Master ABOS Orthopedic Board Review: Skeletal Dysplasias, Bone Tumors, & Arthropathy | Part 13
Key Takeaway
Prepare for your ABOS Board Exam with this orthopedic review. It covers critical topics like skeletal dysplasias (achondroplasia, metaphyseal chondrodysplasia), osteoid osteoma, lipomas, stress fractures, hemophilic arthropathy, and CRPS. Master diagnosis and management for board success.
Master ABOS Orthopedic Board Review: Skeletal Dysplasias, Bone Tumors, & Arthropathy | Part 13
Comprehensive 100-Question Exam
00:00
Start Quiz
Question 1
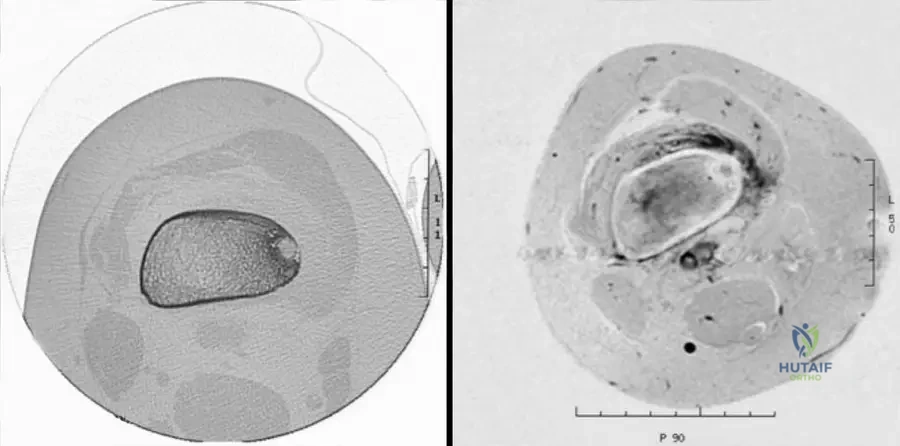
A 15-year-old boy presents with right thigh pain that is worse at night and dramatically improves with ibuprofen. Radiographs and CT show a cortically based lesion with a 1 cm radiolucent nidus surrounded by reactive sclerosis.
What is the primary molecular mediator responsible for this patient's characteristic pain?
Explanation
Question 2
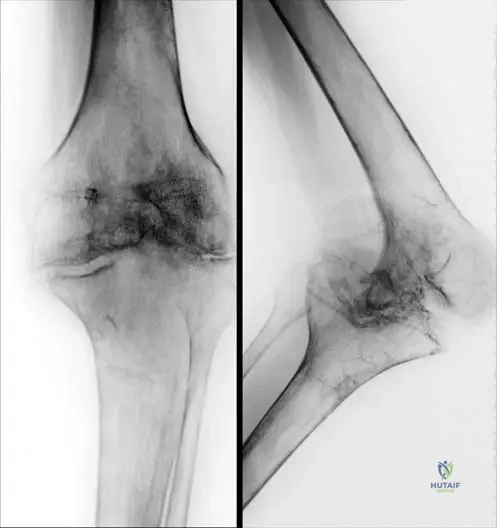
A 55-year-old woman is 8 weeks post-ORIF for a distal radius fracture. She presents with severe, burning pain, allodynia, and skin color changes in her hand. Radiographs reveal periarticular osteopenia.
Which of the following is the most established prophylactic measure to prevent this condition?
Explanation
Question 3
A 5-year-old child presents with short-limbed dwarfism, frontal bossing, and a trident hand. Radiographs show a narrowing of the interpedicular distances in the lumbar spine. What is the genetic basis of this skeletal dysplasia?
Explanation
Question 4
A newborn is diagnosed with Osteogenesis Imperfecta type II. This condition is typically lethal in the perinatal period. What is the fundamental molecular defect associated with this disease?
Explanation
Question 5
A 10-year-old boy presents with a waddling gait, joint pain, and stiffness. Radiographs show delayed and irregular ossification of the capital femoral epiphyses, but normal spine radiographs. A 'double-layer' patella is noted on lateral knee X-rays. Which gene is most commonly mutated?
Explanation
Question 6
A patient with Spondyloepiphyseal Dysplasia Congenita (SEDC) requires preoperative clearance for lower extremity osteotomies. Which of the following preoperative imaging studies is most critical for this patient?
Explanation
Question 7
A neonate is evaluated for short-limbed dwarfism, a 'hitchhiker' thumb, clubfeet, and swelling of the external ear (cauliflower ear). This condition is inherited in an autosomal recessive manner. What is the underlying pathophysiologic defect?
Explanation
Question 8
A 12-year-old girl is noted to have excessive shoulder mobility, allowing her to touch her shoulders together anteriorly. She also has delayed eruption of secondary teeth. A mutation in which of the following transcription factors is responsible?
Explanation
Question 9
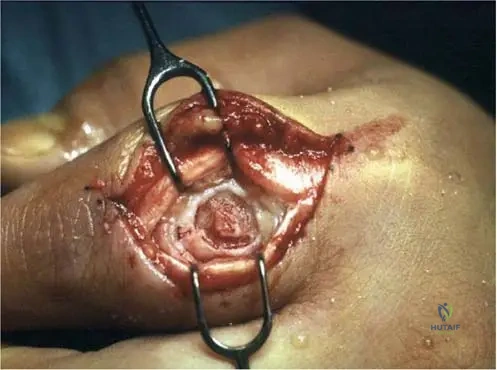
A 22-year-old male has an osteoid osteoma of the proximal femur treated with radiofrequency ablation.
What is the most critical anatomical structure to protect during ablation if the lesion is located in the posterior aspect of the femoral neck?
Explanation
Question 10
A 35-year-old woman presents with a large, lytic, epiphyseal lesion of the distal femur that extends to the subchondral bone. Biopsy confirms a Giant Cell Tumor of bone. Medical management with denosumab is planned. Denosumab targets which of the following?
Explanation
Question 11
A 14-year-old boy presents with fever, weight loss, and a diaphysial lesion of the femur with a 'periosteal onion-skin' reaction. Biopsy shows small round blue cells. The t(11;22) translocation associated with this tumor results in which fusion protein?
Explanation
Question 12
A 60-year-old man presents with dull, aching pain in his right pelvis. Radiographs reveal a large lytic lesion in the ilium with intralesional calcifications demonstrating a 'ring and arc' pattern. Biopsy confirms conventional high-grade chondrosarcoma. What is the mainstay of treatment?
Explanation
Question 13
A 30-year-old female complains of chronic knee swelling and locking. MRI demonstrates a large, nodular, intra-articular soft tissue mass with low signal intensity on both T1 and T2 weighted images (blooming artifact on gradient echo). Which medical therapy is FDA-approved for severe, unresectable cases of this condition?
Explanation
Question 14
A 14-year-old boy presents with progressive right thigh pain that is significantly worse at night and reliably relieved by ibuprofen. Radiographs reveal a cortical lesion with a central radiolucent nidus and surrounding reactive sclerosis.
What is the primary biochemical mediator responsible for this classic pain pattern?

Explanation
Question 15
A 16-year-old male presents with painful, progressive scoliosis. Imaging confirms the presence of an osteoid osteoma in the lumbar spine.
Where is this lesion most typically located relative to the scoliotic deformity?

Explanation
Question 16
A 50-year-old female presents 8 weeks after a distal radius fracture with severe, burning pain in her hand, hyperhidrosis, and trophic skin changes. Radiographs show patchy periarticular osteopenia.
According to the Budapest criteria for this condition, which clinical presentation is required for diagnosis?
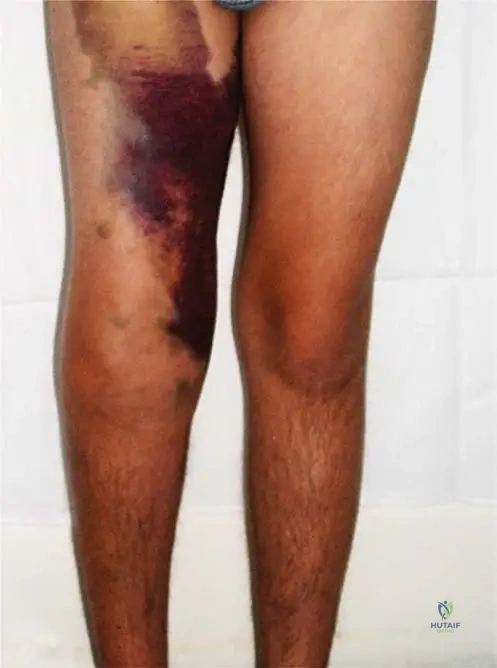
Explanation
Question 17
Which of the following prophylactic regimens is supported by prospective randomized controlled trials to reduce the risk of Complex Regional Pain Syndrome (Algodystrophy) following a distal radius fracture?
Explanation
Question 18
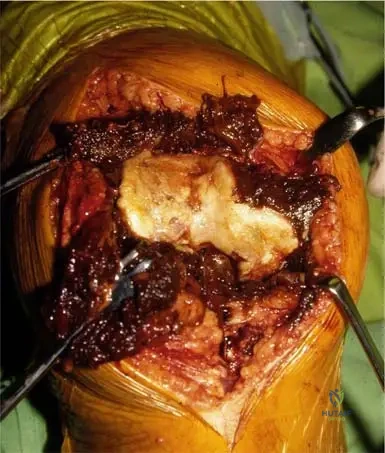
A 19-year-old male is undergoing definitive, minimally invasive treatment for a functionally limiting osteoid osteoma in the proximal femur.
During CT-guided radiofrequency ablation (RFA), what is the optimal target temperature and duration to ensure destruction of the nidus?
Explanation
Question 19
A 32-year-old female presents with knee pain. Radiographs show an eccentric, lytic lesion in the distal femoral epiphysis reaching the subchondral bone. Biopsy confirms Giant Cell Tumor of Bone. When utilizing Denosumab for unresectable disease, what is the specific molecular target?
Explanation
Question 20
A neonate is born with extremely short limbs, severe clubfeet, a 'hitchhiker' thumb, and cystic swelling of the ear pinnae (cauliflower ears). Radiographs show short, thick tubular bones. What is the underlying genetic defect?
Explanation
Question 21
A 12-year-old boy presents with a painful, enlarging mass in the mid-diaphysis of his femur. Radiographs show a permeative, 'onion-skin' periosteal reaction. Biopsy reveals uniform, small round blue cells that are CD99 positive. Cytogenetic analysis most commonly demonstrates which chromosomal translocation?
Explanation
Question 22
A 6-year-old boy presents with a waddling gait and bilateral knee pain. Radiographs reveal delayed and irregular ossification of multiple epiphyses and a characteristic 'double-layered' patella. A mutation in the gene encoding which protein is most commonly responsible?
Explanation
Question 23
A 55-year-old male with poorly controlled diabetes presents with a unilaterally swollen, erythematous, and warm foot without an open ulcer. Pedal pulses are strong. Radiographs reveal early fragmentation and subluxation of the tarsometatarsal joints. What is the most appropriate initial management?
Explanation
Question 24
A 10-year-old boy with severe Hemophilia A complains of progressive right knee pain and swelling following recurrent hemarthroses. What is the primary pathophysiologic mechanism driving irreversible cartilage destruction in hemophilic arthropathy?
Explanation
Question 25
A 60-year-old male is diagnosed with a Grade 2 conventional chondrosarcoma of the proximal humerus following an incisional biopsy. Staging reveals no metastatic disease. What is the standard definitive treatment?
Explanation
Question 26
A 65-year-old female with an 18-year history of rheumatoid arthritis is being evaluated prior to a total knee arthroplasty. Flexion-extension cervical spine radiographs reveal a 9 mm anterior atlanto-dens interval (ADI). What pathomechanical process is primarily responsible for this finding?
Explanation
Question 27
A 15-year-old girl is diagnosed with a conventional high-grade osteosarcoma of the distal femur. She completes a standard course of neoadjuvant chemotherapy before undergoing surgical resection. Which histological finding in the resected specimen is the most powerful predictor of long-term survival?
Explanation
Question 28
A 18-year-old male presents with chronic right thigh pain that is classically worse at night and dramatically relieved by NSAIDs. Radiographs show dense cortical thickening in the proximal femoral diaphysis. Advanced imaging confirms the diagnosis.
What is the gold standard minimally invasive treatment for this condition if medical management fails?

Explanation
Question 29
A 45-year-old female presents 6 weeks after non-operative management of a distal radius fracture. She describes severe burning pain out of proportion to the injury, alongside stiffness and shiny skin changes.
Which of the following prophylactic medications, if given at the time of injury, has been shown to reduce the incidence of this condition?

Explanation
Question 30
A 14-year-old boy presents with a painful left-sided thoracic scoliosis. The pain is severe at night and awakes him from sleep. A spinal osteoid osteoma is suspected. Where is the lesion most likely located in relation to his scoliotic curve?
Explanation
Question 31
A 4-year-old boy presents with disproportionate short stature, frontal bossing, and rhizomelic shortening of the limbs. Radiographs reveal narrowing of the interpedicular distances in the lumbar spine. What is the underlying genetic mechanism for this condition?
Explanation
Question 32
A 7-year-old boy presents with a waddling gait, bilateral knee pain, and mild short stature. Lateral knee radiographs demonstrate a classic "double-layer" patella. A diagnosis of Multiple Epiphyseal Dysplasia (MED) is suspected. A mutation in which gene is most commonly implicated?
Explanation
Question 33
A 2-year-old girl is evaluated for multiple low-energy long bone fractures. Physical examination reveals blue sclerae and mild joint hyperlaxity. Which of the following describes the most likely underlying pathophysiological defect?
Explanation
Question 34
A newborn presents with severe short-trunk dwarfism, a cleft palate, and bilateral rigid clubfeet. Radiographs reveal delayed ossification of the epiphyses and platyspondyly. A diagnosis of Spondyloepiphyseal Dysplasia Congenita (SEDC) is established. This condition is caused by a defect in which type of collagen?
Explanation
Question 35
A 55-year-old man presents with worsening deep pelvic pain. Radiographs demonstrate a large lytic lesion in the ilium with distinct "ring and arc" calcifications. Core needle biopsy confirms a low-to-intermediate grade primary malignant bone tumor. What is the standard of care for definitive management?
Explanation
Question 36
A 12-year-old boy presents with a 3-week history of severe right thigh pain, low-grade fever, and diaphoresis. Radiographs reveal a permeative diaphyseal lesion with an "onion skin" periosteal reaction. Which chromosomal translocation is most strongly associated with this diagnosis?
Explanation
Question 37
A 30-year-old female presents with progressive aching pain in her left knee. Radiographs reveal an eccentric, expansile, lytic lesion in the distal femur that extends directly to the subchondral bone without a sclerotic rim. If surgical curettage is chosen, what is the best recommended local adjuvant to reduce the recurrence rate?
Explanation
Question 38
A 10-year-old boy with severe Hemophilia A presents with a chronically swollen, boggy right knee and significantly restricted range of motion. Radiographs show advanced joint space narrowing and epiphyseal overgrowth. What is the primary cellular mechanism driving joint destruction in this condition?
Explanation
Question 39
A newborn is evaluated for multiple skeletal deformities including severe short stature, "hitchhiker" thumbs, cauliflower ear deformities, and severe rigid clubfeet. Which gene mutation is responsible for this patient's condition?
Explanation
Question 40
A 55-year-old male with poorly controlled diabetes mellitus presents with a massively swollen, warm, and erythematous right foot. He denies pain and lacks protective sensation. Radiographs reveal midfoot bony fragmentation, joint subluxation, and extensive debris. There are no skin ulcerations. What is the most appropriate initial management?
Explanation
Question 41
A 15-year-old male presents with severe pain and swelling of the distal femur. Radiographs reveal a mixed lytic and blastic metaphyseal lesion breaching the cortex, with a classic "sunburst" periosteal reaction and Codman's triangle. Where is the most common site of metastasis for this tumor?
Explanation
Question 42
An 8-year-old girl is referred for evaluation of unusually delayed tooth eruption. On examination, she is noted to have a large head, delayed closure of cranial sutures, and she is able to easily bring her shoulders together anteriorly. Which genetic mutation is highly characteristic of this condition?
Explanation
Question 43
A 65-year-old female presents with acute, intense pain, swelling, and warmth in her left knee. Aspiration yields cloudy synovial fluid. Microscopic analysis of the fluid reveals rhomboid-shaped crystals that exhibit weak positive birefringence under polarized light. What is the primary constituent of these crystals?
Explanation
Question 44
A 14-year-old female presents with an enlarging, painful bump on her proximal humerus. Radiographs show an eccentric, expansile, lytic lesion. MRI demonstrates prominent multiple fluid-fluid levels within the lesion. Which specific genetic rearrangement is most strongly linked to the primary form of this lesion?
Explanation
Question 45
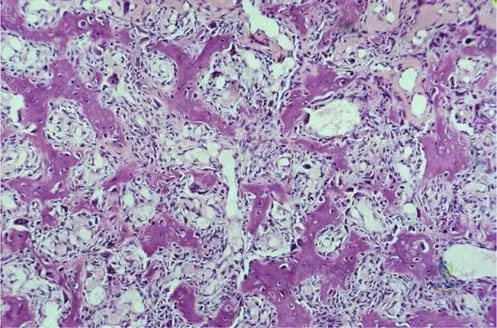
A 22-year-old male with chronic hip pain and stiffness shows poor response to NSAIDs. Radiographs reveal a small radiolucency in the intracapsular femoral neck with very minimal surrounding sclerosis.
Why do intra-articular osteoid osteomas typically lack the extensive, dense reactive bone sclerosis seen in extra-articular diaphyseal lesions?
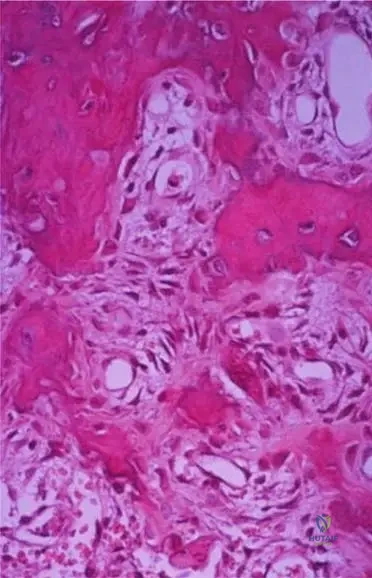
Explanation
Question 46
An 18-year-old male presents with persistent right anterior thigh pain that worsens at night. He reports significant relief of symptoms within 30 minutes of taking ibuprofen. Radiographs and a subsequent CT scan demonstrate a 1 cm radiolucent nidus surrounded by dense sclerotic bone in the femoral diaphysis.
If the patient cannot tolerate long-term NSAID therapy, what is the most appropriate first-line definitive intervention?

Explanation
Question 47
A 9-month-old infant with diagnosed achondroplasia presents with central sleep apnea, progressive lower extremity weakness, and hyperreflexia. What is the most likely anatomic etiology of these neurological symptoms?
Explanation
Question 48
A 14-year-old boy presents with progressive knee pain and a palpable mass over the distal femur. Radiographs reveal a mixed lytic and sclerotic lesion with a sunburst periosteal reaction and a Codman's triangle. Core needle biopsy confirms a high-grade intramedullary osteosarcoma. Following neoadjuvant chemotherapy and wide surgical resection, which of the following is the single most important prognostic factor for long-term survival?
Explanation
Question 49
A 55-year-old male with long-standing, poorly controlled type 2 diabetes presents with a swollen, erythematous, and painless right foot. The erythema resolves significantly when the leg is elevated. Radiographs reveal soft tissue swelling, periarticular osteopenia, and early fragmentation at the tarsometatarsal joint. What is the most appropriate initial management?
Explanation
Question 50
A 7-year-old girl is evaluated for multiple recurrent long bone fractures following minimal trauma. Clinical examination reveals bluish discoloration of the sclerae, joint hypermobility, and opalescent, discolored teeth. This patient's condition is most commonly caused by a mutation affecting which of the following?
Explanation
Question 51
An 11-year-old boy presents with fever, weight loss, and severe thigh pain. Radiographs show a large destructive diaphyseal lesion in the femur with a multi-layered "onion-skin" periosteal reaction. Cytogenetic analysis of the biopsy specimen reveals a t(11;22)(q24;q12) chromosomal translocation. This translocation results in the formation of which of the following fusion genes?
Explanation
Question 52
A 48-year-old female with a 15-year history of rheumatoid arthritis presents with progressive neck pain and intermittent "electric shock" sensations radiating down her arms when she flexes her neck. Flexion-extension cervical spine radiographs reveal an Anterior Atlanto-Dental Interval (AADI) of 11 mm and a Posterior Atlanto-Dental Interval (PADI) of 12 mm. What is the most appropriate management?
Explanation
Question 53
A 32-year-old female presents with knee pain. Radiographs demonstrate an eccentric, lytic, epiphyseal-metaphyseal lesion in the proximal tibia extending to the subchondral bone. Histopathology reveals abundant multinucleated giant cells distributed uniformly among mononuclear stromal cells. The neoplastic mononuclear cells in this tumor typically express high levels of which molecule to drive local bone destruction?
Explanation
Question 54
An 8-year-old child presents with a waddling gait, short stature, and bilateral knee pain. Radiographs demonstrate delayed, irregular, and fragmented ossification centers of the capital femoral epiphyses and distal femoral epiphyses, but the spine and skull appear completely normal. Mutations in which gene are most commonly associated with the autosomal dominant form of this dysplasia?
Explanation
Question 55
A 16-year-old male with severe Hemophilia A presents with chronic swelling, reduced range of motion, and joint destruction of the right knee. What is the primary pathophysiological mechanism that leads to progressive cartilage destruction in hemophilic arthropathy?
Explanation
Question 56
A 62-year-old male complains of a dull, deep ache in his right pelvis for the past 6 months. Radiographs reveal a large, ill-defined destructive lytic lesion in the right ilium with internal "ring and arc" calcifications. Core biopsy confirms a Grade 2 conventional chondrosarcoma. What is the most appropriate management strategy?
Explanation
Question 57
A 6-year-old child presents with short-limb dwarfism, a normal head circumference, and normal facial features. Radiographs show delayed epiphyseal ossification, flared metaphyses, and platyspondyly with central anterior beaking of the vertebrae. Which of the following best differentiates this condition from classic achondroplasia?
Explanation
Question 58
An 18-year-old male with Multiple Hereditary Exostoses (MHE) reports a rapid increase in the size of a palpable mass on his proximal femur accompanied by new, resting pain. MRI shows an osteochondroma with a cartilage cap thickness of 3 cm. Malignant transformation in this syndrome most frequently results in which of the following histological entities?
Explanation
Question 59
A 22-year-old male undergoes surgical excision of a cortically based bone lesion in his tibia. He had a long history of night pain dramatically relieved by salicylates.
Histologic examination of the central nidus of this lesion is most likely to demonstrate which of the following?

Explanation
Question 60
A 45-year-old female sustained a minor crush injury to her hand three months ago. She now presents with severe, burning pain that is disproportionate to the inciting event, significant allodynia, altered skin color, and asymmetric sweating.
She is diagnosed with Complex Regional Pain Syndrome (CRPS). Which of the following clinical features explicitly differentiates CRPS Type II from CRPS Type I?

Explanation
Question 61
A newborn is noted to have severe short-limb dwarfism, rigid bilateral clubfeet, "hitchhiker" thumbs, and cystic swelling of the pinnae of the ears (cauliflower ear). Radiographs show short, thick tubular bones. This autosomal recessive skeletal dysplasia is caused by a mutation in which of the following genes?
Explanation
Question 62
A 35-year-old asymptomatic female is found to have an incidental well-circumscribed, purely radiolucent lesion with internal stippled calcification in the proximal phalanx of her ring finger following a radiograph taken for a minor sprain. There is no cortical breakthrough or soft tissue extension. What is the most appropriate management?
Explanation
Question 63
A 12-year-old boy presents with an unusual ability to appose his shoulders anteriorly across his chest. Examination reveals an open anterior fontanelle, delayed eruption of his secondary dentition, and a somewhat prominent forehead. Radiographs show hypoplasia of the clavicles. Which essential transcription factor for osteoblast differentiation is mutated in this condition?
Explanation
Question 64
A 50-year-old male presents with severe, progressive back stiffness and large joint pain. Physical examination reveals dark, bluish-black pigmentation of the sclerae and ear cartilage. Radiographs of the spine exhibit profound, widespread calcification of the intervertebral discs. This specific arthropathy is secondary to a deficiency in which of the following enzymes?
Explanation
Question 65
A 15-year-old boy complains of diaphyseal tibial pain that is significantly worse at night and reliably relieved by ibuprofen. Imaging demonstrates a radiolucent nidus with dense surrounding sclerosis.
What is the primary chemical mediator responsible for the severe pain associated with this lesion?

Explanation
Question 66
A 55-year-old woman presents 6 weeks post-distal radius fracture with severe, disproportionate hand pain, diffuse swelling, and shiny, hypersensitive skin.
Which of the following is an evidence-based pharmacologic prophylactic measure that has been shown to reduce the incidence of this specific syndrome following distal radius fractures?
Explanation
Question 67
The parents of a child recently diagnosed with achondroplasia ask for genetic counseling. You explain that the condition is caused by a specific mutation in the FGFR3 gene. Which of the following best describes the pathophysiologic consequence of this mutation?
Explanation
Question 68
A 10-year-old boy with severe Hemophilia A presents to the emergency department with an acute, warm, and severely swollen right knee. What is the absolute most appropriate initial step in management for this acute hemarthrosis?
Explanation
Question 69
A 30-year-old female presents with mechanical knee pain. Imaging reveals an eccentric, purely lytic epiphyseal lesion of the distal femur extending to the subchondral bone. Biopsy confirms numerous multinucleated giant cells. Which of the following targeted systemic therapies is indicated for unresectable forms of this disease?
Explanation
Question 70
A 14-year-old boy presents with a painful diaphyseal femur mass, low-grade fever, and an elevated ESR. Radiographs demonstrate an ill-defined permeative lesion with a prominent "onion skin" periosteal reaction. Cytogenetic analysis of the biopsy is most likely to identify which of the following?
Explanation
Question 71
A 6-year-old child with blue sclerae, hearing loss, and a history of multiple low-energy fractures is diagnosed with Sillence Type I Osteogenesis Imperfecta (OI). Which of the following best describes the underlying collagen defect?
Explanation
Question 72
A 16-year-old male presents with severe, painful, and rigid scoliosis. Advanced imaging reveals a small radiolucent nidus with dense surrounding sclerosis in the posterior elements of the T8 vertebra.
In relation to the scoliotic curve, where is this lesion almost universally located?

Explanation
Question 73
A 60-year-old diabetic patient presents with a red, hot, swollen foot. Radiographs demonstrate acute bony fragmentation, joint subluxation, and periarticular debris. Inflammatory markers are mildly elevated, but there is no ulceration. This presentation corresponds to Eichenholtz Stage 1. What is the most appropriate initial management?
Explanation
Question 74
A 55-year-old male presents with a progressive, dull ache in his left pelvis. Radiographs show a large lytic lesion in the ilium with internal "popcorn-like" stippled calcifications. Biopsy confirms a grade II (intermediate) chondrosarcoma. What is the primary modality of treatment?
Explanation
Question 75
A 40-year-old male develops suspected Complex Regional Pain Syndrome (CRPS) following a crush injury to the foot.
If a triple-phase technetium-99m bone scan is performed to aid diagnosis, what is the classic imaging finding?

Explanation
Question 76
A 9-year-old child presents with a waddling gait, bilateral knee pain, and short stature. Radiographs demonstrate small, irregular, fragmented epiphyses and a characteristic "double-layered" patella. A mutation in which of the following genes is most highly associated with this specific classic presentation?
Explanation
Question 77
A 50-year-old patient presents with rapidly progressive, severe hip and knee osteoarthritis out of proportion to their age. During total knee arthroplasty, the articular cartilage is noted to be distinctly black and brittle. The underlying systemic disease is caused by an inherited deficiency in which enzyme?
Explanation
Question 78
A 16-year-old male presents with severe nocturnal thigh pain that resolves with ibuprofen. Radiographs and CT reveal a cortically based lesion in the proximal femur with a central radiolucency.
If this lesion were excised, what classic histologic feature would confirm the diagnosis?

Explanation
Question 79
A 52-year-old female presents with severe, burning hand pain, swelling, and shiny skin 10 weeks after open reduction and internal fixation of a distal radius fracture.
According to the Budapest Criteria, which of the following is an absolute requirement for the clinical diagnosis of Complex Regional Pain Syndrome (CRPS)?

Explanation
Question 80
A 4-year-old boy presents with short-limbed dwarfism, a waddling gait, and normal craniofacial features. Radiographs reveal delayed epiphyseal ossification and platyspondyly, but a normal interpedicular distance in the lumbar spine. Which gene mutation is most likely responsible for this condition?
Explanation
Question 81
A 35-year-old woman presents with a lytic lesion in the distal femur. Biopsy reveals a benign, locally aggressive tumor characterized by mononuclear stromal cells and numerous multinucleated giant cells. Which of the following describes the cellular target of denosumab in the medical management of this tumor?
Explanation
Question 82
A 65-year-old man undergoes resection of a large pelvic mass showing popcorn calcifications on radiographs. Histology confirms a low-grade malignant cartilage-forming tumor. Which of the following genetic mutations is most frequently associated with the conventional form of this tumor?
Explanation
Question 83
A 12-year-old boy presents with fever, weight loss, and mid-shaft femur pain. Radiographs reveal a permeative diaphyseal lesion with an onion-skin periosteal reaction. A t(11;22) chromosomal translocation is identified. What is the most specific immunohistochemical marker for this neoplasm?
Explanation
Question 84
A 2-year-old girl with blue sclerae and a history of multiple low-energy fractures is diagnosed with Osteogenesis Imperfecta (OI). Which of the following describes the most common underlying biochemical defect in the mildest and most common form of this disease (Type I)?
Explanation
Question 85
A 6-year-old child presents with a short trunk, severe coxa vara, a cleft palate, and high myopia. Radiographs show delayed ossification of the capital femoral epiphyses and platyspondyly. Which of the following mutations is responsible for this skeletal dysplasia?
Explanation
Question 86
A newborn is noted to have a large anterior fontanelle, midface hypoplasia, and excessive mobility of the shoulders, allowing them to be opposed anteriorly. A mutation in the RUNX2 (CBFA1) gene is suspected. What is the primary role of the protein encoded by this gene?
Explanation
Question 87
A 14-year-old male with severe Hemophilia A presents with chronic knee swelling and restricted range of motion. What is the primary pathophysiologic mechanism driving joint destruction in hemophilic arthropathy?
Explanation
Question 88
During a total hip arthroplasty on a 55-year-old man with severe degenerative joint disease and a history of dark urine, the surgeon notes that the articular cartilage is stark black. This condition is caused by a deficiency in which of the following enzymes?
Explanation
Question 89
A 16-year-old female presents with pain in her proximal tibia. MRI reveals an expansile, multiloculated lesion with prominent fluid-fluid levels. Genetic analysis confirms a translocation involving t(16;17). Which gene is upregulated as a result of this translocation?
Explanation
Question 90
A neonate is evaluated for short-limbed dwarfism, bilateral clubfeet, "hitchhiker" thumbs, and cystic swelling of the external ears (cauliflower ears). Which of the following pathophysiologic mechanisms best explains this patient's condition?
Explanation
Question 91
A 14-year-old boy presents with a painful scoliosis that is worse at night.
Imaging reveals an osteoid osteoma in the posterior elements of the thoracic spine. Which of the following is the most classic presentation of spinal deformity in this setting?

Explanation
Question 92
A 10-year-old boy with multiple painless bony bumps around his knees and shoulders is diagnosed with Multiple Hereditary Exostoses (MHE). What is the underlying molecular pathogenesis resulting from the most common genetic mutations in this disorder?
Explanation
Question 93
A 7-year-old girl presents with precocious puberty, a large café-au-lait spot with irregular "coast of Maine" borders on her torso, and a limp. Radiographs show a "ground-glass" expansile lesion in her proximal femur. The somatic mutation responsible for this syndrome occurs in which of the following genes?
Explanation
Question 94
A 5-year-old child with normal intelligence presents with short-trunk dwarfism, corneal clouding, and knock-knees. Radiographs demonstrate severe platyspondyly with anterior beaking of the vertebral bodies and odontoid hypoplasia. Which of the following substances is excessively accumulating in this patient's tissues?
Explanation
Question 95
A 15-year-old boy completes neoadjuvant chemotherapy followed by wide surgical resection for a high-grade conventional osteosarcoma of the distal femur. Pathological evaluation of the resected specimen is performed. Which of the following findings is the most significant predictor of long-term survival?
Explanation
Question 96
A 45-year-old woman is evaluated for a stiff, painful, and swollen ankle 8 weeks after a cast was removed for a non-operative distal fibula fracture.
What is the most characteristic early radiographic finding in a patient developing Complex Regional Pain Syndrome (CRPS)?

Explanation
Question 97
A 55-year-old male with poorly controlled type 2 diabetes presents with a swollen, warm, and erythematous foot without ulceration. Radiographs reveal fragmentation and destruction of the tarsometatarsal joints. According to the neurovascular theory of Charcot arthropathy, which of the following directly drives the increased osteoclastic bone resorption?
Explanation
Question 98
A 14-year-old male presents with a painful spinal deformity that is worse at night. Imaging reveals an osteoid osteoma in the right T10 lamina. Which of the following best describes the typical curve pattern and natural history of his scoliosis following definitive radiofrequency ablation of the nidus?
Explanation
Question 99
A 45-year-old woman presents 3 months after a conservatively managed distal radius fracture with severe hand pain, hyperalgesia, swelling, and shiny skin.
A triple-phase bone scan is ordered to aid in the diagnosis of Complex Regional Pain Syndrome (CRPS). Which of the following bone scan findings is most characteristic of this condition?

Explanation
Question 100
A 6-year-old boy presents with short stature, a waddling gait, and bilateral hip pain. Radiographs reveal flattened, irregular, and fragmented capital femoral epiphyses. His spine radiographs are completely normal with no vertebral body abnormalities. A mutation in the gene encoding which of the following proteins is most likely responsible for this patient's condition?
Explanation
None
