exam
00:00
Start Quiz
Question 1
A 62-year-old male with long-standing ankylosing spondylitis presents to the emergency department with new-onset mechanical neck pain after a low-energy fall from a standing height. Neurological examination is unremarkable. Standard AP and lateral radiographs of the cervical spine demonstrate extensive syndesmophytes but no obvious fracture. What is the most appropriate next step in management?
Explanation
Question 2
A 14-year-old boy presents with progressively worsening thigh pain and low-grade fevers. Imaging reveals a permeative diaphyseal lesion with an "onion-skin" periosteal reaction. Biopsy demonstrates sheets of small round blue cells. Which chromosomal translocation is most characteristically associated with this pathology?
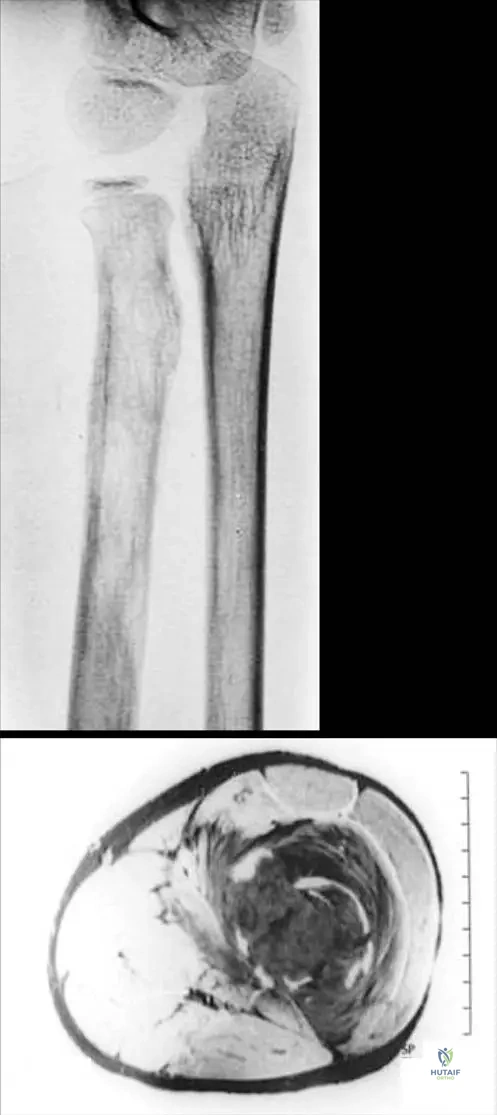
Explanation
Question 3
In the evaluation of congenital scoliosis, predicting the natural history of curve progression is critical. Which of the following congenital spinal anomalies has the highest rate of spontaneous curve progression?
Explanation
Question 4
The fundamental pathophysiology of achondroplasia involves a gain-of-function mutation in the FGFR3 gene. What is the specific effect of this mutation on the physeal growth plate?
Explanation
Question 5
A 55-year-old man presents with a painful, enlarging mass in his right hemipelvis. Biopsy confirms dedifferentiated chondrosarcoma. Staging scans are negative for metastasis. What is the mainstay of definitive treatment for this lesion?
Explanation
Question 6
A 14-year-old girl with adolescent idiopathic scoliosis has a progressive right thoracic curve that now measures 52 degrees. Her Risser stage is 4, and she has had menarche 2 years ago. What is the most appropriate management?
Explanation
Question 7
A 12-year-old girl is diagnosed with the bone tumor seen in the provided radiograph, characterized histologically by Homer-Wright rosettes and a strong PAS-positive reaction. Which immunohistochemical surface marker is characteristically highly expressed in this tumor?
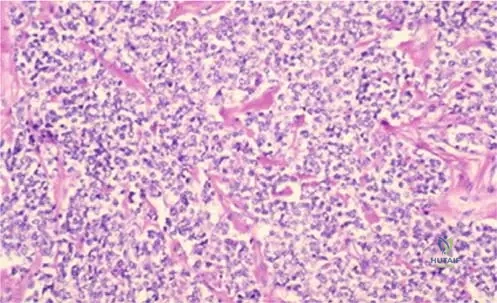
Explanation
Question 8
A 45-year-old man with advanced ankylosing spondylitis undergoes bilateral total hip arthroplasty due to severe secondary osteoarthritis and autofusion. Which postoperative complication is he at significantly higher risk for compared to the general THA population?
Explanation
Question 9
A 4-year-old child presents with frequent long bone fractures after minimal trauma, blue sclerae, and dentinogenesis imperfecta. Genetic testing confirms Osteogenesis Imperfecta. Which of the following describes the underlying molecular defect?
Explanation
Question 10
A 12-year-old non-ambulatory boy with Duchenne muscular dystrophy presents with a 45-degree thoracolumbar scoliosis and progressive difficulty maintaining a seated posture. Pulmonary function is declining but acceptable for surgery. What is the most appropriate surgical strategy?
Explanation
Question 11
Which of the following primary malignant bone tumors is classically associated with mutations in the retinoblastoma (RB1) gene and the TP53 gene?
Explanation
Question 12
A 60-year-old male with long-standing ankylosing spondylitis presents with a severe chin-on-chest deformity and a global sagittal imbalance preventing him from looking straight ahead. A lumbar pedicle subtraction osteotomy (PSO) is planned. Which vertebral level is most commonly chosen for a PSO to correct global sagittal imbalance?
Explanation
Question 13
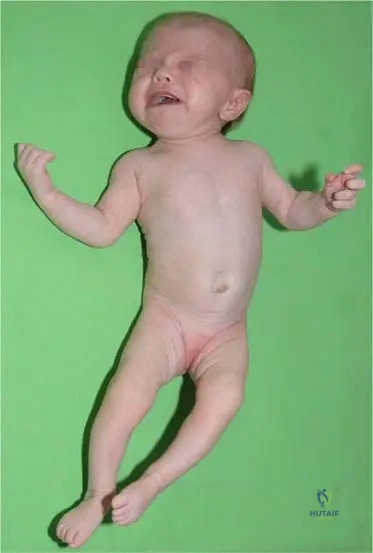
A newborn is evaluated for skeletal dysplasia. Physical examination reveals short-limbed dwarfism, bilateral rigid clubfeet, "hitchhiker" thumbs, and cystic swelling of the external ears (cauliflower ears). Which gene is most likely mutated in this patient?
Explanation
Question 14
In the Lenke classification system for adolescent idiopathic scoliosis, a lumbar modifier of "C" indicates the relationship between the center sacral vertical line (CSVL) and the apical lumbar vertebra. Which of the following defines a "C" modifier?
Explanation
Question 15
A 15-year-old male is diagnosed with Ewing sarcoma of the proximal fibula, as suggested by the aggressive periosteal reaction in the provided radiograph. Which of the following best outlines the standard modern treatment protocol for localized Ewing sarcoma?
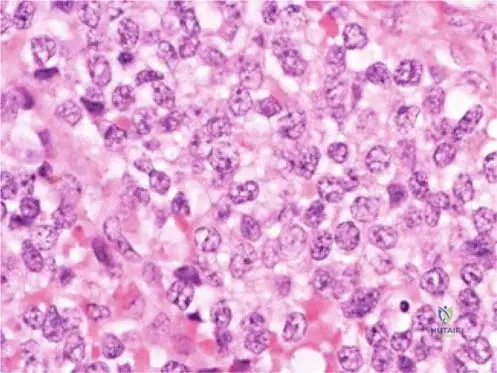
Explanation
Question 16
A 12-year-old boy presents with severe thigh pain, swelling, and low-grade fever. Radiograph shows a permeative diaphyseal lesion with an 'onion-skin' periosteal reaction. Which chromosomal translocation is most characteristically associated with this pathology?

Explanation
Question 17
A 55-year-old man with advanced ankylosing spondylitis sustains a minor ground-level fall. He complains of severe new-onset neck pain but is neurologically intact. CT scan shows a minimally displaced extension-distraction fracture through the C6-C7 disc space. What is the most appropriate management?
Explanation
Question 18
In the Lenke classification for adolescent idiopathic scoliosis, a curve characterized by a structural proximal thoracic curve, a structural main thoracic curve, and a non-structural thoracolumbar/lumbar curve is classified as which type?
Explanation
Question 19
What is the underlying genetic mutation and its functional effect in a patient presenting with achondroplasia?
Explanation
Question 20
Which of the following is the most significant adverse prognostic factor for overall survival in a patient with conventional high-grade osteosarcoma?
Explanation
Question 21
A 45-year-old man with ankylosing spondylitis and fused sacroiliac joints is scheduled for a total hip arthroplasty (THA). Which of the following is a key consideration regarding acetabular cup positioning to minimize the risk of postoperative dislocation?
Explanation
Question 22
A 2-year-old child presents with congenital scoliosis due to a fully segmented hemivertebra at T8. The curve has progressed 15 degrees over the last 6 months. What is the most appropriate surgical treatment?
Explanation
Question 23
A 60-year-old man presents with a painful shoulder. Radiographs reveal a large destructive lesion in the proximal humerus with 'ring and arc' calcifications. Biopsy confirms a grade II chondrosarcoma. What is the optimal treatment?
Explanation
Question 24
Which type of Osteogenesis Imperfecta is characterized by profound bone fragility, multiple in utero fractures, and is typically lethal in the perinatal period?
Explanation
Question 25
A 14-year-old presents with a destructive diaphyseal femur lesion. Biopsy reveals sheets of small round blue cells. Which immunohistochemical marker is highly sensitive and typically strongly positive in this tumor?

Explanation
Question 26
A patient with ankylosing spondylitis presents with a severe chin-on-chest deformity causing difficulty with forward gaze and swallowing. A cervical extension osteotomy is planned. Which anatomical level is most commonly chosen for correcting this specific deformity?
Explanation
Question 27
In a non-ambulatory patient with Duchenne muscular dystrophy, at what scoliotic curve magnitude is spinal fusion typically recommended to prevent severe pulmonary decline and loss of sitting balance?
Explanation
Question 28
A 7-year-old child presents with a waddling gait, knee pain, and short stature. Radiographs show delayed, irregular ossification of multiple epiphyses, but the spine is radiographically normal. Which gene mutation is most commonly associated with the autosomal dominant form of this condition?
Explanation
Question 29
Denosumab is increasingly used for unresectable or recurrent Giant Cell Tumor of bone (GCTB). What is its specific mechanism of action in this disease?
Explanation
Question 30
A 13-year-old girl with adolescent idiopathic scoliosis has a 35-degree right thoracic curve. Pelvic radiographs show ossification over the lateral 50% of the iliac apophysis, with no fusion to the ilium. What is her Risser stage?
Explanation
Question 31
A 16-year-old boy presents with nocturnal thigh pain that is dramatically relieved by NSAIDs. Imaging reveals a 7mm radiolucent nidus surrounded by dense sclerosis in the femoral diaphysis. What is the biochemical basis for the profound pain relief with NSAIDs?
Explanation
Question 32
What percentage of white patients with Ankylosing Spondylitis are positive for the HLA-B27 antigen, and what is the underlying inheritance pattern of the disease?
Explanation
Question 33
A patient presents with absent clavicles, delayed closure of cranial sutures, and supernumerary teeth. Which transcription factor gene is mutated in this autosomal dominant condition?
Explanation
Question 34
Differentiating an active enchondroma from a low-grade (Grade I) chondrosarcoma can be challenging. Which of the following radiographic features is most suggestive of a low-grade chondrosarcoma rather than a benign enchondroma?
Explanation
Question 35
A 14-year-old boy presents with a 2-month history of thigh pain. Radiographs show a permeative diaphyseal lesion with an 'onion-skin' periosteal reaction. Biopsy is performed.
Which of the following chromosomal translocations is most characteristic of this diagnosis?

Explanation
Question 36
A 55-year-old man with a 20-year history of ankylosing spondylitis sustains a low-energy fall. He complains of severe neck pain, but initial plain radiographs in the emergency department are read as negative. He subsequently develops bilateral upper extremity weakness. What is the most appropriate next step in management?
Explanation
Question 37
When evaluating a 14-year-old female with adolescent idiopathic scoliosis, the Center Sacral Vertical Line (CSVL) falls between the medial aspect of the pedicle and the lateral margin of the apical lumbar vertebra. According to the Lenke Classification system, what is the correct lumbar modifier?
Explanation
Question 38
A newborn is evaluated for frontal bossing, midface hypoplasia, and rhizomelic shortening of the limbs. Genetic testing confirms a gain-of-function mutation in the FGFR3 gene. Which physeal zone is primarily affected by this mutation?
Explanation
Question 39
A 12-year-old male is diagnosed with Ewing sarcoma of the pelvis.
Which of the following represents the most significant adverse prognostic factor for this patient?

Explanation
Question 40
A 48-year-old man with ankylosing spondylitis presents with a severe chin-on-chest deformity and loss of forward gaze. After thorough clinical and radiographic evaluation, a pedicle subtraction osteotomy (PSO) is planned. Which anatomical level is generally considered the safest and most effective for this procedure?
Explanation
Question 41
A newborn infant is noted to have a congenital scoliosis secondary to a fully segmented hemivertebra at T8. Which of the following screening examinations is mandatory as part of the initial workup?
Explanation
Question 42
A 2-year-old child presents with short-limbed dwarfism, hitchhiker thumbs, bilateral rigid clubfeet, and cystic swelling of the pinnae. What is the underlying genetic defect responsible for this condition?
Explanation
Question 43
A 16-year-old male presents with deep nocturnal aching in his proximal tibia that is dramatically relieved by ibuprofen. Radiographs show localized cortical thickening with a small 5mm radiolucent nidus. What is the primary mechanism by which the pharmacologic agent provides pain relief in this condition?
Explanation
Question 44
A 12-year-old non-ambulatory boy with Duchenne muscular dystrophy presents with a progressive scoliosis measuring 35 degrees. His forced vital capacity (FVC) is 45% of predicted. What is the most appropriate management regarding his spinal deformity?
Explanation
Question 45
A 45-year-old man with long-standing ankylosing spondylitis presents with localized, severe back pain after a bout of coughing. Radiographs reveal a destructive discovertebral lesion at T11-T12 with surrounding sclerosis and localized kyphosis. What is the most likely diagnosis?
Explanation
Question 46
A 10-year-old girl with Neurofibromatosis Type 1 (NF1) presents with a 40-degree sharp, short-segment thoracic scoliosis. Radiographs demonstrate severe vertebral scalloping and penciling of three adjacent ribs on the convex side. Which of the following is the most appropriate surgical strategy?
Explanation
Question 47
A 15-year-old boy completes neoadjuvant chemotherapy for a conventional osteosarcoma of the distal femur and subsequently undergoes wide local excision. Histopathologic analysis of the resected specimen shows 95% tumor necrosis. What is the clinical significance of this finding?
Explanation
Question 48
A 4-year-old child with a history of recurrent fractures, blue sclerae, and dentinogenesis imperfecta is started on intravenous pamidronate. What is the primary mechanism of action of this medication in treating this patient's underlying condition?
Explanation
Question 49
A 13-year-old premenarchal female with a Risser 0 score presents with a 24-degree right thoracic idiopathic scoliosis. What is the primary indication for initiating brace treatment in this patient?
Explanation
Question 50
A 45-year-old man with long-standing Ankylosing Spondylitis sustains a minor fall. He complains of severe lower cervical neck pain but is neurologically intact. Initial plain radiographs of the cervical spine are reported as negative. What is the most appropriate next step in management?
Explanation
Question 51
A 15-year-old boy presents with progressive knee pain and a palpable mass. Biopsy reveals small round blue cells. The provided radiograph is shown.
Which chromosomal translocation is most characteristically associated with this pathology?

Explanation
Question 52
A 6-month-old infant with achondroplasia presents with central sleep apnea, progressive hyperreflexia, and poor head control. What is the most likely anatomic cause of this presentation?
Explanation
Question 53
A 12-year-old girl is diagnosed with the bone lesion shown in the provided imaging.
Immunohistochemistry of the biopsy specimen is most likely to be strongly positive for which of the following cell surface markers?

Explanation
Question 54
A 14-year-old non-ambulatory male with spastic quadriplegic cerebral palsy presents with a 75-degree thoracolumbar scoliosis and significant pelvic obliquity. What is the most critical biomechanical objective when planning posterior surgical stabilization?
Explanation
Question 55
A 55-year-old man with ankylosing spondylitis presents with a severe chin-on-chest deformity. Preoperative planning for a single-level lumbar pedicle subtraction osteotomy (PSO) is performed. Which of the following best describes the expected sagittal correction from a single-level lumbar PSO?
Explanation
Question 56
A 12-year-old premenarchal female presents with a right thoracic adolescent idiopathic scoliosis (AIS) measuring 25 degrees. Her Risser stage is 0. Based on standard progression risk charts, what is her approximate risk of curve progression?
Explanation
Question 57
A 65-year-old male with long-standing ankylosing spondylitis presents after a low-energy fall with severe neck pain. CT reveals a highly displaced, unstable extension-type fracture through the C6-C7 disc space. Neurological exam is intact. What is the most appropriate definitive management?
Explanation
Question 58
An 11-year-old boy presents with progressive leg pain and fever. Radiographs show a permeative diaphyseal lesion with an "onion skin" periosteal reaction. Biopsy confirms the diagnosis.
Which genetic translocation is most commonly associated with this pathology?

Explanation
Question 59
A 4-year-old boy with achondroplasia presents with delayed walking. Physical examination reveals a flexible thoracolumbar kyphosis. What is the most appropriate initial management for his spinal deformity?
Explanation
Question 60
Which type of congenital vertebral anomaly carries the highest risk for rapid, relentless scoliosis progression during skeletal growth?
Explanation
Question 61
A 14-year-old female is diagnosed with Ewing sarcoma of the distal femur.
Which of the following is the most important prognostic factor for her overall survival?

Explanation
Question 62
A 45-year-old male with severe ankylosing spondylitis presents with a fixed thoracolumbar kyphosis. A pedicle subtraction osteotomy (PSO) is planned. Which anatomical level is typically the safest and most appropriate for a PSO to correct global sagittal imbalance?
Explanation
Question 63
A 10-year-old boy presents with multiple bony prominences around his knees and wrists.
He is diagnosed with Multiple Hereditary Exostoses (MHE). What is the underlying pathophysiology of this disorder?

Explanation
Question 64
A 15-year-old male presents with persistent distal femoral pain. Biopsy reveals high-grade osteosarcoma. Following neoadjuvant chemotherapy, surgical resection is performed. What percentage of tumor necrosis in the resection specimen is required to be considered a favorable response?
Explanation
Question 65
A 14-year-old non-ambulatory male with Duchenne Muscular Dystrophy (DMD) has a progressive 45-degree scoliosis. His FVC is currently 40% of predicted. What is the most appropriate management?
Explanation
Question 66
A 32-year-old female presents with an eccentric, lytic, epiphyseal lesion in the proximal tibia. Biopsy confirms Giant Cell Tumor (GCT). Which targeted medical therapy has proven effective as a neoadjuvant treatment for advanced or unresectable GCTs?
Explanation
Question 67
A newborn presents with multiple fractures, blue sclerae, and severe osteopenia. Which type of Osteogenesis Imperfecta is universally lethal in the perinatal period?
Explanation
Question 68
A 24-year-old male presents with chronic insidious-onset lower back pain that improves with exercise but not with rest. Which initial radiographic finding is most characteristic of early Ankylosing Spondylitis?
Explanation
Question 69
A 19-year-old male reports persistent nocturnal thigh pain that is completely relieved by ibuprofen. Imaging reveals a 7mm radiolucent nidus surrounded by reactive sclerosis in the femoral diaphysis. What is the standard, minimally invasive definitive treatment?
Explanation
Question 70
A 3-year-old child presents with a progressive 60-degree idiopathic scoliosis. What is the primary rationale for utilizing a growth-friendly construct rather than an immediate definitive spinal fusion?
Explanation
Question 71
In the multidisciplinary management of Ewing sarcoma of the extremity, what is the standard sequence of treatment?

Explanation
Question 72
A 12-year-old premenarchal female presents for evaluation of adolescent idiopathic scoliosis. Radiographs demonstrate a 28-degree right thoracic curve. Her Risser stage is 0. What is the most appropriate next step in management?
Explanation
Question 73
An 18-year-old male presents with a 6-month history of painful scoliosis. Imaging reveals a 3.5 cm expansile, radiolucent lesion in the posterior elements of L4. He reports the pain is dull, continuous, and not significantly relieved by NSAIDs. What is the most likely diagnosis?
Explanation
Question 74
A 55-year-old male with long-standing ankylosing spondylitis sustains a low-energy fall. CT imaging reveals an acute extension-distraction fracture through the T10-T11 ossified disc space. Due to the altered biomechanics of the ankylosed spine, this patient is at the highest risk for which of the following acute complications?
Explanation
Question 75
Achondroplasia is the most common form of short-limb dwarfism and frequently presents with spinal manifestations. Which of the following radiographic findings is a hallmark of the lumbar spine in patients with this condition?
Explanation
Question 76
A 10-year-old boy presents with progressive thigh pain and low-grade fever. Radiographs and subsequent MRI demonstrate a large permeative lesion in the femoral diaphysis.
Biopsy confirms Ewing sarcoma. Aside from the presence of metastasis, which of the following is an independent poor prognostic factor for survival?

Explanation
Question 77
In the evaluation of a 6-month-old infant with infantile idiopathic scoliosis, which of the following radiographic parameters is most highly predictive of curve progression?
Explanation
Question 78
A 60-year-old male presents with deep pelvic pain. Imaging reveals a 10 cm destructive iliac wing lesion with intralesional stippled and "popcorn" calcifications. Core biopsy confirms a Grade II conventional chondrosarcoma. What is the most appropriate definitive management?
Explanation
Question 79
Osteogenesis imperfecta (OI) leads to frequent fractures and progressive spinal deformity. According to the Sillence classification, which type of OI is characterized as perinatal lethal?
Explanation
Question 80
A 45-year-old male with severe ankylosing spondylitis presents with a fixed "chin-on-chest" deformity, rendering him unable to gaze horizontally. Surgical correction is planned. Which anatomic level is generally preferred for an extension osteotomy to correct this specific deformity?
Explanation
Question 81
A 14-year-old male undergoes 10 weeks of neoadjuvant chemotherapy for an osteosarcoma of the distal femur, followed by wide surgical resection. Histologic mapping of the resected specimen demonstrates 95% tumor necrosis. What is the significance of this finding according to the Huvos grading system?
Explanation
Question 82
A 13-year-old boy with Duchenne Muscular Dystrophy (DMD) has recently become wheelchair-bound. His forced vital capacity (FVC) is 50% of predicted, and standing radiographs reveal a progressive 35-degree thoracolumbar scoliosis with significant pelvic obliquity. What is the most appropriate management?
Explanation
Question 83
Denosumab is highly effective in the management of unresectable Giant Cell Tumors of bone. What is the exact mechanism of action of this pharmacological agent?
Explanation
Question 84
A neonate is evaluated for severe micromelic dwarfism. Clinical examination reveals a "hitchhiker" thumb, cauliflower ears, and rigid clubfeet. Radiographs of the spine are notable for severe kyphoscoliosis. A mutation in which of the following genes is responsible for this condition?
Explanation
Question 85
In predicting the natural history of congenital scoliosis, the morphological type of the vertebral anomaly is the most critical factor. Which of the following anomalies carries the highest risk for rapid and severe curve progression?
Explanation
Question 86
A 40-year-old male with long-standing, severe ankylosing spondylitis is scheduled to undergo bilateral total hip arthroplasty for debilitating hip ankylosis. Postoperatively, this specific patient population is at a drastically increased risk for which of the following complications?
Explanation
Question 87
A 9-year-old girl presents with an aggressive lytic lesion of the fibula.
Biopsy demonstrates uniform sheets of small round blue cells. Cytogenetics reveals a t(11;22) translocation. Which immunohistochemical marker is characteristically strongly positive in this tumor?

Explanation
Question 88
Scoliosis is the most common musculoskeletal manifestation of Neurofibromatosis Type 1 (NF1). When evaluating an NF1 patient with a progressive spinal deformity, which combination of radiographic features is pathognomonic for "dystrophic" scoliosis?
Explanation
Question 89
A 12-year-old premenarchal female (Risser 0) presents with a right thoracic adolescent idiopathic scoliosis curve measuring 35 degrees. According to the Bracing in Adolescent Idiopathic Scoliosis Trial (BRAIST), which of the following is the most appropriate recommendation to prevent curve progression to surgical magnitude?
Explanation
Question 90
A 55-year-old male with long-standing ankylosing spondylitis sustains an extension-distraction fracture through the C6-C7 disc space. Following posterior instrumentation and fusion, he experiences an unexpected postoperative neurological decline in the recovery room. What is the most likely cause of this complication?
Explanation
Question 91
A 15-year-old boy presents with progressive diaphyseal thigh pain. Radiographs demonstrate the lesion shown below.
A biopsy confirms a CD99 positive small round blue cell tumor. What is the most critical prognostic factor for overall survival in this patient?

Explanation
Question 92
A 4-year-old boy with frontal bossing, rhizomelic shortening, and a trident hand presents for an orthopedic evaluation. He has a known mutation in the FGFR3 gene. Which of the following best describes the pathophysiologic mechanism of his bone dysplasia?
Explanation
Question 93
A 14-year-old male with non-ambulatory spastic cerebral palsy presents with a progressive 85-degree thoracolumbar scoliosis and severe pelvic obliquity. Posterior spinal fusion to the pelvis is planned. What is the primary biomechanical advantage of utilizing S2-alar-iliac (S2AI) or iliac screws over traditional Galveston rod techniques?
Explanation
Question 94
A 16-year-old girl is undergoing treatment for a conventional high-grade osteosarcoma of the distal femur. Following neoadjuvant chemotherapy, she undergoes wide surgical resection. The pathology report indicates 95% tumor necrosis. What does this histologic finding predict?
Explanation
Question 95
A 28-year-old male with HLA-B27 positive ankylosing spondylitis presents with progressive sacroiliitis and morning stiffness. He has failed a 3-month trial of continuous treatment with two different nonsteroidal anti-inflammatory drugs (NSAIDs). According to current clinical guidelines, what is the most appropriate next pharmacological intervention?
Explanation
Question 96
A 6-year-old girl with multiple recurrent long bone fractures, blue sclerae, and dentinogenesis imperfecta is diagnosed with Osteogenesis Imperfecta (Type III). Her orthopedic surgeon recommends the initiation of intravenous pamidronate. What is the primary mechanism by which this medication improves bone density in this patient?
Explanation
Question 97
A 32-year-old female presents with an eccentric, lytic lesion in the proximal tibia extending to the subchondral bone. Biopsy confirms a Giant Cell Tumor of Bone (GCTB). Due to the tumor's proximity to the joint, neoadjuvant denosumab is planned to consolidate the lesion before curettage. What is the specific mechanism of action of denosumab?
Explanation
None
