Minimally Invasive Percutaneous Osteotomy for Ankle Malunion with Gradual External Fixation: An Intraoperative Masterclass
Key Takeaway
This masterclass details a minimally invasive approach to correct complex ankle malunions following arthrodesis. We utilize a percutaneous Gigli saw osteotomy and gradual external fixation to achieve multiplanar realignment. Fellows will learn comprehensive anatomy, meticulous intraoperative steps, critical pearls to avoid pitfalls, and robust postoperative management strategies for successful patient outcomes.
Welcome, fellows, to the operating theater. Today, we're tackling a challenging case: a malunited ankle arthrodesis. These are not straightforward revisions, often fraught with compromised soft tissues and complex multiplanar deformities. Our approach, a minimally invasive percutaneous Gigli saw osteotomy combined with gradual external fixation, aims to optimize soft tissue preservation and achieve precise, multiplanar correction.
Understanding the Challenge: Malunited Ankle Arthrodesis
Ankle arthrodesis remains the gold standard for painful arthroses, instability, severe malalignment, and even joint sepsis when salvage is required. However, despite its efficacy, complications are not uncommon. We've seen nonunion rates as high as 30% and overall complication rates reaching 60% in the literature. Among these, malunion stands out as particularly detrimental due to its profound impact on functional outcome.
A malaligned ankle fusion leads to a cascade of problems: accelerated subtalar degeneration, reduced overall foot flexibility, compensatory foot deformities, and persistent, debilitating pain with ambulation. Correcting these deformities is paramount not only for pain relief but also to preserve the functional mobility of neighboring joints, which bear increased stress in the presence of malalignment.
Our technique specifically addresses these complex deformities through a subperiosteal Gigli saw osteotomy. This limits soft tissue compromise, which is critical in previously operated fields, and optimizes the environment for bone healing. The gradual correction afforded by external fixation allows for accurate multiplanar realignment—rotation, angulation, and translation—while simultaneously addressing any limb-length discrepancies.
Preoperative Planning and Patient Positioning
Thorough preoperative planning is the cornerstone of success in these complex cases.
Comprehensive Surgical Anatomy
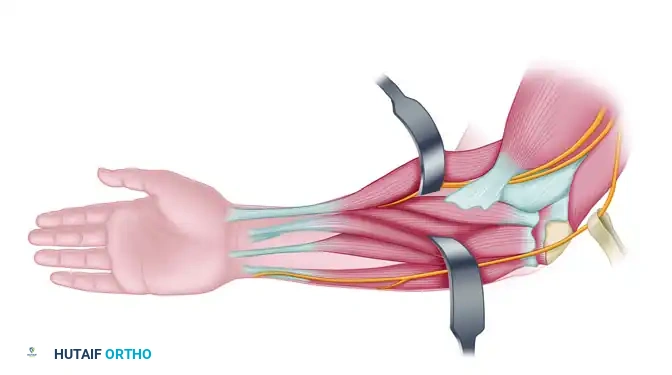
Before we even consider making an incision, let's review the critical anatomy of the distal tibia and ankle region. We are working in a tight space, often scarred, with vital neurovascular structures in close proximity.
- Anterior Compartment:
- Neurovascular Bundle: The deep peroneal nerve and anterior tibial artery and veins run closely along the interosseous membrane and anterior aspect of the tibia. Our subperiosteal dissection anteriorly must be meticulously performed to shield these structures.
- Tendons: The tibialis anterior, extensor hallucis longus, and extensor digitorum longus tendons are superficial to the neurovascular bundle. We must identify and protect them, especially the tibialis anterior, which serves as a key landmark for our first incision.
- Lateral Compartment:
- Tendons: The peroneal tendons (peroneus longus and brevis) lie superficial to the fibula. We'll encounter them during the lateral passage of our instruments and the Gigli saw. Care must be taken to avoid fraying or injury.
- Nerve: The superficial peroneal nerve typically pierces the deep fascia in the distal leg and becomes superficial, providing sensation to the dorsum of the foot. Its branches are at risk during lateral skin incisions and subcutaneous dissection.
- Posterior Compartment:
- Neurovascular Bundle: The posterior tibial artery, posterior tibial veins, and tibial nerve run within the tarsal tunnel, posterior to the medial malleolus, deep to the flexor retinaculum. Our posterior subperiosteal passage will be deep to the flexor tendons but superficial to this critical bundle.
- Tendons: The tibialis posterior, flexor digitorum longus, and flexor hallucis longus tendons (from anterior to posterior) lie posterior to the tibia and medial malleolus. The Gigli saw will pass deep to these structures during the posterior sweep.
- Medial Compartment:
- Nerve: The saphenous nerve and vein are superficial, along the medial aspect of the ankle. Our medial incisions must be thoughtfully placed.
- Osteology: We are targeting the previous fusion mass. Understanding its exact location, morphology, and the nature of the malunion (e.g., equinus, varus, valgus, translation) is crucial. A CT scan can be invaluable for 3D visualization.
Preoperative Imaging and Templating
Before the patient enters the room, we've already performed extensive imaging.
* Standard Radiographs: AP, lateral, and mortise views of the ankle, along with long-leg alignment films, are essential to quantify the multiplanar deformity and any associated limb-length discrepancy (LLD).
* CT Scan: For highly complex, multiplanar deformities or to delineate the precise morphology of the fusion mass and identify any areas of nonunion, a CT scan is invaluable. This allows for detailed 3D templating of the osteotomy.
* Correction Planning: We will use these images to determine the exact level of the osteotomy, typically through the previous fusion site, and to plan the desired final alignment: a plantigrade foot, with the calcaneal bisection line parallel or slightly valgus (0° to 2°) to the mid-diaphyseal line of the tibia in the axial plane. We also aim for a final limb length that is approximately 1 cm shorter than the unaffected limb, which helps prevent over-tensioning of the Achilles and provides a functional advantage.
Patient Positioning and Setup
Alright, team, let's get our patient positioned.
1. General Anesthesia: Our patient is already under general anesthesia.
2. Supine Position: We position the patient supine on the radiolucent operating table.
3. Ipsilateral Hip Bump: Crucially, we place an ipsilateral hip bump. This externally rotates the hip slightly, bringing the foot into a "foot-forward" position, which allows for optimal C-arm access for both AP and lateral fluoroscopic views without needing to reposition the patient or the C-arm excessively.
4. Tourniquet Placement: A nonsterile thigh tourniquet is applied high on the thigh. We'll inflate this only during the Gigli saw passage to minimize blood loss and improve visualization, then deflate it for fixator application.
5. Sterile Prep and Drape: The entire leg, from the toes up to the level of the tourniquet, is meticulously prepped with chlorhexidine or povidone-iodine solution and draped in the usual sterile fashion.
6. Fluoroscopy Setup: The C-arm is brought in and draped sterilely. We'll obtain initial AP and lateral views to confirm our planned osteotomy level.
7. Marking the Osteotomy: Under video fluoroscopy, using a sterile marking pen, we carefully indicate the desired level of the osteotomy on both the anteroposterior (AP) and lateral views of the distal tibia. This is typically through the previous fusion mass, ensuring we are in non-sclerotic, viable bone if possible. Once confirmed, the tourniquet is inflated to 300 mmHg or 100 mmHg above systolic pressure.
Step-by-Step Intraoperative Execution: The Percutaneous Osteotomy
Now, let's get scrubbed in and begin the percutaneous osteotomy. Remember, the goal here is to perform a subperiosteal osteotomy through the malunion site, minimizing soft tissue disruption.
Incision 1: Anteromedial Approach
- First Incision: "Alright, team, let's make our first incision. Using a #15 blade, make a small, approximately 1.5 to 2 cm transverse incision on the anteromedial aspect of the distal tibia. This incision is strategically placed just medial to the palpable tibialis anterior tendon. Palpate that tendon carefully, fellows, and ensure you're just medial to it. This provides a safe entry point and protects the tendon."
- Subperiosteal Dissection (Anterior): "Now, take a small curved Cobb elevator or a narrow periosteal elevator. Through this first incision, gently dissect down to the bone. Once on the periosteum, elevate it meticulously. We're creating a subperiosteal tunnel across the entire anterior aspect of the tibia, from this medial incision towards the lateral side. Keep the elevator firmly against the bone. This subperiosteal plane is critical – it protects the deep peroneal nerve, anterior tibial artery, and the extensor tendons lying anteriorly."
- Rocking Motion: "As you advance, use a gentle rocking motion with the elevator to ensure complete periosteal elevation across the anterior tibia at our planned osteotomy level. We want to feel the tip of the elevator reach the lateral aspect of the ankle malunion."
Incision 2: Anterolateral Exit
- Tenting the Skin: "Observe the lateral skin as the tip of your periosteal elevator pushes against it. You'll see the skin tenting. This is our guide. Make a small, vertical second incision, about 1.5 to 2 cm, directly over where the skin is tented by the elevator. This vertical orientation helps accommodate the saw passage."
- Suture Passage (Medial to Lateral): "Now, fellows, let's pass our guide suture. Take a curved tonsil hemostat and grasp a No. 2 Ethibond suture. Pass the hemostat and suture through our first (anteromedial) incision, following the previously created subperiosteal tunnel across the anterior tibia, and retrieve it through the second (anterolateral) incision. Confirm the suture is fully subperiosteal."
- Gigli Saw Attachment and Passage (Anterior): "Once the suture is through, attach one end of the Gigli saw, specifically the wire portion, to the Ethibond suture. Now, with gentle traction on the suture from the lateral side, pull the Gigli saw from medial to lateral through this same subperiosteal tunnel, anterior to the ankle fusion mass. Take your time, ensure smooth passage. We don't want to snag any soft tissues."
- Fluoroscopic Confirmation: "Stop right there. Before we proceed, let's get an image intensifier shot. Confirm the position of the Gigli saw. It must be precisely at the desired level of our osteotomy on both AP and lateral views. Adjust if necessary. This is a critical check to ensure we're cutting exactly where we planned."
Incision 3: Posterolateral Approach
- Posterior Subperiosteal Dissection: "Alright, with the saw confirmed, let's move to the posterior aspect. From our second (anterolateral) incision, take your periosteal elevator again. We're now going to pass it posterior subperiosteally. This passage will be behind the fibula, aiming for the posterolateral corner of the ankle malunion. Again, keep the elevator firmly against the bone to protect the peroneal tendons laterally and the posterior neurovascular structures."
- Tenting and Third Incision: "As the elevator extends posteriorly, you'll see the skin tenting posterolaterally. Make a small, vertical third incision at this point, again about 1.5 to 2 cm. Remove the elevator."
Incision 4: Posteromedial Exit and Circumferential Saw Passage
- Suture Retrieval (Posterior-Lateral to Lateral): "Now, we need to get the Gigli saw from the second incision to the third. Pass your curved tonsil hemostat from the third (posterolateral) incision, subperiosteally, to retrieve the Ethibond suture (which is still attached to the Gigli saw) from the second (anterolateral) incision. Carefully pull the suture and the attached Gigli saw through the third incision."
- Elevator Passage (Posterior-Lateral to Medial): "Next, we'll continue our posterior subperiosteal dissection. From the third (posterolateral) incision, extend the periosteal elevator subperiosteally posterior to the ankle malunion. This path will take us deep to the flexor tendons (tibialis posterior, FDL, FHL) and superficial to the posterior neurovascular bundle. We want to exit medially, just anterior to the posterior tibialis tendon."
- Tenting and Fourth Incision: "Observe the medial skin. Where the elevator tents the skin, make a transverse fourth incision. This will be on the posteromedial aspect of the ankle."
- Final Suture and Gigli Saw Passage (Posterior-Medial): "Using the curved tonsil hemostat again, pass it from the fourth (posteromedial) incision to the third (posterolateral) incision. Grasp the remaining Ethibond suture (still attached to the Gigli saw) and pull it through the fourth incision. At this point, fellows, the Gigli saw is now circumferentially around the ankle malunion, completely subperiosteal."
Surgical Warning: During the posterior passage of the Gigli saw, extreme care must be taken to maintain the subperiosteal plane and protect the peroneal tendons laterally and the posterior neurovascular bundle and flexor tendons medially. Any extra-periosteal dissection significantly increases the risk of neurovascular injury and soft tissue compromise.
The Osteotomy
- Gigli Saw Handles: "Attach both Gigli saw handles securely. Now, we're ready to cut. We'll use a controlled, reciprocating motion, cutting from lateral to medial across the bone."
- Controlled Cutting and Protection: "As you saw, keep your hands wide, maintaining tension, and use long, smooth strokes. The bone will start to give. Crucially, as you approach the medial side, just before the medial bone is completely cut through, STOP."
- Medial Soft Tissue Protection: "Now, take a fresh periosteal elevator. Pass it between the fourth (posteromedial) and first (anteromedial) incisions, directly crossing the Gigli saw. This elevator acts as a shield. Once it's in place, continue your cutting motion. The elevator will block further progression of the saw, thereby preventing any inadvertent medial soft tissue damage as the osteotomy completes. This is a vital step to protect the saphenous nerve and vein and the medial skin."
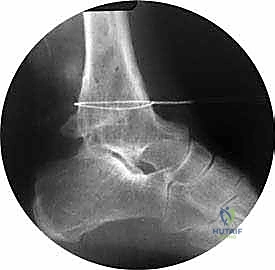
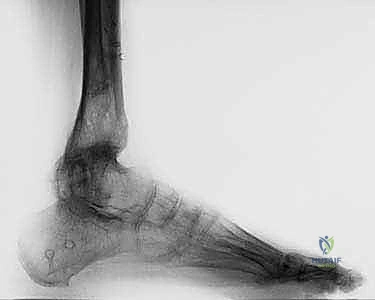
TECH FIG 2A: Lateral intraoperative radiographic view showing the Gigli saw passed at the level of the ankle malunion.
4. Confirm Completion: "Once the cut feels complete, remove the Gigli saw. Let's get a final image intensifier shot to confirm the osteotomy is complete and extends fully across the bone in both AP and lateral planes."
5. Tourniquet Deflation and Closure: "With the osteotomy confirmed, deflate the tourniquet. We should see minimal bleeding due to the subperiosteal nature of the cut. Irrigate the small incisions thoroughly. Close the small skin incisions with 3-0 or 4-0 absorbable sutures in a simple interrupted fashion. Apply sterile dressings."
External Fixation Application
With the osteotomy complete, our next step is to apply the external fixator. We'll use either an Ilizarov external fixator or a Taylor Spatial Frame (TSF), depending on the complexity and surgeon preference. Today, we'll demonstrate with a TSF, which offers precise multiplanar correction capabilities.
Principles of Frame Application
- Stable Fixation: The primary goal is to achieve stable fixation proximal and distal to the osteotomy site.
- Gradual Correction: The frame allows for controlled, gradual correction of the deformity and simultaneous lengthening if needed.
- Plantigrade Foot: Our ultimate aim is to achieve a plantigrade foot position with proper anatomical alignment.
Proximal Tibial Ring Application
- Proximal Ring Placement: "Let's start with our proximal ring. This full ring will be mounted on the distal tibia, well clear of our osteotomy site. It needs to be perpendicular to the long axis of the tibia in both the AP and lateral fluoroscopic views. Use your C-arm to confirm its orientation."
- Initial Wire Fixation: "We'll secure this proximal ring with a 1.8 mm smooth wire. Pass it from lateral to medial, crossing the distal tibia. Ensure it's perpendicular to the AP long axis of the tibia. Once in place, tension this wire appropriately using a wire tensioner. We're aiming for about 90-110 kgf of tension to provide rigid fixation."
- Half-Pin Augmentation: "To enhance stability, we'll add half-pins. Insert an anterior 6 mm half-pin into this ring, ensuring it's perpendicular to the tibia in the sagittal plane. Then, we'll add two additional 6 mm half-pins, either proximal or distal to the initial wire, in a delta fashion. These pins should also be perpendicular to the tibia in the sagittal plane, creating a stable construct for the proximal segment."
Distal Foot Ring Application
- Foot Ring Mounting: "Now for the distal foot ring. This ring needs to be mounted parallel to the plantar aspect of the foot. We'll use a foot board – a rigid intraoperative board that simulates weight-bearing – to ensure we achieve a true plantigrade position for the foot ring mounting. Place the foot firmly on the board and secure the ring parallel to it."
- Calcaneal Wires: "We'll secure the foot ring with 1.8 mm tensioned smooth wires. First, let's place two crossing calcaneal wires. These wires should pass through the calcaneus, providing strong fixation to the hindfoot. Tension them appropriately."
- Talar Wires: "Next, we need talar fixation. We'll place two talar wires. An oblique wire, typically from posterolateral to anteromedial, provides excellent rotational control. Additionally, a medial-to-lateral talar wire will further increase stability. For cases requiring subtalar joint distraction or compression, we can use the Russian technique by rotating the talar wire fixation bolts. This can provide compression across the osteotomy site by pushing proximally on the talus, if desired, or allow for fine adjustments."
- Forefoot Wires: "Finally, two forefoot wires will complete the distal fixation, ensuring the entire foot is rigidly held within the frame."
- Confirm Alignment: "Once all wires are in place and tensioned, check your fluoroscopy again. Ensure the distal foot ring is indeed parallel to the plantar aspect of the foot. At the end of correction, this will mean the foot and tibial rings will be parallel, confirming a plantigrade foot position."
Taylor Spatial Frame Assembly
- Strut Application: "With both proximal and distal rings securely fixed, we'll now connect them with six struts to complete the Taylor Spatial Frame. These struts are the workhorses of our gradual correction."

TECH FIG 2B: Lateral radiographic view showing posterior opening wedge of regenerate bone formation and posterior translation of the foot during distraction treatment with the Taylor spatial frame.
2. Computer Planning: "The frame is now built according to the patient's specific deformity. Post-application, we'll enter the frame parameters and radiographic deformity measurements into an Internet-based computer planning program. This program will generate a precise, daily patient turn schedule, detailing how much and in which direction each strut needs to be adjusted to achieve our planned correction."
3. Final Checks: "Perform a final check of all nuts, bolts, and wire tensions. Ensure all pins and wires are well-seated and there's no excessive skin tension around the pin sites. Apply sterile dressings around all pin sites."
💡 Pearls and Pitfalls
Here are some critical pearls and potential pitfalls to keep in mind for this procedure:
Surgical Warning: Optimal Ankle Alignment
- In the axial plane, the calcaneal bisection line should be parallel or slightly valgus (0° to 2°) and coincide with the mid-diaphyseal line of the tibia. This ensures neutral hindfoot alignment.
- The affected limb should ultimately be approximately 1 cm shorter than the unaffected limb. This slight shortening helps to prevent over-tensioning of the Achilles tendon and provides a functional advantage, particularly in activities requiring dorsiflexion.
- Obtaining proper alignment of an ankle fusion is paramount; even subtle malalignment can lead to significant functional limitations and adjacent joint degeneration.Pearl: Soft Tissue Preservation
- The subperiosteal Gigli saw osteotomy through a prior malaligned fusion site is key. It significantly limits soft tissue compromise compared to open osteotomies, optimizing the environment for bone and soft tissue healing in an often-scarred field.
- External fixation provides gradual, accurate multiplanar (rotation, angulation, and translation) realignment, while simultaneously correcting limb length. This gradual correction is far less traumatic to soft tissues than acute corrections.Pitfall: Neurovascular Injury
- Risk: Deep peroneal nerve, anterior tibial artery (anteriorly); tibial nerve, posterior tibial artery, flexor tendons (posteriorly); superficial peroneal nerve, peroneal tendons (laterally); saphenous nerve/vein (medially).
- Salvage: Meticulous subperiosteal dissection is the primary preventative measure. If injury is suspected (e.g., motor weakness, sensory deficit, pulselessness), immediately investigate. For nerve injury, consider neurolysis or repair. For vascular injury, immediate vascular surgery consultation for repair is mandatory.Pitfall: Incomplete Osteotomy
- Risk: If the Gigli saw cut is not complete, the bone will not move freely for correction, leading to persistent deformity or hardware failure.
- Salvage: Always confirm osteotomy completion with image intensifier in both AP and lateral views. If incomplete, consider using a small osteotome through a limited open approach, carefully protecting soft tissues, to complete the cut.Pitfall: Pin Site Infection
- Risk: Common complication, ranging from superficial cellulitis to deep osteomyelitis.
- Salvage: Meticulous daily pin site care is crucial. For superficial infections, oral antibiotics and increased local care. For deeper infections, consider targeted antibiotics, debridement, and potentially pin exchange or removal if severe. Education of the patient and caregivers is vital.Pitfall: Premature or Delayed Consolidation
- Risk: Bone healing too quickly before full correction, or too slowly leading
REFERENCES
-
Ahlberg A, Henricson AS. Late results of ankle fusion. Acta Orthop Scand 1981;52:103–105.
-
Ben Amor H, Kallel S, Karray S, et al. [Consequences of tibiotalar arthrodesis on the foot: a retrospective study of 36 cases with 8.5 years of follow-up]. Acta Orthop Belg 1999;65:48–56.