Masterclass in Operative Pediatric Orthopaedics and Spinal Surgery: Advanced Techniques and Biomechanics
Key Takeaway
This comprehensive masterclass details advanced operative techniques in pediatric orthopaedics and spinal surgery. Designed for residents and consultants, it provides evidence-based protocols for managing tibia vara, osteogenesis imperfecta, cerebral palsy deformities, slipped capital femoral epiphysis (SCFE), and complex spinal arthrodesis. Step-by-step surgical approaches, biomechanical principles, and postoperative management strategies are meticulously outlined to optimize clinical outcomes and minimize surgical complications.
Introduction to Advanced Pediatric and Spinal Orthopaedics
The operative management of pediatric orthopaedic conditions and complex spinal pathologies requires a profound understanding of evolving biomechanics, physeal anatomy, and neuromuscular physiology. Unlike adult orthopaedics, where the primary goal is often the restoration of pre-morbid anatomy, pediatric surgery must account for remaining growth, modulating forces to correct deformities over time.
This masterclass synthesizes the foundational operative techniques utilized in pediatric deformity correction, neuromuscular disorders (such as Cerebral Palsy), pediatric traumatology, and complex spinal arthrodesis. Designed for the practicing consultant and advanced fellow, this guide provides rigorous, step-by-step protocols, biomechanical rationales, and evidence-based postoperative management strategies.
Section 1: Pediatric Deformity Correction
Metaphyseal Osteotomy for Tibia Vara (Blount’s Disease)
Tibia vara, or Blount’s disease, is characterized by a progressive varus deformity, internal tibial torsion, and procurvatum secondary to a growth disturbance of the medial aspect of the proximal tibial physis.
Indications:
* Failure of conservative management (bracing) in infantile Blount’s disease (Langenskiöld stages II-IV).
* Adolescent Blount’s disease with significant mechanical axis deviation.
* Joint depression or physeal bar formation requiring concurrent elevation or resection.
Biomechanics:
The mechanical axis is shifted medially, creating a vicious cycle of asymmetric compressive forces across the medial physis (Heuter-Volkmann principle), further inhibiting medial growth. Osteotomy aims to overcorrect the mechanical axis slightly lateral to the center of the knee joint to unload the medial compartment.
Surgical Approach and Steps (Rab/Greene Techniques):
1. Positioning: Supine on a radiolucent table. A sterile tourniquet is applied. Fluoroscopy must be positioned to allow true AP and lateral views of the tibia.
2. Fibular Osteotomy: A mandatory first step to allow tibial correction. A lateral incision is made over the middle third of the fibula. The periosteum is incised, and an oblique osteotomy is performed.
> Surgical Warning: Meticulous subperiosteal dissection is required to protect the superficial peroneal nerve. Avoid the proximal third of the fibula to prevent common peroneal nerve injury.
3. Tibial Exposure: An anterior longitudinal or transverse incision is made distal to the tibial tubercle. The pes anserinus is retracted or partially elevated.
4. The Osteotomy: A dome, chevron, or opening/closing wedge osteotomy is performed distal to the tibial tubercle to avoid altering the patellofemoral mechanics. Guide pins are placed to dictate the plane of the cut.
5. Correction and Fixation: The distal fragment is translated laterally, externally rotated, and valgus is induced. Fixation is achieved via crossed Steinmann pins, a pediatric locking plate, or a circular external fixator (Ilizarov/Taylor Spatial Frame) for gradual correction in severe adolescent cases.
6. Postoperative Protocol: Non-weight-bearing (NWB) in a long-leg cast for 6 weeks if internal fixation is used. Pin removal occurs at 4–6 weeks post-radiographic union.
Osteogenesis Imperfecta: Sofield-Millar and Telescoping Rods
Osteogenesis imperfecta (OI) presents with profound bone fragility due to Type I collagen defects. The Sofield-Millar procedure (fragmentation and realignment) remains the gold standard for severe bowing.
Indications:
* Recurrent fractures of the femur or tibia.
* Severe diaphyseal bowing preventing ambulation or orthotic fitting.
Surgical Approach and Steps:
1. Exposure: A direct lateral approach to the femur or an anterior approach to the tibia.
2. Subperiosteal Dissection: The periosteum is incised longitudinally and carefully elevated. In OI, the periosteum is often thick and highly vascular, providing the primary osteogenic potential for healing.
3. Multiple Osteotomies: The diaphysis is sectioned into multiple cylindrical segments ("shish kebab" technique) using an oscillating saw.
4. Intramedullary Fixation: The segments are threaded onto an intramedullary device. Modern techniques utilize telescoping rods (e.g., Bailey-Dubow or Fassier-Duval) that expand as the child grows, preventing the rod from migrating out of the epiphysis.
5. Closure: The periosteal sleeve is meticulously closed over the bone segments to ensure rapid consolidation.
Section 2: Neuromuscular Orthopaedics (Cerebral Palsy)
The orthopaedic management of Cerebral Palsy (CP) focuses on preventing contractures, maintaining joint congruity, and optimizing the biomechanics of gait.
Combined One-Stage Correction of Spastic Dislocated Hip (San Diego Procedure)
Spastic hip dysplasia is driven by the overactivity of adductors and flexors, leading to progressive subluxation and eventual painful dislocation.
Indications:
* Reimer’s Migration Percentage (MP) > 40%.
* Painful, dislocated hip in a non-ambulatory patient (GMFCS IV-V) to allow sitting and perineal hygiene.
Surgical Approach and Steps:
1. Soft Tissue Release: Open adductor longus tenotomy and iliopsoas release at the lesser trochanter.
2. Femoral Varus Derotation Osteotomy (VDRO): A lateral approach to the proximal femur. A subtrochanteric osteotomy is performed. The distal fragment is externally rotated (to correct excessive femoral anteversion) and angled into varus (target neck-shaft angle 110°-120°). Fixation is achieved with a pediatric blade plate or locking proximal femoral plate.
3. Pelvic Osteotomy (Dega or San Diego): If acetabular dysplasia is present (acetabular index > 25°), an incomplete transiliac osteotomy is performed. The outer cortex is hinged over the triradiate cartilage, and a bone graft (often from the femoral shortening) is impacted into the osteotomy site to provide anterolateral coverage.
4. Capsulorrhaphy: The redundant capsule is plicated to ensure joint stability.
Clinical Pearl: In severe spasticity, avoid excessive varus (angles < 100°), as this can lead to greater trochanteric overgrowth, abductor weakness, and a paradoxical Trendelenburg gait in ambulatory patients.
Soft Tissue Lengthening: Achilles and Gastrocnemius
Equinus contracture is the most common deformity in CP. Differentiating between isolated gastrocnemius tightness and combined gastrocnemius-soleus tightness is critical (Silfverskiöld test).
- Strayer Procedure (Gastrocnemius Recession): Indicated for isolated gastrocnemius contracture. The gastrocnemius aponeurosis is sectioned distal to the musculotendinous junction, sparing the soleus.
- Z-Plasty or Percutaneous Achilles Lengthening (TAL): Indicated for combined contractures.
> Surgical Warning: Over-lengthening the Achilles tendon in a spastic patient is a catastrophic error, leading to an irreversible calcaneus gait and crouch stance. Always under-lengthen slightly and cast in neutral, never in maximum dorsiflexion.
Section 3: Pediatric Traumatology
Slipped Capital Femoral Epiphysis (SCFE)
SCFE involves the translation of the femoral neck anterolaterally while the epiphysis remains in the acetabulum.
Indications:
* All confirmed cases of SCFE require urgent surgical stabilization to prevent further slippage and minimize the risk of avascular necrosis (AVN).
Surgical Approach and Steps (In Situ Fixation):
1. Positioning: Supine on a fracture table. Crucial: Do not forcefully reduce a chronic or stable slip, as this drastically increases the risk of AVN. Positional reduction (gentle internal rotation) is acceptable only in acute, unstable slips.
2. Entry Point: Using fluoroscopy, the entry point is identified on the anterior base of the femoral neck.
3. Guide Wire Placement: A guide wire is advanced perpendicular to the physis. It must remain strictly within the center of the epiphysis on both AP and lateral views.
4. Screw Fixation: A single, partially threaded cannulated screw (typically 6.5mm or 7.3mm) is advanced. The threads must fully cross the physis and engage the epiphysis without penetrating the joint space.
5. Approach to the Contralateral Hip: Prophylactic pinning of the contralateral hip is strongly considered in patients with endocrinopathies, renal failure, or those under 10 years of age.
Pitfall: The "blind spot" of the femoral head. Because the epiphysis is displaced posteriorly, a screw that appears central on the AP view may be exiting the anterior neck on the lateral view. Always utilize the "approach-withdraw" fluoroscopic technique to confirm the screw is entirely intraosseous.
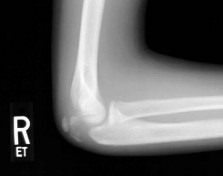
Supracondylar Humerus Fractures
Biomechanics: Extension-type fractures (95%) result from a fall on an outstretched hand, causing the olecranon to act as a fulcrum, driving the distal fragment posteriorly.
Operative Technique (Closed Reduction and Percutaneous Pinning - CRPP):
1. Reduction: Traction is applied with the elbow in extension and supination to unlock the fragments. Medial/lateral translation is corrected. The elbow is then hyperflexed while applying anterior pressure to the olecranon to correct posterior displacement.
2. Pinning: Two or three lateral-entry smooth K-wires (1.6mm or 2.0mm) are placed in a divergent or parallel configuration.
3. Crossed Pins vs. Lateral Pins: While crossed pins (one medial, one lateral) offer superior torsional biomechanical stability, the medial pin carries a documented risk of iatrogenic ulnar nerve injury. Modern evidence strongly supports the use of 2-3 divergent lateral pins, which provide equivalent clinical stability without the ulnar nerve risk, provided the pins engage both the medial and lateral columns.
Section 4: Spinal Anatomy and Surgical Approaches
Spinal surgery demands an exacting knowledge of neurovascular anatomy. The approaches detailed below are foundational for trauma, deformity (scoliosis/kyphosis), and degenerative conditions.
Anterior Cervical Approach (Smith-Robinson)
Indications: Cervical disc herniation, cervical spondylotic myelopathy, anterior column fractures, and infections (C3-C7).
Surgical Steps:
1. Incision: A transverse incision is made within a natural skin crease, typically on the left side to decrease the risk of recurrent laryngeal nerve injury (the left nerve has a more predictable, vertical course).
2. Superficial Dissection: The platysma is divided in line with the incision. The superficial cervical fascia is incised anterior to the sternocleidomastoid (SCM) muscle.
3. Deep Dissection: The dissection proceeds through the avascular plane between the carotid sheath (carotid artery, internal jugular vein, vagus nerve) laterally, and the visceral axis (trachea, esophagus, thyroid) medially.
4. Prevertebral Fascia: The prevertebral fascia is identified and incised longitudinally to expose the longus colli muscles and the anterior longitudinal ligament (ALL).
5. Exposure: The longus colli muscles are elevated subperiosteally, and self-retaining retractors are placed beneath their medial borders to protect the sympathetic chain.
Posterior C1-C2 Fusion (Harms Technique)
Indications: Atlantoaxial instability (e.g., Down syndrome, rheumatoid arthritis, odontoid fractures).
Biomechanics: The Harms construct (C1 lateral mass screws and C2 pedicle or pars screws) provides rigid, 3-column biomechanical stability, eliminating the need for postoperative halo immobilization and offering superior fusion rates compared to traditional wiring techniques (Gallie/Brooks).
Surgical Steps:
1. Positioning: Prone, with the head secured in a Mayfield clamp. The neck is positioned in a neutral or slightly extended posture to reduce C1-C2 subluxation.
2. Exposure: A midline posterior incision from the inion to C3. The paraspinal musculature is elevated off the posterior arch of C1 and the lamina of C2.
3. C1 Lateral Mass Screws: The C2 nerve root is retracted inferiorly. The entry point is at the intersection of the posterior arch and the midpoint of the C1 lateral mass. The drill is directed 10°-15° medially and 15° cephalad to avoid the vertebral artery laterally and the atlanto-occipital joint superiorly.
4. C2 Pedicle/Pars Screws: The entry point for a C2 pedicle screw is in the cranial and lateral quadrant of the C2 isthmus. The trajectory is 20°-30° medial and 20° cephalad.
> Surgical Warning: Preoperative CT angiography or high-resolution MRI is mandatory to evaluate for anomalous vertebral artery anatomy (e.g., a high-riding vertebral artery or a ponticulus posticus), which precludes the use of standard C2 pedicle screws. In such cases, C2 translaminar screws (Wright technique) are the safest alternative.
5. Rod Placement and Bone Grafting: Polyaxial screw heads are aligned, and a titanium or cobalt-chrome rod is secured. The posterior arch of C1 and lamina of C2 are decorticated, and autologous iliac crest bone graft is packed into the interlaminar space.
Thoracic and Lumbar Segmental Fixation (Pedicle Screws)
Indications: Scoliosis, spinal trauma, tumor resection, and spondylolisthesis.
Biomechanics: Pedicle screws traverse all three columns of the spine, providing the most rigid construct available. They resist pull-out, bending, and rotational forces far better than hooks or sublaminar wires.
Surgical Steps:
1. Exposure: Standard posterior midline approach, exposing the spinous processes, laminae, facet joints, and transverse processes.
2. Entry Point Identification:
* Thoracic Spine: The intersection of the bisected transverse process and the lateral border of the superior articular facet.
* Lumbar Spine: The intersection of the pars interarticularis, the base of the superior articular process, and the midline of the transverse process.
3. Preparation: The cortex is burred, and a pedicle probe is advanced down the cancellous channel of the pedicle into the vertebral body. The trajectory converges medially (more convergence in the lumbar spine than the thoracic spine) and parallels the superior endplate.
4. Verification: A ball-tipped feeler is used to palpate the five walls of the pedicle tract (medial, lateral, superior, inferior, and anterior) to ensure no cortical breaches have occurred.
5. Screw Insertion: The appropriately sized pedicle screw is inserted. Intraoperative fluoroscopy or neuro-navigation (O-arm) is utilized to confirm placement before rod reduction.
Conclusion
Mastery of operative orthopaedics in the pediatric and spinal domains requires an uncompromising dedication to anatomical precision and biomechanical principles. Whether executing a complex metaphyseal osteotomy for Blount's disease, navigating the distorted anatomy of a spastic hip in Cerebral Palsy, or placing instrumentation millimeters from the vertebral artery, the surgeon must rely on rigorous preoperative planning and meticulous intraoperative execution. Adherence to the evidence-based techniques outlined in this masterclass will ensure optimal functional outcomes and minimize the risk of catastrophic complications in these vulnerable patient populations.
You Might Also Like